Pediatric Anaphylaxis: Critical Aspects of ED Management
Pediatric Anaphylaxis: Critical Aspects of ED Management
Authors: Lara Zibners, MD, Attending Physician, Pediatric Emergency Department, The Mount Sinai Hospital, New York; Dimitri Laddis, MD, Fellow, Pediatric Emergency Medicine, The Mount Sinai School of Medicine, New York; Karin Berger Sadow, MD, Director, Division of Pediatric Emergency Medicine, Department of Emergency Medicine, The Mount Sinai School of Medicine, New York
Peer Reviewer: Paul Ishimine, MD, FACEP, FAAP, Director of Pediatric Emergency Medicine, Department of Emergency Medicine, University of California San Diego Medical Center; Attending Physician, Division of Pediatric Emergency Medicine, Children's Hospital and Health Center, San Diego; Assistant Clinical Professor of Medicine and Pediatrics, University of California, San Diego School of Medicine
Anaphylaxis is a true life-threatening emergency that may occur following a variety of exposures. Foods, such as peanuts and tree nuts, antibiotics, and more recently, latex have all been implicated as potential triggers of a severe analpylactic reaction. Certain factors, such as a delay in the administration of epinephrine or an oral route of exposure, have been associated with a higher risk of a biphasic reaction. Early recognition and aggressive management are critical for achieving a good outcome. Appropriate periods of observation and disposition are also important for the child who has had an anaphylactic reaction.
The authors review the presentation and management strategies for a child with anaphylaxis. — The Editor
Introduction
Some accounts in the literature tell us that Menes, the first Egyptian pharaoh, died as a result of an unfortunate encounter with a wasp. While other historians credit a hippopotamus with killing the pharaoh, this story remains perhaps the earliest recorded account of a death due to anaphylaxis.1 Modern historians credit Paul Portier and Charles Richet, French scientists in 1902, with identifying this life-threatening reaction in their description of hypersensitivity reactions in dogs previously immunized with sea anemone venom. An experiment designed to grant sting protection to the animals took an unexpected turn when the dogs experienced fatal reactions to otherwise nonfatal doses of venom. The scientists coined the term anaphylaxis, from the Greek words ana (against) and phylaxis (protection), and Richet later would win the Nobel Prize for this work in 1913.1-4
Anaphylaxis is a life-threatening event that may result from exposure to any number of offending agents and present with a wide array of symptoms. It is estimated that anywhere from 1.2% to 15% of the U.S. population may experience an episode of anaphylaxis.5 The ability to quickly recognize this condition in a patient presenting to the emergency department (ED)—with often times a vague history and a variety of physical findings—can be challenging. In this article, we will review the spectrum of findings associated with anaphylaxis, provide an organized, systematic approach to its management, and discuss the important issues regarding the disposition of such a patient from the ED.
Definitions
Anaphylaxis is best defined as an acute event resulting from an immediate hypersensitivity reaction involving more than one organ system.6 Anaphylaxis is a Type I hypersensitivity immune response, resulting from re-exposure of a previously sensitized individual to a substance. Antigen re-exposure initiates an IgE-mediated response with the sudden release of mast and basophil cell-derived mediators triggering a physiologic cascade.7 The exposure can be via any route including inhalation, intravenous (IV), transdermal, or oral (PO). The most common known causes are food, medications, exercise, and insect venom. Unfortunately, however, many cases may have no identifiable cause.8
While anaphylaxis has been referred to as "the maximal variant of an acute allergic reaction,"6 it is important to note that the presence of life-threatening symptoms does not define an allergic reaction as anaphylaxis. Rather, it is the involvement of more than one organ system that differentiates this condition from other allergic conditions. The American Academy of Allergy, Asthma & Immunology describes anaphylaxis as "a collection of symptoms affecting multiple systems in the body the most dangerous symptoms include breathing difficulties and a drop in blood pressure or shock, which are potentially fatal."9
Anaphylactoid reactions are not immune mediated and may occur upon primary exposure to a substance. These may mimic anaphylaxis (and even be life threatening).10,11 For example, a patient receiving IV radiocontrast media for the first time may experience a life-threatening reaction.12 These reactions are not IgE-mediated, and the effects are instead a result of the direct release of chemical mediators by the offending agent. The signs of an anaphylactoid reaction are indistinguishable from those of anaphylaxis, and the treatment remains the same. Therefore, for the purposes of this article, both reactions will be referred to simply as anaphylaxis.13
Anaphylaxis also can be described as uniphasic, biphasic, or protracted.14 A reaction can be termed uniphasic when the symptoms resolve within 1-2 hours of initiation of appropriate treatment and do not reappear. A biphasic reaction involves an initial (also termed early or acute) phase, followed by a symptom-free interval (lasting hours, sometimes more than a day) indistinguishable from a uniphasic reaction. There is, then, a late phase or recurrence, which may be even more severe than the initial reaction.15,16 The reported rates of biphasic reactions vary widely in the literature, and it is difficult to predict which patients will experience such a biphasic reaction. However, the oral route of exposure has been associated with an increased risk of biphasic reactions.17,18 A small number of patients may have a protracted course: They remain severely symptomatic despite vigorous therapy during a period of days. Some investigators have identified parenteral exposures as being more likely to require intensive care hospitalization.19
Pathophysiology
The acute and late manifestations of anaphylaxis are the result of substances, most notably histamine, released during the degranulation of mast cells and basophils. Histamine has a potent effect on vascular tissue resulting in hypotension and tissue edema typical of an anaphylactic reaction.7,20 Additional immune components and other substances including complement, fibrinogen, and clotting factors also may be involved.21 The list of mediators and substances released during degranulation is extensive and beyond the scope of this article. However, their activity, through direct receptor or inflammatory pathway activation, contributes to the acute and late phases of anaphylaxis, as well as the severity and duration of the reaction.
