Polypharmacy in the Elderly: Clinical Challenges in Emergency Practice
Polypharmacy in the Elderly: Clinical Challenges in Emergency Practice
Part II: High-Risk Drugs, Diagnosis, and the Role of the Emergency Physician
Authors: Katherine M. Prybys, DO, ACTM, Assistant Professor of Emergency Medicine, University of Maryland Medical System, Baltimore; Kraig A. Melville, MD, FACEP, FAAEM, Chief, Emergency Medical Services, Calvert Memorial Hospital, Prince Frederick, MD; Jeahan R. Hanna, MD, Chief Resident, Emergency Medicine, University of Maryland Medical System, Baltimore.
Peer Reviewers: Andrew Gee, MD, Fellow, Division of Toxicology, Department of Emergency Medicine and Traumatology, Hartford Hospital, Hartford, CT; Peter A. Chyka, PharmD, Professor, Pharmacy Practice and Pharmacoeconomics; Executive Director, Southern Poison Center, University of Tennessee, Memphis.
Polypharmacy has become the exception rather than the rule among elderly patients accessing the emergency department. Typically, such co-morbid conditions as heart disease, diabetes, and hypertension co-exist, requiring patients to take multiple medications, many of them associated with a predictable incidence of adverse side effects.
Drug-related adverse patient events are an important cause of admission to the hospital and, as a result, emergency physicians must be skilled in detecting adverse drug reactions, drug interactions, and interactions between prescribed medications and over-the-counter drugs such as non-steroidal anti-inflammatory drugs (NSAIDs).
Part II of this two-part series on polypharmacy outlines a systematic approach to emergency evaluation of the older patient taking multiple medications. Drug-related side effects associated with antihypertensive agents, cardiovascular drugs, and NSAIDs are discussed in detail, and approaches to managing life-threatening events are presented.—The Editor
High-Risk Drugs
Many studies have found that only a limited number of drugs are responsible for the majority of adverse drug events (ADEs) and clinically relevant drug interactions.1,2 An even smaller number of medications is responsible for the most serious drug-related complications. These medications include anticoagulants, antihypertensives, carbamazepine, digoxin, narcotic analgesics, nonsteroidal anti-inflammatory drugs (NSAIDs), and theophylline.3,4 Many of these medications have narrow therapeutic-to-toxic ratios and require meticulous monitoring.5 These drugs should serve as "red flags" to clinicians when they are noted in patients’ medication lists. (See Table 1.)
 |
Warfarin. Drug interactions with warfarin can result in devastating consequences. Warfarin toxicity is responsible for many cases of serious drug-related morbidity and mortality, and is associated with a high incidence of hospitalizations and a high risk of fatal bleeding. Intracranial hemorrhage, the most feared complication of excessive anticoagulation, occurs in 2% of patients on long-term anticoagulant therapy.6 Warfarin’s effect is potentiated when a second drug inhibits its metabolism and causes drug accumulation. The effect on prothrombin time usually appears within 2-3 days, but does not peak until days 7-10.5 The anticoagulant effect also can be potentiated by the addition of drugs or herbs with synergistic effects. Although the list of drugs that interact with warfarin is extremely long, drugs that are particularly troublesome include antibiotics, acetaminophen, aspirin, and NSAIDs.7,8 (See Table 2.)
 |
All antibiotics can potentiate warfarin’s effect by inhibiting intestinal flora that produce vitamin K; however, antibiotics of particular concern include ciprofloxacin, clarithromycin, erythromycin, metronidazole, and trimethoprim-sulfamethoxazole. These drugs are P450 inhibitors that will decrease warfarin’s metabolism. They should be avoided whenever possible with warfarin use.9 If these drugs must be used, close monitoring of prothrombin time and International Normalized Ratio (INR) is essential.
Acetaminophen is a widely used over-the-counter medication whose potential to cause serious drug interaction with warfarin use generally is under-recognized by the public and clinicians. There is a highly significant dose-response relationship between acetaminophen and warfarin that is independent of other variables. This interaction is thought to result secondary to acetaminophen’s effect on the P450 system and its hypothrombinemic response. Study patients taking more than 1.3 g (four regular-strength 325 mg tablets) per day for longer than one week have a tenfold increased risk of having an INR greater than 6.0 when compared to controls.10
Aspirin is another widely used over-the-counter medication that increases the risk of bleeding when coadministered with warfarin. Aspirin causes this interaction by platelet function inhibition, gastric mucosal damage, and hypothrombinemic response.9 For patients in whom the benefits of combined warfarin-aspirin therapy outweigh the risk of bleeding, low-dose aspirin has been shown to be safer, yet effective.
