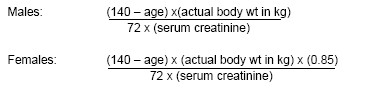Cardioprotection in the Emergency Department: Part II
Cardioprotection in the Emergency Department: Part II
Authors: Michael C. Plewa, MD, FAAEM, FACEP, Research Director, St. Vincent Mercy Medical Center, Toledo, OH; Kevin M. Casey, DO, FACEP, FAAEM, Assistant Director, Emergency Department, St. Vincent Mercy Medical Center, Toledo, OH; and Randall W. King, MD, FACEP, Director, Emergency Medicine Residency, St. Vincent Mercy Medical Center, Toledo, OH; Assistant Clinical Professor, University of Toledo College of Medicine.
Peer Reviewers: Brian Tiffany, MD, PhD, Chairman, Department of Emergency Medicine, Chandler Regional Hospital, Scottsdale, AZ; and Gregory A. Volturo, MD, FACEP, Professor of Emergency Medicine and Medicine, Vice-Chair, Department of Emergency Medicine, University of Massachusetts Medical School, Worcester.
In Part 1 of this two-part article, the authors discussed some of the "sexy" aspects of acute coronary syndrome (ACS) patient management in the emergency department: the early use of antiplatelet and antithrombotic agents to enhance coronary artery perfusion. In the right combination with reperfusion therapy (thrombolytics or primary coronary intervention), these agents have a significant benefit in the right patient. The art of ACS management is selecting a combination that is the best possible for a particular patient. The "right" combination can have a dramatic improvement in patient outcome. The debates regarding these decisions are at the cutting edge of ACS management.
In Part 2, the authors discuss the "less sexy" aspects ACS mangement, those agents and treatments that have either a long history of use in ACS patients or are still too new to judge, but share the common feature that their use in combination with current antiplatelet, antithrombotic, and reperfusion therapy has not been shown to add clinically important benefit in improving outcome. Before being relegated to the scrap heap, it is worth remembering that some agents (oxygen, morphine, nitroglycerin) can relieve patient symptoms, and others (angiotensin-converting enzyme inhibitors, insulin) have benefit in selected patients. Thus, it is important for the emergency physician to be knowledgeable about these agents, their uses, benefits, and contraindications.
—J. Stephan Stapczynski, MD, Editor
Anti-ischemic Therapy
Oxygen. Since myocardial ischemia of acute coronary syndromes (ACS) involves an imbalance between oxygen supply and demand, it is intuitively obvious that increasing oxygen content could salvage myocardium. However, the 2004 ACC/AHA ST elevation myocardial infarction (STEMI) guidelines recommend oxygen primarily to those with oxygen saturations less than 90%, and to all uncomplicated STEMI patients during the first 6 hours. Although supplemental oxygen may limit myocardial ischemia1 and ST segment elevation,2 there is evidence to suggest that high-flow oxygen treatment can decrease cardiac output, increase oxidative stress,3 and increase systemic4 and coronary vascular resistance,5 although the clinical implications of these detrimental effects remain to be determined.
Authors' Bottom Line Recommendations: Use oxygen, perhaps the least amount necessary, for ACS patients with persistent pain, dyspnea, arrhythmias, and STEMI, and discontinue oxygen within hours of symptom resolution.
Morphine Sulfate. Morphine sulfate has been used for years as an analgesic, anxiolytic, and vasodilator for ACS. Theoretically, the relief of pain may diminish the hyperadrenergic state and decrease heart rate and blood pressure, with subsequent reductions in myocardial oxygen demand. Contraindications to morphine use are true allergy, active bronchospasm, hypotension, and respiratory depression. Complications can include hypotension, nausea, and vomiting in as many as 20% of cases, and rarely respiratory depression.
Although there are no randomized clinical trials supporting the use of morphine, or comparison trials with other opioid analgesics, the ACC/AHA guidelines recommend IV morphine for both ACS and STEMI.6,7 In contrast, however, the ongoing CRUSADE initiative8 has detected an increased risk of death (odds ratio 1.48 (95% CI 1.33-1.64)) in those receiving any morphine. It remains to be seen whether this increased mortality is related to morphine itself, or simply that morphine use is a marker for persistent or severe pain.
Authors' Bottom Line Recommendations: Use small increments (2-4 mg) of IV morphine to any ACS patient with refractory pain, carefully avoiding hypotension and respiratory depression.
Nitrates. Nitroglycerin is a nitric oxide donor, has anti-aggregatory effects on platelets,9 and functions predominantly as a vasodilator, with reductions in preload and afterload, and thereby myocardial wall tension and oxygen demand, and improvements in collateral circulation and relief of coronary spasm.
Nitroglycerin is contraindicated in hypotension (systolic blood pressure < 90 mmHg or > 30 mmHg below baseline), severe bradycardia (< 50 bpm) or tachycardia (> 100 bpm), right ventricular infarction, hypertrophic cardiomyopathy (worsening the outflow tract obstruction), and severe aortic stenosis. Patients using phosphodiesterase-5 inhibitors for erectile dysfunction, such as sildenafil (Viagra) or vardenafil (Levitra) within the previous 24 hours, or tadalafil (Cialis) within the previous 36 hours, should not receive nitroglycerin (or other nitrates) because of the risk of severe hypotension (or death) mediated by nitric oxide vasodilation.10
Adverse effects of nitroglycerin include headache, hypotension, reflex tachycardia, and increased contractility (which can be offset by beta-blocker), tolerance beyond 24 hours, and methemoglobinemia with prolonged infusion. Intravenous nitroglycerin can also result in heparin11 and alteplase (TPA) resistance12 by decreasing the serum levels of these agents.
Despite routine use in patients with chest pain, outcomes-based evidence supporting its benefit in conjunction with the current approach to ACS and acute myocardial infarction (AMI) are not strong. In unstable angina (UA), nitroglycerin improves ischemic symptoms,13-15 but long-term improvements have been difficult to demonstrate. Prior to the use of thrombolytics, nitroglycerin use in AMI may have decreased mortality by as much as 35%.16 With the use of thrombolytics, the ISIS-417 trial with 58,050 patients and the GISSI-318 trial, with 19,394 patients, failed to demonstrate benefit of nitroglycerin in AMI in terms of 5-week or 6-week mortality, respectively, although these studies were confounded by the frequent use of nitroglycerin in the control groups.
In the setting of myocardial ischemia, nitroglycerin is initially administered sublingually. If the pain and/or ischemia persist, IV nitroglycerin is given at a dose of 10 micrograms/min and increased by 10-20 micrograms/min approximately every 5-10 minutes until symptoms and/or ischemia improve or the mean arterial pressure diminishes by 10% of previous values (but not less than 90 mmHg, or less than 30 mmHg of baseline). It is speculated that low-dose nitrates may diminish infarct size when dosed to decrease blood pressure by 10%,19 yet when blood pressure drops below mean arterial pressure of 80 mmHg, nitroglycerin may potentially increase infarct size. Rapid discontinuation of nitroglycerin therapy can result in ischemia.20 Topical and oral nitrates may be as effective as IV nitroglycerin, but are not as easily titrated on or off.