The Causes of Anaphylaxis
Food Anaphylaxis. Food allergy is the most common cause of anaphylaxis in children, and it has been estimated that food-induced anaphylaxis results in approximately 125-200 fatalities (of all ages) every year in the United States.22-24 Peanuts, tree nuts (e.g., walnuts, almonds, coconut), milk, and eggs are the most common foods implicated in children.25,26 It is estimated that 80% to 90% of food-related anaphylactic events in children were caused by peanuts and tree nuts.27,28 Children with peanut allergy often are sensitized early in life, and this persistent hypersensitivity is likely to last throughout their lifetime.24,29,30 In addition, there is some cross-reactivity (e.g. peanuts and soy) between related food groups that may cause symptoms.27,31 The time from ingestion to symptom onset may vary but is typically within minutes. Food allergies in children are particularly hazardous because it is extremely difficult to prevent inadvertent exposure. Some pre-schools, camps, and daycare centers provide a "nut free" environment, but even with a known allergy and vigilant caregivers, an accidental exposure is unforeseeable. Food allergy may even precede the introduction of the offending food into a child's diet. In these cases, allergy is thought to result from sensitization in uteri or by breast-feeding.32
Iatrogenic/Drug Anaphylaxis. Other, often very severe, causes of anaphylactic reactions are iatrogenic, with antibiotics and nonsteroidal anti-inflammatory drugs (NSAIDs) being the most common.8 The administration of any medication bears potential risk for an allergic reaction. For medications with a known higher risk of allergic reactions, or for patients with a history of allergic response, a discussion of the risks and benefits is prudent. One particular area of difficulty for the physician is the selection of an appropriate antibiotic when given a history of an "allergy." Quite often allergy symptoms, such as diarrhea or abdominal discomfort, described by the caregiver are nothing more than common side effects of that medication. More challenging, perhaps, is the patient who develops a rash while taking an antibiotic. Is the rash a true drug allergy or perhaps only a viral exanthem? Eliciting a history of urticaria (hives), pruritus, and subsequent similar reactions may indeed warrant the avoidance of certain drugs.
Although penicillins are the most common cause of reported drug allergy, it is a small number of patients reporting a "penicillin allergy" who truly have positive allergy testing.33 Also, the incidence of cross-reactivity with other antibiotics, including cephalosporins, is relatively low. The practice of not administering cephalosporins to patients with a self-reported history of penicillin allergy is largely unsubstantiated and outdated. Early cephalosporins were contaminated with trace amounts of penicillin, which may account for some early reports of cephalosporin-related anaphylaxis in patients with a history of penicillin allergy. Subsequent studies have demonstrated that the risk of anaphylaxis in response to a cephalosporin in a patient with a history of a penicillin allergy is similar to the risk of reacting to any, even unrelated, antibiotic.34
NSAIDs and aspirin also are commonly implicated in anaphylactic reactions, but these reactions appear to be medication specific with little risk of cross-reactivity.33 Older NSAIDs that block cyclooxygenase-1 (COX-1) are more likely to cross-react, especially at higher doses. Newer, selective COX-2 inhibitors do not cross-react, although patients may become sensitized to these specifically.35,36 Whether many drugs—NSAIDs in particular—represent anaphylactic or rather anaphylactoid reactions is a moot point for the purposes of this article, but one that may be important when considering cross-reactivity.
Latex-induced Anaphylaxis. This form of anaphylaxis is of particular significance in the hospital setting. Individuals at higher risk for this type of hypersensitivity include health care workers, those with occupational latex exposure, children with neural tube defects, and children with genitourinary abnormalities.37,38 While latex-free gloves are largely ubiquitous, inadvertent exposure, such as through the latex port of an intravenous line, still may occur. For these individuals, extreme care must be taken to eliminate their exposure to latex allergens. Of note, in one study where latex accounted for 25% of anaphylaxis in children, it also accounted for 45% of intensive care cases.19
Radiopaque contrast media is yet another cause of iatrogenic anaphylactic (or anaphylactoid) reactions in children. Although the incidence of any reaction is lower (1-3%) now, with the use of nonionic agents, there is still a real risk of severe reaction (0.03%), and even death (1-3 per 100,000) to any patient requiring contrast for imaging.12,39 In patients who are known to have had a prior reaction to contrast media, a pretreatment regimen of antihistamines and corticosteroids has been shown to be effective in preventing subsequent reactions. The prophylactic use of ephedrine as an oral "epinephrine analog" has been described but remains controversial.40,41
Insect Venom Anaphylaxis. Insect venom is another commonly implicated causative agent in anaphylactic reactions, responsible for 40 to 50 deaths in the United States annually.19,42 These patients may have an advantage in receiving prompt medical attention, given the relatively high awareness in the population about insect sting allergy, and also the painful and alarming nature of the exposure (sting) itself. Hymenoptera (bees, wasps and fire ants) are the most common culprits, and there is cross-reactivity between the venoms of each insect. Stings are more common in men than women.43 It has been suggested that a patient's most severe prior reaction may be used as a predictor of the severity of a future sting reaction.44 Others suggest that sensitivity invariably declines with age and repeated stings.45 Regardless, venom immune therapy (VIT), commonly known as "allergy shots", has been shown to improve patients' quality of life and chances of surviving a sting. However, epinephrine and rapid treatment remain the mainstays of managing even these "treated" patients.46
Exercise-induced Anaphylaxis. Exercise-induced anaphylaxis is a less obvious cause of anaphylaxis, although surprisingly common, accounting for 6% to 9% of cases.38,47 Following vigorous physical activity, certain individuals may exhibit signs and symptoms of anaphylaxis comparable in severity and duration to any other cause of anaphylaxis.48 It is not uncommon for these patients to have vascular collapse or upper respiratory tract obstruction. The diagnosis is confirmed when symptoms of exercise-induced anaphylaxis are reproduced in a testing facility.33,49
Such exercise-induced reactions are commonly food related (termed food-associated exercise-induced anaphylaxis): the reaction only occurs with an ingestion of a food (often one of the foods implicated in food hypersensitivity) within 2 hours prior to exercise.26 The food or exercise alone will not cause symptoms, and there are no proven measures to prevent an episode of exercise-induced anaphylaxis with the exception of avoiding the known inciting food. These patients should be counseled to carry epinephrine and not to exercise alone.50
Other Causes of Anaphylaxis. Another rare but reported cause of anaphylaxis is seminal fluid-induced anaphylaxis.33 Considering that sexual activity in the adolescent population is not a rarity, the possibility must be considered in an adolescent patient presenting to the pediatric ED in anaphylaxis and without a clear inciting factor. This hypersensitivity may be to either antigens present in the semen or those passed unwittingly via the seminal fluid, such as when the male ingests a food to which the partner has a known sensitivity.
