Special Feature: Right Ventricular Myocardial Infarction
Right Ventricular Myocardial Infarction
By William J. Brady, MD
Myocardial infarction of the right ventricle (RV) most often occurs in the setting of inferior wall myocardial infarction; the culprit artery is most often the right coronary artery (RCA). RV infarction complicates approximately 25% of inferior wall acute myocardial infarctions (AMI); it is very uncommon in anterior and lateral wall AMI. Isolated RV infarction is exceedingly rare.1 This co-infarction pattern of the inferior wall of the left ventricle and the RV is attributable to the coronary anatomy; the occlusive lesion is found in the right coronary artery (RCA), usually in the proximal third of the vessel, with involvement of various downstream arterial branches. The RCA and related branches perfuse the right atrium, RV, and additional portions of the left ventricle. The right conus artery, which usually originates from the aorta, supplies the upper anterior wall of the RV. Lastly, the posterior descending artery supplies a segment of the RV.
The classic triad of hypotension, clear lung fields, and jugular venous distension in a patient with an inferior wall AMI on electrocardiogram (ECG) is highly suggestive of RV infarction. Left ventricular filling pressures are dependent upon cardiac preload; with RV infarction, a significant reduction in preload occurs, and hypotension likely results; this hypotension may be worsened by nitroglycerin and morphine administration due to their vasodilating properties. However, the clinician is cautioned regarding hypotension in inferior AMI; other etiologies must be considered as well.
Electrocardiographic Manifestations of Right Ventricular Infarction
The most frequent electrocardiographic presentation is acute inferior wall ST-segment elevation AMI (STEMI).2 (See Figure 1.)
Figure 1. 12-lead ECG with STEMI of the Inferior Wall
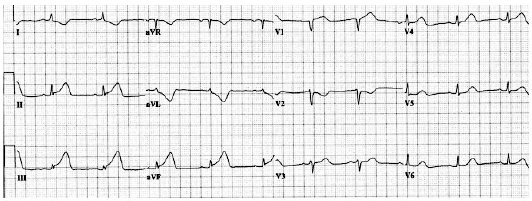 |
| Figure 1. Note that the degree of ST- segment elevation is greatest in lead III compared with leads II and aVF. Also, note the slight ST-segment elevation in lead V1. After nitroglycerin treatment, the patient developed hypotension, which promptly responded to IV normal saline infusion. The ECG findings, along with the clinical information, strongly suggest a right ventricular infarction in the setting of inferior wall ST-segment elevation infarction. |
A specific pattern of ST-segment elevation in the inferior wall STEMI suggests RV AMI. ST-segment elevation of greatest magnitude in lead III (compared with leads II and aVF) is highly predictive of acute RV infarction (Figures 1 and 2); it suggests the right coronary artery is more likely the culprit vessel, rather than the left circumflex artery.2
Figure 2. Lead V1 in a Patient with Inferior Wall AMI
 |
Figure 2. The ST-segment elevation (note its subtlety) in this lead suggests right ventricular infarction; this is true if ST-segment elevation also exists in the inferior leads. Reciprocal ST-segment depression usually is seen in leads aVL and I as well. |
The single electrocardiographic lead from the traditional 12-lead ECG, which best reflects RV injury is lead V1 ST-segment elevation in lead V1 usually is seen in RV AMI, if co-existing acute posterior infarction is not present (See Figure 3). RV AMI occasionally may present with ST-segment elevation in other standard precordial leads (V1 to V3, or even continuing to V5) mimicking an antero-septal AMI. In RV AMI, ST-segment elevation de-creases in magnitude from V1 to V5, whereas the opposite pattern is noted in anterior wall infarction.
Figure 3. Right Ventricular Infarction: Right-sided Leads
 |
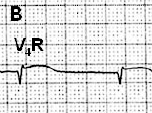 |
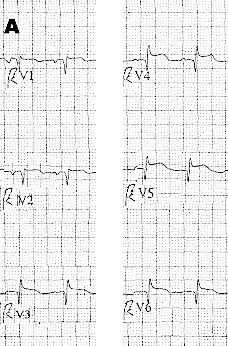
| Figure 3. Figure A: Right precordial leads V1R to V6R demonstrating ST-segment elevation of RV infarction; the Q waves are normal and don’t reflect chronicity. Figure B: Single lead V4R with ST-segment elevation. |
An important electrocardiographic abnormality suggestive of RV AMI is ST-segment elevation in additional right-sided leads. Although all six right-sided leads—V1R to V6R—may be used (Figure 3A), lead V4R has been found to be the single best lead for detection of RV infarction (Figure 3B). The degree of ST-segment elevation in any electrocardiographic lead, whether a standard or additional lead, may be of a small magnitude due to the relatively small muscle mass in the RV. With less ventricular myocardium, a reduced current of injury is noted, producing lower magnitude ST-segment elevation.
Diagnostic Adjuncts and Therapeutic Options
Additional diagnostic options include echocardiography and right heart catheterization. Echocardiography may demonstrate regional wall motion abnormalities, decreased right ventricular systolic function, and/or right ventricular dilitation. Right heart catheterization, or Swan-Ganz catheter monitoring, may demonstrate elevated right atrial pressures that equal or exceed pulmonary capillary wedge pressure, resulting from a noncompliant RV and impaired left ventricular filling.
Management priorities include standard therapy (e.g., anti-thrombotic, anti-coagulant, fibrinolytic) for an acute coronary syndrome, as well as attention to preload augmentation, inotropic support, and afterload reduction. To restore preload, the clinician should administer an IV fluid bolus to maintain a blood pressure of at least 90 mmHg and/or a pulmonary capillary wedge pressure of 15 mmHg. Vasodilating (e.g., nitroglycerin) and diuretic agents should be used cautiously, if at all. When aggressive saline loading does not correct the hypotension, inotropic medication may be required. Ionotropic agents, such as dobutamine or amrinone, improve RV function, thereby improving perfusion. Severe right heart failure unresponsive to ionotropic support may respond to afterload reduction or pressor support.
Patients with inferior wall STEMI with RV infarction have a markedly worse prognosis (both acute cardiovascular complications and death) compared with patients with isolated inferior wall STEMI.3 The subset of patients with RV infarction who develop decreased cardiac output and hypotension has increased, early in-hospital mortality. In most cases, RV function typically returns to normal. Patients sustaining severe RV damage, however, may have persistent RV dysfunction and develop chronic right heart failure.
Dr. Brady, Associate Professor of Emergency Medicine and Internal Medicine, Vice Chair, Emergency Medicine, University of Virginia, Charlottesville, is on the Editorial Board of Emergency Medicine Alert.
References
1. Anderson HR, et al. Right ventricular infarction; frequency, size and topography in coronary artery disease: A prospective study comprising 107 consecutive autopsies from a coronary care unit. J Am Coll Cardiol 1987;10:1223-1232.
2. Saw J, et al. Value of ST elevation in lead III greater than lead II in inferior wall acute myocardial infarction for predicting in-hospital mortality and diagnosing right ventricular infarction. Am J Cardiol 2001;87; 4:448-450.
3. Zehender M, et al. Eligibility for and benefit of thrombolytic therapy in inferior wall myocardial infarction: Focus on the prognostic importance of right ventricular infarction. J Am Coll Cardiol 1994;24:362-369.
Myocardial infarction of the right ventricle most often occurs in the setting of inferior wall myocardial infarction; the culprit artery is most often the right coronary artery. RV infarction complicates approximately 25% of inferior wall acute myocardial infarctions.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
