Physical Abuse of Children: Identification, Evaluation, and Management in the Emergency Department Setting
Physical Abuse of Children: Identification, Evaluation, and Management in the Emergency Department Setting
Authors: N. Ewen Wang, MD, Assistant Professor of Surgery, Associate Director of Pediatric Emergency Medicine, Stanford University Hospital, Stanford, CA; and Bronwyn Baz, MD, Lucile Packard Children's Hospital, Stanford University Medical Center, Palo Alto, CA.
Peer reviewer: Kristen Bechtel, MD, Associate Professor of Pediatrics, Yale University School of Medicine, New Haven, CT.
Approximately one in five of children evaluated in EDs are physically abused, emergency physicians (EPs) have a responsibility to consider abuse in the differential of every injured child.1 Although there is increasing awareness of the emergency physician's role in diagnosing abuse, EPs still frequently fail to diagnose child abuse.1 This article reviews the identification, evaluation, and management of a child with possible physical abuse.
— The Editor
Background
Physical abuse has a number of manifestations, but is most simply defined as injury inflicted upon a child by a caregiver. Recognition of child abuse in the ED setting is essential for both timely treatment and prevention of further injury. The identification of child abuse requires the completion of a thorough medical and social evaluation, and should be followed by the notification of child protective services. This sensitive and often difficult situation presents a unique challenge for both the medical staff and the family, and requires thoughtful coordination and cooperation between such disciplines as ED personnel, social workers, child protective services, law enforcement personnel, and inpatient hospital staff if the child's injury is serious enough to warrant hospital admission.
This article focuses on the evaluation of physically injured children presenting to the ED. As physically abused children commonly present to an ED for treatment, emergency medicine practitioners must keep in mind that child abuse may be the cause of a child's injury, as this may be the first significant intervention to prevent future abusive injury.
Epidemiology
The incidence of child abuse in the United States is difficult to ascertain, but is believed to be much higher than reported. The National Incidence Study of Child Abuse and Neglect reports that maltreated children who are investigated by Child Protective Services (CPS) represent only the "tip of the iceberg."2 Moreover, the findings of the Third National Incidence Study of Child Abuse and Neglect (NIS-3) show a substantial and significant increase in the incidence of children who are seriously harmed; this most likely indicates an increase in abuse incidence, rather than an increase in reporting.2 Child abuse is believed to be the etiology of 10% of traumatic injuries in children younger than age 5.3 Approximately 1,300 children die each year from inflicted injuries,4,5 and nearly 45% of those children are younger than age 1.4,6
In 2003, approximately 2.9 million reports involving 5.5 million children were made to CPS agencies; of these, nearly 70% were categorized as needing further investigation. Approximately 906,000 children were found to have been abused and/or neglected; of these substantiated cases, 25% were due to physical abuse. The range of injuries, in order of frequency of occurrence, includes: bruises, skeletal fractures, CNS (central nervous system) injuries, and burns.2,7,8
Although reports of suspected abuse are more often made for minority than Caucasian children, race has not been found to be a significant factor in substantiated cases of abuse, according to NIS-2 and NIS-3 data.4,6,9 Though gender also is not a statistically significant factor in substantiated cases of abuse, boys are more likely to incur serious injury.2,7,10 Finally, according to data from the U.S. Department of Health and Human Services/Administration for Children and Families in 2004, the most largely victimized age group is the youngest (less than one year of age), with a rate of 16.1 per 1,000 children of the same age group. The oldest children (ages 12-17 years) were victimized the least frequently.11
The abused child is at risk for both the physical and the psychological ramifications that occur as a result of battering. It is estimated that 37% of children with maltreatment injuries develop future special medical needs, most often from disability, and particularly from CNS injuries and thermal burns. The incidence of disability caused by maltreatment is estimated to be 147 per 100,000 children.7,10 Moreover, according to U.S. Department of Health and Human Service data, an estimated 1,490 children died in 2004 (compared to 1,460 children for 2003) from abuse or neglect, at a rate of 2.03 deaths per 100,000 children. Of note, 81% of those fatalities were in abused children younger than age 4. Most fatalities were associated with neglect only (35.5%), combinations of maltreatment types (30.2%), and physical abuse only (28.3%).11
Another unfortunate consequence of battering is the risk that the child himself will grow up to become a perpetrator, acting out the violence that was once modeled to him as normal problem-solving behavior.4 These children also have a higher risk of developing psychological sequelae, including psychiatric disorders such as depression, suicidal impulses, and post-traumatic stress disorder (PTSD), as well as risk-taking behaviors such as an earlier age of sexual activity and drug and alcohol use.12
Scope of the Problem: Risks for Abuse
Factors that put children at risk for physical abuse involve characteristics of both the perpetrator and the child, and are commonly exacerbated by social and environmental stressors. Perpetrators, in order of frequency, are most commonly fathers, mothers' boyfriends, babysitters (female), and mothers.13,14 Risk factors for the perpetrator include history of abuse or neglect as a child, lower level of education, young or single parenthood, and unstable social situations.15 A caretaker also may be more likely to perpetrate abuse when suffering from a psychiatric illness, when under the influence of drugs or alcohol, or when inexperienced and unprepared for parenthood.4,12,15,16
