Advanced Emergency Ultrasound Applications
Advanced Emergency Ultrasound Applications
Authors:
Teresa S. Wu, MD, FACEP, Director, EM Ultrasound Program, Co-director, Simulation Based Training Program, Associate Program Director, EM Residency Program, Maricopa Medical Center, Clinical Associate Professor, Emergency Medicine, University of Arizona School of Medicine, Phoenix.
Ryan Finlayson, MD, Emergency Medicine Resident, Maricopa Medical Center, Department of Emergency Medicine, Phoenix, AZ.
Peer Reviewer:
Michael Blaivas, MD, Professor of Emergency Medicine, Associate Professor of Internal Medicine, Vice President, Society of Ultrasound Education, Department of Emergency Medicine, Northside Hospital Forsyth, Cumming, GA.
Introduction
You are nearing the end of a busy shift in your emergency department (ED) when pre-hospital providers arrive with your next patient. They bring in a 69-year-old male with a chief complaint of headache and chest pain. Emergency medical services (EMS) activated him as a "code STEMI" in the field. He is hypertensive, diaphoretic, and complaining of a headache and chest pain on arrival.
Your cardiologist and the cardiac catheterization team are standing at the bedside ready to whisk him away to the catheterization suite, but as your nursing team hooks the patient up to the monitor, his vital signs and clinical presentation give you pause. The patient's blood pressure is 210/112 mmHg, his heart rate is 115 beats per minute, his respiratory rate is 32 breaths/minute, with an oxygen saturation of 100%. He is sitting upright holding his head with one hand and his chest with the other. A portable chest X-ray demonstrates a normal mediastinum and no other acute abnormalities, but you have a sneaking suspicion that something just isn't quite right.
His 12-lead ECG in the ED demonstrates a clear ST-segment elevation in leads II, III, aVF with reciprocal changes noted in the lateral leads, and your cardiologist is champing at the bit to take him to the catheterization lab to meet the recommended door-to-PCI times. The patient is complaining that his headache is getting worse, and you know you have only a few minutes to make a critical decision that could potentially save this patient's life. You perform a quick bedside ocular ultrasound to evaluate his optic nerves bilaterally, and what you see is enough to change the patient's entire management course. His nerve sheaths are dilated to 6.5 mm bilaterally, suggesting that he has acute increased intracranial pressure. With a chief complaint of a severe headache, you decide to send this patient to the CT scanner to rule-out an intracranial hemorrhage before he goes up to the catheterization lab.
As the scanner images are loading up on your PACS system, you breathe a long sigh of relief and pat yourself on the back for staying true to your convictions. The patient's scans demonstrate a large intracranial hemorrhage that precluded him from receiving emergent anticoagulation and PCI.
Does this clinical scenario sound far-fetched for your hospital ED? Perhaps now it does, but remember what occurred before rapid sequence intubation with sedatives and neuromuscular paralytic agents, procedural sedation with intravenous opiates and sedatives, and synchronized cardioversion became common practice in the ED? The history of emergency medicine is full of techniques and procedures that have been adapted for use in the emergency department.
Over the past few years, emergency physicians have discovered more and more ways to utilize bedside ultrasonography in their clinical practice. As the field of emergency ultrasound has developed, practitioners have learned that they can perform bedside scans to help make critical diagnoses and guide them during complicated procedures. This article provides an overview of some of the advanced emergency ultrasound applications used in clinical practice today.
Ultrasound-guided Pericardiocentesis
Indications. The pericardium is a two-layered structure that surrounds the heart. The outer layer, the parietal pericardium, is separated from the inner layer, the visceral pericardium, by 25-50 mL of fluid. A pericardial effusion develops when infectious, serous, hemorrhagic, serosanguinous, or chylous fluid accumulates in between the parietal and visceral pericardium.
Making the diagnosis of a pericardial effusion is often difficult based on clinical findings alone. Patients with a pericardial effusion may present with a myriad of symptoms including, but not limited to, chest pain, shortness of breath, dizziness, dyspnea on exertion, nausea, vomiting, diaphoresis, fevers, chills, or weight loss secondary to the underlying etiology. On physical examination, diminished heart sounds or a pericardial friction rub are noted in only one-third of patients with a pericardial effusion.
