The Quality - Cost Connection: Keep digging to uncover root causes

Keep digging to uncover root causes
What do you do when your RCA hits dead end?
By Patrice Spath, RHIT
Brown-Spath & Associates
Forest Grove, OR
It can happen in any hospital. A cardiac surgery patient develops sepsis following a peripheral IV device-related infection. This infection ultimately contributes to the patient's death. Per Joint Commission standards, this event should undergo a root cause analysis (RCA).
A team is appointed to look into the cause of the infection, yet the review doesn't go as smoothly as other sentinel event investigations. First, the team finds it difficult to describe the steps leading up to the event. Nothing stands out as extraordinary and the team eventually decides that the root cause cannot be identified. The patient's infection is presumed to be an unfortunate, but unavoidable, complication.
It's not common, but on occasion an RCA team is stuck and can't find the root cause of a sentinel event. Deficiencies in the quality of care or medical errors may not be readily apparent by using traditional investigation techniques such as cause-and-effect diagrams or by answering questions on The Joint Commission's root cause analysis template. If the team reaches a dead end in the investigation, alternate inquiry methods can help evaluate the event and potential causes.
One such method is a barrier analysis. Using this technique, the RCA team would examine the effectiveness of safeguards or barriers in place to protect patients from experiencing an IV device-related infection. The team identifies all existing safeguards (e.g., IV site care, regular catheter replacement, etc.) and the facts surrounding the function of each safeguard. It may be necessary to obtain input from people not represented on the team. The goal is to identify barriers that should have worked to prevent the infection and resulting sepsis and identify any new barriers that need to be put in place. The team examines each safeguard to determine whether it failed or succeeded. In addition, the team determines what additional physical, human action, and/or administrative controls might have prevented the event. In Figure 1is a partially completed barrier analysis for the infection event. A separate barrier analysis could be done for the problem of sepsis, which might have been prevented if the IV site infection had been promptly identified and adequately managed.

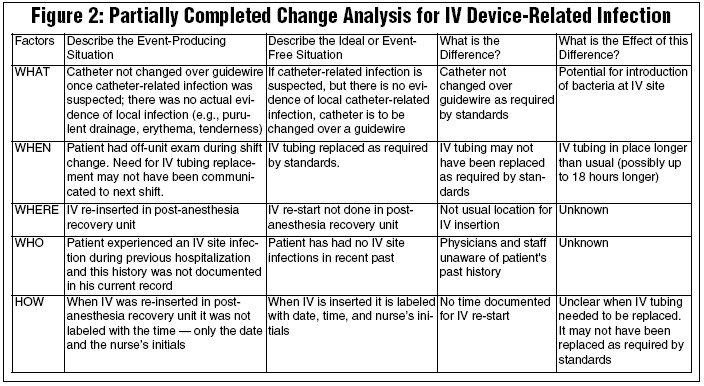
Change analysis is another investigative technique. This tool is used to analyze the differences between usual practices and what happened during the incident-producing situation. Using change analysis the team identifies specific factors or differences that caused the outcome of a certain task to deviate from the anticipated outcome. The team is instructed to identify changes as well as the results of those changes. The distinction is important, because identifying only the results of change may not prompt the team to identify all causal factors of an event.
A partially completed change analysis worksheet for the infection event is shown in Figure 2. Change analysis involved the following steps:
- Describe the event situation and describe the same or similar situation that did not result in an undesirable event.
- To expand the thinking of the team, these descriptions are categorized into major factors that influence performance. The categories here are: what, when, where, who, and how. The factors listed in this example are only guidelines.
- For each factor thought to influence performance, describe the "event-producing situation" relevant to that factor and the "ideal or event-free" situation. Issues to consider in each of the major factors (not relevant to every type of event):
What
- What is the undesirable outcome?
- What occurred to create the undesirable outcome?
- What occurred prior to the precipitating event?
- What occurred following the precipitating event?
- What operational activities were under way when the tasks leading to the event occurred?
- What supplies/equipment were being used?
- What barriers should have been in place to prevent the undesirable outcome?
- What barriers were in place but failed to stop the undesirable outcome?
When
- When did the activities leading up to the event occur?
- Was the facility on any special status at the time (e.g., emergency admissions only, high inpatient census, etc.)?
- Did the time of day or day of the week have an effect on the outcome? Staff availability? Physician availability?
- For how many continuous hours had involved staff been working?
Where
- Where did the activities leading up to the event occur?
- What were the physical conditions in the area(s)?
- Where was the event first identified?
- Was location a factor in causing the event?
Who
- Who were the direct/indirect people involved in care for the patient prior to the event?
- Which people were involved in caring for the patient following the event?
- What were the training/qualifications of the people involved?
- Who was supervising the activities?
- What patient factors might have increased the likelihood of the event? Which of these factors were controllable?
How
- Was the event caused by an inappropriate action?
- Did procedures exist for the activities/tasks involved?
- Are procedures based on literature evidence or "best practices?"
- Did the procedures related to the tasks have sufficient detail?
- Did the procedure have sufficient fail-safe mechanisms?
- Did the procedure cover work tasks in proper sequence?
Once the "event situation" and the "event-free situation" are described, the team evaluates the differences or variances to determine each factor's impact on the undesirable outcome.
If techniques such as barrier analysis and change analysis fail to uncover the root cause of the IV site infection, the team should turn their focus to how the patient was managed once the infection was first suspected.
It can happen in any hospital. A cardiac surgery patient develops sepsis following a peripheral IV device-related infection. This infection ultimately contributes to the patient's death. Per Joint Commission standards, this event should undergo a root cause analysis (RCA).Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