The development of anaphylaxis in the presence of synergistic co-factors (e.g., food and exercise, or drugs and exercise)49 is often puzzling. In addition, reactions labeled as "idiopathic" or "unknown" account for more than 30% of anaphylaxis cases.51,52 In these cases, there was no known exposure to likely agents, or the reaction could not be reproduced with exposure to individual agents.53 Efforts to better define the cause of anaphylaxis through laboratory studies may provide further information on cases of idiopathic anaphylaxis.54,55
Diagnosis and Symptoms
Anaphylaxis may present as an array of symptoms involving multiple organ systems. Cutaneous symptoms, such as urticaria or itching, are present in nearly all anaphylactic reactions,44 although their absence should not preclude a diagnosis of anaphylaxis.33,56 Other symptoms are listed in Table 1. Familiarity with these symptoms, particularly the paradoxical ones, such as bradycardia in the setting of shock, may lead to more effective recognition and treatment of anaphylaxis.
| Table 1. Symptoms of Anaphylactic Reactions |
|
|
Schemes designed to grade the severity of anaphylaxis may be useful in determining prognosis, although a uniform approach to this has not permeated emergency medicine practice. In such schemes, severity is based upon the type and number of organ systems involved.10,24,44 Intuitively, it may be reasonable to categorize the life-threatening symptoms such as airway edema, respiratory distress, cardiovascular compromise, and loss of consciousness as severe. On the other hand, anaphylactic reactions that do not involve life-threatening symptoms may be intuitively termed mild. It has been suggested that the more subtle distinctions afforded by a five-tier grading system may have some utility in prognosis, such as predicting a late phase reaction.24 A three-tier system proposed by Brown, (Table 2) however, may offer a reasonable, relatively intuitive, yet evidence-based approach to severity grading.
| Table 2. Grading System for Generalized Hypersensitivity Reactions |
|
|
Management
Prehospital Management. The successful treatment of anaphylaxis may well depend upon what transpires before the patient reaches the hospital.57,58 Indeed, it has been well described that delay in treating anaphylaxis with epinephrine is a factor in fatalities.28,42,59-62
Many patients presenting to the ED with anaphylaxis have a known history of allergy to the offending agent. These patients often know to take an antihistamine, and many have been prescribed an epinephrine auto-injector,63-65 although there may be some confusion and reluctance regarding its use. This hesitation may stem from misconceptions in the lay population about epinephrine, such as: 1) Mild symptoms will serve as a warning of a severe attack; 2) Medical attention is being sought, therefore, administering epinephrine can wait until it is administered by a professional; and 3) Epinephrine will always work when given, even if it is delayed.66 In addition, the epinephrine auto-injector may not be readily available at the time of the exposure.
When a patient arrives in the ED, it is important to determine what, if any, medications the patient received in the field. A patient brought in by emergency medical services may well have been pretreated with epinephrine, antihistamines, and intravenous fluids. For the sake of clarity, the following discussion of ED management will assume no such prehospital treatment, although additional use of epinephrine may be required, even if given in the field.
Assessment in the Emergency Department
History. A patient presenting with signs and symptoms consistent with anaphylaxis is a true medical emergency. A rapid assessment of the "ABC's" should be initiated while simultaneously acquiring a brief, targeted history. The history should start with questions about the exposure, including whether the patient has a known allergy. It is important to obtain some basic information about the patient's symptoms and whether the patient was treated prior to arrival. This information will affect management decisions in the ED. One also should inquire about a history of co-morbid illnesses, such as asthma or atopy, because these may be predictive of a more severe reaction.67
Timely intervention is crucial in all patients presenting with clinical symptoms consistent with anaphylaxis. A history of previous allergic or anaphylactic reactions — including their severity and nature (uniphasic, biphasic, or protracted) — will be useful in anticipating complications and determining disposition. Even in the presence of only mild symptoms, one may decide to use epinephrine solely based upon the history of a previous, severe reaction to the same type of exposure.24
Airway. The patient's airway should be assessed immediately for patency. The presence of potentially complicating factors (e.g., facial or mucosal edema, hoarseness, or stridor) should prompt rapid intervention. In the presence of any airway symptoms, intramuscular (IM) epinephrine administration should be the first intervention. Additional airway management, such as endotracheal intubation, may be obviated by the timely vasoconstricting effects of epinephrine but may become necessary in refractory cases. In most cases, early administration of corticosteroids will prevent late-phase airway edema. The presence of airway edema may make orotracheal intubation extremely challenging. In this case, advanced airway techniques (e.g., needle cricothyrotomy or a surgical airway) may be viable options.
Breathing. Following rapid assessment and securing of the airway, the patient's breathing should be evaluated. Both increased and decreased respiratory rates should alert the physician to potentially worsening respiratory status. In addition, the presence of retractions, nasal flaring, grunting, or seesaw respirations should be noted. The lung fields should be assessed for air exchange and the presence of bronchospasm. Supplemental oxygen should be supplied, and bronchospasm treated aggressively. In addition to intramuscular epinephrine, beta-agonists (e.g., nebulized albuterol) should be given. Steroids also play a role in the treatment of bronchial obstruction in the setting of anaphylaxis, although the effects likely will be seen after the acute phase.
