Hemoptysis
August 15, 2014
Reprints
Hemoptysis
Executive Summary
- The most common causes of hemoptysis in the United States are bronchitis, bronchiectasis, bronchogenic cancer, and tuberculosis. Metastatic lesions in the lung rarely cause hemoptysis.
- Massive hemoptysis is defined as that causing 200-1000 mL within a 24-hour period or associated with hemodynamic instability or respiratory insufficiency.
- Hemoptysis is rare in children, and the most common causes are foreign body aspiration, lower respiratory infections, or bronchiectasis associated with cystic fibrosis.
- CT and bronchoscopy are the primary diagnostic tools for massive hemoptysis. Severe cases may require bronchial artery embolization or even emergent surgery. Intubation of the right main stem bronchus provides initial stabilization in patients with massive hemorrhage from the left lung.
Introduction
Hemoptysis is defined as expectoration of blood from the lower respiratory tract. There are numerous conditions that cause hemoptysis, ranging from mild conditions such as bronchitis to life-threatening conditions such as pulmonary embolism or lung cancer. Hemoptysis is a serious symptom and may be evidence of an underlying disease process. Although rare, massive hemoptysis can cause hemodynamic instability and rapid deterioration with significant morbidity and mortality. In the literature, there is no widely accepted definition of massive hemoptysis, and specific figures remain controversial. Amounts of blood ranging from a rate of 200 mL to 1000 mL over a 24-hour period have been proposed to define massive hemoptysis.1 Quantifying the amount can be difficult, if not impossible, in certain cases. Thus, from a practical perspective, massive hemoptysis can be defined as expectoration of blood that impairs respiratory function and adequate gas exchange and is potentially life-threatening due to hemodynamic changes. The exact incidence of massive hemoptysis is elusive given the varying definition, but it is estimated that only about 5% of cases of hemoptysis are considered to be massive.1 The mortality rate for massive hemoptysis is thought to be as high as 50-85%.2 The majority of cases of hemoptysis are not life-threatening. The emergency physician has to make a decision within a much shorter observation period than 24 hours to determine whether the hemoptysis is causing life-threatening airway obstruction or asphyxiation.
Pathophysiology
Bronchial and pulmonary arteries make up the two major arterial systems supplying the lung. They are vastly different in that the bronchial artery is under high systemic pressures and is responsible for providing the lung tissue with oxygenated blood. The pulmonary arterial system, on the other hand, is under much lower pressures and is responsible for bringing deoxygenated blood to the lungs for gas exchange. Approximately 90% of massive hemoptysis originates from the bronchial artery circulation, while only 5% originates from the pulmonary artery circulation, and even then, generally only under conditions of acute or chronic pulmonary hypertension.1 The bronchial arteries directly arise from the thoracic aorta at the level of the fifth or sixth thoracic vertebrae approximately 60% of the time. Typically there are two bronchial arteries on the left and one on the right. The pulmonary artery arises from the right ventricle and bifurcates into the right and left main pulmonary arteries. The majority of cases of non-massive hemoptysis usually do not involve these arteries, but rather originate from capillaries from the tracheobronchial tree. The mucosa becomes inflamed and edematous from an infection or tumor that leads to tearing of the superficial blood vessels.
History and Physical
First, the physician must discern whether or not the bleeding is originating from the lungs. Gastrointestinal bleeding and nasopharyngeal bleeding should be ruled out. This can largely be done by history and physical examination, but differentiating these can be challenging at times, especially in a critically ill patient who cannot provide a history. Gastric fluid is nearly always acidic, so pH paper can be of help. Once it is determined that the presentation is true hemoptysis, the clinician can then attempt to narrow the differential diagnosis. Attempt to estimate the amount of hemoptysis. A detailed history is key to ascertaining the etiology of the hemoptysis.
Information about past medical history, with special attention to pulmonary diseases such as asthma, chronic obstructive pulmonary disease (COPD), bronchiectasis, lung cancer, and tuberculosis, is important. Signs and symptoms of cough, fever, sputum production, weight loss, night sweats, smoking history, and environmental exposures should be noted. In most instances of bronchiectasis, there is a typical history of chronic productive cough, purulent sputum, and recurrent flares of pneumonitis. Similarly, patients with chronic bronchitis have a longstanding productive cough. Lung abscess may present with fever, cough, and purulent expectoration. Pulmonary embolus (PE) risk factors should also be sought, including previous history of PE, deep vein thrombosis (DVT), travel history, and recent surgeries. Heart failure and valvular heart disease history should be obtained. Medication history, including anticoagulants such as warfarin, aspirin, clopidogrel, and rivaroxaban, should also be obtained. Medications such as bevacizumab have been known to cause minor to life-threatening hemoptysis.3 Patients from, or who have recently traveled to, third-world countries should be suspected of having tuberculosis or parasites such as paragonimiasis (lung fluke). Patients should be asked about illicit drug use, as "crack" cocaine smokers can develop diffuse alveolar hemorrhage.4 (See Figure 1.) Previous episodes of hemoptysis can also provide vital information or clues as to the cause.