Authors' Bottom Line Recommendations: In the absence of strong data to suggest nitroglycerin is harmful, and may be of some benefit, nitroglycerin still is recommended for patients with ongoing ischemic symptoms. However, if a patient is being treated with either unfractionated heparin (UFH) or alteplase and does not have an alternate IV access site, it is reasonable to discontinue nitroglycerin in favor of these agents.
Beta-Blockade. Beta-blockers alleviate myocardial oxygen demand by reducing heart rate, systemic blood pressure, and myocardial contractility. Slowing of the heart rate also improves coronary blood flow by increasing the duration of diastole. Beta-blockers also have antiarrhythmic potential.
Beta-blockers are contraindicated in shock, moderate to severe (decompensated) left ventricular (LV) failure, hypotension (systolic blood pressure < 100 mmHg), bradycardia (heart rate < 50 bpm), PR interval prolongation > 0.24 seconds, 2nd or 3rd degree atrioventricular block (or sick-sinus syndrome) without a pacemaker, active asthma or reactive airway disease, as well as MI precipitated by cocaine. Small IV doses of a short-acting beta-1-selective agent such as esmolol (Brevibloc) may be given cautiously to those with shortness of breath, wheezing, rales, or borderline heart rate or blood pressure.
Side effects include bradycardia, hypotension, heart failure, and exacerbation of bronchospasm. Beta-blockers have the theoretic potential to increase coronary spasm through unopposed alpha-adrenergic stimulation,21 or to worsen coronary resistance by inhibiting the adrenergically medicated vasodilation.
Several large trials have studied beta-blockers in AMI prior to the routine use of thrombolysis or percutaneous coronary intervention (PCI). In a systematic review22 of 55 trials involving 53,268 AMI patients, the early use of beta-blockers decreased overall mortality by 1.1% absolute risk reduction (ARR) (number needed to treat [NNT]=91), 17% relative risk reduction (RRR). (See Table 1 for abbreviation definitions.) The ISIS-1 trial23 demonstrated a 0.6% ARR (NNT=167), 14% RRR in 7-day mortality in 16,027 AMI patients. In contrast, the MIAMI trial24 of 5,778 AMI patients, was unable to demonstrate a decrease in 15-day mortality with early use of metoprolol (Lopressor).
| Table 1. Abbreviations |
| ARR = Absolute risk reduction ARD = Absolute risk difference NNT = Numbers needed to treat NNH = Numbers needed to harm RRR = Relative risk reductions |
Results in the era of thrombolysis are also conflicting. In the TIMI IIB25 trial with 1434 AMI patients, metoprolol failed to demonstrate a significant difference in mortality at 6 weeks, although there was a 2.4% ARR (NNT=42), 47% RRR in reinfarction and recurrent chest pain at one week. A small study26 of AMI patients showed a 6% absolute (number needed to harm [NNH] = 17), 95% relative increase in nonfatal pulmonary edema in 100 atenolol (Tenormin) patients vs. 100 control patients, without overall change in mortality. In the GUSTO-I trial,27 30-day mortality was diminished in AMI patients treated with oral atenolol, whereas those treated with IV atenolol had 30% higher risk of death, as well as greater likelihood of heart failure, shock, recurrent ischemia, and need for pacemaker than those treated with oral atenolol.
The recently published COMMIT/SCC trial28 assessed 28-day death, reinfarction, ventricular fibrillation (VF), or cardiac arrest following metoprolol in 45,852 patients with suspected MI and has raised some controversy. The metoprolol dose was the usual 5 mg IV x 3, followed by 200 mg orally daily. Although there was a 0.5% ARR (NNT=200), 18% RRR in reinfarction, and 0.5% ARR (NNT=200), 17% RRR in ventricular fibrillation, there was no significant difference in composite endpoint of death, reinfarction, or VF/cardiac arrest (9.4% vs 9.9%). Interestingly, there was a 1.1% absolute (NNH=91), 29% relative increase in cardiogenic shock, with the majority of these events occurring within the first day of entry. In interpreting this trial, one must be aware that only 34% of subjects were randomized within 6 hours of symptom onset, and only 67% within 12 hours. None of the patients underwent PCI, and only 54% received thrombolytic therapy (usually urokinase), and 25% had Killip class II (rales < one-third lung field, S3 gallop, elevated jugular venous pressure) or III (rales > one-third lung field, frank pulmonary edema without hypotension < 90 mmHg) heart failure. Also, those patients at high risk for cardiogenic shock at study entry had worse outcomes. This study is a reminder that patients with heart failure (especially Killip class III) should not receive beta-blockade acutely.
In AMI patients undergoing PCI, there are a few positive studies. The PAMI retrospective study showed a significant 4.4% ARR (NNT=23), 67% RRR in 6-month mortality rate for IV beta-blockade in patients undergoing PCI with multivessel disease.29 In the CADILLAC study,30 30-day mortality was reduced with pretreatment with beta-blockers prior to PCI, 1.3% ARR (NNT=77), 46% RRR.
There are a few smaller studies (not adequately powered to detect survival differences) supporting the use of beta-blockers in UA-ACS with improvements in secondary outcome variables such as reduced ischemia,31-34 and an approximately 13% reduction in progression to AMI noted in a systematic review.35
There are no comparison trials to suggest one beta-blocker is more effective than another in ACS, and metoprolol, propranolol, or atenolol are the usual choices. (See Table 2.) Typical doses for some commonly used agents are listed in Table 2 and are given with target heart rate of 50-60 bpm.
| Table 2. Beta-Blockers for ACS and STEMI |
|
|
Authors' Bottom Line Recommendations: Begin an oral beta-blocker early for all ACS patients without contraindications, carefully excluding those with LV systolic dysfunction, bradycardia, or hypotension, and consider IV beta-blocker in patients with ongoing chest pain, especially if tachycardia or hypertension is present.
Calcium Channel Blockade. Calcium channel blockers have theoretic advantages in coronary disease, including rate control, vasodilation, left ventricular relaxation, afterload reduction, and antianginal and antihypertensive properties. Despite this, several trials using the calcium channel blockers nifedipine (Adalat or Procardia) or verapamil (Calan, Covera, Isoptin, Verelan) acutely during MI have shown either no benefit or a trend toward increased harm with regard to mortality, including the TRENT trial36 in 4491 patients, relative risk (RR) 1.07 (0.86-1.34); the SPRINT II trial37 in 1358 patients, RR 1.33 (0.98-1.80); and the DAVIT I trial38 in 1436 patients, RR 0.91 (0.67-1.24). Teo et al39 noted no improvement (and perhaps a trend toward increased mortality) in a meta-analysis of 24 studies of various calcium channel blockers in AMI. Similarly, a systematic review40 of 28 randomized trials including more than 19,000 MI or UA patients found no evidence of benefit in preventing death or recurrent MI with calcium channel blockers.