Bedside 2-D ultrasonography can be used to evaluate for the presence of a pericardial effusion, to estimate the size of the effusion, and to determine if tamponade physiology is present. Once enough fluid accumulates between the parietal and visceral pericardium, diastolic filling pressures can become compromised. If the diastolic filling pressure cannot overcome the increased intrapericardial pressures, systemic venous return is impaired, and right ventricular (RV) and right atrial (RA) collapse will be noted on bedside ultrasonography.
The amount of pericardial fluid required to cause tamponade depends primarily on the rate of accumulation and not the absolute volume of fluid. Cardiac tamponade can be seen following the rapid accumulation of as little as 150 mL of pericardial fluid.
Once cardiac tamponade has been diagnosed, bedside ultrasound can be used to guide an emergent pericardiocentesis.
Contraindications. There are no absolute contraindications for performing a bedside 2-D evaluation of the pericardial space, but note that performing a bedside ultrasound should not delay definitive or operative interventions when warranted. If a large pericardial effusion is visualized and the patient is hemodynamically stable, the pericardiocentesis or pericardial window can be performed in the cardiac catheterization laboratory or operating room, respectively. In patients who are hemodynamically unstable, an emergent pericardiocentesis will need to be performed at the bedside.
Risks. There are no inherent increased risks to utilizing bedside ultrasound to guide a pericardiocentesis. Performing a pericardiocentesis via the landmark approach (in a "blind" fashion), puts the patient at risk for perforation or laceration of the right ventricle and other adjacent structures. If the subxiphoid approach is utilized, inadvertent perforation of the liver, stomach, and intestines has been described in the literature. During an intercostal or apical pericardiocentesis, the patient is at risk for accidental puncture of the ventricles or pulmonary pleura. Using ultrasound guidance can significantly decrease these risks.
Benefits. Bedside echocardiography can determine if a pericardial effusion is present, can help estimate the size of the effusion, and be used to determine the best approach to performing a pericardiocentesis.1,2 If the patient is unstable and there is evidence of end-diastolic right atrial or right ventricular collapse, the physician should proceed with an ultrasound-guided pericardiocentesis at the bedside. With ultrasound guidance, the operator can map out surrounding structures and visualize the trajectory of the needle during the procedure.
How to Perform the Procedure.
Prep and drape the patient and the ultrasound transducer in a sterile fashion.
Use a 5-2MHz curvilinear transducer or a 5-1MHz phased array transducer to visualize the heart and adjacent structures. The phased array transducer has a smaller footprint and is easier to manipulate between the ribs and around the sternum. If a smaller footprint probe is not readily available, the low frequency curvilinear probe is the next best option.
Obtain both subxiphoid and parasternal or apical views of the pericardial space and adjacent structures to determine the best site for performing a pericardiocentesis. Determine which site provides direct access to the maximum amount of pericardial fluid while minimizing the risk of puncturing adjacent organs.3,4
Traditionally, a subxiphoid view of the heart is the easiest window to obtain and typically provides the best view of all four chambers of the heart because the liver serves as an excellent acoustic window. If the subxiphoid approach is utilized, recognize that there is a high chance of liver puncture during the procedure.
The parasternal view of the heart can also be utilized to guide the emergent pericardiocentesis via an intercostal approach.5,6 Utilizing this approach puts the patient at risk for puncture of the left anterior descending artery or the internal mammary artery.
The apical view of the heart can be more difficult to obtain during a bedside scan but often provides unobstructed access to the pericardial sac.4,7 Once the heart is adequately visualized along the 6th-7th intercostal space at the anterior to mid-axillary line, the apical approach for a pericardiocentesis allows the operator to enter the pericardial sac without risk of injuring adjacent organs. Note that the apical approach can put patients at higher risk for accidental pleural puncture and subsequent pneumothorax.
Use the depth markers on the side of the ultrasound image to determine the needle length required to enter the pericardial space. (See Figure 1.)
Figure 1: Pericardial Effusion
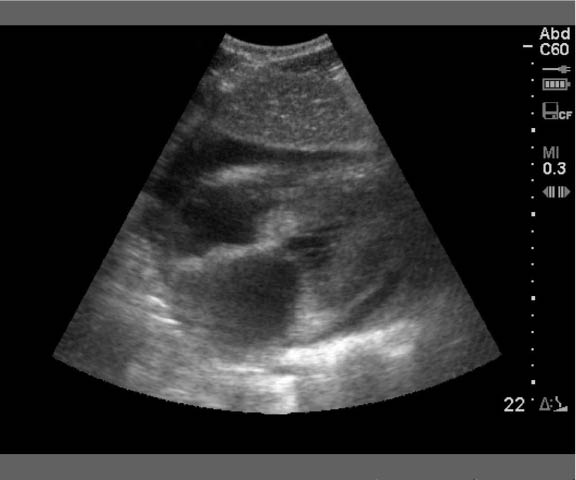
To perform the procedure, the operator will need a pericardiocentesis kit, a triple lumen central venous access kit, or a long, large-gauge needle (5-10 cm, 16-18 gauge) attached to a 3-way stopcock and saline-filled syringe.