NSAIDS also can potentiate the anticoagulant effects of warfarin by inhibiting platelet function, and potentially, displacing warfarin from its protein-bound state and inhibiting hepatic enzymes. Use of NSAIDs in the elderly is associated with a three- to fivefold increase in risk of peptic ulcer disease. Studies have shown that concurrent users of NSAIDs and oral anticoagulants had a nearly 13-fold increase in the risk of hemorrhagic peptic ulcer disease when compared with controls.11 The newer cyclooxgenase-2 inhibitor agents probably are safer options, as they have not been shown to inhibit platelets or increase the incidence of gastric ulceration.12,13
Angiotensin Converting Enzyme (ACE) Inhibitors. The use of ACE inhibitors in the elderly has become widespread, owing to the significant clinical benefits that these drugs impart. Unfortunately, these agents also can cause several important, life-threatening, adverse effects.14 ACE inhibitors have been shown to be responsible for the development of hyperkalemia in 9-38% of hospitalized patients. In addition, it has been shown that 10% of outpatients treated with ACE inhibitors develop hyperkalemia.15 ACE inhibitors cause hyperkalemia by reducing aldosterone secretion, which impairs the secretion of potassium. ACE inhibitor-induced hyperkalemia can become hazardous when potassium-sparing diuretics such as spironolactone, amiloride, and triamterene or potassium supplements are used concurrently.16 NSAIDs also can cause hyperkalemia by inhibiting renal prostaglandin synthesis, leading to decreased renin and aldosterone and impaired potassium excretion. Hyperkalemia has been seen most commonly with the use of indomethacin.9
Calcium Channel Blockers (CCBs). Used primarily for hypertension and tachyarrhythmia therapy, this class is virtually ubiquitous in the elderly population. Recently, indications have expanded, with CCBs used as therapy for angina, chronic pain, migraines, and esophageal spasm.17 Polypharmacy concerns arise with the coadministration of beta-blockers and/or digoxin. Occasionally used for patients with recalcitrant hypertension, or in hypertensive patients with dysrhythmia, this combination has potential complications, such as symptomatic bradycardia, heart block, and profound hypotension, that can be disastrous.
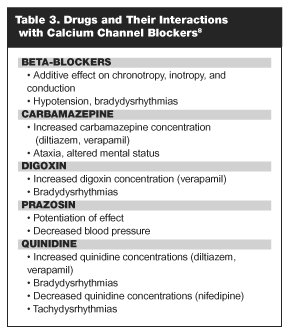
More insidious are the potential drug interactions due to the class metabolism by the cytochrome P450 system, isozyme CYP3A4.18 Both verapamil and diltiazem have been shown to inhibit hepatic metabolism of CYP clearance drugs.19 In turn, serum concentrations of CCBs can be affected by the same means. Decreased CYP3A4 activity by erythromycin or other pharmaceuticals can lead to increased CCB concentrations and resultant hypotension and bradycardia. Conversely, increased activity by an enzyme inducer, such as rifampin, can result in significantly decreased concentrations and subsequent marked hypertension or tachydysrhythmia.18 (See Table 3.)
