Minor Head Trauma in Pediatric Patients
Minor Head Trauma in Pediatric Patients
Authors:
Tyler Ayalin, MD, Advocate Christ Medical Center, Department of Emergency Medicine, Oak Lawn, IL
Charlene Kiang, MD, Stanford Hospital and Clinics, Department of Emergency Medicine, Stanford, CA
Laleh Gharabaghian, MD, Clinical Instructor of Surgery/Emergency Medicine; Stanford University School of Medicine, Stanford, CA
N. Ewen Wang, MD, Associate Professor of Surgery/Emergency Medicine; Associate Director, Pediatric Emergency Medicine, Stanford University School of Medicine, Stanford, CA
Peer Reviewer:
Christopher J. Haines, DO, FAAP, FACEP, Assistant Professor of Emergency Medicine and Pediatrics, Drexel University College of Medicine; Director, Department of Emergency Medicine and Medical Director, Critical Care Team, St. Christopher's Hospital for Children, Philadelphia, PA.
Pediatric head trauma is one of the most common presenting complaints to the emergency department (ED). In an earlier article on pediatric head trauma, the authors addressed the epidemiology, pathophysiology, diagnosis, and management of moderate to severe pediatric traumatic brain injury (TBI). This article will focus on pediatric minor head trauma.
Every year approximately 600,000 children are evaluated in EDs for head injuries.1 Children between the ages of 0-4 years and 15-19 years are most likely of any age to sustain head injuries.2 Although the overall numbers of head injuries are high, the majority of cases fall into the category of minor head injury. Computed tomography (CT) scans are the modality of choice for diagnosing pathology of the brain. However, for children with head trauma, fewer than 10 percent of CT scans performed show traumatic brain injuries and even fewer identify injuries that require neurosurgical intervention.3,4
CT scans are widely used diagnostic tests and generally are considered safe, but their use does increase the risk of malignant transformation.5 The lifetime risk of developing cancer in the pediatric age group secondary to CT radiation is estimated to be 1 in 1,000 to 1 in 5,000 CT scans performed.5,6 The radiation exposure risk becomes more apparent when applied to the large population of children presenting to the ED with head injuries. Assuming a scan rate of approximately 20 percent for head injuries and 600,000 visits per year for head trauma, 24 to 120 children per year would develop radiation-induced brain malignancies in their lifetime.
The goal of the emergency physician (EP) is to detect the cases when significant brain injury results from apparently minor head trauma. Several evidence-based decision rules have been proposed, thus providing EPs with tools to decrease the risk of undetected occult intracranial injury while also limiting the number of CT scans performed. This article will review ED identification of minor head injury, the initial assessment, the tools (decision rules) created to identify patients who should be imaged, and the management of pediatric minor head injuries and concussions.
Ann Dietrich, MD, FAAP, FACEP
Definitions
Minor head injury/trauma is defined as head trauma that results in a normal Glasgow Coma Score (GCS) and no neurologic sequelae at the time of assessment. The American Academy of Pediatrics defines minor head injury as "those [patients] who have normal mental status at the time of initial examination, who have no abnormal or focal findings on neurologic examination, and who have no physical evidence of skull fracture."7
Traumatic brain injury (TBI) is a term that signifies any degree of brain injury, typically associated with a neurologic or cognitive impairment. This spectrum of injury may include mild concussion through severe intracranial injury. A percentage of children with minor head trauma will have occult TBI.
Concussion is a subset of mild traumatic brain injury. Although there is some degree of overlap, the difference lies in that there is a mild degree of cognitive sequelae associated with a concussion (for example, loss of consciousness, amnesia, or confusion). The American Academy of Neurology defines concussion as a "trauma-induced alteration in mental status that may or may not be associated with loss of consciousness." Concussions are common, with an estimated 1.6 to 3.8 million concussions each year occurring in the United States.8
Evaluation of Minor Head Injury: Contribution of Age, History, and Physical Exam
Prior to gathering the history, an initial assessment of the child should include a determination of the patient's GCS (See Table 1). This will help create a reference point from which to guide subsequent management. The strict definition of minor head injury includes only patients with a GCS of 15.
