Borderline Personality: Somatic Presentations in the Primary Care Setting
Borderline Personality: Somatic Presentations in the Primary Care Setting
Authors: Randy A. Sansone, MD, Professor, Departments of Psychiatry and Internal Medicine, Wright State University School of Medicine, Dayton, OH; Director of Psychiatry Education, Kettering Medical Center, Kettering, OH; and Lori A. Sansone, MD, Family Medicine Physician, Wright-Patterson Air Force Base, Dayton, OH. The views and opinions expressed in this article are those of the authors and do not reflect the official policy or the position of the United States Air Force, Department of Defense, or U.S. Government.
Peer Reviewer: Ashley Benjamin, MD, MA, Staff Psychiatrist, Ambulatory Mental Health Clinic, Oklahoma City VAMC, Assistant Clinical Professor, Department of Psychiatry and Behavioral Sciences, University of Oklahoma Health Sciences Center, Oklahoma City, OK.
Introduction
Clinicians are typically introduced to the academic phenomenon of borderline personality disorder (BPD) during their psychiatric rotations in medical school. In these settings, the psychological characteristics of the disorder tend to be more prominent, with trainees keenly learning the association between dramatic self-harm behaviors (e.g., self-mutilation, multiple suicide attempts, self-induced vomiting) and BPD. In contrast, in the primary care setting, the symptoms of BPD may manifest primarily as various somatic complaints. Rather than being diagnosed with BPD, these challenging primary care patients typically are designated as "difficult patients." This article will review the traditional psychiatric characteristics of BPD and then highlight the manner in which the associated psychodynamics of these individuals may generate multiple somatic symptoms in primary care settings.
Borderline Personality Disdorer: A Working Definition
Originally coined by Stern in the 1930s,1 the term "borderline" initially was used to describe a group of psychiatric patients who demonstrated multiple neurotic symptoms in conjunction with fleeting episodes of psychosis. Because these individuals appeared to vacillate between the two symptom domains of neurosis and psychosis, they were described by Stern as being "on the border" or "borderline."
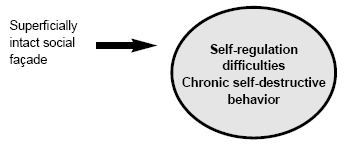
In contemporary terms, a pragmatic or working definition of BPD encompasses the following three patient characteristics: an intact social façade, such that during brief periods of social interaction (e.g., primary care appointments), patients with BPD can appear amazingly intact; chronic self-regulation problems (e.g., eating disorders, substance abuse, alcohol abuse, abuse of prescription medications, promiscuity, difficulty regulating monies, inability to regulate pain); and longstanding self-harm behavior (e.g., self-mutilation such as cutting, burning, hitting, or scarring oneself; multiple suicide attempts; self-defeating behavior, particularly in the areas of relationships and employment; intentional endangerment of one's health). The relationships among these longstanding characteristics might be conceptualized using the paradigm of a coated chocolate candy. The hard coating would represent the intact social façade, whereas the soft chocolate interior would represent the chronic difficulties with self-regulation and self-harm behavior. (See Figure 1.)
| Figure 1. The Relationships Among the Three Fundamental Clinical Characteristics of Borderline Personality Disorder |
|
Because of the seemingly paradoxical nature of BPD (i.e., a relatively intact social veneer juxtaposed with relentless self-regulation difficulties and chronic self-harm behavior), this intriguing disorder has been dramatized in a number of films. These include "Leave Her to Heaven" (1945), "Play Misty for Me" (1971), "The Rose" (1979), "Fatal Attraction" (1987), "Misery" (1990), "Single White Female" (1992), and "The Crush" (1993). In keeping with the general definition of BPD, all of these films illustrate protagonists who appear "normal" but are truly chaotic and destructive to themselves as well as others.
The Epidemiology of BPD
Prevalence Rates of BPD. General U.S. Population. According to the Diagnostic and Statistical Manual of Mental Disorders, 4th edition, text revision,2 the prevalence of BPD in the general population is approximately 2%. In contrast, Stone3 states that the prevalence of this disorder may be as high as 10%. Interestingly, in the general population, the prevalence of all personality disorders is between 5% and 10%.4 Therefore, if Stone's estimate is accurate, BPD could be the most prevalent personality disorder in the U.S. general population.
Mental health settings. As one would expect, BPD is a common personality disorder in psychiatric settings.5 According to the DSM-IV-TR,2 the prevalence of BPD is 20% among psychiatric inpatients and 10% among psychiatric outpatients. In addition, up to 50% of psychiatric inpatients with a personality disorder diagnosis suffer from BPD.6 In contrast to the preceding findings, we have found in our studies even higher rates of BPD among inpatient (i.e., up to 50%)7 and outpatient (i.e., up to 22%)8 psychiatric samples.
Primary Care Settings. There has been only one rigorous empirical study of the prevalence of BPD in a primary care setting. In this study of outpatients in an internal medicine setting, investigators found a prevalence rate of 6.4%.9 Studies with self-report measures, which tend to over-diagnose the disorder, have generally found in resident primary care clinics rates of borderline personality symptomatology between 20% and 30%.10
International Populations. Although BPD may be over-represented in Westernized countries,11 the disorder also has been documented in less developed countries.12-14 Whether there is a genuinely higher prevalence of BPD in Westernized countries, or whether the disorder in non-Westernized countries is masked behind a host of misleading somatic symptoms (i.e., the tempering effects of culture on symptoms) and/or under-diagnosed by practitioners, is unknown.
