Orthopedic Pearls and Pitfalls
Orthopedic Pearls and Pitfalls
Authors: Carl R. Menckhoff, MD, FACEP, FAAEM, Associate Professor, Department of Emergency Medicine, Medical College of Georgia, Augusta; and Cherie Welter, MD, Resident Physician, Department of Emergency Medicine, Medical College of Georgia, Augusta.
Peer Reviewers: David J. Robinson, MD, MS, FACEP, Associate Professor and Interim Chairman, Department of Emergency Medicine, University of Texas Health Science Center at Houston; and Carl A. Germann, MD, Attending Physician, Maine Medical Center, Portland.
Introduction
Orthopedic injuries are frequently encountered in the emergency department. It is important to recognize and correctly treat these injuries to minimize any damage and optimize outcome. According to two studies,1,2 17-51% of negligence claims involved missed fractures. This article will discuss 10 orthopedic problems that have a higher potential to be missed, and how to correctly identify and manage them.
Flexor Digitorum Superficialis and Profundus Injuries
A 45-year-old female presents to the emergency department after cutting her finger with a knife while preparing dinner. The examination reveals that she has a 1 cm laceration over the volar aspect of the third proximal phalanx of her left hand. Sensation and circulation are intact. When asked to make a fist, she is able to do so without difficulty.
Epidemiology. Flexor tendon injuries to the hand are not as common as extensor injuries. Due to a double flexor mechanism, however, they are frequently more subtle than injuries to the single extensor apparatus.
Patterns of Injury. Injuries can involve the flexor digitorum superficialis (FDS), flexor digitorum profundus (FDP), or both depending on the location. Laceration is the most common mechanism of injury, although avulsion of the FDP is well documented in athletes and often referred to as a rugby jersey injury. The classic mechanism for the rugby jersey injury is when a player grabs the jersey of another player causing extension forces on the forcibly flexed finger, avulsing the FDP from its insertion on the distal phalanx.
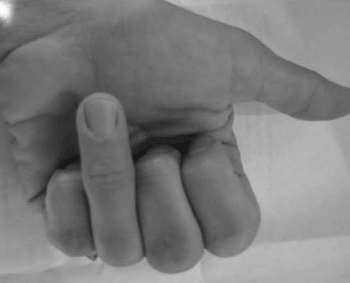
Evaluation. The history of this injury will reveal either a laceration or forced extension of the finger. On inspection, an injury to the FDP will usually preclude the patient from making a complete fist (see Figure 1), while an FDS injury will often seem grossly normal. After a sensory and vascular examination, the digits should, therefore, be examined individually to assure normal function of both the deep and superficial flexor tendons.
| Figure 1. FDP Rupture |
|
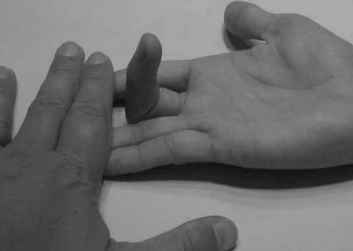
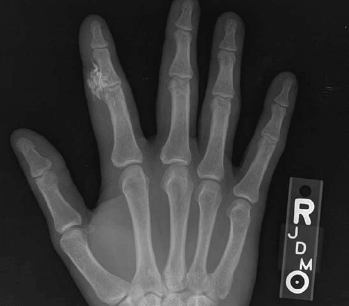
The FDS originates in the forearm where the muscle splits into four, allowing for independent movement of the four FDS tendons. The FDP is also in the forearm, but the ulnar three digits share a common muscle belly, thus inhibiting independent use of their FDP tendons. The index finger is partially separate, allowing for some independent movement. The tendon of the FDP initially lies deep to the FDS at the metacarpophalangeal joint (MCPJ). As the FDS splits to insert on the middle phalanx, the FDP then comes through it to insert on the distal phalanx. Because of these anatomic features, independent flexion of a finger while the others are held in extension (thereby taking the FDP out of play), requires intact FDS function. (See Figure 2.) To examine the FDP, one can simply hold the proximal interphalangeal joint (PIPJ) of the digit in extension and test for the ability to flex the distal interphalangeal joint (DIPJ). (See Figure 3.)
| Figure 2. FDS Test |
|
| Figure 3. FDP Test |
|
Imaging. In the case of lacerations, radiographs will usually be normal, although they may be obtained if there is a concern for fracture or foreign body retention. In the case of FDP avulsion, an x-ray may show an avulsion fracture of the proximal volar distal phalanx and presence of a fracture fragment retracted proximally along the finger.
Management. All FDS or FDP lacerations should be considered for operative repair, ideally done within 24 hours.3 However, if no hand surgeon is readily available, primary wound repair can be performed with splinting of the MCP joint at 70 degrees and the IP joints at 10-15 degrees of flexion, and referral to a hand surgeon for delayed closure within 2 weeks.4
In the case of an FDP rupture, patients can be placed in a splint with prompt referral to a hand surgeon.5 Repair should be within a week because if it is delayed the tendon can retract into the palm and repair becomes much more difficult.
Key Points. The key for emergency physicians is to identify that these injuries are present. Careful examination of the integrity of the FDS and FDP is critical as if the injury is missed, or repair delayed, outcome may be severely compromised.
High Pressure Injection Injuries
A 34-year-old crane operator presents to the emergency department after a hydraulic line sprang a leak. He states that he is fine except for a 1 mm wound to his finger and that he would not have come in except that his supervisor told him he had to before he could return to work. On examination, he is asymptomatic with minimal tenderness at the wound site. (See Figure 4.)
| Figure 4. High-Pressure Injection Injury (Wound) |
|
Epidemiology. While high-pressure injection injuries to the hand are uncommon, the associated morbidity is severe, with amputation rates of 30-80%.6-8
Patterns of Injury. Almost all of these injuries occur from use of industrial equipment where high-pressure lines and injectors are used as conduits for materials such as water, grease, hydraulic fluid, paint, oil, and more. If possible, it is important to determine the pressure involved since greater than 7000 psi has been associated with almost 100% amputation rates, whereas less than 7000 psi is non-prognostic. The type of material injected also plays a role. For example grease tends to cause more fibrosis, whereas paint causes an immediate tissue necrosis if the tissues are not completely debrided. Other factors that worsen prognosis are delayed debridement and injection into the digit (rather than into the palm).9
Evaluation. The key to successful diagnosis of these injuries is the realization that they may appear innocuous, and the patient may seem asymptomatic. Injection sites are often very small, and the patient may have little or no swelling of the digit. A good neurovascular examination with two-point discrimination on each side of the finger should be performed and well documented. Normal two-point discrimination is < 5 mm, borderline in 6-10 mm, and values > 11 mm are abnormal.