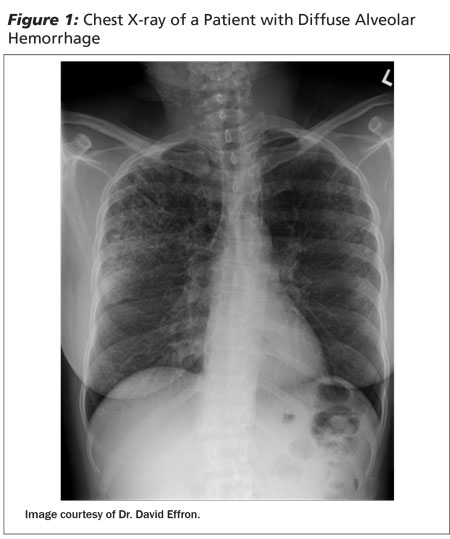
In addition to history, the physical exam can provide key additional information about the etiology of hemoptysis. Vital signs and telemetry monitoring with pulse oximetry are important for all patients with massive hemoptysis. Patients with hypotension or hypoxemia should be managed aggressively. A detailed pulmonary, nose, and oropharyngeal exam should be performed. The presence of stridor can indicate the presence of a foreign body in the upper airway. The general appearance and nutritional status can provide clues to making the diagnosis such as tuberculosis and malignancy. Lymph nodes, including cervical, supraclavicular, and axillary, should be examined. The cardiovascular examination may yield the presence of murmurs, which could provide clues to the diagnosis of valvular disorders such as mitral stenosis, or congestive heart failure. The presence of unilateral calf swelling could indicate the presence of thromboembolic disease. The skin should be carefully examined for the presence of rashes, petechia, purpura, and pallor. For example, the presence of a rash with a saddle nose deformity could indicate Wegener’s granulomatosis.
Causes
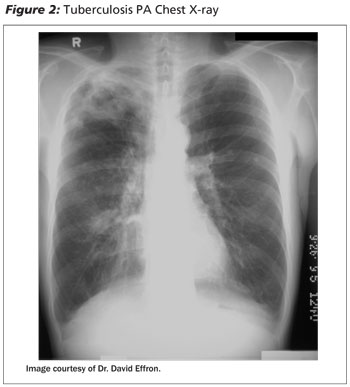
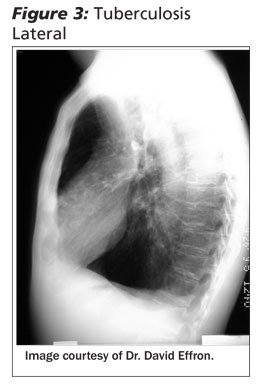
The list of potential causes of hemoptysis is extensive. (See Table 1.) In developed countries such as the United States, chronic inflammatory lung disease and bronchogenic carcinoma are the most common causes of hemoptysis, while in third world countries, tuberculosis (see Figures 2 and 3) remains the most common cause.5 One recent prospective study of 184 patients in Greece showed that the etiologies of admitted patients with hemoptysis were bronchiectasis (26%), chronic bronchitis (23%), acute bronchitis (15%), and lung cancer (13%).6 Another recent study of 154 patients in Spain showed that the leading causes of life-threatening hemoptysis were bronchiectasis and tuberculosis.7 The cause is unknown in up to 5-10% of patients.1
Table 1: Causes of Hemoptysis
Pulmonary
- Acute and chronic bronchitis
- Pneumonia
- Tuberculosis*
- Lung abscess*
- Neoplasm*
- Fungal infection*
- Bronchiectasis*
- Pneumonitis (chemical, inhalational, etc.)
- Cystic fibrosis*
- Pulmonary contusion/trauma
- Parasites
Cardiovascular
- Pulmonary embolism
- Congestive heart failure
- Arteriovenous malformation
- Pulmonary hypertension
- Mitral stenosis
- Vasculitis (Wegener’s, Goodpasture’s, SLE)
- Aortopulmonary fistula
- Endocarditis
- Coagulopathy (DIC, VWD, hemophilia, thrombocytopenia, warfarin)
Others
- Foreign body
- Iatrogenic (post bronchoscopy, biopsy, tracheostomy complications)
- Medications
- Trauma
- Cocaine
VWD= von Willebrand’s disease
DIC= Disseminated intravascular coagulation
SLE= Systemic lupus erythematosis
*= More likely causes for massive hemoptysis
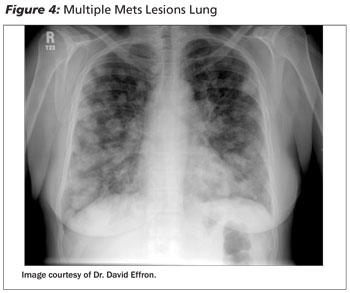
Patients who are older than the age of 40 and have an extensive smoking history are at increased risk for neoplasm.8 Although a large portion of lung cancers are due to metastasis, hemoptysis is rarely caused by metastatic lung cancer.9 (See Figure 4.) In pediatric populations, lower respiratory infection, foreign body aspiration, and bronchiectasis secondary to cystic fibrosis are the most common causes of hemoptysis. Hemoptysis in children is a relatively rare phenomenon.10 Patients who recently emigrated from, or traveled to, a third world country are at increased risk for tuberculosis.