Innate factors that put the child at greater risk for abuse include young age (67% of abused children are younger than age 1 and 80% are younger than age 3), chronic illness and disability, speech and language disorders, learning disability, conduct disorders (e.g., hyperactivity), and psychological illness.4,17 Although the data is controversial, it is thought that medical conditions such as prematurity and low birth weight also may be independent risk factors of abuse later in life.18,19 Most importantly, history of previous abuse is a significant risk factor for future abuse: a physically abused child has a 50% chance of suffering further abuse and a 10% chance of dying from the abuse if it is not identified and addressed at initial presentation.1 Moreover, children whose mothers suffer from domestic violence are up to 15 times more likely to be abused. It has been recommended that screening and intervening on behalf of the battered parent may be an effective abuse prevention strategy.20
Environmental and social factors increasing a child's risk for abuse include acute and chronic problems such as financial and family stressors (divorce, separation, conflict), and illness, all of which may contribute to instability and violence in the home. Cultural factors may include social isolation, lack of support from extended family, and the modeling and acceptance of violence (such as corporal punishment and domestic violence) for resolving conflict.4,16
Types and Biomechanics of Injuries to Children
Abusive injuries to infants and children have unique characteristics due to their immature physiology, especially in regard to skeletal and CNS injuries. Orofacial injuries also are unique to children, and are found in up to one-half of physically abused children.21
Bruises. Bruises, including ecchymoses and hematomas, are the most commonly found injury in abusive trauma, accounting for up to 40% of injuries. Bruises result from direct blunt force to the skin with resulting rupture of capillaries and leakage of blood into subcutaneous tissue.21,22 Discoloration may appear immediately, or hours to days after the injury is sustained.23 As bruises heal, the discoloration progresses through a spectrum of colors as the hemoglobin from extravasated blood is broken down and removed.10 Healing of bruises may take place over a period of one to three weeks, depending on factors that include the victim's gender, health, medications (aspirin, ibuprofen) he/she may be taking, skin tone, and environmental factors. All of these factors may alter the resolution and color sequence of bruises.24
Although bruises at different stages of healing have been described as characteristic of abusive injury, caution should be used when attempting to determine the age of bruises because of a wide variability in bruise development.25 A study by Langlois and Gresham attempted the first analysis of how accurately the age of a bruise can be determined by its color. Data on color and age were analyzed in 89 photographs of bruises. Their conclusions suggested that the development of bruise color is variable, and although yellow is the color of a relatively older bruise, it may appear much earlier than forensic charts suggest.26
Although the age of a bruise cannot be accurately determined from its color, observations of location, size, and color of the bruise can be valuable in distinguishing between accidental and abusive trauma.26 For this reason, it is reasonable for a clinician to estimate a range of time (days to weeks) rather than specific dates as to when the bruise developed, based on its clinical appearance. The estimated age of a bruise should never be the sole criteria for a diagnosis of child abuse, but rather one component of a comprehensive assessment.25
Distinguishing between normal traumatic bruises and inflicted injuries in children can be difficult, but recognizable geometric shapes from implements such as belts, whips, and hand prints are suggestive of abusive injury. Additionally, location and approximate ages of bruises can be helpful for determining if a bruise is due to abuse.27 Accidental bruising most often occurs over bony prominences, such as joints (elbows, knees) or pretibial areas, the forehead, and the front of the body, as a result of play. Bruising to the back of the body, inner arms or thighs, trunk, genitalia, cheeks, ears, eyes, and neck are more suggestive of abusive injury.28,29 Other important clues include bruising in non-ambulatory babies, which is rare in accidental trauma;30 multiple and/or clustered bruises, especially bruises of different ages and healing stages, suggesting repeated inflicted injuries; and specific bruising patterns, as mentioned above.10,29 (See Figure 1.)31
| Figure 1. Abusive Bruises |
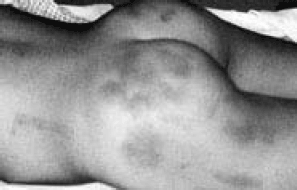 |
| Photo used with permission from David M. Pressel, MD, PhD. |
Finally, the features of bruises that are suggestive of child abuse are listed in Table 1 (also see Figure 2).
| Table 1. Features of Bruises Suggestive of Abuse10,32 |
|
| Figure 2. Loop Marks |
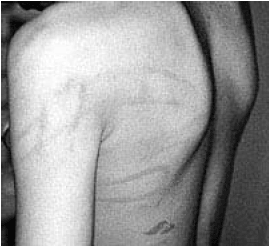 |
| Photo used with permission from David M. Pressel, MD, PhD. |
Bite Marks. Bite marks are associated with both physical and sexual abuse of children.4,33,34 They can appear as circular, elliptical, or arrow-shaped bruises or abrasions, and may have central clearing or associated erythema and petechiae. Human and animal bite marks may be differentiated by their depth. Human bites tend to be more superficial, do not always leave individual tooth marks, and lack the tearing and deep punctures of animal bites.34 Further, adult bite marks may be differentiated from a child's by the adult tooth pattern and by the maxillary intercanine distance, which is at least 2.5-3 cm.33,34
Forensic investigation is an important component of bite evaluation and documentation. The pattern, size, contour, and color of a bite mark can be evaluated by a forensic odontologist or pathologist.33 If neither is available, a physician or dentist who is knowledgeable in patterns of child abuse injuries can evaluate the bite-mark characteristics. Contact information for American Board of Forensic Odontology (ABFO)-certified odontologists can be obtained from the ABFO web site (www.abfo.org).
