Diagnosis and Emergency Department Management of Urologic Emergencies in the Male Patient: Part I
Diagnosis and Emergency Department Management of Urologic Emergencies in the Male Patient
Part I: Scrotal Disorders
Authors: Gary D. Hals, MD, PhD, Attending Physician, Department of Emergency Medicine, Palmetto Richland Memorial Hospital, Columbia, SC; Tom Dietrich, MD, Resident Physician, Palmetto Richland Memorial Hospital, Columbia, SC; and David Ford, MD, Attending Physician, Department of Emergency Medicine, Palmetto Richland Memorial Hospital, Columbia, SC.
Peer Reviewers: William B. Ignatoff, MD, Emergency Physician, Emergency Room Associates, Carondelet Health Network, St. Joseph’s and St. Mary’s Hospitals, Tucson, AZ; and Brooks F. Bock, MD, FACEP, Dayanandan Professor and Chair, Department of Emergency Medicine, Wayne State University, Detroit Receiving Hospital, Detroit, MI.
Urologic emergencies present formidable challenges to diagnosis and management. Consider the following case studies:
• A 14-year-old male presents to the emergency department (ED) with complaints of testicular pain upon awakening that morning. He has had several episodes of similar pain that resolved spontaneously in the past, but this time the pain is persisting.
• A 23-year-old man complains of three days of painful urination and a swollen testicle.
The diagnoses for the patients above—testicular torsion and acute epididymitis, respectively—share a common thread. They are variations of acute urological emergencies that need proper recognition and treatment from the emergency physician.
The problem with urologic emergencies, specifically the acute scrotum, is that providing proper recognition and treatment is not always straightforward. In up to 90% of cases of acute scrotal pain, the diagnosis will be divided between testicular torsion, appendage torsion, and acute epididymitis. A summary of data from 17 papers, encompassing 3021 patients of all ages, shows the diagnoses divided roughly evenly among the three disorders.1 Progression of time often expands the degree of overlap between history and physical exam with these disorders. Changing one of the cases mentioned above illustrates the dilemma a physician can face: an unclear picture, fraught with potential misdiagnosis. A 20-year-old man presents with six hours of testicular swelling, painful urination, fever, and vomiting. Fever and urinary symptoms suggest epididymitis, but the acute presentation and vomiting suggest torsion. The diagnosis now is much more uncertain, but critical time already has passed if the patient has testicular torsion. Testicular salvage is inversely proportional to duration of ischemia, and salvage rates drop after six hours to less than 70% .2 The emergency physician now is between the proverbial rock and hard place. Should the urologist be consulted immediately? Or should an imaging study be ordered first? If so, which one? No physician can make the correct decision every time, but awareness of the features of epididymitis and testicular torsion, along with the most recent recommendations from the literature, can make choosing the correct approach more a matter of skill than luck. Taking every patient directly to surgery for exploration and treatment is no longer the recommended course for every case of acute scrotal pain.1 It is reserved for those patients with strong clinical presentations suggesting torsion. Thus, the burden rests on the shoulders of the emergency physician to sort patients out. The emergency physician rapidly and efficiently must determine which patients require surgical care and which safely can be treated and released.
When males present to the ED with complaints of acute genital pain, they often are anxious for rapid pain relief and quick resolution of the problem. While urological consultants ultimately will perform in-depth management of some patients, in many cases the emergency physician may be able to resolve the problem. This two-part article reviews the disorders that prompt emergent presentation for urological evaluation, and discusses their treatment. Imaging techniques have advanced remarkably over the last decade, and the application of these new modalities in the evaluation of urological emergencies also will be discussed. Renal calculi and urinary tract infections have been covered in recent issues of Emergency Medicine Reports; therefore, these topics will not be discussed in detail in this article.—The Editor
Male Urologic Examination
Proper physical examination can be very helpful in diagnosis of urological emergencies. Using the same standard approach to examine each patient will help ensure that no aspect of the exam is overlooked and that all pertinent structures are evaluated on each patient. Adequate lighting is a prerequisite, and a warm exam room will help ensure the scrotum is not contracted, hindering the examination. Begin with visual inspection. If uncircumcised, the foreskin should be retracted for complete examination of the glans. The presence of ulcerations will be a sign of sexually transmitted diseases (STDs) such as syphilis, chancroid, or herpes. The location of the meatus also should be noted. In hypospadias (ventral opening), the urethral orifice often may be stenotic to the point of being symptomatic. A mass in the scrotum may be transilluminated with a strong light in a darkened room. Hydroceles will transmit light and appear red, whereas solid masses (tumors) will not pass light. When a new hydrocele is diagnosed in a patient between the ages of 18 and 35 years, it is important to remember that 10% of tumors will be associated with a secondary hydrocele and urologic follow-up should be arranged for further evaluation. Absence of a testis from the scrotum may indicate cryptorchidism or an undescended testicle. Again, cancer risk is increased in these patients and urologic referral is indicated.
The testes should be palpated carefully with the fingers. Any nodularity or asymmetric firmness is abnormal and indicates a possible neoplasm. The epididymis is located on the posterior aspect of the testicle, and normally is somewhat painful to palpation. However, when acutely inflamed, the epididymis will not be distinguishable from the testicle. Have the patient stand and re-examine the testicles to determine if they are aligned on a horizontal axis. Normally, testicles align vertically, and horizontal lie is a risk factor for torsion.
The normal prostate is heart-shaped, with the apex located distally. Before examining the prostate gland, it is prudent to collect a urine specimen for routine urinalysis. This is important since prostatic palpation or massage may force prostatic secretions into the posterior urethra, contaminating the urine. Actually, while prostatic massage used to be a mainstay of examination, present thinking is that the acutely inflamed prostate should not be massaged. This is due to the possibility of precipitating bacteremia3 and to the incredible pain caused by massaging the acutely infected prostate. To facilitate complete examination of the prostate, the patient should lean over the examination table in such a way that his body is horizontal with respect to the table, with his feet about shoulder width apart and his legs straight. Slowly insert the index finger into the rectum and contact the prostate gland after about 4-5 cm of insertion. One should try to distinguish tenderness of the gland itself from normal discomfort associated with the exam. The prostate normally has the consistency of the tip of the nose, while cancerous nodules feel more like the bony area of the chin. Most cancer tends to arise in the lateral areas of the prostate. The average prostate is about 4 cm in length and width. It is important to note that the severity of prostatic hypertrophy is measured by the amount of residual urine and the severity of symptoms, rather than by the size of the gland on digital palpation. It may be of normal size when measured by digital palpation, even in the presence of severe hypertrophy with acute urinary retention. Finally, the inguinal canals should be examined for enlarged lymph nodes or the presence of hernias.