Non-massive Hemoptysis
The majority of cases of hemoptysis are not massive and not life-threatening.11 The most common cause of mild hemoptysis is bronchitis.12 No consensus guidelines exist for management of non-massive hemoptysis; however, Figure 5 shows a suggested algorithm based on the literature.

Diagnostic Evaluation
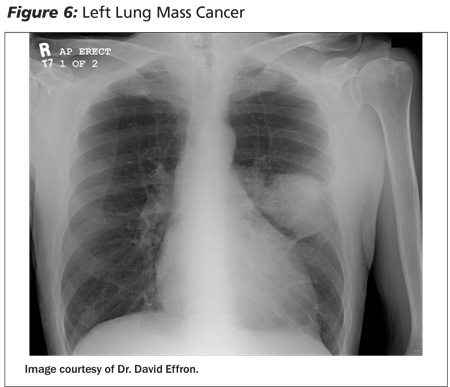
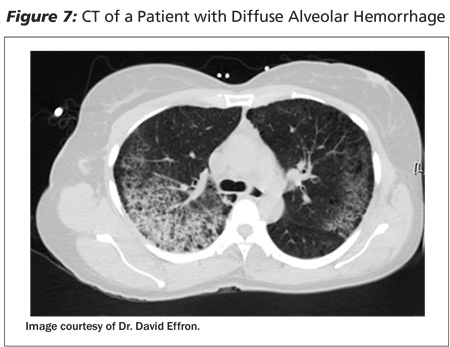
After the history and physical exam, a chest radiograph is performed to assess for masses, infections, evidence of bronchiectasis, or parenchymal disease. (See Figure 6.) Diffuse hemorrhage into the alveola can cause a patchy infiltrate. (See Figure 1.) The chest radiograph may aid in localizing the region of bleeding, but 15-30% of patients with hemoptysis will have a normal chest radiograph.13 If the chest radiograph does not provide a clear diagnosis, further diagnostic modalities, including CT scans and bronchoscopy, should be considered to find the location of the bleeding to allow for therapeutic intervention. (See Figure 7.) In many cases, these can be performed as an outpatient.
Initial recommended laboratory studies include complete blood count with differential to look for evidence of anemia, infection, or thrombocytopenia. (See Table 2.) Coagulation studies, including prothrombin time and partial prothrombin time, are ordered in appropriate cases to rule out any coagulopathies.
Table 2: Suggested Laboratory Tests
- Complete blood count with differential
- Complete metabolic panel
- Coagulation studies including PT/INR and PTT
- Type and screen/cross
- D-dimer
- Arterial blood gas
- Sputum culture, fungal culture
- Gram stain, including acid-fast bacillus
- Tuberculin skin testing
- Urinalysis
If a mass or lesion is identified and the patient has stable vital signs, the patient can be referred back to his or her primary care doctor or to a pulmonologist for further outpatient workup, which may include CT scan, bronchoscopy, or biopsy.11 CT of the chest should be considered if chest radiography shows parenchymal disease, particularly in patients without established follow-up.
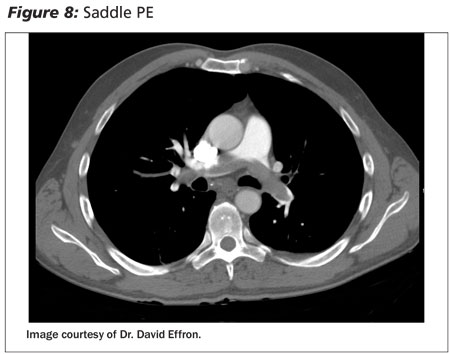
Patients with a normal chest radiograph and no risk factors for lung carcinoma can be managed on an outpatient basis with close monitoring. If pulmonary embolus is suspected, a chest CT angiogram is appropriate. (See Figure 8.) The patient can be observed in the emergency department and/or in the hospital if clinically indicated.
