ECG Review: Chest Pain After Bypass
ECG Review
Chest Pain After Bypass
By Ken Grauer, MD, Professor, Department of Community Health and Family Medicine, University of Florida Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
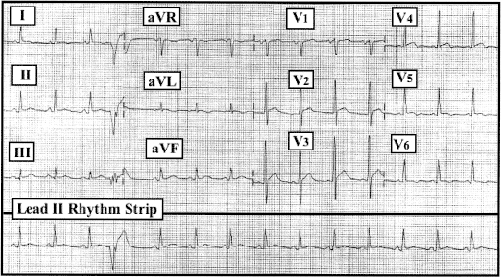 |
Figure: 12-lead ECG and lead II rhythm strip obtained from a 59-year-old man after coronary bypass. |
Clinical Scenario:
The 12-lead ECG and lead II rhythm strip in the Figure were obtained from a 59-year old man several days after coronary bypass. He complained of postitional chest pain. How would you interpret his ECG given this clinical context?
Interpretation/Answer:
The rhythm is sinus at a rate of 90/minute. One PVC (premature ventricular contraction) is seen. All intervals are normal. The mean QRS axis is +40°. There is no sign of chamber enlargement. A small, narrow q wave is seen in leads III and V6. Transition is early (occurring between leads V1 to V2). However, the most interesting finding on this tracing is the subtle ST segment elevation that is seen in virtually all leads except aVR, aVL, and V1. There is beginning T wave inversion in leads V5, V6.
The finding of diffuse (albeit subtle) ST segment elevation in the absence of ST segment depression and only minimal (beginning) T wave inversion as seen here should strongly suggest acute pericarditis as the diagnosis. This is consistent with the clinical scenario in this case (ie, occurrence shortly after coronary bypass surgery and positional nature of the chest pain). Even though no pericardial friction rub was heard, the history, negative troponins, and serial ECGs obtained in this case were felt to confirm the diagnosis.
The 12-lead ECG and lead II rhythm strip in the Figure were obtained from a 59-year old man several days after coronary bypass. He complained of postitional chest pain. How would you interpret his ECG given this clinical context?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
