Discharge Planning Advisor: ‘Everybody wins’ as CM, home health join forces
Discharge Planning Advisor: Everybody wins’ as CM, home health join forces
Looming JCAHO survey prompts affiliation
A couple of years ago, Lisa Zerull, RN, MS, the force behind the dramatically successful community nurse case management (CNCM) program at Valley Health System in Winchester, VA, faced a new challenge: She was informed by the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) that it would begin surveying the program based on the agency’s home care standards, in conjunction with the health system’s home health program.
"In the past, JCAHO hadn’t really looked at us," she says, adding she believes that may be the case with other, similar programs that simply aren’t on the accrediting body’s radar screen.
Not wanting to reinvent the wheel, Zerull went to Valley Health’s home health director and said, "How can we work with you to ensure a good survey?" Drawing on the policies and procedures and performance improvement process developed by director Patty Klinefelter during her 16 years in home health, Zerull says, "I just molded [them] to fit our program."
The home health program, Zerull notes, has received perfect scores in its two most recent JCAHO surveys.
The successful collaboration between the two entities, which for years had operated separately, began a discussion that ultimately led to a joining of forces, Zerull says, although that didn’t happen immediately.
"We started a dialogue, with the thought that we have so much to share, the opportunity to educate both sides on what we do," she notes.
"But in the initial dialogue, there were some turf issues." Home health personnel had the perception that the CNCMs were caring for patients who should have been under home health and were in effect providing free care for those patients, she says.
Finally, Zerull adds, "I said, OK, why don’t you screen, do the intake, and tell us who we can care for?’"
Because the two programs constituted "home and health services," it made sense to have one telephone number for physicians, emergency department clinicians, or hospital case managers to call to arrange care for their patients, she says.
Referrals to CNCM
"We drew upon one another’s expertise to come up with a plan that worked for both sides. It was better for home health to handle the central intake process to assure that the appropriate level of community care was being offered," Zerull adds.
The central intake system began in October 2000, Zerull notes, and JCAHO surveyed the programs in March 2001. The joint score was 99, she says, adding with a laugh that the point subtracted "was not because of us." It had to do with the incorrect labeling of a bag being used in home-administered chemotherapy.
With the advent of the central intake process, she notes, the percentage of patients referred to CNCM by way of home health has gone from 6% to 80%.
When the patient’s condition doesn’t meet home health criteria, he or she can be referred to the CNCM program, Zerull explains. "Home health is the acute model, and we’re the subacute model. We’re just valuing the level of care that each [program] brings."
The CNCM nurses "do nothing invasive," she adds. "The only two instances where we obtain a physician order is if we’re filling a pillbox and for pulse oximetry."
As patients’ care needs change, they may be traded back and forth between the two programs, Zerull notes.
"[Home health] may follow a patient for six weeks and then refer the patient to us. We may see them for three or four months and then they’re in the hospital and once again qualify for home health."
Future plans include having one nurse who can wear both hats, which would enhance the continuity of care, she says. "Relationship is one of the greatest predictors of wellness. If you have a socially isolated 80-year-old who is now dealing with a chronic illness, one of the bright spots in her life is that visit from a nurse case manager."
The idea is problematic from an administrative standpoint, however, she says. The CNCM nurses see their patients a maximum of once a week, and those visits are scheduled according to geographic area, she adds.
If a patient now needs to be seen three times a week, the nurse could find him- or herself driving back and forth between locations far removed from each other, Zerull says.
Combining the two programs has had many benefits, she points out. In addition to increased staff and patient satisfaction, physicians enjoy the advantage of being able to call only one telephone number or make one referral to arrange patient care, she adds.
Zerull was warned early on to "keep [the CNCM program] away from home health because it will confuse physicians," she says, but Valley Health staff take steps to make sure that is not a problem. "We educate them that when they write the order for home care, they write home and community services,’ and we determine the best level of care. Everybody wins with this solution."
The home health program now can make use of a CNCM innovation whereby the computer system flags the names of patients who are admitted to the hospital, Zerull notes.
"We get an automatic e-mail [regarding the admission], and we don’t make a wasted visit." she says.
The affiliation also has made possible a contingency staffing plan, she says. When one of the CNCM nurses was dealing with the possibility of taking time off to have open-heart surgery, "[home health] had nurses who could fill in," Zerull adds. "Before, we were it. We had to cover our own time."
Valley Health’s CNCM program began in 1992, when Zerull’s job was to coordinate acute-care case management, she says.
"The 16 case managers from the hospitals would come together as a team and say, We’re great at mobilizing patients through the system and doing discharge planning, but the chronic care patients keep coming back into the system.’"
Using as a model a Tucson, AZ, program that since has disbanded due to lack of funding, Zerull put together a proposal for CNCM and, to justify it, gathered data on patients who were high users of the system but weren’t homebound and so didn’t meet home health criteria.
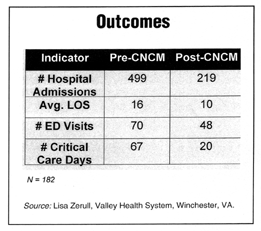
After the program was in place, figures showed, and continue to show, around a 50% reduction in emergency department (ED) visits, length of stay (LOS), and critical-care days, she says.
The CNCM program has continued to save money for Valley Health, a two-hospital system with a rural, tri-state service area, she says.
Each year, outcomes illustrate that the cost of seven to 10 home visits equals the cost of just one day’s hospital stay, Zerull says, not to mention the improvement in patients’ quality of life.
Looking at an actual patient known as "Joe," for example, records show that after participation in the CNCM program, the number of annual hospital admissions went from five to one, with average LOS reduced from 12 days to four days, she explains. The cost of Joe’s care went from about $120,000 to about $12,000. Noncompliant before, the patient now closely follows the prescribed regimen of care, including medications, diet, and exercise, Zerull adds.
Then there is the more intangible result of Joe changing from a "sick mindset" to the perception of a higher level of wellness, she says.
Despite such successes, Zerull reports little progress in her effort to have the Centers for Medicare & Medicaid Services — then known as HCFA — answer the question posed in the July 2000 issue of Discharge Planning Advisor: What if there were eight years of data (now 10 years of data) illustrating that it’s cheaper to pay per visit for community nursing care for the chronically ill than to pay for periodic acute care episodes at the hospital — and that patient outcomes are better, too?
Because programs such as Valley Health’s CNCM save money rather than make money, she points out, they probably will not get much support from chief executive officers.
If the nation’s hospital CEOs "can see the benefit of keeping people out of the hospital," the dynamics of health care can change, Zerull adds. "It’s a prevention mindset vs. an illness/treatment mindset."
If a chronically ill patient is in and out of the hospital, she says, "we’re saying that it’s too expensive to use critical care days. With Medicare, you get a set rate reimbursement, by DRG. That means, for example, for congestive heart failure, you’re getting $6,300, no matter how long the patient stays in the hospital."
To continue with the example of the chronic patient named Joe, Zerull explains, "If Joe comes in, is put on a ventilator, has four or five critical care days, and then goes home in 12 days, the system has to absorb the cost of care for anything over that $6,000."
The aim of the CNCM program is to teach such patients to go to the physician’s office or the ED before they’re in crisis, she adds, so that hospital stay might only be four days.

(For more information, contact:
- Lisa Zerull, Program Director, Community Nurse Case Management Program, Valley Health System, Winchester, VA. Web site: [email protected].)
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