It generally is agreed that the rapid onset, short-acting dihydropyridines (nifedipine) are to be avoided because of increases in mortality,41,42 although verapamil or diltiazem (Cardizem, Cartia, Dilacor, Tiazac) may be considered because of potential beneficial effects. In a study of 874 AMI patients undergoing thrombolysis, 300 mg diltiazem within 36-96 hours of onset had an insignificant trend toward reduced 6-month cardiac death, non-fatal reinfarction, or refractory ischemia, but a 24% RRR in non-fatal reinfarction and refractory ischemia.43
Calcium channel blockers, such as verapamil or diltiazem, should be reserved for those situations in which rate or blood pressure control is desired in a patient where beta-blockers are contraindicated (such as in cocaine-related ischemia or infarction) or ineffective, or with presumptive coronary vasospasm (Prinzmetal's angina), and are to be used cautiously in those with LV dysfunction.
Contraindications to calcium channel blocker use include hypotension, bradycardia, atrioventricular block, and LV dysfunction with pulmonary edema or cardiogenic shock.
Authors' Bottom Line Recommendations: Generally avoid calcium channel blockers except in the rare instances when heart rate or blood pressure control is desired, and when beta-blockers are inappropriate or ineffective, such as cocaine-induced ACS or presumed vasospasm.
Angiotensin-Converting Enzyme (ACE) Inhibitors and Angiotensin Receptor Blockers (ARB). Angiotensin II may worsen myocardial ischemia via several mechanisms, including vasoconstriction, enhancing plaque rupture, thrombosis, endothelial dysfunction, oxidative stress, inflammation, and vascular remodeling. It is believed that following AMI, angiotensin II is responsible for myocardial stretching, fibrosis, and remodeling, which can lead to LV dysfunction and heart failure. ACE inhibitors, which inhibit the formation of angiotensin II, and ARBs, which block the type I angiotensin II receptor, therefore, have beneficial effects in ACS. ACE inhibitors and ARBs have myocardial protective effects including stabilization of plaque, nitric-oxide mediated vasodilation, antiplatelet and antithrombotic effects, reduction in blood pressure, and antiproliferative and antimigratory effects on vascular smooth muscle cells and white blood cells.44
Although ACE inhibitors and ARBs have been used following AMI with significant benefits in mortality and prevention of heart failure, it is their very early use that is of interest to emergency physicians. ACE inhibitors given within the first 24 hours of AMI are considered beneficial. ISIS-4,17 a study of early oral captopril (Capoten) 6.25 mg, followed by doses up to 50 mg twice daily in 58,050 AMI patients provided a 0.5% ARR (NNT=200), 7% RRR in 5-week mortality. In the GISSI-3 trial,18 oral lisinopril (Prinivil, Zestril) 5 mg, followed by daily doses up to 10 mg, decreased 42-day mortality by 12% RRR in 19,394 AMI patients. However, the CONSENSUS II trial45 of 6090 AMI patients, enalaprilat (Vasotec IV) 1 mg IV, followed by oral enalapril (Vasotec), had a trend toward higher 1- and 6-month mortality rates and worsening heart failure rates.
In a review of ACE inhibitor use in AMI, Latini46 noted a reduction in mortality rate of approximately 30% as early as 24 hours after presentation. Similarly, another overview47 of nearly 100,000 AMI patients given an ACE inhibitor within 36 hours suggests that the majority of the 0.5% ARR (NNT=200), 7% RRR in 30-day mortality occurs within the first week. In each of these trials, hypotension was the primary side effect.
ACE inhibitors or ARBs have not been investigated in the very early phase of ACS without MI, although two large trials, HOPE48 and EUROPA,49 have demonstrated 20% and 22% RRR in death, MI, stroke, or cardiac arrest with long-term (4-5 years) therapy with ramipril (Altace) or perindopril (Aceon), respectively. Since ARBs are not more effective than ACE inhibitors,50,51 they are used primarily in patients unable to tolerate ACE inhibitors. ACE inhibitors are contraindicated in hypotension, renal failure, renal artery stenosis, hypersensitivity, and history of worsening renal function, cough, or angioedema with prior ACE inhibitor use. Initial doses of ACE inhibitors are captopril 6.25 mg every 8 hours increased to maximum of 50 mg every 8 hours; enalapril 2.5 mg increased to maximum of 20 mg twice daily; or lisinopril 2.5 mg increased to maximum of 10 mg daily.
Authors' Bottom Line Recommendations:
- Consider the early use of an ACE inhibitor (or an ARB if the patient is unable to take an ACE inhibitor) in AMI patients without hypotension, especially when heart failure symptoms or history of diminished LV function are present.
- Consider using an ACE inhibitor (or an ARB if the patient is unable to take an ACE inhibitor) in ACS patients with persistent hypertension despite use of beta-blockers and nitrates.
Special Situations
Several situations deserve individual attention. First, patients already on warfarin commonly are excluded from clinical trials of antithrombotic or antiplatelet agents in ACS. Therefore, there is insufficient information to guide decisions regarding the use, especially of antiplatelet agents, in ACS patients already on warfarin. In general, when INR levels are within a therapeutic range (INR = 2-3 generally or 2.5-3.5 with a mechanical valve), UFH or low molecular weight heparin (LMWH) can be withheld, and aspirin, clopidogrel, or GP IIb/IIIa agents may be used cautiously. When INR levels are supratherapeutic, the authors feel it would be prudent to withhold UFH or LMWH as well as antiplatelet agents, although there are no studies or consensus guidelines to support this recommendation.
Second, several populations are at increased risk of bleeding52 because of excessive dosing of medications, including the elderly, women, and those with low body weight, diabetes mellitus, or congestive heart failure. Excessive dosing occurred in 42% of 3354 ACS patients overall in the CRUSADE registry,52 in 33% with UFH, in 14% with enoxaparin, and in 27% with GP IIb/IIIa inhibitors, resulting in 39% and 36% higher rates of bleeding for enoxaparin and GP IIb/IIIa inhibitors, respectively. Major bleeding was defined as any intracranial bleeding, a transfusion of at least 2 units of packed red blood cells, or a drop in hematocrit greater than 12%. Overall, major bleeding occurred in 11.5% of the population (not receiving coronary artery bypass graft [CABG]), and increased dramatically with excess dosing of GP IIb/IIIa agents, to 14.5% with mild and 29% with major excess dosing.