Circulation. Cardiovascular assessment should begin with swift assessment of the patient's color and perfusion, heart rate, and blood pressure. The patient should be placed supine and in the Trendelenberg position, if possible, to maximize blood flow to vital organs. Cardiac monitoring should be started, and intraveous access obtained. If there are any cardiovascular anomalies, intramuscular epinephrine should be administered immediately. The hypotensive patient may require massive volume repletion to maintain perfusion pressures. An initial bolus of 20 mL/kg of normal saline should be given rapidly and repeated as necessary to treat shock. It is not uncommon for a patient in hypovolemic anaphylactic shock to require as much as 100 mL/kg during the initial phase of fluid resuscitation. Refractory hypotension or evidence of poor perfusion may require the addition of vasopressor therapy.
Treatment in the Emergency Department
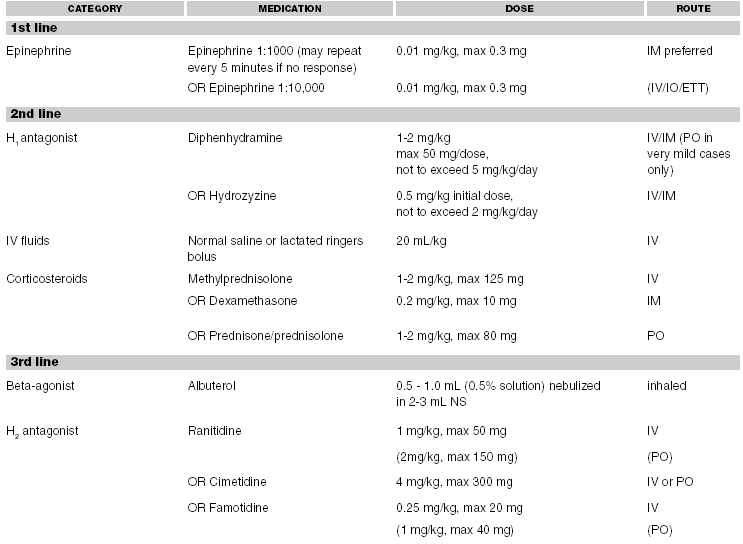
Epinephrine. This initial assessment of the "ABC's" and initiation of therapy often occurs almost simultaneously. (See Table 3.) The immediate administration of epinephrine can halt the progression of an acute phase reaction, reverse its effects, and prevent a biphasic reaction.17 Epinephrine is a direct antagonist of the chemical effects of histamine on a cellular level. It has multiple beneficial effects in the setting of anaphylaxis. In addition to being an effective bronchodilator, it is a potent vasoconstrictor and increases blood pressure, heart rate, and contractility while preventing further capillary leakage. Moreover, epinephrine inhibits further cell mediator release. The dose of epinephrine is 0.01 mg/kg (0.01mL/kg of 1:1000) with a maximum of 0.3 mg (0.3 mL). Although the risk to a child of appropriately dosed epinephrine is small, overdosing may lead to adverse effects.59,68,69 More commonly, incorrect administration will result in less than optimal effectiveness.64 Intramuscular administration is the route of choice and has been demonstrated to be superior to the subcutaneous route in both adults and children, with more rapid absorption and less time to peak levels.70,71 Intravenous or intraosseous administration of 0.01 mg/kg (0.1 mL/kg of 1:10,000) epinephrine solution should be reserved for patients who present in arrest or who have severe symptoms (e.g., profound hypotension or poor perfusion) that do not respond to the initial intramuscular dose. A continuous infusion of epinephrine may be needed in patients who remain symptomatic or unstable. The use of inhaled epinephrine is not an effective substitute for intramuscular injection. Nebulized epinephrine may be a helpful adjunct in the treatment of upper airway edema and stridor, but unlike viral laryngotracheobronchitis (croup), local delivery of epinephrine is not sufficient, and epinephrine must be delivered systemically. It has been shown that effective plasma levels are not attained by inhalation of epinephrine alone.72
| Table 3. Standard Medication Regimen in Anaphylaxis |
|
|
Antihistamines. H1 antagonists (e.g., diphenhydramine or hydroxyzine) work as direct competitors for binding sites with histamine. While their effect is slower than epinephrine, they are important for the amelioration of symptoms, halting further progression and preventing late-phase reactions. Diphenhydramine can be administered at 1-2 mg/kg IV, IM, or PO. The oral route should be reserved for those patients with mild symptoms. H2 antagonists (e.g., ranitidine or famotidine) may be used as adjuncts to the H1 blockade. There is some competitive antagonism for H1 binding sites with these agents, and it has been shown that the concurrent administration of both H1 and H2 antagonists increases the effectiveness of both.24,33,73The newer, nonsedating H1 antagonists (e.g., loratadine, cetirizine, fexofenadine, and their datives) commonly are deemed not indicated for the management of anaphylaxis.74 While diphenhydramine is officially approved for the use in anaphylaxis, these newer drugs are not yet so. However, many physicians do use these medications off-label for patients suffering from anaphylaxis, and it is possible that their rapid absorption, long half-lives, and minimal side effects eventually may render them the antihistamines of choice.
