Facial Trauma: Challenges, Controversies, and Therapeutic Options
Facial Trauma: Challenges, Controversies, and Therapeutic Options
Authors:
Alisa Gibson, MD, DMD, Visiting Instructor, Department of Emergency Medicine, University of Maryland, Baltimore, MD
Kimberly Boswell, MD, Resident III, Department of Emergency Medicine, University of Maryland, Baltimore, MD
Peer Reviewer:
Howard A. Werman, MD, Medical Director, MedFlight; and Professor of Clinical Emergency Medicine, The Ohio State University, Columbus, OH
Our faces play a role in almost every part of our lives. The structure and components of the face are involved in our ability to eat, speak, and see, and often are the features first noticed when we meet someone. Trauma involving the face is fairly common: More than 3 million facial injuries occur in the United States each year. More than 50 percent of patients with maxillofacial injuries have multisystem trauma, requiring coordination between emergency physicians and surgical specialists.1 Young men between the ages of 20 and 30 years are the individuals who most commonly sustain facial trauma, and the primary cause is assault.2 Alcohol is frequently involved.3 Other common causes of facial trauma include motor vehicle collisions (MVC), sports injuries, penetrating trauma, and falls. The ability to manage these injuries efficiently and expertly is crucial for the emergency physician.
Ann Dietrich, MD, FAAP, FACEP, Editor
Initial Assessment and Examination
The initial assessment of the patient with facial trauma is identical to that of any trauma patient. Airway patency is paramount, and intervention may be required. Concomitant intracranial injury, significant facial bleeding, bilateral mandibular fractures, or massive trauma to the lower two-thirds of the face (such as that caused by a gunshot wound) all may necessitate intubation. If there is any concern regarding airway protection, particularly in patients who will be immobilized for other injuries, patients should have a definitive airway placed. With the airway secured, a thorough evaluation of facial injuries typically can be delayed until other major injuries have been assessed and stabilized.
Patients with facial trauma should be placed in a cervical collar and presumed to have a cervical injury until proven otherwise. The reported incidence of cervical spine fractures among patient with facial trauma varies widely, from as low as 0.3% to as high as 24%.4,5 Not surprisingly, higher percentages of cervical spine injuries are found in patients with multiple facial fractures as well as among those whose injuries result from MVCs.
General Facial Injury Assessment
The presence of any facial trauma should prompt a complete systematic examination for other facial injuries. Assess lacerations and wounds for active bleeding, depth of penetration, foreign bodies, and transection of nerves or ducts. Carefully evaluate areas of ecchymosis and hematomas. Periorbital edema and ecchymosis may indicate underlying orbital rim or zygomaticomaxillary complex (ZMC) fracture. Battle's sign, or bruising behind the ear, should raise concern for a basilar skull fracture. Hematomas in the maxillary buccal vestibule often are seen in patients with ZMC fracture, while ecchymosis on the floor of the mouth suggests an anterior mandibular fracture. The neurologic examination should include evaluation of all cranial nerves, paying special attention to the trigeminal and facial nerves, as these may be damaged by lacerations or fractures. Any trauma to or around the eye mandates a complete ophthalmologic assessment, including visual acuity, extraocular motion, and a slit lamp examination. Palpate all bony areas for step-off deformities. Assess midface stability by placing one hand on the forehead and then grasping the anterior maxilla with the other hand. Look for trismus, as well as any objective or subjective malocclusion. The intraoral examination should include a careful search for lacerations and loose, fractured, or missing teeth.6,7
Midfacial Fractures
Midfacial fractures involve the zygoma, maxilla, and nasoorbital ethmoid complex. Although fractures of isolated bones do occur, it is more common to see fracture patterns involving more than one bone. Midface fractures often occur in conjunction with other injuries, as was the case in 54.8% of soldiers in one series.8 Other facial bone fractures, facial lacerations, limb fractures, skull fractures, and intracranial injuries usually are present depending on the mechanism of injury. Diagnosis typically is confirmed by computed tomography (CT) scan. General management in the emergency department (ED) consists of making the diagnosis, controlling bleeding, and initiating referral to a surgeon.
ZMC fractures, also known as trimalar or tripod fractures, involve the zygoma, lateral orbit, and maxilla. Fractures of the zygomatic arch may occur in isolation, typically caused by a direct blow. Their management is the same as mid-facial fractures, so they are discussed together. Because of the amount of facial swelling, these fractures are easy to miss. If left untreated, they may lead to a cosmetic deformity. They also can cause difficulty with mouth opening as a result of impingement of fracture segments on the coronoid process of the mandible. Therefore, a low threshold for CT scan is critical. On examination, these patients often have periorbital edema and ecchymosis as well as subconjunctival hemorrhage. Palpate for step-off deformities and compare the zygomatic arches for symmetry (best done by looking from behind the patient's head). Assess for range of mouth opening (normal is > 30 mm). On intraoral examination, a hematoma may be found in the buccal vestibule. Careful documentation of paresthesias is crucialinjury to the maxillary branch of the trigeminal nerve is present in 70%–90% of patients with this fracture9 and may be permanent. Surgery frequently is required but often is delayed 7–10 days to allow time for the swelling to decrease.