Massive Hemoptysis Initial Management
The mantra of emergency medicine certainly applies to hemoptysis — airway, breathing, and circulation (ABCs). Due to the high morbidity and mortality associated with massive hemoptysis, the ABCs are addressed prior to further diagnosis and workup. Airway protection is paramount; it only takes 400 mL of blood in the alveolar space to cause substantial impediment to gas exchange.14 If the bleeding side can be localized, the patient is placed in a lateral decubitus position with the bleeding side down to spare the contralateral side from further aspiration. The patient should be intubated early in cases of massive hemoptysis, preferably with an endotracheal tube greater than 8.0 mm to allow for bronchoscopy. If the bleeding is confirmed or suspected to be left sided, blind right main stem intubation with a single lumen endotracheal tube can be performed.15
Selective intubation with a dual lumen endotracheal tube is ideal, but is best performed by an experienced anesthesiologist or pulmonologist.16 Two large-bore intravenous lines are placed and volume resuscitation with intravenous fluids and/or blood transfusion considered. If the patient has a known coagulopathy, it can be rapidly reversed with appropriate agents such as fresh frozen plasma, prothrombin complex concentrate, or platelets.
There is evidence that antifibrinolytic agents may reduce both the duration and volume of bleeding in patients with hemoptysis. This category of agent includes tranexamic acid (TXA), aminocaproic acid, nafamostat, and aprotinin. Of these, only TXA has been studied for use in limiting hemoptysis. This hemostatic agent, marketed in the United States as Cyklokapron® or Lysteda®, may be given orally or intravenously.17 In a Cochrane review, two randomized, controlled trials utilizing TXA for control of hemoptysis were found; one included only hospitalized patients presenting with hemoptysis secondary to tuberculosis. Pooled together, there was a significant reduction in the duration of bleeding after therapy between patients receiving TXA and those receiving placebo. Doses were in the range of 500-1000 mg TXA administered orally 3 times daily for 3-7 days. While neither study reported severe adverse effects of antifibrinolytic therapy, such as venous thromboembolism, stroke, renal failure, or acute myocardial infarction, the report concluded that there was insufficient evidence to determine if antifibrinolytic agents of any kind should be used in the treatment of hemoptysis.18 There are reports in which TXA successfully controlled hemoptysis associated with cystic fibrosis.19
If available at one’s institution, call for consultations early. Proposed services include pulmonary medicine, interventional radiology, anesthesiology, and thoracic surgery, as appropriate. The patient should be transferred to a tertiary center if the necessary services are not available.
Diagnostic Evaluation
Once the patient is stabilized, laboratory and radiographic studies can be ordered. Type and screen/cross are ordered for patients who may require blood transfusion. Urinalysis and metabolic panel should be ordered to assess for renal function in patients for whom vasculitis such as Wegener’s or Goodpasture’s syndrome is a consideration. In patients who are suspected of having a pulmonary embolism, a D-dimer or chest CT angiogram might be indicated. Blood gas analysis should be ordered if clinically indicated.
If infection is in the differential, sputum culture and stain should be ordered, including acid-fast bacillus testing and fungal culture.
In stable patients with significant hemoptysis, contrast chest computed tomography (CT) should be obtained once the patient is stable. In one study with 184 patients, 40% of patients with a negative chest radiograph had a positive CT.6 CT has the advantage in that it is readily available, and is noninvasive. CT scan alone can localize the site of bleeding in 63-100% of patients.13,20 A relatively new diagnostic tool, multi-detector CT (MDCT) can be of high diagnostic value. In a study involving 22 patients with hemoptysis, 100% of bronchial and 62% of nonbronchial arteries were detected on MDCT.21
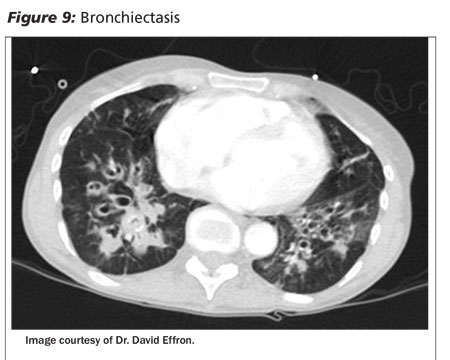
Recent studies show CT to be more useful than fiberoptic bronchoscopy in initial evaluation of patients with hemoptysis. It is far more accurate in determining the etiology of hemoptysis (60-77% vs. 2.5-8%), and is nearly as good (70% vs. 88.8%) as fiberoptic bronchoscopy in localizing bleeding sites.22,23 (See Figure 9.)
Bronchoscopy allows for direct visualization and is able to identify mucosal lesions that would otherwise not be seen on CT. If the patient is unstable, if CT does not readily identify the site of bleeding, or if the diagnosis is still not clear, bronchoscopy should be performed by a pulmonologist.