Corticosteroids. Steroid administration, either IV or PO, also is believed to be an important adjunctive therapy in the treatment of anaphylaxis, although there are no placebo-controlled trials to support their use.33 While they are believed to have no immediate therapeutic effect, steroids may block or reduce late-phase reactions, as well as being valuable therapy in the management of bronchial obstruction (particularly in asthmatic patients).75 Dosing is based upon equivalents of 1-2 mg/kg of methylprednisolone (IV) every 6 hours. Dexamethasone 0.2 mg/kg may be useful when given intramuscularly. It has been suggested that in milder cases, 0.5-2 mg/kg prednisone (PO) also may be effective.33 Paradoxically, hypersensitivity to a variety of corticosteroids has been described. 76-78
Special Considerations (See Table 4). A special situation to consider is the patient taking beta-blockers, such as a child with congenital heart disease or renal disease. Beta-blockers have been shown to increase the severity and possibly the incidence of anaphylaxis. In addition, these drugs may render standard anaphylaxis medications (e.g., epinephrine) ineffective. In the setting of a beta-antagonist, the effects of epinephrine may be only alpha-adrenergic.79-81
| Table 4. Medications for Special Situations in Anaphylaxis |
|
|
The patient taking a beta-blocker may benefit from the administration of atropine, intravenous glucagon, or aminophylline. Atropine commonly is given in a nebulized form for the treatment of acute wheezing and may be helpful in patients for whom albuterol may not be effective. In addition, bradycardia is a potential cardiovascular symptom of anaphylaxis and intravenous atropine also may be indicated. Glucagon bypasses the beta-adrenergic receptor and directly activates the adrenergic cascade. In addition, aminophylline—while always an available adjunct in the management of severe bronchospasm—should be strongly considered in this patient population because it also bypasses the beta-receptor.20
Another special consideration is anaphylaxis induced by an injection or sting. In this setting, the application of a venous tourniquet proximal to the site of injection may be helpful to control the distribution of the inciting agent. A local infiltration of epinephrine at the site also may produce vasoconstriction that will impede its absorption. Local applications of ice packs also may be helpful.82
Laboratory Evaluation. Laboratory markers, such as tryptase, may be elevated in the setting of an allergic reaction.54,83,84 However, the emergency treatment of anaphylaxis should not be delayed pending laboratory confirmation; therefore, these markers are of no utility in the evaluation of a patient presenting to the ED with anaphylaxis.
Disposition
The decision to discharge a patient from the ED depends upon many factors. The severity of the reaction, the degree of resuscitation required, the home environment, the risk of a late-phase reaction, and access to emergency care are just a few of the factors to be considered.
The rate of biphasic reactions varies significantly among studies (5%-20%), and it is difficult to predict which patients are at a higher risk for recurrence of symptoms.15,18,85 A delay in the administration of epinephrine,17 the requirement of multiple initial doses of epinephrine,16 a delay in the onset of symptoms more than 30 minutes post-exposure, and oral route of exposure to the inciting agent14 are factors that have been associated with an increased risk for a biphasic reaction. The asymptomatic interval between acute and late phase reactions can vary from 1 hour to more than 12 hours (30 hours has been reported).14,17,18,33 Similarly, suggestions for what constitutes an appropriate length of observation in the ED after successful treatment vary. It does appear reasonable that the patient who has experienced a mild reaction and has responded quickly to initial interventions may be considered for discharge after a 4 to 6 hour period of observation in the ED.24,82,86 It is recommended to continue the use of oral steroids and antihistamines (H1 and H2 blockers) for 2-5 days.87 The patient should be prescribed an epinephrine auto-injector.
The risk of recurrence of symptoms must be reflected in the discharge instructions and emphasized with the family. As always, the patient's primary care physician should be contacted upon the patient's arrival to the ED and continually updated on the patient's condition. Early involvement of a physician who is familiar with the patient and his family may prove invaluable when making decisions regarding disposition and follow-up. If the primary care physician proves unreachable, the patient should be instructed to contact his/her primary medical home within 24 hours of the ED visit. In addition, referral to an allergist for both counseling and testing is appropriate following an episode of anaphylaxis.
Any patient who experiences a moderate to severe or prolonged course, particularly if there is airway or cardiovascular involvement, should be hospitalized. Any doubt about the family's ability to seek medical attention quickly or any question about the home environment or social situation are additional indications for hospital admission.87,88
Patient Education
Perhaps the most important steps in preparing to discharge a patient from the ED after an episode of anaphylaxis are educating the patient and family about the avoidance of the suspected offending agent and the indications and use of epinephrine in the prehospital setting.89
Any patient being discharged to home should have a prescription for a self-administration epinephrine kit. Spring-loaded portable auto-injectors deliver 0.3 mg or 0.15 mg of epinephrine. The auto-injector is designed for injection into the lateral thigh muscle and can be used through clothing. The pre-measured auto-injector is the preferred route of administration of epinephrine in the prehospital setting because it eliminates the confusion of attempting to administer epinephrine via the "vial-ampule-and-syringe" method, which has been shown to result in delayed administration as well as inconsistency in dosing.65
Large-dose (0.3mg) auto-injectors should be prescribed for patients weighing more than 30 kg. However, there are a few circumstances in which this higher dose may be considered for patients weighing less than 30 kg: 1) patients with a history of asthma or severe allergic events, 2) patients with poor access to emergency medical care, and 3) patients weighing close to 30 kg.63,90 For children 15-30 kg, the lower dose auto-injector typically should be prescribed. Failure to transition to the larger dose auto-injector when the child grows is a common cause of under-dosing epinephrine. Children weighing less than 15 kg should, in our opinion, also should be prescribed the lower dose auto-injector. The risks to the child of higher than recommended doses of epinephrine are likely to be outweighed by the benefits of rapid delivery afforded by the auto-injector technology.
Demonstrating the use of the auto-injector can prevent inadvertent and harmful injection of epinephrine into the patient or caregiver's thumb,91-93 and help ensure that the drug is effectively delivered. Every ED should have access to empty auto-injectors for teaching purposes, and every physician should know how to use one. In addition, every prescription should be accompanied by a demonstration and a discussion of the indications for its use. It should be emphasized that the early administration of epinephrine may be lifesaving; when in doubt, it is often wiser to give the medication than to delay therapy.66 The family should be reminded that the administration of epinephrine via an auto-injector is not definitive care. They should be instructed to alert emergency services upon administration of the drug and expect evaluation and treatment at a medical facility. Of note, a family can be reassured that an outdated auto-injector still may be useful, although suboptimal, and should be given if it is the only auto-injector available and as long as there is no discoloration or apparent precipitates.94
In addition to always keeping an auto-injector readily available, patients and caregivers also should be instructed to always have diphenhydramine available. Diphenhydramine is available in a variety of preparations, including a dissolvable "fastmelt" form, which is convenient to carry and generally well tolerated by children.
