Management of Migraine: Part I
Author: James R. Couch, MD, PhD, Professor and Chair, Department of Neurology, University of Oklahoma Health Sciences Center, Oklahoma City, Okla.
Editor’s Note—Part I of this manuscript will discuss the definition of the primary headaches, the pathophysiology of migraines, diagnosis, and medical therapies, as well as the background and pharmacology of triptans. Part II will discuss the use of triptans, preventive therapies, prophylactic agents, chronic tension-type headaches, and cluster headaches.
Epidemiology
Headache has been termed the most common symptom of migraines. In an earlier study, Management of Migraines, based on patient’s attending primary care physician’s offices indicated that more than 60% of the patients had headache as a primary or secondary complaint. Another study of 1600 nonclinic subjects found that 90% of these had had a headache in the previous year, and half of those had had a severe headache. Headache is typically divided into primary (idiopathic) or secondary (organic) headache. Secondary headaches are those resulting from a definable pathophysiologic process occurring in the head or neck such as meningitis, subarachnoid hemorrhage, intracerebral hemorrhage, sinusitis, mastoiditis, etc. Primary headaches are those for which the headache itself is the primary problem and there is not another definable pathophysiologic process that produces a problem other than the headache syndrome. The major primary headaches are migraine, tension, and cluster headaches. Of these, migraine is the entity for which patients will most often seek medical help. Tension headache, while more common, is less likely to be severe enough to be the primary reason for which the patient will see a physician.
Tension headache occurs in 65-70% of the population. Cluster headache is an unusual entity that occurs in less than 0.5% of the population. In a recent study by Stewart and Lipton looking at a population and asking about headache occurrence in the last year, migraine occurred in approximately 7% of the men and 18% of them women. Studies from Europe with a definite different methodology in looking at lifetime occurrence suggested that migraine may occur in up to 33% of women and 13% of men.
The onset of migraine may be at any age; however, 70% of migraineurs have their first headache before age 30 and 95% before age 65. Many times, in older patients with apparent new onset of headache, careful questioning will be elucidating the occurrence of migraine at an earlier age.
Definition of the Primary Headaches
Migraine
Migraine is a syndrome with symptoms that extend well beyond pain and whose manifestations may be divided into 5 areas:
• Pain;
• Symptoms of general irritability (photophobia, phonophobia, osmophobia);
• Gastrointestinal symptoms (nausea, vomiting, diarrhea);
• Neurologic symptoms (teichopsia or sensations of flashing lights, whether informed or unformed patterns, visual loss, hemiparesis, hemisensory loss, aphasia/dysphasia, loss of consciousness or vertigo are the major neurologic features); and
• Mood changes (irritability, depression, euphoria, dysphoria).
The pain may be unilateral or bilateral, throbbing, pressure-like, focal or generalized and ranging from mild to very intense. In addition, the patient may have brief sharp stabs of pain occurring focally in one area of the head. At times the pain may be very severe in the neck and even radiate into the arm or upper chest. Nausea, photophobia, and phonophobia are seen in 85-90% of migraineurs. Visual symptoms may be seen in around 50% and the other neurologic symptoms in 10-25%. Individual patients may not manifest all symptoms with every headache. At times the headache may consist primarily of severe pain and at other times, the patient may have more prominent irritability, gastrointestinal, or neurologic symptoms with relatively minimal pain (migraine-sans-migraine).
Cluster Headache
Cluster headache is a syndrome in which there is always pain around one eye and the pain is always unilateral. Usually the pain has rapid onset over 5-10 minutes with pain ascending to an intense peak lasting 15-90 minutes and then remitting relatively rapidly. The Patient may have residual soreness in the area of the cluster headache for the next one to several hours. These headaches are very stereotyped and occur in episodes or clusters with the episode lasting 8-16 weeks. Typically the patient starts with the frequency of one to several per week and builds to a frequency of several per day over 1-3 weeks. After a few to 12 weeks, there is gradual waning of the frequency and then remission of the headaches. Cluster headache cycles tend to occur 1-2 times per year but may skip several years at times. Cluster headache tends to occur in males 3-4:1 over females while migraine occurs 2-1 in females over males.