Blood-group substances and DNA (in epithelial cells) can be secreted in saliva and may be deposited in bites. Even if they have dried, they can be collected using the double-swab technique: 1) a sterile cotton swab moistened with distilled water is used to wipe the area in question, dried, and then placed in a specimen tube; 2) a second sterile, dry cotton swab is used to clean the same area and then is dried and placed in a specimen tube; 3) a third control sample should be obtained from an uninvolved area of the child's skin. (All samples should be sent to a certified forensic laboratory for prompt analysis. The chain of custody must be maintained on all samples submitted for forensic analysis.)33
Thorough documentation in the patient's chart of any suspicious bruise or bite mark is recommended, using written description, drawings, and careful photographic evidence with a color wheel and ruler.26
Fractures. Fractures are the second most common injury in physical abuse, and are detected in 30-55% of abused children.29 Understanding the unique physiology of children's' skeletal injuries is crucial for correctly differentiating between injuries incurred from normal childhood trauma and those from abusive trauma in the emergency setting. A child's skeleton is more porous than an adult's, and is more prone to compression injuries that may result in green stick and buckle fractures. Further, the periosteum is more prone to separation from the bone in a child, but their joint capsules and ligaments are known to be more resistant to mechanical stressors than bone and cartilage, making joint dislocations less likely in childhood. Finally, bone healing is more rapid in children than in adults.10,36
Dating of skeletal injuries is particularly important in the evaluation of physical abuse, as it may assist investigators in determining who had access to the child during the period of time that the skeletal injury is thought to have occurred. In general, fractures of long bones and ribs heal in relatively predictable stages: initial healing, soft callus, hard callus, and remodeling.10,37 The timing of metaphyseal fractures are more difficult because of the relative lack of disruption in the periosteum at the time of the fracture. Skull fractures heal differently than long bones and ribs, making the dating of injury more difficult.10
Skeletal injuries that are suspicious for abusive trauma include diaphyseal fractures, which are the most commonly found fracture in abuse and often result from transverse forces applied perpendicularly to the long axis of the bone. Spiral fractures from rotational forces, such as twisting or torquing of the extremity, especially in non-ambulatory children, are considered by some to be pathognomonic for abuse.38
Metaphyseal fractures also are considered to be pathognomonic for abuse. These fractures are subtle findings on radiographs, often appearing as chips or fractures from the corner of the bone known as "bucket handle" fractures.31 (See Figure 3.) This type of fracture is particularly important to detect, as injury to the metaphyseal plate may limit future growth if not adequately treated in a timely manner.10
| Figure 3. Metaphyseal Bucket Handle Fracture |
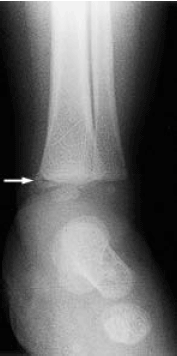 |
| Photo used with permission from David M. Pressel, MD, PhD. |
Rib fractures account for up to 27% of all abusive skeletal injuries,37 and occur as a result of direct blows as well as anteroposterior compression of the chest wall, such as occurs when holding and shaking an infant. Most abusive rib fractures are posterior and adjacent to the vertebral body, due to the levering of forces over the transverse process of the vertebra.31 (See Figure 4.) To diagnose these difficult-to-detect fractures, skeletal surveys are recommended in children younger than age 2 in whom abuse is suspected. Radionuclide bone scanning also may detect new rib fractures and subtle long bone fractures not evident on skeletal survey.1
| Figure 4. Posterior Rib Fractures |
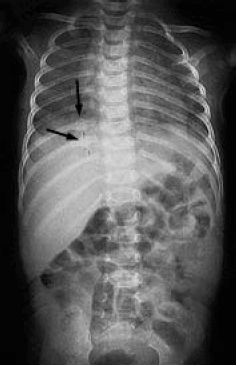 |
| Photo used with permission from David M. Pressel, MD, PhD. |
A study reviewing the value of repeat skeletal surveys within two weeks after the original survey found that follow-up skeletal survey identified additional fractures or clarified tentative findings in children who were suspected victims of physical abuse.39 The authors concluded that follow-up skeletal survey should be completed on all patients who have an initial skeletal survey performed for suspected physical child abuse and for whom child abuse is still a concern.39
Central Nervous System (CNS) Trauma
The EP frequently is required to differentiate between accidental household falls and abusive trauma as the cause of head injuries in infants and toddlers. The ability to distinguish between accidental and abusive head injury may be facilitated by an understanding of the biomechanics of brain injury. Sudden angular deceleration of the brain and cerebral vessels from violent shaking results in diffuse brain injury, such as subdural hemorrhage, which is a hallmark of inflicted craniocerebral trauma ("shaken-baby syndrome"), rather than specific contact forces applied to the surface of the head as seen in household falls.13 Thus, this angular type of force is distinctly different from those generated in most cases of accidental traumas (household falls) in young children, which involve low-velocity translational forces.13
CNS trauma is found in up to one-quarter of abused children, and represents the most serious form of injury in physical abuse.13
Abusive head trauma is the most common cause of morbidity and mortality in physically abused infants;13,14 in one case review study, 23% of children with inflicted head injuries died.14 Further, the authors found that male victims accounted for 60.3% of the cases, although death rates for boys and girls did not vary significantly. They also noted that male caretakers and babysitters are at greater risk for abusing infants.14
Sequelae include intracranial hemorrhage (subdural and subarachnoid), as well as contusions and intraparenchymal bleeding. The classic presentation linking CNS trauma and abuse is "shaken baby syndrome," with the findings of subdural hematoma; retinal hemorrhages (65-95% of cases); and skeletal fractures, including metaphyseal and posterior rib fractures (30-70% of cases) caused when the child is shaken violently back and forth.10 Significantly, although retinal hemorrhages, rib fractures, and subdural hemorrhage are the classic triad associated with head trauma, it should be emphasized that a minority of patients will have all three findings. Clinical deterioration from an acute SDH (subdural hematoma) occurs at the time of injury without a "lucid interval;" rapid onset of morbidity and mortality from traumatic brain injury in a previously healthy child is particularly suspicious for abusive trauma.10
Abusive head injury may present with a wide spectrum of symptoms and clinical findings.33 Subsequently, children who have more mild forms of head trauma and less ominous symptoms, such as vomiting and irritability, may not be recognized until they present later with a more serious injury.40 Thus, the EP's timely diagnosis of abusive head trauma is essential for preventing a child from suffering further brain injury and potentially more severe sequelae.