Table 1. Glasgow Coma Scale (Maximum Score of 15)
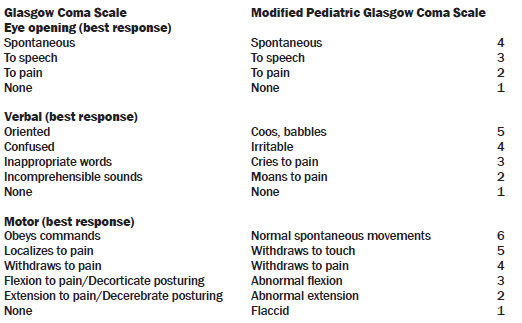
Age. Most of the literature has separated children into two groups: those older than two years and those younger than two years. Language and communication are limited in children younger than two years of age, making assessment more difficult. In addition, children in this age group have limited ability to cooperate with the physical examination, and occult brain injury is more difficult to diagnose.9 Child abuse also is more prevalent in this young age group.10 Physiologically, children in this age group are more likely to sustain skull fractures from minor mechanisms of injury.10 In general, the threshold for imaging should be higher in the younger child.
History. The history in pediatric head trauma should focus on three key areas: the mechanism of injury, behavioral symptoms, and neurologic symptoms. EPs should obtain a detailed history of the events of the injury, including the time course since the injury and all associated symptoms.
The mechanism of head injury is a key feature to obtain in the history. Certain mechanisms of injury are more common for particular age groups. Children ages 0-4 are more likely to sustain traumatic brain injuries from falls. Thus, in the neonatal and infant age group, it is important to ask about the height of the fall and the circumstances in which it occurred. Children who fall distances greater than 3 feet have been shown to be more at risk for significant brain injury.3,11 Toddlers can fall from ground level or run into stationary objects; these mechanisms typically will have a relatively minor force of impact.
Children ages 5-14 typically develop brain injuries from being struck by objects or from an assault. Sports-related injuries frequently occur in this age group. It is important to know the circumstances, the type of object, and the force applied. High-speed or heavy objects are more concerning for significant brain injuries.11,12
For teenagers ages 15-18 years, motor vehicle collisions become a more prevalent cause of traumatic brain injury. These patients should be asked about the speed of the vehicles, airbag deployment, the restraint device used (air bag, seat belt), and the injuries to other passengers involved. High-speed motor vehicle collisions (greater than 35 mph), rollover accidents, collisions involving cyclists or pedestrians, death of another passenger, and passenger ejection all have been shown to increase risk for significant brain injury.3,11
Behavioral symptoms are an important indicator of the severity of head injury in the pediatric population. Although clinicians should raise their suspicion of brain injury if any history of abnormal behavior or altered level of consciousness is present, these symptoms are not specific. In other words, more children will manifest these symptoms than those who actually have a significant traumatic brain injury. Studies have validated that a parent's perception of abnormal behavior alone is a significant risk factor for TBI.3 Abnormal behavioral symptoms include: increased or decreased activity level compared to baseline, somnolence, agitation, poor concentration, slowing of speech, increased irritability, and repetitive questioning.
Finally, the history should include a thorough assessment of the patient's neurologic function. Loss of consciousness is a risk factor for significant brain injury, but longer periods do not directly correlate with severity of injury.3 Visual changes, focal or generalized sensory changes, and muscle weakness should be assessed. Clinicians also should ask about symptoms of dizziness, vertigo, imbalance, coordination difficulties, and gait disturbances. Symptoms suggestive of increased intracranial pressure should be elucidated (i.e., severe headache, lethargy, nausea, and vomiting). Persistent, repeated vomiting is more concerning for significant brain injury than an isolated episode of vomiting, which is not uncommon after minor head trauma. The same is true for a worsening headache and any history of amnesia.4,11 A seizure at any point after the head trauma can occur in minor and severe head injury.11
Physical Examination. Vital signs will be normal in patients with isolated minor head trauma. The neurologic exam should be thorough and, by definition, completely normal in cases of true minor head injury. Any neurologic deficit should prompt further workup. Pupils should be symmetric and reactive. Patients should not have signs of lateralizing or focal weakness. Children not old enough to follow commands to test strength should be observed for equal spontaneous movement of their extremities. Sensation should be normal. Cerebellar testing should be performed. Children old enough to walk should be gait tested. The cranial nerves should all be intact.
The scalp of the minor head injury patient often has no findings, but should be evaluated for signs of more significant injury. Skull fractures increase a patient's risk of having TBI.10,13 Bony crepitus or step-offs should be identified and further evaluated diagnostically. Classically described exam findings of a basilar skull fracture should not be present: otorrhea/rhinorrhea, periorbital ecchymoses (raccoon eyes), posterior auricular hematoma (Battle's sign), and hemotympanum (See Figures 1 and 2).