ACS patients with moderately and severely diminished renal function, estimated by creatinine clearance values of 30-60 mL/min and less than 30 mL/min, respectively, are 3.9 and 8.7 times as likely to die, respectively, and 3.5 and 1.9 times as likely to have major bleeding, respectively, as patients with normal renal function.53 Several medications should be given in decreased doses in the setting of renal insufficiency, including enoxaparin, bivalirudin, tirofiban, and eptifibatide. It is important to calculate the estimated creatinine clearance, for example by using the Cockcroft-Gault Equation (see Figure 1), especially in elderly or low body weight patients with relatively normal serum creatinine values that might not otherwise be suspected of having diminished creatinine clearance.
| Figre 1. Cockcroft-Gault Equation for Creatinine clearance |
|
|
Patients with pericarditis or thoracic aortic dissection may mimic ACS in symptoms and perhaps even ECG findings, yet administration of antiplatelet and antithrombotic agents in these situations could increase bleeding complications. Pericarditis should be suspected in patients with sharp pain, positional changes (worsened in the supine or lateral decubitus position), friction rub, and PR deviations on ECG. A pericardial effusion, which the authors believe is the major risk factor for hemorrhagic complications, may not result in increased cardiac silhouette on chest radiography and is best excluded by bedside echocardiography. Aortic dissection is a difficult clinical diagnosis,54 but should be suspected in the setting of abruptly severe pain, radiation into the back, neurologic symptoms, or risk factors (such as previous hypertension, congenital or inflammatory disease of the aorta or aortic valve, connective tissue disease, pregnancy, atherosclerosis, or smoking). In the absence of guidelines, the authors feel it is prudent to obtain bilateral blood pressures and upright chest radiography (knowing their low sensitivity)55 prior to use of antithrombotic and antiplatelet medications in all patients with a significant suspicion of aortic dissection, and to withhold these agents while pursuing definitive testing (transesophageal echocardiography, contrast enhanced computerized tomography, or angiography) if there is a pressure differential greater than 20 mmHg or radiographic findings of aortic disease (e.g., wide mediastinum, indistinct or widened aortic knob, apical capping, pleural effusion)54 with a high suspicion for aortic dissection.
Lastly, patients with left main disease or left main equivalent (> 70% stenosis of proximal LAD and proximal left circumflex arteries) have traditionally been managed with CABG over PCI. In these patients, avoiding clopidogrel and abciximab may be advantageous, however early diagnosis of these patients in the ED based on clinical findings is difficult. During AMI, ST elevation in aVR > V1 may help identify left main occlusion56 with accuracy of approximately 80%.57 Finding lateral ST depression (I, aVL, V5, V6) in NSTEMI may identify patients more likely (odds ratio of 2.7) to have left main or three-vessel coronary disease.58 Each of these findings can raise suspicion of left main equivalent disease, although neither has adequate accuracy to guide therapeutic decisions.
Blood Transfusion. Although transfusion in critically ill patients has come under recent scrutiny because of increased mortality rates, anemic patients with ACS are at greater risk for worsened ischemia and infarct extension,59 and traditionally have been transfused more liberally (to maintain a hematocrit of 30%). A retrospective review60 of 78,974 Medicare records noted increased 30-day mortality with transfusion for baseline hematocrit values above 36% and a decreased 30-day mortality with transfusion for baseline hematocrit values below 30%. A recent observational study of 24,112 subjects in three ACS PCI trials has refuted this finding, demonstrating increased mortality with transfusion for hematocrit above 25%.61 In the absence of prospective, randomized, clinical trials of transfusion for anemic ACS patients, recommendations are based on expert opinion and observational studies. Transfusion is likely of no benefit and probable harm when the hematocrit is greater than 25%, whereas benefit of transfusion is likely when the hematocrit is less than 21%.59
Glycemic Control. Elevations of serum glucose during AMI are as much associated with increased mortality62,63 as are low levels of serum glucose.64,65 Several trials have addressed the use of intensive insulin therapy on outcome following AMI. In the DIGAMI trial,66 a 24-hour insulin-glucose infusion was followed by subcutaneous insulin 4 times daily for more than three months vs. insulin as needed in 620 diabetics with AMI, and found a 7% ARR, (NNT=14), 27% RRR in death at 1 year and 11% ARR (NNT=9), 25% RRR in death beyond 3 years. In the HI-5 trial67 240 acute MI patients with diabetes or elevated admission blood glucose over 140 mg/dL received 24 hours of insulin-glucose infusion to maintain glucose between 72 and 170 mg/dL, followed by standard care. Although there were no significant differences in mortality at 3 or 6 months, those with mean blood glucose less than 144 mg/dL during the first 24 hours had a 9% ARR (NNT=11), 82% RRR in mortality at 6 months.
The 2004 ACC/AHA guidelines7 recommend insulin infusions for patients with hyperglycemia in AMI with complicated course, even in the absence of a known diagnosis of diabetes mellitus. Insulin infusions should target blood glucose values between 100 and 140 mg/dL and be adjusted at regular intervals (initially every hour) based on serum glucose measurements. One method of initiating an insulin infusion68 is to divide the glucose level by 100, round off to the nearest 0.5 value, then give this as the insulin bolus and infusion rate per hour. (For example, a patient with BS of 220 will get a 2.0 unit insulin bolus then 2.0 units/hr insulin infusion, whereas a patient with BS of 440 will get a 4.5 unit insulin bolus then 4.5 units/hr insulin infusion.)
Experimental Therapy
Although promising experimental therapies (such as GIK and magnesium) have not always translated into improved outcomes in large clinical trials, several experimental interventions are being studied in animal models and early clinical investigations with the hope of identifying agents that can limit infarct size and improve survival.69-71 These include adenosine, anti-apoptotic agents, antioxidants, bradykinin infusion, K(ATP) channel openers, endothelin receptor antagonists, endovascular cooling, glycogen depletion, inhibitors of renin-angiotensin system, N(+)/H(+) exchange inhibitors, natriuretic peptides, neutrophil inhibitors, niacin, nitric oxide donors, oxygen free radical scavengers, and post-conditioning (inducing brief ischemic episodes after the initial ischemic insult).
GIK. Glucose-insulin-potassium (GIK) provides metabolic support for ischemic myocardium by increasing anaerobic glycolysis and efficiency of ATP production, diminishing free fatty acid levels, restoring glycogen storage, and protecting cell membrane, sodium, and calcium homeostasis.72
Small trials in the pre-thrombolytic era suggested benefit from GIK. A meta-analysis73 of 1932 MI patients in 9 trials of GIK given within 48 hours of chest pain noted a significant 4.9% ARR (NNT=20), 30% RRR in mortality. Another meta-analysis74 of 16 trials, including the ECLA trial, suggested that high-dose GIK infusion has a 2.4% ARR (NNT=42), 27% RRR in all-cause in-hospital mortality.
