Patient Safety Alert
Tracking your medical errors just became a priority
President’s call for mandatory reporting system spurs search for solutions; Congress considers bill
Medical errors can no longer be dirty little secrets. The president, Congress and several federal regulatory agencies are working to turn your dirty laundry into national databases.
President Bill Clinton in February called for mandatory reporting of serious medical errors and set in motion regulatory reforms that will leave few places to hide. The first bill addressing medical errors was introduced in the Senate in early February, as well. From now on, you’re going to have to find a foolproof way to solve your adverse event problems.
The current reform movement started when the Institute of Medicine, a branch of the National Academy of Sciences, released its searing report, To Err is Human: Building a Better Health System, last November.
The report claims that medical errors kill between 44,000 and 98,000 people each year. It recommended sweeping changes, most of which the President incorporated into his plans. Here is what Clinton set in motion:
• A new Center for Quality Improvement and Patient Safety, funded with $20 million. The Center will fund research on patient safety; develop national goals; issue an annual report; promote the translation of research findings into improved practices and policies; and educate the public.
• This year, the Health Care Financing Administration will publish regulations requiring the more than 6,000 hospitals participating in Medicare to implement error reduction programs that include new systems to decrease medication errors.
• Also within one year, the Food and Drug Administration will develop new label standards to prevent common drug interaction problems and dosage errors.
• While 23 states (18 of which require hospital reporting) currently have mandatory reporting systems to track medical errors, the President’s plan will have a nationwide, state-based system in place within three years. When fully implemented, this system will require reporting of preventable medical errors that cause serious injury or death, and will encourage voluntary reporting of other medical errors and close calls. Information will be aggregated and made public.
• The National Quality Forum will develop a set of patient safety measurements that will serve as the basis for a uniform system of data collection. Then HCFA will launch a pilot project in up to 100 hospitals to help them implement confidential mandatory reporting systems.
The IOM report and the President’s proposals have galvanized large employers and managed care organizations to revamp the way medicine is practiced. "The public’s awareness and concern about the findings in the IOM report on patient safety continue to grow," asserts Donald M. Berwick, MD, president and CEO of the Institute for Healthcare Improvement in Boston. He was one of the 19 experts who worked on the report.
"Several Congressional committees are spotlighting the issues in hearings and many health care organizations are taking a serious look at how they can become much safer," Berwick adds.
The first of what is expected to be several bills dealing with medical errors was introduced February 8 by Senators Arlen Specter (R-PA) and Tom Harkin (D-IA). Their "Medical Error Reduction Act" calls for 15 separate demonstration projects to test how best to gather information on medical errors. Five of the projects would require that mistakes be reported and that those reports be kept confidential. Five would have voluntary reporting with information kept confidential, and five would have mandatory reporting with patients and families informed of medical mistakes made in their care.
Even before the IOM issued its report, and Clinton and Congress announced their proposals, the industry was working on solutions, notes Lou Diamond, MB, ChB, on the board of directors of the National Patient Safety Foundation (NPSF), an arm of the American Medical Association.
One initiative was born last December, when eight executives from some of the nation’s largest corporations, including General Electric and General Motors, formed an organization they call The Leapfrog Group. Its purpose is to encourage employers to look closely at the health care insurance companies they contract with for their employees and insist upon safe medicine.
"The initiative will require that hospitals put in place various types of safety programs," says Diamond. The group hasn’t dealt with specifics yet, but reporting systems will be a part of that, and decision support tools will be prominent in everyone’s mind. "Once this initiative takes hold, hospitals that make the fewest mistakes will attract the most patients and contracts," he says.
While many of the details of the President’s plans are still to be hammered out, it is obvious that hospitals will be required to implement error tracking and reporting systems. As these reports will be aggregated and the data disseminated by state and federal agencies, it is also apparent that the system will have to be automated.