Tension Headache
Tension headache is typically a less severe headache that may be unilateral or bilateral and is not associated with any of the migraine or cluster headache feature given above. It is quite common for migraine headaches to have intermittent tension headaches along with their migraine if the migraine becomes more frequent.
Pathophysiology of Migraine
The pathophysiology of migraine is unknown. Current theory attributes migraine primarily to the trigeminal vascular system. In this model, nerve endings from the trigeminal nerve that end on cranial blood vessels release calcitonin G-related protein (CGRP) into the wall of these blood vessels causing edema and pain in that area of the artery. These pain signals are transmitted to the trigemino-caudal nucleus (spinal V nucleus) in the pons and medulla. These impulses are then transmitted to the cerebral cortex. Other neural influences play a role in a cortical phenomenon termed spreading neuronal depression or spreading depression, which seems to have a major part in generation of the migraine headache. Space does not permit a more detailed explanation of these theories. Please refer to references 14, 15, 17, and 24 for further information.
Diagnosis
It is critical to establish a correct diagnosis. Establishing a profile of critical features of the headache is very helpful. Table 1 provides an outline of the essential features for a headache profile. Figure 1 provides an algorithm of approach to the headache patient. The first consideration is to rule out secondary or organic headache. Once this has been done, elucidation of the primary headache type can be carried out. As a short definition, migraine can be defined as a recurrent headache over a number of years that is relatively stereotyped, not associated with neurologic signs or progressive neurologic deterioration, and is associated with nausea, photophobia, and phonophobia.
 |
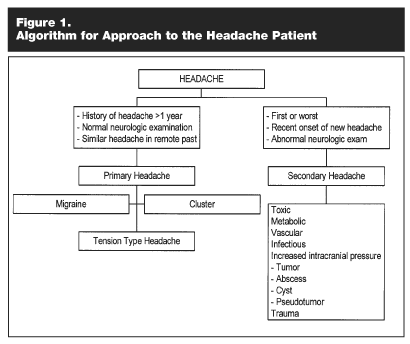 |
As far as diagnostic studies, the CT scan and the MRI scan are very helpful in ruling out intracranial pathology, especially in patients that have a new onset headache. In patients with a headache that has been present and unchanged for many years and who have a normal neurologic examination, imaging studies are likely to be normal and a diagnostic payoff is small here. Other diagnostic studies would include the chem 20 and CBC to help rule out toxic or metabolic origin of the headache. Endocrine studies are seldom helpful if there are not other indications of endocrinopathy.
The differential diagnosis of migraine is both short and long. The major issue is to distinguish between primary and secondary headaches. Migraine is essentially a diagnosis of exclusion. The possibility of a secondary headache must first be given strong and thorough consideration. Once secondary headache has been ruled out, then a shorter list of headaches causes migraine, tension, and cluster headache to be the most common primary headaches. There is certainly a number of other less common primary headaches, but these 3 constitute the large majority of problems. As indicated above, a primary headache that is associated with nausea, photophobia, phonophobia, and worsening by movement is very likely to be a migraine headache. If the headache has been recurrent and relatively stereotyped over a number of years and is associated with a normal neurologic examination, chances that the headache is migraine become very large. Cluster headache can be recognized by its pattern as described above. Tension headache as a brief clinical definition, is a primary headache without features of migraine or cluster headaches.
