Fractures in Older Adults
May 1, 2014
Reprints
AUTHORS
Lauren T. Southerland, MD, Department of Emergency Medicine, The Ohio State University School of Medicine, Columbus
Michael Barrie, MD, Department of Emergency Medicine, The Ohio State University School of Medicine, Columbus. James Falk, MD, Department of Emergency Medicine, The Ohio State University School of Medicine, Columbus
PEER REVIEWER
Jay Menaker, MD, FACEP, Associate Professor of Surgery/ Emergency Medicine, University of Maryland School of Medicine, Baltimore; Medical Director, Lung Rescue Unit, R Adams Cowley Shock Trauma Center, Baltimore
As the population ages and continues to retain an increasingly high level of function, including driving and recreational activities, a unique pattern of injuries is emerging in older patients. The authors review risk factors for fractures, impact of comorbidities, and unique aspects for management strategies.
— Ann M. Dietrich, MD, Editor
Executive Summary
- Five-year survival after an osteoporotic hip fracture is similar to that of patients with breast or other cancer. Almost one in 13 (7.5%) of those with fragility fractures will die within 90 days of fracture.
- Each standard deviation decrease in BMD increases the relative risk of fracture by 1.5. Nearly all 80-year-old women have low BMD, with 27% being osteopenic and 70% osteoporotic.
- Thoracic and lumbar vertebral fractures are common from low-impact or high-impact trauma, and are estimated at 27% of fragility fractures.
- Patients diagnosed with a fracture in the ED should be considered high risk for future fractures and referred for preventative care, such as BMD testing, initiation of low BMD treatment, geriatric assessment, or home safety assessment.
Introduction
Older adults, adults 65 years and older, have both an increased rate of trauma and an increased predisposition to injury from even minimal force. This makes older adults a high-risk population for traumatic fracture from high- or low-impact mechanisms. High-impact fractures occur from falls from a height, motor vehicle collisions (MVCs), and sporting injuries. The number of high-impact fractures seen in older adults will continue to increase over the next 15 years as the U.S. population ages. For example, by 2030, motor vehicle crashes involving drivers older than 65 years are projected to increase 178%, and older adults will account for 25% of total driver fatalities.1 High-impact fractures have high mortality rates, and even those who survive to discharge have increased mortality over the following year.2 Surprisingly, MVCs are not the most common or the deadliest causes of fractures in older adults. Low-impact fractures, commonly called fragility fractures, have even higher mortality. Older patients with injuries from a fall have five times the mortality that their same age colleagues have from injuries from MVCs.3 Five-year survival after an osteoporotic hip fracture is similar to that of patients with breast or other cancer.4 Almost one in 13 (7.5%) of those with fragility fractures will die within 90 days of fracture.5 Low-impact fractures from falls at standing height or lower are commonly associated with decreased bone mineral density (BMD). Falls resulted in 13.5% of older adult emergency department (ED) visits in 2010, and a fracture was the most common injury noted.6,7 In total, U.S. older adults suffered from 2.5 million fractures in 2009-2010.8
A fracture can be a devastating blow to an older adult’s health and independence, decreasing functional status and quality of life permanently.9 While some may recover their independence, half of older adults will require home health care in the 6 months following a fracture, and many will have long-term functional decline.10 Spine, hip, or upper leg fractures decrease long-term quality of life just as much as chronic diseases such as diabetes or chronic lung disease.11 Acutely, the pain and shock of an injury may precipitate delirium, complicating diagnosis and treatment, increasing the need for further medication, and increasing the rate of long-term cognitive deficits. In addition to the morbidity related to the initial fracture, the risk of further falls and subsequent fractures is also greatly increased. Almost a quarter of older adults will have a second fracture within the next 5 years, and the risk of hip fracture is 17-fold higher in the first month after a fragility fracture.12-14 Understanding the risk factors for fractures, the effects of common comorbidities, the differences in the type of fractures seen in older adults, and the different management strategies is important to optimize the care of this high-risk population.
Fracture Risk Factors in Older Adults
Due to the physiologic changes of aging as well as common comorbidities, older adults are at high risk for fractures. Difficulties with gait, vision, and proprioception (due to neuropathy or medications) contribute to falls. Household hazards such as throw rugs and lintels can contribute to falls. The utility of different fall risk interventions was assessed in a recent Cochrane Review.15
While interventions to prevent falls have had only moderate success, treatment of low bone mineral density (BMD) has been shown to significantly reduce fracture rates. Low BMD is classified as osteoporosis (< 2.5 standard deviations below normal) or osteopenia (between 1 and 2.5 standard deviations below normal) based on hip or vertebral DXA scan. Osteoporosis affects more than 10 million Americans, in addition to the numbers of untested older adults or those with only osteopenia. Each standard deviation decrease in BMD increases the relative risk of fracture by 1.5.16 Nearly all 80-year old-women have low BMD, with 27% being osteopenic and 70% osteoporotic.17 Men especially may not know that they have low BMD, as the screening rate in the United States for older men is as low as 11%.18 Despite the lack of screening, men account for more than 25% of osteoporosis-related fractures.19 As BMD testing currently is not feasible in the ED setting, any adult with a fracture (high or low impact) should be referred for outpatient testing. In older adults without osteoporosis, fracture risk factors include falls in the prior 12 months, any prior fractures, and any decrease in BMD.20 Risk stratifying patients by BMD alone or even by FRAX guidelines (World Health Organization screening guidelines) may not be sufficient to identify patients at high risk for fracture.21 Therefore, all older adults should be considered to be high risk for fracture, and imaging should be ordered liberally.
Multiple medical conditions also increase the risk of fracture. Any condition requiring chronic glucocorticoid use, such as inflammatory bowel disease, celiac disease, chronic obstructive pulmonary disease, and rheumatoid arthritis, decreases BMD.22 Neurologic, endocrine, renal, and other problems also predispose older adults to fracture. (See Table 1.) Patients on dialysis have an increased risk of fracture that is most often seen in older Caucasian females.23 An episode of acute kidney injury that requires dialysis, even if only temporarily, increases the risk of fracture.24
Other risk factors include changes in body mass index (BMI), socioeconomic factors, and prior fracture history. Low BMI is a risk factor for hip and osteoporotic fractures, but is a protective factor for lower leg fracture. High BMI is a risk factor for upper arm (humerus and elbow) and ankle fractures.25,26 Socioeconomic factors also may play a role in patient health and are especially important in the older adult population. Poverty itself is a risk factor for low BMD and fragility fractures, and the risk may begin with low socioeconomic status in childhood.27,28 The best predictor of future fracture, however, is prior fracture.22 Prior wrist fracture doubles the risk of any future fracture.29 Men with a prior non-hip, non-vertebral fracture have a 41% chance of having a second fracture within 5 years of the initial fracture.30 Further fractures decrease an older adult’s life expectancy significantly.31 Patients diagnosed with a fracture in the ED should be considered high risk for future fractures and referred for preventative care, such as BMD testing, initiation of low BMD treatment, geriatric assessment, or home safety assessment.
Medications that Contribute to Fracture Risk and Complications
In addition to chronic glucocorticoid use, many other medications have been implicated in increasing the fracture risk in the elderly. Antipsychotic use in skilled nursing facility patients increases the risk of hip fracture in the first year after initiation,32 and changes in any psychotropic medication including selective serotonin reuptake inhibitors (SSRIs) are associated with increased fall and fracture risk.33 Long-term warfarin use increases the risk of osteoporotic fractures in elderly men with atrial fibrillation (versus those with atrial fibrillation not on warfarin), but a similar effect was not noticed in women.34 Similarly, chronic levothyroxine use increases the risk of hip fracture in men but not in women.35 This gender disparity may be due to the already elevated risk in women compared to men so that the effect of medications is less apparent in women.
