Evaluating and Treating Sexual Assault in the Emergency Department
Part I: Initial ED Care, Physical Exam, and Evidence Collection
Author: Ralph J. Riviello, MD, FACEP, Assistant Professor and Clinical Research Director, Department of Emergency Medicine, Jefferson Medical College, Philadelphia, PA; Medical Director, Sexual Assault Treatment Center, Thomas Jefferson University Hospital, Philadelphia, PA.
Peer Reviewers: Allison Harvey, MD, FACEP, FAAEM, Clinical Faculty, Palmetto Richland Memorial Hospital Residency Program, SAME Medical Director Palmetto Health, Columbia, SC.; Mita Carroll, MD, FAAP, FACEP, Pediatric Emergency Physician Northwest Acute Care Specialists, Portland, OR, and Vancouver, WA.
This issue covers Part I of a two-part series on evaluation and management of sexual assault in the emergency department (ED). Part I of the series discusses initial ED care, physical exam, and evidence collection. Part II will cover laboratory analysis, pharmacotherapy, disposition, follow-up, documentation, and court testimony. —The Editor
Introduction
Sexual Assault is a violent crime that can affect anyone. The National Violence Against Women Survey (NVAWS) estimated that 302,091 women and 92,748 men were raped in the 12 months prior to the survey.1 Victims often experience more than one rape. In the study, women experienced 2.9 rapes and men experienced 1.9 rapes, on average.1 According to the NVAWS, 1 in 6 women and 1 in 33 men in the United States has experienced an attempted or completed rape in their life. In 8 out of 10 rape cases, the victim knew the perpetrator.1 The FBI Uniform Crime Report (UCR) is a nationwide effort of 17,000 law enforcement agencies that report crimes to the FBI. In 2003 there were 93,433 rapes reported to the UCR.2 (The UCR defines rape as carnal knowledge of a female forcibly and against her will. Statutory rape without force and other sexual offenses are excluded.) The National College Women Sexual Victimization Study estimated that between 1 in 4 and 1 in 5 college women experienced completed or attempted rape during their college years.3
The Youth Risk Behavior Surveillance System (YRBSS), a national survey of high school students, found approximately 9% of students reported having been forced to have sexual intercourse against their will in their lifetime. Female students (11.9%) were more likely than male students (6.1%) to report having been sexually assaulted. Overall, 12.3% of Black students, 10.4% of Hispanic students, and 7.3% of White students reported forced sexual intercourse.4
Of all crimes, rape is one of the most underreported, making it difficult to count. The National Women’s Study found that 84% of women did not report their rapes to police.5 A study in 2000 confirmed that less than one-half of victims report the crime to the police or seek medical care.6 Bureau of Justice Statistics reports that between 1992 and 2000, only 31% of sexual assaults were reported to the police.7 When reported, there is a 50.8% probability an arrest will be made, with a 16.3% probability the rapist will be sent to prison.8 The average sentence is 128 days.8
There are several well documented physical and psychological consequences to rape. Between 4 and 30% of rape victims contract sexually transmitted diseases, including HIV.9,10 A study by Holmes estimated that more than 32,000 pregnancies result each year from rape in victims ages 12 to 45 years.11 Many long-lasting physical symptoms and illnesses have been associated with sexual victimization, including chronic pelvic pain, premenstrual syndrome, gastrointestinal disorders, and other chronic pain disorders (i.e., headache, back pain, and facial pain).9
The psychological consequences have both immediate and long-term impacts. Sexual violence victims exhibit a variety of psychological symptoms similar to those of victims of other types of trauma. Immediate reactions to rape include shock, disbelief, denial, fear, confusion, anxiety, and withdrawal.12 Symptoms of post-traumatic stress disorder (PTSD) usually are present immediately after a rape and approximately one-third of victims will have symptoms that continue for three months or become chronic.13 Long-term effects include anxiety, substance abuse, sleep disturbances, depression, alienation, and sexual dysfunction. Rape survivors often distrust others and replay the assault in their minds, and are at increased risk of revictimization.14 Women with a history of sexual assault are more likely to attempt or commit suicide than other women. Rape can strain relationships because of negative effects on the victim’s family, friends, and intimate partners. Victims of sexual violence are more likely than non-victims to engage in risky sexual behavior, including unprotected sex, having sex at an early age, multiple sexual partners, teen pregnancy, and trading sex for food, money, or other items.15,16 Rape victims are more likely than non-victims to smoke cigarettes, overeat, drink alcohol, and are not likely to use seat belts.17
Anyone can be a victim of rape. Women are clearly more likely to be victims than men. In the National Crime Victimization Survey, 87% of victims were women.18 Among women, the NVAWS found that American Indian and Alaskan Native women were more likely (34%) to report they were raped than African American women (19%) or White women (18%).1 In 2002, Krug et al, described vulnerability factors for victimization.19 These include: young age, drug or alcohol use, prior history of sexual violence, multiple sexual partners, and poverty.