Figure 1. Periorbital Ecchymoses (Raccoon Eyes)
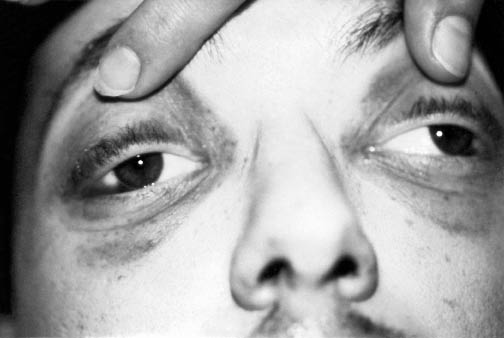
Figure 2. Posterior Auricular Hematoma (Battle's Sign)
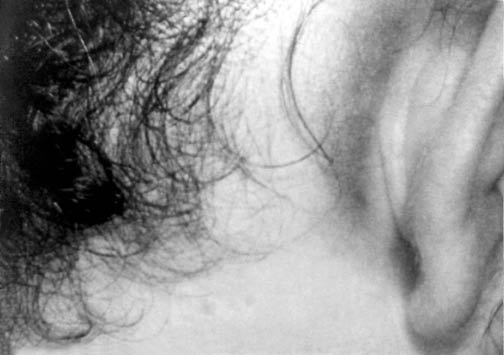
One of the more apparent clinical exam findings in children with minor head trauma will be the presence of a scalp hematoma. The size and location of the hematoma are important for prognosis. Large, boggy hematomas have been shown to increase the likelihood of a significant brain injury, but "large" is not well defined.11 In general, children with temporal and parietal hematomas have a higher risk for brain injury than children with frontal and occipital hematomas.3 Any hematoma present in a child younger than age 2 should raise suspicion of an intracranial injury. The fontanelles of young children should be examined and documented; flat fontanelles do not exclude a significant injury, but bulging fontanelles are very concerning.
Workup: To Image or Not to Image
ED management of patients with minor head injury focuses on diagnostic workup/imaging, pain management, ED observation, patient disposition, and parent/provider education. After the initial assessment, the EP must synthesize the history and physical findings and decide if the potential risk of TBI is sufficient to warrant CT imaging. History and physical exam, while crucial, are non-specific. Validated tools to help the physician assess population-based risk are imperative to the appropriate management of minor head injury. The physician should then incorporate the pros and cons of radiation vs. the risk of a significant TBI in a discussion with the parents regarding the decision to image.
Clinical Decision Rules
Within the last few years, several large-scale studies have focused on deriving head injury "decision rules" to aid physicians in identifying children at risk for serious intracranial pathology or the converse, children unlikely to have significant injury. Palchak et al demonstrated that a decision rule was slightly better than clinician judgment at identifying traumatic brain injuries ultimately diagnosed by CT scan.14
This article will review some of the major pediatric studies and their overall application to practice. They are designed to help the clinician decide on the major management questions in pediatric minor head injury regarding risk stratification and imaging.
CHALICE. Dunning et al published Children's Head injury Algorithm for the prediction of Important Clinical Events (CHALICE) in 2006.12 This prospective cohort study conducted from 2000-2002 at 10 hospitals in England enrolled 22,772 patients aged 16 years and under. The aim of the study was to derive a highly sensitive decision rule for determining which head injury patients are at high risk for significant intracranial injury. This study included all head injuries, not only mild, with the argument that this population more accurately reflected a general head injury population. The study group identified a total of 14 high-risk clinical variables (see Table 2) from the history and physical exam associated with clinically significant intracranial injury. Clinically significant injury was defined as: death, neurosurgical intervention, and any acute traumatic intracranial pathology by CT scan except for non-depressed skull fractures. According to this rule, children with any of the high-risk criteria should undergo CT scan, while children with none of the criteria are considered low risk. The decision rule had an overall sensitivity of 98% (confidence interval [CI] 96-100%) and specificity of 87% (CI 86-87%).