With regard to the organic headaches, this topic is really beyond the scope of this article. Figure 1 has a brief overview of the organic headaches. Several situations should be mentioned for which the primary care physician should always be on the lookout. First is the problem of subarachnoid hemorrhage, which typically causes a new onset headache and is often the worst headache of the patient’s life. The patient may remain awake or become rapidly somnolent and comatose. Usually, the headache is associated with meningismus. Anterior flexion of the neck evokes muscle spasm in the neck and frequently flexion of the legs to shorten an inflamed thecal sac (Koenig’s Sign) or straight leg raising elicits pain in the back as well as the neck again by stretching the thecal sac (Brudzinski’s Sign). The patient may have a history of having brief leaks of blood from the aneurysm into the subarachnoid space and have transient headaches prior to the major hemorrhage (sentinel headache).
Second, the problem of temporal arteritis (giant cell arteritis) is one that occurs in older patients, usually older than 60 years, and becomes more common as the patient gets older. There is no characteristic headache for temporal arteritis and the pain may be unilateral, bilateral, throbbing, or steady. The pain is typically moderate in intensity but may be more severe and typically will respond well, although temporarily, to nonsteroidal inflammatory agents. Temporal arteritis is a systemic disease and patients may show malaise, fever, weight loss, cardiac hepatic, or renal signs. Polymyalgia rheumatica may occur in up to 50% of patients. The diagnosis is made with a high sedimentation rate (Westergren), which is above 80 mms per hour in a majority of cases but may be only between 30 and 80 in a minority. The treatment is with steroids started as soon as possible in doses of 60-80 mgs per day with a temporal artery biopsy obtained within 48 hours. The course may be from 4 months to several years. As long as the sed rate is elevated and the patient has headaches when steroids are tapered, the process of temporal arteritis is probably still active and requires treatment.
Finally, sinus headache is a very common lay diagnosis. Patients who have headache with pain in the central facial region and who do not have purulent or sanguinopurulent discharge from the nose, often will have migraine as opposed to sinus headache. Likewise, if the headache is not associated with exposure to allergens or occurring only at certain times of the year when particular allergens are in season, there is good likelihood the headache is more likely to be migraine than sinus.
Medical Therapies
Medical therapies for migraine can be divided into symptomatic and prophylactic, or preventive therapies. Symptomatic therapy can be further subdivided into nonspecific therapies and specific abortive therapy. An algorithm for migraine therapy is presented in Figure 2.
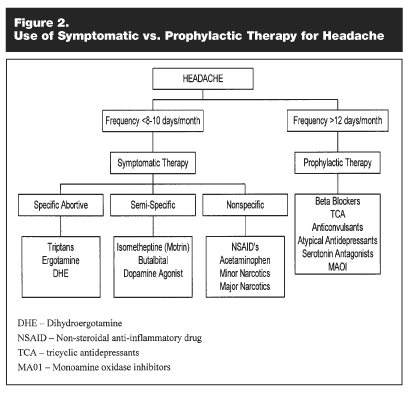 |
Symptomatic therapies for migraine are oriented primarily toward relief of pain. Pain is the symptom that brings the majority of patients to seek medical help. Nausea and vomiting are the next most common symptoms that lead patients to seek medical help, and antinauseants may often be part of a successful migraine treatment regimen.
It is of note that successful treatment of the pain and nausea of migraine usually produces remission of the entire migraine syndrome. Typically, the various symptoms of the migraine syndrome tend to occur together. In some cases, migrainous neurologic or gastrointestinal (GI) symptoms may occur in the absence of pain, a syndrome known as migraine-sans-migraine. There are, however, occasional examples of prolonged migrainous aura that do not respond to antimigrainous therapy.
Nonspecific Symptomatic Therapy
Analgesics
The simplest treatment for migraine are nonsteroidal anti-inflammatory drugs (NSAIDs) such as aspirin, ibuprofen, or naproxen, all of which are now available in over-the-counter preparations and may be effective for a large number of patients—many of whom are never seen by physicians. Any NSAID that relieves pain may be used. At times, larger dosages of NSAIDs, such as 800 mg of ibuprofen or 500 mg of naproxen, may be effective in relieving migraine. Addition of an antinauseant, such as promethazine or hydroxyzine (25-50 mg), may be helpful in relieving the GI symptoms of migraine as well as extending the effect of the analgesic medication.