Under ultrasound guidance, insert the needle and aim toward the pericardial sac. Gently aspirate back on the syringe as you advance the needle slowly. Monitor the needle trajectory as you aim toward the pericardial effusion. (See Figures 2 and 3.)
Figure 2: Needle Entering the Pericardial Sac, Subxiphoid Approach
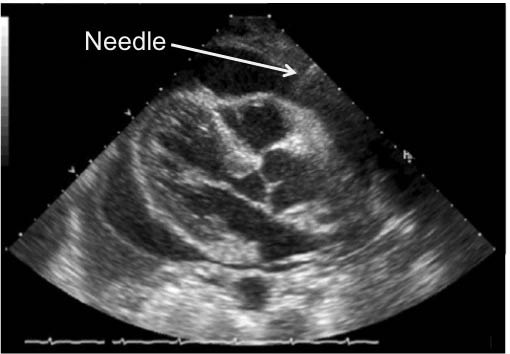
Visualizing the needle entering the pericardial sac via the subxiphoid approach
Figure 3: Needle Entering the Pericardial Sac, Apical Approach
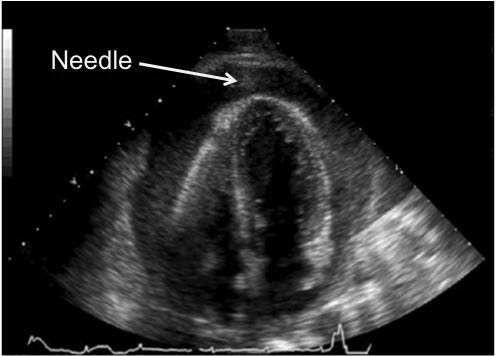
Visualizing the needle entering the pericardial sac via the apical approach
Continue applying negative pressure on the syringe until the parietal pericardium is penetrated and pericardial fluid or blood is noted in the syringe.
Once the needle tip is clearly in the pericardial space, attach a 20-60 cc syringe to the 3-way stopcock and continue fluid aspiration until the patient's blood pressure improves or until there is resolution of tamponade on ultrasound.
If with continued aspiration, fluid should stop draining and a significant pericardial effusion is still visible on ultrasound, inject 1-2 mL of normal saline as needed to flush the needle and confirm the needle tip location under direct ultrasound visualization. If the needle tip is in the pericardial space, bubbling from saline injection will be noted within the pericardial sac.
Insert a catheter into the pericardial space via the Seldinger technique to allow for continuous aspiration. If a commercial pericardiocentesis tray is not readily available, a central venous access catheter can be used as a substitute.
Pearls and Pitfalls.
Although the phased array (5-1MHz) transducer is the most common probe used during an ultrasound-guided pericardiocentesis, note that a high frequency linear transducer (10-5MHz) may give you optimal needle visualization during the apical approach. (Figure 4) Use the phased array transducer to locate the largest collection of unobstructed pericardial fluid and then switch over to the linear transducer to guide the needle during the pericardiocentesis if the fluid collection lies superficially. If a phased array transducer is not readily available, a low frequency curvilinear transducer (5-2MHz) can be manipulated in between the ribs or under the xiphoid process to visualize the heart and surrounding structures.
Figure 4: Needle Entry into Pericardial Sac Via Apical Approach
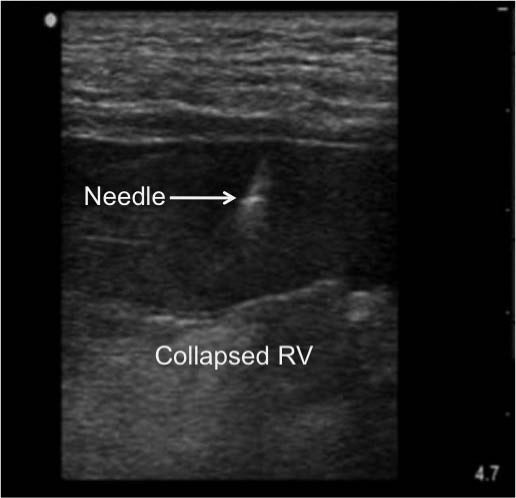
Visualizing the needle entering the pericardial sac using a linear array transducer via the apical approach
In general, obtaining a view of the needle in the long axis will optimize visualization of the needle and its trajectory throughout the entire procedure.