So where are the adverse events tracking and reporting programs? While commercial vendors may respond with tailored programs once the need is clearly defined, if you are looking for a comprehensive program today, the list is short. To give you an idea of what such a program would be able to do for your facility, we’ve profiled two hospitals that use Safety-Centered Solutions Inc. software. (See "Two hospitals solve adverse events problems," below). Thomson Healthcare (parent company of American Health Consultants in Atlanta, the producer of this newsletter) created a strategic partnership with Safety-Centered Solutions in 1999. Because of this relationship, we’re able to describe some proprietary aspects of SCS’ program, and give you a better look at what these crucial decision support programs can do.
For more information, contact:
Donald M. Berwick, MD, president and CEO, Institute for Healthcare Improvement, Boston. Contact: (617) 754-4800.
Lou Diamond, MB, ChB, board of directors, National Patient Safety Foundation, Chicago, Illinois. Contact: (312) 464-4848.
Two hospitals solve adverse events problems
Program tracks individual events and trends
The 249-bed John D. Archbold Memorial Hospital in the small, south Georgia town of Thomasville, and the 424-bed University Community Hospital (UCH) in bustling Tampa, FL, have very little in common but similar types of adverse events and a similar approach to solving them.
Both had been experiencing long delays in their emergency departments (ED) a year or so ago. "When we looked at our baseline data, we saw exactly how long. We did some timeliness studies and made some changes, and immediately there was a decrease in wait times," says Kathy MacQuirter, RN, director of Quality Improvement, Risk Management, and Case Management at Archbold.
The staff at UCH analyzed its ED wait times, as well, and found that children and young adults with minor illnesses had been waiting at least six hours to be seen. Their solution: UCH created a separate express care unit. Staff is rewarded with bonuses if patients are treated within two hours.
At both Archbold and UCH, the staffs use a unique adverse event tracking and reporting software program called Excalibur Patient Safety Net. System users at each hospital say the program has prompted several changes in their systems that have substantially reduced medical error problems. Excalibur is medical errors analysis software marketed by Safety-Centered Solutions, Tampa, FL, and is comprised of eighteen clinical modules, among them Medication Errors, Adverse Drug Reactions, and Patient Falls. Safety-Centered Solutions tailors the system to meet the hospital’s needs by bundling or unbundling these modules and pricing accordingly by modules selected (e.g., medication safety or surgical events only).
Clinicians who discover an error or adverse event fill out a data collection form onscreen and describe what happened. The software organizes and summarizes the information so users can see how widespread problems are. Then Excalibur determines the resources, costs and time required to solve the problem. Reporters of mistakes can remain anonymous if they want to.
As long as the data entered is thorough, users of Excalibur can pull accurate reports relating to frequency, costs and continual trends of errors within a specified timeframe. The reports can be on any number of subjects, such as errors of omission or improper dosing, patient falls, bedsores or surgical accidents. The system, which tracks over 1,200 different types of adverse events, emphasizes gathering information and using it to develop better processes, and as such, it focuses on systems, not individuals.
"We knew we had to get on board with the software because a focus on safety is so important to an organization, especially now," MacQuirter says. Archbold administrators also envisioned the software as an excellent performance improvement tool that would "identify trends and fix the system and process problems instead of pointing fingers and naming names," she adds.
"You could shoot nurses forever and never discover that the real source of a problem is something like poor communication between units," reasons David S. Spencer, a former hospital administrator and CEO of Safety-Centered Solutions. "If you don’t look at all the events, you don’t have enough data to draw meaningful conclusions."
MacQuirter says the adverse events tracking and reporting software has helped Archbold identify a number of potentially dangerous tendencies, so clinicians could deal with them. As soon as the staff began working with the program more than a year ago, managers ran a number of baseline studies, looking at trends across the entire hospital.
"We started by creating a team on patient falls," MacQuirter says. "Falls were a high-risk area that we’d looked at before, but until we had this software, we didn’t have the ability to tie in with it any financial information. It makes more of an impact with data showing the cost of those falls." She says the people seeing the data are amazed at how much one fall can cost the hospital.