LeFort fractures are more complex. (See Figure 1.) A LeFort I fracture is a horizontal fracture of the maxilla, above the roots of the teeth. A LeFort II fracture separates the entire maxilla and nasal complex from the rest of the face and the cranial base. A LeFort III fracture is a total disarticulation of the midface, and extends through the orbits to separate the maxilla, nasoorbital ethmoid complex, and zygomatic arch away from the cranial base. These fractures often are evident on exam, when testing for maxillary mobility (by grasping and gently pulling on the anterior maxilla). The fracture may be unilateral, so mobility should be tested on the right and left as well as at the midline. Alternatively, different LeFort fractures can be seen on each side. Intraorally, there may be a visible split through the palate, bruising of the palate, or an anterior open bite. Significant bleeding can be seen with all of these fracture patterns, and cerebrospinal fluid (CSF) leak may complicate LeFort type II and III.6,7,10
Figure 1. LeFort Fractures
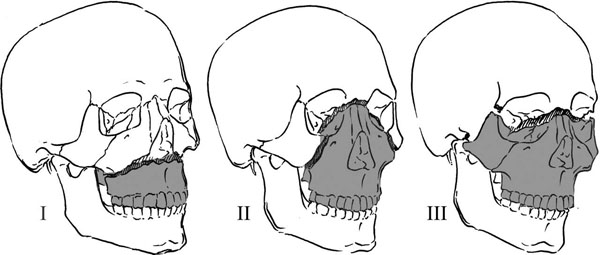
Bleeding related to facial fractures can be extensive. Life-threatening hemorrhage occurs in 1.2%–11.5% of patients with maxillofacial injuries, most commonly in those with LeFort or midface fractures.11,12 Severe bleeding is usually attributable to disruption of the maxillary artery (which passes within the LeFort fracture borders). It is difficult, if not impossible, to locate the precise origin of the bleeding since it frequently involves both the hard and soft tissues of the midface. In addition, since the fractures tend to track in a posterior direction, the damaged vessel may be located in an area too deep to be accessible to the emergency physician. For example, the pterygomaxiallary fossa, involved in LeFort fractures, contains the third segment of the internal maxillary arterya common culprit in severe bleeding.4,12 Nasal packing, the treatment of choice, can be lifesaving. Although anterior packing typically is sufficient for epistaxis, posterior packing generally is required for severe bleeding related to midface fractures. It is important to consult facial surgeons early, because if the maxilla is mobile, packing may cause further displacement and worsen the bleeding. In these cases, urgent reduction and intermaxillary fixation or even ligation of the external carotid artery is required.4,11,13 An alternative management strategy that increasingly is being used is transcatheter arterial embolization. The current literature is limited to case reports, but success rates of 87.5%–100% are reported when treating intractable hemorrhage in patients with maxillofacial trauma.11,14,15
Midface fractures that extend into the anterior cranial base put patients at risk for CSF leak. The leak most commonly occurs at the cribriform plate of the ethmoid bone, associated with nasoorbitoethmoid fractures or LeFort fractures.13 Detection of CSF rhinorrhea or otorrhea is not always simple when the presence of blood obscures other fluids; therefore, a high level of suspicion and a careful examination are critical. A simple procedure for detection of CSF is the "halo" test. CSF separates from blood when it is placed on filter paper, resulting in a central area of blood with an outer ring or halo. However, this sign does not clinch the diagnosis, because water, saline, and nasal secretions also will produce a halo when mixed with blood.16 Analysis of the fluid's glucose content (using glucose oxidase paper) is another common test, but it is extremely unreliable because nasal secretions contain reducing substances that will produce a false-positive result. The current "gold standard" for identification of CSF is the β-2 transferrin assay.17-19 If CSF rhinorrhea is confirmed (or highly suspected), a neurosurgical consultation is warranted, as surgical repair of the dura may be required.18,20 Once the diagnosis is made, the biggest management issue facing the emergency physician is the use of prophylactic antibiotics. The reported incidence of meningitis varies widely, from 0%–50%,13,19-21 and the ability of prophylactic antibiotics to convey benefit to the patient is debatable. Some studies documented lower rates of meningitis if antibiotics were given,20 but most published reports do not support their use.19,22 In fact, some studies actually showed a higher incidence of meningitis when patients received prophylactic antibiotics.21,23 The decision should be discussed with the neurosurgeons if possible, as they will be providing definitive management.
Nasoorbital ethmoid complex fractures typically occur after significant force to the bridge of the nose. The medial canthal ligaments usually are disrupted, resulting in traumatic telecanthus (widening of the intercanthal distance). This gives the patient the appearance of having wide-set eyes and results in a significant cosmetic deformity if it is not repaired. Because these fractures often extend through the cribriform plate, examine the patient for CSF leak and anosmia. If a CSF leak is present, management is similar to that for LeFort fractures as discussed above.6,7
Orbital Fractures
Orbital fractures may be isolated or part of other injury complexes, such as nasoorbital ethmoid, orbitozygomatic, and LeFort III fractures. In one series of soldiers with 1,142 blowout fractures, other facial fractures occurred in 50.9% and ocular injuries were found in 29.8%.8 Because of the high incidence of ocular injuries among patients with orbital fractures, a complete eye examination is mandatory. Isolated fractures that involve the orbital floor or medial wall are referred to as "blowout fractures." The mechanism is usually a direct blow to the orbit or globe leading to sudden pressure elevation and disruption of the weakest part of the orbit. Patients usually have periorbital edema and ecchymosis and subconjunctival hemorrhage and may complain of diplopia, cheek numbness (relationship to infraorbital nerve), and swelling that worsened after they blew their nose. Extraocular movements should be tested carefully. Restriction of superior gaze is the most common finding and usually indicates entrapment of the inferior rectus muscle. Enophthalmos usually is not seen until the swelling has decreased. The presence of exophthalmos should raise concern for retrobulbar hematoma, a true emergency.7,24
The ED management of most orbital fractures involves making the diagnosis, making appropriate surgical referral, and providing good discharge instructions. Most of these fractures are repaired 7–10 days later if the patient has persistent diplopia or enophthalmos. Patients should be discharged with sinus precautions and advised not to drive until the diplopia has resolved.7 However, two conditions associated with orbital fractures mandate immediate intervention and consultation by a surgeon in the EDmuscle entrapment and retrobulbar hematoma.
If an extraocular muscle becomes entrapped by tissue edema, immediate operative repair may not be necessary. Orbital floor fractures that lie in a longitudinal anterior-posterior direction can result in a hinged "trapdoor" phenomenon that traps the soft tissues and can cause muscle necrosis. The fracture itself, as well as the amount of tissue herniation, may not be very impressive on CT scan, so the clinical examination is key in this diagnosis. If there is any question of entrapment in an unresponsive patient, a forced duction test should be performed.25 The distinction between these two types of fractures should be made in conjunction with a facial surgeon, since the first is relatively benign while the other can lead to permanent paresis.