Anticoagulation use is also common and complicates fracture management. The use of oral anticoagulants may be associated with decreased BMD and increased fracture risk.36 The evaluation of a patient on anticoagulation with a closed fracture should include an assessment for compartment syndrome due to expanding hematomas. Open fractures in any extremity may require anticoagulation reversal and transfusion. Perioperative bleeding is especially a concern in pelvic, acetabular, femur, and tibial fractures, and these injuries frequently require transfusions.37 Patients on clopidogrel may have worse immediate outcomes with emergent surgery for hip fracture, but delaying surgery seven days to regain normal platelet function is associated with increased one-year mortality.38,39 In fact, a delay to surgery of more than 24 hours for any reason is associated with increased mortality in patients with hip fractures.40 Reversing anticoagulation reduces hospital length of stay and complications in hip fracture patients.41 Vitamin K reversal for orthopedic trauma patients on warfarin is both effective and cost effective.42
Treatment of underlying predisposing factors such as reversal of anticoagulation (if indicated) and abnormal bone mineral density treatment can decrease morbidity and mortality. Treatment with calcium and vitamin D reduces overall three-year mortality from a hip fracture in men by 43% and in women (with the addition of anti-osteoporotic medications) by 36%.43 The addition of calcium and vitamin D in the first six weeks after a proximal humerus fracture has been shown to increase callus formation and BMD.44 Oral vitamin supplementation of 700-800 IU must be given to achieve this effect, which is greater than the typical 400 IU in multivitamins.45,46 The effect of osteoporosis treatment on morbidity and mortality for other types of fragility fractures is not as well characterized. Given the benign side-effect profile of vitamin D supplementation, we recommend all older adults with fractures be discharged on vitamin D supplementation with follow up by their primary care physician. Overall, older adults with fractures would benefit from a full medication review with attention to risks for immediate fracture treatment, as well as subsequent fracture prevention.
Table 1. Common Comorbidities that Increase the Risk of Fracture in Older Adults9,98,16,17
| Gastrointestinal | Inflammatory bowel disease, celiac disease |
| Neurologic | Multiple sclerosis, Parkinson's disease |
| Pulmonary |
COPD, pulmonary fibrosis with steroid use |
| Endocrine | Type 1 diabetes, Addison's disease |
| Hematologic | Hemophilia A, hemophilia B |
| Renal |
End stage renal disease and possibly long-term renal insufficiency |
| Rheumatologic | Rheumatoid arthritis |
| Oncologic | Cancer with bony metastases |
Table 2. Incidence of Fractures in Older Adult Men and Women30,53,54,70,73,83,99-101
| Fracture | Incidence (per 10,000 patient years) | |
|---|---|---|
| Women | Men | |
| Lower vertebral- clinical and incidental‡ | 680 | 700 |
| Hip‡ | 50-76 | 33-36 |
| C-spine** | 18-85 | 18-85 |
| Non hip, non vertebral, low trauma‡ | 154 | 78 |
| Distal Radius† | 75 | 19 |
| Ankle* | 58 | 24 |
| Proximal Humerus†† | 42 | 15 |
| Rib | 40© | 35* |
| Overall | 2 million /year | |
Overview of Common Fractures
Older adults are prone to different fractures and fracture mechanisms than a younger cohort. The fracture incidences tend to change after age 50, when post-menopausal changes to BMD start. The most common fractures in older adults are vertebral fracture from compression or trauma, followed by hip and distal radius fractures. (See Table 2.) One in two women and one in five men will suffer from an osteoporotic fragility fracture, which is defined as any low-energy trauma fracture. The most common fragility fractures are proximal humerus, hip, distal radius, and spinal fractures.
Thoracic and Lumbar Vertebral Fractures
Thoracic (see Figure 1) and lumbar vertebral fractures (see Figure 2) are common from low-impact or high-impact trauma, and are estimated at 27% of fragility fractures.19 Degenerative changes in the more mobile thoracolumbar junction and lumbar spine place older adults at higher risk for injuries to this area in high-impact traumas such as MVCs. Trauma registries demonstrate that the oldest old (80+ years) tend to have more upper thoracic and T-L junction injuries, while the younger old (60-79 years) may have more lumbar spinal fractures. Younger adults tend to have flexion-distraction fractures, while older adults suffer the higher mortality extension fractures.47 Stable compression fractures or mild burst fractures seen on X-ray and without neurologic symptoms may not need further imaging, but it is important to recognize that significant soft-tissue injuries can be missed with these injuries, and CT or MRI may better clarify the extent of the injury. Helical spine CT is 99% accurate in identifying spinal fractures, as compared to 87% accuracy of 2-view thoracolumbar X-rays (which may be even less accurate with low BMD). CT also aids in the assessment of fracture age and acuity.48 Acute vertebral fractures have a three-year survival rate of 40-60% depending on the type of treatment. Acute fractures can be treated with analgesics only, or treated surgically with balloon kyphoplasty or vertebroplasty, which is best done in the first two months after an acute fracture.49 Surgical treatment decreases mortality and chronic pain and increases quality of life compared to medical management.50,51
Figure 1. Multiple Thoracic Spine Fractures
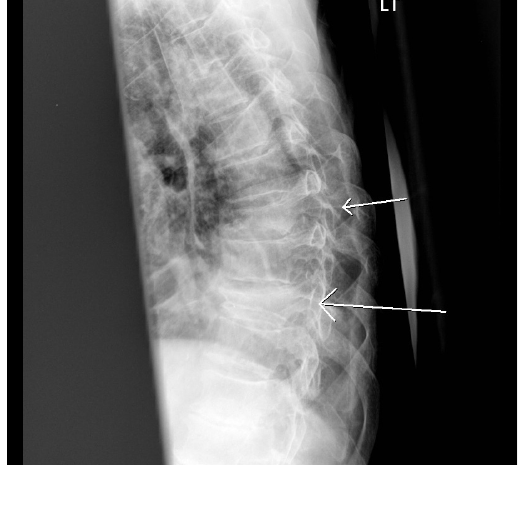
Figure 2. L1 Compression Fracture
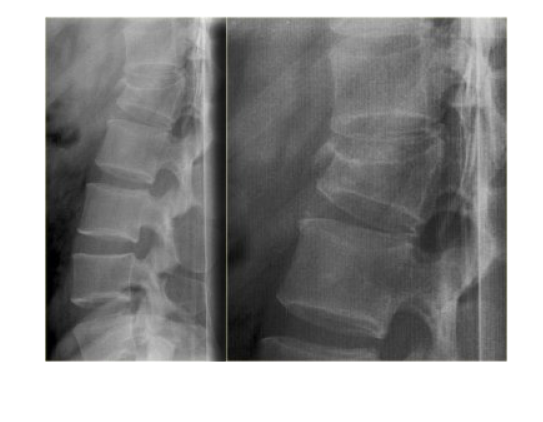
Thoracic and lumbar compression fractures from low BMD or low-impact trauma are a significant health problem. The prevalence is around 20% in both women and men 70 years and older, and most are between T6 and L1.52 Asymptomatic compression fractures are often noted on routine chest X-rays. In one study of women with one or more risk factors for compression fractures, 31% had an undiagnosed moderate or severe vertebral fracture, and of these women, 75% did not have osteoporosis on DXA scan.53 Additionally, 18% may develop a new compression fracture in the year following diagnosis of the initial compression fracture.51 Therefore, prevention is very important, even if these fractures are asymptomatic. ED referral or discussion with the patient about treatment options is also important, as most compression fractures will be treated on an outpatient basis unless there is uncontrollable pain or concern for cord injury.