 |
Digoxin. A large number of elderly patients receive digitalis therapy. The risk of an adverse event caused by digoxin increases with age due to the physiologic changes associated with aging that affect pharmacokinetics. In fact, patients older than age 85 have double the risk of experiencing an adverse drug effect from digoxin as patients age 65-74.20 Digoxin is a high-risk medication that must be monitored closely because it has a narrow margin between therapeutic and toxic doses. The kidneys excrete the majority of digoxin, thus, patients with renal insufficiency, congestive heart failure, and dehydration are at highest risk for ADEs. Clarithromycin, erythromycin, and tetracycline have been shown to increase digoxin level by altering the gut flora that is important in digoxin metabolism. The most important drugs causing interaction with digoxin, however, are the antiarrhythmics. Quinidine, for example, causes an increase in digoxin concentration in 90% of patients. This is caused by quinidine’s ability to reduce significantly digoxin clearance and displace digoxin from its binding sites. Amiodarone also increases digoxin level by reducing its renal clearance. Within 24 hours after adding amiodarone, digoxin concentrations were seen to increase by 25-70% .21 Verapamil, as well, increases serum digoxin concentrations as much as 70% by altering renal clearance.22
Serotonergic Drugs. Administration of two or more serotonergic enhancing drugs can produce a mild to life-threatening drug interaction known as serotonin syndrome. Seriously ill patients can progress rapidly to coma, seizures, and cardiac arrest. In a review of 100 cases of serotonin syndrome, 42% of patients required admission to an intensive care unit, and 25% required intubation and ventilatory support. An estimated 15-20 deaths have been attributed to serotonin syndrome. This syndrome is characterized by abnormalities in three areas: 1) central nervous system (CNS) abnormalities such as confusion, seizure, and coma; 2) autonomic nervous system dysfunction such as hyperthermia, diaphoresis, tachycardia, and hypertension; and 3) neuromuscular activity such as myoclonus, hyperreflexia, and muscle rigidity.23 A common clinical scenario involves a patient taking a selective serotonin reuptake inhibitor (SSRI) (i.e., fluoxetine, serataline, paroxetine, trazadone) or monoamine oxidase inhibitor (MAOI) (i.e., phenelzine, tranylcypromine), and a second serotonergic agent is added. Common inciting agents include St. John’s wort, meperidine, dextromethorphan, amphetamines, and cocaine.
NSAIDs. These drugs commonly are prescribed for the elderly, yet most likely account for the greatest incidence of ADEs in the United States. In fact, it is estimated that if deaths from gastrointestinal effects of NSAIDs were tabulated separately in the National Vital Statistics reports, they would constitute the 15th most common cause of death in the United States.12 The most common adverse effects of NSAIDs are gastrointestinal disease, such as dyspepsia, gastritis, and gastroduodenal ulcer. Proven risk factors for development of gastroduodenal ulcers include advanced age and concomitant use of corticosteroids, other NSAIDs, or anticoagulants. NSAIDs also can cause nephrotoxic effects that include renal failure and acute or chronic interstitial nephritis. These drugs interact with coumadin, digoxin, beta-blockers, ACE inhibitors, lithium, and thiazides.24
Diagnosis
The diagnosis of adverse drug effects should be considered for every elderly patient presenting to the emergency department (ED). These drug-related complications occur frequently in the elderly and are difficult to recognize. Symptoms often are vague, and clinical manifestations nonspecific. In addition, the clinical presentation of adverse drug reactions may mimic that of other common illnesses in the geriatric age group. Cognitive impairment such as confusion, hallucination, dementia, and depression are among the most common clinical presentations of drug-induced illness. Falls also are frequent presenting complaints.25,26 A common pitfall for the clinician is to attribute these nonspecific clinical manifestations erroneously to the patient’s aging state or underlying medical illness. The clinician unwittingly may prescribe a new drug to treat the manifestations of an adverse drug reaction, placing the patient at additional risk of experiencing adverse drug effects.27 It is essential that the clinician directly question the patient several times about medication history, since many patients initially forget to mention their use of over-the-counter drugs or herbal preparations. Specific questioning regarding medication use has been shown to be more sensitive in detection of their use.28
Some pathology caused by the adverse effect of polypharmacy is not subtle. Hypotension, bradycardia, coma, and bleeding diatheses are well-documented results of inappropriate drug combinations. Drug-related complications always should be considered in clinical presentations involving significant derangements of physiology, and can be checked easily by reviewing the patient’s current medication usage.