Retrobulbar hematoma is a vision-threatening emergency. A small amount of blood behind the eye can significantly increase the pressure in this small space with bony walls, causing ischemia and death of the optic nerve. Patients may have exophthalmos, visual loss, an afferent pupillary defect, extraocular movement restriction, and increased intraocular pressure. This is a clinical diagnosis, and although it can be seen on CT scan, imaging should never delay treatment. Urgent decompression with lateral canthotomy can be vision saving. Medical treatment with topical b-blockers, intravenous (IV) mannitol, or IV carbonic anhydrase inhibitor can be used as an adjunct to decrease intraocular pressure but should not delay or substitute for surgical treatment (lateral canthotomy).24,26,27 The patient should be referred urgently to an ophthalmologist to perform if possible, but this procedure is within the scope of the emergency physician.
Mandibular Fractures
Mandibular fractures are one of the most common facial fractures despite the significant force required to fracture the jaw. The most common cause of mandibular fracture is blunt force, usually a result of assault, MVCs, falls, and sports incidents. Pathologic fractures also can occur in the mandible. Penetrating injuries resulting in mandibular fracture usually are caused by shootings.
The common teaching is that mandibular fractures are multifocal. This is based on the understanding that the mandible is a closed ring-like structure, so compromise to a single aspect of the structure must be paralleled by compromise to the opposing side. However, recent research by Escott and Branstetter found that up to 42% of mandibular fractures occur as an isolated fracture to one side of the structure; the majority of unifocal fractures were minimally displaced simple fractures.28 The multiple types of mandibular fractures are classified primarily based on their anatomic location but also on characteristics common to all fractures, including the degree of angulation and complexity of the fracture itself (open vs. closed and simple vs. comminuted). The majority of fractures involve the condyle, angle, or symphysis of the mandible.
a.patient with an isolated mandibular fracture, like many fractures, has pain and swelling at the site of injury, usually caused by a traumatic event. Bleeding from lacerations, ecchymosis, or edema may cause asymmetry of the face. In the presence of multiple fractures, swelling of the whole lower face can produce generalized deformity. Many patients with these injuries are unable to open their mouth more than 5 cm and may have significant malocclusion of the teeth. The teeth may be loose or missing, and lacerations may be present inside or outside the mouth. Special attention should be paid to intraoral lacerations, because they may indicate an open fracture of the mandible or suggest an injury to Wharton's duct (the submandibular duct) or Stensen's duct (which drains the parotid gland into the mouth). The opening of Stensen's duct in the mouth lies adjacent to the second upper molar. Evaluate the duct by compressing the parotid gland externally while looking at the duct's outlet in the mouth. If blood is expressed from the duct, consultation for surgical repair is required to prevent fistula formation.
In the past, plain radiographs were the diagnostic test used most commonly to assess mandibular fractures; however, it is nearly impossible to visualize the entire mandible on plain film. Today, a panorex or panoramic radiograph, allows accurate identification of fractures of the mandible, teeth, and alveolar ridge. (See Figures 2 and 3.) CT scans also are highly accurate for the diagnosis of fractures and may be more beneficial in the setting of multiple facial injuries.
Figure 2. Mandibular Fracture
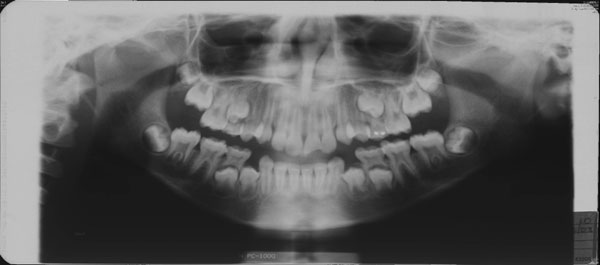
Figure 3. Mandibular Fracture
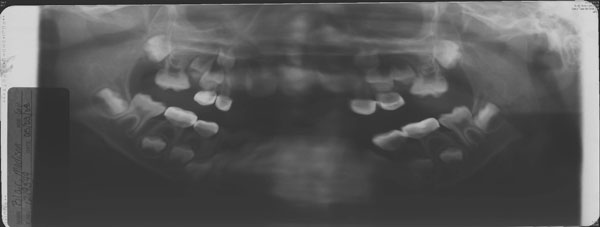
The alveolar ridge of the mandible contains the dental sockets. Fractures of this ridge must be diagnosed in a timely manner, as they are considered open fractures, with a significantly increased risk of infection and complication. Additional information about alveolar fractures is presented in the section on dental trauma.
a. for all trauma patients, management of the airway and other life-threatening injuries precedes diagnosis and treatment of facial fractures. Repair of a mandibular fracture can be deferred until the patient is stable and all other significant injuries have been treated sufficiently.
When a mandibular fracture is identified, pain management should be employed for the patient's comfort and to facilitate a thorough oral examination. Consultation with an oral or plastic surgeon should be requested, because reduction of the fracture will be necessary. The emergency physician should contact treatment centers on controlling pain and obtain proper radiographic studies in preparation for consultation.
The stability of the fracture can determine the need for urgent or delayed follow-up. The emergency physician should be able to recognize the difference and formulate a disposition based on this information. Open fractures and unstable fractures of any kind require evaluation by a consultant in addition to antibiotics and likely inpatient hospitalization for definitive treatment. Fractures of the mandible that are closed in nature can be stable or unstable depending on the direction of the fracture line. Downward running fractures from posterior to anterior typically are stable, given the location of the musculature that helps pull the body together across the fracture line. Fractures that run downward from the anterior to posterior of the mandibular body are considered unstable because the musculature causes stress and displacement of the fracture. Edentulous patients with mandibular fractures are considered unstable, unless the patient has dentures that continue to fit comfortably. The dentures act as a splint, stabilizing the fracture until further treatment can be obtained. Any patients who are deemed to have an isolated stable, closed fracture can be discharged home safely with outpatient follow-up. These patients should be given pain control in the form of nonsteroidal anti-inflammatory drugs and a short course of narcotics if appropriate. Antibiotics are not necessary. Patients should be encouraged to adhere to a soft or pureed diet until further evaluation.
Most mandibular fractures are managed surgically with one of two options. Open reduction and fixation, involving the use of plates and screws, is undertaken in the operating room. Mandibulomaxillary fixation and closed reduction ("wiring the jaw") is used when open reduction is not an option or when a simple minimally displaced fracture is being treated. The choice is influenced by the patient's disposition and the potential for complications. Follow-up is mandatory for patients who undergo definitive fixation to ensure the injury is healing properly.