Rigid bronchoscopy can be used in unstable patients with massive hemoptysis for diagnosis and therapeutic intervention. However, rigid bronchoscopy typically is performed in the operating room under general anesthesia rather than at the beFlexible fiberoptic bronchoscopy can be performed in more stable patients and at the bedside in the emergency department.24 Rigid bronchoscopy has the advantage of suction and evacuation of large clots; however, fiberoptic bronchoscopy allows for deeper visualization of the tracheobronchial tree.15
Bronchoscopy and CT in many ways can provide complementary information with respect to etiology and localization of bleeding. (See Table 3.) In one study, sensitivity of diagnosis of lung cancer was 93% when both studies were performed, compared to 42% for bronchoscopy alone and 67% for CT alone.25 If the decision is made to perform flexible bronchoscopy, it should be performed within 48 hours, as early bronchoscopy is able to identify active bleeding in 41%, compared to 8% for delayed bronchoscopy.26 The treatment modality of bronchoscopy will be further discussed in the treatment section.
Table 3: Comparison of Computed Tomography and Bronchoscopy
Computed Tomography Scan |
Bronchoscopy |
|
Pros |
|
|
Cons |
|
|
Advanced Therapy for Hemoptysis
Death from massive hemoptysis is from asphyxiation rather than exsanguination.27 From a historical perspective, resection of the diseased lung has often been the definitive treatment.2
Many patients with hemoptysis are poor surgical candidates due to poor lung capacity, hypoxia, or severe pulmonary disease, and other therapies are now available. The diagnosis and therapy often involves a pulmonary critical care specialist, an interventional radiologist, and a thoracic surgeon working together.
Recent advances in non-surgical endovascular treatment can be used to treat moderate bleeding, defined as three episodes of 100 mL in one week, or even mild hemoptysis cases.28 Bronchial artery embolization, or BAE, was first described in 1973,29 and is now considered the most effective non-surgical treatment of massive hemoptysis.30 It may be performed without bronchoscopy. In the baseline healthy state, bronchial arteries make up only 1% of the arterial supply of the lungs, but with chronic inflammation of the lungs, these arteries enlarge and proliferate. Since they are under higher pressure than the normal pulmonary circulation, control of hemoptysis must entail control of hemorrhage from these vessels.
Bronchial arteries arise from the descending aorta at the level of the third to eighth thoracic vertebral body, and at T5 or T6 most typically. In a minority of cases, they may arise from other sources such as the subclavian, brachiocephalic, or internal mammary arteries.31 The numbers and sites of origin of the bronchial arteries vary widely by individual. Most commonly, there is a single right bronchial artery and two left bronchial arteries arising at the T5/6 level, but even this pattern occurs only approximately 40% of the time. Notably, a spinal artery originates from a bronchial artery in 5% of patients. Early users of BAE encountered difficulties cannulating the bronchial artery or visualizing a spinal artery branch. With the development of microcatheters to cannulate smaller caliber vessels, it has been possible to more reliably cannulate a bronchial artery distal to the origin of a spinal branch, and avoid neurological complications.16
Arterial access is obtained via the femoral artery so that bilateral bronchial angiography can be performed. If the feeders originating from the subclavian artery cannot be accessed from the femoral artery, brachial artery puncture may be performed. Angiography of the intercostal, subclavian, or inferior phrenic arteries may be performed depending on the site of disease and in order to control the hemorrhage. Typical angiographic findings include bronchial artery hypertrophy, increased vascularity, and arteriovenous shunting. Embolization has been performed under fluoroscopy using polyvinyl alcohol (PVA) particles in most cases, although 3-5 mm coils, absorbable gelatin pledgets/sponges, trisacryl gelatin, and isobutyl-2-cyanoacrylate have been used as well. The success rate of BAE is excellent, and it has largely replaced surgery as the primary intervention for therapy of significant active hemoptysis. One study reported that bronchial artery embolization was successful in stopping the bleeding in 98.5% of patients, with control of hemoptysis at one month in 90%.2 Others report success rates in controlling hemoptysis via embolization in approximately 75-90%.21,32-34
In patients with primary lung cancer, hemoptysis is more likely to be caused by necrosis and inflammation of blood vessels within the tumor rather than direct invasion of blood vessels by the tumor itself. Arterial embolization therapy is effective in controlling hemoptysis due to primary lung cancer.35
Post-embolization thoracic aortography may be required if the initial embolization proves unsuccessful. Inferior phrenic artery and intercostal arteries can be overlooked if thoracic aortography was not performed. As noted earlier, the anatomy of the bronchial circulation is variable; bronchial arteries, for example, originate from the inferior aspect of the aortic arch in a minority of people, and the artery of Adamkiewicz arises from the right intercostobronchial artery in a minority of people. Recurrence of hemoptysis may be due to these anatomic variants or other causes, including incomplete embolization of the bronchial vessels, recanalization of the embolized arteries, development of collateral circulation in response to continuing inflammation, or the presence of non-bronchial systemic arteries.16 Because of these factors, embolization may be ineffective or may need to be repeated.