The majority of the time, the perpetrator of the rape is known to the victim. The National Women’s Study found that 19% of perpetrators were intimate partners, 27% were family members, and 29% were relatives, friends, or acquaintances. Only 22% of perpetrators were strangers.5 Krug also has identified factors that increase the risk a man will commit rape.19 These factors relate to individual attitudes and beliefs as well as social concerns. (See summary in Table 1.)

Emergency physicians are most frequently the first medical contact for victims of sexual assault. Victims can present to the ED at any time following the assault. In addition, patients experiencing any of the long-term consequences of rape may seek care in the ED repeatedly for alternate complaints, without the true cause of their problem identified. This paper will focus on the emergent care of the adult/adolescent sexual assault victim.
Definitions
Rape is a legal term first defined in 1756 as carnal knowledge of a woman not one’s wife by force or against her will. Although state laws vary, most broadly define rape using gender-neutral language. Most states use three criteria: 1) any vaginal, anal, or oral penetration by a penis, object, or other body part; 2) lack of consent, communicated with verbal or physical signs of resistance, or if the victim is unable to consent by means of incapacitation because of age, disability, or drug or alcohol intoxication; and 3) threat of or actual use of force. Incapacitation also includes provisions for children, the disabled, and the elderly.20
Sexual assault is a broader term characterized as any unwanted sexual contact, thus encompassing a range of behaviors including rape, incest, fondling, molestation, or grabbing. In general, statutory rape occurs when a person of the age of consent has sex with someone below the age of consent. The age of consent differs from state to state. Sodomy is the term used to describe anal penetration and in many states carries additional penalties.
Sexual Assault Response Team
It is not the responsibility of healthcare workers to understand the specific legal definitions of sexual assault but to have an organized approach to the care of sexual assault survivors. ED care of the sexual assault victim focuses on three areas: 1) providing medical care and evaluation for injury; 2) forensic evaluation and evidence collection; and 3) disease and pregnancy prophylaxis. It is not the job of the examining physician or nurse to determine if a rape or sexual assault occurred. Rather, the clinician’s role is to document the events and circumstances as reported by the victim, identify and document physical injury and forensic exam findings, collect forensic evidence, provide treatment, and arrange follow-up care.
Care of the sexual assault survivor begins well before the patient arrives in the ED. There needs to be a community-wide plan of care for victims that encompasses all aspects of services, including medical, law enforcement, rape crisis centers, and the courts. This often is referred to as the Sexual Assault Response Team (SART). Healthcare providers should be aware of the protocols in place in the areas where they practice and follow established guidelines. Often protocols designate hospitals or centers for forensic evaluation, define police jurisdictions, and support the rape crisis center. In general, care of the sexual assault victim is a coordinated, compassionate team response including all the components described above.
Rape crisis centers first were developed in the 1970s in Philadelphia, San Francisco, and Washington, DC.20 These centers usually are staffed by lay people, often sexual assault survivors themselves, and serve a vital function in the prevention, acute treatment, and follow-up of rape survivors. Some of their functions include public education, staffing hotlines, hospital escort, advocacy and support in court, and short-term counseling services.
Traditionally, sexual assault exams have been performed by physicians. This often resulted in a hurried exam by a busy physician whose focus was complying with protocols of evidence collection, not care of the victim. Also, victims have had to endure long waiting times in a public area; have not been allowed to eat, drink, or urinate while they waited (for fear of destroying evidence); have had their injuries taken less seriously than other trauma victims; and have had their psychological needs overlooked. The physicians and nurses had little or no training in the management of these patients or in principles of evidence collection.21 As research became available, it was clear a better system was needed to care for rape survivors in the ED. Often ED nurses performed most of the exam and evidence collection, a fact that spurred the development of the Sexual Assault Nurse Examiner (SANE) program. In 1976, the first SANE program was created in Memphis, TN.22 Shortly thereafter, other cities followed and in 1992, the first meeting of SANE from the United States and Canada occurred. This meeting lead to the development of the International Association of Forensic Nurses (IAFN).