However, recent large trials suggest GIK fails to benefit patients with AMI. GIPS-175 and GIPS-II76 found no difference in 30-day mortality (4.8% vs 5.8%, and 2.9% vs 1.8%) in 940 and 889 AMI subjects, respectively, treated with PCI and GIK infusion. CREATE-ECLA77 studied GIK infusion in 20,201 patients with STEMI and found no difference in 30-day mortality rates (10.0% vs 9.7%), no difference in cardiac arrest (1.5% vs 1.4%), cardiogenic shock (6.3% vs 6.6%), or reinfarction (2.4% vs 2.3%).
Magnesium. Theoretic reasons magnesium may be beneficial in ACS include reductions in afterload, free radical formation, platelet aggregation, calcium influx related reperfusion injury, catecholamine release, protection from reperfusion "stunning" of the myocardium, and enhancement of coronary vasodilation and collateral blood flow.78
The LIMIT-2 trial79 studied an IV dose of magnesium sulfate prior to thrombolysis in 2316 patients with possible acute MI and found a 2.5% ARR (NNT=40), 24% RRR in 28-day mortality, and 4% ARR (NNT=25), 21% RRR in CAD-related mortality during long-term 4-year follow-up. More recent trials, including ISIS-417 and MAGIC80 have not shown benefit. ISIS-417 studied 58,050 patients with suspected MI and found no benefit (trend toward 6% increased mortality) from magnesium infusion of 8 mmol (2 g magnesium sulfate) bolus followed by 72 mmol (18 g magnesium sulfate) over 24 hours. However, in ISIS-4 the magnesium infusion was delayed approximately 8 hours in comparison to 3 hours in the LIMIT-2 trial,79 initiated approximately 2 hours after thrombolytic administration in as many as half of all patients, and serum magnesium levels were not elevated at the time of coronary artery reperfusion. The MAGIC trial80 used 2 g magnesium sulfate bolus over 15 minutes followed by 17 g over 24 hours prior to reperfusion in 6213 patients with STEMI and found no benefit in 30-day mortality (15.3% vs 15.2%).
Authors' Bottom Line Recommendations: Magnesium infusion may not be of benefit in ACS unless the patient has known or suspected magnesium deficiency.
Statins. Statins (inhibitors of 3-hydroxy-3-methylglutaryl co-enzyme A reductase) effectively diminish low-density lipoprotein cholesterol, but also have antioxidant, anti-inflammatory, antiplatelet, and plaque-stabilizing properties.81 Experimental evidence suggests statins improve endothelial function by inhibiting superoxide production as well as increasing nitric oxide production. Although a recent meta-analysis82 of early (within 14 days of presentation) statin (including pravastatin [Pravachol], fluvastatin [Lescol], atorvastatin [Lipitor], and simvastatin [Zocor]) use during ACS in 12 trials including 13,024 patients failed to demonstrate significant risk reduction in death, MI, and stroke at 1 and 4 months, they did confirm a 20% RRR in unstable angina at 4 months. Data from the National Registry of Myocardial Infarction 483 suggests that very early use of a statin, started within the first 24 hours of AMI presentation (N=21,978), in comparison to no statin use (N=126,128), decreased mortality by 10% ARR (NNT=10), 65% RRR. Similarly, another observational study84 of 3226 patients with AMI, comparing very early (24 hours) use of statin (N=220) to no statin use (N=3006), detected a decrease of 6.5% ARR (NNT=15), 71% RRR, in in-hospital mortality, with lower peak CK and CK-MB values, suggesting statins can limit infarct size. In a small, prospective trial85 of 72 patients with STEMI undergoing thrombolytic therapy, immediate provastatin 40 mg/day therapy decreased ventricular arrhythmias by 37% ARR (NNT=3), 57% RRR, regardless of initial cholesterol level.
Authors' Bottom Line Recommendations: Currently, clarification and consensus of the most effective time and dose of a statin in ACS is lacking. In light of this, clinicians might consider early administration in the ED of any statin to patients with ACS, regardless of baseline cholesterol, if not previously on statin therapy.
Conclusion
Therapeutic decisions for the ED patient with ACS often are complex and sometimes controversial, and may best be guided by preparing algorithms or checklists. Choosing among the numerous pharmacologic interventions is dependent on the likelihood of ACS, the ECG and biomarker findings, the anticipated time to PCI, and the potential risk for complications often determined by previous LV failure, heparin-induced thrombocytopenia (HIT), renal insufficiency, prior anticoagulation, and likelihood of left main or triple vessel disease. The following is a list of recommendations to optimize efforts as emergency physicians in caring for ACS patients, to potentially salvage myocardium, improve outcome, and minimize complications.
- Initiate early dialogue with cardiologists, especially interventionalists, regarding several of the therapies that are likely to be chosen by personal preference as much as by scientific validity, including:
- Loading dose and timing of clopidogrel prior to PCI;
- Choice of GP IIb/IIIa inhibitor;
- Upstream use of GP IIb/IIIa inhibitor prior to PCI;
- UFH vs. enoxaparin vs. bivalirudin, especially in PCI cases;
- Dose and timing of ACE inhibitors or ARBs;
- Dose and timing of statins; and
- Insulin infusion in STEMI or high-risk ACS with elevated serum glucose.
Identify the high-risk ACS patient most likely to benefit from the combination of anti-ischemic, antithrombotic, and multiple antiplatelet therapies. (See Table 3.) These include patients with ongoing rest pain, hemodynamic changes, signs of LV failure, elevated biomarkers (especially troponin), or ECG changes such as ST depressions or deep T-wave inversions. Become familiar with the TIMI risk score, and be aggressive with patients with a score greater than 4.
| Table 3. Therapy for High-Risk ACS |
| • Oxygen • Nitroglycerin if ongoing chest pain or anticipated PCI • Morphine if ongoing chest pain despite nitroglycerin • Beta-blocker (IV if tachycardia or hypertension) • Aspirin 160-325 mg, chewed • Clopidogrel loading dose (except when CABG anticipated) • GP IIb/IIIa inhibitor (consider abciximab if PCI anticipated) • UFH or enoxaparin or bivalirudin • Consider ACE inhibitor or ARB if hypertensive • Consider statin • Consider insulin infusion if glucose > 140 mg/dL |
- Avoid the "more is better" mentality.
- More aspirin along with clopidogrel increases bleeding risk.
- Be aware of dose adjustments of eptifibatide, tirofiban, enoxaparin, and bivalirudin in renal insufficiency.
- Be aware of dose adjustment of UFH with thrombolytics and GP IIb/IIIa inhibitors.
- Theoretical concerns exist for high-dose nitroglycerin, morphine, and high concentrations of supplemental oxygen worsening outcome.