Nasal Fractures
The nose consists of two bones that join to form a pyramid-like structure as well as cartilage and soft tissue. Its anterior location on the face places it at higher risk for injury. The nose often is injured in MVCs, sports incidents, falls, and assaults. The nasal bones are probably the most commonly fractured facial structure.29
Patients with nasal fractures typically present with pain, swelling, and deformity of the nose. Infraorbital ecchymosis is also a common finding. Epistaxis may or may not be present by the time the patient presents to the ED. Evaluate the septum thoroughly to look for a septal hematoma, which is associated with septal necrosis and ultimately a saddle-nose deformity if it is not treated appropriately. Evaluate the nasal passages for any evidence of open nasal or septal fracture; the presence of open fractures will alter management requiring antibiotics and evaluation by a consultant for open reduction of the fracture.
If an isolated nasal fracture is suspected, plain radiographs are sufficient for the diagnosis; however, if concern exists about the possibility of additional facial fractures, a CT scan of the facial bones is warranted. (See Figure 4.) It is important to exclude any involvement of the nasoorbitoethmoid complex. Most isolated nasal bone fractures are managed based on external appearance once the swelling has resolved and management at that time is dictated by a surgeon.
Figure 4. Nasal Fracture
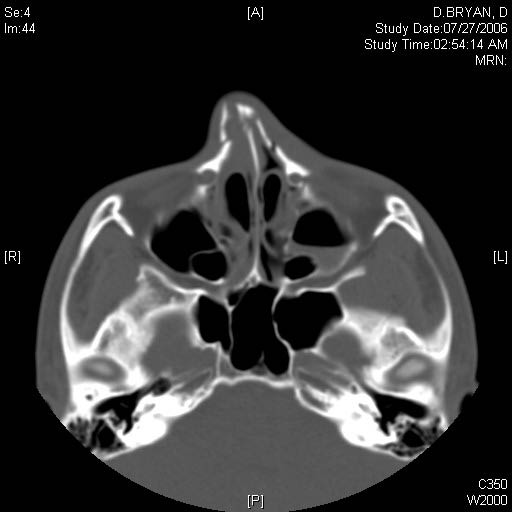
Initial management in the ED centers on symptom management. Epistaxis should be stopped using traditional techniques and pain should be controlled. If a septal hematoma is identified, incise it and remove the clot, then pack the nose anteriorly to prevent reaccumulation of the hematoma. Prescribe a course of antibiotics for anyone who receives nasal packing to prevent toxic shock syndrome and sinusitis. Antibiotics also are indicated in the presence of an open nasal bone fracture and should be aimed at treating organisms expected in the nasopharynx. If deformity (lateral or depressed) of the nose is obvious and severe, closed reduction may be necessary. Closed reduction was once the mainstay of treatment for most nasal fractures. Today, it remains common, but open reduction is more frequently employed. Open reduction is used to correct significant fracture and dislocation of the nasal bone and to close an open septum.
For most patients with nasal bone fractures, outpatient follow-up with a plastic surgeon 3 or 4 days following the injury is imperative. At that time, any swelling that obscured deformities will have subsided, so that the need for further repair can be assessed.30
Frontal Sinus Fractures
The frontal sinus bone consists of an anterior and a posterior table, one or both of which can be fractured. In actuality, fracture of this bone is uncommon because it is highly resilient. When frontal sinus fractures do occur, they can be complicated by CSF leak, increasing the risk for infection.
Patients with frontal sinus fractures tend to present with swelling, pain, ecchymosis, and deformity. They might have pain only with palpation of the frontal sinus. A step-off deformity may be detected. Rhinorrhea in these patients should be considered a CSF leak, and the need for further evaluation for a definitive diagnosis should be assumed.
CT scan is the primary radiographic technique used in the diagnosis. In most patients with facial trauma, more than one fracture is present, making plain radiographs inadequate and thus outdated. Thin CT cuts of the frontal sinus should be requested if a fracture is suspected.
Frontal sinus fractures are diagnosed and categorized based on location (anterior table, posterior table, or both) as well as the amount of displacement. Fractures of the anterior table are most common, followed by fracture of both tables; isolated fractures of the posterior table are relatively uncommon, accounting for < 6% of these injuries.31 Fractures involving the posterior table increase the risk of CSF leak, because of the proximity of the dura and the risk of tear with fracture.
The repair of frontal sinus fractures typically is based on two factors: the degree of comminution or displacement and the presence of a CSF leak. A 1–2 mm displacement can be managed nonoperatively. Patients with a frontal sinus fracture who are stable enough for discharge should be made aware of the possibility of CSF leak and instructed to return to the ED for repeat evaluation if they suspect one. Greater than 2 mm displacement, significant comminution, or a CSF leak mandates consultation with a neurosurgeon for evaluation and possible surgical repair. Fractures with more than 2 mm displacement and without a CSF leak can be repaired electively in 7–10 days. Antibiotics are not necessary. If a CSF leak occurs before the repair, the patient should be reevaluated for possible hospital admission and antibiotics should be considered in consultation with a neurosurgeon. It is not uncommon for CSF leaks to resolve spontaneously in 5–7 days.
Patients rarely have isolated frontal bone fractures, and thus disposition often is obvious based on the extent of their other injuries. Perioperative antibiotics are a standard of care in hospitals. A recent study by Lauder et al found that additional antibiotics before or after the perioperative period do not change the rates of infection secondary to facial fractures. It was suggested, however, that the greater the severity and number of facial fractures, the higher the rates of infection, thus a likely benefit of using antibiotics outside the perioperative window.32
Ocular/Globe Trauma
In the setting of facial trauma, the globes and visual acuity should be evaluated carefully. The anatomy of the orbit is highly protective of the globe and often prevents globe injury, but orbital fractures are a common finding in patients with facial trauma. The injury that causes the most concern when facial trauma involves the region of the eye is globe rupture, which is typically the result of blunt trauma. The most common site of globe rupture is where the sclera is thinnest (at the insertion of the extraocular muscles, at the site of a previous injury, or in a surgical scar).33 Pressure placed on the globe by a penetrating or blunt force causes tears within the sclera, defining "globe rupture."
a. open globe, which is usually caused by a penetrating injury, requires emergent ophthalmologic intervention. This injury needs to be diagnosed rapidly, and the eye must be protected from further injury as soon as the diagnosis is made.