The growth of SANE programs in the United States has been widespread and rapid. Nurses in training undergo 40 hours of classroom work that includes forensic history taking, forensic evidence collection, pelvic examination and colposcopy, photography, medical treatment and care, and training on testifying in court. In addition, the nurses are required to complete a clinical preceptorship.21,23 The guidelines for training are outlined by the IAFN and certification training is available following the completion of a minimum number of exams.24
Sexual assault nurse examiners have proved to be invaluable to EDs and rape centers, as well as to the victims they serve. The SANE is able to dedicate his/her time to the victim, allowing the victim-centered examination process to proceed in a timely, organized, and unhurried fashion. Studies have found that SANE provide more accurate evidence collection and near perfect documentation, are credible witnesses, and in most instances can testify as expert witnesses.23,25,26 There are several resources available to assist in developing a SANE program in the ED.21,23
Initial ED Care
Rape survivors should be given top priority when they arrive in the ED. They should be triaged immediately and placed in a safe, non-threatening environment. Before the forensic evaluation begins, the patient should be screened for serious and/or life-threatening injuries. As with all ED patients, the ABCs (airway, breathing, and circulation) should be evaluated and stabilized before proceeding. In seriously injured patients, forensic examination should be performed after stabilization, or in the operating room following operative procedures. Other patients should be advised not to eat, drink, or urinate until they are evaluated by the examiner.
The rape crisis center should be contacted so that an advocate can come to the ED to be with the victim. In addition, the police should be notified. Rape/sexual assault statutes in most states stipulate mandatory reporting by medical personnel. Victims have the right to refuse to talk to the police or participate in the investigation and prosecution of the perpetrator. Nonetheless, the police should be contacted by ED personnel in all cases. Victims should be made aware of reporting requirements and should be encouraged to report the assault to the police. This is important because of the time sensitive nature of evidence collection. Victims can consent to evidence collection then later decline to participate in formal legal action. Many states have crime victim compensation programs that pay for medical examination and care. Many of these programs generally require police reporting.
It is widely accepted that the appropriate time for evidence collection is within 72 hours of the assault. As expected, the closer to the time of the assault, the greater the chance of evidence recovery. Most programs will not collect evidence more than 72 hours after an assault unless the victim has not showered or changed clothes or has complaints of pain or injury. Evidence collection after 72 hours often is decided on a case-by-case basis and is a practice of increasing frequency with the technologic advancements of forensic science.
The victim should be allowed to have a rape crisis counselor/victim advocate, friend, and/or family member with him/her in the exam room. Police presence during the history taking and physical exam varies among jurisdictions. Some feel that the victim may be intimidated, while others support the practice of police presence to limit repetitive history-taking and minimize discrepancies in reported details.
Patient demographic information should be collected, including the date and time of arrival to the ED, date/time of examination, and date/time of discharge. Information regarding law enforcement response also should be documented, including the name of the officer taking the report, agency or district, ID or badge number, and phone number. Prior to evidence collection, patient consent should be obtained for forensic evidence collection and physical examination, photographs of findings, release of information and evidence to health authorities and law enforcement, presence of a patient advocate, and any other consent issues as dictated by local protocol.
When obtaining forensic evidence, some general tips include the following:
- Use only paper to package evidence;
- Wipe wet stains with a dry swab;
- Wipe dried stains with a wet swab;
- Air dry all evidence;
- Wear exam gloves and change them frequently to prevent cross contamination; and
- Use a wet gauze to moisten sticky seals (do not lick them).
History
As with any medical encounter, the evaluation begins with taking the history. History taking of victims is divided into two parts—the medical history and the forensic history. The medical history includes past medical and surgical history, medications, allergies, family and social history, tetanus status, and contraception use. Other information elicited can include obstetric history; last menstrual period; drug or alcohol ingestion; last consensual sexual experience, tampon use, or douching; and history of sexually transmitted diseases. (See Table 2.)

The forensic history is a history of the assault and can be used to guide evidence collection. Depending on protocols in the jurisdiction, this can be a very detailed history or can be brief and focused, with the detailed questioning of assault events reserved for the police investigator. The forensic history includes a description of the incident; number and identity of assailants (if known); time and location of attack; specifics of sexual contact (including oral, anal, and/or vaginal contact, and fondling); contact with ejaculate, urine, or vaginal secretions; use of weapons, restraints, contraceptives, condoms, or force by perpetrator; and the use of objects to penetrate or coerce the victim. In addition, post-assault activities are important to document. These include changing clothes, bathing, urinating, defecating, and douching. If the oral cavity was involved, the victim should be asked if he or she has eaten, drunk, smoked, brushed his/her teeth, or gargled since the attack. (See Table 3.)

All information taken in the history should be recorded accurately using the victim’s words. All direct quotes made by the victim should be denoted with quotation marks. Strongly consider including the clinician’s questions in the documentation, also in quotes. Information can be documented in the usual ED medical record or in a specific chart designed for use in an individual state, county, or hospital.
Physical Exam and Forensic Evidence Collection
The physical exam is a head-to-toe assessment looking for physical injuries and visible evidence. Before starting, the victim should be provided information concerning the physical exam, forensic evidence collection process, diagnostic testing for sexually transmitted infections, and any other necessary procedures. In addition, the patient should be should be informed that he/she is in charge of the exam and can ask for the exam to stop at any time or can refuse any part of the exam. The survivor should be made to feel that he/she is in control of the medical evaluation.