Patients and families should be counseled to avoid the suspected triggers, and that recurrent reactions, as well as reactions to new triggers, are not uncommon.9,85 In a patient with a food allergy, the parents should be encouraged: 1) to gain knowledge of potentially cross-reacting agents, 2) to read food labels, and 3) to know, to their best ability, the ingredients of every food presented to the child. The parents should also educate other care providers, such as school or daycare staff.
Medicolegal Lessons
Given the fairly standard approach to the treatment of anaphylaxis, claims of medical malpractice in cases of anaphylaxis are uncommon. However, when claims are made, they are typically in response:
1) to failures to recognize the condition and its severity,
2) to failure to provide anticipatory guidance regarding preventive measures, or
3) to the complications of epinephrine use.87
Conclusion
Anaphylaxis is a life-threatening hypersensitivity reaction characterized by its effects on multiple organ systems. Contrary to common misconception, it may be fatal, even in the absence of respiratory involvement. Treatment is usually straightforward, and the early administration of intramuscular epinephrine is the mainstay of therapy. A systematic approach to the resuscitation of a patient who presents with anaphylaxis is useful for the emergency physician. If one considers the diagnosis of anaphylaxis in any patient with multiple somatic complaints in the presence of pruritis or rash, this should lead to enhanced recognition and timely treatment. A familiarity with the symptoms of anaphylaxis and their significance in determining the severity of an event will be useful in making treatment and disposition decisions. Perhaps the most lifesaving intervention is the time taken to counsel families to recognize and appropriately manage anaphylactic events, with prevention being the ultimate goal.
References
1. Whitley S. The history of immediate hypersensitivity reactions. Anesthesiology 1995;82(1);316.
2. Portier P, Richet C. De l'action anaphylactique de quelques venins. Comptes Rendus de Societe Biologique 1902;54;170-72.
3. Cohen SG, Zelaya-Quesada M. Portier, Richet, and the discovery of anaphylaxis: a centennial. J Allergy Clin Immunol 2002;110(2);331-36.
4. The Nobel Prize in Physiology or Medicine 1913. Available at: www.nobelprize.org.
5. Neugut AI, Ghatak AT, Miller RL. Anaphylaxis in the United States: an investigation into its epidemiology. Arch Intern Med 2001;161(1); 15-21.
6. Ring J, Brockow K, Behrendt H. History and classification of anaphylaxis. Novartis Found Symp 2004;257;6-16; discussion 16-24, 45-50;276-85.
7. Kemp S F, Lockey RF. Anaphylaxis: a review of causes and mechanisms. J Allergy Clin Immunol 2002;110(3);341-48.
8. Brown AF, McKinnon D, Chu K. Emergency department anaphylaxis: a review of 142 patients in a single year. J Allergy Clin Immunol 2001;108(5);861-66.
9. American Academy of Asthma, Allergy and Immunology Board of Directors. Anaphylaxis in schools and other child-care settings. J Allergy Clin Immunol 1998;102;173-76.
10. Ring J, Behrendt H. Anaphylaxis and anaphylactoid reactions. Classification and pathophysiology. Clin Rev Allergy Immunol 1999; 17(4);387-99.
11. Murrant T, Bihari D. Anaphylaxis and anaphylactoid reactions. Int J Clin Pract; 2000;54(5);322-28.
12. Greenberger PA. Contrast media reactions. J Allergy Clin Immunol 1984;74(4 Pt 2);600-05.
13. The diagnosis and management of anaphylaxis. Joint Task Force on Practice Parameters, American Academy of Allergy, Asthma and Immunology, American College of Allergy, Asthma and Immunology, and the Joint Council of Allergy, Asthma and Immunology. J Allergy Clin Immunol 1998 Jun;101(6 Pt 2):S465-52813.
14. Stark BJ, Sullivan TJ. Biphasic and protracted anaphylaxis. J Allergy Clin Immunol 1986;78(1 Pt 1);76-83.
15. Douglas DM, Sukenick E, Andrade W, Brown JS. Biphasic systemic anaphylaxis: an inpatient and outpatient study. J Allergy Clin Immunol 1994;93(6);977-85.
16. Brazil E, MacNamara AF. "Not so immediate" hypersensitivity—the danger of biphasic anaphylactic reactions. J Accid Emerg Med 1998; 15(4);252-53.
17. Lee JM, Greenes DS. Biphasic anaphylactic reactions in pediatrics. Pediatrics 2000;106(4);762-66.
18. Popa VT, Lerner SA. Biphasic systemic anaphylactic reaction: three illustrative cases. Ann Allergy 1984;53(2);151-55.
19. Dibs SD, Baker MD. Anaphylaxis in children: a 5-year experience. Pediatrics 1997;99(1);E7.
20. Kemp SF. Current concepts in pathophysiology, diagnosis, and management of anaphylaxis. Immunol Allergy Clin North Am 2001;21(4);611-34.
21. Smith PL, Kagey-Sobotka A, Bleecker ER, et al. Physiologic manifestations of human anaphylaxis. J Clin Invest 1980;66(5);1072-80.
22. Yunginger JW. Lethal food allergy in children. N Engl J Med 1992; 327(6);421-22.
23. Burks W, Bannon GA, Sicherer S, Sampson HA. Peanut-induced anaphylactic reactions. Int Arch Allergy Immunol 1999;119(3);165-72.
24. Sampson HA. Anaphylaxis and emergency treatment. Pediatrics 2003;111(6 Pt 3);1601-08.
25. Sicherer SH. Food allergy. Lancet 2002;360(9334);701-10.
26. Sampson HA. Food anaphylaxis. Br Med Bull 2000;56(4);925-35.
27. Foucard T, Malmheden-Yman I. Food-induced anaphylaxis. Pediatr Allergy Immunol 2001;12 Suppl 14;97-101.
28. Bock SA, Munoz-Furlong A, Sampson HA. Fatalities due to anaphylactic reactions to foods. J Allergy Clin Immunol 2001;107(1);191-93.