Gender Distribution of BPD. According to the DSM-IV-TR,2 more women than men suffer from BPD. However, this postulated gender difference may be due to the unintentional effects of sampling bias.15 To explain this, women with BPD tend to have histrionic features, self-directed self-harm behavior (e.g., self-cutting), and Axis I diagnoses of eating disorders and post-traumatic stress disorder.16 Because of these preceding symptoms, women with this disorder tend to be relegated to psychiatric treatment settings, where empirical studies take place. In contrast, men with BPD tend to have antisocial features, externally directed self-harm behavior (e.g., bar fights, reckless driving, domestic violence), and Axis I diagnoses of substance abuse.16 Therefore, men with this disorder tend to be misdiagnosed with antisocial personality disorder and often wind up in prison settings.17,18
BPD in the Elderly. One would expect that a personality disorder such as BPD would, to some degree, persist into older adulthood. However, psychiatric clinicians seem to encounter the traditional behavioral features of the disorder more commonly in younger patients. Regardless, there are older patients with BPD, partially reinforcing the concept that personality disorders tend to be relatively stable over time. According to research findings, aging individuals with BPD may manifest difficulties with planning and setting goals, self-destructive behavior in the form of not eating and weight loss, polypharmacy, and noncompliance with reasonable treatment expectations,19 as well as guilt-inducing somatization, and prolonged and elaborate medical treatments.20
Tobacco Use and BPD. Given that tobacco use is a legitimate healthcare concern in primary care settings, it is important to note that such use may also function as a possible indicator of BPD. Specifically, two empirical studies have found relatively strong correlations between patients with BPD and tobacco use.21,22 This statistical relationship indicates that, compared with the general population, cigarette smokers are more likely to suffer from BPD. This relationship may be explained through the fundamental characteristics of the personality disorder, namely self-regulation difficulties (i.e., repetitive and excessive nicotine exposure with subsequent addiction) and self-destructive behavior (i.e., unconscious risk-taking with regard to the medical morbidities that are associated with cigarette smoking).
The Diagnosis of BPD
DSM-IV-TR. The contemporary diagnostic approach to BPD is described in the DSM-IV-TR.2 Using this approach, five of nine criteria are required for diagnosis. These criteria are: frantic efforts to avoid abandonment; a history of unstable and intense relationships with others; identity disturbance; impulsivity in at least two functional areas such as spending, sex, substance use, eating, or driving; recurrent suicidal threats or behaviors as well as self-mutilation; affective instability with marked reactivity of mood; chronic feelings of emptiness; inappropriate and intense anger or difficulty controlling anger; and transient stress-induced paranoid ideation or severe dissociative symptoms. Unfortunately, most medical clinicians (and many mental health clinicians) have difficulty recollecting all of these criteria. In addition, for patients with predominantly somatic presentations, these criteria are fairly inadequate.
Clinical Quick Screen: Impulsivity and Affect. In an effort to develop a quick, facile, and accurate means of BPD diagnosis in primary care settings, we have adapted and streamlined the criteria described in the Diagnostic Interview for Borderlines.23 This measure for the diagnosis of BPD is a semi-structured interview that consists of 5 core criteria (original measure). Two of the criteria—impulsivity, which includes both self-regulation difficulties and self-destructive behavior, and affect—are known to be relatively stable and reliable clinical features over time in those with BPD.24 Because of this, for clinicians in primary care settings, these two items alone function as extremely specific and reliable screening criteria. Not only are "impulsivity" and "affect" easy criteria to remember, but they also capture the fundamental psychiatric features of the disorder and thereby facilitate the communication of clinical findings when dialoguing patients with mental health clinicians. (On a side note, affect is the observed emotional expression, reactivity, and/or feeling of the patient, whereas mood is the reported state of being; therefore, while affect was the descriptive term used in the original diagnostic interview, mood more accurately captures what is actually being explored.) The specific clinical characteristics subsumed by these two criteria are presented in Table 1.
| Table 1. Clinical Screening Criteria for Borderline Personality Disorder: Impulsivity and Affect |
|
When suspicious clinical findings are evident, the Impulsivity/Affect queries may be framed to the patient as a "screening assessment." The interview is fairly straightforward in that the questions are direct. The patient should be advised at the outset to limit their responses to either "yes" or "no." As for the verbal styling of the interview, the clinician might query, "Have you ever had anorexia or bulimia nervosa? Been obese? Had drug or alcohol problems, or prescription drug problems? Had difficulty regulating money, such as credit-card problems, gambling debts, or bankruptcies? How many sexual partners have you had in your lifetime? (More than 20 is suggestive of BPD.) Any chronic pain syndromes? Any self-mutilation or suicide attempts? Any intimate-partner violence? Any high-risk behaviors that put you in danger? Since the age of 15, what percent of the time have you been in a normal mood?" (Less than 20% normal mood is suggestive of BPD.) Again, the patient must evidence both longstanding self-regulation difficulties and self-destructive behavior as well as chronically dysphoric mood. Because the interview content is so easy to recall and engage, nursing and ancillary staff could readily be trained to screen high-risk patients.