Complications of BAE include failure to control bleeding, likely attributable to non-bronchial collateral arteries from other arteries, such as the phrenic, intercostal, mammary, or subclavian arteries.36 Particles too small in diameter can cause pulmonary infarction or spinal infarction, which is the most dreaded consequence of bronchial artery embolization.37 If the microcatheter tip is not distal to any radicular/spinal arteries before embolization is performed, spinal cord infarction may occur, resulting in lower extremity paralysis. Passage of larger (500 µm) microspheres through bronchopulmonary shunts has been reported to cause myocardial infarction and stroke following management of hemoptysis.38 Bronchial or esophageal necrosis can occur, as these are organs supplied by the bronchial arteries. Other complications related to the procedure include contrast-induced nephropathy, groin hematoma, transient dysphagia, and dissection of the aorta or great vessels.31
Bronchoscopy can be used prior to angiography in order to locate or lateralize the site of bleeding. Bronchoscopy allows local therapy, such as laser coagulation, topical cellulose mesh,16 thrombin or fibrinogen instillation, or local infusion of chilled normal saline or vasoactive drugs such as 1:20,000 epinephrine, to control bleeding.31 However, it frequently fails to determine the site or side of bleeding. In patients with severe hemoptysis, the airways may be filled with blood, rendering any endobronchial treatment ineffective. Nonetheless, urgent bronchoscopy has a role in therapy, since it can be used to introduce balloon-tip catheters into the bleeding bronchus for tamponade of a hemorrhagic artery. This was first described in 1974, and required a rigid bronchoscope.39 Biocompatible sealants such as N-butyl cyanoacrylate have been used for tamponade as well.15 By doing this, the nonbleeding bronchi or other lung is protected from aspiration. Tamponade and isolation of the bleeding site has been achieved via bronchoscopy by placement of two covered self-expanding airway stents in a patient with cancer. This was strictly a palliative procedure, but the hemoptysis was controlled until the patient’s death four months later.40
Double-lumen balloon catheters have since been developed, which may pass through a fiberoptic bronchoscope.1 Tamponade by balloon is only temporizing until the patient undergoes more definitive therapy, such as bronchial artery embolization, surgery, radiation, or chemotherapy. Rigid bronchoscopy is efficient at securing airway patency and preventing asphyxia, allowing isolation of the unaffected lung. It has a wider lumen, allowing coagulation therapy via laser, electrocautery, or argon plasma coagulation (APC).16 Flexible bronchoscopy has the advantage of being able to explore the fifth or sixth bronchial division and can be performed in the emergency department. It can also afford a view of the upper lobes.15
One study concluded that bronchoscopy may not be necessary in the management of severe hemoptysis due to the risk of hypoxia, airway compromise from sedation, delay in definitive therapy, and cost.41 This opinion was supported by others who felt that there was no need for bronchoscopy during active severe bleeding.2 High resolution CT may replace fiberoptic bronchoscopy in the immediate management of hemoptysis, or perhaps guide the bronchoscopy.22
In cases of mild or moderate hemoptysis, the optimal timing of bronchoscopy is controversial. The diagnostic yield of flexible bronchoscopy is higher if performed early while bleeding is still active, but the timing does not appear to alter therapy or clinical outcome.16
Computed tomography and CT angiography, while not therapeutic, can be superior diagnostic modalities to bronchoscopy in the evaluation of acute hemoptysis. CT can demonstrate underlying pathology, vascular lesions such as arteriovenous malformations, thoracic aneurysm, bronchiectasis, aspergilloma, and carcinoma. As well as demonstrating specific pathologies, the feeding arteries may be identified.21 MDCT is capable of detecting the origin and ostial position of bronchial arteries and detecting nonbronchial systemic arteries. MDCT can determine the bleeding bronchial artery by measuring the tortuosity of the vessel, parenchymal enhancement, detecting a specific hypertrophied vessel — that is with a diameter of > 1.5 mm — or an active leak from the vessel. After analysis of the bronchial and systemic arteries, the pulmonary vessels may be analyzed to try to determine if the bleeding vessel is of bronchial or pulmonary origin.31 While these tend not to be a source of massive hemoptysis, Rasmussen aneurysms, pulmonary artery aneurysms and pseudoaneurysms, and pulmonary vessels abutting tuberculous cavities can bleed extensively. Therefore, while not a therapeutic modality, MDCT does enable and direct arterial percutaneous transcatheter embolization.37
MDCT may, in fact, be more accurate than conventional angiography in identifying bronchial and nonbronchial systemic arteries by identifying pleural thickening near a parenchymal opacity or enhancing vessels near an extrapleural fat layer.21,42 The disadvantages of CT are chiefly radiation exposure, the need to use contrast material and its attendant risk for nephrotoxicity, and time delays in obtaining the study.
Recurrent bleeding after initial control of hemoptysis is not uncommon, especially in patients with neoplasia, or diffuse disease, such as cystic fibrosis, tuberculosis, or aspergilloma.