Scrotal Disorders
Anatomy. The scrotum is a sac composed of the following components (listed from the surface inward): loose skin, dartos muscle, external spermatic fascia or Colles’ fascia, cremasteric muscle, internal spermatic fascia, and the tunica vaginalis. (See Figure 1.) The dartos muscle is a thin muscle that shrinks the scrotum in size when contracted. The external spermatic fascia is a continuation of the external oblique aponeurosis, and the cremasteric muscle is a continuation of the internal oblique. It serves to elevate the testicle and one side of the scrotum when contracted. The tunica vaginalis is the actual covering of the testicle, and normally anchors it to the posterior wall of the scrotum. The testes are anchored inferiorly to the scrotum by the scrotal ligament (gubernaculum). Inappropriately high attachment of the tunica vaginalis, termed a "bell-clapper deformity," allows the testicle to rotate freely on the spermatic cord within the tunica vaginalis. Rotation leading to decreased blood supply and ischemia of the testicle is the basis of testicular torsion.
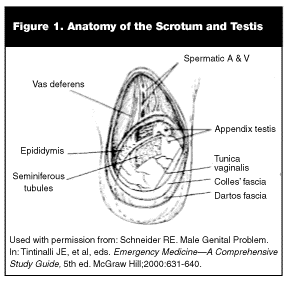 |
Each testicle is 4-6 cm in length and 3-4 cm in width. The epididymis is attached directly to the posterolateral aspect of the testicle. Its function is to allow storage and maturation of sperm. The appendix testis and appendix epididymis are vestigial structures that serve no known physiologic function. When present, the appendix testis is attached to the superior pole of the testicle. The appendix epididymis can be found at the head of the epididymis. Both of these structures can undergo torsion, prompting the patient to present with symptoms of an acute scrotum. The vas deferens extends from the tail of the epididymis upward into the spermatic cord, where it joins the seminal vesicles and attaches to the prostatic urethra. On testicular exam, the vas deferens is easily palpable as a separate muscular tube.
The Acute Scrotum. Acute scrotal pain is responsible for approximately 0.5% of total ED visits.4 These patients may have truly emergent conditions and require prompt attention by the emergency physician. The urgency in diagnosis and treatment of these patients stems from the time constraints of attempting testicular salvage in cases of testicular torsion, as described in the following section. Taken together, appendage torsion, testicular torsion, and acute epididymitis account for 85-90% of all final diagnoses in presentation of an acute scrotum.1 Although torsion is a primary concern, testicular torsion will be the ultimate diagnosis in only 25% of patients with acute scrotal pain.4 Thus the dilemma: Testicular torsion will be in the differential of nearly every patient presenting with an acute scrotum, but will be the final diagnosis in only 25% of these patients. The treatment for testicular torsion is early, rapid, surgical intervention, while for epididymitis and appendage torsion the treatment is medical.
Although testicular torsion is a primary concern, the other causes of acute scrotal pain are numerous and include torsion of the appendices testis, epididymitis, epidydymo-orchitis, renal colic, trauma, hydrocele, varicocele, testicular cancer, hernia, and Henoch-Schonlein purpura (HSP) in children. (See Table 1.)
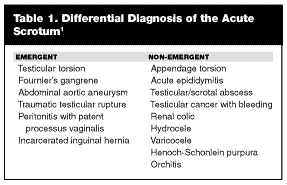 |
Hernias and HSP will not be discussed in detail, but the following points should be made. Inguinal hernias may present as acute scrotal swelling, resulting from protrusion of abdominal contents into the scrotum (via a patent processus vaginalis). Scrotal exam reveals a mass with normal testicles. Incarceration and strangulation can produce significant scrotal swelling and pain that may confuse the physical exam. Often the history of long-standing hernia will be given, but if uncertain, scrotal ultrasound should show normal testicles with a scrotal mass. In HSP, up to 15% of boys will have scrotal complaints. HSP is a multisystem vasculitis, and scrotal involvement without other systemic findings (rash, colicky abdominal pain, arthralgias, and hematuria) is rare. If in doubt, ultrasound findings in HSP are an enlarged epididymis, hydrocele, and thickened scrotal skin with normal testicles.5 One study of 93 children with HSP found that of the 24% with scrotal involvement, 36% of them had surgery for suspected torsion with no findings of testicular torsion.6 The authors suggest that use of ultrasound in these cases likely would have prevented many unnecessary surgeries.
Systemic problems can cause acute scrotal pain, including symptomatic abdominal aortic aneurysm (AAA) and peritonitis from trauma or infection. Anyone older than age 50 with risk factors for AAA should be evaluated (i.e., abdominal ultrasound) to rule out a symptomatic aneurysm as the cause of scrotal pain, unless another cause is evident. Case reports exist of blood or pus traveling into the scrotum through a patent processus vaginalis, with acute scrotal pain misleading the physician about the true nature of the problem.7 The following sections will discuss the various causes of acute scrotal pain/mass. It is important to remember from the outset that acute scrotal pain should be considered testicular torsion until proven otherwise, especially when the patient is near puberty.
Differentiation of Testicular Torsion from Epididymitis
Testicular torsion and acute epididymitis together are the most common causes of the acute scrotum, and ultimately are the final diagnosis in up to 75% of presentations of acute scrotal mass.3 Epididymitis is the most common entity confused with testicular torsion, and a study of relevant malpractice claims found that in 61% of these cases, torsion was misdiagnosed as epididymitis.8 Differentiation of testicular torsion from epididymitis can be difficult, and misdiagnosis rates are as high as 50%, based on clinical impression from physical exam.9 Table 2 summarizes some features that may be helpful in distinguishing the two entities. Several features of each disorder can be helpful in suggesting one diagnosis or the other, but imaging to rule out torsion always should be undertaken. Epididymitis is much less common than torsion in the pre-adolescent, with the average age of presentation in epididymitis being 25 years, compared to 14 years in torsion.3 Symptoms of urethritis can precede epididymitis, but do not in every case. Pain from torsion usually is sudden in onset, peaking in hours, or noticed upon awakening in the morning, while the pain of epididymitis is more gradual, peaking in days. Both processes produce scrotal pain and edema and may make the detection of a horizontal testis difficult. Up to 95% of cases of epididymitis will present with fever, where only 20% of patients with torsion have fever.3 Evidence of urinary tract infection (white blood cells [WBCs] and bacteria in the urine) suggests epididymitis but is not diagnostic, as this finding may be absent in up to 50% of cases of epididymitis.3 Keep in mind that acute epididymitis is the No.1 misdiagnosis of testicular torsion, and if doubt on the diagnosis persists, surgical exploration is the treatment of choice.