Legal Considerations
Current medical systems rely heavily on error-free performance, as evidenced by the lack of fail-safe mechanisms. Many medical institutions deal with medical errors by placing the emphasis on individual accountability and not on system failures.29 The typical response to medical error usually includes increased training efforts and punitive measures directed at the "imperfect" clinician. The public expects physicians to have knowledge of all the current pharmaceuticals on the market and, in particular, potential side effects and drug and food interactions. A survey conducted by the National Patient Safety Foundation found that many people believed that when mistakes did happen, they were the result of physician carelessness, stress, faulty training, or bad communication. Three out of four respondents believed the best solution to medical mistakes would be to get rid of the bad health care providers.30 Emergency clinicians increasingly are being held to an unachievable standard of care, with dire consequences resulting when inevitable human errors do occur.31,32
Studies have shown that a substantial number of patients each year suffer serious morbidity and mortality from medical errors.33 Although the overall rate of medical errors occurring in the emergency setting is unknown, it is no doubt quite high given the brisk and complex nature of this medical specialty. In one study, the ED was shown to have the highest number of adverse events from negligent care, ranging from 52-70%.34,35 A study performed in an intensive care unit revealed that there were an average of 178 activities per patient per day with an error rate of 1.7 per day.36 However, many medication errors are unavoidable and are not due to negligence. It is impossible for the clinician to know what the impact of age-related changes in physiology and disease on drug handling and drug response will be in every patient. Thus, it is difficult to predict which patients will experience significant drug side effects. Idiosyncratic reactions are unpredictable.
Physicians who commit mistakes that have resulted in serious injury or death not only must deal with emotional devastation, but also the fear of potential litigation, including criminal indictment.30,31,37 Frequently, drug injuries result in malpractice claims. When malpractice suits do arise, it is common for the defense to offer a settlement even when there is no negligence. One large study of closed claims revealed that drug injuries accounted for the highest total expenditure.38 The severity of the patient’s disability, not the occurrence of an adverse event, was more predictive of payment to the plaintiff.39 Fortunately, however, most medication errors do not cause injury, and many medical injuries caused by negligence do not result in a malpractice claim.
When a medical error does occur, the best policy is full and timely disclosure of the error to the patient and his or her family.40-42 Patients feel betrayed and angry when they believe health care providers are trying to cover up an error. Many lawsuits are motivated not by negligence, but by poor communication and a breakdown in trust between providers and patients. Institutions that have established guidelines for honest and full disclosure of medical errors and a provision for equitable compensation for loss have found both a cost-effective and ethical solution to the problem.43,44
The Role of the ED and the Emergency Physician
Self-education. Emergency medicine physicians have a large number of yearly patient encounters yielding drug treatment.45 Physicians’ prescribing practices contribute significantly to ADEs.46-48 Common medication errors that occur due to physician prescribing errors include incorrect drug product, dosage form, dosage amount, administration route, and dosing frequency. Illegible handwriting, the use of abbreviations, decimal point misplacements, or miscalculation of dose can have tragic consequences.49-51 The majority of prescribing errors are due to lack of knowledge about pharmaceuticals and geriatric prescribing principles. In one study, 22% of errors were caused by lack of knowledge of the drug prescribed—the most common cause of error.47 One group reviewed similar concepts in their study of medication errors and found that almost 60% of prescribing errors were due to deficits in knowledge and application of knowledge regarding drug therapy and patient characteristics.46 The patient factors most commonly not accounted for in selecting a drug or drug dose were advanced age, renal impairment, and patient weight. They also found that inappropriate concurrent drug therapies involving drug-drug interactions and duplicative therapies were frequent.
More sophisticated systems can check for drug-drug and drug-allergy interactions. Clinicians must make it their responsibility to educate themselves continually regarding medication errors and polypharmacy issues in the elderly. Since it is impossible for a clinician to have in-depth knowledge about every pharmaceutical product available on the market, the use of easily accessible, up-to-date databases has become imperative. Software that allows for drug-drug interaction recognition is available to all practitioners. For example, medical screening software, such as PDA-based mobilePDR is updated regularly and can screen out dangerous drug combinations to help prevent potentially serious interactions. Other sources of pharmaceutical information are listed in Table 4.
 |
Medication Screens. The ED is the hospital’s primary contact with the community. Conversely, for many individuals in the community, the ED serves as their primary source of medical care. Historically, more than 40% of patients treated in the ED lack a usual source of health care.13 The number of ED visits nationally in 1999 was 102.8 million. This allows for a vast screening of the general population for polypharmacy issues. Conscientious attempts must be made to obtain a complete medicine history, including herbal and over-the-counter preparations, from the patient and attendant family. This information can be obtained by reviewing all of the patient’s medication bottles or medication lists. For patients who are unable to provide information or cannot remember their medications, an old medical chart can be extremely useful. Several hospital information systems are designed to maintain and display a current medication list. The patient’s current drug regimen must be assessed fully before a new drug is prescribed to prevent potential drug interactions.
