A Simple Screen for Cancer?
A Simple Screen for Cancer?
Abstract & Commentary
By Allan J. Wilke, MD, Residency Program Director, Associate Professor of Family Medicine, University of Alabama at Birmingham School of MedicineHuntsville Regional Medical Campus, Huntsville. Dr. Wilke reports no financial relationship to this field of study.
Synopsis: An elevated white blood cell count is a risk factor for several cancers in women.
Source: Margolis KL, et al. Arch Intern Med. 2007;167:1837-1844.
The notion that inflammation and cancer are linked, and that the relationship is possibly causal, has been with us for a long time.1 Using the Women's Health Initiative (WHI) database, Margolis and colleagues prospectively examined the correlation of the white blood cell (WBC) count and the development of cancer of the breast, the colon and rectum, the endometrium, and the lung. After exclusion (including those with WBC < 2.5 X 109 cells/L or > 15.0 X 109 cells/L), 143,748 women were available for study. The examination of the relationship of WBC and endometrial cancer was limited to the 85,621 women who still had uteruses. Subgroup analysis for breast cancer and colorectal cancer was performed on women who had negative screening (normal mammograms or negative fecal occult blood testing, colonoscopy, or sigmoidoscopy, respectively) before admission into the study. The subjects had a single WBC drawn on enrollment and annual or semiannual follow up, when they were quizzed on any new diagnosis of cancer (other than non-melanoma skin cancer). Any new diagnosis was confirmed by medical record review. The WBC counts were divided into quartiles, 2.50-4.79, 4.80-5.69, 5.70-6.79, and 6.80-15.00 X 109 cells/L. The women were on average 63 years old, white (82%), and overweight (35%) or obese (30%). Twenty percent used aspirin regularly. In multivariate analysis, using the first (lowest) quartile as the reference (hazard ratio [HR] = 1), elevated WBC counts (fourth quartile) were statistically significantly associated with invasive (but not in situ) breast cancer, colorectal cancer, endometrial cancer, and lung cancer. This data is summarized in the table below.
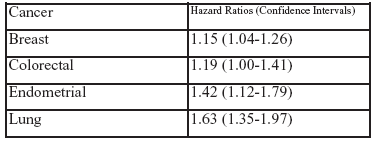 |
To parry the concern that the cancers were subclinical (ie, they were present, but undetectable, at the start of the study, the author recalculated the rates after excluding cancers that were discovered within the first two years of the study. The results were unchanged. When they looked at individuals who had negative screening for breast or colorectal cancer at baseline, there were statistically insignificant trends for increased risk.
Commentary
That an elevated WBC count is associated with cancer incidence and mortality is not a novel concept.2 The authors speculate about the plausibility of their results and present interesting intermediate data that linkinflammation to the initiation and promulgation of cancer. This involves the cellular production of cytokines and chemotactic molecules and their involvement with cell growth, migration, and differentiation. The topic was reviewed in 2002.3
Certainly, the prospect of an ordinary blood test that can screen for four cancers is appealing. However, there are some problems with this study. One of the things that bothered me was the selection of the WBC quartiles. The authors did not provide a rationale for having different-sized intervals. The fourth quartile's range overlaps the "normal" range for my hospital's laboratory (4.8-10.8 X 109 cells/L). The hazard ratios were not huge (at best, a 63% increased risk for lung cancer) and for colorectal cancer, barely significant, since the confidence interval included 1.00.
How can we put the results of this study to good use? In their accompanying editorial, Roy and Khadekar remark, "While this association was statistically significant, the magnitude of the difference was somewhat unimpressive ... Moreover, because there are obviously numerous factors that can affect the WBC count, the authors' suggestion of possible future clinical value seems somewhat unrealistic."4 I agree. The WBC is too blunt an instrument to use as a screening test. On the other hand, if your female patient presents with an elevated WBC and you cannot reasonably account for the elevation, consider recommending follow-up testing (mammography, endometrial biopsy, colonoscopy, chest x-ray), based on her risk factors and any previous testing.
References
1. Balkwill F, Mantovani A. Lancet. 2001;357:539-545.
2. Shankar A, et al. Arch Intern Med. 2006;166:188-194.
3. Shacter E, Weitzman SA. Oncology (Williston Park). 2002;16:217-226, 229; discussion 230-232.
4. Roy HK, Khandekar JD. Arch Intern Med. 2007;167:1822-1824.
An elevated white blood cell count is a risk factor for several cancers in women.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