Table 2. CHALICE High-Risk Variables
History
- Loss of consciousness > 5 minutes
- History of amnesia > 5 minutes
- Abnormal drowsiness as determined by the physician
- > 3 episodes of vomiting
- Suspicion of non-accidental trauma
- Seizure after head injury in a patient without history of epilepsy
Physical Exam
- GCS < 14, or GCS < 15 if < 1 year old
- Suspicion of depressed skull fracture or tense fontanelle
- Signs of basilar skull fracture (blood or CSF from ear or nose, panda eyes, Battle's sign, hemotympanum, facial crepitus)
- Focal neurologic findings
- Bruise, swelling, or laceration > 5 cm if < 1 year old
Mechanism
- Road traffic accident > 40 mph
- Fall > 3 meters in height
- High-speed injury from a projectile or object
Adapted from: Dunning J, Daly JP, Lomas JP, et al. Derivation of the children's head injury algorithm for the prediction of important clinical events decision rule for head injury in children. Arch Dis Child 2006;91:885-891.
As a decision rule, CHALICE was designed to be highly sensitive. This study has not been prospectively validated, and a recent retrospective study from Australia showed that the number of CT scans performed would double if the CHALICE rule were applied.15
The CHALICE study was designed to identify important clinical risk factors for significant TBI. In practice, it is difficult to use because the 14 high-risk variables are unwieldy. The high sensitivity of the rule was obtained at the cost of potentially increasing the rate of CT imaging instead of providing a tool to focus imaging decisions.
PECARN. Kupperman et al published a large prospective cohort study, which both derived and validated a pediatric head injury decision rule for determining patients at very low risk for intracranial injury.3 Patients were enrolled from 2004-2006 at 25 U.S. EDs participating in a Pediatric Emergency Care Research Network (PECARN) study. A total of 42,412 patients were included for both the derivation and validation group. Patients with GCS less than 14 and patients with trivial mechanisms were excluded. Importantly, there were 10,718 children under age two analyzed separately. The primary outcome measure was "clinically important traumatic brain injury" defined as: need for neurosurgery, intubation for more than 24 hours, or hospital admission for two nights. Study follow-up extended to 90 days post-discharge.
For children older than two years, six high-risk predictors (see Figure 3) were identified. The two most significant risk factors for clinically important TBI included altered mental status and clinical signs of basilar skull fracture. Negative predictive value for the group of children older than two was 99.95% (CI 99.81-99.99%), and the sensitivity was 96.8% (CI 89-99.6%). For children younger than two years of age, six different high-risk predictors (see Figure 4) were identified. The two most significant predictors of clinically important TBI were altered mental status and palpable or suspected skull fracture. Negative predictive value was 100% (CI 99.7-100) for the younger than two age group and sensitivity was 100% (CI 86.3-100).
Figure 3. PECARN High-Risk Variables for Age ≥ 2
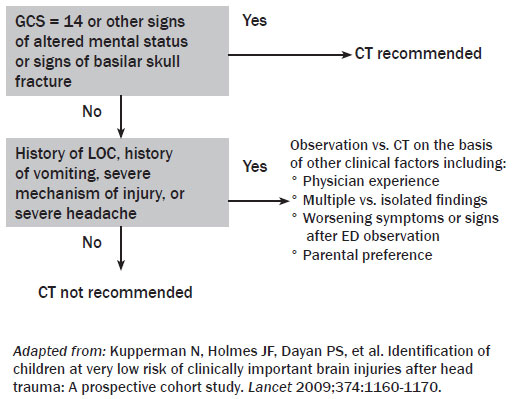
Figure 4. PECARN High-Risk Variables for Age < 2
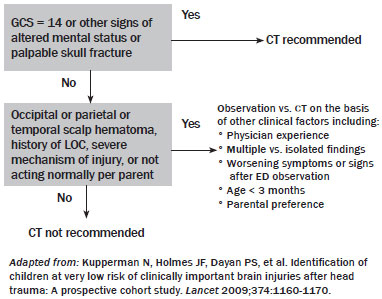
Children with none of the six high-risk variables were considered very low risk for TBI, and CT was not recommended. Children with none of the two highest risk criteria, but any of the other four high-risk criteria, were still considered low risk with a 0.9% risk of a significant brain injury. The authors recommended a consideration of observation vs. CT depending on: parental preference, young age (less than three months), worsening symptoms during ED observation, and physician impression.
The PECARN study is a large, well-designed study that is fully applicable to clinical practice. Although this validated tool helps the clinician identify patients at very low risk for clinically important TBI and very high risk patients, there is still a "gray zone." These patients are considered at a low risk of TBI (0.9%), and the rule defers to physician discretion. To date, it is also the largest study of patients younger than two years old. In addition to the high sensitivity of this decision rule, it is estimated that 20%-25% of CT scans could be avoided utilizing this rule, in contrast to the CHALICE study.