Patients with globe injuries will present with obvious injuries to the face and may have obvious trauma to the orbital region. Periorbital edema or ecchymosis may be present and may increase the difficulty of performing a good examination. Subconjunctival hemorrhage may be present as well, and the anterior chamber needs to be examined for hyphema and lens dislocation. The patient may have blurred vision or might not be able to see. He or she might describe a foreign body sensation. Of course, if the patient is unconscious, he or she will not be able to assist the emergency physician with the ophthalmic evaluation.
Evaluate the visual acuity in both eyes using a Snellen chart (use a bedside chart if necessary). Test the patient's extraocular movements; consider any deficit an indication of possible orbital fracture with muscle entrapment. Test the peripheral vision as well. The application of fluorescein in conjunction with a Wood's lamp or slit lamp can be used to diagnose a corneal abrasion or an open globe injury. Uptake of fluorescein in a given spot on the cornea indicates abrasion and a Seidel test can be performed to determine the possibility of open globe injury. A Seidel test is positive when fluorescein, applied to the site of suspected injury, streams down into a bright green pool, giving the appearance of a running waterfall.34
Measurement of intraocular pressures is imperative and can be done at the bedside with a Tono-Pen® tonometer. Elevated pressures in one or both eyes should cause concern and lead to an ophthalmology consult.
If a globe rupture or open globe injury is suspected at any point in the evaluation or actually is confirmed, no further examination should take place. An eye shield should be placed over the eye immediately, with care being taken to place no pressure on the globe. An immediate ophthalmology consult should be obtained. Globe rupture has a poor prognosis, but expeditious diagnosis and treatment can improve the patient's likelihood of retaining vision.35
Dental Trauma
Dental trauma is extremely common: One-fourth of the U.S. population has experienced injury to one or more of their permanent incisors.36 The worldwide prevalence of dental trauma seen in the ED is high, estimated to affect 4%–10% of patients. The overwhelming majority of these patients are under 15 years of age.36
Dental trauma often accompanies facial fractures. While the fractures may demand more immediate treatment, documenting the dental trauma (and informing the patient of it) is imperative. One study of 273 patients with facial fractures examined the rate of coincident dental trauma. Among patients with fractures to non-tooth-bearing bones, 10% experienced dental trauma. For those with trauma to the mandible, that rate increased to 39%.37 Another study found that 64% of patients with bilateral mandibular condylar fractures had damage to the dentition.36
a.thorough assessment of dental trauma mandates cleaning all of the blood and debris away from the mouth. The easiest way to accomplish this is to have the patient swish and spit several times; local anesthesia or parenteral pain medication may be required. Exploring lacerations should include a careful search for foreign bodies, particularly fragments of broken teeth. Take note of areas of bleeding from the gum, which may indicate damage to the underlying bony structures. Assess the temporomandibular joint for range of motion, since limited mouth opening or asymmetry often indicates a fracture or dislocation. Any malocclusion calls for imaging to look for fracture. If the patient is missing a tooth, assume that it has been aspirated, swallowed, or impaled in the soft tissue.
Crown fractures are the most common injury to teeth, accounting for 65%–75% of all injuries to the permanent dentition. They range from enamel involvement only (Ellis class I), which usually causes minimal pain, to a fracture through the enamel, dentin, and pulp, which carries a much worse prognosis. If the fracture involves enamel and dentin only (Ellis class II), a temporary filling that covers the dentin generally does not affect whether or not the tooth will die, so emergent dental treatment is not necessary.38 In contrast, if the pulp is exposed (Ellis class III), there is a much higher rate of healing (72%–100%) if the tooth is restored by a dentist within 3 hours.36
Root fractures are relatively rare. Treatment delays of up to several days have no influence on healing.38
Luxation injuries occur when a tooth is displaced from its socket. They can be intrusive (tooth pushed further into the jaw), extrusive (tooth pulled partially out of the jaw), or lateral. The injuries often involve fractures of the alveolar bone as well. When dealing with luxation injuries, the tooth should be repositioned into its anatomic location and splinted, if possible. However, clinical trials have not been able to demonstrate a benefit on healing between this method of treatment vs. no treatment.38 Also, although antibiotics generally have been recommended to prevent bacterial invasion of the injured periodontium and pulp, some research suggests this treatment actually may have a negative impact on healing.38
Tooth avulsion injuries are rare (accounting for 0.5%–3% of all injuries affecting permanent teeth) but are among the injuries most likely to be seen in the ED. Minimizing extraoral time is the most important factor in healing. Immediate reimplantation by the patient leads to the highest success rate. While gross contamination of the root surface has been shown to increase root resorption, so has rinsing of the root surface. Antibiotics have not been shown to improve healing, but since this is an open fracture, the patient's tetanus status should be updated. When replanting the tooth, hold it by the crown, minimizing contact with the root (which could further damage the periodontal ligament). If a clot has formed in the socket, remove it only if it interferes with seating the tooth. The tooth should be pushed firmly into the socket (local anesthesia is usually required); once in place, have the patient bite onto a gauze roll. The patient should see a dentist that day and should be advised that even if the tooth reattaches, it almost certainly will require a root canal. Teeth that have been avulsed longer than 1 hour or have been stored dry have a very poor prognosis. Reimplantation can be considered on an individual basis, with the patient understanding that even with expensive and lengthy dental follow-up, there is a high chance that he or she will still lose the tooth. While no discussion of avulsed teeth would be complete without including the preferred transport mediums (in order of preference: Hank's balanced salt solution, saliva, saline, milk, water), this is generally a moot point once the patient is seen in the ED.36,38-40
a.veolar bone fractures occur in 5%–9% of all patients with dentoalveolar injuries and usually are associated with other injuries to the teeth.36 If they involve only one tooth (typically seen in conjunction with a luxation injury), no additional immediate treatment usually is required other than prompt referral to a dentist. However, if the fracture is segmental (involving multiple teeth), an oral surgeon should be consulted while the patient is in the ED. Segmental fractures should be suspected when multiple teeth move while one is checking the mobility of a single tooth. They should be confirmed by imaging. Dental x-ray films are certainly adequate; however, since they are not widely available in the ED, a panorex or CT scan is reasonable. Treatment usually involves a rigid splint.36,39
Lacerations/Burns
Many trauma patients sustain lacerations to the face and head. The primary goals of repair are wound healing, preventing infection, and achieving good functional and cosmetic outcomes. Cosmetic repair of lacerations to the eye, lip, and ear is of utmost importance, given the need to maintain symmetry. (See Table 1.) In the evaluation of how to repair a laceration for the best cosmetic appearance, use Langer's lines to determine if deep suturing is needed. Anatomically important structures are located close to the aforementioned parts and are easily damaged by trauma.