Imaging. Plain radiographs may be helpful and show subcutaneous air or the spread of injected material. (See Figure 5.) Many materials are not radiopaque, however, and a normal radiograph does not exclude the necessity for debridement.
| Figure 5. High-Pressure Injection Injury (X-ray with Injected Material) |
|
Management. Management of these patients in the ED consists of pain control, tetanus prophylaxis, antibiotics to cover skin flora, and urgent hand consultation for surgical debridement. Digital blocks are contraindicated due to the risk of increasing pressure in an already compromised digit and have been associated with worsened outcomes.3
Key Points. Always consider this diagnosis in industrial workers who present with small wounds to their hands. If the history is elicited that the injury was from a high pressure line, obtain as much information about the pressures and materials involved, treat the patient as above, and consult a hand specialist emergently.
Achilles Tendon Rupture
A 40-year-old male presents to the ED complaining of ankle pain. He states he was playing softball (today was the first day of the spring beer league) and when he took off to run to first base, he felt like somebody kicked him and now he has trouble walking.
Epidemiology. Achilles tendon injuries appear to be on the rise with the median age of rupture being 35 years and the primary victims being white-collar men who participate in intermittent athletics.10,11 The reason for this rise is unclear, although it is thought to be due to an increase in middle-aged people participating in athletics. This injury is important to consider because historically 25% of Achilles tendon ruptures are missed on initial presentation.12
Patterns of Injury. The most common mechanism of injury is a sudden, forceful plantar flexion that can occur with jumping or sudden acceleration, for example. Ruptures also can occur from direct trauma. Other factors that predispose to tendon rupture are gout, lupus, rheumatoid arthritis, chronic renal failure, and steroid or fluoroquinolone use. The most common site of rupture is 2-6 cm above the calcaneus,11 which corresponds to the area of the tendon with the least blood supply.
Evaluation. The classic history is that of a sudden acceleration followed by a sudden pain or "pop," although painless ruptures do occur. The patient will usually complain of difficulty walking and difficulty pressing down with the foot.
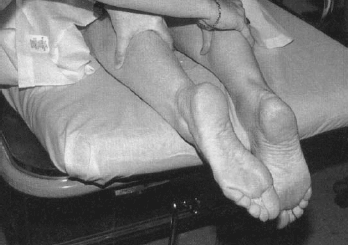
On examination, a palpable defect may be felt above the calcaneus, but the cornerstone for evaluation of this injury is the Thompson test. This is performed with the patient prone and feet hanging over the end of the exam table (alternatively the knees can be flexed to 90 degrees). The calf is then squeezed and the foot observed for plantar flexion. If the Achilles tendon is intact (at least partially) then plantar flexion of the foot should be seen. If there is complete rupture of the tendon, there will be no flexion. (See Figure 6.) It should be noted that the ability to actively plantar flex is not a good test due to multiple other contributors to plantar flexion of the foot (i.e., flexor digitorum longus, flexor hallucis longus, peroneus longus and brevis, and the tibialis posterior).
| Figure 6. Thompson Test (Right Leg Is Abnormal) |
|
Imaging. Radiographs of the ankle are usually not necessary (unless ankle injury is suspected), although if obtained they may show opacification of Kager's triangle, a fatty radiolucent space anterior to the Achilles tendon. If clinically indicated, MRI or ultrasound can be used to demonstrate partial or complete tendon ruptures.
Management. Emergency department management of the Achilles tendon rupture consists of a posterior splint in the gravity equinus position (toes down), non-weight bearing, pain control, and referral to an orthopedist within 2 days. The decision of surgical versus non-surgical treatment is still controversial and, at this point, should be deferred to the orthopedist.
Key Points. Suspect Achilles tendon rupture in anyone with a history of sudden acceleration or pain around the ankle or calf and perform a Thompson test.
Calcaneus Fracture
A 16-year-old cheerleader fell from the top of a three-level pyramid during practice and landed on her feet. She is now complaining of pain in her foot and the inability to bear weight.
Epidemiology. The calcaneus is the largest and most frequently fractured tarsal bone, comprising approximately 60% of all foot fractures.13-15 Eighty to ninety percent of patients with this injury are in their prime working years, which is important as 20% of people may be incapacitated for up to 3 years.13,14
Patterns of Injury. The classic mechanism of injury involves a high-energy axial loading onto the calcaneus, as in a fall or jump from height, or a motor vehicle collision. Because calcaneus fractures are usually high-force injuries, a high index of suspicion must be maintained for other injuries. Approximately 7% will have a contralateral calcaneus fracture, 10% will have an injury to the vertebral column, and 25% will have other lower extremity fractures.14
Evaluation. The patient will usually give a history consistent with transmission of high-energy forces into the foot. On examination, the patient will feel tenderness to palpation over the heel and almost always will be unable to bear weight on the posterior part of the foot. Plantar ecchymosis, if present, is also highly suggestive of a calcaneal fracture. Due to the high incidence of concomitant injuries, a thorough physical examination should be done, paying special attention to the lower extremities and spine.
