Medical Problems of Diving and the Primary Care Physician — Part III, Medical Evaluation and Fitness for Diving
Authors: Michael B. Strauss, MD, FACS, AAOS, Medical Director of the Baromedical Department, Long Beach Memorial Medical Center, Long Beach California, Clinical Professor, Orthopaedic Surgery, University of California Irvine College of Medicine, Irvine, Calif; and Igor V. Aksenov, MD, PhD, Associate Dean and Professor, Saba University School of Medicine (Saba, Netherlands-Antilles), Director, Hyperbaric Medicine Program, Medical Director, Saba Marine Park.
Editor’s Note—This is the final in a 3-part series on the medical problems of diving. Part I focused on diving medicine and physiology. Part II covered the medical problems of the sports diver, including panic, diver-blackout, exposure problems, injuries from marine animals, descent problems, ascent problems, arterial gas embolism, decompression sickness, and complications from medical problems of diving, including near drowning/drowning, shock, and cardiac arrest. The following manuscript will focus on medical standards for the different types of diving, female divers and pregnancy considerations, and finally, drugs and diving.
Medical Standards for the Different Types of Diving
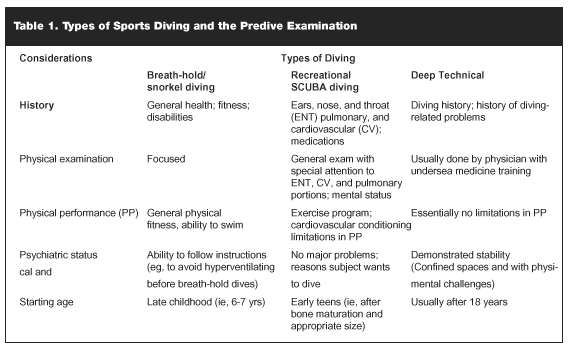
The primary care physician (PCP) may be asked to perform medical examinations and give opinions regarding fitness for diving. Sport diving, regardless of the type, requires good physical and mental health. Medical clearance for sport diving, although based on objective as well as subjective considerations, must also consider the type of diving that will be done, namely, snorkel/breath-hold, SCUBA, or deep technical (see Table 1). There are absolute medical contraindications to diving for reasons of safety, aggravation of the condition, pre-existing conditions or performance requirements (see Table 2). If the condition is severe enough, the individual will usually choose not to dive.
 |
 |
Breath-hold/Snorkel Diving. Minimum if any medical screening is done for this type of diving. However, we recommend that if the PCP is aware of his or her patient’s interest in this type of diving that they evaluate them for any conditions that could affect physical performance, stamina, and alertness. Cardiac arrhythmias may be precipitated by the stresses of breath holding, the diving reflex, and cold water. A history of epilepsy is considered by most authorities to be a contraindication to diving. Patients with a history of recurrent ear and sinus infections, while not a contraindication to diving, should be instructed in the proactive use of vasoconstrictors at the first signs of middle ear and sinus congestion. Fitness and swimming ability should be established by the ability to swim several hundred yards comfortably in open water without swimming aids. Mild-to-moderate overweight is not a problem for this type of diving. Age, likewise, is not a contraindication. Children, with supervision, should be able to participate in this type of diving as soon as they can use fins, mask, and snorkel comfortably, usually at 6-7 years of age.
Sports SCUBA Diving. Although a medical examination is not required by the SCUBA diving certifying agencies in the United States to begin diving lessons, each student is required to complete a health questionnaire. If any of the answers are positive for disease conditions, a medical examination with medical clearance by a physician is required before allowing the prospective student to begin SCUBA diving training. While this is the essence of preventive medicine, it offers the certifying agencies protection from the liability of training a diver who is at risk for a serious MPD. Operators of most sports SCUBA diving charters require that their clients complete a similar health questionnaire, release from liability form before allowing the divers to use their equipment.
When a PCP is asked to provide a medical clearance in the above situations, guidelines can be helpful. For example, histories of asthma and ear, nose, and throat problems that are well controlled and do not interfere with physical performance are not contraindications for SCUBA diving. If there is any risk of pulmonary disease, a chest x-ray is advised. If the diver is older than 40 years, we recommend an electrocardiogram with exercise stress testing. Diabetes, moderate obesity, behavior problems, phobias (eg, to confined spaces), neuropathies, hearing loss, and residuals of severe musculoskeletal injuries are examples of relative contraindications to diving. A history of heart problems is also a relative contraindication to diving. Verification of fitness, stamina, and reasonable cardiac reserve is essential before giving an OK to SCUBA dive. The individual with such a history, but cleared to dive, should be encouraged to dive in areas that minimize exertional stresses, such as diving off a boat in warm, clear, calm waters. If the prospective diver is motivated, and complications have not developed from the problems considered to be relative contraindications, we generally allow him or her to dive. Advice should be given about avoiding injury, strict adherence to diving safety practices, and selection of a dive buddy who is competent and aware of the diver’s limitations.