- Aggressive use of beta-blockers in patients with mild LV dysfunction may worsen outcome.
- Avoid routine transfusion in mild to moderately anemic ACS patients.
There are several therapies to avoid in certain situations.
- Avoid clopidogrel loading in patients with high likelihood of urgent or emergent CABG.
- Avoid clopidogrel in the absence of elevated troponin or ECG changes.
- Avoid abciximab in ACS patients not anticipated to undergo PCI.
- Avoid GP IIb/IIIa inhibitors in the absence of elevated troponin or ECG changes.
- Avoid crossover from enoxaparin to UFH, or UFH to enoxaparin, within 12 hours of prior dosing, which can lead to excess bleeding.
- Avoid calcium channel blockers except in rare indications.
References
1. Maroko PR, Radvany P, Braunwald E, et al. Reduction of infarct size by oxygen inhalation following acute coronary occlusion. Circulation 1975;52:360-368.
2. Madias JE, Hood WB. Reduction of precordial ST-segment elevation in patients with anterior myocardial infarction by oxygen breathing. Circulation 1976;53:1198-1200.
3. Carpagnano GE, Kharitonov SA, Foschino-Barbaro MP, et al. Supplementary oxygen in healthy subjects and those with COPD increases oxidative stress and airway inflammation. Thorax 2004;59:1016-1019.
4. Crawford P, Good PA, Gutierrez E, et al. Effects of supplemental oxygen on forearm vasodilation in humans. J Appl Physiol 1997;82:1601-1606.
5. McNulty PH, King N, Scott S, et al. Effects of supplemental oxygen administration on coronary blood flow in patients undergoing cardiac catheterization. Am J Physiol Heart Circ Physiol 2005;288:1057-1062.
6. Braunwald E, Antman EM, Beasley JW, et al. ACC/AHA 2002 guideline update for the management of patients with unstable angina and non-ST-segment elevation myocardial infarction: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on the Management of Patients With Unstable Angina). 2002. Available at: http://www.acc.org/qualityandscience/clinical/guidelines/unstable/update%5Findex.htm.
7. Antman EM, Anbe DT, Armstrong PW, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). Circulation 2004;110;e82-e293.
8. Meine TJ, Roe MT, Chen AY, et al; CRUSADE Investigators. Association of intravenous morphine use and outcomes in acute coronary syndromes: Results from the CRUSADE Quality Improvement Initiative. Am Heart J 2005;149:1043-1049.
9. Chirkov YY, Holmes AS, Willoughby SR, et al. Stable angina and acute coronary syndromes are associated with nitric oxide resistance in platelets. J Am Coll Cardiol 2001;37:1851-1857.
10. Cheitlin MD, Hutter AM Jr, Brindis RG, et al. ACC/AHA expert consensus document: Use of sildenafil (Viagra) in patients with cardiovascular disease: American College of Cardiology/American Heart Association. J Am Coll Cardiol 1999;33:273-282.
11. Habbab MA, Haft JI. Heparin resistance induced by intravenous nitroglycerin: A word of caution when both drugs are used concomitantly. Arch Intern Med 1987;147:857-860.
12. Romeo F, Rosano GM, Martuscelli E, et al. Concurrent nitroglycerin administration reduces the efficacy of recombinant tissue-type plasminogen activator in patients with acute anterior wall myocardial infarction. Am Heart J 1995;130:692-697.
13. Karlberg KE, Saldeen T, Wallin R, et al. Intravenous nitroglycerin reduces ischaemia in unstable angina pectoris: A double-blind placebo-controlled study. J Intern Med 1998;243:25-31.
14. DePace NL, Herling IM, Kotler MN, et al. Intravenous nitroglycerin for rest angina. Potential pathophysiologic mechanism of action. Arch Intern Med 1982;142:1806-1809.
15. Kaplan K, Davison R, Parker M, et al. Intravenous nitroglycerin for the treatment of angina at rest unresponsive to standard nitrate therapy. Am J Cardiol 1983;51:694-698.
16. Yusuf S, Collins R, MacMahon S, Peto R. Effect of intravenous nitrates on mortality in acute myocardial infarction: An overview of the randomized trials. Lancet 1988;1:1088-1092.
17. ISIS-4 (Fourth International Study of Infarct Survival) Collaborative Group. ISIS-4: A randomized factorial trial assessing early oral captopril, oral mononitrate, and intravenous magnesium sulphate in 58,050 patients with suspected acute myocardial infarction. Lancet 1995;345:669-685.
18. GISSI-3: Gruppo Italiano per lo Studio della Sopravvivenza nell'infarto Miocardico. Effects of lisinopril and transdermal glyceryl trinitrate singly and together on 6-week mortality and ventricular function after acute myocardial infarction. Lancet 1994;343:1115-1122.
19. Jugdutt BI. Nitrates in myocardial infarction. Cardiovasc Drugs Ther 1994;8:635-646.
20. Figueras J, Lidon R, Cortadellas J. Rebound myocardial ischaemia following abrupt interruption of intravenous nitroglycerin infusion in patients with unstable angina at rest. Eur Heart J 1991;12:405-411.
21. Robertson RM, Wood AJ, Vaughn WK, et al. Exacerbation of vasotonic angina pectoris by propranolol. Circulation 1982;65:281-285.
22. Teo KK, Yusuf S, Furberg CD. Effects of prophylactic antiarrhythmic drug therapy in acute myocardial infarction: An overview of results from randomized controlled trials. JAMA 1993;270:1589-1595.
23. ISIS-1 (First International Study of Infarct Survival) Collaborative Group. Randomised trial of intravenous atenolol among 15 027 cases of suspected acute myocardial infarction: ISIS-1. Lancet 1986;2:57-66.
24. The MIAMI Trial Research Group. Metoprolol in Acute Myocardial Infarction (MIAMI): A randomized placebo-controlled international trial. Eur Heart J 1985;6:199-226.
25. Roberts R, Rogers WJ, Mueller HS, et al. Immediate versus deferred beta-blockade following thrombolytic therapy in patients with acute myocardial infarction: Results of the Thrombolysis in Myocardial Infarction (TIMI) II-B Study. Circulation 1991;83:422-437.
26. Van de Werf F, Janssens L, Brzostek T, et al. Short-term effects of early intravenous treatment with a beta-adrenergic blocking agent or a specific bradycardic agent in patients with acute myocardial infarction receiving thrombolytic therapy. J Am Coll Cardiol 1993;22:407-416.
27. Pfisterer M, Cox JL, Granger CB, et al. Atenolol use and clinical outcomes after thrombolysis for acute myocardial infarction: The GUSTO-I experience. Global Utilization of Streptokinase and TPA (alteplase) for Occluded Coronary Arteries. J Am Coll Cardiol 1998;32:634-640.
