Diagnosing UTI is as Simple as 1, 2, 3
Diagnosing UTI is as Simple as 1, 2, 3
Abstract & Commentary
By Allan J. Wilke, MD, Residency Program Director, Associate Professor of Family Medicine, University of Alabama at Birmingham School of MedicineHuntsville Regional Medical Campus, Huntsville. Dr. Wilke reports no financial relationship to this field of study.
Synopsis: Three criteria identify women who would benefit from empiric antibiotics for cystitis.
Source: McIsaac WJ, et al. Arch Intern Med. 2007;167:2201-2206.
While the practice of using empiric antibiotics to treat women who present with symptoms of cystitis is common and recommended,1 physicians are not adept at identifying which women actually need treatment. In a recent study,2 physicians prescribed antibiotics 60% of the time that cultures were negative and did not prescribe them for 25% of women who had positive cultures. Building on and extending their previous work,3 McIsaac and colleagues tested a 4-item decision aid. The four criteria were: burning or pain on urination, symptoms present for only 1 day, leukocytes on dipstick, and nitrites on dipstick. The presence of two or more criteria predicted a positive culture at least 70% of the time, and the rule recommended an antibiotic prescription and no culture. Women with only one or no criteria had a probability of infection of 30%. In this situation, the recommendation was for a urine culture and an antibiotic only if the culture were positive. The current validation study was conducted in April 2002 in the community practices of Canadian family physicians. Inclusion criteria were female gender and age 16 or greater with symptoms suggestive of acute cystitis. Women who were pregnant, living in nursing homes, immunocompromised, taking antibiotics, or who had renal tract abnormalities or indwelling catheters were excluded. The 331 subjects (average age 45.2 years) provided a clean-catch urine sample that was dipped for leukocytes and nitrites and sent for culture. The physicians recorded the subjects' signs and symptoms, their diagnoses, and whether they were prescribed antibiotics. They had the leukocyte and nitrite results and were asked to indicate whether they would normally have obtained a urine culture in each case.
The patients rated the severity of their symptoms on a four-point scale (none, mild, moderate, severe). They were asked whether they would be willing to wait for the report of the urine culture before a decision was made on prescribing antibiotics. A urine culture was termed positive if it contained ≥ 102 colony-forming units (CFU)/ml.
Ninety-eight percent of women reported at least one urinary symptom (frequency, urgency, burning or pain). Two hundred eight (63%) cultures were positive. As the number of criteria increased, so did the percentage of positive cultures (0, 1, 2, 3, and 4 criteria and 24%, 41%, 68%, 76%, and 88%, respectively). The UTI signs and symptoms that were statistically significant were urgency, burning/painful voiding, voiding small amounts, flank pain/discomfort, greater than trace leukocytes, and positive nitrites. Only one day duration of symptoms was not associated with a positive culture. This criterion was dropped and the probabilities of positive culture were calculated with the remaining 3 criteria:
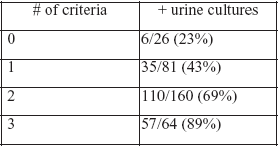 |
Using this decision aid, 224 women (those with ≥ 2 criteria) would have been prescribed an antibiotic without getting a culture, and 107 women (≤ 1 criterion) would have been cultured and told to wait until the results were available before getting an antibiotic. Of the 224 women getting antibiotics, 57 (25%) would not have needed them ("unnecessary antibiotics"). Of the 107 women awaiting culture, 41 (38%) would eventually need them.
In reality, the physicians prescribed antibiotics to 292 women, 68 more than would have received them if the physicians had followed the decision rule. 95 women received "unnecessary antibiotics," 38 more than would have received them, again, if the rule had been followed. The physicians ordered 259 urine cultures, 152 more than the decision rule recommended.
Three hundred nineteen women were asked whether they would be willing to wait for urine culture results before receiving a prescription for antibiotics. One hundred forty reported they definitely would not. These women reported more severe symptoms than women who were willing to wait. Applying the decision rule to this group of 319 women, 36 would have received a recommendation to wait. Only nine women in this group of 36 had a positive culture.
When the investigators looked at the strategy of prescribing empiric antibiotics based on symptoms alone (that is, women with at least two symptoms and without leukocyte and nitrite results), 294 of 327 women would have received antibiotics and 100 of these would have received them unnecessarily.
Commentary
This seems like a relatively easy decision rule to remember and apply. Choosing the proper antibiotic may not be as easy. Escherichia coli is the most frequent offender in urinary tract infections, followed by Staphylococcus saprophyticus (especially in younger women), Klebsiella species, Proteus species, and enterococci. According to my hospital's microbiology laboratory, trimethoprim/ sulfamethoxazole (TMP/SMX, Bactrim®), the most common antibiotic ordered empirically for women with cystitis, was effective against E. coli only 79% of the time. Coincidentally, levofloxacin also earned a 79% rating. Amoxicillin fared far worse at 54%. My lab does not publish the susceptibilities for S. saprophyticus, but it is generally considered susceptible to TMP/SMX. Ordering TMP/SMX would be great if the culprit is Klebsiella species (96%), but not so great if it's Proteus mirabilis (78%). Nitrofurantoin is a good second-line drug. However, it has no activity against Proteus, and you generally cannot get away with anything less than seven days of treatment.
There are a couple of thoughts about this study that gave me pause. The cutoff of 102 colony-forming units for a positive culture is lower than the one I generally use, but it is a one that shows up frequently in studies of urinary tract infections. The effect is to include many more women in the "culture-positive" group, including people that I probably would not have treated. The other thought is how to handle the patient who will not wait for culture results. One strategy would be to "cave-in", prescribe an antibiotic, and hope for the best, including no adverse drug reaction. My preferred strategy would be to discuss the risks, including adverse drug reactions and the development of antibiotic resistance, and the benefits of taking an antibiotic. If the patient symptoms were severe, one could turn to a urinary anesthetic such as phenazopyridine (Pyridium®). My impression, though, is that the recent news of community-based methicillin-resistant Staphylococcus aureus has made patients more receptive to thinking twice before taking an antibiotic.
References
1. Warren JW, et al. Clin Infect Dis. 1999;29:745-758.
2. O'Brien K, et al. J Antimicrob Chemother. 2007;59:1200-1203.
3. McIsaac WJ, et al. Arch Intern Med. 2002;162:600-605.
Three criteria identify women who would benefit from empiric antibiotics for cystitis.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