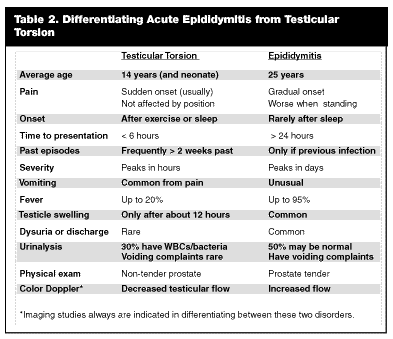 |
Testicular Torsion. Testicular torsion is a true urologic emergency, with surgical intervention being the only definitive treatment. Testicular torsion has an annual incidence of 1 in 4000 males younger than age 25.10 It is primarily a disease of men younger than age 30, although the reported range is from newborn to 78 years.1 The highest incidence is around puberty, at ages 12-15 years, with the peak occurring at age 14. One needs to remember that there is also a second, smaller peak in incidence in the first year of life. More importantly, presentation of an acute scrotum in the first year of life is much more likely to be due to testicular torsion than presentation as an adult. Up to 80% of these young patients will have testicular torsion,11 and the majority of them will have a non-viable testicle. Any young child younger than age 1 with an acute scrotum should have immediate urologic consultation.
The pathological basis for torsion is the "bell-clapper deformity." (See Figure 2A.) This defect is not rare, and has been shown to be present in 12% of asymptomatic men.12 The normal testicle descends into the scrotum during development through an outpouching of the peritoneum, the processus vaginalis. Normally, the testicle is anchored to the posterior wall of the scrotum, preventing rotation of the testicle within the scrotum. The bell-clapper deformity is an inappropriately high attachment of the tunica vaginalis, which allows the testicle to rotate inside the scrotum around the spermatic cord. This type of torsion is called intravaginal, as the testicle is rotating inside the processus vaginalis, whereas neonatal torsion is extravaginal, as the tunica vaginalis and the testicle both rotate around the spermatic cord. The volume of each testicle increases by 5-6 times during puberty, accounting for the increased risk of torsion in this age range. Twisting of the spermatic cord first causes venous congestion, followed by arterial compromise and ischemia. The spermatogenic cells of the seminiferous tubules are more sensitive to ischemia than the endocrine-producing Leydig cells. Thus, "saving" the testicle still can result in loss of sperm production on the affected side.
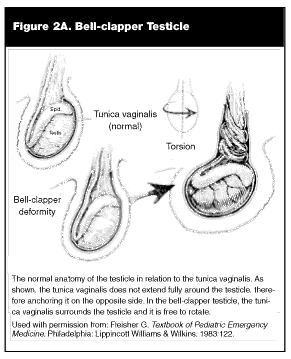 |
The direct and feared complication of torsion is the theoretically preventable loss of the affected testicle. Testicular salvage rate is approximately 50% overall, but varies widely, depending on the time to treatment. Rates up to 80-100% are reported in those treated within 4-6 hours of onset of symptoms, and fall to 20% if corrected in 24 hours.13 After 24-48 hours, testicular salvage is not possible.11 As with other diseases in which delays in treatment directly are correlated with patient outcome (appendicitis, myocardial infarction, etc.), a clear path has been laid for lawyers to follow when one fails to diagnose testicular torsion. One study of claims against urologists found that 74% of cases reviewed were filed for misdiagnosis, with acute epididymitis being the most common misdiagnosis (61%).8
The clinical diagnosis of testicular torsion is fraught with pitfalls. Torsion even has been reported in patients after orchiopexy designed to prevent repeat episodes.14 Presumably, this results from degradation over time of absorbable sutures. Diagnosis of testicular torsion by history and physical alone is of limited value, as there is a wide variety of presentations and no pathognomonic signs. The classic history is sudden onset of severe, constant, unilateral testicular pain. Atypical presentations are not rare, with patients reporting slow onset of pain in up to 25% of cases,15 or intermittent and stuttering pain. An important clue is that nearly 41% of patients report a history of previous similar pain that resolved spontaneously.9 The onset of pain can be correlated with mild physical exercise, trauma, or sexual activity, but many patients report pain upon awakening as well. The history of trauma is present in up to 20% of cases,16 and can mislead the physician into thinking the testicle is only "bruised."17 A red and inflamed scrotum may mimic an infectious etiology. Systemic symptoms are common in patients with torsion. Nausea, vomiting, and abdominal pain are seen in 20-30% of cases; 16% report fever; and urinary frequency is seen in 4%.18 One study demonstrated a positive predictive value of nausea and vomiting of 96% and 98%, respectively, in patients with suspected torsion,16 but the sensitivity of nausea and vomiting was only 69% and 60%, respectively. The important point is that vomiting is rare in acute epididymitis, but common in torsion. Furthermore, instead of sudden onset, the pain may be inguinal or lower abdominal in location and may be gradual in onset in up to 25% of patients.15 A rare but important case is torsion of an undescended (abdominal) testicle. Only 60 cases have been reported,19 and 66% involved testicular cancer (seminoma). This entity should be considered in the case of a male with abdominal pain and history of untreated undescended testicle.20
Physical exam alone is extremely unreliable, and misdiagnosis rates can be as high as 50% when based solely on physical exam.9 Classical findings include an elevated testicle, larger and with horizontal position compared to the other side. (See Figure 2B.)