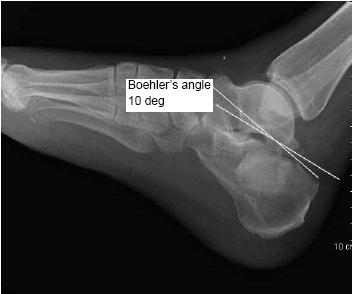
Imaging. AP, lateral (see Figure 7) and Harris axial (see Figure 8) radiographs should be obtained. The AP view shows the anterosuperior calcaneus and the calcaneocuboid joint. The lateral gives the best view of the calcaneal body and posterior facet. The axial view demonstrates the calcaneal tuberosity and the sustentaculo-talar and subtalar joints. Because of the many articular surfaces involved, fracture lines may not be seen on plain films, so it is important to look for other signs of fracture. Boehler's angle (see Figure 7) is measured by the intersection of 2 lines: one drawn from the posterior tuberosity through the apex of the posterior facet, and the other drawn from the apex of the anterior process through the apex of the posterior facet. The normal angle is 20-40 degrees and, if less than 20 degrees, suggests a compression fracture.16
| Figure 7. Calcaneus Fracture and Boehler's Angle |
|
| Figure 8. Harris Axial View |
|
If further delineation of a fracture is needed, or if a high clinical suspicion exists in the face of negative plain films, then CT is the study of choice. MRI can also be used in selected cases.
Management. Once a fracture is confirmed by imaging, treatment depends on whether it is intra-articular or extra-articular. Intra-articular fractures account for 75%, are associated with higher morbidity, and are usually operative. As such, these injuries require orthopedic consultation while the patient is in the ED. Extra-articular fractures can usually be treated conservatively with padding, compressive dressings, posterior splinting, and follow-up with an orthopedist. They may then be treated with casting for 6-8 weeks. The exception to this is the displaced extra-articular fracture, which often will require surgical reduction, and therefore should be evaluated by the orthopedist while the patient is in the ED. Most operative reductions take place after a few days to allow for the swelling to decrease.
The amount of soft-tissue damage that is involved in these injuries should not be underestimated and good instructions need to be given to the patient to watch for skin breakdown, infection, and signs of compartment syndrome.
Key Points. Consider calcaneus fractures with an axial load mechanism of injury, measure Boehler's angle when fracture lines are not obvious, and remember to look for concomitant injuries.
Knee Dislocation
A 19-year-old male is brought into the emergency department after sustaining a hyperextension injury to his right knee during a football game. He experienced immediate severe pain. There is no obvious knee deformity or swelling.
Epidemiology. Tibial femoral knee dislocation is a serious injury that requires prompt evaluation and initial management to prevent potential limb-threatening complications. It is uncommon, accounting for less than 0.2% of all orthopedic injuries.17,18 The true incidence is likely higher, as up to 50% of knee dislocations spontaneously reduce or are reduced in the field by emergency personnel.19,20 More than half of the cases are the result of high-energy trauma such as motor vehicle crashes (MVC), one-third are from sports injuries, and the remainder are from falls and industrial injuries.17,19-21 Most occur in young men in their teens and 20s.17,20
Patterns of Injury. Anterior dislocation (tibial plateau forced anterior to the femoral condyles) is the most common type of knee dislocation and is caused by hyperextension of the knee. This is followed by posterior dislocation (tibial plateau forced posterior to the femoral condyles), which is the result of high-velocity direct trauma to the flexed knee such as the dashboard-type injury. The remaining dislocations are lateral, medial, or rotary dislocations caused by valgus, varus, or rotational forces.17-21
Extensive ligamentous disruption is always present with knee dislocation, most commonly involving both the anterior cruciate ligament and posterior cruciate ligament. Keep in mind the mechanism of injury and have a high index of suspicion for dislocation in a grossly unstable knee that is reduced on presentation.17,18,21
Popliteal artery injury ranges from 10% to 32%, and has been reported to be as high as 40% in high-velocity injuries. Up to half of these patients will require limb amputation.17,21 Length of time to revascularization is directly related to amputation rate, and a rate of 86% has been reported after a delay of 6-8 hours.18
The common peroneal nerve is injured in 20% of cases, and is associated more often with posterolateral dislocations. As with any type of dislocation, examine neurologic status before and after any manipulation. This, however, can be challenging in the multiply injured major trauma patient.17,18,20
Evaluation. Begin with a brief history of the mechanism of injury and a focused physical examination of the patient. Perform a complete trauma evaluation on patients with high-velocity mechanisms. The patient will usually be in a great deal of pain. There may be an obvious knee deformity or the knee may look normal if it has reduced prior to arrival. Swelling may or may not be present. Assess the vascular status of the extremity by evaluating dorsalis pedis and posterior tibial pulses and comparing them with the uninjured extremity. Altered sensation on the top of the foot or inability to dorsiflex and evert the foot indicates a peroneal nerve injury.
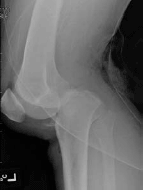
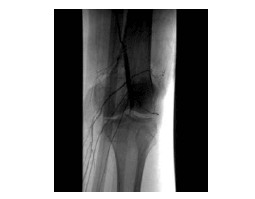
Imaging. Obtain plain anteroposterior and lateral (see Figure 9) radiographs in all cases of known or suspected knee dislocation to classify the direction of dislocation, identify associated fractures and avulsions, and confirm reduction. Do not, however, delay reduction of an ischemic limb to obtain films. The use of routine angiography (see Figure 10) has been debated. Some believe it is indicated in all instances regardless of vascular status, as the incidence of arterial injury is the same in patients who present dislocated and those who are reduced on arrival. While some evidence suggests that it is not required in all cases, it is still indicated in all patients with ischemia, pulse deficit, ankle-brachial index (ABI) of less than 0.9 or any other signs of impaired circulation.17,18,20,21 The ankle-brachial index is the ratio of systolic blood pressure in the foot to the systolic blood pressure in the arm. The highest systolic pressure in the arm is used (both arms are measured in the conventional way). A cuff is applied to the calf and a Doppler is used over the dorsal pedis and posterior tibial artery to obtain the highest systolic pressure. The ratio is then calculated. Computed tomography angiography is an alternative imaging modality used at some institutions in place of traditional angiography.
| Figure 9. Posterior Knee Dislocation |
|
| Figure 10. Angiogram Demonstrating Disruption of the Popliteal Artery |
|
Management. Consult vascular surgery and orthopedics immediately for hard signs of vascular injury (distal ischemia as evidenced by diminished or absent pulses, or a color/temperature change, active hemorrhage, expanding/pulsatile hematoma), irreducible or open dislocations, abnormal ABI (< 0.9), or abnormal duplex Doppler studies. Reduce the dislocated knee with obvious distal limb ischemia immediately through gentle traction-countertraction under conscious sedation. Repeat the neurovascular examination, stabilize the limb in a long leg splint, and obtain post-reduction radiographs and a formal angiogram. Consult vascular surgery as urgent revascularization may be required.17,18,20,21 Patients with no evidence for vascular injury and a normal ABI should be admitted for observation and frequent serial examinations to monitor the neurovascular function of the injured limb.