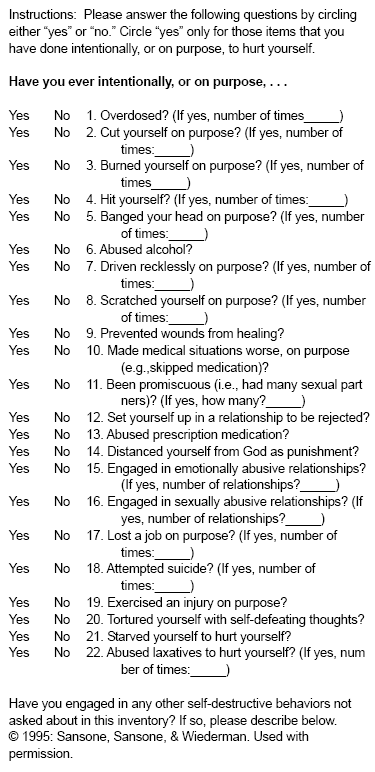
Self-Report Measures. Not surprisingly, there are several available self-report measures for the diagnosis of BPD. Three are particularly clinically promising: the Self-Harm Inventory (SHI)25; the borderline scale of the Personality Diagnostic Questionnaire-4 (PDQ-4)26; and the McLean Screening Inventory for Borderline Personality Disorder (MSI-BPD).27 Each of these measures is one-page in length and easily scored (e.g., for the SHI, the endorsement of 5 or more "yes" responses is highly suggestive of BPD; for the PDQ-4, the endorsement of 5 or more "yes" responses is highly suggestive with the last item being scored if two impulsive behaviors are checked by the respondent). The SHI and the borderline scale of the PDQ-4 are displayed in Tables 2 and 3, respectively, and may be used by clinicians without a fee. As caveats, self-report measures are prone to over-diagnosis and the sensitivity of these measures in detecting BPD in highly somatic primary care patients is unknown.
| Table 2. The Self-Harm Inventory25 |
|
| Table 3. The Borderline Scale of the Personality Diagostic Questionnaire 426* |
|
Borderline Personality Traits. Whatever the elected diagnostic approach, a number of patients may not meet the full criteria for BPD. However, many of these individuals will have traits of the disorder, or even subthreshold symptoms, that briefly intensify with stress. While patients with BPD traits may appear relatively high functioning from a general perspective, the presence of personality disorder features still may culminate in an individual who, under stress, is difficult to manage medically.
Borderline Personality Vs. Bipolar Disorder. BPD and bipolar disorder share a number of symptom domains, particularly impulsivity and mood lability. However, there are distinct differences between these two psychiatric disorders. First, the psychiatric symptoms of BPD are relatively constant albeit fluctuating, whereas the symptoms in bipolar disorder traditionally appear within discrete episodes. Second, the impulsivity in BPD is nihilistic and negative, whereas the impulsivity is bipolar disorder has an expansive and hedonistic flavor. Finally, the mood lability in BPD is characterized by rapid oscillation from normal to intensely dysphoric moods, whereas the mood lability in bipolar disorder is of longer duration and from normal to either distinctly elevated or depressed moods. Despite these clinical differences, the two disorders can be difficult to differentiate from one another, particularly in atypical cases. In addition, both may co-exist within the same individual.
The Etiology of BPD
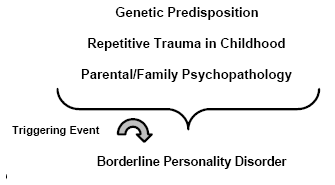
Like many psychiatric disorders, BPD is conceptualized as a multi-determined disorder. In other words, there appear to be a number of risk factors for the disorder, with each cumulatively heightening the probability of syndrome emergence. These factors include genetics28 (i.e., the inheritance of specific temperamental factors,29 not actual personality disorder symptoms), repetitive trauma in early childhood,30,31 parental and/or family psychopathology,32 and possibly a traumatic triggering event.33 (See Figure 2.) Note that while these factors are presented as independent etiological variables, they are likely to be highly inter-related.
| Figure 2. The Multi-Determined Etiology of Borderline Personality Disorder |
|
It must emphasized that in patients with BPD, mental health clinicians frequently encounter histories of childhood trauma, suggesting that this is a very common substrate. The clinically relevant types of childhood trauma appear to be sexual, emotional, and physical abuses as well as the witnessing of violence. (Physical neglect in childhood has not per se been consistently associated with the diagnosis of BPD in adulthood.) Because of the prevalence of these histories of trauma, many patients with BPD have the lingering and persistent symptoms of post-traumatic stress disorder, particularly the clinical features of hypervigilance and hyperarousal. Despite the observed frequency of traumatic childhood histories in patients with BPD, some authors describe non-traumatic pathways to the disorder as well.34
Psychological Themes and Somatic Symptoms
Now that the working definition, epidemiology, diagnosis, and etiology of BPD have been reviewed, the fundamental psychological themes that may culminate in somatic symptoms in patients with BPD will be described.
Self-Destructive Behaviors and Medically Self-Harming Behaviors. As emphasized previously, BPD is invariably associated with longstanding self-harm behavior. Because of training and experience, clinicians typically associate dramatic self-harm behaviors with the diagnosis of BPD, such as self-mutilation and repetitive suicide attempts. However, self-destructive behavior in patients with BPD may also clinically manifest as medically self-harming behavior.
The authors initially confirmed the presence of medically self-harming behaviors in a outpatient sample of family practice patients.35 This study examined a broad range of intentional behaviors that might negatively affect health such as exposing oneself to an infected person on purpose to become sick; creating physical symptoms to attract the attention of a physician or nurse; purposefully misusing prescription medication to worsen an illness; not following instructions given by a physician or nurse in an effort to prolong medical illness; tampering with medical equipment to create false readings; lying about treatment recommendations to one's family to prolong illness; and preventing wounds from healing. Nearly 7% of the 411 participants in this study acknowledged such behaviors. While the findings of this descriptive study confirmed the existence of intentional medically self-harming behaviors among primary care patients, the authors did not know if these behaviors were genuinely associated with the diagnosis of BPD.