An analysis of missed cases of abusive head trauma (AHT) found that 31.2% of abused children with head injuries had been seen by health care personnel who had not recognized the AHT.41 The average time to correct diagnosis for these children was seven days, and AHT was more likely to be unrecognized in very young Caucasian children from intact families and in patients without respiratory distress or seizures. Significantly, 27.8% were re-injured after the missed diagnosis, and 40.7% suffered medical complications related to the missed diagnosis. The misinterpretation of radiological studies contributed to delay in diagnosis of seven of the children with unrecognized AHT, and five deaths in the group with unrecognized AHT might have been prevented by earlier recognition of abuse.41
Consequently, it is crucial for EP's to consider inflicted head trauma in infants and young children presenting with nonspecific clinical signs. Unfortunately, the diagnosis of AHT often is challenging for even the experienced EP, as caregivers rarely provide a history of trauma. A study by Duhaime and Partington, however, found that children presented with nonspecific symptoms such as vomiting or fussiness in 57% (8 of 14) of the patients with AHT. This suggests that these infants may be the ones at highest risk for missed head trauma.42 Thus, infants presenting with the symptoms noted above deserve careful consideration and screening for AHT.
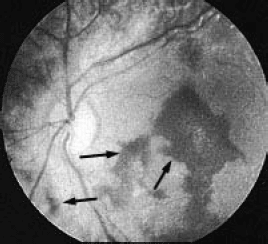
In addition to the above symptoms, retinal hemorrhage may serve as a useful sign in the EP's diagnosis of AHT. Retinal hemorrhages are seen more often in abusive head injury, are often bilateral, and tend to involve the pre-retinal layer.43 Further, they found that children with abusive head injury were more likely to have retinal hemorrhages covering the macula and extending to the periphery of the retina.31 (See Figure 5.) Importantly, unilateral retinal hemorrhages can be seen in children with accidental head injury. Other distinguishing characteristics between abusive and accidental head injury in children younger than age 2 included abnormal mental status and seizures in abused children, whereas scalp hematomas were more likely in children with accidental head injury.43
| Figure 5. Retinal Hemorrhages |
 |
| Photo used with permission from David M. Pressel, MD, PhD. |
Burns
Burns, which are found in up to 20% of abused children, are frequently due to intentional injury.22 Burns result from contact between heat energy and skin, and may be caused by liquids (causing scalding burns), chemicals, contact with hot and/or dry objects, flames (causing flash burns), and electricity. Three concentric zones of tissue damage are found in relation to the heat source: coagulation, stasis, and hyperemia. Skin closest to the heat source undergoes coagulation necrosis as cellular proteins denature; thus, no regeneration is possible. Stasis results from less direct heat exposure, and cellular repair may be possible. Hyperemia is the least direct injury to skin cells and has the greatest potential for repair.10,44
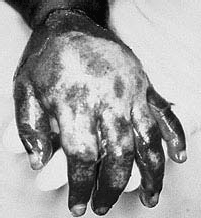
Specific burn patterns should raise suspicion for intentional injury, and include brands or contact burns (grill or grid patterns), cigarette burns, immersion burns31 (see Figure 6), microwave oven burns, and stun gun burns. Patterned or brand burns from an intentional burn such as a cigarette, radiator grill, or curling iron are uniformly deep and leave clear outlines of the identifiable object on the skin, whereas unintentional burns are shallow and leave only part of an outline due to the withdrawal reflex.4 Cigarette burns, for instance, usually leave a complete circle, 8-10 mm in diameter, often with an indurated margin, and are often painless due to deep, third-degree tissue damage. Microwave burns (inflicted by holding a child's extremity in an operating microwave) and stun gun burns cause partial to full-thickness burns; abusive stun-gun injuries are usually multiple, paired burns 0.5 cm in diameter and 5 cm apart.4,45,46
| Figure 6. Immersion Burn |
 |
| Photo used with permission from David M. Pressel, MD, PhD. |
In detail, burn patterns consistent with abuse include: forced immersion burns resulting in sharp stocking and glove demarcations with sparing of flexural/protected areas such as antecubital or popliteal fossae and no splash or drip marks; bilateral or "mirror image" burns or localized burns to genitals, buttocks, and perineum not consistent with accidental trauma; and splash/spill-type burns attributed to a developmental level not consistent with the child's age and abilities. Finally, evidence of delay in seeking care for burns and presence of other injuries are highly suspicious, especially when the physical examination is incompatible with the provided history.10,47
Burns have been attributed to abuse, neglect, or unstable family factors in up to 8% of cases in pediatric burn units.4,48 Social factors that are associated with abusive burns include children living in single-parent families and previous history of investigation for abuse. Medical factors associated with inflicted burns include increased requirement for intensive care or skin grafting and, most importantly, higher mortality rates. In two studies, mortality from abusive burns was found to be 5.6-9.6%, as opposed to 2.6-6% from accidental burns.4,48
Facial Injuries
Oral and facial injuries are common in physical abuse, occurring in up to one-half of cases.21 Toddlers do frequently have injuries to the lips or maxillary frenulum due to accidental falls. However, these injuries in non-ambulatory children are suspicious for forced feeding, such as when the bottle is jammed forcefully into the child's mouth. Lip or frenulum injuries may also result from facial blows.21
Other types of orofacial injuries observed in abuse may include: facial fractures (e.g., the mandible or other facial bones); deviated septum or other damage to the nose from direct trauma or foreign body penetration; periorbital injuries ("raccoon eyes"); post-auricular ecchymosis or blood behind the tympanic membranes; bruising and scarring at the angles of the mouth, such as would occur when a gag is placed around the mouth; traumatic alopecia from hair pulling (patchy areas of missing hair without the scaling and inflammation seen in tinea capitis, occasionally associated with scalp bruising or subgaleal hematoma); and burns from forced ingestion of scalding liquids or caustic materials, or dental fractures and tooth discoloration from repeated direct trauma.4,33,49-51