The ED may set up a system that reviews patients’ medication lists to recognize any pharmaceutical problems. An example would be a protocol requiring that all patients who present to the ED and who have multiple medications automatically have their drug lists reviewed by a pharmacist or computerized query system. If a problem with high-risk drug combinations or dosage was identified, the patient, ED clinician, and the primary care physician would be notified. This concept needs to be investigated further to establish its clinical utility and efficacy.
Clinical Guidelines/Pathways. Treatment guidelines are becoming increasingly popular in clinical medicine. They are designed to serve as safeguards and to standardize and improve medical therapy for some of the most common and highest-morbidity pathologies.52 Guidelines should include strict medication regimens and internalized restrictions to minimize potential adverse polypharmacy effects. Examples are the use of weight-based heparin in thrombolytic pathways to reduce the possibility of hemorrhage, and sildenafil citrate advisories regarding nitroglycerin use to avoid inducing serious hypotension. Nearly 700 evidence-based treatment guidelines are available easily to clinicians from the National Guideline Clearinghouse. The web site is www.guideline.gov.
Communicate with Staff. Nurses often experience a more extensive and relaxed communication with patients and their families than ED physicians do. Nurses spend much more time with patients than physicians do, and they usually are the first and last point of medical contact for patients. Nurses may encounter information that the ED physician is not privy to, as patients may become annoyed and uncooperative if they must give their histories more than once and therefore may leave out pertinent details when questioned repeatedly. Therefore, nurses can provide valuable clinical information to the treating clinician. In addition, since nurses administer medications and give the patient discharge instructions, they can serve as a screen for prescribing mistakes. In one study, nurses were the principal interceptors of medication errors, detecting half of physician ordering errors.47 This result occurred within a hospital-wide system that included pharmacists; in the ED, nurses are the emergency physician’s only check and balance.
Utilize Supportive Services for the Patient. Employ social service consultation to arrange patient and family education regarding medication usage. Social services also can aid in ensuring completion of prescriptions, communication with primary care providers, referral to consultants, lab follow-up to obtain serum testing, and transportation to appointments.
Simplify Treatment Regimens. One group showed that patients with multiple daily doses of a medication have a 75% rate of noncompliance.53 Because more mature patients have even greater difficulty with multiple daily dosing, try to utilize once- or twice-daily schedules. If possible, discuss the opportunity to simplify already existing treatment regimens with the primary care physician or consultant.
Conservative Initial Drug Dosing. The use of lower initial drug doses may help avoid serious adverse reactions in older patients. In addition, lower drug dosages may reduce drug side effects and interactions while improving patient compliance. Elderly individuals have a reduced rate of drug clearance due to decreased renal and hepatic function in comparison to younger adults. Despite these pharmacokinetic differences, most drug inserts do not recommend reduced initial doses for elderly patients. Many times, lower doses are appropriate because a large number of studies have been conducted that support the therapeutic effectiveness of lower drug doses. For example, multiple studies show the effectiveness of ibuprofen at 200 mg doses three to four times per day.54 Furthermore, for many drugs, pharmacokinetic data for the elderly are not available. Patients who describe long histories of numerous drug intolerances are likely to be slow metabolizers and require low-dose medication. For all other elderly patients, the adage "start low and go slow" should be heeded.
Safer Alternative Drug Therapy. The potential benefits of any medication must be weighed against the risks of adverse drug effects. Many times, safer alternative drug options can be utilized for elderly patients. For example, an elderly patient who requests medication to aid sleep may be served better by the use of an antihistamine, such as diphenhydramine or low-dose trazodone, instead of a benzodiazepine. Antihypertensive agents provide another example. Thiazide diuretics are quite effective in lowering blood pressure, but they cause several adverse effects that limit their use. In addition to causing potassium and sodium loss, they may cause extremity swelling, which can resemble gout-like symptoms. In a study of more than 9000 Medicaid patients who were age 65 or older, the risk of being started on treatment for gout was almost double in patients who received thiazide diuretics when compared to patients who were treated with non-thiazide therapies. In addition, the risk of being treated for gout was much less when a lower dose of thiazide was prescribed, and the lower dose was found to be effective in lowering blood pressure.55 NSAIDs also are responsible for a huge number of adverse drug effects in the general population. Safer treatment alternatives include acetaminophen or cyclooxygenase-2 inhibitors.12,13 Finally, cimetidine is responsible for a large number of clinically significant drug interactions. Cimetidine, a potent inhibitor of the P450 system, causes increases in serum concentrations of many concurrently administered drugs.24,56 Ranitidine, famotidine, and nizatidine are safer alternative H2-blocker drugs.