A second study examined medically self-harming behaviors and their relationship to BPD in an outpatient sample of internal medicine patients.10 As predicted, medically self-harming behaviors were significantly more prevalent among those patients with the diagnosis of BPD. From these collective data, the authors concluded that: patients with BPD may actively engage in medically self-harming behaviors and patients with the resulting somatic symptoms are likely to present in medical settings.36
Medically self-harming behavior may develop in a number of ways. Some consider one of the most common pathways to be medication noncompliance, with the subsequent resurgence of genuine medical symptoms (e.g., diabetic ketoacidosis due to insulin noncompliance, the exacerbation of asthma symptoms due to noncompliance with medications, recurrent seizures due to anticonvulsant noncompliance). Likewise, some patients may take unnecessary health risks to develop illness, such as intentional and repetitive exposure to contagious individuals (e.g., having unprotected sexual relations with an HIV-positive individual) or smoking cigarettes. Others may augment illness (e.g., intentionally infect their own wounds). All of these behaviors should be viewed as self-injury equivalents (i.e., interpreted as overt self-harm behaviors).
On occasion, some patients may intentionally create or propagate the illusion of illness and may meet the criteria for factitious disorder. Factitious disorder was formerly designated as Munchausen's syndrome and is characterized by the intentional feigning of medical symptoms to maintain the "sick role." It is the authors' opinion that the majority of individuals with factitious syndromes suffer from BPD—an impression that is shared by others.37-40 This includes those patients who engage in Munchausen's syndrome by proxy, in which typically a mother pretends that her child has a serious medical disorder.41
Self-Regulation Difficulties and Medical Symptoms. Self-regulation difficulties are another inherent clinical feature in patients with BPD. In the primary care setting, this psychodynamic may manifest as the inability to effectively regulate pain, substance and/or prescription abuse, and/or obesity.
Chronic Pain Syndromes. Harper42 effectively summarized the borderline patient's intolerance to pain by stating, "it [is] particularly difficult for…[the borderline patient]…to endure prolonged acute pain" "the borderline patient's tolerance of discomfort will typically be of shorter duration than other individuals." In support of Harper's clinical impression, using a semi-structured interview for diagnosis in a primary care sample of chronic pain patients, the authors found that 50% met the diagnostic criteria for BPD.43 BPD features have also been confirmed among chronic pain patients through the use of projective psychological testing.44
The preceding data are additionally but indirectly supported by several studies that confirm the existence of opioid abuse among individuals with BPD. In one study, investigators found that 15% of patients with BPD had histories of opioid abuse or dependence.45 In a Greek study of young adult inpatients with BPD, 5% acknowledged opioid misuse.46 In another study, compared to patients with BPD in remission, those with continuing symptoms reported the sustained use of pain medications.47 Finally, clinicians have described an association between BPD and oral narcotic use among patients with inflammatory bowel disease.48 These data reinforce the clinical observation that some patients with BPD are unable to effectively regulate pain and may subsequently over-utilize pain medications including opioid analgesics.
One study in the literature indicates the prognostic significance of BPD when comorbid with pain syndromes. In this study, investigators found that the presence of BPD reduced subsequent employment likelihood in a group of patients with work-related chronic upper extremity pain.49
Substance Abuse/Prescription Abuse. Several studies deftly illustrate the high rates of comorbidity between BPD and various types of substance abuse. For example, among outpatients and inpatients with BPD, 46-76% evidence drug abuse or dependence.50-52 To complement the preceding findings, psychiatric inpatients with and without BPD were compared. Significantly higher rates of substance abuse treatment were found among the former.53 While illicit substance abuse among patients with BPD is reliably apparent, as a caveat, the authors are not aware of any studies that have directly analyzed the appropriateness or bona fide legitimacy of prescriptions (e.g., narcotic analgesics, high-potency benzodiazepines, controlled psychostimulants) in patients with BPD.
Obesity/Binge Eating Disorder. Obesity is a complex, multi-determined disorder with overlapping genetic, neurohormonal, and cultural underpinnings.54 However, these etiological factors do not exclude the possibility of an underlying psychiatric contribution to obesity as well. BPD would be a prime psychiatric candidate because of the inherent self-regulation difficulties associated with this disorder.
There is ample empirical evidence that a substantial minority of obese individuals suffer from comorbid BPD. Among the seven existing empirical studies in the literature, three samples are composed of gastric surgery candidates and the remaining samples consist of patients from primary care, weight-management, eating disorder, and mental health settings. While the prevalence of BPD in these studies ranges from 2.2% to 94.1%,55 among the 15 measures for BPD (i.e., several studies used more than one measure for BPD), 10 detected BPD at rates of 25% or higher. The highest prevalence rates for BPD were among the obese from the eating disorder and mental health settings (i.e., psychological settings) while the lowest prevalence rates were among individuals seeking weight control in non-psychological settings (i.e., participants from primary care settings). Therefore, the nature of the treatment setting appears to have a strong influence on the prevalence of BPD in a given obese population.56
Binge eating disorder, a tentative DSM psychiatric disorder for further consideration, is characterized by a recurrent pattern of binge eating that occurs at least twice a week for a minimum period of 6 months. Because there is no compensatory behavior (e.g., vomiting, fasting, exercise) to counter episodes of immense calorie ingestion, many patients with this disorder are overweight, although weight status per se is not a diagnostic criterion. In the community, in weight-loss clinics, and among individuals with body mass indices greater than 40, the prevalence of binge eating disorder is 5%, up to 30%, and up to 50%, respectively.57 Among individuals who suffer from this disorder, the eight available empirical studies indicate that the prevalence of BPD ranges from 2% to 30%, with an average of around 12%.58
While self-regulation difficulties are evident in the eating patterns of many obese individuals, overt self-harm behavior—a necessary feature for the diagnosis of BPD—may not be so apparent. However, being overweight in a weight-conscious culture might be viewed as very self-defeating behavior—one that easily invites social ridicule, isolation, and rejection. In addition, the medical consequences of being overweight (e.g., hyperlipidemia, hypertension, diabetes, asthma exacerbation, excessive stress on weight-bearing joints) could function as self-destructive behavior in these individuals as well.