A nationwide database found that over a 10-year period, of approximately 457,500 admissions in the United States for hemoptysis, 2671 (0.58%) underwent surgery. Of these, 2205 had a lobectomy performed and 466 underwent pneumonectomy.43 Massive hemoptysis caused by vascular injury, arteriovenous malformation, iatrogenic injury to the pulmonary artery, leaking thoracic aneurysm with communication to a bronchus, or hydatid cyst are conditions in which bronchial artery embolization is inadequate to control hemorrhage. Bronchial adenomas or mycetomas/aspergillomas, as localized diseases, may be treated surgically.1
Patients with nonresectable tumor, diffuse/bilateral lung disease (e.g, cystic fibrosis, multiple avascular malformations, multifocal bronchiectasis), poor pulmonary reserve, poor functional status, or other comorbid conditions are often poor surgical candidates.
Surgery is largely reserved for failure of BAE and bronchoscopy, technical failures of arteriography, or in situations in which the patient’s clinical status does not allow for transfer to an interventional radiology suite.44,45 Surgery is associated with better survival when performed in a nonurgent setting. Mortality rates following surgical intervention for hemoptysis range from 7-18%, but rise to 40% in the emergency setting.30
Conclusion
Hemoptysis is not an uncommon chief complaint in the emergency department. Massive hemoptysis, which represents less than 5% of the cases of hemoptysis, is defined as blood greater than 200 to 1000 mL in less than 24 hours, or any quantity causing hemodynamic instability and capable of causing asphyxia, and can be life-threatening. The differential diagnosis of hemoptysis is extensive, with bronchitis, bronchiectasis, bronchogenic carcinoma, and tuberculosis being the most common overall causes. When managing hemoptysis, ABCs should be addressed first, followed by a thorough history and physical exam. Both CT scans and bronchoscopy can greatly aid in the investigation of hemoptysis. Bronchoscopy is advantageous in that it can be both diagnostic as well as therapeutic, while CT is better at diagnosing the etiology of hemoptysis and is readily available. In addition to bronchoscopic interventions, bronchial artery embolization has largely replaced surgery as the primary method of treatment for massive hemoptysis. Surgery is reserved for cases that have failed BAE.
References
- Jean-Baptiste E. Clinical assessment and management of massive hemoptysis. Crit Care Med 2000;28(5):1642-1647.
- Poyanli A, et al. Endovascular therapy in the management of moderate and massive haemoptysis. Br J Radiol 2007;80(953):331-336.
- Cho YJ, Murgu SD, Colt HG. Bronchoscopy for bevacizumab-related hemoptysis. Lung Cancer 2007;56(3):465-468.
- Haim DY, et al. The pulmonary complications of crack cocaine. A comprehensive review. Chest 1995;107(1):233-240.
- Tintinalli JE, Stapczynski JS. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. McGraw-Hill; New York: 2011:1 online resource (xl, 2120 pages).
- Tsoumakidou M, et al. A prospective analysis of 184 hemoptysis cases: Diagnostic impact of chest X-ray, computed tomography, bronchoscopy. Respiration 2006;73(6):808-814.
- Orriols R, et al. [Life-threatening hemoptysis: study of 154 patients]. Med Clin (Barc) 2012;139(6):255-260.
- O’Neil KM, Lazarus AA. Hemoptysis. Indications for bronchoscopy. Arch Intern Med 1991;151(1):171-174.
- Reisz G, et al. The causes of hemoptysis revisited. A review of the etiologies of hemoptysis between 1986 and 1995. Mo Med 1997;94(10):633-635.
- Godfrey S. Hemoptysis in children. Pediatr Pulmonol Suppl 2004;26:
177-179. - Hurt K, Bilton D. Haemoptysis: Diagnosis and treatment. Acute Med 2012;11(1):39-45.
- Bidwell JL, Pachner RW. Hemoptysis: Diagnosis and management. Am Fam Physician 2005;72(7):1253-1260.
- Hsiao EI, et al. Utility of fiberoptic bronchoscopy before bronchial artery embolization for massive hemoptysis. AJR Am J Roentgenol 2001;177(4):861-867.
- Fishman AP, Elias JA. Fishman’s Pulmonary Diseases and Disorders, 4th ed. New York: McGraw-Hill Medical; 2008.
- Jean-Baptiste E. Management of hemoptysis in the emergency department. Hospital Physician 2005;41(1):53-59.
- Sakr L, Dutau H. Massive hemoptysis: An update on the role of bronchoscopy in diagnosis and management. Respiration 2010;80(1):38-58.
- Moen CA, Burrell A, Dunning J. Does tranexamic acid stop haemoptysis? Interact Cardiovasc Thorac Surg 2013;17(6):991-994.