Hip Fractures
Hip fractures (fractures of the proximal femur, including subcapital neck, intertrochanteric, subtrochanteric, and others) are some of the most common types of fragility fractures and are associated with the highest mortality. The incidence of hip fractures worldwide may be decreasing slightly due to implementation of national screening guidelines and preventative treatment .54 (See Table 2.) Women more commonly suffer hip fractures at a rate of 4.5:1, but this difference is minimized after age 70.55 Other risk factors may include low vitamin K and vitamin D levels.56
The clinical presentation of hip fracture classically occurs after a fall in an older individual, but can present after any type of traumatic injury. In most instances, a hip fracture can be diagnosed from the history and physical exam. Patients are usually unable to bear weight on the affected side, have tenderness to palpation over the greater trochanter, and pain with external rotation, abduction, or axial loading of the hip. More obvious fractures will present with the leg in external rotation and shortened. The diagnostic imaging modality of choice is plain film X-rays of hip (see Figure 3), but CT or MRI may help characterize more subtle fractures, as X-rays are only 90-98% sensitive.57 Occult, or X-ray-negative hip fractures, make up 3-9% of hip fractures. Currently, MRI is the gold standard for the detection of occult fractures and should be considered in any at-risk patient unable to bear weight after a traumatic event.57
Figure 3. Hip Fracture
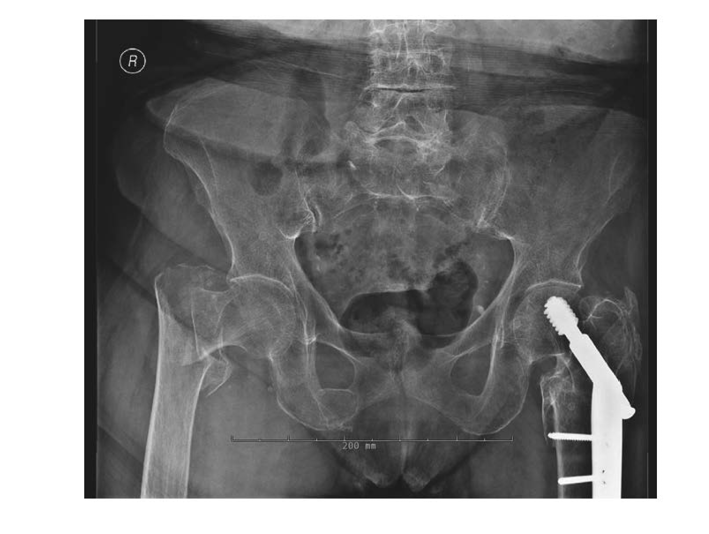
Treatment strategies include various surgical options. It is important to optimize pre-operative health, but delays in surgery have been shown to increase mortality.38-40 Older adult patients commonly experience peri-operative complications such as hypoxia, delirium, anemia requiring transfusion, congestive heart failure, acute renal injury, and myocardial infarction.58 The most common post-operative complications are pneumonia, acute renal injury, and pressure ulcers.59 The risk of mortality is much higher in those who suffer one or more complications. Those at highest risk of mortality and complications include patients on dialysis, those presenting in shock, patients with obesity, history of cardiopulmonary disease, diabetes, or a delay to surgery of more than 48 hours.59 In high-impact trauma patients, such as MVCs or motorcycle collisions, patients with any type of femur fracture (hip or distal) are more likely to have a perioperative MI; however, overall their mortality is similar to other older adult trauma patients without a femur fracture.60 Despite definitive surgical management, hip fractures in the elderly have a high mortality rate of 8.1% at 30 days and 21.6% at one year,58 and a similar five-year survival rate as breast cancer patients.4 For those who survive, many do not regain their previous level of functioning and require skilled nursing care or home health assistance. The emergency physician can decrease morbidity and mortality by having a low threshold to proceed to CT or MRI to rule out occult fracture, facilitating pre-operative clearance (decreasing time to surgery), and discussing delirium and pressure ulcer prevention with family and staff. Depending on the anesthesia and hospitalist staff, pre-operative clearance usually involves a pulmonary exam and chest X-ray, a cardiac exam with EKG and possibly echocardiogram if the patient has a history of heart failure or valve disorders, and a medication review. Pre-operative labs such as a type and cross, coagulation parameters (PT and PTT), and basic blood counts and chemistries are also required. Many of these tests can be obtained quickly in the ED.
Cervical Spine Fracture
Cervical spine (c-spine) injury (see Figures 4 and 5) is a significant cause of morbidity and mortality in the geriatric trauma patient. Older adults account for 19% of c-spine injuries,61 but the likelihood of a c-spine injury is twice as high as that for a younger trauma patient,62 with many requiring surgical intervention. Rollover motor vehicle accidents and older age increase the risk of c-spine fracture.63 Low-impact mechanisms, however, cause more than 50% of c-spine fractures.61 The injury pattern in older patients with cervical injury is also different than in younger patients. Due to the decreased range of motion of the cervical spine, elderly patients are more likely to sustain higher level c-spine fractures (see Figures 6 and 7), while younger patients are more likely to sustain lower c-spine injury. Elderly patients are also more likely to have additional intracranial injuries compared to younger patients.
Figure 4. Cervical Spine Fracture
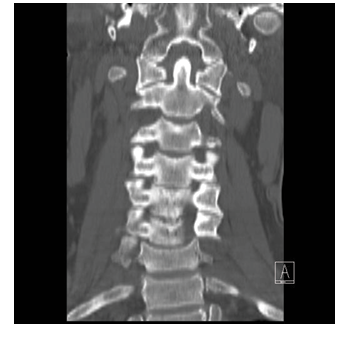
Figure 5. Cervical Spine Fracture
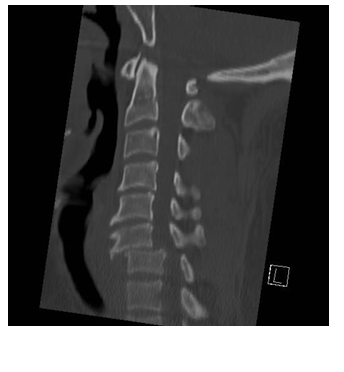
Figure 6. C1 Fracture
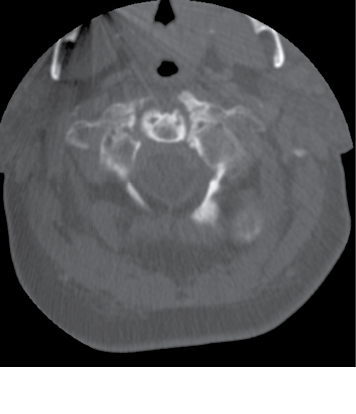
Figure 7. C2 Fracture
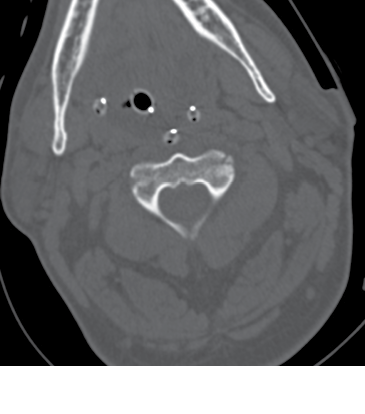
The diagnosis of c-spine fractures in the elderly can be elusive. The NEXUS study provides practitioners with a set of clinical criteria that, if met, put the patient in a very low risk category for c-spine injury.64 This landmark study did include a sufficient number of geriatric patients, and a geriatric subgroup analysis shows 100% sensitivity for clinically significant injuries.62 However, many are reluctant to apply this clinical decision rule in the geriatric population due to the number of older adults with fractures from minimal trauma with minimal symptoms.65,66 Various retrospective studies describe limitations,63,67 but no clear prospective evidence has shown these criteria to be inferior in the geriatric population. The Canadian C-spine Criteria uses age 65 and greater as a high-risk feature that requires imaging, but fewer clinicians use these criteria, as it is a more complicated algorithm to implement.65 The clinical exam is difficult in geriatric patients, as they commonly have decreased range of motion at baseline, baseline pathology that can make plain films difficult to interpret, and may have clinically significant spinal injuries with minimal symptoms. Therefore, CT (see Figure 8) should be the first imaging used to evaluate for c-spine injury in older patients.