If you have not mastered the long-axis approach (this technique is described in the previous issue, "Basic Emergency Ultrasound-guided Procedures," Volume 32, Number 5, Feb. 14, 2011), aim the ultrasound beams so they bisect the needle tip as it punctures the skin and enters the subcutaneous tissue. Utilize tissue movement and artifacts, such as ring down, to help visualize the needle trajectory. (See Figure 7 from "Basic Emergency Ultrasound-guided Procedures," Volume 32, Number 5, Feb. 14, 2011.) You may need to fan or slide the probe away from the puncture site to maintain visualization of the needle tip as you advance the needle deeper into the patient.
Figure 5: Patient Positioning for Thoracentesis
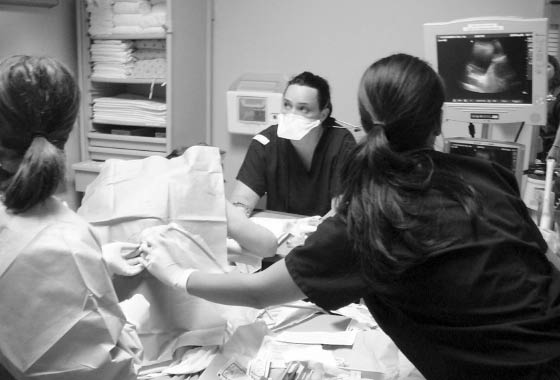
Patient positioning in a seated position for a thoracentesis via the posterior approach
Figure 6: Ultrasound Image of Lung Parenchyma Floating in a Pleural Effusion
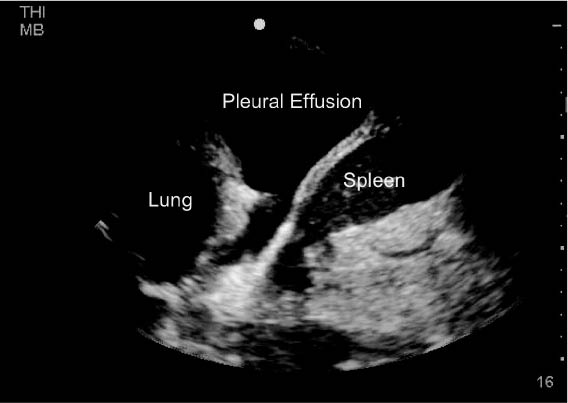
Ultrasound image of lung parenchyma floating in a pleural effusion cephalad to the diaphragm and spleen
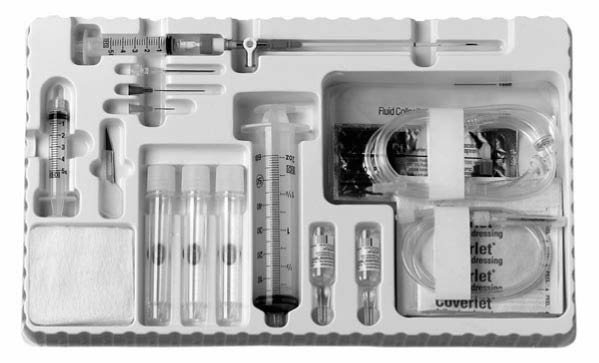
Figure 7: Thoracentesis Kit
Stroke volume of the collapsed RV increases 77% with the removal of the first 200 mL of the pericardial effusion. Remember that rapid fluid removal can cause significant hemodynamic changes from the sudden increase in left ventricular (LV) preload. These changes can result in sudden pulmonary edema, circulatory collapse, profound bradycardia, and rebound hypertension. Remove enough fluid to achieve return of spontaneous circulation and an adequate perfusing blood pressure.8
If there is time, utilize ultrasound to locate and visualize surrounding vascular structures. During the pericardiocentesis, attempt to avoid local vascular structures such as the intermammary artery, which lies 3-5 cm lateral to the sternal border, and the intercostal arteries that run along the lower rib margin.9
During the procedure, reconfirm needle or catheter placement by examining the bloody aspirate for clot. Remember that intracardiac blood will clot, whereas blood that has transmigrated into the pericardial sac will not clot because it is defibrinated. Note that traumatic effusions will have blood in the pericardial sac that originated from the ventricles. In these situations, blood in the pericardiac sac will often clot. When in doubt, inject a small amount of normal saline and visualize the anatomic distribution of the saline bubbles on bedside ultrasound.