- Prutsky G, Domecq JP, Salazar CA, Accinelli R. Antifibrinolytic therapy to reduce haemoptysis from any cause (Review). The Cochrane Collaboration, John Wiley & Sons 2012;4:1-18
- Wong LT, et al. Treatment of recurrent hemoptysis in a child with cystic fibrosis by repeated bronchial artery embolizations and long-term tranexamic acid. Pediatr Pulmonol 1996;22(4):275-279.
- Abal AT, Nair PC, Cherian J. Haemoptysis: Aetiology, evaluation and outcome — a prospective study in a third-world country. Respir Med 2001;95(7):548-552.
- Yoon YC, et al. Hemoptysis: Bronchial and nonbronchial systemic arteries at 16-detector row CT. Radiology 2005;234(1):292-298.
- Khalil A, et al. Utility of high-resolution chest CT scan in the emergency management of haemoptysis in the intensive care unit: Severity, localization and aetiology. Br J Radiol 2007;80(949):21-25.
- Revel MP, et al. Can CT replace bronchoscopy in the detection of the site and cause of bleeding in patients with large or massive hemoptysis? AJR Am J Roentgenol 2002;179(5):1217-1224.
- Haponik EF, Fein A, Chin R. Managing life-threatening hemoptysis: Has anything really changed? Chest 2000;118(5):
1431-1435. - Hirshberg B, et al. Hemoptysis: Etiology, evaluation, and outcome in a tertiary referral hospital. Chest 1997;112(2):
440-444. - Gong H, Jr., Salvatierra C. Clinical efficacy of early and delayed fiberoptic bronchoscopy in patients with hemoptysis. Am Rev Respir Dis 1981;124(3):221-225.
- Uflacker R, et al. Management of massive hemoptysis by bronchial artery embolization. Radiology 1983;146(3):627-634.
- Antonelli M, et al. Bronchial artery embolization for the management of nonmassive hemoptysis in cystic fibrosis. Chest 2002;121(3):796-801.
- Remy J, et al. [Treatment, by embolization, of severe or repeated hemoptysis associated with systemic hypervascularization]. Nouv Presse Med 1973;2(31):2060.
- Chun JY, Morgan R, Belli AM. Radiological management of hemoptysis: A comprehensive review of diagnostic imaging and bronchial arterial embolization. Cardiovasc Intervent Radiol 2010;33(2):240-250.
- Kalva SP. Bronchial artery embolization. Tech Vasc Interv Radiol 2009;12(2):
130-138. - Kato A, et al. Bronchial artery embolization for hemoptysis due to benign diseases: Immediate and long-term results. Cardiovasc Intervent Radiol 2000;23(5):351-357.
- Mal H, et al. Immediate and long-term results of bronchial artery embolization for life-threatening hemoptysis. Chest 1999;115(4):996-1001.
- Ramakantan R, et al. Massive hemoptysis due to pulmonary tuberculosis: Control with bronchial artery embolization. Radiology 1996;200(3):691-694.
- Park HS, et al. Bronchial artery and systemic artery embolization in the management of primary lung cancer patients with hemoptysis. Cardiovasc Intervent Radiol 2007;30(4):638-643.
- Cowling MG, Belli AM. A potential pitfall in bronchial artery embolization. Clin Radiol 1995;50(2):105-107.
- Ponnuswamy I, et al. 64-detector row CT evaluation of bronchial and non-bronchial systemic arteries in life-threatening haemoptysis. Br J Radiol 2012;85(1017):e666-672.
- Vinaya KN, White RI, Jr., Sloan JM. Reassessing bronchial artery embolotherapy with newer spherical embolic materials. J Vasc Interv Radiol 2004;15(3):304-305.
- Hiebert CA. Balloon catheter control of life-threatening hemoptysis. Chest 1974;66(3):308-309.
- Brandes JC, Schmidt E, Yung R. Occlusive endobronchial stent placement as a novel management approach to massive hemoptysis from lung cancer.
J Thorac Oncol 2008;3(9):1071-1072. - Kaminski J. [Frequency and causes of hemoptysis and role of bronchoscopy in patients with normal chest roentgenogram hospitalized in the Department of Physiopneumonology Silesian Medical University in the years 1961-1996]. Pneumonol Alergol Pol 2001;69(11-12):663-668.
- Remy-Jardin M, et al. Bronchial and nonbronchial systemic arteries at multi-detector row CT angiography: Comparison with conventional angiography. Radiology 2004;233(3):741-749.
- Paul S, et al. Prevalence and outcomes of anatomic lung resection for hemoptysis: An analysis of the nationwide inpatient sample database. Ann Thorac Surg 2013;96(2):391-398.
- Dweik RA, Stoller JK. Role of bronchoscopy in massive hemoptysis. Clin Chest Med 1999;20(1):89-105.
- Ong TH, Eng P. Massive hemoptysis requiring intensive care. Intensive Care Med 2003;29(2):317-320.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