Figure 8. C4 Fracture
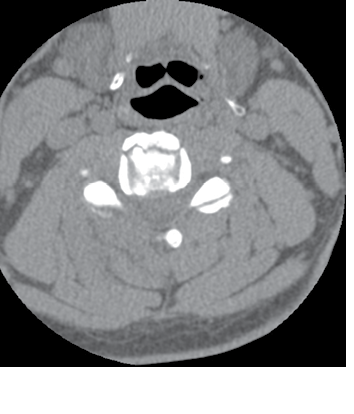
Treatment options include non-operative immobilization with cervical collar or surgery for internal fixation. Type II dens fractures are the most common type of cervical fracture in the elderly, and, thus, the best studied to determine the benefits from surgery. Some findings show protective effects with surgery in younger populations of geriatric patients.68 Other non-randomized studies have shown a functional and mortality benefit with surgical intervention in those patients healthy enough to undergo surgery.69 The only available studies to guide treatment options are limited to retrospective, uncontrolled studies. The decision to operate on cervical spine fractures in older adults depends on previous functional status and comorbidities in addition to the clinical judgment of the neurosurgical team. Despite intervention, mortality with c-spine injury is high; one-year mortality from dens fractures comparable to hip fractures at 37.5%.70
Distal Forearm Fractures
Distal forearm fractures account for 19% of osteoporosis-related fractures19 and are almost always caused by a fall on an outstretched hand or an MVC. (See Figures 9 and 10.) Theoretically, as balance and motor coordination decrease with age, older women are more likely to fall onto their hip than an outstretched hand. However, the incidence of distal radius fracture still increases with age, with an increase from 34 per 10,000 patient years in women ages 50-54 to 101 in those 85 years and older.71 This is more than double the incidence in men. Women are four times more likely to have a distal radius fracture overall, but men are five times more likely than women to have a high-impact fracture.71 Older adults with distal radius fractures have a tendency toward better health than their peers with proximal humerus or hip fractures, and distal forearm fractures do not appear to increase mortality.72 However, there is still an increased risk for further fractures.12 Emergency department management includes a high index of suspicion in any older adult with wrist pain, and splinting or orthopedic consultation, as indicated, based on the severity and displacement of the fracture. While the patient population with distal forearm fractures tend to be high functioning, their ability to compensate for the immobilization of one hand may be decreased, especially if they normally walk with an assistive device. A home safety and functional assessment is indicated prior to discharge, with admission for rehabilitation placement if needed.
Figure 9. Distal Forearm Fracture
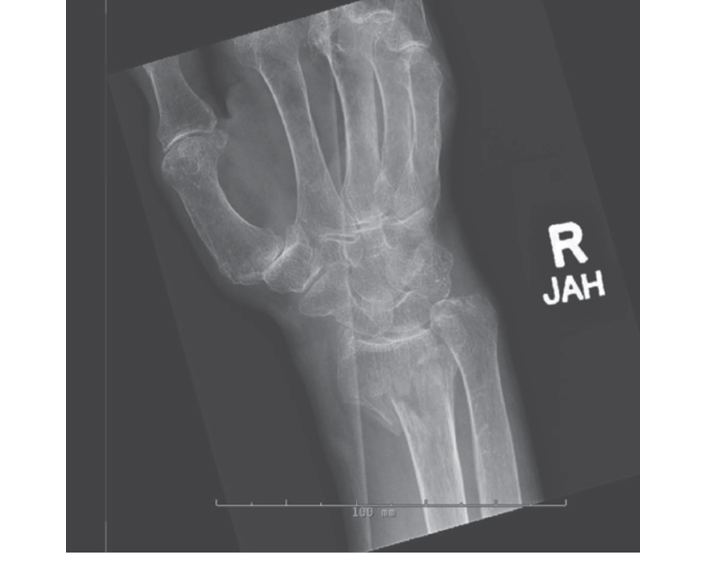
Figure 10. Distal Forearm Fracture
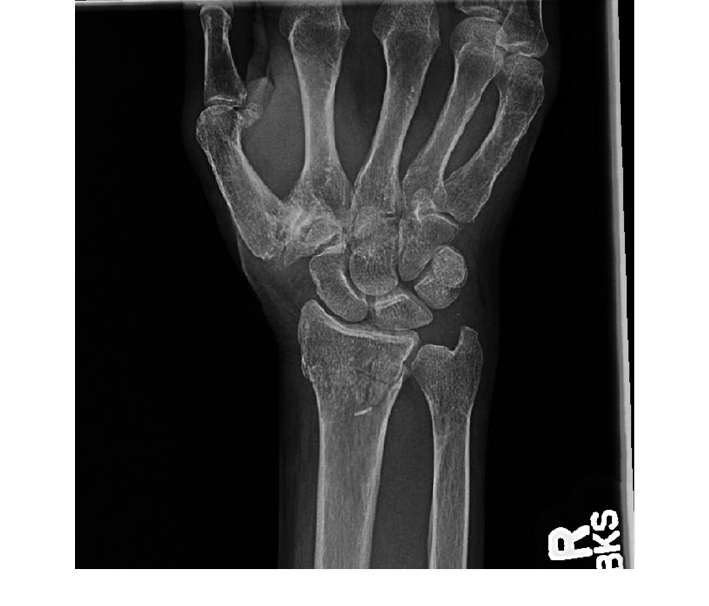
Ankle and Other Lower Extremity Fractures
Ankle, knee, and foot fractures are often seen after falls. Older adults suffer 20-30% of foot and ankle fractures, with an incidence of 42/10,000.73,74 In addition to the risk factors for any fracture, an elevated BMI is associated with a higher risk for ankle fractures.75 X-rays are usually sufficient to diagnose fractures. Surgical intervention is needed frequently for trimalleolar fractures (74%), but less frequently for isolated malleolar fractures (11-22%).74 Surgical repair in patients with increasing age, diabetes, or smoking history have a complication rate greater than 20%, but surgery may provide improved long-term function.76 A comparison of adults older than 70 years of age with ankle fractures treated conservatively (reduction and casting) versus operatively found that more than 25% of the conservative group had failure and required surgery at a later stage. Additionally, 72% of those treated operatively returned to their prior weight-bearing levels of activity, as opposed to only 42% in the conservative group.77 Operative ankle fractures should be treated aggressively without prolonged delay to reduce the rate of wound and other complications.78,79 Patella fractures usually occur from direct fall onto the knee. Depending on extensor tendon disruption and comminution, these may be treated operatively or conservatively. Both treatment courses result in 82% of patients returning to their prior functional status.80
Knee, foot, and ankle fractures may not be associated with low BMD as frequently as distal radius or vertebral fractures.81 However, these patients should still be referred for testing for low BMD to ensure appropriate treatment. Treatment of any older adult with a lower extremity fracture should also include a safety assessment with assistive devices, as many of these patients may not be able to appropriately use crutches or a walker with a cast or splint on a lower extremity.
Proximal Humerus Fractures
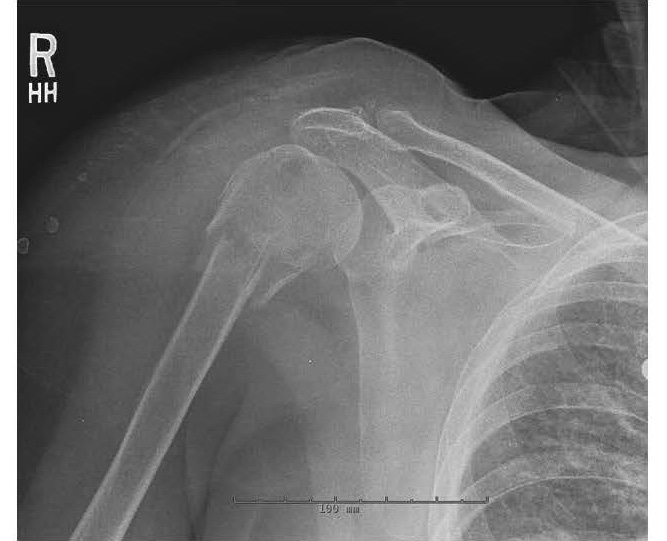
Men and women share similar risk factors for proximal humerus fractures, most notably decreased BMD.82 In addition to low BMD and falls risk factors, antiepileptic use, diabetes mellitus, obesity, and left-handedness all increase the risk of proximal humerus fracture.83 The risk increases with age, starting around 45 years old and peaking around 85 years old.84 Older adults with proximal humerus fractures tend to be less physically and mentally impaired than age-matched colleagues with hip fractures, but they still have increased mortality in the initial year after fracture.72 Women account for two-thirds of proximal humerus fractures in older adults, while men make up a greater proportion in younger adults. (See Figure 11.) Additionally, these fractures are more likely to be complicated by comminution or displacement in older adults.85 In non-displaced fractures, there is insufficient evidence to recommend surgery versus immobilization, and, therefore, most non-displaced proximal humerus fractures are treated with a shoulder immobilizer and early physical therapy.86 Despite treatment, proximal humerus fractures can decrease quality of life and independence chronically. If patients have not recovered good range of motion and strength within a year, they will continue to have chronic difficulties.87 Additionally, this fracture may decrease a patient’s ability to use adaptive equipment such as a walker, cane, or grab bars; a home healthcare needs and safety assessment should be done prior to discharging a patient who may not be able to maintain independence with this injury.