Key Points. Maintain a high index of suspicion for knee dislocation in high-energy trauma and in patients with extensive bruising, hemarthrosis, or joint instability. Arterial injury can be present despite normal arterial pulses or Doppler signals, so consider angiography for most suspected or known knee dislocations. Prompt recognition and treatment are critical for limb salvage. Emergent surgery is indicated for open dislocations, vascular injury, compartment syndrome, and irreducible dislocations. Outcome is directly related to length of ischemia.
Lunate and Perilunate Injuries
A 25-year-old man presents to the ED with a complaint of right wrist pain. He was climbing down a ladder and slipped on the third step, falling on his outstretched hand. The wrist is swollen but without gross deformity.
Epidemiology. Carpal fracture/dislocations are uncommon injuries but carry significant morbidity if not recognized early and treated appropriately.22,23 Wrist injuries account for 2.5% of all ED visits and lunate and perilunate injuries make up an estimated 10% of all carpal injuries.23 The incidence of lunate fracture (0.5-6.5%) is rare in comparison to the incidence of scaphoid fracture (70-90%).22 Most carpal injuries occur in young men in high-energy accidents.24
Patterns of Injury. Motor vehicle and motorcycle crashes, falls from heights, and sports injuries are common causes of carpal injuries. The mechanism of injury is a fall on the outstretched hand causing hyperextension and ulnar deviation of the wrist.22,24,25
Carpal dislocations are a continuum of progressive ligamentous injuries caused by various degrees of wrist dorsiflexion, ulnar deviation, and forearm supination. Usually, there are carpal instabilities as well as associated fractures within this continuum of injuries. Distinct stages of injury are described, beginning with scapholunate joint disruption and progressing to sequential injury around the lunate. Normally, the capitate, lunate, and radius line up in a row (best seen on a lateral wrist radiograph). In perilunate dislocations, the capitate is dorsally dislocated, and in lunate dislocations the lunate rotates in a volar direction.23-25
Median nerve injuries may occur immediately as a result of either contusion to the nerve by a direct blow or increased carpal tunnel pressure from hemorrhage. Delayed median nerve symptoms are caused by soft-tissue swelling and formation of a hematoma.23-25
Evaluation. Lunate and perilunate injuries often are subtle and difficult to appreciate clinically or radiographically. A multicenter review showed that these diagnoses were initially missed in 25% of patients.22,24 So, be systematic in evaluating wrist injuries and only use wrist sprain as a diagnosis of exclusion.
Patients will usually have a history of a fall on an outstretched hand. They complain of pain and swelling on the volar aspect or dorsum of the wrist and limited movement. There is often tenderness over the dorsum of the wrist and a deformity may be observed, but it may be mild. Diminished two-point sensation in a median nerve distribution may be present indicating acute carpal tunnel syndrome.23-25 Evaluate with plain radiographs as described below.
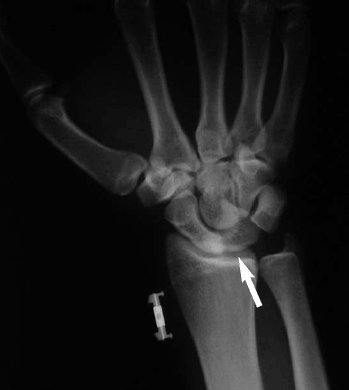
Imaging. Obtain posterior-anterior (PA) and lateral plain radiographs of the wrist. On PA view, the spaces between the carpal bones should be equal (1-2 mm).25 An asymmetric or increased intercarpal space suggests ligamentous disruption. A scapholunate space > 3 mm is known as a "Terry Thomas" sign (after the British comedian with a gap between his teeth) and indicates a scapholunate ligamentous injury.
Identify three arcs representing the articular surfaces of proximal and distal carpal rows. They should be smooth and continuous. Disruption of the radiocarpal arc is suggestive of lunate dislocation, while disruption of the midcarpal arc suggests a perilunate dislocation.23 The lunate is normally quadrangular in shape on PA view. A lunate dislocation results in a triangular appearance known as the "piece of pie" sign.23,25 (See Figure 11.)
| Figure 11. AP X-ray Showing a Lunate Dislocation with "Piece of Pie" Appearance of the Lunate |
|
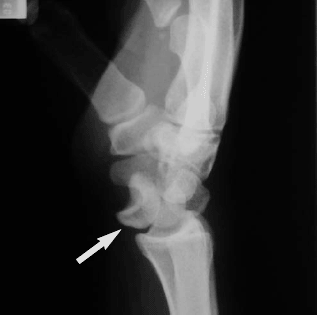
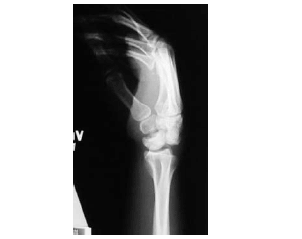
On the lateral view, the capitate, lunate, and radius normally line up in a row, with the capitate resting in the cup of the moon-shaped lunate, and the lunate resting in the cup of the radius. Loss of this linear relationship indicates a lunate or perilunate dislocation. In a lunate dislocation, the lunate is rotated volarly and looks like a cup tipped forward spilling into the palm. This is called the "spilled teacup" sign. (See Figure 12.) In a perilunate dislocation, the capitate lies dorsally to the lunate, and sometimes can move proximally and contact the radius.23-25 (See Figure 13.)