Hypervigilance/Hyperarousal and Somatic Preoccupation. As was emphasized previously, many patients with BPD have histories of childhood trauma. In the aftermath of maltreatment and adversity in childhood, many adult patients have symptoms or features of post-traumatic stress disorder. For this discussion, the most relevant of these are the phenomena of hypervigilance and hyperarousal.
When described in the traditional psychiatric literature, hypervigilance/ hyperarousal are presented in an external context—i.e., in terms of the outside environment. However, these symptoms may also reflect the patient's orientation to their internal environment as well. As a result, patients with BPD tend to be keenly sensitive to and aware of their internal environments, particularly with regard to minute changes in body sensations and/or body rhythms. This excessive scrutiny of the soma by some patients with BPD may account for the clinical phenomenon of somatic preoccupation. For this discussion, somatic preoccupation is defined as the cultivation of and fixation upon somatic symptoms that tend to be innumerable, diffuse, and difficult to diagnostically confirm or verify through either physical examination or laboratory studies.
A relationship between BPD and somatic preoccupation has been clinically described by a number of authors.59-65 In addition, there are limited but supportive empirical findings as well. For example, in one study, the psychological test responses of patients with BPD confirmed a proneness to reporting somatic complaints.66 Among a group of patients with dissociative identity disorder, there was not only a high prevalence of BPD but also 15 reported somatic symptoms per participant.67 Finally, investigators have reported that up to one-third of borderline patients suffer from somatization disorder51,68—a polysomatic psychiatric disorder that entails the endorsement of eight different somatic symptoms that fall into the domains of pain and gastrointestinal, sexual, and pseudoneurological areas.2
In addition to the preceding studies, the relationship between BPD and somatic preoccupation was empirically examined in a sample of 120 internal medicine outpatients.10 As predicted, a statistically significant correlation was found between these two phenomena. Using a different type of statistical approach (i.e., path analysis) among the preceding primary care sample, BPD again was found to be a meaningful contributor to somatic preoccupation.69 These data confirm that among individuals with BPD in primary care settings, a subset demonstrate somatic symptoms that generally may be described as somatic preoccupation. Some of these polysymptomatic patients may even meet the formal criteria for somatization disorder. Somatization disorder was not evaluated in either of the preceding studies.
In our clinical experience in primary care settings, somatic patients with BPD appear to generate an ongoing variety of ill-defined medical symptoms that eventually attract a variety of diagnostic labels. These labels often entail psychophysiological diagnoses such as migraine headaches, irritable bowel syndrome, chronic fatigue syndrome, fibromyalgia, chronic pain syndromes, and multiple chemical sensitivities. Indeed, in a study in which primary care patients were queried about the preceding 6 syndromes, a greater number of diagnostic endorsements related to higher scores on the study measures for BPD.70 Again, the development of these psychophysiological syndromes in patients with BPD is likely to be an outgrowth of these individuals' exquisite sensitivity to their own internal environments—a sensitivity that is likely to be amplified by comorbid mood and anxiety disorders.
Medical Symptomatology and Victimhood. In the majority of cases, it seems that individuals with BPD are genuinely legitimate victims of their damaging early environments. Their life histories seem to be riddled with adversity and maltreatment as well as poor support from caretakers and other family members. As a probable result of their enforced role as a victim in childhood, many unfortunately recapitulate this role in adulthood, which partially may explain their high rates of re-victimization.71
Kroll72 deftly emphasized the crucial importance of the victim theme in the adulthoods of individuals with BPD when he described the victim role as "basic … in understanding borderlines." Kroll underscored how borderline individuals engage others to, "act upon [them], usually in a negative, rejecting, or aggressive way, but sometimes in a caretaking … way." Kroll also emphasized the importance of such patients portraying themselves as helpless and incompetent.
What better way to remain helpless and incompetent (i.e., to be a victim) than to suffer from chronic, unrelenting medical pseudo-illness? However, to sustain this role, the patient is unconsciously obligated to remain medically debilitated. Therefore, the sufferer must maintain a sense of symptom chronicity, which requires the propagation of unresponsive symptoms despite numerous attempts at treatment. This latter feature probably explains the clinical observation of high utilization of primary care resources by patients with BPD, which is supported by a number of studies.73-75 These high utilization patterns tend to manifest as multiple office visits and telephone calls; voluminous medical records; large numbers of medical diagnoses; and excessive medication prescriptions, trials, and failures, including frequent "allergic reactions" to prescribed medications. (See Table 4.)