Ultrasound-guided Thoracentesis
Indications. The pleura is a two-layered structure that surrounds the lungs. The outer layer (the parietal pleura) and the inner layer (the visceral pleura) are separated and lubricated by a small amount of pleural fluid. Pleural fluid is drained under normal circumstances by the lymphatic system, which normally removes 0.1 mL/kg/hour but has the capacity to drain as much as 3 mL/kg/hour.8 A pleural effusion develops when serous, hemorrhagic, serosanguinous, or chylous fluid accumulates in between the parietal and visceral pleura, resulting in atelectasis and increasing the risk of respiratory compromise by limiting local lung expansion. Chronic pleural effusions can provide a medium for the development of infections and adhesions.
Traditionally, auscultation, percussion, and tactile fremitus are the clinical exam tools taught to detect effusions and consolidations within the thorax. Patient habitus and the provider's skill set can limit the sensitivity and specificity of these findings. Bedside ultrasound can be used to detect the presence of a pleural effusion and determine its relative size and location in a safe and rapid manner.10
Once a pleural effusion is identified, ultrasound can also be used to guide a therapeutic or diagnostic thoracentesis. Performing the procedure under ultrasound guidance reduces the rate of complications such as accidental lung parenchymal puncture, cardiac lacerations, and splenic or liver puncture.11 If continuous pleural drainage is desired, insertion of a pigtail catheter can be done under direct ultrasound visualization to guide catheter placement.12
Contraindications. There are no absolute contraindications for using ultrasound to guide a thoracentesis attempt. Prior to performing an ultrasound-guided or landmark-guided thoracentesis, bear in mind a few precautionary recommendations. If the patient is thrombocytopenic with a platelet count < 50,000/mm3 or in a hypocoagulable state with an aPTT or PT > 2 times the normal limit, transfusion with replacement factors or blood products should be initiated prior to the thoracentesis. Patients who have a coagulation disorder or renal failure and uremic platelets should be monitored following the procedure for acute pleural fluid re-accumulation and active bleeding. Remember to avoid puncturing tissue with overlying cellulitis, herpes zoster, or other infectious lesions.13
Risks. Because the diaphragm traverses as high as the nipple line, there is potential for damage to adjacent structures in both the abdomen and the thorax. Vascular injury or accidental parenchymal puncture are the two most common complications, followed by infection, hemothorax, bronchopulmonary fistula, tension pneumothorax, splenic rupture, abdominal hemorrhage, air embolism, or unilateral pulmonary edema.8 Rapid drainage of a large volume of fluid can result in significant hypotension and re-expansion pulmonary edema. Most experts recommend limiting the volume of drainage in the acute phase to 1-1.5 liters.14
Benefits. Ultrasound can be used to provide useful clinical data in a quick and safe manner. A bedside scan of the patient's thorax can determine if a pleural effusion is truly present, can estimate the size of the effusion, and can be used to map out the optimal site for needle and catheter insertion for the greatest chance of a successful tap while minimizing complications.15
How to Perform the Procedure.
Position the patient to optimize consolidation of fluid into a dependent location. Traditionally, the patient is placed in a seated position, leaning forward, with his or her arms draped over a bedside stand or table (Figure 5). If the patient cannot tolerate this position, have the patient lie supine and elevate the head of the bed 30-45°.
Prep and drape the patient and the ultrasound transducer in a sterile fashion.
Use a 5-2MHz curvilinear transducer or a 5-1MHz phased array transducer to visualize the lung and adjacent structures. The phased array transducer has a smaller footprint and is easier to manipulate between the ribs.
Clearly identify the lung parenchyma, the pleural fluid, the diaphragm, and adjacent organs such as the liver, spleen, and heart.
Remember that the lungs and adjacent organs will have a mixed echogenic appearance on ultrasound (gray), whereas the pleural fluid will typically appear more hypoechoic, and the diaphragm will appear hyperechoic (white). (Figure 6). The pleural effusion may appear more echogenic depending on the amount of protein and inflammatory constituents present.
Map out the superior and inferior borders of the fluid collection and determine the best site to perform the thoracentesis.
