Spontaneous CSF Leaks and Connective Tissue Disorders: Is There a Connection?
Spontaneous CSF Leaks and Connective Tissue Disorders: Is There a Connection?
Abstract & Commentary
Source: Mokri B, et al. Neurology. 2002;58:814-816.
One of the editors recently examined a tall and slender young woman with a spontaneous CSF leak and a history of a spontaneous internal carotid artery dissection 6 years before. An underlying connective tissue disorder was suspected but not proven. Mokri and associates have reported a series of patients with spontaneous intracranial hypotension due to a spontaneous CSF leak in whom there was clinical evidence of an underlying connective tissue disorder.
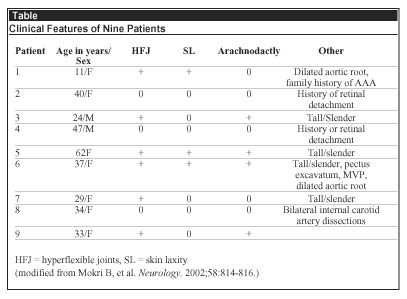
Of 58 consecutive patients seen at the Mayo Clinic with spontaneous CSF leaks, 9 exhibited clinical features of connective tissue disorder (see Table).
 |
Connective tissue disorders such as Marfan syndrome, neurofibromatosis, autosomal dominant polycystic kidney disease, and familial osteosclerosis are associated with abnormalities of the meninges. Meningeal diverticula and ectasia of the dural sac are frequent MRI findings in Marfan patients (Fattori R, et al. Lancet. 1999;354:910-913). In Marfan syndrome, mutations of the gene for fibrillin-1 lead to defects in collagen and elastin, especially in the walls of blood vessels. Spontaneous retinal detachment and spontaneous arterial dissections occur in Marfan syndrome, Ehlers-Danlos syndrome, and osteogenesis imperfecta. Brandt et al have demonstrated ultrastructural abnormalities of collagen and elastin in patients with carotid dissection (Brandt T, et al. Ann Neurol. 1998;44:281-285).
Mokri et al suggest that in some patients with spontaneous CSF leak, a disorder of connective tissue is present that leads to dural weakness and rupture.
Commentary
Like Mokri et al, this editor believes that the occurrence of both an internal carotid artery dissection and a spontaneous CSF leak in the same patient is more than just a coincidence. Unfortunately, at present, in patients who do not have the clinical phenotype of a fibrillinopathy, the association between spontaneous CSF leak and connective tissue disorder is hypothetical and will remain so until ultrastructural studies of skin biopsies and analysis of cultured dermal fibroblasts become routinely available to clinicians. —John J. Caronna
Dr. Caronna, Vice-Chairman, Department of Neurology, Cornell University Medical Center; Professor of Clinical Neurology, New York Hospital, is Associate Editor of Neurology Alert.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