28. Chen ZM, Jiang LX, Chen YP, et al; COMMIT (ClOpidogrel and Metoprolol in Myocardial Infarction Trial) collaborative group. Addition of clopidogrel to aspirin in 45,852 patients with acute myocardial infarction: Randomized placebo-controlled trial. Lancet 2005;366:1607-1621.
29. Kernis SJ, Harjai KJ, Stone GW, et al. Does beta-blocker therapy improve clinical outcomes of acute myocardial infarction after successful primary angioplasty? J Am Coll Cardiol 2004;43:1773-1779.
30. Halkin A, Grines CL, Cox DA, et al. Impact of intravenous beta-blockade before primary angioplasty on survival in patients undergoing mechanical reperfusion therapy for acute myocardial infarction. J Am Coll Cardiol 2004;43:
1780-1787.
31. The Holland Interuniversity Nifedipine/Metoprolol Trial (HINT) Research Group. Early treatment of unstable angina in the coronary care unit: A randomized, double blind, placebo controlled comparison of recurrent ischaemia in patients treated with nifedipine or metoprolol or both. Br Heart J 1986;56:400-413.
32. Brunner M, Faber TS, Greve B, et al. Usefulness of carvedilol in unstable angina pectoris. Am J Cardiol 2000;85:1173-1178.
33. Gottlieb SO, Weisfeldt ML, Ouyang P, et al. Effect of the addition of propranolol to therapy with nifedipine for unstable angina pectoris: a randomized, double-blind, placebo-controlled trial. Circulation 1986;73:331-337.
34. Hohnloser SH, Meinertz T, Klingenheben T, et al. Usefulness of esmolol in unstable angina pectoris. European Esmolol Study Group. Am J Cardiol 1991;67:1319-1323.
35. Yusuf S, Wittes J, Friedman L. Overview of results of randomized clinical trials in heart disease, II: Unstable angina, heart failure, primary prevention with aspirin, and risk factor modification. JAMA 1988;260:2259-2263.
36. Wilcox RG, Hampton JR, Banks DC, et al. Trial of Early Nifedipine in Acute Myocardial Infarction: The TRENT study. BMJ 1986;293:1204-1208.
37. Goldbourt U, Behar S, Reicher-Reiss H, et al. Early administration of nifedipine in suspected acute myocardial infarction: The Secondary Prevention Reinfarction Israel Nifedipine Trial 2 Study. Arch Intern Med 1993;153:345-353.
38. The Danish Study Group on Verapamil in Myocardial Infarction. Verapamil in acute myocardial infarction. Eur Heart J 1984;5:516-528.
39. Teo KK, Yusuf S, Furberg CD. Effects of prophylactic antiarrhythmic drug therapy in acute myocardial infarction: An overview of results from randomized controlled trials. JAMA 1993;270:1589-1595.
40. Held PH, Yusuf S, Furberg CD. Calcium channel blockers in acute myocardial infarction and unstable angina: An overview. BMJ 1989;299:1187-1192.
41. Furberg CD, Psaty BM, Meyer JV. Nifedipine. Dose-related increase in mortality in patients with coronary heart disease. Circulation 1995;92:1326-1331.
42. Lubsen J, Tijssen JG. Efficacy of nifedipine and metoprolol in the early treatment of unstable angina in the coronary care unit: Findings from the Holland Ineruniversity Nifedipine/metoprolol Trial (HINT). Am J Cardiol 1987;60:18A-25A.
43. Boden WE, van Gilst WH, Scheldewaert RG, et al. Diltiazem in acute myocardial infarction treated with thrombolytic agents: A randomized placebo-controlled trial. Incomplete Infarction Trial of European Research Collaborators Evaluating Prognosis post-Thrombolysis (INTERCEPT). Lancet 2000;355:1751-1756.
44. Cheng JW, Ngo MN. Current perspective on the use of angiotensin-converting enzyme inhibitors in the management of coronary (atherosclerotic) artery disease. Ann Pharmacother 1997;31:1499-1506.
45. Swedberg K, Held P, Kjekshus J, et al. Effects of the early administration of enalapril on mortality in patients with acute myocardial infarction: Results of the Cooperative New Scandinavian Enalapril Survival Study II (CONSENSUS II). N Engl J Med 1992;327:678-684.
46. Latini R, Maggioni AP, Flather M, et al. ACE inhibitor use in patients with myocardial infarction: summary of evidence from clinical trials. Circulation 1995;92:3132-3137.
47. ACE Inhibitor Myocardial Infarction Collaborative Group. Indications for ACE inhibitors in the early treatment of acute myocardial infarction: Systematic overview of individual data from 100,000 patients in randomized trials. Circulation 1998;97:2202-2212.
48. Yusuf S, Sleight P, Pogue J, et al; the Heart Outcomes Prevention Evaluation Study Investigators. Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. N Engl J Med 2000;342:145-153.
49. Fox KM. Efficacy of perindopril in reduction of cardiovascular events among patients with stable coronary artery disease: Randomized, double-blind, placebo-controlled, multicentre trial (the EUROPA study). Lancet 2003;362:782-788.
50. Dickstein K, Kjekshus J, OPTIMAAL Steering Committee of the OPTIMAAL Study Group. Effects of losartan and captopril on mortality and morbidity in high-risk patients after acute myocardial infarction: The OPTIMAAL randomized trial. Optimal Trial in Myocardial Infarction with Angiotensin II Antagonist Losartan. Lancet 2002;360:752-760.
51. Pfeffer MA, McMurray JJ, Velazquez EJ, et al, Valsartan in Acute Myocardial Infarction Trial Investigators. Valsartan, captopril, or both in myocardial infarction complicated by heart failure, left ventricular dysfunction, or both. N Engl J Med 2003;349:1893-1906.
52. Alexander KP, Chen AY, Roe MT, et al. Excess dosing of antiplatelet and antithrombin agents in the treatment of non-ST-segment elevation acute coronary syndromes. JAMA 2005;294:3108-3116.
53. Santopinto JJ, Fox KAA, Goldberg RJ, et al. Creatinine clearance and adverse hospital outcomes in patients with acute coronary syndromes: Findings from the global registry of acute coronary events (GRACE). Heart 2003;89:1003-1008.
54. Klompas M. Does this patient have an acute thoracic aortic dissection? JAMA 2002;287:2262-2272.
55. Hartnell GG, Wakeley CJ, Tottle A, et al. Limitations of chest radiography in discriminating between aortic dissection and myocardial infarction: Implications for thrombolysis. J Thorac Imaging 1993;8:152-155.
56. Gaitonde RS, Sharma N, Ali-Hasan S, et al. Prediction of significant left main coronary artery stenosis by the 12-lead electrocardiogram in patients with rest angina pectoris and the withholding of clopidogrel therapy. Am J Cardiol 2003;92:846-848.