The rape kit then is collected. The rape kit contains all the equipment needed to collect and properly store forensic evidence and allows for an organized approach to evidence collection. The specific components of the rape kit vary from jurisdiction to jurisdiction. The following description of evidence collection includes many techniques, some of which may not apply to some jurisdictions. In addition, some jurisdictions prefer air-dried swabs, microscope slides, or both. The procedures primarily are adapted from the American College of Emergency Physicians’ Evaluation and Management of the Sexually Assaulted or Sexually Abused Patient and the Department of Justice’s National Protocol for Sexual Assault Medical Forensic Examinations.27,28
Clothing. First, the victim is asked to disrobe. If the victim is wearing the same clothing worn during the assault, it needs to be collected as evidence. The patient is asked to disrobe while standing over a paper sheet. The clothing is left on the sheet and then the examiner folds the clothes and places each article of clothing in an individual paper bag that then is sealed and labeled. Underwear is of particular importance and should be collected in all cases of actual or attempted vaginal or anal penetration. Underwear is placed in a separate small bag that is sealed and labeled. Semen and other body fluids can be transferred from the perpetrator or the victim to the victim’s underwear. Thus, collection of clothing is not confined to those items worn during the attack, but includes the clothing put on immediately after the assault. If the victim has changed clothes, the police often will go to the victim’s house or crime scene to retrieve them for crime lab forensic analysis.
Debris. Any obvious debris found on the patient’s body should be collected on a sheet of paper. This can include plant material, soil, grass, fibers, hair, etc. It should be labeled and sealed after it has been secured in a paper bindle. A bindle is made by collecting the evidence material on a piece of clean paper, then folding the paper in half. The half-sized paper is the folded into thirds by folding the right flap, then the left. The paper then is folded in half again, and the open end is sealed with a piece of tape and initialed. Often, this paper is included in the forensic evidence collection kit.
Dried Secretions. The body should be inspected for dried secretions, bite marks, bruises, and burns. These areas should be described thoroughly and their locations documented on a body map. Photo documentation of these injuries is encouraged. A Wood’s lamp or alternative light source (ALS) (i.e., BlueMaxx, Crimescope, and others) is used to aid in identification of areas of dried secretions (specifically, sputum and semen). The dried secretions are potentially DNA-rich areas. Areas of particular attention are the breasts, abdomen, upper thighs, and vulva. Perpetrators may make oral contact (i.e., lick, suck, kiss) with the breasts and/or areola. Victims often may forget this act when recounting the attack. The secretions can be collected by two methods. They can be flaked off the skin and bindled. Alternatively, the double-swab technique can be used.29 A swab moistened with sterile or distilled water is rubbed all over the area. A second dry swab then is rubbed over the same area. Both then are allowed to air dry. In either method, the evidence is labeled and sealed.
The Wood’s Lamp or ALS is a source of UV radiation that emits wavelength of approximately 320-400 nm. Semen fluoresces at approximately 360 nm.23,30 The Wood’s lamp or ALS causes semen, urine, and other oily substances to fluoresce a blue-green to orange color. There is controversy surrounding the Wood’s lamp’s ability to fluoresce semen. The Wood’s lamp is felt to be sub-optimal for detecting semen because the light emitted is at the wrong wavelength.31 Nelson and Santucci found that all emergency physicians studied were able to identify the semen as fluorescing. They found that the ALS was 100% sensitive for identifying semen, but not specific.30 Certain lotions and detergents can cause false positive results. The victim’s body should be completely examined with either light and any areas of fluorescence swabbed and packaged in the rape kit.
Fingernail Scrapings. The fingernails should be inspected for debris and dirt. They should be gently scraped using the stick provided in the rape kit. The debris should be collected into a bindle, sealed, and labeled. If the nail is broken, it should be gently cut and placed in the bindle as well.
Oral Sample. The oral cavity first is inspected for injuries. Forceful oral intercourse can result in submucosal hemorrhages at the junction of the hard and soft palate, termed “fellatio syndrome.”32 Other injuries can include petecchiae, hemorrhages, and abrasions on the uvula and soft palate. Two swabs are placed in the oral cavity between the gums and cheek and under the tongue. If the victim has dentures, they should be removed and swabbed with the same or additional swabs. If microscope slides are provided in the rape kit, smear swabs on microscope slides, air dry swabs and slides, place slides in the holder provided and the swabs in the carton. All evidence should be labeled, sealed, and initialed.
Head Hair Combing. Remove the paper and comb from the kit. The patient can be allowed to do the combing. Place the paper under the patient’s head and comb the hair toward the paper. If there is any matted hair, it should be cut and placed on the collection paper. When completed, place the comb in the center of the paper and fold it into bindle. The bindle is labeled, placed in an envelope, sealed, and initialed.