Acetaminophen is an analgesic but has no anti-inflammatory action. Some patients find 500-1000 mg of acetaminophen an effective treatment for migraine.
Narcotics
As these are potentially habituating drugs, these should not be used until NSAIDs, isometheptene compounds, and triptans (see below) have been tried.
Minor narcotics. Minor narcotics such as codeine (30-60 mg), hydrocodone (5-7.5 mg), oxycodone (5 mg), or propoxyphene (65 mg) to relieve pain. As with the NSAIDs, use of 25 mg of promethazine or hydroxyzine with the minor narcotic extends the effect of the narcotic and helps relieve the GI symptoms of migraine.
Narcotic agonist/antagonist. A narcotic agonist/antagonist medication such as butorphanol (Stadol) at 2-4 mg IM or nalbuphine (Nubain) at 10 mg IM is the next step in nonspecific pain relief. These narcotic agonist/antagonist medications stimulate opiate receptors at low dosages but become narcotic antagonists and can elicit withdrawal syndromes at higher dosages.
Major narcotics. If these medications are ineffective, use of a stronger narcotic, such as meperidine (25-100 mg) or morphine (5-15 mg), may be indicated. These agents are usually given intramuscularly but can be given intravenously at lower dosages. Use of an antinauseant often extends the effect of the narcotic and allows it to be effective at a lower dose. Promethazine or hydroxyzine at 25-75 mg usually are quite effective as adjuvant agents when given with a narcotic.
The use of narcotics should be limited to patients who have only occasional severe headaches (< 1/wk) that are refractory to other nonspecific analgesic approaches or to the specific abortive therapies discussed below. The use of narcotics, minor or major at frequencies of 1/wk or greater is a major signal of actual or impending overuse. If narcotics are used ³ 15 days/month, the likelihood of habituation and development of a rebound-withdrawal headache is high.
Dopamine Antagonists
Occasionally, an antinauseant such as metoclopramide (10 mg), prochlorperazine (10 mg), or droperidol (1-2 mg) given intravenously is very helpful by itself. This approach should be considered before using narcotics.
Specific Symptomatic (Abortive) Therapies
The specific abortive therapies include triptans, dihydroergotamine (DHE), and ergotamine. These are not analgesics or narcotics—that is, they do not stimulate the opiate receptors and are not reversible by naloxone. These medications appear to provide specific antimigraine effects but have no effect on other types of pain. This action cannot be used as a diagnostic tool for migraine, however, since triptans, DHE, and ergotamine may produce temporary relief in patients with headaches of inflammatory (or vascular-inflammatory) origin related to subarachnoid hemorrhage or meningitis. Current theory suggests that abortive medications work by stimulation of the serotonin 1-D and 1B (5HT-1-B, 5HT-1-D) receptors. These are presynaptic receptors on blood vessels (1-B) or central neurons (1-D). Stimulation of presynaptic receptors depolarizes the synapse and reduces transmitter release. Thus, stimulation of presynaptic 5HT-1-B receptors on trigeminal nerve endings decreases release of substance P, calcitonin gene-related peptide, and neuropeptide Y on cranial vessels and, in turn decreases neurovascular inflammation. Similar presynaptic effect at serotonin 1-D central receptors may alter pain transmission in the trigeminocaudal nucleus or other pain transmission or modulating sites and alter pain transmission and perception.
Triptans
Background and Pharmacology
The triptans are a new class of medications, which developed from research on serotonin. Recent investigations into serotonin have identified 4 classes of receptors. The 5HT-1 receptors are presynaptic receptors. The 5HT-2 are postsynaptic receptors. The 5HT-3 receptors are related to the g-protein system, and the 5HT-4 receptors are related to transporter function. The triptans are very potent 5HT-1-B, 1-D receptor agonists and are highly effective in the symptomatic relief of migraine. They can abort the migraine attack producing significant relief in 60-70% of patients and complete relief in 25-40% of patients.