| Table 4. Potential Indicators of High Utilization of Primary Care Resources Among Patients with BPD |
|
• Multiple visits and telephone calls to the office • Voluminous, bulky medical records • Large numbers of medical diagnoses, perhaps "tentative" and/or psychophysiological in nature (e.g., migraine headaches, irritable bowel syndrome, chronic pain syndromes, fibromyalgia, chronic fatigue, multiple chemical sensitivities, temporal-mandibular joint problems) • Excessive medication prescriptions, trials, and failures, with a high number of unusual side effects to medications |
In terms of medical victimhood, disability is perhaps the ultimate societal affirmation of chronic health impairment. In examining the empirical literature on the relationship between BPD and medical disability, the findings are inconclusive. In one study of 50 consecutive evaluations for disability, 12% of patients were diagnosed with "borderline personality organization."76 As mentioned previously, in a study of the long-term employment outcome of 70 individuals with work-related upper-extremity chronic pain, borderline personality was a predictor for poor return-to-work.49 Among a sample of 45 outpatients in an internal medicine clinic, 72% of the employment-disabled vs. 26% of the nondisabled participants met the criteria for borderline personality symptomatology on one of two self-report study measures.77 In a second study of 94 internal medicine outpatients, no relationship was found between medical disability and BPD.78
The authors suspect that the inconsistent findings with regard to the relationship between BPD and medical disability are related to the fact that in primary care settings, non-BPD patients with warranted disability compensation tend to wash out statistical relationships. As a corollary finding, it is important to note that both studies confirmed the existence of a subset of individuals with BPD who are assigned disability compensation for medical reasons. Unfortunately, the present empirical data do not allow for the determination of the medical legitimacy of these disability claims.
Conclusions
BPD traditionally has been conceptualized by clinicians as a constellation of specific psychiatric symptoms. This article has attempted to illustrate how the psychodynamics of this disorder may generate a host of somatic symptoms. These psychodynamics include self-harm behavior, self-regulation difficulties, and hypervigilance/hyperarousal. The respective somatic syndromes that may emerge in primary care settings are medically self-harming behaviors, a host of medical disorders characterized by dysregulation (e.g., chronic pain syndromes, substance and/or prescription drug abuse, obesity), and somatic preoccupation. Importantly, the preceding somatic syndromes often are encountered in an adult patient who psychologically anchors around medical victimhood. Victimhood, in turn, propagates a multitude of ongoing and unresolved medical symptoms, often of an unverifiable nature, which ultimately drive up healthcare costs. These "difficult patients" generate multiple office visits and telephone calls, voluminous medical records, multiple medical diagnoses, excessive prescriptions for medications with multiple medication trials and failures, and excessive sensitivity to drugs. While the treatment approach to these challenging patients is described in detail elsewhere,32 the initial recognition of the authentic underlying psychiatric disorder in these highly somatic individuals is of crucial importance. Without proper diagnosis, appropriate treatment may be delayed or overlooked—a clinical oversight that may unintentionally reinforce the patient's excessive utilization of healthcare resources as well as expose the individual to unnecessary health risks (e.g., complicated medical procedures such as surgeries). Clearly, the presence of a personality disorder complicates the course of medical treatment.79
References
1. Stern A. Psychoanalytic investigation of therapy in the borderline group of neuroses. Psychoanal Q 1938;7:467-489.
2. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th edition, text revision. Washington, DC; 2000.
3. Stone MH. Borderline personality disorder. In: Michels R, Cavenar JO, eds. Psychiatry, 2nd Edition. Philadelphia: Lippincott;1986:1-15.
4. Ellison JM, Shader RI. Pharmacologic treatment of personality disorders: A dimensional approach. In: Shader RI, ed. Manual of Psychiatric Therapeutics. Philadelphia: Lippincott, Williams, & Wilkins;2003:169-183.
5. Quigley BD. Diagnostic relapse in borderline personality: Risk and protective factors. Diss Abst Int 2005;65:3721B.
6. Widiger TA, Rogers JH. Prevalence and comorbidity of personality disorders. Psychiatr Ann 1989;19:132-136.
7. Sansone RA, Songer DA, Gaither GA. Diagnostic approaches to borderline personality and their relationship to self-harm behavior. Int J Psychiatry Clin Pract 2001;5:273-277.
8. Sansone RA, Rytwinski D, Gaither GA. Borderline personality and psychotropic medication prescription in an outpatient psychiatry clinic. Compr Psychiatry 2003;44:454-458.
9. Gross R, Olfson M, Gameroff M, et al. Borderline personality in primary care. Arch Int Med 2002;162:53-60.
10. Sansone RA, Wiederman MW, Sansone LA. Medically self-harming behavior and its relationship to borderline personality symptoms and somatic preoccupation among internal medicine patients. J Nerv Ment Dis 2000;188:45-47.
11. Paris J. Cultural factors in the emergence of borderline pathology. Psychiatry 1996;59:185-192.
12. Hong SH, Kim Y-H. A validation study of the Borderline Personality Disorder Scale in Korean university students. Korean J Clin Psychol 1998;17:259-271.
13. Senol S, Dereboy C, Yuksel N. Borderline disorder in Turkey: A 2- to 4-year follow-up. Soc Psychiatry Psychiatr Epidemiol 1997;32:109-112.
14. Pinto C, Dhavale HS, Nair S, et al. Borderline personality disorder exists in India. J Nerv Ment Dis 2000;188:386-388.
15. Skodol AE, Bender DS. Why are women diagnosed borderline more than men? Psychiatr Q 2003;74:349-360.
16. Johnson DM, Shea MT, Yen S, et al. Gender differences in borderline personality disorder: Findings from the Collaborative Longitudinal Personality Disorders Study. Compr Psychiatry 2003;44:284-292.
17. Burke JM. Male borderline personality disorder with co-morbid disorders as contrasted to females with co-morbid disorders in a correctional setting. Diss Abstr Int 2005;65:4885B.
18. Young MH, Justice JV, Erdberg P. Risk of harm: Inmates who harm themselves while in prison psychiatric treatment. J Forensic Sci 2006;51:156-162.