Table 1. Laceration Repair Chart
Suture, Size Anesthesia or Block Important points to remember
Face Deep: 3-0 or 4-0 absorbable Dependent on location Consider using Langer's lines to ensure a Superficial: 4-0 or 5-0 Blocks may be necessary only if good cosmetic outcome non-absorbable wound distortion may complicate Only use skin glue for linear, small, and Skin glue closure and cosmetic outcome superficial lacerations that are NOT Lidocaine with epinephrine under tension
Eyelid or Deep: 4-0 absorbable Lower Lid: Infraorbital block Colored suture (blue or purple) within theEyebrow Superficial: 5-0 or 6-0 Upper lid or eyebrow: Supraorbital block eyebrow makes removal easier non-absorbable Lidocaine with epinephrine
Lip Deep: 4-0 absorbable Upper lip: Infraorbital block Always align the vermilion border first Superficial: 5-0 non- Lower lip: Mental nerve block Avoid using local infiltration anesthetic absorbable or Prolene Lidocaine with epinephrine
Intraoral Deep: 3-0 or 4-0 absorbable Buccal Mucosa: Long buccal block Closure of wounds > 1-2 cm decreases Superficial: 3-0 chromic gut OR risk of infection Local infiltration Antibacterial mouth rinse should be Lidocaine with epinephrine prescribed
Ear Perichondrium: 4-0 or 5-0 Pre-auricular block using Align cartilage well, then suture over skin; absorbable lidocaine (NO epinephrine) pressure dressing is imperative to Skin: 4-0 or 5-0 non- prevent hematoma absorbable or Prolene
Scalp Staples Local infiltration Shaving hair increases the risk of Deep or galea: 3-0 Lidocaine with epinephrine infection absorbable Superficial: 2-0 or 3-0 non-absorbable
For any laceration, always remember to update the tetanus if necessary!
The head is an extremely vascular part of the body; therefore, injuries can result in substantial bleeding and unrecognized blood loss, making control of bleeding an important focus of initial treatment. All lacerations of the head and face should be anesthetized adequately to facilitate thorough irrigation and closure. Anesthesia can be induced in several ways, including nerve blocks and subcutaneous infiltration. Nerve blocks should be considered in situations in which subcutaneous injection of anesthesia may distort the tissue and compromise accurate approximation, as in the assessment and repair of lacerations involving the eyebrow or vermilion border of the lip. Some of the more commonly used nerve blocks in the face include the supraorbital, infraorbital, and submental blocks. These three blocks cover the majority of the face in different distributions and are easily performed. Lacerations close to the midline may require bilateral blocks as sensory fibers can, and do cross the midline. Irrigation should be done using standard techniques. The wound should be evaluated fully in a clean and bloodless field so that all foreign bodies can be identified and removed. Devitalized tissue should be debrided carefully, and the wound should be closed with sutures sized appropriately for the location of the wound. When required, deep sutures should be placed with absorbable suture material to prevent deformity of the area once healing and scar formation occur. Lacerations to the scalp are treated with proper irrigation and closure, often using staples, rather than sutures, for ease and expediency. Tissue adhesive can be used for lacerations on the face and usually are very effective in closing low tension, straight lacerations. All patients should be educated about signs and symptoms of infection and instructed when to return for suture removal or a wound recheck.
Lacerations that involve the eye or eyelid or that are close to the lateral or medial canthus may need to be evaluated and closed by an ophthalmologist. The concern revolves around possible damage to the lacrimal apparatus. The lacrimal gland is located within the upper eyelid in the lateral position and has an excretory duct that empties into the superolateral eyelid. Comparatively, the lacrimal canals join in the medial canthus to form the nasolacrimal duct, which drains into the ipsilateral nare. Disruption of the lacrimal apparatus has several possible consequences, including dacryocystitis and ectropion formation, if it is not diagnosed and repaired properly. In most cases, isolated damage to the lacrimal apparatus can be repaired within 48 hours following the injury. Injuries secondary to animal bites should be evaluated immediately by an ophthalmologist, because they tend to be heavily contaminated wounds. These patients should be placed on antibiotics. Antibiotic choice should be based on the type of animal bite and whether the antibiotics are for prophylaxis (5 days) or to treat an active infection (14 days). Antibiotic choices include amoxicillin clavulanate, clindamycin, or doxycycline.
a. mentioned above, lacerations that cross the upper or lower vermilion border present important and difficult wound repairs because of the cosmetic outcome. It is important that the margins of the vermilion border be approximated exactly, as misalignment of less than 1 mm is easily noticed once the laceration is healed. The nerve supply to the lower lip is through the mental nerve and to the upper lip through the infraorbital nerve, which can both be anesthetized using regional nerve block techniques.
Intraoral lacerations may not always require closure, because the mucosa heals very quickly and very well on its own. There are two specific indications in which an intraoral laceration should be closed: 1) if the laceration exceeds 1 or 2 cm, increasing the likelihood that food particles may be entrapped and become a nidus for infection, and 2) if the laceration interferes with the patient's ability to chew. All teeth should be evaluated for stability and injury. The oral cavity, especially any intraoral lacerations, should be examined for pieces of broken tooth. Wounds within the mouth potentially are exposed to significant contamination, which makes proper irrigation essential. Intraoral lacerations may require deep suturing with 4-0 or 5-0 absorbable sutures. The superficial laceration can be closed using absorbable sutures as well. The use of prophylactic antibiotics is controversial and has not been sufficiently studied to allow a definite conclusion to be made. The limited evidence suggests antibiotics may be of benefit for some oral lacerations.41 Through-and-through lacerations are considered higher risk for infection, so some clinicians prescribe antibiotics. If a wound is particularly contaminated or has been caused by an animal, antibiotics are appropriate.42 Otherwise, antibiotics are not necessary. A simple oral antibiotic rinse (e.g., Peridex) is beneficial and can be prescribed if desired.