Forced Ingestion and Starvation
Forced ingestion may involve intentional poisoning of children with massive amounts of water, salt, pepper, or various drugs and overlaps with Munchausen syndrome by proxy.4,52,53 Although not as commonly described,54 the sequelae can be particularly grave. Excessive water ingestion may be used as a form of punishment, and presents with hyponatremic seizures, vomiting, coma, and/or death.53 Signs of physical abuse also are often present and should be thoroughly assessed. Salt poisoning also overlaps with Munchausen syndrome by proxy and often presents as recurrent unexplained hypernatremia, with serum sodium levels greater than 200, in the first 6 months of life.55 In this instance, urine sodium and chloride also may be elevated, and renal and endocrinological evaluations are normal.4 Finally, starvation is a less common form of child abuse, but may have higher mortality rates; one case series reported up to 50% mortality.56 Age appears to be a significant risk factor for death: the median age at which children suffer fatalities is 8 months, whereas children ages 8 or older usually survive their injuries. These children also may be at significantly greater risk for fatality from starvation due to their isolation from relatives and medical and school personnel.56
Evaluation for Abuse: History
The evaluation of the injured child requires a complete history of the circumstances and events leading up to the injury. Documentation should be meticulous and legible, as the EP might be called to court years from the actual examination.10 Essential questions are similar to the usual information gathered in history-taking but require more specific data. (See Table 2.) Assessment of the developmental level of the child also is required in the determination of whether the story is compatible with the child's developmental abilities (for instance, a 2-month-old generally will not roll off the table and hit his head).
| Table 2. Documentation of Abuse |
 |
Classic red flags in the history for abusive trauma are listed in Table 3.
| Table 3. Red Flags for Abuse |
 |
Clinical Evaluation: Physical Exam
Children with abusive injuries present with a wide spectrum of severity, from a child who is apneic and unresponsive due to abusive head trauma, to the child who is otherwise well appearing but who has multiple old fractures. For the child with acute severe trauma, the usual trauma evaluation should proceed, beginning with an assessment of the child's airway, breathing, and circulation. The physical examination should be comprehensive, looking for contemporaneous as well as prior injuries. Other physical signs consistent with physical abuse include multiple injuries and types of injuries, as well as injuries at different stages of healing, presence of pathognomonic injuries such as those seen in abusive head trauma (SDH, posterior rib fractures, and retinal hemorrhages), or patterned injuries such as cigarette burns or loop marks (see Table 3).10 Finally, evidence of malnourishment (weight less than third percentile) and neglect such as caries, poor hygiene, and lack of adequate clothing; and poor (harsh or aloof) interaction between caregiver and child are important clues for abuse.
Differential Diagnosis
The diagnosis of accidental versus abusive injuries is crucial for the child's proper medical and social management, and may be confounded by the presence of underlying medical conditions. Whereas the past medical history often will elucidate previously diagnosed conditions, the exploration of the differential diagnosis for physical abuse should be undertaken in those cases that are unclear or suggest an alternative etiology of injury. The workup should include laboratory data as is appropriate based on the child's presentation.10 (See Table 4.) Often, the workup and consults will be completed once the child is admitted. Clinicians should always consider reasonable, alternative medical diagnoses before concluding that the child's injury is most likely from abuse.
| Table 4. Laboratory and Imaging Considerations10 |
 |
Differential diagnoses for bruises are many, and most commonly include Mongolian or slate-gray spots. These are collections of melanocytes causing bluish discoloration in patches over the sacrum, back, and extremities present at birth in up to 80% of African-American children as well as in high percentages of Hispanic and Asian children.57 Hemangiomas also are frequently found in infants, may be reddish to bluish in color, and may have deep as well as superficial components. They tend to be present at birth, evolve relatively rapidly over the first year of life, and then spontaneously regress. Several presentations that may be confused with abusive bruises as well, include: eczema, phytophotodermatitis (reddened areas and erosions from sun exposure), erythema multiforme (variable erythematous lesions from drug or sensitivity reactions), idiopathic thrombocytopenic purpura (ITP) and other bruising or petechiae from coagulopathy or malignancy, unusual genetic syndromes such as Ehlers-Danlos syndrome (loss of normal skin elasticity) or OI type I (discussed below in the skeletal injury differential), and folk healing practices such as cupping (using a heated, usually glass, cup to apply vacuum suction to one's back), coining (applying heated coins to a child's skin, see Figure 7),58 or moxibustion (application of incense to skin believed to have healing power).10
| Figure 7. Coining |
 |
| Photo used with permission from Preston Maxim, MD, San Francisco General Hospital. |
Cigarette burns may be confused with nummular impetigo, phytophotodermatitis, or dermatitis herpetiformis (often associated with autoimmune diseases and characterized by blistering). Finally, as noted above, folk remedies such as cupping, coining, or moxibustion also may cause burns that are suspicious for abusive trauma, but represent an attempt to treat an illness rather than an intent to harm.10 An accurate history taken with the aid of a medical interpreter, when necessary, is essential in discernment of the latter case.