| Figure 12. Lateral X-ray Showing a Lunate Dislocation and "Spilled Teacup" Sign |
|
| Figure 13. Lateral X-ray Showing a Perilunate Dislocation |
|
Management. Consult an orthopedist while the patient is in the ED for all carpal dislocations. Closed reduction should be performed as soon as possible, but is often not successful, especially with lunate dislocations where the ligamentous disruption is often greater. If successful, apply a long-arm splint. Open reduction is required if the dislocation is irreducible or unstable, or if the fracture/dislocation is open. Optimal outcomes are achieved with open reduction and internal fixation with ligament repair, and it is universally recommended for carpal dislocation injuries.23-25 Complications include chronic pain, weakness, limitation of motion, and carpal tunnel syndrome.22-25
Key Points. Carefully evaluate wrist injuries for evidence of carpal instability. Lunate dislocations appear as a "piece-of-pie" on PA and a "spilled teacup" on lateral radiographs. In perilunate dislocations, the capitate lies dorsally on lateral radiographs. If the scapholunate distance is ≥ 3 mm, a ligamentous injury exists. Consult a hand surgeon for management of patients with carpal instability. A delayed or missed diagnosis results in a high incidence of poor outcomes.
Galeazzi and Monteggia Fracture-Dislocation
Case 1. A 32-year-old male presents to the ED after tripping and falling on some lumber at his job site. He complains of left arm pain and holds his flexed arm to his chest, unwilling to move it. There is significant swelling at the elbow.
Case 2. A 27-year-old male sustains a right upper extremity injury after being struck in the forearm by a pool-cue in an altercation. He complains of a painful arm and wrist with limited wrist range of motion. There is significant swelling of the forearm and wrist.
Epidemiology. Upper extremity fractures make up almost half of all fractures in the United States.26
In forearm fractures, elbow or wrist dislocation may accompany the fracture leading to long-term complications if not diagnosed. The Monteggia fracture consists of a fracture to the ulna with dislocation of the proximal radial head. The Galeazzi fracture consists of a radius fracture with dislocation at the distal radio-ulnar joint. These injuries each make up about 3% to 7% of forearm fractures.26,27
Patterns of Injury. The mechanism of injury for both fracture patterns is forced pronation of the forearm during a fall on the outstretched hand. In addition, Monteggia fracture can also be the result of a direct blow to the posterior aspect of the ulna, while Galeazzi fracture can also occur by a direct blow to the dorsoradial aspect of the wrist.26,27 Both can be the result of low-energy mechanisms, such as ground level falls, or high-energy trauma such as motor vehicle crashes or falls from heights.26 The posterior interosseous nerve (a deep branch of the radial nerve) is injured in 17% of Monteggia fractures27 as it lies in close proximity to the neck of the radius and is often stretched when the radial head is dislocated.26,28
Evaluation. Occult dislocations at the elbow and wrist associated with forearm fractures are missed in up to 50% of cases.26,27 Unrecognized and not treated appropriately, these injuries have a high rate of chronic pain and long-term functional limitations.
The clinician should start by obtaining an accurate history of the mechanism of injury. Assess the joints above and below the injury. Clinically, the patient with a Monteggia fracture will have pain and tenderness at the fracture site with severely limited range of motion of the elbow joint. It may be possible to palpate the radial head in the antecubital fossa, laterally or posteriorly. Weakness or inability to extend the fingers or thumb indicates posterior interosseous nerve injury, although sensation is usually not affected. Radiographs will reveal that the ulna is fractured and the radial head is dislocated.
The patient with a Galeazzi fracture will have swelling and deformity of the forearm with pain over the fractured radius. The wrist may be swollen and tender with a prominent ulnar styloid; however, if the dislocation is not severe, these signs may be minimal or absent. Nerve injury rarely occurs in the Galeazzi fracture. Radiographs will reveal a fractured radius with a widened joint space between the distal radius and ulna. The ulnar styloid may also be fractured.
Imaging. Obtain PA and lateral radiographs. The ulna will be clearly fractured with a Monteggia fracture-dislocation. The associated radial head dislocation, though, is often missed. To avoid missing the dislocation, systematically evaluate elbow films every time you view them. A line drawn through the long axis of the radius at the elbow should normally intersect the middle third of the capitellum, regardless of the degree of elbow flexion or extension.26,27
In the Galeazzi fracture-dislocation, the radius fracture is usually obvious, and the radius is shortened on the PA view. There is also an increased space between the distal radius and ulna where they articulate. The normal distance is 1-2 mm, with an increased space indicative of ligamentous injury. On the normal lateral view, the ulna should be no more than 3-4 mm dorsal to the radius. In 60% of cases, an associated ulnar styloid fracture is seen, also indicating likely disruption of the distal radio-ulnar joint.26,27
Management. Consult an orthopedist while the patient is in the ED if you diagnose or suspect a Monteggia or Galeazzi fracture. Complications from missing a radial head dislocation in a Monteggia fracture can lead to chronic irreducible radial head dislocation, with resultant painful and limited pronation and supination.
Monteggia fractures in adults are almost always treated surgically,26,27,29 and since modern techniques of internal fixation have been employed, the outcomes have improved dramatically.29
Galeazzi fractures also generally require open reduction and internal fixation. They are unstable fractures, and complications of delayed surgical treatment include nonunion or malunion of the radius fracture, and recurrent subluxation or dislocation of the distal radio-ulnar joint. These lead to limitation of supination and pronation, weakness, and chronic pain.
Key Points. Evaluate joints above and below the injury. In patients with ulna fractures, carefully check for radial head dislocation. In patients with radius fractures, evaluate for possible distal radio-ulnar joint dislocation. Consult an orthopedic surgeon for management of Monteggia and Galeazzi fractures because delayed or missed diagnoses have a high incidence of long-term pain and disability.
Foreign Bodies
A 21-year-old female presents to the ED stating she stepped on a sewing needle that was in her carpet. She was wearing shoes and she felt the needle go into her foot and break off. She feels the sensation of the broken needle in her foot.