CATCH. In 2010, Osmond et al published a Clinical Decision Rule for the use of Computed Tomography in Children with Minor Head Injury (CATCH).11 This was a derivation, prospective cohort study performed at 10 hospitals in Canada. They enrolled a total of 3,866 patients aged 16 years and under. Study patients included children who had experienced an acute blunt head trauma within 24 hours, and a GCS score of 13-15. Blunt head trauma was defined as head injury with witnessed loss of consciousness, definite amnesia, witnessed disorientation, or two episodes of vomiting 15 minutes apart. Children with less symptomatic injuries and those with signs or symptoms of obvious severe injuries were excluded. The primary outcome measure was need for "neurosurgical intervention" (craniotomy, skull fracture elevation, intracranial pressure monitoring, and intubation) within seven days of injury. The secondary outcome measure was "brain injury" by CT, defined as any acute intracranial finding attributable to the trauma, excluding non-depressed skull fractures.
This study identified four high-risk factors for intervention (see Table 3). The sensitivity of the high-risk factors was 100% (CI 86.2-100%) and the specificity was 70.2% (CI 68.8-71.6%). They also identified three medium-risk factors, which put the patient at higher risk of having a brain injury by CT scan. The sensitivity of these medium risk factors for brain injury by CT was found to be 98.1% (CI 94.6-99.4%). The authors of the study acknowledge that they had relatively few children enrolled under the age of two (n = 277) and that the study needed to be prospectively validated.
Table 3. CATCH High-Risk and Medium-Risk Variables
High-Risk Variables
- GCS < 15 at two hours post injury
- Suspected open/depressed skull fracture
- History of worsening headache
- Irritability on examination
Medium-Risk Variables
- Clinical signs of basilar skull fracture
- Large, boggy scalp hematoma
- Dangerous mechanism of injury
° Motor vehicle crash
° Fall > 3 feet or 5 stairs
° Fall from bicycle without helmet
Adapted from: Osmond MH, Klassen TP, Wells GA, et al. CATCH: A clinical decision rule for the use of computed tomography in children with minor head injury. CMAJ 2010;182:341-348.
The CATCH trial prospectively derived a rule that was designed to be highly sensitive. It is relatively simple, containing four high-risk variables and three medium-risk variables. The rule was derived for children of all ages. The authors make no comment on how the clinician should use this information to guide imaging.
NEXUS II. The National Emergency X-Ray Utilization Study (NEXUS II) (1999-2000) was a multicenter, prospective, observational study that derived a highly sensitive decision instrument for determining which patients were at high risk for what they defined as a clinically significant intracranial injury (ICI).16 Eight clinical variables were derived from the original cohort of 13,728 patients, which had an overall sensitivity of 98.3%. Participating centers utilized a 19-variable decision instrument for assessing patients, and only patients who underwent CT scan were enrolled. The criteria for ICI was defined a priori and ultimately was determined by the final radiologist interpretation of the CT scan. A total of 1,666 patients 0-17 years old were analyzed. A total of 309 of the patients were younger than age 3 and were analyzed separately. A total of 138 patients (8.3%) were determined to have an ICI from this study. The authors applied the derived NEXUS decision instrument for all patients to the pediatric cohort to determine its sensitivity and specificity (leaving out the original criteria of "age greater than 65") as listed in Table 4. When applied to the entire pediatric cohort, the decision instrument had a overall sensitivity of 98.6% and identified 136 of the 138 ICIs. One of the missed cases included a likely missed scalp hematoma on original assessment. The other case that was missed did not have any of the seven criteria. Neither of the two cases required neurosurgical intervention. When applied specifically to children under age 3, the NEXUS II rule had a sensitivity of 100%.
Table 4. NEXUS II High-Risk Variables
- Evidence of significant skull fracture
- Altered level of alertness
- Neurologic deficit
- Persistent vomiting
- Presence of scalp hematoma
- Abnormal behavior
- Coagulopathy
Adapted from: Oman JA, Cooper RJ, Holmes JF, et al. Performance of a decision rule to predict need for computed tomography for children with blunt head trauma. Pediatrics 2006;117:238-246..
