Screening for Ovarian Cancer: One
Screening for Ovarian Cancer: One "Scissor Step" Made
Abstract & Commentary
By Robert L. Coleman, MD, Professor, University of Texas; M.D. Anderson Cancer Center, Houston, is Associate Editor for OB/GYN Clinical Alert.
Dr. Coleman is a retained consultant for GlaxoSmithKline, Eli Lilly Co., Abbott Laboratories, Sanofi-Aventis, and Pfizer; and serves on the speakers bureau for OrthoBiotech.
Synopsis: First results of the UKCTOCS screening trial of postmenopausal women validates that the strategy of either ultrasound or multimodal screening (MMS) can identify women with early-stage ovarian cancer. The MMS strategy produced a substantially higher specificity, reducing the number of repeat screens and surgery. Impact on mortality is pending final analysis in 2014.
Source: Menon U, et al. Sensitivity and specificity of multimodal and ultrasound screening for ovarian cancer, and stage distribution of detected cancers: Results of the prevalence screen of the UK Collaborative Trial of Ovarian Cancer Screening (UKCTOCS). Lancet Oncol 2009;10:327-340.
Successful screening for ovarian cancer, the gynecologic malignancy with the highest case to fatality ratio, has been elusive due to the low prevalence of disease in the general population and the high cost for modalities needed to produce testing specificity acceptable for routine use. The UK Collaborative Trial of Ovarian Cancer Screening (UKCTOCS) was designed to definitively assess the effect of ovarian cancer screening on mortality, as well as, to comprehensively address the cost, acceptance, physical and psychosocial morbidity, and performance characteristics of multimodal screening (MMS) and ultrasound-based screening (USS).
Between 2001 and 2005, a total of 202,638 postmenopausal women aged 50-74 were randomly assigned to control (no screening), annual CA125 screening (based on risk of ovarian cancer [ROC] algorithm) and second-line ultrasound testing (MMS), or annual transvaginal USS alone in a 2:1:1 ratio. In the prevalence screen, 50,078 women (98.9%) underwent MMS and 48,230 (95.2%) underwent USS. Overall, 9% of the MMS cohort and 12% of the USS cohort required repeat testing. Surgery was undertaken in a small proportion of both cohorts, but was significantly more likely following USS. Ovarian neoplasms, benign and malignant, were identified in both screening cohorts.
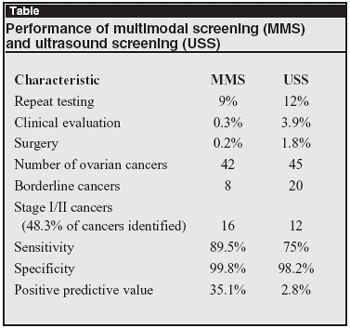
The proportion of stage I/II cases was 48.3% and was balanced between the two screening algorithms. However, specificity was significantly higher for the MMS (99.8%) strategy relative to USS (98.2%). The performance of both screening modalities is encouraging and establishes feasibility (see Table, below). The impact of stage migration following screening as reflected in disease-specific mortality is pending study completion, expected in 2014.
 Commentary
Commentary
Ovarian cancer continues to be the most lethal of the gynecologic malignancies, accounting for more annual deaths in the United States than all other gynecologic malignancies combined. The source of this statistic is inextricably linked to the disproportionate distribution of early- to late-stage disease at initial diagnosis.
The call for effective and acceptable screening has launched several large-scale population-based studies. UKCTOCS is by far the largest and most ambitious of these targeting postmenopausal asymptomatic women aged 50-74. While CA125, the only biomarker tested, and transvaginal ultrasound have been used in previous screening studies (see April 2009 issue of OB/GYN Clinical Alert), the utility of prespecified decision algorithms has enabled much better testing performance, particularly in the MMS cohort.
For instance, in this decision tree, CA125 drawn at baseline is entered into a patented risk assessment model that assigns a score determined as normal, intermediate, or high risk for ovarian cancer. Those that are normal are returned to annual surveillance with CA125 assessment. Those with intermediate risk scores were brought back in 12 weeks for a repeat test. A score based on these 2 values was then assigned and further work-up indicated if persistently intermediate or high risk. These individuals, as well as those with initial high-risk screens, underwent dedicated transvaginal ultrasound screening by 1 of 2 types of skilled ultrasonographers or physicians (depending on risk and interpretability of the initial scan). Abnormal screens were referred for clinical assessment and physician judgment determined the next intervention, including surgical evaluation.
This initial report of the prevalence data is very encouraging, and suggests such a strategy is feasible in the asymptomatic general population. The migration in stage to almost 50% of cancers identified in both screening cohorts as stage I/II is desired and provocative, even though a clear reference point was not provided (control group) and the ultimate impact of that stage migration, mortality, is immature. However, one of the central tenets of screening is cost-effectiveness, particularly in diseases of low prevalence such as ovarian cancer. This highly subsidized clinical trial is unlikely to be cheap enough in many countries around the world to enable widespread adoption. Nevertheless, the "effectiveness" of screening must be clearly delineated, as the balance of the economic impact of such a health care program or policy on years of life gained will surely be the focus of debate.
Suggested Readings
- Partridge E, et al; PLCO Project Team. Results from four rounds of ovarian cancer screening in a randomized trial. Obstet Gynecol 2009;113:775-782.
- Mills GB, et al. Future for ovarian cancer screening: Novel markers from emerging technologies of transcriptional profiling and proteomics. J Natl Cancer Inst 2001;93:1437-1439.
- Van Nagell JR Jr, et al. Ovarian cancer screening in asymptomatic postmenopausal women by transvaginal sonography. Cancer 1991;68:458-462.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
