Special Feature: The Role of Weaning Parameters in 2008
Special Feature
The Role of Weaning Parameters in 2008
By David J. Pierson, MD, Editor, Professor, Pulmonary and Critical Care Medicine, Harborview Medical Center, University of Washington, Seattle, is Editor for Critical Care Alert.
What is Weaning?
Most critically ill patients require mechanical ventilation, and, according to one large survey, the weaning process occupies about 40% of the time that patients spend connected to the ventilator.1 Yet how "weaning" is defined varies a great deal. In the strictest sense weaning should refer to the gradual withdrawal of positive-pressure ventilation and its replacement by the patient's own spontaneous breathing. Most of us broaden this to mean the process of discontinuing ventilatory support, irrespective of its pace or difficulty. However, by "weaning" many clinicians actually mean "extubation," lumping together two processes—liberation from mechanical ventilation and removal of the artificial airway. This imprecision muddies the water for both conceptual understanding and bedside application, and the resulting confusion extends throughout the literature on weaning.2
When the subject of ventilator weaning was last discussed in one of these essays 6 years ago,3 new international evidence-based weaning guidelines had just been released by a combined task force of the American College of Chest Physicians, the Society of Critical Care Medicine, and the American Association for Respiratory Care.4 These landmark guidelines triggered a paradigm shift with respect to discontinuation of mechanical ventilation, from "predicting" (that is, deciding on the basis of clinical and physiological indices when weaning should commence) to "checking" (that is, finding out by means of an empirical trial of spontaneous breathing whether the patient was ready to be liberated from ventilatory support). Although publication of new studies, analyses, and guidelines has continued apace,5 nothing has appeared since publication of the ACCP-SCCM-AARC guidelines to overturn or substantially change this new 21st-century approach to weaning.
The shift from predicting when a patient was ready for a trial of weaning—using various measures and indices collectively referred to as weaning parameters—to an empirical trial of spontaneous breathing to find out whether he or she is ready, has meant that weaning parameters are no longer used routinely in many ICUs. Are weaning parameters still useful? This essay examines the present status of these measurements, including how they may be integrated into the current evidence-based weaning process, and what their findings mean clinically when a spontaneous breathing trial (SBT) is unsuccessful.
What Are The Important Weaning Parameters And What Do Their Results Mean?
The most comprehensive review of weaning parameters I have seen is one by Epstein in the Respiratory Care Clinics of North America, published in 2000.6 In it, the author describes some 50 different assessments that have been studied in the prediction of successful weaning. Included are measures of oxygenation and gas exchange, measures of capacity and load both simple and complex, various integrative indices (some of them fairly complicated, requiring special apparatus), and clinical factors such as mental status and cough effectiveness. Although some centers have adopted specialized measurements such as the airway occlusion pressure (P0.1) in routine management, the weaning parameters used most widely are those initially introduced by Sahn and Lakshminarayan7 and by Yang and Tobin.8
Sahn and Lakshminarayan7 performed simple bedside measurements on 100 consecutive patients whose managing physicians were about to discontinue ventilatory support, and found that the presence of all 4 of the following findings predicted successful weaning in every instance:
- Vital capacity (VC) at least 10 mL/kg
- Maximal inspiratory pressure (MIP) at least-30 cm H2O
- Resting minute ventilation requirement 10L/min or less
- Ability to double this resting minute ventilation during a 15-sec period of voluntary hyperpnea
The first 3 of these threshold values are generally used, while the last (which requires extra effort and a cooperative patient) is less often applied today. To these routine measurements was added the rapid shallow breathing index (RSBI), reported by Yang and Tobin,8 which is the spontaneous respiratory rate divided by the average spontaneous tidal volume (f/VT) assessed during a short period of spontaneous unassisted breathing. For example, in a patient with spontaneous respiratory rate 24 breaths/min and average tidal volume of 400 mL (0.4 L), the RSBI would be 24 divided by 0.4, or 60. Compared with numerous other measurements and combinations of measurements, these investigators found that an RSBI >105 was the best predictor of a failed weaning attempt. Over the last 15 years, the RSBI has become probably the most commonly used weaning parameter.
Weaning in the Era of Evidence-based Medicine
Although there have been hundreds of studies examining the efficacy of different weaning parameters in predicting when patients are ready for discontinuation of ventilatory support, no individual measurement or combination of measurements will detect all patients who could safely be weaned.9 This is illustrated by two large, multicenter weaning trials published in the mid-1990s.10,11 Each of these studies examined the relative efficacy of T-piece trials, pressure support, and intermittent mandatory ventilation as weaning strategies in patients considered difficult to wean by the clinicians managing them. Both studies required a 2-hour SBT for all patients during the screening phase to assure that they still needed ventilatory support—and in each case nearly three-fourths of all screened patients were found ineligible for study entry because they could simply be extubated after the SBT. This illustrates the fact that clinicians are often unable to tell whether a patient is ready for weaning and extubation, despite their experience and the results of various weaning parameters.
