Not Every Stroke Patient Needs a TEE
Not Every Stroke Patient Needs a TEE
Abstract & Commentary
By John J. Caronna, MD, Vice-Chairman, Department of Neurology, Cornell University Medical Center, Professor of Clinical Neurology, NewYork-Presbyterian Hospital. Dr. Caronna reports no consultant, stockholder, speaker's bureau, research, or other relationship related to this field of study.
Synopsis: In patients with an ischemic stroke, a normal carotid DUS examination does not support the routine use of TEE to exclude the presence of complex aortic arch plaque or thrombi.
Source: Harloff A, et al. Do Stroke Patients with Normal Carotid Arteries Require TEE for Exclusion of Relevant Aortic Plaques? J Neurol Neurosurg Psychiatry. 2005;76:1654-1658.
Harloff and colleagues wondered whether patients with clinically significant atherosclerosis of the aortic arch also had atherosclerotic disease of the cervical carotid arteries of comparable severity. If so, the easier to evaluate carotid artery atherosclerosis could serve as an indicator for aortic plaques. Therefore, their aims were:
1. To determine the precise association of carotid and aortic arch atherosclerosis in patients with acute cerebral ischemia; and
2. To test the reliability of carotid duplex ultrasonography (DUS) as a replacement for transesophageal echocardiography (TEE) to exclude or predict the presence of clinically relevant aortic arch atheromas.
In 301 consecutive acute ischemic stroke patients admitted to a stroke unit in Germany, Harloff et al used 2-dimensional DUS of the common carotid and internal carotid (ICA) arteries to determine intima and media thickness (IMT), maximal plaque area, and degree of ICA stenosis; they used TEE to measure aortic wall thickness (AWT).
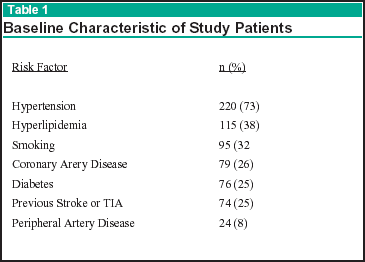
The age of the study patients was 62 ± 11 years (mean + SD). There were 166 women (39%). The prevalence of cardiovascular risk factors is shown in the table below.
 |
Both IMT and AWT increased significantly with the number of cardiovascular risk factors, and were higher in patients with ICA stenosis > 50%. Aortic arch plaques > 4 mm occurred in 62/301 (22%) study subjects, and were almost 3 times more frequent (44 % vs 15%) with ICA stenosis > 50% compared with ICA stenosis < 50%.
Mobile aortic thrombi were detected in 17 patients; AWT was > 50% in 15/17 and < 4 mm in only 2 of these patients. In patients with ICA stenosis > 50%, the incidence of aortic thrombi was almost 3 times higher (11% vs 4%) than in those with ICA stenosis < 50%.
An IMT < 0.9 mm found in 95/301 (32%) patients almost excluded AWT > 4.0 mm (negative predictive value = 96%, 4/95 false negatives). The combination of IMT < 0.9 mm. and no carotid plaques (49/301; 16%) increased negative predictive value to 100%. None of the 95 patients had aortic thrombi on TEE, but 2 of them had left atrial thrombi.
The positive predictive value of IMT > 0.9 was low (30%) and increased only to 33% in the presence of carotid plaques.
Commentary
This study provides information useful to all physicians who treat stroke: In patients with an ischemic stroke, a normal carotid DUS examination does not support the routine use of TEE to exclude the presence of complex aortic arch plaque or thrombi. In contrast, in stroke patients with significant carotid artery atherosclerosis, TEE should be performed to exclude aortic arch disease as a source for cerebral embolism.
In patients with an ischemic stroke, a normal carotid DUS examination does not support the routine use of TEE to exclude the presence of complex aortic arch plaque or thrombi.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