The original NEXUS study was the largest head injury decision rule at the time, and it was an extremely sensitive rule for dividing patients into high- and low-risk groups. This decision instrument is sensitive to detect ICI in children in general, as well as those less than three years of age. The limitation to the NEXUS II rule was that it was not independently derived for only the pediatric population. Also, the NEXUS II rule has not been prospectively validated.16
All of these decision rules are guidelines and are not a substitute for individual physician judgment. In terms of the rule that is the most applicable to practice, the PECARN algorithm is well supported and easy to apply. It stratifies patients into very low-, low-, and high-risk groups. It is also applicable to infants and children under two years of age. Although the other studies identify important clinical features to consider when evaluating a child with mild head injury, they are less helpful in supporting the decision not to image. This article discusses the approach to the minor head injured patients, and some of these studies include patients who do not fall within that definition.
Analgesia
As in any child with a painful traumatic injury, pain should be treated in the ED. Intravenous opiate analgesics are preferred for moderate-severe pain. A study in 2008 demonstrated that NSAID use in adults did not significantly increase the risk of hemorrhagic stroke compared to controls.17 However, no such studies are present in the pediatric literature; thus, in the immediate acute period of 24-48 hours, NSAIDs should be avoided unless hemorrhage has been excluded. The use of oral acetaminophen is regarded as a safe, appropriate outpatient medication for the treatment of pain related to head trauma.
Non-Accidental Head Trauma
Non-accidental causes of trauma must be considered by every clinician when treating any child with a head injury. This is important because 50% of children will suffer from additional abuse, and as many as 10% may die from subsequent abuse.18 It is not a rare occurrence, as 1.3% to 15% of children presenting to the ED with injuries may be victims of abuse.19 Head injury is the number one cause of death from child abuse.20
Physicians should be attuned to historical factors suggestive of abuse. Examples include delayed presentation to care, changing history from the parent, or history incompatible with the child's age and injury. The strongest historical predictor of abuse is if the parent is not able to provide any cause for the injury.21 Other risk factors for non-accidental trauma include previous history of child abuse, a single mother household, low infant birth weight, maternal smoking, and more than two other siblings in the family.22
In addition to a suspicious history, physical exam findings suggestive of abuse include abnormal bruise patterns ("grab marks," bite marks, linear strap marks, multiple stages of healing).23,24
Clinicians must maintain vigilance and consideration that non-accidental trauma may be the cause of pediatric head injury.
Disposition
The disposition of a child with minor head trauma depends on several factors: age of the patient, access to care, and the parents' comfort level. The options include: admission, observation, and discharge home with comprehensive parental instructions.
ED Observation
Patients with a very low suspicion for intracranial injury may be observed for a short period of time after the injury. If the child has clinically improved (more alert, oriented, headache resolution, tolerating oral intake), then observation may be continued at home. In general, for low-risk, asymptomatic patients, a period of caregiver and ED observation of four to six hours post injury is reasonable and supported in consensus guidelines.10
Admission
If a patient has ongoing symptoms during the course of the ED stay, he or she should be imaged. While there may be times when a CT is not performed initially because of parental preference, if the child does not look well, or has high-risk features that the physician is concerned about, then it is reasonable to recommend imaging.
There will be a certain percentage of patients with negative CT scans who continue to be symptomatic. They may become irritable, have pain control issues, or continued vomiting. For these patients, it is reasonable to observe them in the hospital to ensure that their symptoms improve. If they do not improve, additional care and work-up may be warranted. Parents should be informed that the likelihood of a delayed intracranial bleed is exceedingly low, especially with a negative CT scan.10 Children with suspicion for non-accidental trauma also warrant admission for observation and involvement of social services. Furthermore, inpatient observation is also acceptable if parents and caregivers of the child seem unreliable or unable to return to the ED or follow-up.
Isolated linear and non-depressed skull fractures do not necessitate a neurosurgical consult. These children are at low risk of clinical deterioration and may be considered for discharge.25,26 If an intracranial injury is diagnosed, neurosurgical consultation should be obtained. Though the vast majority of traumatic brain injuries are non-surgical, the neurosurgeon is ultimately responsible for intervening should that patient deteriorate and require operative repair. Children with depressed skull fractures or intracranial injury by CT are usually admitted. Whether the child is admitted to the intensive care unit or regular inpatient bed depends on the patient's clinical status, the severity of injuries, and neurosurgeon preference.
The period of time for inpatient observation after head injury has not been established. The AAP practice guidelines recommend at least 24 hours of observation as this is the timeframe in which the majority of complications will present themselves.1
Discharge
If a child has had a negative head CT and is well-appearing, the likelihood of a significant brain injury and delayed sequelae is extremely low.10 Physicians can inform parents that the incidence of delayed bleeding is close to zero.10 These children are safe to discharge home. However, even if a child has undergone a CT scan, parental observation of the child and return precautions for concerning signs of intracranial injury (altered mental status, severe headache, dizziness, lethargy, and persistent vomiting) must be given. Parents should be instructed to follow up with their primary physicians in 24 hours.