Figure 11. Proximal Humerus Fracture
Facial Fractures
The most common mechanisms resulting in facial fractures include falls (50%) and motor vehicle crashes (20%).88,89 These fractures are associated with significant morbidity and mortality, with up to 11% in-hospital mortality.88,89 The most common facial bone injured is the mandible (18%) (see Figures 12 and 13) and then the orbital floor (15%) (see Figure 14) and zygoma (15%) (see Figure 15). Providers should be aware that facial fractures along with upper extremity injuries are the most common presentations of elder abuse. Particular care should be taken to explore possible abuse in high-risk situations, such as when there is a culture of violence in the family or a vulnerable patient with dementia or social isolation.90 If there is any concern for safety, the patient should be admitted until a full social work evaluation can be done.
Figure 12. Bilateral Mandibular Fracture
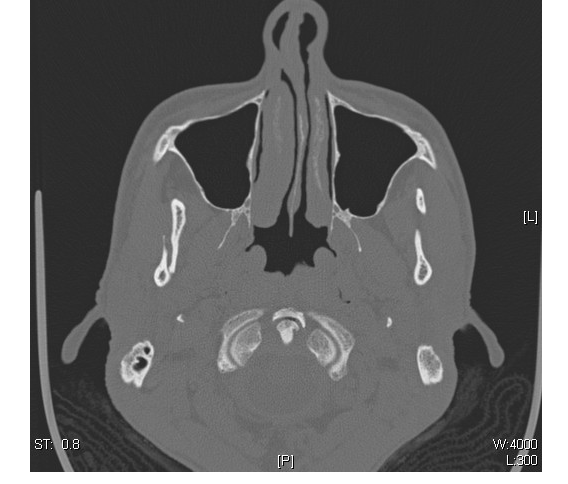
Figure 13. Bilateral Mandibular Fracture
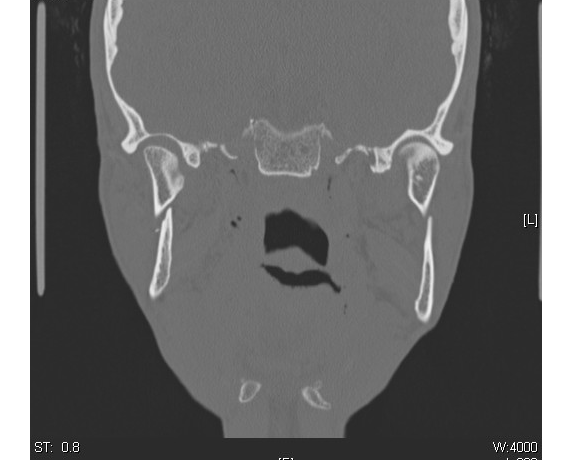
Figure 14. Orbital Floor Fracture
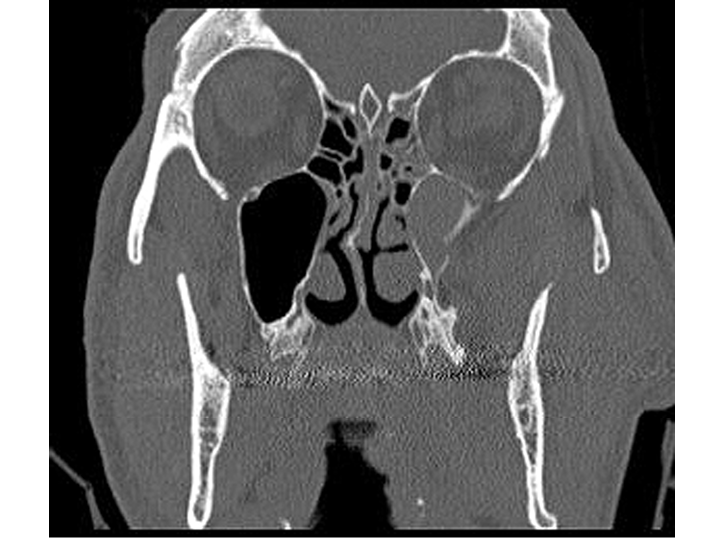
Figure 15. Zygoma Fracture
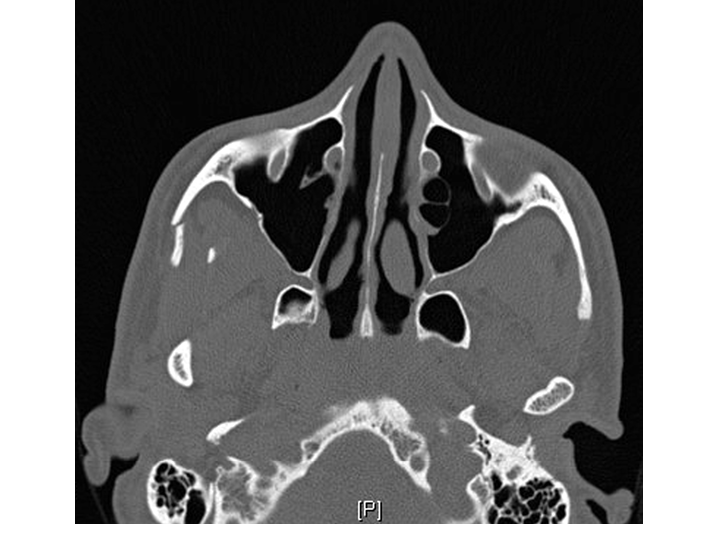
Patients with any trauma and concerning bruising or tenderness of the face should undergo maxillofacial CT imaging. Patients with facial fractures may also sustain other injuries, including brain, extremity fractures, cervical spine fracture, and spinal cord injuries. Additional imaging, such as non-contrast CT of the brain or CT angiography, may be indicated to evaluate for intracranial pathology or blunt carotid injury. The majority of facial fractures in older adults are managed non-operatively.88,89 In one clinical series, 30% of patients died before any operative intervention, 65.9% had non-operative management, and only 5% required internal fixation.
Mandible and LeFort fractures are the most likely to require operative intervention. Functional and cosmetic outcomes that affect quality of life determine the need for intervention. Fractures that interfere with mastication and jaw function are likely to be more problematic for long-term quality of life if left untreated.91 In another reported series, open reduction was used in 28.8% of patients, 26.9% were treated with closed reduction, and 44.2% did not undergo any treatment.92 The variation in treatment for similar fractures again may be dependent upon the baseline characteristics of the patient, including comorbidities and functional status. Emergency department management includes a low suspicion for facial imaging, adequate pain control, and a thorough evaluation of function, including neurologic status, extraocular movements, and ability to masticate and swallow, in addition to specialist consultation as needed.