29. Vander Leek TK, Liu AH, Stefanski K, et al. The natural history of peanut allergy in young children and its association with serum peanut-specific IgE. J Pediatr 2000;137(6);749-55.
30. Spergel JM, Fiedler JM. Natural history of peanut allergy. Curr Opin Pediatr 2001;13(6);517-22.
31. Cantani A, Lucenti P. Natural history of soy allergy and/or intolerance in children, and clinical use of soy-protein formulas. Pediatr Allergy Immunol 1997;8(2);59-74.
32. Vance GH, Holloway JA. Early life exposure to dietary and inhalant allergens. Pediatr Allergy Immunol 2002;13 Suppl 15;14-18.
33. Joint Task Force on Practice Parameters; American Academy of Allergy, Asthma and Immunology; American College of Allergy, Asthma and Immunology; Joint Council of Allergy, Asthma and Immunology. The diagnosis and management of anaphylaxis: an updated practice parameter. J Allergy Clin Immunol 2005 Mar;115(3 Suppl):S483-523.
34. Anne S, Reisman RE. Risk of administering cephalosporin antibiotics to patients with histories of penicillin allergy. Ann Allergy Asthma Immunol 1995;74(2);167-70.
35. Stevenson DD. Aspirin and NSAID sensitivity. Immunol Allergy Clin North Am 2004;24(3);491-505, vii.
36. Stevenson DD. Anaphylactic and anaphylactoid reactions to aspirin and other nonsteroidal anti-inflammatory drugs. Immunol Allergy Clin North Am 2001;21(4);1-3.
37. Randolph C. Latex allergy in pediatrics. Curr Probl Pediatr 2001; 31(5);131-53.
38. Kemp SF, Lockey RF, Wolf BL, Lieberman P. Anaphylaxis. A review of 266 cases. Arch Intern Med 1995;155(16);1749-54.
39. Cochran ST. Anaphylactoid reactions to radiocontrast media. Curr Allergy Asthma Rep 2005;5(1);28-31.
40. Greenberger P A, Patterson R. The prevention of immediate generalized reactions to radiocontrast media in high-risk patients. J Allergy Clin Immunol 1991;87(4);867-72.
41. Thong B Y, Yeow-Chan. Anaphylaxis during surgical and interventional procedures. Ann Allergy Asthma Immunol 2004;92(6);619-28.
42. Sampson HA, Mendelson L, Rosen JP. Fatal and near-fatal anaphylactic reactions to food in children and adolescents. N Engl J Med 1992;327(6);380-84.
43. Bahna SL. Insect sting allergy: a matter of life and death. Pediatr Ann 2000;29(12);753-58.
44. Brown SG. Clinical features and severity grading of anaphylaxis. J Allergy Clin Immunol 2004;114(2);371-76.
45. Graft DF, Schuberth KC, Kagey-Sobotka A, et al. A prospective study of the natural history of large local reactions after Hymenoptera stings in children. J Pediatr 1984;104(5);664-68.
46. Sicherer SH. Advances in anaphylaxis and hypersensitivity reactions to foods, drugs, and insect venom. J Allergy Clin Immunol 2003; 111(3 Suppl);S829-34.
47. Novembre E, Cianferoni A, Bernardini R, et al. Anaphylaxis in children: clinical and allergologic features. Pediatrics 1998;101(4);E8.
48. Hosey RG, Carek PJ, Goo A. Exercise-induced anaphylaxis and urticaria. Am Fam Physician 2001;64(8);1367-72.
49. Harada S, Horikawa T, Ashida M, et al. Aspirin enhances the induction of type I allergic symptoms when combined with food and exercise in patients with food-dependent exercise-induced anaphylaxis. Br J Dermatol 2001;145(2);336-39.
50. Sheffer AL. Anaphylaxis. J Allergy Clin Immunol 1988;81(5 Pt 2); 1048-50.
51. Yocum MW, Butterfield JH, Klein JS, et al. Epidemiology of anaphylaxis in Olmsted County: A population-based study. J Allergy Clin Immunol 1999;104(2 Pt 1);452-56.
52. Stewart AG, Ewan PW. The incidence, aetiology and management of anaphylaxis presenting to an accident and emergency department. QJM 1996;89(11);859-64.
53. Orfan NA, Stoloff RS, Harris KE, Patterson R. Idiopathic anaphylaxis: total experience with 225 patients. Allergy Proc 1992;13(1);35-43.
54. Yunginger JW, Nelson DR, Squillace DL, et al. Laboratory investigation of deaths due to anaphylaxis. J Forensic Sci 1991;36(3);857-65.
55. Pumphrey RS, Stanworth SJ. The clinical spectrum of anaphylaxis in north-west England. Clin Exp Allergy 1996;26(12);1364-70.
56. Hollnberger H, Gruber E, Frank B. Severe anaphylactic shock without exanthema in a case of unknown latex allergy and review of the literature. Paediatr Anaesth 2002;12(6);544-51.
57. Bochner BS, Lichtenstein LM. Anaphylaxis. N Engl J Med 1991; 324(25);1785-90.
58. Simons FE. First-aid treatment of anaphylaxis to food: focus on epinephrine. J Allergy Clin Immunol 2004;113(5);837-44.
59. Pumphrey RS. Lessons for management of anaphylaxis from a study of fatal reactions. Clin Exp Allergy 2000;30(8);1144-50.
60. Barnard JH. Studies of 400 Hymenoptera sting deaths in the United States. J Allergy Clin Immunol 1973;52(5);259-64.
61. Safdar B, Cone DC, Pham KT. Subcutaneous epinephrine in the prehospital setting. Prehosp Emerg Care 2001;5(2);200-07.
62. Frazier CA. Allergic reactions to insect stings: A review of 180 cases. South Med J 1964;57;1023-34.
63. Simons FE, Peterson S, Black CD. Epinephrine dispensing for the out-of-hospital treatment of anaphylaxis in infants and children: a population-based study. Ann Allergy Asthma Immunol 2001;86(6); 622-26.