Pulled Head Hair. Pulled hairs is a practice used to establish a victim’s hair standard. This is a painful process, requiring 25-100 hairs to be plucked, and often is unnecessary because of advanced DNA technologies. Medical centers often defer this step to crime lab personnel only if determined necessary in the course of the investigation. If performed in the ED according to local protocol, the examiner uses his/her gloved hand to pull a minimum of eight full-length head hairs from each of the following areas—top, front, back, left side, and right side. Any unusually colored hairs and hairs from wigs and hairpieces are collected and labeled separately. All hair specimens should be placed in a bindle and folded and labeled. The bindle is placed in an envelope, labeled, sealed, and initialed.
Pubic Hair Combing. The same technique is used as in the head hair combing. The collection paper is placed under the patient’s buttocks and the hair is combed toward the paper. Any dried, matted hairs should be cut and placed on the collection paper. The comb is placed in the bindle and labeled. The bindle is placed in an envelope, labeled, sealed, and initialed.
Pulled Pubic Hair. This is another procedure that may be deferred or unnecessary in some jurisdictions. A similar technique is used as in the pulled head hair collection. A minimum of 25 hairs should be collected.
Genital Exam
After a head-to-toe examination of the patient, proceed with the genital exam. The genital exam serves two purposes: 1) to document injuries and 2) to recover semen (i.e., DNA evidence). The genital exam should be performed whether or not the victim complains of pelvic trauma or discomfort. A study by Rambow, et al,33 found that up to one-third of victims have evidence of genital injuries after a sexual assault in the absence of symptoms. Studies report the presence of traumatic anogenital injuries following sexual assault range from 6 to 87%.34-36 Genital trauma is more likely to occur in postmenopausal females and may require surgical intervention.37 Factors that contribute to the increased presence of injuries include: victim’s age (younger than 20 and older than 49); force used to commit the assault; relationship with perpetrator; use of lubricants; victim position during assault; virginal status of victim; those examined within 24 hours; physical/verbal resistance; greater than high school education; and history of anal assault.35,36,38,39 Another series found that 81% of patients who reported digital-vaginal penetration only had evidence of genital injury.40 Most genital injuries are minor and heal without specific treatment or intervention. Table 4 lists factors that affect the presence of genital injury.35,36,38,39

Physical and genital injury is not an inevitable consequence of rape and the absence of genital injury does not provide proof of consent. Therefore, the lack of injury or presence of minimal genital trauma does not rule out of sexual assault.
Genital examination begins with inspection of the external genitalia and proceeds to speculum examination. It is important to review pertinent genital anatomy before proceeding. (See Figure 1.) The posterior fourchette is a tense band or fold of mucous membrane at the posterior commissure of the vagina connecting the posterior folds of the labia minora. The fossa navicularis is the concavity anterior to the posterior fourchette and posterior to the hymen. The hymen is a membranous collar or semicollar that surrounds the vaginal opening and separates the external genitalia from the vagina. All women have a hymen and its appearance should not be used to determine whether or not a rape occurred. The perineum lies between the posterior fourchette and anus in females and between the scrotum and anus in males.
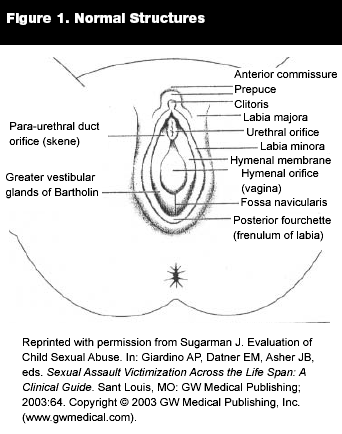
Genital injuries typically are described using the mnemonic TEARS (Tears, Ecchymosis, Abrasions, Redness, and Swelling).41 When describing the location of external genital injuries, they should be referenced as on the face of a clock. Common areas for injury include the posterior fourchette and fossa navicularis. The posterior fourchette is the first area the penis often contacts prior to penetration. Injuries in this area, located between the 5 and 7 o’clock positions, commonly are referred to as mounting injuries. Table 5 lists common sites of anogenital injuries in sexual assault.35 All injuries should be documented and described as well as photographed.

External Genitalia. Visual inspection of the external genitalia should be performed and should include the surrounding areas, especially the lower abdomen and inner thighs. This inspection can be facilitated by using a hand-held magnifying lens.42 Contusions to the inner thighs may be evident as a result of violently forcing the victim’s legs open during the attack. Fluid (i.e., blood, semen, saliva) may be present and also should be collected as previously described. A Wood’s lamp or ALS can be used to assist in the identification of fluid evidence. The labia majora and labia minora should then be gently separated to look for injuries. The external genitalia then should be swabbed using two swabs in a rolling manner. If required, they should be smeared on a slide or allowed to air dry. All envelopes and cartons should be labeled, sealed, and initialed.