Lacerations to the ear pose a potentially difficult situation. Repair of these lacerations is challenging because of the anatomy. The stiff nature and deep grooves present a complex suturing surface. Specific attention to detail is required to ensure a good cosmetic outcome and long-term survival of the tissue. The shape of the ear and the presence of a symmetric partner make a good cosmetic outcome crucial. Being a primarily cartilaginous structure, the ear is avascular in nature, which can complicate tissue survival if a wound is not repaired correctly.
Lacerations to the ear should be irrigated in a standard fashion, with special effort made to not over-irrigate or to irrigate too forcefully, which could devitalize and damage the perichondrium. Approximation of the cartilage is imperative for healing and must be done well prior to closure of the skin. Although suturing of the cartilage is not necessary (assuming good approximation occurs), it can be helpful in the repair process. If the cartilage is sutured, 4-0 or 5-0 absorbable sutures should be used. Once the cartilage has been approximated adequately, closure of the skin finishes the repair. If significant cartilage or skin loss prevents closure with a good cosmetic outcome, surgical consultation should be sought. After repair, vaseline gauze can be used over the sutures and within the crevices of the ear. Apply a pressure dressing to prevent continued bleeding and hematoma formation, which would compromise the ear's minimal vascular supply. A gauze dressing can be placed between the ear and the scalp to prevent pressure necrosis.43
Facial Burns
The American Burn Association estimates that approximately 500,000 people seek medical treatment for burn injuries each year and that approximately 40,000 of them are admitted to the hospital as a result of their injuries.44 More than half of those admitted are treated in burn centers across the country.
Facial burns are serious injuries and are commonly present in conjunction with burns of other areas of the body. Fortunately, the majority of patients who present to emergency departments for treatment of burns have superficial wounds affecting a small percentage of total body surface area (TBSA).
Burns are categorized based on the cause (e.g., thermal, electrical, fire) and then further classified based on depth (superficial thickness, partial thickness, or deep) and the layers of tissue that are involved. TBSA can be estimated quickly using the Rule of 9s. Fluid resuscitation with lactated Ringer's solution should be initiated immediately and is based on the TBSA burned. The most commonly accepted formula for calculating fluid requirement is the Parkland formula.
Inhalation injuries should be one of the initial concerns in a patient who has facial burns. The presence of stridor, wheezing, soot in the airway, or singeing of the eyelashes, brows, or hair should prompt the physician to assume early control of the airway.45
Carbon monoxide (CO) and cyanide poisoning also should be early concerns. The carboxyhemoglobin level should be measured. Treatment is based on symptoms (including headache, vomiting, and mental status), ECG findings, and CO level; however, all burn patients with or without suspected CO poisoning should receive 100% oxygen. Treatment for cyanide poisoning should be initiated empirically if a patient has unexplained metabolic acidosis, a normal CO level, and an elevated venous oxygen level.46
Patients who have significant burns (> 10%–20% of TBSA) or airway involvement should be stabilized and transferred to the closest burn center for further treatment. If transfer to a burn unit is imminent, wrapping the patient in a clean, dry sheet is all that is necessary. If transfer is delayed, wound care should be initiated. First, clean the wounds with sterile saline; then, using sterile technique, debride all blisters, except those on the palms of the hands and soles of the feet. A topical antibiotic dressing should be applied.46
a.l patients who have sustained a burn injury, regardless of percentage of TBSA involved or depth of the burn, should receive a tetanus booster, cleaning, debridement of any blisters, and dressing of the burn with antibiotic ointment. Close follow-up for the development of complications is important.47
The decision to admit a burned patient to the hospital is based on recommendations by the American Burn Association. Any adult who sustains partial-thickness burns over 10%–20% of TBSA, any child younger than 10 years old with partial-thickness burns covering 5%–10% of TBSA, or any partial-or full-thickness burns to the face, genitalia, hands, feet, or crossing any major joints should be transferred immediately to a burn center for evaluation and treatment.
Conclusion
Facial trauma is a common complaint in the emergency department, and management can be challenging. As with any trauma patient, the initial priority is always the ABCs, with particular attention to airway, major bleeding, and associated brain injury. It is important to remember that although the facial injuries may be the most obvious, these patients often have concomitant injuries. Once initial stabilization has occurred, a thorough, systematic examination will guide the remainder of evaluation and management. Given the highly visible nature of these injuries, special attention must be paid to the cosmetic repair techniques. Surgical consultation may be required for many of these patients. Most facial trauma is not life-threatening, although significant morbidity is possible. Careful examination, judicious imaging, and appropriate consultation will ensure the best outcomes for these patients.
References
1. Parsa T, et al. Inital evaluation and management of maxillofacial injuries. eMedicine 2010.
2. Thoren H, et al. Occurrence and types of associated injuries in patients with fractures of the facial bones. J Oral Maxillofac Surg 2010;68:805-810.
3. Ceallaigh PO, et al. Diagnosis and management of common maxillofacial injuries in the emergency department. Part 1: Advanced trauma life support. Emerg Med J 2006;23:796-797.
4. Lynham AJ, et al. Emergency department management of maxillofacial trauma. Emerg Med Australas 2004;16:7-12.
5. Elahi MM, et al. Cervical spine injury in association with craniomaxillofacial fractures. Plast Reconstr Surg 2008;121:201-208.
6. Tucker M. Management of facial fractures. In: Peterson L, ed. Oral & Maxillofacial Surgery. 3rd ed. St. Louis: Mosby; 1998.
7. McKay MM. Facial trauma. In: Marx JA, ed. Rosen's Emergency Medicine: Concepts & Clinical Practice. 7th ed. Philadelphia: Mosby Elsevier; 2009.