The imperfect performance of existing weaning parameters, and the problems identified with the published studies on the prediction of successful weaning, led the ACCP-SCCM-AARC consensus group4 to conclude that performing an SBT was the only reliable way to determine whether a given patient was ready to come off the ventilator, in order to avoid unnecessary prolongation of mechanical ventilation. According to current guidelines, an SBT should be performed in any patient who meets the following 5 general readiness criteria:
- Evidence for some reversal of the underlying cause for acute respiratory failure
- Adequate arterial oxygenation (for example, arterial PO2 at least 60 mm Hg on 40% oxygen with positive end-expiratory pressure 5 cm H2O or less)
- Acceptable acid-base balance (for example, arterial pH 7.25 or higher)
- Hemodynamic stability (absence of active myocardial ischemia, and blood pressure supportable without requirement for significant vasopressor support)
- Sufficient ventilatory drive and neuromuscular function to initiate an inspiratory effort
The evolution of the approach to weaning over the last 4 decades is illustrated schematically in Figure 1. Prior to 1970 clinical judgment was the main gauge of when a patient was ready to be removed from the ventilator and extubated (Figure 1A). Simultaneous with the emergence of weaning parameters in the mid-1970s was an approach, advocated by some, of progressively decreasing the proportion of the patient's overall work of breathing that was provided by the ventilator, reasoning that this transition would be facilitated by the return of spontaneous ventilatory capacity and would result in the earliest possible liberation from mechanical ventilation (Figure 1B). Using this approach, partial ventilatory support was provided initially by intermittent mandatory ventilation, and then beginning in the mid-1980s by pressure support.
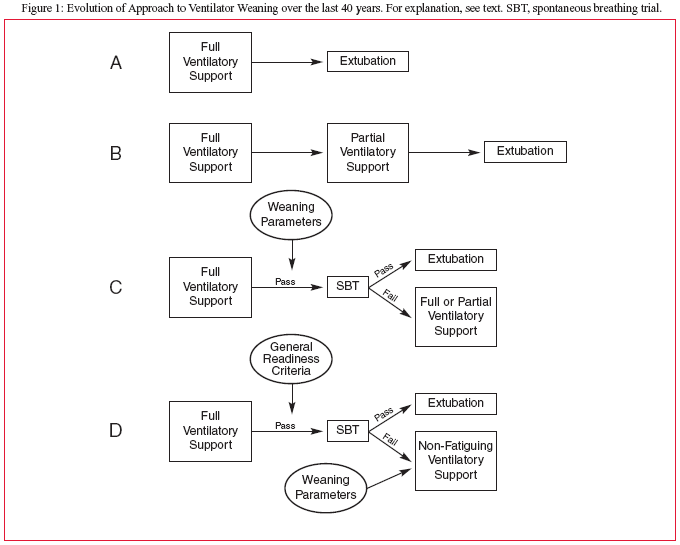
Most commonly, however, as depicted in Figure 1C, patients were managed with full ventilatory support, usually via volume-targeted assist-control ventilation, with measurement of weaning parameters to screen for readiness for weaning. At many institutions, the performance of a fixed set of weaning parameters (in my department consisting of VC, MIP, VE, and RSBI) each morning on every ventilated patient comprised a substantial proportion of each ICU respiratory therapist's duties. The physicians managing the patient then decided whether to attempt weaning based on these weaning parameters. This attempt took the form of an SBT, with success or failure judged on clinical assessment (respiratory rate, heart rate, evident ventilatory effort, and general appearance) plus the findings on arterial blood gas analysis after 30 minutes. Patients who "passed" the SBT were extubated if there were no other contraindications, and those who "failed" were returned to full ventilatory support, and the whole process was repeated the next morning.
Today, based on the systematic review of available studies5,9 and the lessons of the Brochard10 and Esteban11 studies about the accuracy of our ability to judge when someone is ready for weaning, the current approach (Figure 1D) dispenses with weaning parameters in making the initial decision to perform an SBT. Instead, the 5 general readiness criteria listed above are used. Patients who fail the SBT are returned to full ventilatory support—or at least to ventilator settings that eliminate evidence of air-hunger or ongoing work of breathing—and reassessed daily so long as the 5 conditions are met.4 It is at this point that weaning parameters can be helpful—not in the decision to commence weaning but instead to sort out the reason(s) for failure (see Table 1).

A patient who makes no inspiratory effort when ventilatory support is interrupted, or generates an inadequate minute ventilation in the absence of tachypnea, can be assumed to have insufficient ventilatory drive as at least part of the problem. Most often this is due to narcotics and other drugs. When patients breathe rapidly and shallowly on removal or reduction of ventilatory support, or when they cannot generate more than half or three-fourths of the required minute ventilation, the necessary work of breathing exceeds their capabilities. This might be because of excessive work imposed by the breathing circuit (common with pre-1990s ICU ventilator models but less so today if they are set up and adjusted properly), a too-high minute ventilation requirement, airway obstruction, or ventilatory muscle weakness. The last is common, particularly after prolonged critical illness, and is further suggested by a low vital capacity and/or maximum inspiratory pressure.