19. Himelick AJ, Walsh J. Nursing home residents with borderline personality traits: Clinical social work interventions. J Gerontol Soc Work 2002;37:49-63.
20. Trappler B, Backfield J. Clinical characteristics of older psychiatric inpatients with borderline personality disorder. Psychiatr Q 2001;72:29-40.
21. Kolliakou A, Joseph S. Further evidence that tobacco smoking correlates with schizotypal and borderline personality traits. Pers Individ Dif 2000;29:191-194.
22. Williams JH, Wellman NA, Allan LM, et al. Tobacco smoking correlates with schizotypal and borderline personality traits. Pers Individ Dif 1996;20:267-270.
23. Kolb JE, Gunderson JG. Diagnosing borderline patients with a semi-structured interview. Arch Gen Psychiatry 1980;37:37-41.
24. McGlashan TH, Grilo CM, Sanislow CA, et al. Two-year prevalence and stability of individual DSM-IV criteria for schizotypal, borderline, avoidant, and obsessive-compulsive personality disorders: Toward a hybrid model of axis II disorders. Am J Psychiatry 2005;162:883-889.
25. Sansone RA, Wiederman MW, Sansone, LA. The Self-Harm Inventory (SHI): Development of a scale for identifying self-destructive behaviors and borderline personality disorder. J Clin Psychol 1998;54:973-983.
26. Hyler SE. Personality Diagnostic Questionniare-4. New York; 1994.
27. Zanarini MC, Vujanovic AA, Parachini EA, et al. A screening measure for BPD: The McLean Screening Instrument for Borderline Personality Disorder (MSI-BPD). J Personal Disord 2003;17:568-573.
28. Skodol AE, Siever LJ, Livesley WJ, et al. The borderline diagnosis II: Biology, genetics, and clinical course. Biol Psychiatry 2002;51:951-963.
29. Goodman M, New A, Siever L. Trauma, genes, and the neurobiology of personality disorders. In: Yehuda R, McEwen B, eds. Biobehavioral Stress Response: Protective and Damaging Effects. New York: New York Academy of Sciences; 2004:104-116.
30. Sansone RA, Sansone LA. Borderline personality disorder: The enigma. Primary Care Rep 2000;6:219-226.
31. Zanarini MC, Dubo ED, Lewis RE, et al. Childhood factors associated with the development of borderline personality disorder. In: Zanarini MC, ed. Role of Sexual Abuse in the Etiology of Borderline Personality Disorder. Washington, DC: American Psychiatric Press;1997:29-44.
32. Sansone RA, Sansone LA. Borderline Personality in the Medical Setting: Unmasking and Managing the Difficult Patient. Nova Publishers, Hauppauge, NY; 2007.
33. Zanarini MC, Frankenburg FR. Pathways to the development of borderline personality disorder. J Personal Disord 1997;11:93-104.
34. Graybar SR, Boutilier LR. Nontraumatic pathways to borderline personality disorder. Psychother Theory Res Pract Train 2002;39:152-162.
35. Sansone RA, Wiederman MW, Sansone LA, et al. Sabotaging one's own medical care. Arch Fam Med 1997;6:583-586.
36. Sansone RA, Sansone LA. Borderline personality: Different symptoms in different treatment settings? Int J Psychiatry Clin Pract 2003;7:187-191.
37. Ehlers W, Plassman R. Diagnosis of narcissistic self-esteem regulation in patients with factitious illness (Munchausen syndrome). Psychother Psychosom 1994;62:69-77.
38. Goldstein AB. Identification and classification of factitious disorders: An analysis of cases reported during a ten year period. Int J Psychiatry Med 1998;28:221-241.
39. Sutherland AG, Rodin GM. Factitious disorders in a general hospital setting: Clinical features and a review of the literature. Psychosomatics 1990;31:392-399.
40. Rothenhausler H-B, Kapfhammer H-P. Discussion of the connection between factitious disorder and personality disorder. Personlichkeitsstorungen Theorie und Therapie 2005;9:99-105.
41. Bouden A, Krebs MO, Loo H, et al. Munchausen syndrome by proxy: A challenge for medicine. Presse Med 1996;25:567-569.
42. Harper RG. Borderline personality. In: Harper RG, ed. Personality-Guided Therapy in Behavioral Medicine. Washington, DC: American Psychological Association;2004:179-205.
43. Sansone RA, Whitecar P, Meier BP, et al. The prevalence of borderline personality among primary care patients with chronic pain. Gen Hosp Psychiatry 2001;23:193-197.
44. Merceron C, Rossel F, Matthey M-L. Chronic complaint of pain and its psychological approach in projective techniques. Psychol Med 1990;22: 681-686.
45. Dulit RA, Fyer MR, Haas GL, et al. Substance use in borderline personality disorder. Am J Psychiatry 1990;147:1002-1007.
46. Hatzitaskos P, Soldatos CR, Kokkevi A, et al. Substance abuse patterns and their association with psychopathology and type of hostility in male patients with borderline and antisocial personality disorder. Compr Psychiatry 1999;40:278-282.
47. Frankenburg FR, Zanarini MC. The association between borderline personality disorder and chronic medical illnesses, poor health-related lifestyle choices, and costly forms of health care utilization. J Clin Psychiatry 2004;65:1660-1665.
48. Kaplan MA, Korelitz BI. Narcotic dependence in inflammatory bowel disease. J Clin Gastroenterol 1988;10:275-278.
49. Burton K, Polatin PB, Gatchel RJ. Psychosocial factors and the rehabilitation of patients with chronic work-related upper extremity disorders. J Occup Rehabil 1997;7:139-153.