We personally do not recommend that youngsters younger than their early teens be allowed to SCUBA dive. The reasons for this are 3-fold. First, most diving equipment is designed for larger sized individuals. Second, there is the potential for damage to growth centers of the bones due to gas bubbling in the venous sinusoids with their associated sluggish blood flow. In theory this would be a preferential environment for inert gas bubbling to develop. Finally, the question of maturity and judgment in decision-making is a consideration. In this regard, the age to OK SCUBA diving is analogous to driving an automobile. Others have suggested that it is OK for youngsters to SCUBA dive as long as they follow precautions like limiting the depths of their dives (30 feet or less), dive under optimal conditions, and have adult supervision. The decision for older aged individuals to dive must be based on physiological rather than chronological age. There are no specific upper age limits for SCUBA diving. Because of less muscle strength, stamina, and cardiovascular reserve, our advice to older individuals is to dive "conservatively." To date no modifications for diving tables or dive computers have been offered for the older aged diver.
Deep Technical Diving. We feel that the medical exam for this type of diving should be the same as for the commercial diver. That is, it should be done by a physician with special training in underwater medicine. The exams should be done prior to starting these types of diving activities and on a regular basis, at least every 5 years, thereafter. The exams, in addition to a comprehensive history, review of systems, and physical examination should include chest x-rays, blood chemistry panels, hemograms, audiograms, and possible x-rays of the major joints. This latter consideration is made for those divers who made deep and/or long dives that require decompression stops during ascent to ascertain that dysbaric osteonecosis of juxta- articular bone has not occurred. If it has, continuation of diving using compressed gases is not advised.
Female Divers and Pregnancy Considerations
Anatomical and physiological differences. About one third of SCUBA divers are females, as is the ratio for diving instructors. Physiological, anatomical, and psychological differences do exist between sexes. These differences are relatively minor, but they could become important in the underwater environment. The female body contains more fat tissue and less muscle. This fact puts female divers at higher risks for decompression sickness (DCS), but gives some theoretical advantage in cold water since fat serves as insulation. Generally, females have lower physical work capacity and stamina. This could become important in situations like swimming against strong currents or freeing themselves from entanglements.
Even though a third of divers are female, the ratio of females to male deaths in diving is 1 in 10.1 These differences may be explained by diving habits rather than anatomical or physiological differences from males. Females tend to select less dangerous or hazardous situations than men. We feel that for sport diving, female divers, after appropriate training, can reach the same level of performance as male divers. In some respects, females have selective advantages such as better tolerance to cold water, and because of their smaller size, more efficient use of their gas supplies.
Menstruation and Diving. There are 2 points that need to be discussed; 1) Psycholophysiological considerations; and 2) Menstrual blood as an attraction for sharks. Premenstrual and menstrual periods are associated with specific changes in the physiology of women. These changes may or may not have psychological components. They can produce a range of symptoms that affect physical performance and psychological responses. In general, the individual woman diver must decide whether she wants to dive during these times. However, the change of environment (psychological diversion), the buoyancy effects of water, and the relaxation that a well-conducted dive can provide, in our opinion outweighs the symptoms, in all but their severest forms, of the premenstrual syndrome and menstruation. From a physiological point of view blood loss during menses is almost never severe enough to cause hemodynamic changes. However, females may be at increased risk for developing DCS.2-4 These studies, while being suggestive, do not provide a physiological explanation for the increased risk for DCS in women divers.
There is no evidence that menstruation increases the likelihood of shark attacks in the female diver. In fact, Edmonds and colleagues report that female divers experience a much lower incidence of shark attacks than male divers.1 One hypothesis they use to explain this observation is that hemolyzed blood associated with menstruation may act as a shark deterrent.
Use of Oral Contraceptive Agents and Hormonal Replacement Therapy in Diving. Oral contraceptives have side effects. A significant one is the propensity for blood clotting. This causes increased risks for deep venous thrombosis, pulmonary embolism, cerebrovascular accidents, and myocardial infarction. However, there is no evidence that oral contraceptives increase the risk of DCS or other diving-related problems. Also we did not find any data about harmful effects of intrauterine devices and/or barrier methods of contraception for female divers. Although hormonal replacement therapy may reproduce some of the physiological effects of menstruation, we found no information on this subject in women divers.