Discharge Instructions/Prescriptions. Patients always should be counseled regarding potential drug side effects and interactions. Elderly patients who take multiple medications, or who appear particularly frail or incompetent, should be encouraged to have a family member or close friend listen to discharge instructions with them. Patients also should be encouraged to seek medical advice for any concerns in identifying drug side effects.
A significant trend in ED management has been the introduction of computerized discharge instructions and prescriptions. Prescription programs provide a dose selection menu, which includes drug route and dosing frequency and generates a legible copy. Several current platforms automatically compare discharge prescriptions for compatibility to provide the clinician with the potential for intervention. For instance, a patient who is maintained on warfarin therapy is diagnosed with diverticulitis and is prescribed metronidazole. Metronidazole, an inhibitor of the cytochrome P450 system, would increase warfarin levels, leading to significant bleeding complications. Inputting the new prescription with the baseline medication list would result in an alert of the drug interaction to the practitioner.57 The net effect of the application of this software should parallel one group’s findings of inpatient physician order entry where there was an overall 55% reduction in "serious medication errors."58
In addition, a copy of discharge instructions, including prescriptions, should be forwarded to the primary care provider and/or consultant. This would provide them with an updated pharmaceutical list to avoid any unintended error on their part.
Adverse Drug Event Reporting. All ADEs suspected in the ED should be reported. This allows intervention, education, policy revision, and tracking of epidemiology on a national scale. Although fear of litigation deters many clinicians, full disclosure of errors is the best policy and is simply the right thing to do.59,60
In this age of increased public awareness and sensitivity to the issue of medical errors, EDs should have a protocol for responding to serious errors, particularly those resulting in significant patient injury or death.61,62 This plan should address how the staff should interact with patients, families, federal regulatory bodies, accreditation agencies, and the media. Procedures for safeguarding event documentation, containers, and equipment should be included. Arrangements for psychological counseling and other forms of support for staff, patients, and their families should be addressed. (See Tables 4, 5, and 6.)
 |
 |
—Special thanks to Vincent Jackson, PharmD, for advisory assistance on certain parts of this paper.
References
1. Classen DC, Pestotnik SL, Evans S, et al. Computerized surveillance of adverse drug events in hospital patients. JAMA 1991;266: 2847-2851.
2. Goldberg RM, Mabee J, Chan L, et al. Drug-drug and drug-disease interactions in the ED: Analysis of a high-risk population. Am J Emerg Med 1996;14:447-450.
3. Beers MH, Storrie M, Lee G. Potential adverse drug interactions in the emergency room. Arch Intern Med 1990;112:61-64.
4. Herr RD, Caravati EM, Tyler LS, et al. Prospective evaluation of adverse drug interactions in the emergency department. Ann Emerg Med 1992;21:1331-1336.
5. Paauw DS. Commonly overlooked drug interactions. Emerg Med 2001;March:93-97.
6. Freeman MD, Olatidoye AG. Clinically significant drug interactions with oral anticoagulants. Drug Safety 1994;10:381-394.
7. Self TH. Warfarin interactions: How various drugs and disorders alter anticoagulant effects. J Crit Illness 1998;13:356-358.
8. Physicians’ Desk Reference 2002, 56th ed. Medical Economics Company, Montvale NJ:1243-1248.
9. Ament PW, Bertolino JG, Liszewski JL. Clinically significant drug interactions. Am Fam Physician 2000;61:1745-1754.
10. Hylek EM, Heiman H, Skates SJ, et al. Acetaminophen and other risk factors for excessive warfarin anticogaulation. JAMA 1998; 279:657-662.