The triptans, through the 5HT-1-B receptor, have a very strong effect on constriction of the intracranial arteries. The arterial activity is highly cerebroselective but there is also a minimal coronary vasoconstrictive effect.
Whether the major effect of the triptans in stopping migraine is peripheral through 5HT-1-B receptors on trigeminovascular nerve endings or central through the 5HT-1-D endings on CNS neurons is unclear. Perhaps the antimigraine effect may require both actions.
In the clinical trials of triptans, the patients were asked to rate their headaches in terms of pain intensity as none, mild, moderate, or severe and then wait until the pain was at least moderate before taking the medication. Pain level was then reported by the patient on the same scale at 30, 60, 90, and 120 minutes after taking the medication with response at 2 hours as the primary end point (see Figure 3). Response at 4 and 24 hours is often reported; however, rescue medication is usually permitted after 2 hours so the value of these measurements is diminished. The accepted measure of success in studies of triptans is achieving mild or no headache at 2 hours while achieving pain-free is a more severe criterion.
 |
Recurrence of headache is a major issue defined as having re-occurrence of severe or moderate headache following being in response with mild or no headache. This definition created some confusion in that a patient had to be in response in order to have recurrence. The recurrence rate on the placebo was often relatively low but then the placebo response was likewise relatively low. Recurrence rates typically are between 25% and 40%. Recurrence, however, is often mild and can be treated easily with a second dose of the triptan.
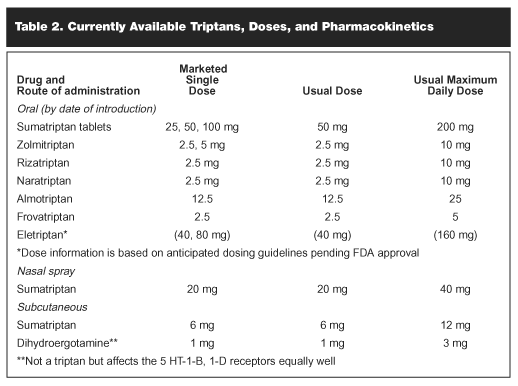
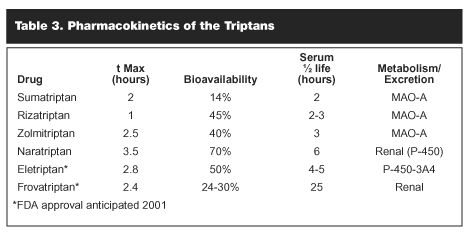
Table 2 lists the medications, which are currently available as well as doses. Table 3 provides information on pharmacokinetics of triptans. Table 4 summarizes the data for the 7 triptan medications showing the percent that achieved response and the percent that achieved pain free. In general, the triptans produced response (mild or no headache) in 60-70% of patients when given as an oral tablet and pain-free status was achieved by 27-41% of patients, depending on the medication. To date, head-to-head studies have been carried out with zolmitriptan and sumatriptan, and rizatriptan and sumatriptan. There have been small differences in the overall response, which have not been statistically significant.
 |
 |
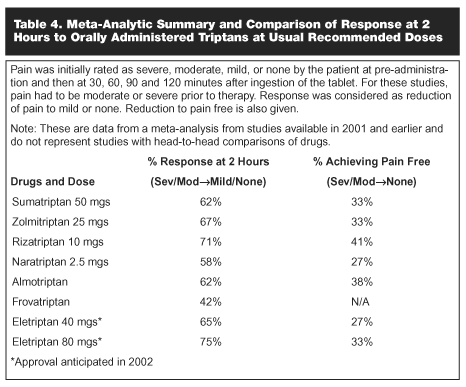 |
The meta-analysis of the triptans in acute migraine therapy by Ferrari et al demonstrated some differences in the responses to triptans at 2 hours. The differences in general were small and the important conclusions were: 1) all triptans worked; and 2) as a group, the triptans were a major step forward in migraine therapy.