For skeletal fractures, the differential diagnosis includes normal variants of bone structures (which may appear suspicious on radiographs), congenital syphilis (causing periosteal elevation on radiograph), Vitamin D-dependent rickets, and osteogenesis imperfecta (OI).10
With respect to OI, there are four types, of which Type IV is the most easily confused with abuse. Features include easy bruising, short stature, abnormal dentition (dentinogenesis imperfecta) bluish sclera (Types I and II) and varying degrees of osteopenia.10 Abusive injury can be distinguished from OI Types I and II due to their characteristic blue sclerae.59 Differentiation between abuse and OI types III and IV may be more difficult. Although rare, type III has normal sclerae but severely fragile bones with frequent fractures and progressive deformity of long bones. However, radiographs of children with mild cases of OI will demonstrate wormian bones in the skull and osteoporosis characteristics. Distinguishing abusive injury from OI Type IV may be more challenging, as the clinical characteristics may be less severe. It often can be identified with careful family history and evaluation for the radiographic findings of OI, such as the presence of wormian bones, osteoporosis, bony deformity, and demineralization.38,59
The differential for CNS injuries includes infections such as meningitis or encephalitis, febrile or idiopathic seizures, and ingestions.10 Specifically, the evaluation for shaken baby syndrome includes the differential diagnosis for SDH and retinal hemorrhages, such as accidental trauma, coagulation disorders, vascular malformations, and rare amino acid metabolic disorders such as glutaric aciduria type I (associated with acute encephalopathy and SDH). Finally, the history should evaluate for the folk healing practice "caida di mollera," where a child with a sunken fontanelle is held upside by the ankles and shaken (in an effort to pop out the fontanelle).10
The differential diagnoses for retinal hemorrhages include vasculitis, vascular obstruction, and toxic febrile illness associated with serious infections.10 The role of the EP is to rule out potentially grave diagnoses in the differential and to contact the pediatrics service for admission to protect the child while the remainder of the social and medical work-up is completed.
Clinical Evaluation: Ancillary Studies
If during the history and physical exam, a concern for abuse has developed, appropriate ancillary studies can be ordered. In cases where inflicted head trauma is suspected, in addition to those cases where a child presents with seizures, altered mental status, and focal neurological findings, a head CT should be obtained to evaluate for skull fractures, intracranial hemorrhage, or hydrocephalus.10 During in-hospital evaluation, a brain MRI with contrast may be useful in dating CNS injuries, which may assist in the identification of the chronicity of the injury and when the child was exposed to a potential perpetrator.10 (See Table 4.)
Due to the frequency of skeletal injury and difficulty in detection of fractures in younger children, a skeletal survey should be considered in the clinical evaluation of all children younger than age 2 in whom there is a concern for abuse. The skeletal survey consists of AP views of humeri, forearms, hands, femurs, lower legs, and feet; chest; pelvis; lateral view axial skeleton (infants); and AP and lateral views of the skull.10 (See Table 4.) Finally, a skeletal survey should be performed during the evaluation of a child with suspected abusive head injury, as extracranial abnormalities may be detected in 30-70% of these children.13
Psychosocial Evaluation of Suspected Child Abuse in the ED
When abuse is suspected, and/or when a young child presents with a severe injury, the immediate involvement of a social worker, especially when they are specifically trained in the area of child abuse, can add invaluable information to the medical team's assessment of the social situation and the child's safety. Consultation with Child Protective Services (CPS) is crucial when abuse is suspected and may be especially helpful when it is uncertain: unusual aspects of the case may be discussed with CPS by phone 24 hours a day. The CPS worker will note the details of the case, including the assessment of the caretakers' background, abilities, environment, and potential risk to other children, and advise whether the case merits further investigation by CPS and potentially by local law enforcement agencies.10
In some cases, the child must be admitted to the hospital for protection while the social and medical evaluations are completed. The family's understanding and cooperation with the investigative process may be facilitated by a preliminary and diplomatic conversation with the child's family, communicating concern for abuse and the consequent necessity for discussion with CPS, additional studies such as the skeletal survey, and admission for the child's appropriate medical management and safety. It must be stressed that the EP's role is to ensure that there are no emergent health issues or injuries that require evaluation and management. While careful communication between the EP and admitting physician must ensure that a thorough history and work-up are done, often the appropriate locale of the thorough history and extensive testing will be during hospital admission.10
Medico-legal Considerations
The mandated reporting law, which exists in all states, requires that a physician make a report to CPS when there is a reasonable suspicion that a child's injury was caused by abuse. The physician should be familiar with the laws for reporting in their respective state. A reasonable suspicion for abuse is defined as when the information gathered by the physician leads to the conclusion that a child's injury or medical condition is most likely due to child abuse. Once a report is made (usually by calling the 24-hour emergency state or county hotline) and written documentation is provided, CPS workers evaluate the provided information, investigate the report if deemed appropriate, and provide support to the family per the state's established timeline.10
Finally, a physician making a report "in good faith" is able to claim immunity from liability if an angry caregiver and/or family files suit against that physician if it is determined that no maltreatment occurred. Additionally, a physician who fails to make a report of suspected abuse may be liable for prosecution for failure to report child abuse under the state's statutes. In cases of physical abuse, the EP may be subpoenaed to testify in court. Thus, the most effective way a physician can advocate for the child in question is to accurately and thoroughly document the medical evaluation performed in the ED.10
Conclusion
In summary, the physical abuse of children has potential for serious long-term sequelae, such as disability and death. While there is a vast spectrum in the presentation of physical abuse, ranging from mild bruising to acute intracranial hemorrhage, each child presenting to the ED for treatment of an injury must be carefully evaluated for the possibility of child abuse. Even mild injuries may be suggestive of more extensive and long-term battering, and a thorough history and physical exam might yield findings to pursue a complete laboratory, radiological, and psychosocial evaluation. The ED evaluation of child abuse requires cooperation and collaboration among many different disciplines, such as the ED providers, social workers, CPS investigators, and law enforcement personnel. Finally, meticulous documentation of the child's medical evaluation in the ED is the most effective way to advocate for the child and to protect the child from further abusive episodes.