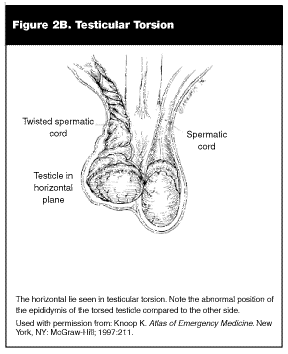 |
The left side is affected more often than the right, 2.5:1 in one series of 62 cases of testicular torsion.21 This may be due to the left side having a slightly longer spermatic cord. Swelling is common in epididymitis, but usually only seen in torsion after 12 hours have passed. Bilateral torsion occurs more commonly in the neonate, but is rare in the adult. Horizontal lie of a testicle can be difficult to appreciate at times, but palpation of the epididymis can help, as it lies along the long axis of the testicle. Thus, on a horizontal testicle, the epididymis will be horizontal in position. An abnormal axis of the unaffected testis (i.e., evidence of bell-clapper deformity) also is suggestive of torsion. One should remember that the testicle can torse 360-720°; therefore, horizontal lie or abnormal position of the epididymis may not be present. Some authors report absence of the cremasteric reflex (elevation greater than 0.5 cm of ipsilateral testis when the inner thigh is stroked) as having a 99% association with testicular torsion.22 While absence certainly would suggest torsion, case reports exist in which torsion is proved with the reflex still present.23 The entire testicle should be tender, as opposed to tenderness in the epididymis in epididymitis or tenderness of the upper pole in torsed appendage. As the pain is due to ischemia of the testicle, it should not be positional. Prehn’s sign, relief of discomfort with elevation of the testicle, supports the diagnosis of epididymitis but is in no way exclusionary of torsion. After 24 hours, the scrotal appearance of testicular torsion may be identical to that of epididymitis and appendiceal torsion.
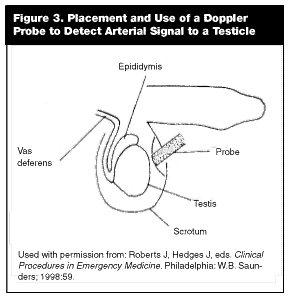
Laboratory evaluation may help suggest epididymitis as a cause, as the urinalysis classically is negative in torsion. However, leukocytosis and pyuria have been reported in up to 30% of cases of torsion, and one report documents several cases of missed torsion secondary to reliance on these data.11 Likewise, the complete blood count will show an elevated WBC count in 60% of cases of torsion. Imaging studies are thus the mainstay of evaluation for possible torsion. A crude measure of testicular blood flow is done with a handheld Doppler probe (normally used to detect pulses). (See Figure 3.) Placing the probe over the normal testicle should allow detection of an arterial pulse. Compression of that testicle’s spermatic cord and artery should block the signal, and can be useful if questions on the source of the signal exist. The flow signal should be absent on the torsed side. Again, this is a crude measure, but if no pulse is detected, it may prompt more urgent urologic consultation. Reappearance of the flow signal and pain relief can be established as goals in manual detorsion.
 |
While imaging studies in patients with suspected testicular torsion have been shown to be highly specific and sensitive, their true use is in patients who present with equivocal exams and histories. Surgical exploration remains the "gold standard" for diagnosis and treatment of testicular torsion when doubt exists. Of the two standard tests, most authors recommend color Doppler ultrasound over radionuclide scanning. Although radionuclide scanning is 94% sensitive and 100% specific, it is limited by interpretation. In addition, the test takes 30 minutes to perform, not including preparation time of the radioisotopes, therefore delaying diagnosis and placing the testicle in jeopardy. Color flow Doppler has a sensitivity of 82-100% and a specificity of 100%, and ED-performed sensitivity and specificity of 95% and 94%, respectively.24,25 While ultrasound evaluation has proven to be a quick, noninvasive, and accurate way of evaluating the acute scrotum, the downside of scrotal ultrasound is that, when performed on very small testicles (neonatal or prepubescent patients), adequate flow may not be demonstrable. However, one study of 65 boys (ages 1-16 years) with acute scrotal pain suggested that ultrasound was still accurate with a sensitivity of 100% and positive predictive value of 73%.26 Furthermore, one needs to keep in mind that the testicle may spontaneously detorse before the exam, yielding a normal study in a patient still at risk for further episodes of torsion. Cases of intermittent torsion that are not detected by ultrasound also have been described.27 The best role for ultrasound appears to be for ruling out torsion when normal flow is detected.28 Otherwise, a non-diagnostic study is an indication for surgical exploration to establish a clear diagnosis.
A new approach recently described makes use of serum markers as an aid in diagnosis of testicular torsion. Interleukin-6 (IL-6) serum levels were compared in a study of 25 patients presenting with an acute scrotum.29 Of the 25 patients, the breakdown of the final diagnoses was: 11 testicular torsions, 10 cases of epididymitis, three appendix torsions, and one varicocele. The authors found that IL-6 levels were elevated significantly in epididymitis compared to testicular torsion. Although limited by a small sample size, advances in serum markers may prove helpful in the future for a laboratory test that may help differentiate testicular torsion from epididymitis. Another serum marker currently being tested is C-reactive protein (CRP). CRP has been shown in 104 patients with acute scrotal pain to be useful to differentiate inflammatory conditions (i.e., epididymitis) from testicular torsion.30 Further study may establish this marker as a useful adjunct in evaluation of scrotal pain.
When a patient has a compelling history and exam, imaging studies are not warranted, as they may only delay definitive treatment and emergent surgical exploration. As the treatment for testicular torsion is urgent surgical exploration and orchipexy, and since time is of the essence, urologic consultation is advised as soon as the diagnosis is suspected. This provides the urologist with the option of taking the patient directly to surgery to avoid the delay of imaging studies that may not be necessary. Even though imaging studies can be very helpful in some cases, in others the results are equivocal and only serve to delay treatment. At least one author recommended, after a review of 99 patients over a five-year period, that patients with a strong suspicion be taken directly to surgery, as lab tests or imaging studies did not aid in the diagnosis of these patients.31 Likewise, early consultation allows the consultant to be involved in choices of timing and type of analgesia.