Epidemiology. Soft-tissue foreign bodies are a common presenting complaint in the ED. A significant amount of foreign bodies are missed by emergency physicians, with one study citing a miss rate of 38%.30 Undiagnosed foreign bodies are also an important cause of liability claims against emergency physicians.30,31 Patients may present with a known or suspected foreign body, or with symptoms due to complications of a foreign body, perhaps unaware of its entry.32 A predominance of lower extremity foreign bodies occur in children and adolescents.31
Patterns of Injury. All wounds have the potential of having a foreign body lodged in the soft tissue, regardless of the wound size. Some cases will be clear-cut, while others may present with symptoms related to complications. A patient who presents with a soft-tissue infection, especially a recurrent one, should be evaluated for possible foreign body. The most common foreign bodies are wood, glass, and metal.33
Evaluation. Obtain a detailed history of the injury as this will alert you to the possibility of a foreign body. Palpate over the wound, mass, or area of tenderness. Pain in association with a mass, sharp pain with deep palpation over a puncture wound, or pain with movement is suggestive of occult foreign body. After adequately anesthetizing the wound, it should be explored visually with good lighting and probed for foreign bodies using blunt-edged forceps. The wooden or plastic end of a cotton swab can also be used to probe the wound for grittiness without the fear of leaving cotton fibers behind in the wound.34 Use sterile technique in a bloodless field for exploration of acute wounds, using a proximal arterial tourniquet if necessary. To do this, apply a blood pressure cuff proximal to the injury, raise the extremity above the heart for at least one minute to adequately exsanguinate it, then inflate the cuff to a pressure greater than the patient's systolic pressure. Although uncomfortable for the patient, the cuff can remain safely inflated for about 2 hours. Absolute safety limits for tourniquet ischemia have not been established, although recommendations range from 1-3 hours. Digit lacerations require careful evaluation due to vital structures such as tendons, nerves, and vessels. Remember to range the extremity while examining the tissue, and that the wound margins may need to be extended to improve visualization.35
Imaging. Plain radiographic films can detect material denser than tissue, such as metal, glass, gravel, and sand. The density of organic material such as wood and plastics is similar to human tissue, and therefore may not be seen on x-ray.30,32,33 Clinical studies have shown that plain x-rays are 98% sensitive when the foreign body is a radiopaque material, however a glass particle less than 15 mm3 in volume has an increased risk of not being visualized.36
Bedside ultrasound can be used to evaluate soft-tissue foreign bodies, and has had variable success in identifying non-radiopaque materials. It can be useful in guiding removal of objects to avoid excessive damage to tissues. Ultrasound has its drawbacks, however, with pockets of air, pus, edema, and calcifications potentially producing confusing echogenicities, interfering with visualization or mimicking a foreign body.30,32-35
If x-rays are negative, ultrasound findings are equivocal, and you still have a high suspicion of foreign body, a CT scan may confirm the diagnosis. CT can be helpful with small or deep objects, detecting organic matter such as wood or plastic, locating the anatomic position of the foreign body, and detecting complications such as abscesses.32
Management. The decision to remove a foreign body should take into account the risks associated with the foreign body remaining in the tissue against the potential damage to tissue caused by its removal. Foreign bodies that cause persistent pain, interfere with anatomic function, or are toxic to the tissues should be removed. If a fracture is present, surgical debridement may be necessary. Likewise, grossly contaminated wounds require irrigation and debridement. Foreign bodies located in proximity to tendons, nerves, and vessels, and those compromising tissue oxygenation should be removed by appropriate subspecialties. In the case of a foreign body in the hand, consult a hand specialist if the object is obscured as blind exploration can cause iatrogenic damage to tissues.33 Provide tetanus prophylaxis and antibiotic coverage when clinically indicated.
In the end, not all foreign bodies can be identified, located, or removed. Carefully document the evaluation and management of the patient and ensure that the patient has received detailed discharge instructions and have adequate follow-up. Retained foreign bodies can lead to serious complications, including cellulitis, abscesses, myonecrosis, necrotizing fasciitis, and gangrene.31 While the role of prophylactic antibiotics in patients with retained foreign bodies is unclear, it is common practice to use a short course (5 days) of antibiotics directed against common skin flora. This is especially true if the wound is at higher risk for infection (i.e., distal on an extremity, contaminated with bacteria, organic foreign body, etc.). Foreign body removal from the heel can be problematic as the callous does not permit easy spreading of the tissue and during recovery the cut callous will be quite painful. Often the foreign body (usually a needle) can be located in 2 planes by either x-ray or ultrasound. A hemostat is then inserted above the callous or the lateral or medial side of the heel, and the tissue is explored until the foreign body is encountered. The object can then be manipulated back out through the callous (reversing its original path). The laceration can then be repaired on the side of the heel, decreasing the recovery pain.
Key Points. Explore wounds thoroughly. Utilize various imaging modalities to identify and locate soft-tissue foreign bodies if the history or physical examination suggests a retained foreign body. Do not remove the foreign body if the process will cause more damage to tissue than allowing it to remain. Consult a hand specialist for foreign bodies imbedded in the intricate anatomy of the hand. Document all efforts made to identify and remove the foreign body as well as patient education and follow-up.
Maisonneuve Fracture
A 19-year-old presents to the ED after he twisted his left ankle during a sporting event. There is swelling and tenderness over the medial malleolus and an ankle injury is suspected.
Epidemiology. Maisonneuve fractures occur in 1-11% of ankle fractures. It is believed that the frequency of this fracture is increasing due to increased physician awareness.37 Ankle injuries occur more often in men and often are the result of sports-related activities.