References
1. Saade DN, Simon HK, Greenwald M. Abused children: missed opportunities for recognition in the ED. Acad Emerg Med 2002;9:524.
2. Sedlak AJ, Broadhurst DD. Third National Incidence Study of Child Abuse and Neglect, US Dept of Health and Human Services; 1996. Accessed on 8/13/07 at www.childwelfare.gov/pubs/statsinfo/nis3.cfm.
3. Kocher MS, Kasser JR. Orthopedic aspects of child abuse. J Am Acad Orthop Surg 2000;8:10-20.
4. Endom E. Epidemiology and clinical manifestations of child abuse. UpToDate Patient Information online.
5. United States Dept of Health and Human Services, Administration on Children, Youth, and Families. Child Maltreatment 2001. US Govt Printing Office, Washington DC, 2003. Accessed 8/13/07 at http://www.acf.hhs.gov/programs/cb/pubs/cm01
6. U.S. Department of Health and Human Services, Children's Bureau Administration on Children, Youth, and Families. Child welfare outcomes 2000: Annual report. Appendix C: Highlights of findings from Child Maltreatment 2000.
7. National Center on Child Abuse and Neglect: National Child Abuse and Neglect Data Service Component. Washington DC: Government Printing Office: 1993. Working Paper 2.
8. U.S. Department of Health and Human Services: Child Maltreatment 2003. In: Chapter Three: Victims. Accessed 8/13/07 at http://www.acf.hhs.gov/programs/cb/pubs/cm03
9. Lane WG, Rubin DM, Monteith R, et al. Racial differences in the evaluation of pediatric fractures for child abuse. JAMA 2002;288:1603-1609.
10. Giardino AP. Child Abuse and Neglect: Physical Abuse. Emedicine 2006 June 15th.Accessed Dec 10th, 2006. Available at: URL: http//www.emedicine.com/ped/topic2648.htm.
11. U.S. Department of Health and Human Services: Administration for Children and Families. Summary: Figures. Child Maltreatment 2004. Accessed 8/15/07 at http://www.acf.hhs.gov/programs/cb/pubs/cm04/sumfig.htm
12. Egami Y, Ford DE, Greenfield SF, et al. Psychiatric profile and sociodemographic characteristics of adults who report physically abusing or neglecting children. Am J Psychiatry 1996;153:921-928.
13. Duhaime AC, Christian CW, Rorke LB, et al. Nonaccidental head injury in infants—the "shaken baby syndrome". N Engl J Med 1998;338:1822-1829.
14. Starling SP, Holden JR, Jenny C. Abuse head trauma: the relationship of perpetrators to their victims. Pediatrics 1995;95:259-262.
15. Jain AM. Emergency department evaluation of child abuse. Emerg Med Clin North Am 1999;17:575-593.
16. Ludwig S. Child abuse. In: Textbook of Pediatric Emergency Medicine. Fleischer GR, Ludwig S, Henretig FM, eds. 5th ed. Philadelphia: Lippincott Williams and Wilkins; 2006:1761.
17. Kini N, Lazoritz S. Evaluation for possible physical or sexual abuse. Pediatr Clin North Am 1998;45:205-219.
18. Strathearn L, Gray PH, O'Callaghan FD, et al. Childhood neglect and cognitive development in extremely low birth weight infants: a prospective study. Pediatrics 2001;108:142-151.
19. Gessner BD, Moore M, Hamilton B, et al. The incidence of infant physical abuse in Alaska. Child Abuse Negl 2004;28:9-23.
20. Jenny C; Committee on Child Abuse and Neglect. Evaluating infants and young children with multiple fractures. Pediatrics 2006;118:1299-1303.
21. Naidoo S. A profile of the oro-facial injuries in child physical abuse at a children's hospital. Child Abuse Negl 2000;24:521-534.
22. Wissow LS. The medical history and physical examination. In: Child Advocacy for the Clinician: An Approach to Child Abuse and Neglect. Baltimore: Williams and Wilkins; 1990:49.
23. Wilson EF. Estimation of the age of cutaneous contusions in child abuse. Pediatrics 1977;60:750-752.
24. Dailey JC, Bowers CM. Aging of bitemarks: a literature review. J Forensic Sci 1997;42:792-795.
25. Schwartz AJ, Ricci LR. How accurately can bruises be aged in abused children? Pediatrics 1996;97:254-257.
26. Langlois NE, Gresham GA. The ageing of bruises: a review and study of the colour changes with time. Forensic Sci Int 1991;50:227-238.
27. Dunstan FD, Guildea ZE, Kontos K, et al. A scoring system for bruise patterns: a tool for identifying abuse. Arch Dis Child 2002;86:330-333.
28. Carpenter RF. The prevalence and distribution of bruising in babies. Arch Dis Child 1999;80:363-366.
29. Maguire S, Mann MK, Sibert J, et al. Are there patterns of bruising in childhood which are diagnostic or suggestive of abuse? A systematic review. Arch Dis Child 2005;90:182-186.