Rib Fractures
Ribs are commonly fractured in high-impact mechanisms. In trauma registries, rib fractures are found in 38% of admitted older adults.93 Diagnosing rib fractures can be difficult, as plain films have low sensitivity, missing 50% of rib fractures. CT imaging of the chest, however, is highly sensitive. In clinical practice, rib fractures missed on plain films do not seem to impact clinical outcomes. One retrospective study found that any rib fracture or pulmonary contusion identified on plain films (see Figure 16) increased the incidence of pulmonary morbidity and mortality, whereas fractures identified only by CT did not increase mortality rates.94
Figure 16. Rib Fractures with Hemothorax
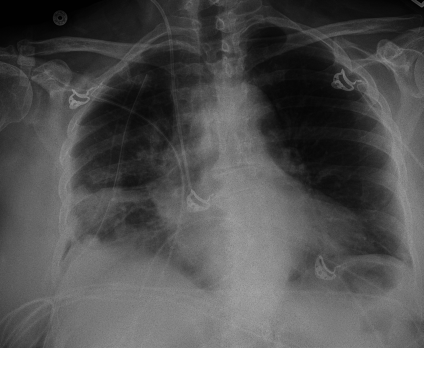
Compared to the younger patient, older adults with rib fractures have greater incidence of morbidity (days on ventilator, pneumonia, etc.), along with an increased mortality. In one series, elderly patients with rib fractures suffered a mortality rate of 22%, compared to 10% for younger patients.93,95 Also, the number of rib fractures correlates with increased morbidity and mortality. Geriatric patients had significantly increased mortality rates if they suffered three or more rib fractures. The incidence of complications of pneumonia or ARDS was also linearly associated with the number of rib fractures. A recent meta-analysis showed that age greater than 65, three or more rib fractures, pre-existing conditions, and pneumonia were strong predictors of mortality in patients with blunt traumatic chest wall injury.96 In addition to increasing morbidity and mortality, a rib fracture in a post-menopausal woman (≥ 45 years old) increases the risk of further rib fracture by fivefold and the risk of any other fractures by more than double. Despite their association with MVC and high-energy trauma, rib fractures in post-menopausal women and older adults are associated with osteoporosis, and these patients should be referred for testing and treatment.97
Treatment of isolated rib fractures is largely supportive and often done as an outpatient. Analgesia is important, as pain from rib fractures generates shallow breathing, leading to atelectasis and susceptibility to pneumonia. Some authors support the use of perioperative epidural anesthesia, which has been shown in limited studies to decrease morbidity and mortality.95 This may limit the need for narcotic analgesia, which is associated with falls, over-sedation, and constipation in older patients. However, there have been no randomized trials to evaluate the potential benefits of epidurals. Surgical intervention may be warranted to improve ventilation when there are significant rib fractures or flail chest that is limiting the mechanical pull of the chest wall.98 Incentive spirometers should be prescribed and instructions given to continue ambulation and deep breathing. If there are multiple comorbidities, concerns about the side effects of analgesics, or concerns about patient understanding, admission for initial pain control and pulmonary toilet is warranted.
Conclusions
Older adults have high rates of fractures, which are associated with higher morbidity, higher mortality, and more frequent social and home health care complications than in younger patients. Any fracture in an older adult may be complicated by low BMD, and all should be referred for testing and treatment. Starting vitamin D supplementation and referring for outpatient BMD testing can be done from the emergency department in order to improve healing and prevent subsequent fractures. Physicians must also give increased attention to a patient’s social situation and ability to care for the injury at home. Physicians should be aware of occult fractures, or X-ray-negative fractures, especially when a patient has persistent pain or inability to ambulate. Once identified, older adults with fractures should be treated swiftly and aggressively. When surgical repair is indicated, it should not be delayed due to the patient’s age, as delays more than 24 hours are associated with higher complication risks. Overall, this is a high-risk population prone to repeat injury that should be treated cautiously, with extra attention given to comorbidities, home safety, and future fracture prevention.
References
- Lyman S, Ferguson SA, Braver ER, Williams AF. Older driver involvements in police reported crashes and fatal crashes: trends and projections. Inj Prev 2002;8:116-120.
- Soba KS, Dong F, Ward JG, et al. Octogenarians and motor vehicle collisions: postdischarge mortality is lower than expected. J Trauma Acute Care Surg 2013;75:1076-1080; discussion 80.
- Sampalis JS, Nathanson R, Vaillancourt J, et al. Assessment of mortality in older trauma patients sustaining injuries from falls or motor vehicle collisions treated in regional level I trauma centers. Ann Surg 2009;249:488-495.
- Lee YK, Lee YJ, Ha YC, Koo KH. Five-year relative survival of patients with osteoporotic hip fracture. J Clin Endocrinol Metab 2013.
- Liem IS, Kammerlander C, Raas C, Gosch M, Blauth M. Is there a difference in timing and cause of death after fractures in the elderly? Clin Orthop Relat Res 2013;471:2846-2851.
- Albert M, McCaig LF, Ashman JJ. Emergency department visits by persons aged 65 and over: United States, 2009-2010. NCHS Data Brief 2013:1-8.
- Owens PL RC, Spector W, Mutter R. Emergency Department Visits for Injurious Falls among the Elderly, 2006. Healthcare Cost and Utilization Project Statistical Brief #80. Agency for Healthcare Research and Quality 2009.
- Betz ME, Ginde AA, Southerland LT, JMC. Emergency department and outpatient treatment of acute injuries among older adults in the United States, 2009-2010. JAGS 2014.
- Madhok R GS. Longer term functional outcome and societal implications of upper limb fractures in the elderly. J R Soc Health 1993;113:179-180.
- Becker DJ, Yun H, Kilgore ML, et al. Health services utilization after fractures: evidence from Medicare. J Gerontol A Biol Sci Med Sci 2010;65:1012-1020.
- Adachi JD, Adami S, Gehlbach S, et al. Impact of prevalent fractures on quality of life: Baseline results from the global longitudinal study of osteoporosis in women. Mayo Clin Proc 2010;85:806-813.
- Chen CW, Huang TL, Su LT, et al. Incidence of subsequent hip fractures is significantly increased within the first month after distal radius fracture in patients older than 60 years. J Trauma Acute Care Surg 2013;74:317-321.
- Ettinger B, Ray GT, Pressman AR, Gluck O. Limb fractures in elderly men as indicators of subsequent fracture risk. Arch Intern Med 2003;163:2741-2747.
- Bliuc D, Nguyen ND, Nguyen TV, Eisman JA, Center JR. Compound risk of high mortality following osteoporotic fracture and refracture in elderly women and men. J Bone Miner Res 2013;28:2317-2324.
- Gillespie LD, Robertson MC, Gillespie WJ, et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev 2012;9:CD007146.
-
Siris ES, Brenneman SK, Miller PD, et al. Predictive value of low BMD for 1-year fracture outcomes is similar for postmenopausal women ages 50-64 and 65 and Older: Results from the National Osteoporosis Risk Assessment (NORA).
J Bone Miner Res 2004;19:1215-1220. - Cooper C. Epidemiology of osteoporosis. Osteoporos Int 1999;9 Suppl 2:S2-S8.
- Lim SY, Lim JH, Nguyen D, et al. Screening for osteoporosis in men aged 70 years and older in a primary care setting in the United States. Am J Mens Health 2013;7:350-354.
- Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A. Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res 2007;22:465-475.
- Nguyen ND, Eisman JA, Center JR, Nguyen TV. Risk factors for fracture in nonosteoporotic men and women. J Clin Endocrinol Metab 2007;92:955-962.
- Aubry-Rozier B, Stoll D, Krieg MA, Lamy O, Hans D. What was your fracture risk evaluated by FRAX(R) the day before your osteoporotic fracture? Clin Rheumatol 2013;32:219-223.
- Sambrook PN, Flahive J, Hooven FH, et al. Predicting fractures in an international cohort using risk factor algorithms without BMD. J Bone Miner Res 2011;26:2770-2777.
- Wagner J, Jhaveri KD, Rosen L, Sunday S, Mathew AT, Fishbane S. Increased bone fractures among elderly United States hemodialysis patients. Nephrol Dial Transplant 2013.
- Wang WJ, Chao CT, Huang YC, et al. The impact of acute kidney injury with temporary dialysis on the risk of fracture. J Bone Miner Res 2013.