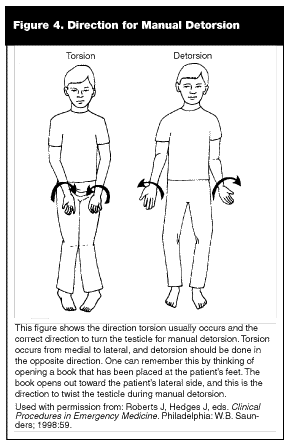
Whether immediate surgical exploration is pending or imaging is to be performed, there are no contraindications to attempting to manually detorse the testicle.32 One needs to remember that this is a temporizing procedure, not a definitive treatment. In most cases of torsion, the testicle twists toward the midline, and one detorses the testicle by twisting it back in the opposite direction. The concept of "opening a book" while standing at the patient’s feet is used to help remember the direction to turn the testicle. (See Figure 4.) One should rotate the testicle 180° at a time, with pain relief (and return of Doppler flow signal) as the goal. Manual detorsion has a variable success rate, reported in the past as 30-70%, but a recent study of 17 patients found a 82% success rate.33 In addition, the affected testicle can be "therapeutically cooled" by packing in ice surrounded by a towel to protect the skin from frostbite. This technique has been shown to preserve testicular function in animals up to 90% at six hours.34
 |
Acute Epididymitis. Acute infection and inflammation of the epididymis is responsible for more than 600,000 physician visits yearly.41 Overall acute epididymitis is one of the most common diagnoses in acute scrotum cases, with some authors estimating that epididymitis causes 75% of these cases.11 The peak incidence of epididymitis, like testicular torsion, is bimodal. A smaller peak occurs around age 2, and a larger peak incidence is seen in individuals 19-35 years of age. Both peaks correspond to peaks in incidence of genitourinary infection. Common complications of acute epididymitis include scrotal/testicular abscess formation, impaired fertility, and even sterility in cases of severe bilateral scarring (10% of acute epididymitis is bilateral). In adults, epididymitis results from retrograde spread of bacteria from the urethra and bladder, whereas in children it is frequently refluxed urine secondary to an underlying anatomic abnormality that produces epididymitis. One study demonstrated that 39% of children with epididymitis had underlying anatomic pathology.11 This high degree of anatomic defects calls for referral of all infants and young children with epididymitis for a genitourinary ultrasound.36 In sexually active adolescents to 35-year-olds, Chlamydia trachomatis and Neisseria gonorrhea are the main causes of epididymitis, with Chlamydia being the predominant pathogen in this age group.37 In the homosexual patient, coliforms play an important role, and fungal infection should be considered as well as syphilic epididymitis.38 In the older patient (older than 35 years) the causal organisms are usual urinary pathogens, including Klebsiella, Pseudomonas, and Escherichia coli, with E. coli being responsible for 80% of cases.37 The elderly patient may have a history of recent urinary instrumentation, and there is a high incidence of underlying urologic pathology (i.e., prostatic hypertrophy). Other causes have been implicated in epididymitis including tuberculous epididymitis, which often is the presenting symptom of renal tuberculosis, and chronic use of amiodarone. Epididymitis occurs in 3-11% of patients on the drug, and only responds to discontinuation or reduction of dosage.39
Infection or inflammation of the epididymis classically presents as a gradual onset of scrotal or testicular pain, frequently associated with dysuria, urinary frequency, fevers, edema, and erythema of the overlying scrotum. The onset of pain typically is more gradual than with testicular torsion, with the peak pain being felt over 24 hours rather than minutes. Patients may have lower abdominal pain and/or flank pain. Although voiding complaints are much more common in epididymitis than torsion, only 10% will have penile discharge. Vomiting is rare with epididymitis, but is more common in torsion. Physical exam, when done early in the course, will reveal a tender epididymis without significant testicular involvement. When advanced, the epididymis will adhere to the testicle and may result in epididymo-orchitis, which often is indistinguishable from testicular torsion. Reactive hydroceles also can form, impairing the physician’s ability to differentiate a tender epididymis from a tender testicle. Prehn’s sign, or relief of pain with scrotal elevation, or the opposite sign of worsening pain with standing, is supposed to help distinguish epididymitis from torsion. The basis is that the pain in torsion is from ischemia and should not be relieved by scrotal elevation. In practice though, one should not rely upon this to differentiate the two disorders. Likewise, the patient with acute epididymitis should retain his cremasteric reflex (classically absent in torsion), but this, too, is unreliable for decision-making in every case. Since the origin of epididymitis is from an ascending infection (urethra toward epididymis), patients theoretically also may have prostatitis and tenderness on exam.
Laboratory tests indicated in patients with suspected epididymitis include urinalysis, urethral swab or culture of urethral discharge, Gram stain of discharge, human immunodeficiency virus (HIV), and syphilis tests in sexually active patients. Classically, patients with acute epididymitis should have pyuria with or without bacteriuria, whereas patients with torsion should have no sign of infection in their urine. However, exceptions to this are well reported, with one study demonstrating that 78% of children with epididymitis had a normal urinalysis.36 Another study reported 24% of patients with testicular torsion had pyuria.40 WBC counts are not useful, as they are abnormal in up to 50% of patients with testicular torsion.41 Color flow Doppler is recommended, as it will demonstrate increased echogenicity secondary to testicular edema in both orchitis and testicular torsion; it will show increased flow to the affected testicle in epididymitis (and orchitis), whereas torsion will show decreased or absent flow.25 Orchitis, inflammation and/or infection of the testicle, can follow from untreated epididymitis. As it is an extension of epididymitis, the same pathogens are responsible, with Chlamydia, N. gonorrhea, E. coli, Klebsiella, and Pseudomonas being the most common.42
Treatment of acute epididymitis requires urgent urologic consultation if one is unable to exclude testicular torsion. Once the diagnosis of epididymitis is established, inpatient management should be considered for patients with suspected testicular/scrotal abscess or systemic toxicity (fever, elevated WBC count, vomiting, etc.). The consultant can select intravenous antibiotics or begin treatment with fluroquinolones to cover the common causes of infection. Outpatient treatment of epididymitis and epididymo-orchitis is aimed at the major pathogens suspected for each age group. Care should be taken to be aware of the incidence of antibiotic resistance in one’s area of practice, as incidences vary widely. In the sexually active patient, from adolescence through 35 years, treatment should be aimed at Chlamydia and N. gonorrhea. Empirically, ofloxacin 300 mg PO bid for 10-21 days may be given; alternatively one dose of ceftriaxone 250 mg IM followed by doxycycline 100 mg PO bid for 10 days, or ceftriaxone and 1 gram of azithromycin, can be used if compliance is an issue.37
Sexual partners should be tested, and the practice of safe sex should be encouraged to prevent recurrence. In patients older than age 35, antibiotic therapy is aimed at the urinary pathogens E. coli, Klebsiella and Pseudomonas, and should be guided by urinalysis and culture. Ofloxacin 200 mg PO bid or ciprofloxacin 500 mg PO bid provide excellent coverage and should be taken for 10-21 days.37 Epididymitis in infants necessitates further work-up for an underlying cause (i.e., septicemia, meningitis, or viremia) and follow-up urologic evaluation for underlying anatomic pathology (renal ultrasound, voiding cystourethrogram). Many studies recommend surgical exploration of suspected epididymitis in the infant secondary to: 1) the limitations of physical exam;36 2) technical difficulty interpreting imaging studies of the infantile testicle; 3) clinical difficulty in differentiating between extravaginal torsion and epididymitis; and 4) the high incidence of testicular torsion associated with the neonatal acute scrotum.11 Symptomatic relief also should be provided to all patients presenting with epididymitis. Testicular elevation, bed rest, sitz baths, ice packs, and analgesia with anti-inflammatories or mild narcotics should be prescribed. Mandatory follow-up with the primary physician should be stressed, as efficacy of treatment is based on repeat clinical exam.