Perineum. A complete and thorough evaluation of the perineum should be performed. During this assessment, the examiner is looking for injuries, debris, and fluid stains. This area should be swabbed as well, and the swabs should be preserved as evidence for the rape kit.
Vagina. Examination of the vagina begins with a thorough inspection of the vaginal opening, or introitus, noting and documenting any injuries. Inspection of the introitus is facilitated by gentle retraction and separation. The colposcope can be used to magnify the area and facilitate the detection of injury. (This will be discussed later.) Next, a speculum lubricated with warm water is inserted into the vagina. This portion of the exam is used in detection of injuries to the vagina and/or cervix. All injuries should be documented using language that is descriptive and detailed. Separate swabs of the vagina and cervix should be taken, paying particular attention to areas where fluid is pooled. These swabs are either smeared onto slides or allowed to air dry, then they are packaged, labeled, and sealed. Any foreign body (condom or tampon) in the vagina also should be collected and packaged in a plastic, wax-lined bag, and placed in the rape kit.43 Also consider the packaging and labeling of the speculum used during the exam; in cases where it is the first object placed in the vagina after the assault, important evidence may be identified on the speculum. If testing for sexually transmitted infections is a part of the ED protocol, obtain swabs for forensic analysis first, then proceed with swabs for gonorrhea, chlamydia, and other medical tests as appropriate.
A Foley catheter can be used to facilitate visualization of the floppy, redundant edges of the hymen in pubertal and post-pubertal girls.44 A study by Jones, et al found that this technique allowed the identification of hymenal abnormalities in nine additional cases (60%).45 The technique involves inserting a Foley catheter into the distal vaginal vault, inflating the balloon and gently retracting it against the hymen. The procedure is easy and often well tolerated.
Vaginal Pool Aspiration. Some jurisdictions may require this to be collected. A plastic catheter and syringe with 3 mL of sterile saline or water is used for vaginal lavage. The fluid then is aspirated and put in the tube provided in the kit. An alternative technique is to use a syringe to collect any pooled vaginal secretions. Remember to tightly seal the cap of the container in which the fluid is stored before placing it in the rape kit. Other protocols may require an alternate collection method, namely, swabbing the fluid with 2-4 dry, cotton-tipped swabs that then are air-dried, packaged, labeled, and sealed.
Anal/rectal Examination. Examination of the anus and rectum should be conducted whether or not the victim reports anal contact. Victims may be embarrassed to report the crime, or do not recall it happening. In most jurisdictions, sodomy is charged as an additional offense with a separate penalty. Any dried secretions in the anal area should be collected by flaking them off or using the double swab technique. Two swabs then are used to swab the anal cavity, taking care to avoid contact with the external skin surfaces. The anal external skin and mucosa should be inspected for injury or swelling. This evaluation can be aided by using a colposcope, clear plastic anoscope, and/or toluidine blue dye. All injuries should be documented and their location reported with respect to the numbers on a clock.
Colposcopy
A colposcope provides medium-powered binocular enlargement and can identify microlacerations not evident to the naked eye. Use of the colposcope in sexual assault examinations was first described by Texiera in 1981.46 The most cited works concerning the use of colposcopy in sexual assault examinations are two studies by Slaughter, et al.35,47 In 1992, Slaughter and Brown were the first to report the regular use of colposcopy for rape examinations. They found that 87% of victims (n = 131) had identifiable injury via colposcope.47 In that series, 11.8% more cases of sexual assault were identified using the colposcope compared to conventional examination. One study found that using a colposcope has been shown to increase the detection of genital trauma from 6% to 53%.48 In addition, the colposcope provides optimal illumination and photographic or videotape documentation of the examination and findings. Videotaping the exam with the aid of a colposcope, as well as the use of photography, can allow other consultants to review the exam and interpret findings without having to repeat it.49 If a colposcope is not available, a 35 mm camera or digital camera with a macro lens can be used to magnify the area and provide photodocumentation of injuries.
The identification of injury with the colposcope can be aided by toluidine blue dye. This is a nuclear stain that does not stain the skin surface. Rather, toluidine blue dye stains the nucleated squamous cells in the deeper layers of the epidermis exposed by laceration, however superficial. Its use was first described by Lauber and Souma, who increased injury identification by 6%.50 In another study, McCauley, et al increased visualization from 4% to 58% with its use.51 If toluidine blue is used, it should be applied before any digital or speculum examination occurs. Although DNA evidence will be preserved, care should be taken to avoid dye entering the vaginal vault. The use of dye in the vaginal area should follow anal application; this practice avoids any cross-contamination from run-off of dye. The protocol for using toluidine blue dye is as follows:
- Prior to dye application, all external genital specimens should be collected for forensic analysis then swabs collected for STD testing as appropriate.