-
Johansson H, Kanis JA, Oden A, et al. A meta-analysis of the association of fracture risk and body mass index in women.
J Bone Miner Res 2014;29:223-33. - David C, Confavreux CB, Mehsen N, Paccou J, Leboime A, Legrand E. Severity of osteoporosis: What is the impact of co-morbidities? Joint Bone Spine 2010;77 Suppl 2:S103-S106.
-
Navarro MC, Sosa M, Saavedra P, et al. Poverty is a risk factor for osteoporotic fractures. Osteoporos Int 2009;20:
393-398. - Crandall CJ, Merkin SS, Seeman TE, Greendale GA, Binkley N, Karlamangla AS. Socioeconomic status over the life-course and adult bone mineral density: The Midlife in the U.S. Study. Bone 2012;51:107-113.
- Barrett-Connor E, Sajjan SG, Siris ES, Miller PD, Chen YT, Markson LE. Wrist fracture as a predictor of future fractures in younger versus older postmenopausal women: Results from the National Osteoporosis Risk Assessment (NORA). Osteoporos Int 2008;19:607-613.
- Bliuc D, Nguyen TV, Eisman JA, Center JR. The impact of nonhip nonvertebral fractures in elderly women and men. J Clin Endocrinol Metab 2014;99:415-423.
- Bliuc D, Nguyen ND, Milch VE, Nguyen TV, Eisman JA, Center JR. Mortality risk associated with low-trauma osteoporotic fracture and subsequent fracture in men and women. JAMA 2009;301:513-521.
- Rigler SK, Shireman TI, Cook-Wiens GJ, et al. Fracture risk in nursing home residents initiating antipsychotic medications. J Am Geriatr Soc 2013;61:715-722.
- Payne RA, Abel GA, Simpson CR, Maxwell SR. Association between prescribing of cardiovascular and psychotropic medications and hospital admission for falls or fractures. Drugs Aging 2013;30:247-254.
- Gage BF, Birman-Deych E, Radford MJ, Nilasena DS, Binder EF. Risk of osteoporotic fracture in elderly patients taking warfarin: Results from the National Registry of Atrial Fibrillation 2. Arch Intern Med 2006;166:241-246.
- Sheppard MC, Holder R, Franklyn JA. Levothyroxine treatment and occurrence of fracture of the hip. Arch Intern Med 2002;162:338-343.
- Caraballo PJ, Gabriel SE, Castro MR, Atkinson EJ, Melton LJ, 3rd. Changes in bone density after exposure to oral anticoagulants: A meta-analysis. Osteoporos Int 1999;9:441-448.
-
Sisak K, Manolis M, Hardy BM, Enninghorst N, Balogh ZJ. Epidemiology of acute transfusions in major orthopaedic trauma. J Orthop Trauma 2013;27:
413-418. - Nwachuku IC, Jones M, Clough TM. Clopidogrel: Is a surgical delay necessary in fractured neck of femur? Ann R Coll Surg Engl 2011;93:310-313.
- Maheshwari R, Acharya M, Monda M, Pandey R. Factors influencing mortality in patients on antiplatelet agents presenting with proximal femoral fractures. J Orthop Surg (Hong Kong) 2011;19:314-316.
- Kesmezacar H, Ayhan E, Unlu MC, Seker A, Karaca S. Predictors of mortality in elderly patients with an intertrochanteric or a femoral neck fracture. J Trauma 2010;68:153-158.
- Tal A, Rubin G, Rozen N. Treatment with vitamin K in hip fracture patients receiving warfarin. Isr Med Assoc J 2013;15:348-351.
-
Tharmarajah P, Pusey J, Keeling D, Willett K. Efficacy of warfarin reversal in orthopedic trauma surgery patients.
J Orthop Trauma 2007;21:26-30. - Nurmi-Luthje I, Luthje P, Kaukonen JP, et al. Post-fracture prescribed calcium and vitamin D supplements alone or, in females, with concomitant anti-osteoporotic drugs is associated with lower mortality in elderly hip fracture patients: a prospective analysis. Drugs Aging 2009;26:409-421.
- Doetsch AM, Faber J, Lynnerup N, Watjen I, Bliddal H, Danneskiold-Samsoe B. The effect of calcium and vitamin D3 supplementation on the healing of the proximal humerus fracture: A randomized placebo-controlled study. Calcif Tissue Int 2004;75:183-188.
- Bischoff-Ferrari HA, Willett WC, Wong JB, Giovannucci E, Dietrich T, Dawson-Hughes B. Fracture prevention with vitamin D supplementation: A meta-analysis of randomized controlled trials. JAMA 2005;293:2257-2264.
- Bischoff-Ferrari HA. Vitamin D and fracture prevention. Rheum Dis Clin North Am 2012;38:107-113.
- Rao RD, Berry C, Yoganandan N, Agarwal A. Occupant and crash characteristics in thoracic and lumbar spine Injuries resulting from motor vehicle collisions. Spine J 2014.
- Hauser CJ, Visvikis G, Hinrichs C, et al. Prospective validation of computed tomographic screening of the thoracolumbar spine in trauma. J Trauma 2003;55:228-234; discussion 34-35.
- Papanastassiou ID, Filis A, Aghayev K, Kokkalis ZT, Gerochristou MA, Vrionis FD. Adverse prognostic factors and optimal intervention time for kyphoplasty/vertebroplasty in osteoporotic fractures. BioMed Research International 2014;2014:925683.
-
Chen AT, Cohen DB, Skolasky RL. Impact of nonoperative treatment, vertebroplasty, and kyphoplasty on survival and morbidity after vertebral compression fracture in the medicare population.
J Bone Joint Surg Am 2013;95:
1729-1736. - Hubschle L, Borgstrom F, Olafsson G, et al. Real-life results of balloon kyphoplasty for vertebral compression fractures from the SWISSspine registry. Spine J 2013.
- Waterloo S, Ahmed LA, Center JR, et al. Prevalence of vertebral fractures in women and men in the population-based Tromso Study. BMC Musculoskelet Disord 2012;13:3.
- van den Berg M, Verdijk NA, van den Bergh JP, et al. Vertebral fractures in women aged 50 years and older with clinical risk factors for fractures in primary care. Maturitas 2011;70:74-79.
- Ettinger B, Black DM, Dawson-Hughes B, Pressman AR, Melton LJ, 3rd. Updated fracture incidence rates for the US version of FRAX. Osteoporos Int 2010;21:25-33.
- Chang KP, Center JR, Nguyen TV, Eisman JA. Incidence of hip and other osteoporotic fractures in elderly men and women: Dubbo Osteoporosis Epidemiology Study. J Bone Miner Res 2004;19:532-536.
- Torbergsen AC, Watne LO, Wyller TB, et al. Vitamin K1 and 25(OH)D are independently and synergistically associated with a risk for hip fracture in an elderly population: A case control study. Clin Nutr 2014.
- The Management of Hip Fracture in Adults [Internet]. In: (UK) NCGC, ed. London: Royal College of Physicians (UK); 2011.
- Chia PH, Gualano L, Seevanayagam S, Weinberg L. Outcomes following fractured neck of femurin an Australian metropolitan teaching hospital. Bone Joint Res 2013;2:162-168.
- Belmont PJ, Jr., Garcia EJ, Romano D, Bader JO, Nelson KJ, Schoenfeld AJ. Risk factors for complications and in-hospital mortality following hip fractures: A study using the National Trauma Data Bank. Arch Orthop Trauma Surg 2014.
- Patel KV, Brennan KL, Davis ML, Jupiter DC, Brennan ML. High-energy femur fractures increase morbidity but not mortality in elderly patients. Clin Orthop Relat Res 2014;472:1030-1035.
-
Wang H, Coppola M, Robinson RD, et al. Geriatric trauma patients with cervical spine fractures due to ground level fall: Five years experience in a level one trauma center. J Clin Med Res 2013;5:
75-83. - Touger M, Gennis P, Nathanson N, et al. Validity of a decision rule to reduce cervical spine radiography in elderly patients with blunt trauma. Ann Emerg Med 2002;40:287-293.