8. Shere JL, et al. An analysis of 3599 midfacial and 1141 orbital blowout fractures among 4426 United States Army Soldiers, 1980-2000. Otolaryngol Head Neck Surg 2004;130:164-170.
9. Ceallaigh PO, et al. Diagnosis and management of common maxillofacial injuries in the emergency department. Part 3: Orbitozygomatic complex and zygomatic arch fractures. Emerg Med J 2007;24:120-122.
10. Ceallaigh PO, et al. Diagnosis and management of common maxillofacial injuries in the emergency department. Part 4: Orbital floor and midface fractures. Emerg Med J 2007;24:292-293.
11. Wu SC, et al. Angioembolization as an effective alternative for hemostasis in intractable life-threatening maxillofacial trauma hemorrhage: Case study. Am J Emerg Med 2007;25:988.e1-5.
12. Ardekian L, et al. Life-threatening complications and irreversible damage following maxillofacial trauma. Injury 1998;29:253-256.
13. Ellis E 3rd, Scott K. Assessment of patients with facial fractures. Emerg Med Clin North Am 2000;18:411-448.
14. Cogbill TH, et al. Management of maxillofacial injuries with severe oronasal hemorrhage: A multicenter perspective. J Trauma 2008;65:994-999.
15. Liu WH, et al. Transarterial embolization in the management of life-threatening hemorrhage after maxillofacial trauma: A case report and review of literature. Am J Emerg Med 2008;26:516.e513-e515.
16. Dula DJ, Fales W. The 'ring sign': Is it a reliable indicator for cerebral spinal fluid? Ann Emerg Med 1993;22:718-720.
17. Welch KC SJ. CSF Rhinorrhea. EMedicine 2009.
18. Abuabara A. Cerebrospinal fluid rhinorrhoea: Diagnosis and management. Med Oral Patol Oral Cir Bucal 2007;12:E397-E400.
19. Bell RB, et al. Management of cerebrospinal fluid leak associated with craniomaxillofacial trauma. J Oral Maxillofac Surg 2004;62:676-684.
20. Friedman JA, et al. Post-traumatic cerebrospinal fluid leakage. World J Surg 2001;25:1062-1066.
21. Choi D, Spann R. Traumatic cerebrospinal fluid leakage: Risk factors and the use of prophylactic antibiotics. Br J Neurosurg 1996;10:571-575.
22. Daudia A, et al. Risk of meningitis with cerebrospinal fluid rhinorrhea. Ann Otol Rhinol Laryngol 2007;116:902-905.
23. Clemenza JW, et al. Craniofacial trauma and cerebrospinal fluid leakage: A retrospective clinical study. J Oral Maxillofac Surg 1995;53:1004-1007.
24. Bord SP, Linden J. Trauma to the globe and orbit. Emerg Med Clin North Am 2008;26:97-123.
25. Mathur N. Orbital Fractures. eMedicine 2009.
26. Shek KC, et al. Acute retrobulbar haemorrhage: An ophthalmic emergency. Emerg Med Australas 2006;18:299-301.
27. Winterton JV, et al. Review of management options for a retrobulbar hemorrhage. J Oral Maxillofac Surg 2007;65:296-299.
28. Escott EJ, Branstetter BF. Incidence and characterization of unifocal mandible fractures on CT. AJNR Am J Neuroradiol 2008;29:890-894.
29. Hwang K, et al. Outcome analysis of sports-related multiple facial fractures. J Craniofac Surg 2009;20:825-829.
30. Mondin V, et al. Management of nasal bone fractures. Am J Otolaryngol 2005;26:181-185.
31. Tollefson TT, Strong EB. Frontal Sinus Fractures. eMedicine 2009.
32. Lauder A, et al. Antibiotic prophylaxis in the management of complex midface and frontal sinus trauma. Larygoscope 2010;120:1940-1945.
33. Golden D. Globe rupture. In: Marx JA, ed. Rosen's Emergency Medicine: Concepts & Clinical Practice. 6th ed. Philadelphia: Mosby Elsevier; 2008.
34. Pokhrel PK, Loftus SA. Ocular emergencies. Am Fam Physician 2007;76:829-836.
35. Kuhn F. Ocular traumatology and the ocular trauma specialist. Graefes Arch Clin Exp Ophthalmol 2008;246:169-174.
36. Dale RA. Dentoalveolar trauma. Emerg Med Clin North Am 2000;18:521-538.
37. Lieger O, et al. Dental injuries in association with facial fractures. J Oral Maxillofac Surg 2009;67:1680-1684.
38. Andreasen JO, et al. Contradictions in the treatment of traumatic dental injuries and ways to proceed in dental trauma research. Dent Traumatol 2010;26:16-22.
39. Ceallaigh PO, et al. Diagnosis and management of common maxillofacial injuries in the emergency department. Part 5: Dentoalveolar injuries. Emerg Med J 2007;24:429-430.
40. Flores MT, et al. Guidelines for the management of traumatic dental injuries. II. Avulsion of permanent teeth. Dent Traumatol 2007;23:130-136.
41. Steele MT, et al. Prophylactic penicillin for intraoral wounds. Ann Emerg Med 1989;18:847-52
42. Mark DG, Granquist EJ. Are prophylactic oral antibiotics indicated for the treatment of intraoral wounds? Ann Emerg Med 2008;52:368-372.
43. Brown DJ, et al. Advanced laceration management. Emerg Med Clin North Am 2007;25:83-99.
44. 2007 Fact Sheet. American Burn Association. Available at: www.ameriburn.org/resources_factsheet.php. Accessed August 26, 2010.
45. Griffin JE, Johnson DL. Management of the maxillofacial burn patient: Current therapy. J Oral Maxillofac Surg 2005;63:247-252.
46. Singer AJ, et al. Thermal burns. In: Marx JA, ed. Rosen's Emergency Medicine: Concepts & Clinical Practice. 7th ed. Philadelphia: Mosby Elsevier; 2009.
47. Gomez R, Cancio LC. Management of burn wounds in the emergency department. Emerg Med Clin North Am 2007;25:135-146.
Our faces play a role in almost every part of our lives. The structure and components of the face are involved in our ability to eat, speak, and see, and often are the features first noticed when we meet someone.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