- Prior to dye application, photodocument all injuries to the area.
- The dye is applied using a sterile cotton swab to the genital area (labia majora, labia minora, posterior fourchette, perineal body, and perianal area).
- The excess dye is gently blotted away with 1% acetic acid solution (vinegar/water) or with lubricating jelly on a cotton ball.
- The area is examined with the colposcope and photographed.27
References
1. Tjaden P, Thoennes N. Full report of the prevalence, incidence, and consequences of violence against women: Findings from the National Violence Against Women Survey. Washington (DC): National Institute of Justice; 2000. Report NCJ 18371.
2. Federal Bureau of Investigation. Crime in the United States 2003. US Department of Justice, October 2004. FBI web site www.fbi.gov/ucr/03cius.htm. Accessed April 20, 2005.
3. Fisher BS, Cullen FT, Turner MG. The sexual victimization of college women. Washington (DC): Department of Justice (US), National Institute of Justice; 2000. Publication No. NCJ 182369. Available at: www.ncjrs.org/pdffiles1/nij/182369.pdf. Accessed February 6, 2005.
4. Centers for Disease Control and Prevention. Youth Risk Behavior Surveillance—United States, 2003. MMWR 2004;53(SS-02):1-96. CDC web site www.cdc.gov/mmwr/PDF/SS/SS5302.pdf.
5. Kilpatrick DG, Edmunds CN, Seymour AK. Rape in America: A report to the nation. Arlington (VA): National Crime Victim Research and Treatment Center and Medical University of South Carolina; 1992.
6. Feldhaus KM, Houry D, Kaminsky R. Lifetime sexual assault prevalence rates and reporting practices in an emergency department population. Ann Emerg Med 2000;36:23-27.
7. Hart TC, Rennison C. Reporting crime to the police, 1992-2000. Washington, DC: Bureau of Justice Statistics, US Department of Justice, March, 2003 NCJ 195710.
8. National Center for Policy Analysis. Crime and punishment in America: 1999. NCPA Report 229, October 1999.
9. Koss MP, Heslet L. Somatic consequences of violence against women. Arch Fam Med 1992;1:53-59.
10. Murphy SM. Rape, sexually transmitted diseases, and human immunodeficiency virus infection. Int J STD AIDS 1990;1:79-82.
11. Holmes MM, Resnick HS, Kilpatrick DG, et al. Rape-related pregnancy: Estimates and descriptive characteristics from a national sample of women. Am J Ob Gyn 1995;85:330-336.
12. Herman JL. Trauma and Recovery. New York (NY): Basic Books; 1992.
13. Rothbaum PO, Foa EB, Riggs DS, et al. A prospective examination of posttraumatic stress disorder in rape victims. J Trauma Stress 1992;5:455-475.
14. DeLahunta EA, Baram DA. Sexual assault. Clin Ob Gyn 1997;40: 648-660.
15. Boyer D, Fine D. Sexual abuse as a factor in adolescent pregnancy and child maltreatment. Fam Plann Perspect 1992:24:4-11.
16. Brener CD, McMahon PM, Warren CW, et al. Forced sexual intercourse and associated health-risk behaviors among female college students in the United States. J Consult Clin Psychol 1999;67: 252-259.
17. Koss MP, Koss PG, Woodruff W. Deleterious effects of criminal victimization on women’s health and medical utilization. Arch Int Med 1991;151:342-357.
18. Department of Justice Criminal Victimization 2002. Washington (DC): US Government Printing Office; 2003. Publication No. NCJ 1994.
19. Krug EG, Dahlberg LL, Mercy JA, et al, eds. World report on violence and health [serial online.] 2002: World Health Organization. Available at www.who.int/violence_injury_prevention/violence/world_report/wrvh1/en/. Accessed March 3, 2005.
20. Linden JA, Young JS. Overview of adolescent and adult sexual assault. In: Giardino AP, Datner EM, Asher JP, eds. Sexual Assault Victimization Across the Life Span: A Clinical Guide. St. Louis: GW Medical Publishing 2003:211-221.
21. LeDray LE. Sexual assault nurse examiner (SANE) development and operation guide. Washington, DC: US Department of Justice, Office of Victims of Crime; 1999.
22. Speck PM, Aiken MM. 20 years of community nursing service: Memphis sexual assault resource center. Tennessee Nurse, April 1994.
23. Houmes BV, Fagan MM, Quintana NM. Establishing a sexual assault nurse examiner program (SANE) in the emergency department. J Emerg Med 2003;25:111-121.
24. International Association of Forensic Nurses.web site www.iafn.org. Accessed July 2005.
25. Taylor WK. Collecting evidence for sexual assault: The role of the sexual assault nurse examiner (SANE). Int J Gynaecol Obstet 2002; 78(Suppl 1):S91-S94.