Note changes in the position and depth of the pleural effusion during inspiration and expiration.
Use the depth markers on the side of the ultrasound image to determine the needle length required to tap the pleural effusion.
Use a commercially available thoracentesis kit (Figure 7) or assemble the following equipment: injection needle (25 gauge, 1.5"); 5 mL Luer lock syringe; lidocaine 1% or 2%; a long 16-18 gauge needle; 3-way stopcock; 10 mL and 60 mL Luer lock syringe; tubing set with aspiration adaptors, specimen vials, or blood tubes; drainage bag or vacuum bottle; sterile drapes or towels; no. 11 blade scalpel; tape; and 4 x 4" gauze pads.
The procedure can be performed in a static or dynamic fashion. Most experts recommend performing the procedure under real-time ultrasound guidance so that the needle trajectory and depth can be continuously monitored. This enables visualization of changes in the position of the lung parenchyma during the respiratory cycle.
After the skin and subcutaneous tissues have been properly anesthetized, insert the needle over the superior aspect of the rib to avoid damaging the neurovascular bundle that courses directly under the inferior edge of the ribs.
Under ultrasound guidance, watch the needle tip as you advance it slowly toward the pleural effusion. Gently aspirate back on the syringe as you advance. Once you have reached the pleural effusion, aspirate 5-10 mL of fluid for analysis. If a catheter is available, insert it into the pleural space via the Seldinger technique and attach the end of the catheter to the tubing set and drainage bag or vacuum bottle.
Pearls and Pitfalls.
Although the curvilinear (5-2MHz) and phased array (5-1MHz) transducers are the most common probes used during an ultrasound-guided thoracentesis, note that a high-frequency linear transducer (10-5MHz) may provide optimal needle visualization for superficial fluid collections. Map out adjacent structures with the lower-frequency transducers first, and then switch over to a higher-frequency transducer to monitor initial needle insertion.
As with most procedures, obtaining in-plane visualization of the needle is most useful in following the needle and its trajectory as you advance it deeper toward the target structure. The limited space between the ribs can make this difficult. You may find it easier to obtain a short-axis view of the needle during most thoracentesis attempts.
Aim the ultrasound beams so they bisect the needle tip as it punctures the skin and enters the subcutaneous tissue. Utilize tissue movement and artifacts, such as ring down, to help you visualize the needle trajectory. (See Figure 7, "Basic Emergency Ultrasound-guided Procedures," Volume 32, Number 5, Feb. 14, 2011.) You may need to fan or slide the probe away from the puncture site to maintain visualization of the needle tip as you advance the needle deeper into the patient.
As you drain the pleural fluid, note that the lung may expand closer and closer to the needle tip. You may need to manipulate the needle under ultrasound guidance during the procedure to prevent accidental puncture of the visceral pleura and lung parenchyma.
Insert the needle a few millimeters past the parietal pleura and withdraw 10-20 mL of fluid for analysis. Advance the thoracentesis catheter over the needle into the pleural space if therapeutic drainage is required.
If you are unsure where your needle tip is, gently inject a few mL of normal saline under direct ultrasound visualization and look for bubbling at the needle tip from the saline injection.
Do not drain more than 1.5 liters of fluid in the acute phase. Hypotension and re-expansion pulmonary edema can result from large volume drainage.
Ultrasound-guided Paracentesis
Indications. Therapeutic paracentesis is one of the oldest documented medical procedures, with cases dating back to 20 BC.8 Paracentesis can be performed for either therapeutic or diagnostic purposes. Most patients requiring a therapeutic paracentesis present with complaints of cardiorespiratory compromise from mechanical constriction or gastrointestinal manifestations such as early satiety, anorexia, sensation of fullness, nausea, vomiting, or abdominal pain. Ascitic fluid can also be drained to determine its etiology and to evaluate for infection, hemorrhage, or malignancy.
Prior to the advent of ultrasound, paracenteses were performed in a "blind" fashion via the landmark approach alone. Complications of a blind puncture include injury to the liver, spleen, stomach, intestines, urinary bladder, or major abdominal vessels. Ultrasound can be used at the beside to determine if any ascitic fluid is present and utilized during the paracentesis to guide needle insertion and catheter placement.