Pregnancy and Diving. Most authorities in diving do not recommend SCUBA diving during pregnancy due to the unknown effects of increased partial pressures of nitrogen on the fetus and the increased propensity for nitrogen deposition in the fetal-maternal lipid tissues. This may make the fetus more susceptible to the harmful effects of bubbling phenomena than the pregnant mother.5 In addition, if the pregnant female requires hyperbaric oxygen recompression treatment for DCS, the increased partial pressures of oxygen may have teratogenic effects on the fetus as had been noted in animal studies.6 Consequently, we feel that snorkeling is OK during pregnancy, but SCUBA diving should be discontinued until after parturition.
Drugs and Diving
Drugs are associated with diving in 4 ways: 1) treatment of concurrent diseases; 2) prevention of MPD; 3) treatment of MPD; and 4) for "recreational" purposes.1,7 The actions of drugs may be altered under pressure such that the side effects that were acceptable on land in a resting person will become unacceptable in the underwater environment during diving and physical activity.8 When a diver is on a prescription drug, 2 problems must be solved. First, it is necessary to know why the patient requires the medication and does it have any contraindications for diving? Second, it is necessary to consider possible side effects of the drug, which could have an additive effect to the MPD. For example, drugs with sedative side effects will likely make the diver more susceptible to nitrogen narcosis. Drugs with stimulant effects may lower the threshold for oxygen toxicity.
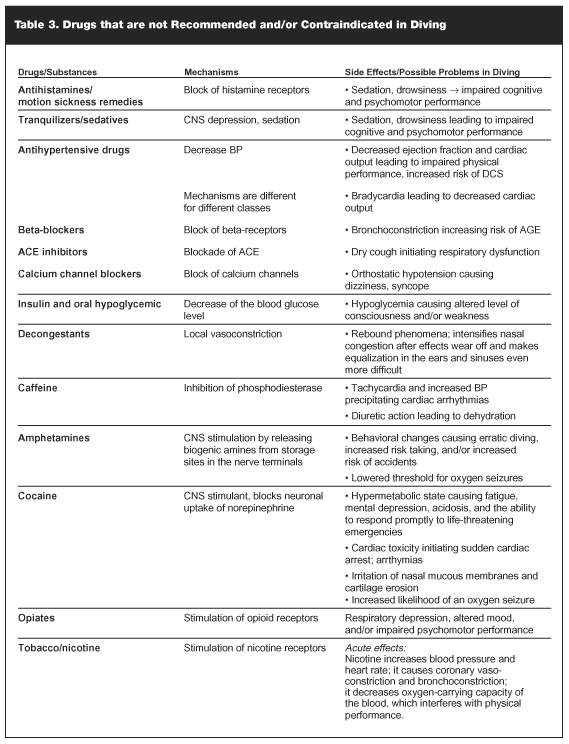
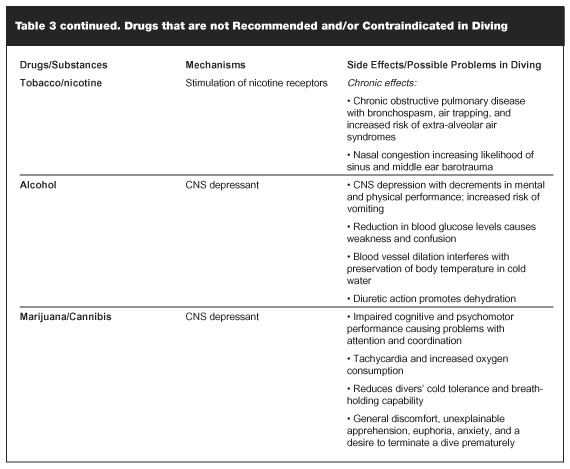
Divers may use "recreational" drugs, legally or illegally. Examples include tobacco, alcohol, amphetamines, cocaine, opiates and marijuana, and a number of other "designer" drugs. For diving purposes, these substances can be considered to have either "downer" (ie, depression) or "upper" (ie, stimulant) effects.9 A Los Angeles, Calif, coroner reported that 20% of diving deaths in Southern California were associated with the use of drugs.1 Alcohol intoxication has been implicated in 50% of drowning (including SCUBA divers’) deaths. When considering drugs and diving, appropriate decisions can be made as to whether the drugs are absolute or relative contraindications to diving based on their categories of action (see Table 3). In general, there is no place for drugs in diving. However, exceptions exist such as using vasoconstrictors to help with middle ear pressure equilibration and in the situations where the diver may be on a prescribed medication for a condition that could impose relative contraindications to diving.