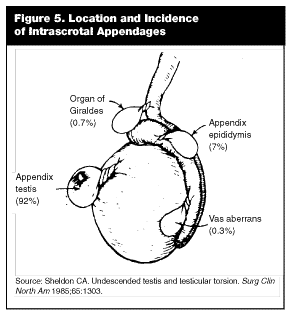
Torsion of the Appendix Testis/Epididymis. Appendage torsion is a very common cause of acute scrotal pain in young boys.43 It is the most common cause of acute scrotal pain in patients age 3-13 years,43 with a peak incidence seen in boys age 9-13 years. The appendix testis is a mullerian duct remnant at the superior testicular pole, and the epididymal appendix is a wolffian duct remnant at the head of the epididymis. (See Figure 5.) They are pedunculated structures about the size of a pea, which serve no known function. They can twist on their attachments, leading to pain from ischemia and necrosis. As illustrated in Figure 5, torsion of the appendix testis is by far the most common form of appendage torsion. This scenario produces symptoms and signs that can be very similar to testicular torsion. Further confusing the picture, torsion of an appendage occurs as often—or more often than—testicular torsion. One study of 543 boys with acute scrotal pain and surgical exploration found 16.8% with testicular torsion and 46% with appendage torsion.44 An important difference from testicular torsion is that no treatment is indicated, as most appendage torsions will resolve spontaneously. As the treatment of one condition is urgent consultation and surgery while treatment of the other is discharge home with pain medicine, the importance of ruling out testicular torsion in these patients is clear.
 |
Torsion of an appendage may present with acute onset of pain, or may present with a stuttering onset of testicular pain over several days. Nausea and vomiting, frequently associated with testicular torsion, are uncommon with torsed appendage. Initially, the pain is located at the superior pole of the testicle, and a tender 3-5 mm knot may be palpable. When this area is brought close to the skin, a bluish discoloration (the "blue dot sign") can be detected when a light is shone on the scrotum. Although this is pathognomonic for an appendage torsion, it only is seen in 20% of cases. If the patient presents later in the course, the scrotum may be swollen, tender, and inflamed, making distinction from testicular torsion difficult. Classically, the testis on the affected side is not enlarged, abnormal in lie, or diffusely tender to palpation, but later in the course this may be difficult to appreciate. Urinalysis may be helpful if acute epididymitis is suspected, as the urine in appendage torsion should be clean. Color flow Doppler is indicated to rule out testicular torsion, as radionuclide imaging is much less accurate (especially if symptoms have been present for more than 24 hours). Ultrasound will demonstrate normal to increased blood flow to the affected testicle compared to the normal testicle. Unfortunately, ultrasound results often are similar to those of acute epididymitis. In these cases, correlation with other findings of epididymitis (fever, voiding complaints, and urinalysis) should help make differentiation possible. If uncertainty exists, urologic consultation is advised. Conservative management usually is sufficient, with bed rest, scrotal elevation, analgesia, and anticipatory calcification or degeneration over 10-14 days. If color flow Doppler is inconclusive and physical exam is suspicious for testicular torsion, immediate surgical exploration is necessary.
Orchitis. Orchitis as a complication of acute epididymitis is more common than an isolated orchitis. A pure orchitis most often is viral and seen as a complication of mumps. Bacterial orchitis without associated epididymitis is rare. Orchitis is seen frequently in pre-adolescents with mumps and complicates up to 20% of these cases.45 Interestingly, the incidence goes down after puberty, with few post-adolescent patients with mumps experiencing orchitis. Mumps orchitis is not a benign disorder, as up to 60% of patients will have unilateral testicular atrophy after the orchitis resolves. Impaired fertility also can result, and is seen in up to 13% of patients with atrophy. Orchitis usually follows the symptoms of parotitis in patients with mumps by 4-7 days. Associated systemic symptoms seen include fever, malaise, myalgias, nausea, and headache. On physical exam, testicular enlargement is seen, with tender, red, swollen scrotal skin. The epididymis only should be enlarged in cases of acute epididymitis. The only laboratory test that confirms the presence of mumps is serum antibody testing. As with any case of an inflamed testicle, ultrasound should be performed to rule out torsion—a more likely diagnosis with immunized patients. Most cases of mumps orchitis resolve within 3-10 days, with only supportive treatment: heat or ice as needed, analgesics, and scrotal support. Given the high rate of testicular atrophy, urologic consultation and follow-up are indicated.
Acute Hydrocele/Varicocele. A hydrocele is a collection of serous fluid surrounding the testicle between the parietal and visceral tunica vaginalis. Alone, it usually is asymptomatic; when symptoms are present, they typically stem from the inflammation producing the hydrocele (i.e., epididymitis). Hydroceles are common and seen, on average, in 1% of adult males. Hydroceles can be an exudate, as in the case of epididymitis or orchitis; a transudate resulting from lymphatic obstruction (as in testicular cancer), testicular torsion (seen in 20% of cases of acute torsion), or appendageal torsion; or may be post-traumatic.
In the context of acute scrotal trauma, presence of a new hydrocele places the patient in a higher risk category for testicular rupture. Ultrasound should be performed to rule out testicular rupture. In infants, hydroceles are frequent occurrences secondary to a failure of obliteration of the processus vaginalis, therefore allowing communication between the peritoneal cavity and the layers of the tunica vaginalis. This communication usually will close by age 1, and surgical intervention is not warranted unless there is excessive expansion. On physical exam, hydroceles classically transilluminate easily with a light, whereas a testicular mass will not. This generally is the case, but is not considered diagnostic. When a patient presents with acute scrotal pain and a hydrocele is detected, remember that the hydrocele may limit the physical exam. Therefore, color Doppler ultrasound is indicated to confirm the diagnosis and rule out other problems. Aspiration of the fluid is not recommended, as it will reaccumulate easily and potentially can cause infection.