Contraindications. There are no absolute contraindications to using ultrasound to guide a paracentesis attempt. Prior to performing an ultrasound-guided or landmark-guided paracentesis, bear in mind a few precautionary recommendations. Many patients who require a diagnostic or therapeutic paracentesis will have liver problems, a coagulopathy, and possibly thrombocytopenia. Some studies recommend that patients with an INR > 2.0 may require transfusion with fresh frozen plasma (FFP) prior to the procedure. Similarly, patients with a platelet count < 20,000/mm3 should receive an infusion of platelets before their paracentesis.16 More recent studies suggest that transfusion is not necessary in ultrasound-guided paracenteses or when performed by experienced personnel.17,18 Do not puncture the skin if an abscess or overlying cellulitis is present. The procedure is not recommended for pregnant patients.
Risks. Performing a paracentesis without ultrasound guidance puts the patient at risk for injury to nearby structures and vessels. Using bedside ultrasound significantly reduces these risks by enabling direct visualization of adjacent organs and structures. The procedure itself carries inherent risks even with ultrasound guidance. These risks include, but are not limited to, persistent fluid leakage through the puncture site, wound infection, abdominal wall hematoma, spontaneous hemoperitoneum, post-procedural hypotension, and dilutional hyponatremia or other electrolyte changes.
Benefits. Ultrasound is considered the gold standard for detecting ascites. It is able to detect as little as 100-250 mL of free fluid in the peritoneum. With high-resolution machines, ultrasound can visualize a collection of 5-10 mL of fluid around the urinary bladder.9,19 A bedside scan of the patient's abdomen can determine if the patient does indeed have ascites, it can estimate the amount of ascites present, and can also be used to map out the optimal site for needle and catheter insertion for the greatest chance of a successful tap while minimizing complications. In a study of 100 patients randomized to either ultrasound-guided or a blinded paracentesis, 95% of the ultrasound group had successful aspiration, while only 61% of those in the blinded group had a successful tap.20 During the procedure, ultrasound guidance can be used to reposition the needle and catheter tip if drainage ceases secondary to patient repositioning, bowel wall interference, or catheter obstruction.
How to Perform the Procedure.
Have the patient empty his or her urinary bladder prior to the procedure.
Position the patient to optimize consolidation of fluid into a dependent location.
Prep and drape the patient and the ultrasound transducer in a sterile fashion.
Use a 5-2MHz curvilinear transducer or a 5-1MHz phased array transducer to visualize the liver, spleen, urinary bladder, and the floating loops of bowel. (Figure 8)
Figure 8: Ascites and Loops of Bowel
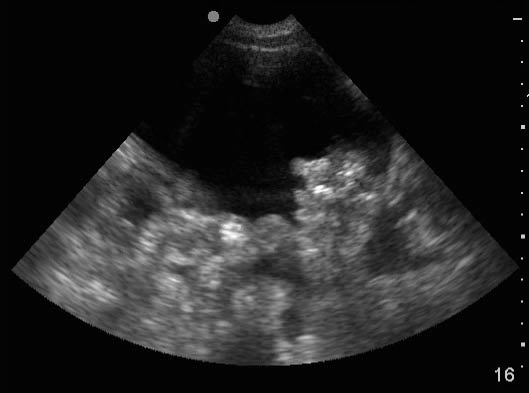
Ultrasound image of loops of hyperechoic bowel floating in anechoic ascitic fluid.
Scan around the abdomen until you find a spot where there is a large collection of ascitic fluid away from adjacent organs and structures. Traditionally, the left or right mid to lower quadrants are accessed via ultrasound guidance.
Anesthetize the skin and subcutaneous tissue at the chosen site with a small amount of local anesthetic (e.g., lidocaine 1% or 2% with epinephrine).
Use ultrasound guidance to determine the trajectory of the needle.
Use the "Z technique" when inserting the needle to reduce the risk of post-procedure fluid leakage and development of iatrogenic peritonitis. Begin by pulling the skin down before you puncture the epidermis and dermis with the needle. Release the skin and then continue to insert the needle through the subcutaneous tissue and fat and into the peritoneum.
Gently aspirate back on the syringe as you advance the needle slowly. Continue to monitor the needle tip on bedside ultrasound. Once ascitic fluid is successfully aspirated back into the syringe, use ultrasound guidance to ensure that the needle tip is in the midpoint of the fluid collection and a safe distance away from floating loops of bowel.
Advance the catheter over the needle or insert a catheter via the Seldinger technique. Note that you may need to make a small nick in the skin and subcutaneous tissue to advance the catheter into the peritoneal cavity.