If a child has not undergone a diagnostic CT scan and is at low risk of serious intracranial pathology, he or she also may be discharged for continued observation at home. For most mild head injuries, the practice of waking the child is not necessary. If a well-appearing child initially presented with persistent symptoms or a more severe mechanism of injury, then caregivers can be instructed to wake the child every four hours of sleep for the next 24 hours.27 Close follow-up should be arranged within 24 hours. A thorough discussion with parents should detail strict return precautions as outlined above and instructions for when to return to the emergency department for evaluation.
Return to Play
Parents of school-age children and teenagers frequently will have questions regarding "return to play" instructions. For patients with concussions, there are specific guidelines.28 Patients should never return to contact sports or rough play prior to the resolution of symptoms, as repeat injuries can be increasingly harmful.
Several cases reports and studies describe the phenomenon known as "Second Impact" syndrome. This syndrome initially was described in an adolescent football player who sustained two head injuries with subsequent death after the second. The first head injury was a concussion, with the patient presenting with headache, nausea, and loss of consciousness. The subsequent minor head injury 4 days later was thought to have resulted in the vascular engorgement and increased intracranial pressure that led to his death.29 The autopsy report was significant for anoxic changes and transtentorial cerebral herniation attributed to impaired autoregulation of cerebral blood flow.
The 3rd international conference on concussion in sports was held in Zurich in 2008. The Zurich consensus statement no longer recommends generalized guidelines regarding "return to play." Previously, the guidelines recommended a certain number of weeks off based on the number and grade of the concussions. Currently, the Zurich recommendations include a step-wise return to activity, which can be found in Table 5.28 Other published recommendations such as those from the Ohio State University involve individualizing a patient's "return to play" based on tests that evaluate dexterity, speed, and mental status compared to baseline.30 If symptoms persist, there are additional neuropsychological tests available for evaluation.
Table 5. Stepwise Return to Play Recommendations
- No activity; complete physical and cognitive rest
- Light aerobic exercise (walking, stationary cycling, keeping intensity < 70% maximal predicted heart rate, and no resistance training)
- Sport-specific exercise
- Non-contact training drills
- Full-contact practice following medical clearance
- Return to unrestricted sport participation
Adapted from: McCrory P, Meeuwisse W, Johnston K, et al. Consensus statement on concussion in sportthe 3rd International Conference on concussion in sport. J Clin Neurosci 2009;16:755-763.
Close follow-up is essential for pediatric head injuries, as repeated injuries can result in a long-term decrease in cognitive functioning. Ultimately, pediatric patients with minor head injuries should not return to play prior to follow-up with their primary physician. Depending on the comfort level of the primary care provider, other consultants such as neurology, sports medicine, or neurosurgery may be involved in clearing a child for return to play. The ED physician should be familiar with these practices and provide recommendation prior to discharge in an effort to prevent premature return to play.
Conclusion
A child presenting with a traumatic head injury will be seen often in the emergency department and acute care setting. The vast majority of these injuries will be minor head injuries. Research from recent years has increased the physician's ability to manage these children according to evidence-based studies. However, these guidelines should always be used in conjunction with physician assessment of history, physical exam, social situation, and quality of follow-up. The management of children with minor head injury is not solely a matter of deciding between obtaining a CT scan or not; it also involves an open discussion with the caregivers, education, and investigation of the overall safety of the child. Practicing all of these aspects in unison will significantly improve the overall health and wellness of pediatric patients with head injury.
References
1. National Center for Injury Prevention and Control. Traumatic Brain injury in the United States: Assessing outcomes in children. CDC, 2006.
2. Faul M, Xu L, Wald MM, Coronado VG. Traumatic brain injury in the United States: Emergency department visits, hospitalizations, and deaths. Atlanta (GA): Centers for Disease Control and Prevention, National Center for Injury Prevention and Control; 2010.
3. Kupperman N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: A prospective cohort study. Lancet 2009;374:1160-1170.
4. Palchak MJ, Holmes JF, Vance CW, et al. A decision rule for identifying children at low risk for brain injuries after blunt head trauma. Ann Emerg Med 2003;42:494-506.
5. Brenner DJ. Estimating cancer risks from pediatric CT: Going from the qualitative to the quantitative. Pediatr Radiol 2002;32:228-331.