From a clinical standpoint, it appears there is significant idiosyncrasy in the response of individuals to triptans. In the clinic it is more important that individual patients may respond well to one triptan and less well to another. The reasons for the idiosyncratic differences are still unclear, nevertheless, failure of one triptan does not necessarily mean failure of all other triptans. If a patient has an inadequate response to a triptan, it is always worthwhile to try the remaining representatives of this group of medications.
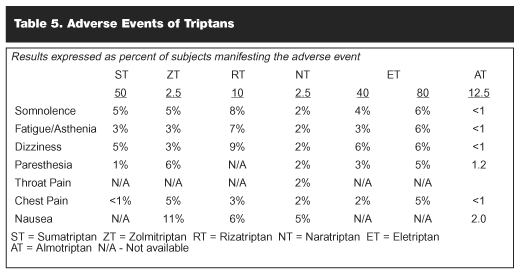
Adverse effects of the triptans are summarized in Table 5. This represents a compilation of a significant number of studies. In general, the central nervous system symptoms of somnolence, fatigue, asthenia, and dizziness are the most common and the most troublesome. Chest pain occurs in a significant number of patients. It is thought to be related to stimulation of esophageal receptors, which causes esophageal spasm, but cardiac origin must be ruled out.
 |
The major adverse event for the triptans relates to the cardiac system. There are rare 5HT-1-B receptors on coronary arteries. It has been shown that triptans can cause approximately 20% constriction of coronary arteries. If the patient has an underlying coronary atherosclerotic lesion, this 20% constriction may be enough to produce occlusion of the vessel. There have been myocardial infarctions reported with the triptans and also with ergotamine and dihydroergotamine (DHE). Patients who are potential recipients of triptans, ergotamines, or DHE should be screened for cardiac disease. If there is any doubt, the patient should have a more extensive cardiac evaluation. (Patients with cardiac disease should not receive triptans or DHE or ergotamine).
Other adverse events like the therapeutic effect are relatively idiosyncratic. If one (triptan) causes significant side effects, caution is needed if an alternative triptan is used.
Finally, it should be pointed out that overuse of triptans can produce rebound withdrawal headaches. Triptan use should be limited to no more than 3 days per week and in general no more than 2-3 doses of a triptan per day. This limitation applies to combined use of all triptans in a given patient.
Recommended Reading
1. Ziegler DK, et al. Characteristics of life headache histories in a non-clinic population. Neurology. 1977;27:265-269.
2. Burstein R, et al. An association between migraine and cutaneous allodynia. Ann Neurol. 2000;47:614-624.
3. Lipton RB, et al. Migraine diagnosis and treatment: Results from the American Migraine Study II. Headache. 2001;41:638-645.
4. Ferrari MD, et al. Oral triptans (serotonin 5-HT1B/1D agonists) in acute migraine treatment: A meta-analysis of 53 trials. Lancet. 2001;358(9293):1668-1675.
5. Cady RK, et al. Treatment of mild headache in disabled migraine sufferers: Results of the Spectrum Study. Headache. 2000;40:792-797.
6. Callahan M, Raskin N. A controlled study of dihydroergotamine in the treatment of acute migraine headache. Headache. 1986;26:168-171.
7. Couch J. Medical management of recurrent tension-type headache. In: Tollison CD, Kunkel RS, eds. Headache Diagnosis and Treatment. Baltimore, Md: Williams & Wilkins; 1993:151-162.
8. Couch J. Complexities of presentation and pathogenesis of migraine headache. In: Cady RK, Fox AW, eds. Treating the Headache Patient. New York, NY: Marcel Dekker; 1995:15-40.
9. Couch J, Hassanein RS. Amitriptyline in migraine prophylaxis. Arch Neurol. 1979;36:695-699.
10. Edmeads J, Johnson FN. The adverse event and tolerability profile of zolmitriptan. Reviews in Contemporary Pharmacotherapy. 2000;11:119-132.