- Kulvatunyou N. Clinical examination in complement with computed tomography scan: an effective method for identification of cervical spine injury. J Trauma 2010;68:1269.
- Hoffman JR, Wolfson AB, Todd K, Mower WR. Selective cervical spine radiography in blunt trauma: Methodology of the National Emergency X-Radiography Utilization Study (NEXUS). Ann Emerg Med 1998;32:461-469.
- Morrison J, Jeanmonod R. Imaging in the NEXUS-negative patient: When we break the rule. Am J Emerg Med 2014;32:67-70.
- Collins NC, McKenzie JV. The NEXUS criteria: Do they stand the test of time? Eur J Emerg Med 2013;20:58-60.
- Schrag SP, Toedter LJ, McQuay N, Jr. Cervical spine fractures in geriatric blunt trauma patients with low-energy mechanism: Are clinical predictors adequate? Am J Surg 2008;195:170-173.
- Schoenfeld AJ, Ochoa LM, Bader JO, Belmont PJ, Jr. Risk factors for immediate postoperative complications and mortality following spine surgery: A study of 3475 patients from the National Surgical Quality Improvement Program. J Bone Joint Surg Am 2011;93:1577-1582.
-
Vaccaro AR, Kepler CK, Kopjar B, et al. Functional and quality-of-life outcomes in geriatric patients with type-II dens fracture. J Bone Joint Surg Am 2013;95:
729-735. - Venkatesan M, Northover JR, Wild JB, et al. Survival analysis of elderly patients with a fracture of the odontoid peg. Bone Joint J 2014;96-B:88-93.
- Diamantopoulos AP, Rohde G, Johnsrud I, Skoie IM, Hochberg M, Haugeberg G. The epidemiology of low- and high-energy distal radius fracture in middle-aged and elderly men and women in Southern Norway. PLoS One 2012;7:e43367.
- Shortt NL, Robinson CM. Mortality after low-energy fractures in patients aged at least 45 years old. J Orthop Trauma 2005;19:396-400.
- Kannus P, Parkkari J, Niemi S, Palvanen M. Epidemiology of osteoporotic ankle fractures in elderly persons in Finland. Ann Intern Med 1996;125:975-978.
- Koval KJ, Lurie J, Zhou W, et al. Ankle fractures in the elderly: What you get depends on where you live and who you see. J Orthop Trauma 2005;19:635-639.
- Strauss EJ, Egol KA. The management of ankle fractures in the elderly. Injury 2007;38 Suppl 3:S2-S9.
- Zaghloul A, Haddad B, Barksfield R, Davis B. Early complications of surgery in operative treatment of ankle fractures in those over 60: A review of 186 cases. Injury 2014;45:780-783.
- Vioreanu M, Dudeney S, Hurson B, Kelly E, O’Rourke K, Quinlan W. Early mobilization in a removable cast compared with immobilization in a cast after operative treatment of ankle fractures: A prospective randomized study. Foot Ankle Int 2007;28:13-19.
- Schepers T, De Vries MR, Van Lieshout EM, Van der Elst M. The timing of ankle fracture surgery and the effect on infectious complications: A case series and systematic review of the literature. Int Orthop 2013;37:489-494.
- Little MT, Berkes MB, Lazaro LE, Sculco PK, Helfet DL, Lorich DG. Complications following treatment of supination external rotation ankle fractures through the posterolateral approach. Foot Ankle Int 2013;34:523-529.
- Shabat S, Mann G, Kish B, Stern A, Sagiv P, Nyska M. Functional results after patellar fractures in elderly patients. Arch Gerontol Geriatr 2003;37:93-98.
- Bridges MJ, Ruddick S. Are metatarsal fractures indicative of osteoporosis in postmenopausal women? Foot Ankle Spec 2011;4:271-273.
- Nguyen TV, Center JR, Sambrook PN, Eisman JA. Risk factors for proximal humerus, forearm, and wrist fractures in elderly men and women: The Dubbo Osteoporosis Epidemiology Study. Am J Epidemiol 2001;153:587-595.
- Chu SP, Kelsey JL, Keegan TH, et al. Risk factors for proximal humerus fracture. Am J Epidemiol 2004;160:360-367.
- Kim SH, Szabo RM, Marder RA. Epidemiology of humerus fractures in the United States: Nationwide emergency department sample, 2008. Arthritis Care Res (Hoboken) 2012;64:407-414.
- Bahrs C, Bauer M, Blumenstock G, et al. The complexity of proximal humeral fractures is age and gender specific. J Orthop Sci 2013;18:465-470.
- Handoll HH, Ollivere BJ, Rollins KE. Interventions for treating proximal humeral fractures in adults. Cochrane Database Syst Rev 2012;12:CD000434.
- Ockert B, Siebenburger G, Kettler M, Braunstein V, Mutschler W. Long-term functional outcomes (median 10 years) after locked plating for displaced fractures of the proximal humerus. J Shoulder Elbow Surg 2014.
- Zelken JA, Khalifian S, Mundinger GS, et al. Defining predictable patterns of craniomaxillofacial injury in the elderly: Analysis of 1,047 patients. J Oral Maxillofac Surg 2014;72:352-361.
- Goldschmidt MJ, Castiglione CL, Assael LA, Litt MD. Craniomaxillofacial trauma in the elderly. J Oral Maxillofac Surg 1995;53:1145-1149.
- Murphy K, Waa S, Jaffer H, Sauter A, Chan A. A literature review of findings in physical elder abuse. Can Assoc Radiol J 2013;64:10-14.
- Marciani RD. Critical systemic and psychosocial considerations in management of trauma in the elderly. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1999;87:272-280.
- Subhashraj K, Ravindran C. Maxillofacial intervention in trauma patients aged 60 years and older. Indian J Dent Res 2008;19:109-111.
-
Keller JM, Sciadini MF, Sinclair E, O’Toole RV. Geriatric trauma: Demographics, injuries, and mortality.
J Orthop Trauma 2012;26:e161-165. - Livingston DH, Shogan B, John P, Lavery RF. CT diagnosis of rib fractures and the prediction of acute respiratory failure. J Trauma 2008;64:905-911.
- Bulger EM, Arneson MA, Mock CN, Jurkovich GJ. Rib fractures in the elderly. J Trauma 2000;48:1040-1046; discussion 6-7.
- Battle CE, Hutchings H, Evans PA. Risk factors that predict mortality in patients with blunt chest wall trauma: A systematic review and meta-analysis. Injury 2012;43:8-17.
-
Sajjan SG, Barrett-Connor E, McHorney CA, Miller PD, Sen SS, Siris E. Rib fracture as a predictor of future fractures in young and older postmenopausal women: National Osteoporosis Risk Assessment (NORA). Osteoporos Int 2012;23:
821-828. - Marasco SF, Davies AR, Cooper J, et al. Prospective randomized controlled trial of operative rib fixation in traumatic flail chest. J Am Coll Surg 2013;216:924-932.
-
Dennison EM, Compston JE, Flahive J, et al. Effect of co-morbidities on fracture risk: Findings from the Global Longitudinal Study of Osteoporosis in Women (GLOW). Bone 2012;50:
1288-1293. - Fredo HL, Rizvi SA, Lied B, Ronning P, Helseth E. The epidemiology of traumatic cervical spine fractures: A prospective population study from Norway. Scand J Trauma Resusc Emerg Med 2012;20:85.
- Barrett-Connor E, Nielson CM, Orwoll E, Bauer DC, Cauley JA. Epidemiology of rib fractures in older men: Osteoporotic Fractures in Men (MrOS) prospective cohort study. BMJ 2010;340:c1069.
- Palvanen M, Kannus P, Niemi S, Parkkari J, Vuori I. Epidemiology of minimal trauma rib fractures in the elderly. Calcif Tissue Int 1998;62:274-277.
MONOGRAPH: As the population ages and continues to retain an increasingly high level of function, a unique pattern of injuries is emerging in older patients.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
