A Not Completely Normal ECG
ECG Review
A Not Completely Normal ECG
By Ken Grauer, MD, Professor, Assistant Director, Family Practice Residency Program, University of Florida.
|
|
|
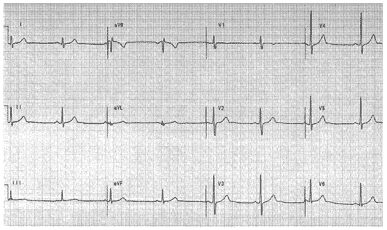
Figure. 12-lead ECG obtained from an otherwise healthy 32-year-old man with atypical chest pain. |
Clinical Scenario: The 12-lead ECG in the Figure was obtained from a healthy 32 year old man who had some atypical chest pain. Although there are no ECG findings suggestive of acute ischemia, we disagree with the computer interpretation that said "sinus bradycardia but otherwise normal". Why?
Interpretation/Answer: The rhythm is sinus bradycardia and arrhythmia at a rate of about 50/minute. PR, QRS and QT intervals are normal. The mean QRS axis is + 70°. There is no ECG evidence of chamber enlargement. Regarding QRST changes, there are very small septal q waves in leads I, aVL, and V6. ST-T waves are normal. S waves are present across the precordial leads (albeit the S wave is small in lead V6). The most remarkable finding on this tracing is the relatively tall R wave in lead V1. Normally the heart's electrical activity is oriented leftward and posteriorly in the transverse plane. As a result, the QRS complex in right-sided lead V1 is usually either all negative (a QS complex), or almost all negative (a small amplitude positive r wave reflecting septal activation followed by a deep S wave). The finding of R = S in lead V1 as seen in this tracing therefore represents a relative increase in right and/or anterior forces. Outside of the pediatric age group where this finding is common as a normal variant, the presence of an R wave that equals or exceeds S wave amplitude in lead V1 should be recognized in adults as more likely to indicate some underlying abnormality. The following differential diagnosis is suggested: i) RBBB (right bundle branch block); ii) WPW (Wolff-Parkinson-White syndrome; iii) RVH (right ventricular hypertrophy); iv) posterior infarction; v) hypertrophic or other cardiomyopathy; or vi) normal variant in an otherwise healthy adult. Normal QRS duration and lack of delta waves rules out the first two possibilities in this example. RVH is unlikely in the absence of supportive findings such as RAE (right atrial enlargement), RAD (right axis deviation), right ventricular strain. Posterior infarction is unlikely in the absence of associated inferior infarction, especially in view of the benign history of this patient. Cardiomyopathies are usually associated with other ECG findings. By the process of elimination, this leaves "normal variant" as the most probable explanation for the relative increase of R wave amplitude in lead V1. Careful physical examination is advised to ensure no abnormal cardiac findings. Consideration should be given to obtaining an echocardiogram to rule out occult structural cardiac abnormality.
A picture of a 12-lead ECG was obtained from a healthy 32 year old man who had some atypical chest pain. Although there are no ECG findings suggestive of acute ischemia, doctors disagree with the computer interpretation ...Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.