When a high minute ventilation requirement is present (eg, exceeding 12-14 L/min for a normal PaCO2) in a patient who fails an SBT, one or both of two basic physiologic processes may be present. Either CO2 production is excessive (which indicates a systemic, metabolic problem, rather than a pulmonary problem), and/or there is excessive wasted ventilation (high dead space, which suggests a pulmonary cause for the high minute ventilation requirement). Bedside assessment using an arterial blood specimen and a metabolic cart or other monitoring system can have practical value in sorting out these two mechanisms.
Measuring Weaning Parameterscine
Soo Hoo and Park12 surveyed 102 respiratory therapists in 9 Los Angeles-area hospitals and found that there was great variation not only in which weaning parameters were used but also in the techniques used to measure them. For tests of spontaneous breathing, a few disconnected the patient from the ventilator—as done in both the classic studies mentioned7,8—but the great majority left the circuit intact, changed the ventilator settings, and simply took the readings off the ventilator's digital display. Various settings of CPAP and pressure support were used during the test of spontaneous breathing—from zero to 10 cm H2O for each, in essentially every possible combination. In addition, there was great variation in the time the therapist waited before recording the weaning parameters—from within the first minute to >15 minutes.
The point here is that most of the time weaning parameters are no longer measured as intended (and studied) by their original proponents. Whatever methodological problems may exist in the published studies, it is by no means clear that any reported predictive value for the various weaning parameters carries over using these variations in technique. For example, in both classic studies,7,8 respiratory rate and minute ventilation were directly measured over a full minute by the investigators, and the average tidal volume was calculated. The ventilator's digital readout of minute ventilation reflects a running estimate determined from rate and tidal volume over several breaths or some fixed (short) time interval, which varies and may or may not reflect what would be measured over a full minute.
In addition, a patient's spontaneous breathing pattern when ventilator breaths suddenly stop may take at least a couple of minutes to stabilize. The values for rate, tidal volume, and minute ventilation taken from the ventilator's digital readout during the first 30-60 seconds of spontaneous breathing may not reflect the patient's subsequent, stable breathing pattern. While minimizing circuit interruptions is important for infection control and other reasons, the clinician should wait a minimum of two minutes before determining rate, tidal volume, and minute ventilation in order to most accurately predict the patient's capabilities for purposes of weaning.
Weaning vs Extubation: A Word of Caution
Management of a patient with acute respiratory failure must deal satisfactorily with 4 separate processes:
- Oxygenation
- Ventilation
- Airway Protection
- Secretion Clearance
An SBT assesses only the first two of these processes. That is, a patient who passes an SBT is able to breathe without assistance and attain satisfactory oxygenation of the blood. However, although most patients who have recovered to this extent can also maintain an open upper airway and adequately clear respiratory secretions, there are some who cannot, and extubating such patients is likely to fail.
Coplin et al13 studied brain-injured patients who met accepted criteria for weaning but who remained unconscious. The investigators noted 6 factors related to the need for airway care, in an attempt to derive a set of "extubation parameters" unrelated to the ability to maintain adequate oxygenation and ventilation. The 6 factors were the quantity, viscosity, and appearance of the suctioned secretions, the presence of a gag reflex, whether the patient coughed spontaneously without stimulation, and the frequency of airway suctioning. Of these, only the last 2 (absence of spontaneous cough, and requirement for suctioning at least every 2-3 hours) were statistically correlated with the need for re-intubation once the patients had been extubated. In a more recent study by Mokhlesi and colleagues,14 of several factors examined, the only predictors of the need for reintubation among patients extubated following a successful SBT were moderate to copious secretions, a Glasgow Coma Scale score of 10 points or less, and an arterial PCO2 >44 during the SBT.
Thus, although we still do not have very good ways to predict whether a patient can maintain a patent airway and adequately clear respiratory secretions after extubation, separate consideration beyond the results of an SBT should be given to this aspect of the process of liberation from ventilatory support.
References
- Esteban A, et al. Chest. 1994;106:1188-1193.
- Pierson DJ: Respir Care. 1995;40:228-232.
- Pierson DJ. Crit Care Alert. 2002 Apr;10(1):4-8.
- MacIntyre NR, Cook DJ, et al. Chest. 2001(Dec);120(6 suppl):375s-395s.
- Boles JM, et al. Eur Respir J. 2007;29(5):1033-1056.
- Epstein SK. Respir Care Clin North Am. 2000;6(2):253-301.
- Sahn SA, Lakshminarayan S. Chest. 1973;63:1002-1005.
- Yang KL, Tobin MJ. N Engl J Med. 1991;324:1445-1450.
- Meade M, et al. Chest. 2001;120(6 Suppl):400s-424s.
- Brochard L, et al. Am J Respir Crit Care Med. 1994;150:896-903.
- Esteban A, et al. N Engl J Med. 1995;332:345-350.
- Soo Hoo GW, Park L. Chest. 2002;121(6):1947-1955.
- Coplin WM, et al. Am J Respir Crit Care Med. 2000;161:1530-1536.
- Mokhlesi B, et al. Respir Care. 2007 Dec;52(12):1710-1717.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