A varicocele is a collection of dilated veins of the pampiniform plexus and is present in up to 20% of all males.12 Varicoceles usually are present on the left. This is believed to be due to increased hydrostatic pressures, as the left testicular vein drains into the left renal vein at a right angle, and the right testicular vein drains into the vena cava at a less acute angle. The varicocele may be more prominent while standing and may resolve when supine. Varicoceles usually are painless, but the patient may complain of a "heaviness." Varicoceles classically are described as feeling like a "bag of worms." They usually are detected in adolescence during routine physical exam, may cause a disparity in testicular size, and may affect future fertility. A right-sided varicocele may represent an obstruction of the vena cava, and a new-onset varicocele in an older patient may be the first sign of a renal mass. These two conditions require consultation and/or referral to a urologist, whereas most other cases can be handled with outpatient referral to a urologist.
Testicular Cancer. Several cases of well-known patients with testicular cancer (i.e., bicyclist Lance Armstrong, Philadelphia Philly John Kruk) have helped patients become more aware of testicular cancer as an entity, but many patients still remain unaware of the warning signs. Early diagnosis is the key to survival, with five-year survival rates as high as 90% in many series with early detection.12 Testicular cancer represents about 1% of cancers affecting males but is the most common solid malignancy affecting men ages 20-34, with more than 6800 cases in the United States in 1994. Seminomas are the most common type of testicular cancer in adults. Cryptorchidism is a definite risk factor for cancer, with testicular malignancy rates 3-14 times greater in these patients.46
The patient may remain asymptomatic, even after wide metastasis. However, up to 20% of patients may experience acute scrotal pain secondary to an acute hemorrhage into the tumor.47 Epididymitis is the most common entity confused with testicular cancer, with misdiagnosis rates as high as 16%.10 The patient may note "heaviness" in the scrotum, and may complain of a firm, non-tender, testicular mass. Physical exam can be complicated by a reactive hydrocele, seen in up to 10% of patients with testicular cancer. Therefore, any patient presenting with a hydrocele requires follow-up to rule out an occult cancer. Testicular cancer also should be suspected in any patient presenting with intra-abdominal mass; hematospermia; gynecomastia; axillary, supraclavicular, or inguinal lymphadenopathy; or a chronic cough that does not respond to antibiotics.48 Appropriate laboratory tests begin with testicular ultrasound if unsure of the diagnosis, but may include computed tomography (CT) of the chest and abdomen, and specific serum markers such as alpha-fetoprotein (AFP), beta-hCG, and LDH levels for staging and identification of the specific tumor type. Pure seminomas will have normal AFP levels. Disposition includes urology consultation, and perhaps hospitalization, in any case of suspected testicular malignancy.
Scrotal/Testicular Trauma. Briefly, scrotal and testicular injuries can be simple or complex. The scrotal skin is loose and flexible, but can become lacerated. Superficial lacerations can be closed by a simple, interrupted technique using 4-0 chromic or vicryl absorbable suture. Any skin loss from the scrotum requires consultation, as skin flaps or other elaborate surgical procedures are required to cover the exposed testes. Testicular injuries include contusion, laceration, fracture, complete rupture, amputation, and dislocation (anatomic displacement from the scrotum). Color Doppler ultrasound provides the most information on the scope of the injury, and should be ordered for anyone with a history of testicular trauma. Ultrasound findings include scrotal hematoma, hematocele, intratesticular hematoma, and testicular rupture. Presence of a hydrocele after trauma should heighten suspicion for testicular rupture, as up to 50% of patients with testicular rupture have a new hydrocele on presentation.1 Only testicular contusion is treated conservatively, whereas fracture, dislocation (rare reports of closed reduction exist), laceration, rupture, and amputation require surgical intervention.49 Amputated testes can be reimplanted, but optimally this should be done within 6-8 hours. Dislocation is a relatively rare event, often associated with multiple trauma or significant directed blunt trauma.50 It can be unilateral or bilateral, and easily is missed or overlooked. In nearly 80% of cases, the missing testis is found in the abdominal wall.51 On physical exam, an ecchymotic scrotum with an absent testis or testes can be seen. Dislocation with scrotal hematoma or testicular rupture can present confusing physical exams, and one case report describes a young man in whom a scrotal hematoma led to misdiagnosis of testicular dislocation for four months.52 Ultrasound is indicated to rule out dislocation and often is required for the final diagnosis.
References
1. Burgher SW. The difficult diagnosis: Acute scrotal pain. Emerg Med Clin North Am 1998;16:781-809.
2. Anderson JB, Williamson RCN. The fate of human testes following unilateral torsion of the spermatic cord. Br J Urol 1986;58:698-704.
3. Harwood-Nuss AL, Etheredge W, McKenna I. Urologic Emergencies. In: Rosen P, et al, eds. Emergency Medicine: Concepts and Clinical Practice, 4th ed. St. Louis: Mosby; 1998:2227-2261.
4. Anderson PA, Giacomantonio JM, Schwartz RD. Acute scrotal pain in children: Prospective study of diagnosis and management. Can J Surg 1989;32:29-32.
5. Ben-Sira L, Laor T. Severe scrotal pain in boys with Henoch-Schonlein purpura: Incidence and sonography. Pediatr Radiol 2000;30:125-128.
6. Ioannides AS, Turnock R. An audit of the management of the acute scrotum in children with Henoch-Schonlein Purpura. J R Coll Surg Edinb 2001;46:98-99.
7. Munter DW, Faleski EJ. Blunt scrotal trauma: Emergency department evaluation and management. Am J Emerg Med 1989;18:227-234.
8. Matteson JR, Stock JA, Hanna MK, et al. Medicolegal aspects of testicular torsion. Urology 2001;57:783-786.
9. Schul MW, Keating MA. The acute pediatric scrotum. J Emerg Med 1993;11:565-577.
10. Swartz D. The acute scrotal mass. In: Harwood-Nuss A, ed. The Clinical Practice of Emergency Medicine, 2nd ed. Philadelphia: JB Lippincott; 1996:232-240.
11. Lewis AG, Bukowski TP, Jarvis PD, et al. Evaluation of acute scrotum in the emergency department. J Pediatr Surg 1995;30:277-282.
12. Junnila J, Lassen P. Testicular masses. Am Fam Phys 1998;57:685-692.
13. Haynes BE, Bessen HA, Haynes VE. The diagnosis of testicular torsion. JAMA 1983;249:2522-2527.
14. Tryfonas G, Violaki A, Tsikopoulos G, et al. Late postoperative results in males treated for testicular torsion during childhood. J Pediatr Surg 1994;29:553-556.