 |
 |
Concluding Remarks
The information in this article should help the PCP add another dimension (ie, the primary care of the sports diver), to his or her practice. The extent of involvement may be haphazard, ie, the rare situation of caring for an established patient who develops a MPD, or proactive. The proactive approach is for the PCP to establish networks with diving certification agencies, sports diving clubs, hyperbaric units, and/or the Diver Alert Network and become known for his or her interest and willingness to provide care for the sports diver as well as doing diving physicals and medical certifications. This approach is analogous to the PCP becoming involved as a team physician.
Nothing gives the diver a greater sense of confidence in the physician who is performing his or her diving physical or managing the diving problem than to know that the physician is a diver also. There are many opportunities for the PCP to become an "expert" in undersea medicine. Many physician continuing medical education diving medicine courses (most with associated SCUBA diving activities) are conducted each year. Many are listed on the internet or in Pressure, a publication of the Undersea and Hyperbaric Medicine Society (UHMS, 10531 Metropolitan Ave, Kensington, MD 20895, Tel.: 301-942-2980; Fax: 301-942-7804; Internet: www.uhms.org; e-mail: [email protected]). For the most comprehensive training, the PCP should consider the annual NOAA (National Oceanographic and Atmospheric Administration) 2-week course held in Seattle, Wash. With completion of this course, the PCP will have training sufficient to manage all aspects of the MPD including those requiring use of the recompression chamber. Another alternative is for the PCP to take a 1-year fellowship in hyperbaric medicine. Upon completion of the fellowship and accompanying clinical experiences, the physician becomes eligible to obtain board certification in undersea medicine under the auspices of the American Board of Preventive Medicine.
We appreciate that the subject of diving medicine is much greater than can be presented in a single review article. Many excellent textbooks and review articles are available for those who desire additional information on this subject.10,11,1,12-16 However, we feel that our paper meets the 3 objectives stated in Part I and will provide the PCP a background for appropriately dealing with the sports divers in his or her practice.
References
1. Edmonds C, et al, eds. Diving and Subaquatic Medicine. Flagstaff, Ariz: Best Publishing; 2002.
2. Ruge FW. Relationship of menstrual history to altitude chamber decompression sickness. Aviat Space Environ Med. 1990;61:657-659.
3. Lee VM, et al. The menstrual cycle and decompression illness—What are the risks? Undersea Hyperb Med. 1998; 25;(Suppl):11.
4. Robertson AG. Decompression sickness risk in women. Undersea Biomed Res. 1992;19:216-217.
5. Camporesi EM. Diving and pregnancy. Semin Perinatol. 1996;20(4):292-302.
6. Ferm YH. Teratogenic effects of hyperbaric oxygen. Proc Soc Exp Biol Med. 1964;1116:975-976.
7. Harrison LJ. Drugs and diving. J Fla Med Assoc. 1992;79(3):165-167.
8. Rump AF, et al. Effects of hyperbaric and hyperoxic conditions on the disposition of drugs: Theoretical considerations and a review of the literature. Gen Pharmacol. 1999;32(1):127-133.
9. Groner-Strauss W, Strauss MB. Divers face special peril in use/abuse of drugs. Phys Sportsmed. 1976;4:30-36.
10. Melamed Y, et al. Medical problems associated with underwater diving. N Engl J Med. 1992;326:30-35.
11. Dick APK, Massy EW. Neurologic presentation of decompression sickness and air embolism in sport divers. Neurology. 1985;35:667-671.
12. Bennett PB, Elliot DH, eds. The Physiology and Medicine of Diving. 4th ed. Philadelphia, Pa: WB Saunders; 1993.
13. Bove AA, Davis JC, eds. Bove and Davis’ Diving Medicine. 3rd ed. Philadelphia, Pa: WB Saunders; 1997.
14. Joiner JT, ed. NOAA Diving Manual: Diving for Science and Technology. 4th ed. Washington DC: US Dept. of Commerce, National Oceanic and Atmospheric Administration; 2001.
15. Strauss MB, Borer RC, Jr. Diving medicine: Contemporary topics and their controversies. Am J Emerg Med. 2001;19(3):232-238.
16. US Navy Diving Manual. NAVSEA 09994-LP-001-9110. Flagstaff, Ariz: Best Publishing; 1993.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