Patterns of Injury. The Maisonneuve fracture is described as a fracture of the proximal fibula with associated syndesmotic disruption and injury to the medial ankle structure. The mechanism of injury is often a rotary force applied to the ankle that causes either a medial malleolar fracture or disruption of the deltoid ligament, followed by transmission of forces through the syndesmosis between the tibia and fibula, causing a fracture of the proximal fibula.37-39
Evaluation. Obtain an accurate history of the mechanism of injury. Clinically, the ankle will likely be edematous, ecchymotic, and may be grossly deformed. There is usually point tenderness at or near the medial malleolus. Check the neurovascular status of the foot and compare with the uninjured extremity. Promptly reduce a dislocated ankle if there is vascular compromise or skin tenting. The key to diagnosis of the Maisonneuve injury is to examine the proximal portion of the fibula in every ankle injury.37,38 The patient may initially be asymptomatic, but will exhibit tenderness over the proximal fibular area when palpated. If there is any suspicion of a Maisonneuve fracture, obtain full-length tibiofibular radiographs.
Imaging. Obtain AP, lateral, and oblique (mortise) plain radiographs of the ankle. While the medial malleolus may be fractured, often the radiographs appear normal. Injury of the syndesmosis is suggested when the medial clear space is widened (> 4 mm) in the absence of a lateral malleolar fracture. Tibiofibular radiographs will reveal the proximal fibular fracture.
Management. Consult an orthopedist for known or suspected cases of Maisonneuve fracture, as untreated fractures yield poor outcomes. Definitive treatment is usually surgical.38
Key Points. Obtain a detailed history of the ankle injury and thoroughly examine the proximal fibula in all ankle injuries. Ankle radiographs may appear normal but a medial joint space > 4 mm suggests an injury to the syndesmosis. Obtain tibiofibular radiographs for tenderness over the proximal fibula. Consult an orthopedist for known or suspected Maisonneuve fractures.
Slipped Capital Femoral Epiphysis
An obese 12-year-old male presents to the ED with an 8-month history of knee pain and a limp. The pain has increased to the point that it occurs at rest. He denies hip or groin pain. There is no history of trauma.
Epidemiology. Slipped capital femoral epiphysis (SCFE) is the most common orthopedic hip disorder in adolescence. It occurs in 3-5 cases per 100,000 population per year, is twice as common in boys, and the incidence is slightly higher in African-Americans. Overweight adolescents have an increased risk for SCFE, most commonly developing the condition during their growth spurt.40
Pathophysiology. SCFE is a displacement of the femoral head epiphysis through the growth plate (physis) during periods of rapid growth due to cumulative stress or an acute traumatic event. The pathogenesis is multifactorial and not completely understood. Traumatic, endocrine, hereditary, vascular, and toxic factors have been associated with SCFE.41 Interestingly, most (75%) patients will have no history of trauma.40
Evaluation. The diagnosis of SCFE is often missed on initial presentation, with delay in diagnosis reported to be an average of 6 months.40 Because the history is usually nonspecific and the physical examination elusive, a high index of suspicion is required to avoid complications related to delayed diagnosis. The patient with SCFE may present with complaints of hip, groin, or knee pain. Up to one-half of patients will not complain of any hip pain. Referred knee or thigh pain is common initially, and may be felt as a dull ache. Pain is exacerbated with exercise, and as the slip progresses, the pain becomes constant and more severe. Eventually the patient experiences pain at rest, holds the hip in external rotation, and walks with a limp. Physical examination may reveal decreased range of motion of the hip, and a hip that externally rotates as the physician flexes it. The physical examination may, however, also be completely normal.40
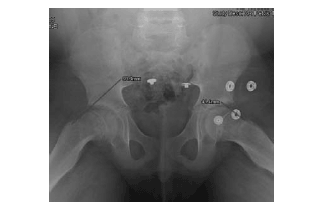
Imaging. Obtain an AP view of the pelvis (see Figure 14) and frog leg lateral view of the affected hip on all children and adolescents with unexplained hip, groin, thigh, or knee pain, or who present with a limp. On AP view, a line drawn along the superior femoral neck (Klein's line) normally should cross a portion of the femoral epiphysis. If the epiphysis falls below this line (see Figure 14—the right hip) or intersects a smaller portion compared to the other side, an SCFE likely is present. On the frog leg lateral view, the slip is usually more obvious, with the femoral head displaced posterior and medial to the neck. Early in this disorder, radiographic findings may be more subtle, and additional imaging such as ultrasound, CT, MRI, and bone scans can aid in the diagnosis.
| Figure 14. SCFE with Klein's Line |
|
Management. As soon as the diagnosis is suspected, the patient should be made completely non-weight bearing pending confirmation and, once diagnosed, an orthopedist should be consulted. A stable slip can progress to an unstable, more severe slip with increased morbidity if unrecognized or untreated in a timely manner. Outcomes are generally good, but depend largely on the degree of slip that is present. Complications include chondrolysis, avascular necrosis, and osteoarthritis.40
Key Points. Suspect SCFE in obese children between the ages of 10 and 15 with vague complaints of hip, groin, thigh, or knee pain, or with a limp. Obtain AP pelvis and frog leg lateral radiographs to identify SCFE. Consult orthopedics urgently when SCFE is diagnosed. Early diagnosis and repair results in better outcomes.
Conclusion
The orthopedic injuries described in this review are fraught with the potential for misdiagnosis or mismanagement. With a heightened awareness and knowledge of the subtleties of the history, physical examination, and radiographic findings, accurate diagnosis and effective treatment can be achieved
References
1. Gwynne A, Barber P, Tavener F. A review of 105 negligence claims against accident and emergency departments. J Accid Emerg Med 1997;14:243-245.
2. Karcz A, Korn R, Burke MC, et al. Malpractice claims against emergency physicians in Massachusetts: 1975-1993. Am J Emerg Med 1996;14:341-345
3. Harrison B, Holland P. Diagnosis and management of hand injuries in the ED. Emerg Med Practice 2005;7:1-26.
4. Neumeister M, Wilhelmi BJ. eMedicine Journal (serial online) Jan 2005. Available at http://www.emedicine.com/orthoped/topic94.htm.
5. Perron AD, Brady WJ, Keats TE, et al. Orthopedic pitfalls in the ED: Closed tendon injuries of the hand. Am J Emerg Med 2001;19:76-80.
6. Vasilevski D, Noorbergen M, Depierreux M, et al. High pressure injection injuries to the hand. Am J Emerg Med 2000;18:820-824.