11. Shorr RI, Ray WA, Daugherty JR, et al. Concurrent use of NSAIDs and oral anticoagulants places elderly persons at high risk for hemorrhagic peptic ulcer disease. Arch Intern Med 1993;153: 1665-1670.
12. Wolfe MM, Lichtenstein DR, Singh G. Gastrointestinal toxicity of nonsteroidal anti-inflammatory drugs. N Eng J Med 1999;340: 1888-1899.
13. FitzGerald GA, Patrono C. The coxibs, selective inhibitors of cyclooxgenase-2. N Engl J Med 2001;345:433-441.
14. Alderman C. Adverse effects of angiotensin converting enzyme inhibitors. Ann Pharmaco Therapy 1996;30:55.
15. Perazella MA. Drug-induced hyperkalemia: Old culprits and new offenders. Am J Med 2000;109:307-314.
16. Rimmer JM, Horn JF, Gennari FJ. Hyperkalemia as a complication of drug therapy. Arch Intern Med 1987;147:867-869.
17. Kerns W, Kline J, Ford M. Beta-blocker and calcium channel toxicity. Emerg Med Clin North Am 1994;12:365-390.
18. Self TH. Calcium channel blocker- drug interactions: Underrecognized effects with commonly used agents. J Crit Illness 1998;13: 580-581.
19. Hunt BA, Self TH, Lalonde RL, et al. Calcium channel blockers as inhibitors of drug metabolism. Chest 1989;96:393-399.
20. Warren Jl, McBean Am, Hass, SL, et al. Hospitalization with adverse events caused by digitalis therapy among elderly Medicare benficiaries. Arch Intern Med 1994;154:1482-1487.
21. Marcus FI. Pharmacokinetic interactions between digoxin and other drugs. J Am Coll Cardiol 1985;5:22A.
22. Goodman LS. Digitalis. In: Haddad, et al., (eds.) Clinical management of poisoning and drug overdose. 3rd ed. Philadelphia: W.B. Saunders Company 1998:1001-1020.
23. Mills KC. Serotonin Syndrome: A clinical update. Crit Care Clin 1997;13:763-783.
24. Albrich M, Bosker G. Drug Therapy, Drug Prescribing and Systematic Detection of Adverse Drug Reactions. In: Bosker G, et al, (eds.) Geriatric Emergency Medicine. St Louis: Mosby-Yearbook Inc; 1990:33-61.
25. Gurwitz JH, Field TS, Avorn J, et al. The incidence and preventability of adverse events in nursing homes. Am J Med 2000;109:87-94.
26. Brennan TA, Leape LL, Laird NM, et al. Incidence of adverse events and negligence in hospitalized patients. Results of the Harvard Medical Practice Study I. N Engl J Med 1991;324:370-376.
27. Rochon PA, Gurwitz JH. Optimising drug treatment for the elderly people: The prescribing cascade. BMJ 1997;315:1096-1099.
28. Metz JM, Jones H, Devine P, et al. Cancer patients use unconventional medical therapies far more frequently than standard history and physical examination suggest. Cancer J 2001;7(2):145-154.
29. Institute for Safe Medication Practices. Medication Safety Alert. ISMP survey shows weaknesses persist in hospitals’ error detection, reporting and analysis. Nov. 15, 2000 issue. www.ismp.org/MSAarticles/ReportingSurvey.html. Accessed 5/8/2002.
30. Public Opinion of patient safety issues: Research findings. Prepared for: National Safety Foundation at the AMA. Lou Harris & Associates. September 1997.
31. Asch DA, Parker RM. The Libby Zion case: One step forward or two steps backward? N Engl J Med 1988;318:771-775.
32. Institute for Safe Medication Practices. Medication Safety Alert. Lesson from Denver: Look beyond blaming individuals for error. Feb. 11,1998;3 (3). www.ismp.org/MSAarticles/Denver.html. Accessed 5/5/2002.
33. Kohn LT, Corrigan J, Donaldson MS, et al. (eds). To Err is Human: Building a Safer Health System. Washington, D.C.: National Academy Press; 2000.
34. Leape LL, Brennan TA, Laird N, et al. The nature of adverse events in hospitalized patients. Results of the Harvard Medical Practice Study II. N Engl J Med 1991;324:377-384.