57. Yamaji H, Iwasaki K, Kusachi S, et al. Prediction of acute left main coronary artery obstruction by 12-lead electrocardiography. ST segment elevation in lead aVR with less ST segment elevation in lead V(1). J Am Coll Cardiol 2001;38:1348-1354.
58. Barrabes JA, Figueras J, Moure C, et al. Prognostic significance of ST segment depression in lateral leads I, aVL, V5 and V6 on the admission electrocardiogram in patients with a first acute myocardial infarction without ST segment elevation. J Am Coll Cardiol 2000;35:1813-1819.
59. Hebert PC, Fergusson DA. Do transfusions get to the heart of the matter? JAMA 2004;292:1610-1612.
60. Wu WC, Rathore SS, Wang Y, et al. Blood transfusion in elderly patients with acute myocardial infarction. N Engl J Med 2001;345:1230-1236.
61. Rao SV, Jollis JG, Harrington RA, et al. Relationship of blood transfusion and clinical outcomes in patients with acute coronary syndromes. JAMA 2004;292:1555-1562.
62. Capes SE, Hunt D, Malmberg K, et al. Stress hyperglycaemia and increased risk of death after myocardial infarction in patients with and without diabetes: A systematic overview. Lancet 2000;355:773-778.
63. Kosiborod M, Rathore SS, Inzucchi SE, et al. Admission glucose and mortality in elderly patients hospitalized with acute myocardial infarction: Implications for patients with and without recognized diabetes. Circulation 2005;111:3078-3086.
64. Pinto DS, Skolnick AH, Kirtane AJ, et al. U-shaped relationship of blood glucose with adverse outcomes among patients with ST-segment elevation myocardial infarction. J Am Coll Cardiol 2005;46:178-180.
65. Svensson AM, McGuire DK, Abrahamsson P, et al. Association between hyper- and hypoglycaemia and 2 year all-cause mortality risk in diabetic patients with acute coronary events. Eur Heart J 2005;26:1255-1261.
66. Malmberg K. Prospective randomised study of intensive insulin treatment on long term survival after acute myocardial infarction in patients with diabetes mellitus. DIGAMI (Diabetes Mellitus, Insulin Glucose Infusion in Acute Myocardial Infarction) Study Group. BMJ 1997;314:1512-1515.
67. Cheung NW, Wong VW, McLean M. The Hyperglycemia: Intensive Insulin Infusion In Infarction (HI-5) Study: A randomized controlled trial of insulin infusion therapy for myocardial infarction. Diabetes Care 2006;29:765-770.
68. Goldberg PA, Siegel MD, Sherwin RS, et al. Implementation of a safe and effective insulin infusion protocol in a medical intensive care unit. Diabetes Care 2004;27:461-467.
69. Bolli R, Becker L, Gross G, et al. Myocardial protection at a crossroads: the need for translation into clinical therapy. Circ Res 2004;95;125-134.
70. Kloner RA, Rezkalla SH. Cardiac protection during acute myocardial infarction: where do we stand in 2004? J Am Coll Cardiol 2004;44:276-286.
71. Wang QD, Pernow J, Sjoquist PO, et al. Pharmacological possibilities for protection against myocardial reperfusion injury. Cardiovasc Res 2002;55:25-37.
72. Khoury VK, Haluska B, Prins J, et al. Effects of glucose-insulin-potassium infusion on chronic ishaemic left ventricular dysfunction. Heart 2003;89:61-65.
73. Fath-Ordoubadi F, Beatt KJ. Glucose-insulin-potassium therapy for treatment of acute myocardial infarction: An overview of randomized placebo-controlled trials. Circulation 1997;96:1152-1156.
74. Yusuf S, Mehta SR, Diaz R, et al. Challenges in the conduct of large simple trials of important generic questions in resource-poor settings: The CREATE and ECLA trial program evaluating GIK (glucose, insulin and potassium) and low-molecular-weight heparin in acute myocardial infarction. Am Heart J 2004;148:1068-1078.
75. van der Horst IC, Zijlstra F, van't Hof AW, et al. Glucose-insulin-potassium infusion in patients treated with primary angioplasty for acute myocardial infarction: The glucose-insulin-potassium study: A randomized trial. J Am Coll Cardiol 2003;42:784-791.
76. Timmer JR, Svilaas T, Ottervanger JP, et al. Glucose-insulin-potassium infusion in patients with acute myocardial infarction without signs of heart failure: The Glucose-Insulin-Potassium Study (GIPS)-II. J Am Coll Cardiol 2006;47:1730-1731.
77. Mehta SR, Yusuf S, Diaz R, et al. Effect of glucose-insulin-potassium infusion on mortality in patients with acute ST-segment elevation myocardial infarction: the CREATE-ECLA randomized controlled trial. JAMA 2005;293:437-446.
78. Shechter M. Does magnesium have a role in the treatment of patients with coronary artery disease? Am J Cardiovasc Drugs 2003;3:231-239.
79. Woods KL, Fletcher S. Long-term outcome after intravenous magnesium sulphate in suspected acute myocardial infarction: The second Leicester Intravenous Magnesium Intervention Trial (LIMIT-2). Lancet 1994;343:816-819.
80. Magnesium in Coronaries (MAGIC) Trial Investigators. Early administration of intravenous magnesium to high-risk patients with acute myocardial infarction in the Magnesium in Coronaries (MAGIC) Trial: A randomized controlled trial. Lancet 2002;360:1190-1196.
81. Schieffer B, Drexler, H. Role of 3-hydroxy -3-methylglutaryl coenzyme A reductase inhibitors, angiotensin-converting enzyme inhibitors, cyclooxygenase-2 inhibitors, and aspirin in anti-inflammatory and immunomodulatory treatment of cardiovascular disease. Am J Cardiol 2003:91;12H-18H.
82. Briel M, Schwartz GG, Thompson PL, et al. Effects of early treatment with statins on short-term clinical outcomes in acute coronary syndromes. A meta-analysis of randomized controlled trials. JAMA 2006;295:2046-2056.
83. Fonarow GC, Wright RS, Spencer FA, et al; National Registry of Myocardial Infarction 4 Investigators. Effect of statin use within the first 24 hours of admission for acute myocardial infarction on early morbidity and mortality. Am J Cardiol 2005;96:611-616.
84. Wright RS, Bybee K, Miller WL, et al. Reduced risks of death and CHF are associated with statin therapy administered acutely within the first 24 h of AMI. Int J Cardiol 2006;108:314-319.
85. Kayikcioglu M, Can L, Evrengul H, et al. The effect of statin therapy on ventricular late potentials in acute myocardial infarction. Int J Cardiol 2003;90:63-72.
In this article, the authors discuss the "less sexy" aspects ACS mangement, those agents and treatments that have either a long history of use in ACS patients or are still too new to judge.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.