26. Sievers V, Murphy S, Miller JJ. Sexual assault evidence collection more accurate when completed by sexual assault nurse examiners: Colorado’s experience. J Emerg Nurs 2003;29:511-514.
27. American College of Emergency Physicians. Evaluation and management of the sexually assaulted and abused patient. Dallas, TX: ACEP; 1999.
28. Office on Violence Against Women. A national protocol for sexual assault medical forensic examinations: Adults/adolescents. Washington, DC: US Department of Justice; 2004, NCJ 206554. www.ncjrs.org/pdffiles/ovw/206554.pdf. Accessed February 23, 2005.
29. Girardin BW, Faugrio DK, Seneski PC, et al. Care of the sexually assaulted patient. In: Color Atlas of Sexual Assault. St Louis, MO: Mosby: 1997;83-127.
30. Nelson DG, Santucci KA. An alternate light source to detect semen. Acad Emerg Med 2002;9:1045-1048.
31. Santucci KA, Nelson DG, McQuillen KK, et al. Wood’s lamp utility in the identification of semen. Pediatrics 1999;104:1342-1344.
32. Reyes I, Datner EM. The evaluation of the sexual assault victim. In: Giardino AP, Datner EM, Asher JP (eds). Sexual Assault Victimization Across the Life Span: A Clinical Guide. St. Louis: GW Medical Publishing 2003:241-250.
33. Rambow B, Adkinson C, Frost TH, et al. Female sexual assault: Medical and legal implications. Ann Emerg Med 1992;21:717-731.
34. Slaughter L, Brown CRV. Cervical findings in rape victims. Am J Ob Gyn 1991;164:528-529.
35. Slaughter L, Brown CR, Crowley S, et al. Patterns of genital injury in female sexual assault victims. Am J Obtet Gynecol 1997:176: 609-616
36. Sugar NF, Fine DN, Eckert LO. Physical injury after sexual assault: Findings of a large case series. Am J Ob Gyn 2004;190:71-76.
37. Ramin SM, Saton AJ, Stone IC, et al. Sexual assault in postmenopausal women. Obstet Gynecol 1992;80:860-864.
38. Stermac L, DuMont J, Kalemba V. Comparison of sexual assaults by strangers and known assailants in an urban population of women. CMAJ 1995;153:1089-1094.
39. Sachs CJ, Chu LD. Predictors of genitorectal injury in female victims of suspected sexual assault. Acad Emerg Med 2002;9:146-151.
40. Rossman L, Jones JS, Dunnuck C, et al. Genital trauma associated with forced digital penetration. Am J Emerg Med 2004;22:101-104.
41. Girardin BW, Faugrio DK, Seneski PC, et al. Findings in sexual assault and consensual intercourse. In: Color Atlas of Sexual Assault. St Louis, MO: Mosby: 1997;19-65.
42. Bectel K, Podrazik M. Evaluation of the adolescent rape victim. Ped Clin North Am 1999;46:809-823.
43. Harner MA. Forensic issues in caring for the adult sexual assault victim. In: Giardino AP, Datner EM, Asher JP, eds. Sexual Assault Victimization Across the Life Span: A Clinical Guide. St. Louis: GW Medical Publishing 2003:251-262.
44. Ferrell J. Foley catheter balloon technique for visualizing the hymen in female adolescent sexual abuse victims. J Emerg Nurs 1995;21: 585-586.
45. Jones JS, Dunnuck C, Rossman L, et al. Adolescent Foley catheter technique for visualizing hymenal injuries in adolescent sexual assault. Acad Emerg Med 2003;10:1001-1004.
46. Teixeira WRG. Hymenal colposcopic examination in sexual offenses. Am J Forensic Med and Path 1981;2:209-215.
47. Slaughter L, Brown CRV. Colposcopy to establish physical finding in rape victims. Am J Ob Gyn 1992;166:83-86.
48. Lenahan LC, Ernst A, Johnson B. Colposcopy in evaluation of the adult sexual assault victim. Am J Emerg Med 1998;16:183-184.
49. Sommers MS, Fisher BS, Karjane HM. Using colposcopy in the rape exam: Healthcare, forensic, and criminal justice issues. J Forensic Nursing 2005;1:28-34.
50. Lauber AA, Souma ML. Use of toluidine blue for documentation of traumatic intercourse. Obstet Gynecol 1982;60:644-648.
51. McCauley J, Guzinski G, Welch R, et al. Toluidine blue in the corroboration of rape in the adult victim. Am J Emerg Med 1987;5: 105-108.
This issue covers Part I of a two-part series on evaluation and management of sexual assault in the emergency department. Part I of the series discusses initial ED care, physical exam, and evidence collection. Part II will cover laboratory analysis, pharmacotherapy, disposition, follow-up, documentation, and court testimony.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