15. Melekos MD, Asbach HW, Markou SA. Etiology of acute scrotum in 100 boys with regard to age distribution. J Urol 1988;139:1023-1025.
16. Jefferson RH, Perez LM, Joesph DB. Critical analysis of the clinical presentation of the acute scrotum: A 9-year experience at a single institution. J Urol 1997;158:1198-2000.
17. Seng YJ, Moissinac K. Trauma induced testicular torsion: A reminder for the unwary. J Accid Emerg Med 2000;17:381-382.
18. Kadish HA, Bolte RG. A retrospective review of pediatric patients with epididymitis, testicular torsion, and torsion of testicular appendages. Pediatrics 1998;102;73-76.
19. Lewis RL, Roller MD, Parra BL, et al. Torsion of an intra-abdominal testis. Curr Surg 2000;57:497-499.
20. Lee KF, Tang YC, Leong HT. Emergency laparoscopic orchidectomy for torsion of intra-abdominal testis: A case report. J R Coll Surg Edinb 2001;46:110-112.
21. Sidler D, Brown RA, Millar AJ, et al. A 25-year review of the acute scrotum in children. S Afr Med J 1997;87:1696-1698.
22. Rabinowitz R. The importance of the cremasteric reflex in acute scrotal swelling in children. J Urol 1984;132:89-90.
23. Hughes ME, Currier SJ, Della-Guistina D. Normal cremasteric reflex in a case of testicular torsion. Am J Emerg Med 2001;19:241-242.
24. Wilbert D, Schaerfe C, Stern W, et al. Evaluation of the acute scrotum by color-coded Doppler ultrasonography. J Urol 1993;149:1475-1477.
25. Blaivas M, Sierzenski P, Lambert M. Emergency evaluation of patients presenting with acute scrotum using bedside ultrasonography. Acad Emer Med 2001;8:85-89.
26. Weber D, Rosslein R, Fliegel C. Color Doppler sonography in the diagnosis of acute scrotum in boys. Eur J Pediatr Surg 2000;10:235-241.
27. Babcock DS. Which is the most sensitive study for testicular nuclear scan? AJR Am J Roentgenol 1995;165:224.
28. Kravchick S, Cytron S, Leibovici O, et al. Color Doppler sonography: Its real role in the evaluation of children with highly suspected testicular torsion. Eur Radiol 2001;11:1000-1005.
29. Rivers KK, Rivers EP, Stricker HJ, et al. The clinical utility of serologic markers in the evaluation of the acute scrotum. Acad Emerg Med 2000;7:1069-1072.
30. Doehn C, Fornara P, Kausch I, et al. Value of acute-phase proteins in the differential diagnosis of acute scrotum. Eur Urol 2001;39:215-221.
31. Dunne PJ, O’Loughlin BS. Testicular torsion: Time is the enemy. Aust N Z J Surg 2000;70:441-442.
32. Fenner MN, Roszhart DA, Texter JH. Testicular scanning: Evaluating the acute scrotum in the clinical setting. Urology 1991;38:2237-2241.
33. Cornel EB, Karthaus HF. Manuel derotation of the twisted spermatic cord. BJU Int 1999;83:672-674.
34. Miller DC, Peron SE, Keck RW, et al. Effects of hypothermia on testicular ischemia. J Urol 1990;143:1046-1048.
35. Ireton RC, Berger RE. Prostatitis and epididymitis. Urol Clin North Am 1984;11:83-94.
36. Bennett RT, Gill B, Kogan SJ. Epididymitis in children: The circumcision factor? J Urol 1988;160:1842-1844.
37. Joly-Guillou ML, Lasry S. Practical recommendations for the drug treatment of bacterial infections of the male genital tract including urethritis, epididymitis, and prostatitis. Drugs 1999;57:743-750.
38. Marks L. The acute scrotum. Crit Decisions Emerg Med 1997;2:11-17.
39. Gasparich JP, Mason JT, Greene HL, et al. Non-infectious epididymitis associated with amiodarone therapy. Lancet 1984;2:1211.
40. Rajfer J. Congential anomalies of the testis. In: Walsh PC, ed. Campbell’s Urology, 6th ed. Philadelphia: WB Saunders; 1992: 572.
41. Knight PJ, Vassy LE. The diagnosis and treatment of the acute scrotum in children and adolescents. Ann Surg 1984;200:664-673.
42. Zdrodowska-Stefanow B, Ostaszewska I, Darewicz B, et al. Role of Chlamydia trachomatis in epididymitis. Part I: Direct and serologic diagnosis. Med Sci Monit 2000;6:1113-1118.
43. Campobasso P, Donadio P, Spata E, et al. Acute scrotum in children: Analysis of 265 consecutive cases. Pediatr Med Chir 1996;18:15-20.
44. Van Glabeke E, Khairouni A, Larroquet M, et al. Acute scrotal pain in children: Result of 543 surgical explorations. Pediatr Surg 1999;15:353-357.
45. Casella R, Leibundgut B, Lehmann K, et al. Mumps orchitis: Report of a mini-epidemic. J Urol 1977;158:2158-2161.
46. Farrer JH, Walker AH, Raifer J. Management of the postpubertal cryptorchid testes: A statistical review. J Urol 1985;134:1071-1076.
47. Schneider RE. Male Genital Problem. In: Tintinalli JE, et al, eds. Emergency Medicine—A Comprehensive Study Guide, 5th ed. New York: McGraw-Hill; 2000:631-640.
48. Kassabian VS, Graham SD. Urologic and Male Genital Cancers. In: Murphy GP, et al. American Cancer Society Textbook of Clinical Oncology, 2nd ed. American Cancer Society; 1995:324-327.
49. Madden JF. Closed reduction of a traumatically dislocated testicle. Acad Emerg Med 1994;1:272-275.
50. Shefi S, Mor Y, Dotan ZA, et al. Traumatic testicular dislocation: A case report and review of the published reports. Urology 1999; 54:744.
51. Schneider RE. Genitourniary trauma. In: Rosen P, et al eds. Emergency Medicine: Concepts and Clinical Practice, 4th ed. St. Louis: Mosby; 1998:582-601.
52. Hayami S, Ishigooka M, Suzuki Y, et al. Pathological changes of traumatic dislocated testis. Urol Int 1996;56:129-132.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