7. Hogan CJ, Ruland, RT. High-pressure injection injuries to the upper extremity: A review of the literature. J Orthopaedic Trauma 2006;20:503-511.
8. Schnall SB, Mirzayan R. High-pressure injection injuries to the hand. Hand Clinics 1999;15:245-248.
9. Gelberman RH, Posch JL, Jurist JM. High-pressure injection injuries of the hand. J Bone Joint Surgery 1975;57:935-937.
10. Ufberg J, Harrigan RA, Cruz T, et al. Orthopedic pitfalls in the ED: Achilles tendon rupture. Am J Emerg Med 2004;22:596-600.
11. Jozsa L, Kvist M, Balint BJ, et al. The role of recreational sport activity in Achilles tendon rupture. Am J Sports Med 1989;17:338-343.
12. Arner O, Lindholm A. Subcutaneous rupture of the Achilles tendon: A study of 92 cases. Acta Chir Scandinavica 1959;S239:7-51.
13. Germann CA, Perron AD, Miller MD, et al. Orthopedic pitfalls in the ED: Calcaneal fractures. Am J Emerg Med 2004;22:607-611.
14. Weedler IS, Charted J. Emergency department evaluation and treatment of ankle and foot injuries. Emerg Med Clin North Am 2000;18:85-113.
15. Fitzgibbons TC, McMullen ST, Mormino MA. Fractures and dislocations of the calcaneus. In: Rockwood and Green, eds. Fractures in Adults. 5th ed. Philadelphia: Lippincott-Raven; 2001:2133-2179.
16. Knight JR, Gross EA, Bradley GH, et al. Boehler's angle and the critical angle of Gissane are of limited use in diagnosing calcaneus fractures in the ED. Am J Emerg Med 2006;24:423-427.
17. Robertson A, Nutton RW, Keating JF. Dislocation of the knee. J Bone Joint Surgery Br 2006;88-B:06-711.
18. Rihn JA, Cha PS, Groff YJ, et al. The acutely dislocated knee: Evaluation and management. J American Academy Orthopaedic Surgeons 2004;12:334-346.
19. Laing AJ, Tansey C, Hussey AJ, et al. Occult knee dislocation: The importance of secondary survey. J Emerg Med 2004;21:635-636.
20. Lyn E, Pallin K, Antosia RE. Knee and lower leg. In: Marx, JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine, Philadelphia: Mosby; 2006:787-790.
21. Perron AD, Brady WJ, Sing RF. Orthopedic pitfalls in the ED: Vascular injury associated with knee dislocation. Am J Emerg Med 2001;19:583-588.
22. Amaravati RS, Saji MJ, Rajagopal HP. Greater arc injury of the wrist with fractured lunate bone: A case report. J Orthopaedic Surgery 2005;13:310-313.
23. Perron AD, Brady WJ, Keats TE, et al. Orthopedic pitfalls in the ED: Lunate and perilunate injuries. Am J Emerg Med 2001;19:157-162.
24. Weil WM, Slade JF, Trumble TE. Open and arthroscopic treatment of perilunate injuries. Clinical Orthopaedics and Related Research 2006;445:120-132.
25. Woolfrey KGH, Eisenhauer MA. Wrist and forearm. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine. Philadelphia: Mosby; 2006: 622-631.
26. Perron AD, Hersh RE, Brady WJ, et al. Orthopedic pitfalls in the ED: Galeazzi and Monteggia fracture-dislocation. Am J Emerg Med 2001;19:225-228.
27. Woolfrey KGH, Eisenhauer MA. Wrist and forearm. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine. Philadelphia: Mosby; 2006: 642-643.
28. Morgan SJ, Smith WR. Musculoskeletal trauma and conditions of the extremity. In: Markovchick VJ, Pons PT, eds. Emergency Medicine Secrets. Philadelphia: Hanley and Belfus, Inc.; 2003: 517.
29. Ring D, Jupiter JB, Waters PM. Monteggia fractures in children and adults. J Amer Academy Orthopaedic Surgeons 1998;6:215-224.
30. Dean AJ, Gronczewski CA, Costantino TG. Technique for emergency medicine bedside ultrasound identification of a radiolucent foreign body. J Emerg Med 2003;24:303-308.
31. Lyn E, Pallin D, Antosia RE. Knee and lower leg. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine. Philadelphia: Mosby; 2006: 805.
32. Thomas SH, Brown DFM. Foreign bodies. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine. Philadelphia: Mosby; 2006: 878-879.
33. Lyn E, Antosia RE. Hand. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine. Philadelphia: Mosby; 2006: 618-619.
34. Severyn RA. Tricks of the trade. In: Markovchick VJ, Pons PT, eds. Emergency Medicine Secrets. Philadelphia: Hanley and Belfus, Inc.; 2003: 585.
35. Simon B, Hern HG. Wound management principles. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine. Philadelphia: Mosby; 2006: 845.
36. Flom LL, Ellis GL. Radiologic evaluation of foreign bodies. Emerg Med Clin North Am 1992;10:163.
37. Hensel KS, Harpstrite JK. Maisonneuve fracture associated with a bimalleolar ankle fracture-dislocation: A case report. J Orthopedic Trauma 2002;16:525-528.
38. Levy BA, Vogt KJ, Herrera DA, et al. Maisonneuve fracture equivalent with proximal tibiofibular dislocation. J Bone Joint Surgery 2006;88-A:1111-1116.
39. Hanson JA, Fotoohi M, Wilson AJ. Maisonneuve fracture of the fibula: Implications for imaging ankle injury. Am J Radiology 1999;173:702.
40. Perron AD, Miller MD, Brady WJ. Orthopedic pitfalls in the ED: Slipped capital femoral epiphysis. Am J Emerg Med 2002;20:484-487.
41. Billing L, Bogren HG, Wallin J. Reliable x-ray diagnosis of slipped capital femoral epiphysis by combining the conventional and a new simplified geometrical method. Pediatric Radiology 2002;32:423-430.
Orthopedic injuries are frequently encountered in the emergency department. It is important to recognize and correctly treat these injuries to minimize any damage and optimize outcome.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.