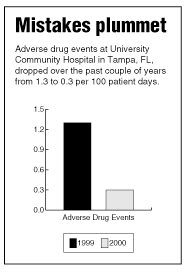 |
Victoria Rich, RN, PhD, vice president of patient services at UCH, and her colleagues take the problem of medical errors very seriously because their facility was the site of two highly publicized and unfortunate incidents over the past 10 years one where a patient died from an allergic reaction to a painkiller, which had been administered by mistake, and another where a patient had the wrong leg amputated. Since those errors took place, the institution has evolved into one that Rich says is open and honest. "We’ve turned this place around in terms of how we deal with medical errors," she says. "Now we understand that it’s the system that fails, not any individual."
"Culture is difficult to change," says Norm Stein, the CEO at UCH. "But once you do it, the result is a proactive organization that works very well." For example, adverse drug events went from 1.3 to 0.3 per 100 patient days. Before every surgery the staff now reviews the planned procedure aloud, "like pilots going over their checklist before a takeoff," says Rich. "It typically takes two minutes. We’ve caught 18 near-misses by doing that."
UCH personnel report errors and adverse incidents to a staffer assigned to log errors into Excalibur. Then four teams analyze the data in targeted areas and use what they find to bring about change. For example, a wound care team discovered a troubling rate of decubiti.
"We began monitoring wound care, specifically nosocomial stage 2 decubiti," says Rich. Rich’s team tracked stage 2 decubiti and found, through drilling down the data within the Excalibur program, that patients were contracting the sores mainly in the recovery room and in the ED.
"Patients used to have to lie on stretchers waiting for beds after surgery and in the ED," says Rich. "This year, every patient who’s waiting is put on a regular hospital bed rather than on a stretcher, and he’s turned every two hours, just as though he were an inpatient. It may seem to be a little thing, but it has a huge benefit."
That benefit translates directly to the hospital’s bottom line. "Bed sores are costly to any organization, and the system told us how much money we had spent on decubiti," says Rich. "If we didn’t have (the database), and had an increase in decubiti, we wouldn’t have looked at the fact that the skin breaks came from the patient’s point of entry. I probably would not have connected that the patients came in through the ED waiting for the bed. It’s a good find," says Rich.
Demanding zero tolerance
Archbold’s managers are mining their adverse events for similar savings. After tackling patient falls, MacQuirter’s staff at Archbold focused on medication errors, looking most closely at antibiotic omission during the transfer from the ED. "That’s where most errors were," she says.
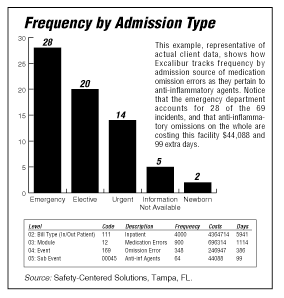 |
According to Almeda Simpson, RPh, the director of pharmacy services, Archbold is changing its procedures based on what the analysis found. "Our error rate is currently way below the national, but 1% is not good enough. We’re trying to get it to zero." After all, she says, would a 1% error rate be acceptable if it were your child?
As one of the newest generation of medical errors analysis and decision support program, Excalibur gets high marks for user friendliness. "We used to have a software program for tracking incident reports, but if you wanted to trend something, you’d have to create a report, then lay out the numbers on an Excel spreadsheet," says MacQuirter. Excalibur generates a report at the stroke of a few keys.
"I’m not a computer person," Rich says, "and I can do it. It takes three to four hours to learn and practice the system." She says the system follows the way your mind works.
"The managers and I have it on our own PCs," says Rich, "so we can drill down to a particular department and look at information in many different ways. If I get a hunch about a trend, I pull up the data to see if I’m right. As long as you put good, complete information in, you’re going to get good information back."
For more information, contact:
Kathy MacQuirter, director, Quality Improvement, Risk Management, and Case Management, John D. Archbold Memorial Hospital, Thomasville, GA. Contact: (912) 228-2767; [email protected].
Almeda Simpson, RPh, director of pharmacy services, John D. Archbold Memorial Hospital, Thomasville, GA. Contact: (912) 228-2000.
Victoria Rich, RN, PhD, vice president, patient services, University Community Hospital, Tampa, FL. Contact: (813) 972-7208.
David S. Spencer, CEO, Safety-Centered Solutions (www.scCARE.com), Tampa, FL. Contact: (877) 739-6751; (813) 626-0299, [email protected].
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