11. Ferrari MD, Saxena PR. Clinical and experimental effects of sumatriptan in humans. Trends Pharmacol Sci. 1993;14:129-133.
12. Ferrari MD, et al. Oral triptans (serotonin 5-HT1B/1D agonists) in acute migraine treatment: A meta-analysis of 53 trials. Lancet. 2001;358:1668-1675.
13. Goadsby PJ, Lipton RB. Newer triptans: Emphasis on rizatriptan. Neurology. 2000;55(suppl 2):S8-S14.
14. Goadsby PJ, Peatfield R. Zolmitriptan in the acute treatment of migraine: An overview. Reviews in Contemporary Pharmacotherapy. 2000;11:91-97.
15. Goadsby PJ. Serotonin receptor agonists in migraine. CNS Drugs. 1998;10:271-286.
16. Hargreaves RJ, Shepheard SL. Pathophysiology of migraine—New insights. Can J Neurol Sci. 1999;26(suppl 3):S12-S19.
17. Hoffert MJ, et al. Transnasal butorphanol in the treatment of acute migraine. Headache. 1994;35:65-69.
18. Humphrey PPA, Feniuk W. Mode of action of the anti-migraine-drug sumatriptan. Trends Pharmacol Sci. 1991;12:444-445.
19. Schwartz BS, et al. Epidemiology of tension-type headache. JAMA. 1998;279:381-383.
20. Lipton RB, et al. Stratified care vs step care: Strategies for migraine. JAMA. 2000;284:2599-2065.
21. Lipton RB, et al. Sumatriptan for the range of headaches in migraine sufferers: Results of the Spectrum. Headache. 2000;40:783-791.
22. Mathew NI, et al. Migraine prophylaxis with divalproex. Arch Neurol. 1995;52:281-286.
23. Moskowitz MA. Neurogenic versus vascular mechanisms of sumatriptan and ergot alkaloids in migraine. Trends Pharmacol Sci. 1992;13:307-311.
24. Nappi G, Johnson FN. The clinical efficacy of zolmitriptan. Reviews in Contemporary Pharmacotherapy. 2000;11:99-118.
25. Silberstein SD, Young WB. Safety and efficacy of ergotamine tartrate and dihydroergotamine in the treatment of migraine and status migrainous. Neurology. 1995;45:577-584.
26. Silberstein SD. The pharmacology of ergotamine and dihydroergotamine. Headache. 1997;37(suppl 1):S15-S25.
27. Silberstein SD. Practice parameter: Evidence-based guidelines for migraine headache (An evidence-based review). Neurology. 2000;55:754-762.
28. Storer RJ, Goadsby PG. Microiontophoretic application of serotonin agonists inhibits trigeminal cell firing in the cat. Brain. 1997;120 (pt 12):2171-2177.
29. The subcutaneous sumatriptan international study group. Treatment of migraine Attacks with sumatriptan. N Engl J Med. 1991;325:316-321.
30. Tfelt-Hansen P, Johnson ES. Nonsteroidal anti-inflammatory drugs in the treatment of the acute migraine Attack. In: Olesen J, Tfelt-Hansen P, Welch KMA, eds. The Headaches. New York, NY: Raven Press;1993:305-311.
31. Tfelt-Hansen P, et al. Oral rizatriptan versus oral sumatriptan: A direct comparative study in the acute treatment of migraine. Headache. 1998;38:748-755.
32. Weiller C, et al. Brain stem activation in spontaneous human migraine attacks. Nature Med. 1995;1:658-660.
33. Williamson DJ, et al. Intravital microscope studies on the effects of neurokinin agonists and calcitonin gene-related peptide on dural vessel diameter in the anesthetized rat. Cephalalgia. 1997;17:518-524.
34. Young WB, et al. Cardiac risk factors and the use of triptans. A survey study. Headache. 2000;40:587-591.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