35. Thomas EJ, Studdert DM, Burstin HR, et al. Incidence and types of adverse events and negligent care in Utah and Colorado. Med Care 2000;38:261-271.
36. Leape L. Error in medicine. JAMA 1994;272:1851-1857.
37. Schaikewitz PS. To reduce errors, focus on procedures, not casting blame. ED Legal Letter 1999:1-13.
38. Bates DW, Spell N, Cullen DJ, et al. The costs of adverse drug events in hospitalized patients. JAMA 1997;277:307-311.
39. Brennan TA, Sox CM, Burstin HR. Relationship between negligent adverse events and the outcomes of medical-malpractice litigation. N Engl J Med 1996;335:1963-1967.
40. Institute for Safe Medication Practices Medication Safety Alert. Case update: Epinephrine death in Florida. Dec. 4,1996;1(24) issue. www.ismp.org/MSAarticles/epinephrine.html. Accessed 5/8/2002.
41. Institute for Safe Medication Practices. Medication Safety Alert. Full and timely disclosure of errors to patients: Honesty is the best policy. Feb. 23, 2000;5 (4). www.ismp.org/MSAarticles/Disclosure.html. Accessed 5/8/2002.
42. Green JA. Minimizing malpractice risks by role clarification. The confusing transition from tort to contract. Ann Intern Med 1998; 109:234-241.
43. Wu AW. Handling hospital errors: Is disclosure the best defense? Ann Intern Med 1999;131:970-972.
44. Kraman SS, Hamm G. Risk management: Extreme honesty may be the best policy. Ann Intern Med 1999;131:963-967.
45. Burt CW, McCraig LF. Trends in hospital emergency department utilization: United States, 1992-1999. National Center for Health Statistics. Vital Health Stat 2001;13(150).
46. Lesar TS, Briceland L, Stein DS. Factors related to errors in medication prescribing. JAMA 1997;277:312-317.
47. Leape LL, Bates DW, Cullen DJ, et al. Systems analysis of adverse drug events. JAMA 1995;274:35-43.
48. Borzo G. Prescribing errors put doctors under scrutiny. Fam Pract News 2001;Feb:33.
49. Belkin,L. How can we save the next victim? The New York Times Magazine June 15, 1997; section 6: page 28, col. 1.
50. Bedell SE, Deitz DC, Leeman D, et al. Incidence and characteristics of preventable iatrogenic cardiac arrest. JAMA 1991;265: 2815-2820.
51. Institute for Safe Medication Practices. Medication Safety Alert. Handwriting on the wall? July 16,1997 issue. www.ismp.org/MSAarticles/Handwriting.html. Accessed 5/8/2002.
52. Grissinger M. Medication errors: Action is needed to avert fatal errors from concomitant use of heparin products. Pharm & Therap 2001;26:462.
53. Murphy C, et al. Issues in patient compliance. Drugs 1997; 54: 797-800.
54. Cohen JS. Avoiding adverse reactions: Effective lower-dose drug therapies for older patients. Geriatrics 2000;55:54-64.
55. Novielli K, Koenig JB, White E, et al. Individualized prescribing for the elderly. Pharm &Therap; Supplement:1-35.
56. Chutka DS, Evans JM, Fleming KC, et al. Drug prescribing for the elderly patient. Mayo Clin Proc 1995;70:685-693.
57. Finch CK, Self TH. 10 Common prescribing errors: How to avoid them. Consultant 2000;May:766-771.
58. Bates DW, Leape LL, Cullen DJ, et al. Effect of computerized physician order entry and a team intervention on prevention of serious medication errors. JAMA 1998;280:1311-1316.
59. Goldman SA, Kennedy DL, Graham DJ, et al. The clinical impact of adverse event reporting. A Medwatch continuing education article. October, 1996:1-11.
60. Wu AW, Folkman S, McPhee SJ, et al. Do house officers learn from their mistakes? JAMA 1991;265:2089-2094.
61. Cohen MR. Responding to serious medication error. Hosp Pharm 1991;26:1024-1025.
62. Institute for Safe Medication Practices Medication. Medication Safety Alert. Preparing for a damaging medication error. Sept. 24, 1997 issue. www.ismp.org/MSAarticles/Preparation.html. Accessed 5/8/2002.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