6. Brenner DK. Hall EJ. Computed tomographyAn increasing source of radiation exposure. N Engl J Med 2007;357:2277-2284.
7. Clinical Practice guidelines: The management of minor closed head injury in children. Pediatrics 1999;104:1407-1415.
8. Langlois JA, Rutland-Brown W, Wald MM. The epidemiology and impact of traumatic brain injury: A brief overview. J Head Trauma Rehabil 2006;21:375-378.
9. Greenes D, Schutzman S. Occult intracranial injury in infants. Ann Emerg Med 1998;32:680-686.
10. Schutzman SA, Barnes P, Duhaime AC, et al. Evaluation and management of children younger than two years old with apparently minor head trauma: proposed guidelines. Pediatrics 2001;107:983-993.
11. Osmond MH, Klassen TP, Wells GA, et al. CATCH: A clinical decision rule for the use of computed tomography in children with minor head injury. CMAJ 2010;182:341-348.
12. Dunning J, Daly JP, Lomas JP, et al. Derivation of the children's head injury algorithm for the prediction of important clinical events decision rule for head injury in children. Arch Dis Child 2006; 91:885-891.
13. Erlichman DB, Blumfield E, Rajpathak S, Weiss A. Association of linear skull fractures and intracranial hemorrhage in children with minor head trauma. Pediatr Radiol 2010;40:1375-1379.
14. Palchak MJ, Holmes JF, Kupperman N. Clinician judgement versus a decision rule for identifying children at risk of traumatic brain injury on computed tomography after blunt head trauma. Pediatr Emerg Care 2009;25:61-65.
15. Crowe L, Anderson V, Babl FE. Application of the Chalice clinical prediction rule for intracranial injury in children outside of the UK. Arch Dis Child 2010.
16. Oman, JA, Cooper RJ, Holmes JF, et al. Performance of a Decision Rule to Predict Need for Computed Tomography for Children with Blunt Head Trauma. Pediatrics 2006;117:238-246.
17. Choi NK, Park BJ, Jeong SW, et al. Nonaspirin nonsteroidal anti-inflammatory drugs and hemorrhagic stroke risk: The Acute Brain Bleeding Analysis Study. Stroke 2008;39:845-849.
18. Saade, DN, Simon, HK, Greenwald, M. Abused children. Missed opportunities for recognition in the ED. Acad Emerg Med 2002;9:524.
19. Pless IB, Sibald AD, Smith MA, Russell MD. A reappraisal of the frequency of child abuse seen in pediatric emergency rooms. Child Abuse Negl. 1987;11:193-200.
20. Alexander RC, Levitt CJ, Smith W. Abusive head trauma. In: Reece RM, Ludwig S. Child Abuse: Medical Management and Diagnosis. 2nd ed. Philadelphia, PA: Lippicott, Williams Wilkins; 2001: 47-80.
21. Hettler, J, Greenes DS. Can the initial history predict whether a child with head injury has been abused? Pediatrics 2003; 111: 3.
22. Wu, SS, Ma CX, Carter RL, et al. Risk factors for infant maltreatment: A population-based study. Child Abuse Negl 2004; 28: 1253-1264.
23. Kellogg, ND. Evaluation of suspected child physical abuse. Pediatrics 2007; 119; 1232-1241.
24. Wagner, GN. Bitemark identification in child abuse cases. Pediatric Dent 1986; 8:96-100.
25. Greenes DS, Schutzman SA. Infants with isolated skull fracture: What are their clinical characteristics and do they require hospitalization? Ann Emerg Med 1997; 30: 253-259
26. Kadish HA, Schunk JE. Pediatric basilar skull fracture: do children with normal neurologic findings and no intracranial injury require hospitalization? Ann Emerg Med 1995; 26: 37-41.
27. Schutzman SA. Minor head injury in infants and children. Uptodate.com 2010. Accessed July 22. 2010.
28. McCrory P, Meeuwisse W, Johnston K, et al. Consensus statement on concussion in sportthe 3rd International Conference on concussion in sport. J Clin Neurosci 2009;16:755-763.
29. Saunders RL, Harbaugh RE. The second impact in catastrophic contact-sports head trauma. JAMA 1984;252: 538-539.
30. Hunt T, Asplund C. Concussion assessment and management. Clin Sports Med 2010;29:5-17.
Pediatric head trauma is one of the most common presenting complaints to the emergency department (ED).Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