64. Simons FE. Epinephrine (adrenaline) in the first-aid, out-of-hospital treatment of anaphylaxis. Novartis Found Symp 2004;257;228-43; discussion 243-7, 276-85.
65. Simons FE, Chan ES, Gu X, Simons KJ. Epinephrine for the out-of-hospital (first-aid) treatment of anaphylaxis in infants: Is the ampule/syringe/needle method practical? J Allergy Clin Immunol 2001;108(6);1040-44.
66. American Academy of Asthma, Allergy & Immunology. Advocacy Statement: The Use of Epinenephrine in the Treatment of Anaphylaxis. Available at: www.aaaai.org/media/resources/academy_statements/advocacy_statements/ps26.asp
67. Settipane GA, Klein DE, Boyd GK. Relationship of atopy and anaphylactic sensitization: a bee sting allergy model. Clin Allergy 1978; 8(3);259-65.
68. Davis CO, Wax PM. Prehospital epinephrine overdose in a child resulting in ventricular dysrhythmias and myocardial ischemia. Pediatr Emerg Care 1999;15(2);116-18.
69. Horowitz BZ, Jadallah S, Derlet RW. Fatal intracranial bleeding associated with prehospital use of epinephrine. Ann Emerg Med;1996; 28(6);725-27.
70. Simons FE, Gu X, Simons KJ. Epinephrine absorption in adults: intramuscular versus subcutaneous injection. J Allergy Clin Immunol 2001;108(5);871-73.
71. Simons FE, Roberts JR, Gu X, Simons KJ. Epinephrine absorption in children with a history of anaphylaxis. J Allergy Clin Immunol 1998; 101(1 Pt 1);33-37.
72. Simons FE, Gu X, Johnston LM, Simons KJ. Can epinephrine inhalations be substituted for epinephrine injection in children at risk for systemic anaphylaxis? Pediatrics 2000;106(5);1040-44.
73. Brown AF. Therapeutic controversies in the management of acute anaphylaxis. J Accid Emerg Med 1998;15(2);89-95.
74. Simons FE. H1-antihistamines in children. Clin Allergy Immunol 2002;17;437-64.
75. Miura T, Inagaki N, Yoshida K, et al. Mechanisms for glucocorticoid inhibition of immediate hypersensitivity reactions in rats. Jpn J Pharmacol 1992;59(1);77-87.
76. Schonwald S. Methylprednisolone anaphylaxis. Am J Emerg Med 1999;17(6);583-85.
77. Figueredo E, Cuesta-Herranz, JI, De Las Heras M, et al. Anaphylaxis to dexamethasone. Allergy 1997;52(8);877.
78. Erdmann SM, Abuzahra F, Merk HF, et al. Anaphylaxis induced by glucocorticoids. J Am Board Fam Pract 2005;18(2);143-46.
79. Lang DM, Alpern MB, Visintainer PF, Smith,ST. Increased risk for anaphylactoid reaction from contrast media in patients on beta-adrenergic blockers or with asthma. Ann Intern Med 1991;115(4);270-76.
80. Toogood JH. Risk of anaphylaxis in patients receiving beta-blocker drugs. J Allergy Clin Immunol 1988;81(1);1-5.
81. Toogood JH. Beta-blocker therapy and the risk of anaphylaxis. CMAJ 1987;136(9);929-33.
82. Stevenson MD, Ruddy RM. Asthma and allergic emergencies. In: Fleisher GR, Ludwig S, Henretig FM (eds.) Pediatric Emergency Medicine. Philadelphia:Lippincott Williams & Wilkins;2006;1067-68.
83. Edston E, van Hage-Hamsten M, Johansson SG. Tryptase—at last a useful diagnostic marker for anaphylactic death. Allergy 1996;51(6); 443-45.
84. Lin RY, Schwartz LB, Curry A, et al. Histamine and tryptase levels in patients with acute allergic reactions: An emergency department-based study. J Allergy Clin Immunol 2000;106(1 Pt 1);65-71.
85. Mullins RJ. Anaphylaxis: risk factors for recurrence. Clin Exp Allergy 2003;33(8);1033-40.
86. Edwards KH, Johnston C. Allergic and immunologic disorders. In: Barkin RM, Caputo GL, Jaffe DM, et al (eds). Pediatric Emergency Medicine: Concepts and Clinical Practice. St. Louis:Mosby; 1992:619-630..
87. Krause R. (2004). Anaphylaxis. eMedicine.
88. Gavalas M, Sadana A, Metcalf S. Guidelines for the management of anaphylaxis in the emergency department. J Accid Emerg Med 1998; 15(2);96-98.
89. Schwartz HJ. Acute allergic disease in a hospital emergency room: a retrospective evaluation of one year's experience. Allergy Proc 1995; 16(5);247-50.
90. Simons FE, Gu X, Silver NA, Simons KJ. EpiPen Jr versus EpiPen in young children weighing 15 to 30 kg at risk for anaphylaxis. J Allergy Clin Immunol 2002;109(1);171-75.
91. McCauley W A, Gerace RV, Scilley C. Treatment of accidental digital injection of epinephrine. Ann Emerg Med 1991;20(6);665-68.
92. Burkhart KK. The reversal of the ischemic effects of epinephrine on a finger with local injections of phentolamine. J Emerg Med 1992; 10(4);496.
93. Maguire WM, Reisdorff EJ, Smith D, Wiegenstein JG. Epinephrine-induced vasospasm reversed by phentolamine digital block. Am J Emerg Med 1990;8(1);46-47.
94. Simons FE, Gu X, Simons KJ. Outdated EpiPen and EpiPen Jr autoinjectors: past their prime? J Allergy Clin Immunol 2000;105(5); 1025-30.
Anaphylaxis is a true life-threatening emergency that may occur following a variety of exposures. Foods, such as peanuts and tree nuts, antibiotics, and more recently, latex have all been implicated as potential triggers of a severe analpylactic reaction.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.