50. McGlashan TH, Grilo CM, Skodol AE, et al. The Collaborative Longitudinal Personality Disorders Study: Baseline Axis I/II and II/II diagnostic co-occurrence. Acta Psychiatr Scand 2000;102:256-264.
51. Prasad RB, Val ER, Lahmeyer HW, et al. Associated diagnoses (comorbidity) in patients with borderline personality disorder. Psychiatr J Univ Ott 1990;15:22-27.
52. Zanarini MC, Frankenburg FR, Dubo ED, et al. Axis I comorbidity of borderline personality disorder. Am J Psychiatry 1998;155:1733-1739.
53. Sansone RA, Songer DA, Miller KA. Childhood abuse, mental healthcare utilization, self-harm behavior, and multiple psychiatric diagnoses among inpatients with and without a borderline diagnosis. Compr Psychiatry 2005;46:117-120.
54. Sansone RA, Sansone LA. Obesity and borderline personality: An integrated research perspective. In: Swain PI, ed. Focus on Eating Disorders Research. Hauppauge, New York: Nova Publishers;2003:195-208.
55. Sansone RA, Wiederman MW, Sansone LA. The prevalence of borderline personality disorder among individuals with obesity: A critical review of the literature. Eat Behav 2000;1:93-104.
56. Sansone RA, Sansone LA, Morris DW. Prevalence of borderline personality symptoms in two groups of obese subjects. Am J Psychiatry 1996;153:117-118.
57. Sansone RA, Sansone LA. The eating disorders. In: Klykylo WM, Kay J, eds. Clinical Child Psychiatry, 2nd edition. London: John Wiley;2005:311-326.
58. Sansone RA, Levitt JL, Sansone LA. The prevalence of personality disorders in those with eating disorders. In: Sansone RA, Levitt JL, eds. Personality Disorders and Eating Disorders: Exploring the Frontier. New York: Routledge;2006:23-29.
59. Schreter RK. Treating the untreatables: A group experience with somaticizing borderline patients. Int J Psychiatry Med 1980;10:205-215.
60. Giovacchini PL. The regressed patient and the psychosomatic focus. In: Boyer LB, Giovacchini PL, eds. Master Clinicians on Treating the Regressed Patient. Northvale, NJ:Aronson;1993:85-106.
61. Giovacchini PL. Treatment issues with borderline patients and the psychosomatic focus. Am J Psychother 1993;47:228-244.
62. Bernstein AE. The mind body interface revisited. Psychother Patient 1988;4:45-56.
63. Hull JW, Okie J, Gibbons B, et al. Acting up and physical illness: temporal patterns and emerging structure. J Am Psychoanal Assoc 1992;40:1161-1183.
64. Janssen PL. Scenarios of borderline disturbances. Prax Psychother Psychosom 1990;35:1-12.
65. Spitzer C, Barnow S. Somatization as a unique dimension in personality disorders. Personlichkeitsstorungen Theorie und Therapie 2005;9:106-115.
66. Lloyd C, Overall JE, Kimsey LR, et al. A comparison of the MMPI-168 profiles of borderline and nonborderline outpatients. J Nerv Ment Dis 1983;171:207-215.
67. Ross CA, Miller SD, Reagor P, et al. Structured interview data on 102 cases of multiple personality disorder from four centers. Am J Psychiatry 1990;147:596-601.
68. Hudziak JJ, Boffeli TJ, Kriesman JJ, et al. Clinical study of the relation of borderline personality disorder to Briquet's syndrome (hysteria), somatization disorder, antisocial personality disorder, and substance abuse disorders. Am J Psychiatry 1996;153:1598-1606.
69. Sansone RA, Wiederman MW, Sansone LA. Adult somatic preoccupation and its relationship to childhood trauma. Violence Vict 2001;16:39-48.
70. Sansone RA, Pole M, Dakroub H, et al. Childhood trauma, borderline personality symptomatology, and psychophysiological and pain disorders in adulthood. Psychosomatics 2006;47:158-162.
71. Zanarini MC, Frankenburg FR, Reich DB, et al. Violence in the lives of adult borderline patients. J Nerv Ment Dis 1999;187:65-71.
72. Kroll J. The Challenge of the Borderline Patient: Competency in Diagnosis and Treatment. New York: W. W. Norton & Co;1988.
73. Sansone RA, Sansone LA, Wiederman MW. Borderline personality disorder and health care utilization in a primary care setting. South Med J 1996;89:1162-1165.
74. Sansone RA, Wiederman MW, Sansone LA. Health care utilization and history of trauma among women in a primary care setting. Violence Vict 1997;12:165-172.
75. Sansone RA, Wiederman MW, Sansone LA. Borderline personality symptomatology, experience of multiple types of trauma, and health care utilization among women in a primary care setting. J Clin Psychiatry 1998;59:108-111.
76. Mikkelsen EJ. The psychology of disability. Psychiatr Ann 1977;7:90-99.
77. Sansone RA, Hruschka J, Vasudevan A, et al. Disability and borderline personality symptoms. Psychosomatics 2003;44:442.
78. Sansone RA, Butler M, Dakroub H, et al. Borderline personality symptomatology and employment disability among outpatients in an internal medicine clinic. Prim Care Companion 2006;8:153-157.
79. Zanarini MC, Frankenburg R. Personality disorders and medical comorbidity. Curr Opin Psychiatry 2006;19:428-431.
Clinicians are typically introduced to the academic phenomenon of borderline personality disorder (BPD) during their psychiatric rotations in medical school.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.