30. Pressel DM. Evaluation of physical abuse in children. Am Fam Physician 2000;61:3057-3064.
31. Sugar NF, Taylor JA, Feldman KW. Bruises in infants and toddlers: those who don't cruise rarely bruise. Puget Sound Pediatric Research Network. Arch Pediatr Adoles Med 1999;153:399-403.
32. Committee on Child Abuse and Neglect. Academy of Pediatrics. When inflicted skin injuries constitute child abuse. Pediatrics 2002;110:644-645.
33. Kellogg N; American Academy of Pediatrics Committee on Child Abuse and Neglect. Oral and dental aspects of child abuse and neglect. Pediatrics 2005;116:1565-1568.
34. Jessee SA. Orofacial manifestations of child abuse and neglect. Am Fam Physician 1995;52:1829-1834.
35. Albert MJ, Drvaric DM. Injuries resulting from pathologic forces: child abuse. In: Pediatric Fractures: A Practical Approach to Assessment and Treatment. MacEwen GD, Kasser JR, Heinrich SD, eds. Baltimore: Williams and Wilkins; 1993:388.
36. Spivak BS. Biomechanics of nonaccidental trauma. In: Ludwig S, Kornberg AE, eds. Child Abuse: Medical Reference. 2nd ed. New York: Churchill Livingstone; 1992:61-78.
37. Kleinman PK. Diagnostic Imaging of Child Abuse. 2nd ed. St Louis: Mosby-Yearbook, Inc.; 1998.
38. Kleinman PK. The spectrum of non-accidental injury and its imitators in children. In: Musculoskeletal Diseases: Diagnostic Imaging and Interventional Techniques. Hodler J, Zollikofer, von Schulthess GK, Zollikofer CL, eds. Milan: Springer; 2005:169-174.
39. Zimmerman S, Makaroff K, Care M, et al. Utility of follow-up skeletal surveys in suspected child physical abuse evaluations. Child Abuse Negl 2005;29:1075-1083.
40. Bechtel K, Stoessel K, Leventhal JM, et al. Characteristics that distinguish accidental from abusive injury in hospitalized young children with head trauma. Pediatrics 2004;114:165-168.
41. Jenny C, Hymel KP, Ritzen A, et al. Analysis of missed cases of abusive head trauma. JAMA 1999;281:621-626.
42. Duhaime AC, Partington MD. Overview and clinical presentation of inflicted head injury in infants. Neurosurg Clin N Am 2002;13:149-154.
43. Bechtel K, Berger R. Inflicted traumatic brain injury: making the diagnosis in the emergency department. Clin Pediatr Emerg Med 2006;7:138-142.
44. Robson MC, Heggers JP. Pathophysiology of the burn wound. In: Burns in Children: Pediatric Burn Management. Carvajal HF, Parks D, eds. Chicago: Year Book; 1988:27-32.
45. Alexander RC, Surrell JA, Cohle SD. Microwave oven burns to children: an unusual manifestation of child abuse. Pediatrics 1987; 79:255-260.
46. Burdett-Smith P. Stun gun injury. J Accid Emerg Med 1997;14:402-404.
47. Hansbrough JF, Hansbrough W. Pediatric burns. Pediatr Rev 1999;20:17-23.
48. Andronicus M, Oates RK, Peat J, et al. Non-accidental burns in children. Burns 1998;24:552-558.
49. Wissow LS. Head and internal injuries. In: Child Advocacy for the Clinician: An Approach to Child Abuse and Neglect. Baltimore: Williams and Wilkins; 1990:67.
50. Crouse CD, Faust RA. Child abuse and the otolaryngologist: part II. Otolaryngol Head Neck Surg 2003;128:311-317.
51. Saraswat A. Child abuse and trichotillomania. BMJ 2005;330:83-84.
52. Friedman EM. Caustic ingestions and foreign body aspirations: an overlooked form of child abuse. Ann Otol Rhinol Laryngol 1987;96:709-712.
53. Arieff AI, Kronlund BA. Fatal child abuse by forced water intoxication. Pediatrics 1999;103:1292-1295.
54. Thomas JN. Child abuse and neglect. CHNMC Clinical Proceedings. 1984 May-August. Accessed 8/13/07 at http://www.dvinstitute.org/conferences/proceedings/1995/joyce.pdf
55. Meadow R. Non-accidental salt-poisoning. Arch Dis Child 1993; 68:448-452.
56. Kellogg ND, Lukefahr JL. Criminally prosecuted cases of child starvation. Pediatrics 2005;116:1309-1316.
57. Bittner S, Newberger E. Pediatric understanding of child abuse and neglect. Pediatr in Review 1981;2:197-207.
58. Maxim P. San Francisco General Hospital Emergency Department, UCSF, Continuing Education, Clinical Images website. Accessed on 8/15/07 at http://sfghed.ucsf.edu/Education/ClinicImages/Coining%20clin.jpg
59. Kleinman PK. Differentiation of child abuse and osteogenesis imperfecta: medical and legal implications. AJR Am J Roentgenol 1990;154:1047-1048.
60. Oral and dental aspects of child abuse and neglect. American Academy of Pediatrics. Committee on Child Abuse and Neglect. American Academy of Pediatric Dentistry. Ad Hoc Work Group on Child Abuse and Neglect. Pediatrics 1999;104(2 pt 1):348-350.
61. Potash AS. Pediatrics, Child Abuse. EMedicine. Accessed on 8/13/07 at http://www.emedicine.com/emerg/topic368.htm
Approximately one in five of children evaluated in EDs are physically abused, emergency physicians (EPs) have a responsibility to consider abuse in the differential of every injured child.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