Collect the desired amount of ascitic fluid for diagnostic analysis and therapeutic relief of symptoms.
Pearls and Pitfalls.
For every 1 cm of fluid visible around the loops of bowel, there is likely 1 L of ascitic fluid that can be drained.21
Draining more than 6 L of fluid at a time puts the patient at risk for third-spacing and hypotension.
As with most procedures, obtaining an in line view of the needle will allow optimal visualization of the needle and its trajectory as you advance it into the peritoneal space. Be cautious of bowel that might float just outside of your narrow long-axis view. Obtaining an oblique view of the needle as it enters the peritoneal cavity can maximize visualization of the needle and surrounding structures.
As you drain the pleural fluid, note that the loops of bowel may move closer to your needle tip. You may need to manipulate the needle under ultrasound guidance during the procedure to prevent accidental puncture of the bowel.
If fluid stops draining during the procedure, use ultrasound to determine if a loop of bowel has been siphoned against the catheter tip. Gentle injection of a few mL of normal saline can determine where the catheter tip lies, can clear any small clots in the catheter ports, and can help dislodge bowel wall that may have been suctioned against the catheter tip.
Ultrasound-guided Lumbar Puncture
Indications. Adults have approximately 140 mL of cerebrospinal fluid (CSF), with 25% of that volume contained in the spinal canal. With an average production rate of 0.35 mL/min, the amount of fluid removed during a typical lumbar puncture can be regenerated in about an hour. Because the spinal canal portion of the CSF is continuous with the cranial portion, contents are considered homogeneous throughout, and can be examined for signs of bleeding, infection, or inflammatory markers. A sample of the CSF can be safely obtained at the level of the cauda equina, via hollow-needle cannulation of the spinal canal with minimal risk to neurologic or vascular structures.
The most common reasons for CSF analysis are for the evaluation of suspected meningitis or subarachnoid hemorrhage. Less common reasons include analysis for idiopathic intracranial hypertension (or pseudotomor cerebri), tertiary syphilis, demyelinating diseases, or other inflammatory processes of the central nervous system (CNS). Traditionally, a lumbar puncture is performed using the landmark approach to approximate the location of the L4-L5 interspinous space. Ultrasound can be used at the bedside to map out the interspinous spaces and help guide the lumbar puncture.
Contraindications. There are no absolute contraindications to using ultrasound to guide a lumbar puncture attempt. Prior to performing an ultrasound-guided or landmark-guided lumbar puncture, bear in mind a few precautionary recommendations. Avoid puncturing through skin with overlying cellulitis, herpes zoster, or other signs of infection. Relative contraindications to performing a lumbar puncture include elevated intracranial pressure or space-occupying CNS mass lesion. Be cautious in patients who are unable to cooperate with the procedure. Procedural sedation may be required.
Risks. Performing a lumbar puncture without ultrasound guidance puts the patient at risk for injury to nearby structures and vessels. Using bedside ultrasound significantly reduces these risks by enabling direct visualization of the interspinous space and minimizing the number of unsuccessful attempts.22,23 Note that performing a lumbar puncture carries inherent risks even with ultrasound guidance. These risks include, but are not limited to, accidental puncture of nerves, blood vessels, and adjacent bones and organs.
Benefits. Obesity, pregnancy, scoliosis, previous spinal surgery, and generalized edema can make it difficult to perform a lumbar puncture based on the traditional landmark approach. Even in patients with clearly palpable landmarks, studies have demonstrated clinician error in correctly identifying vertebral and interspace level by the palpation technique alone.24 Ultrasound can be used at the bedside to localize the spinous processes and the best interspinous space to perform the procedure. Studies have repeatedly shown that ultrasound guidance results in improved landmark identification, resulting in fewer attempts to successfully obtain a CSF sample.22,23,25-27
How to Perform the Procedure.
Position the patient in a seated position, leaning forward, with his or her arms and head resting on a bedside table. If an opening pressure is to be measured, have the patient lie in a lateral decubitus position with the head and legs tucked toward the patient's umbilicus.
In most patients, the procedure can be performed with a high-frequency linear array transducer (13-5MHz). In patients with overlying edema or obesity, you may need a lower-frequency 5-2MHz curvilinear transducer to optimally visualize the spinous processes and interspinous space.
Prep and drape the patient and the ultrasound transducer in a sterile fashion.
Start by scanning with the probe in a transverse fashion at the level of the iliac crests, perpendicular to the long axis of the patient's spine. (Figure 9)
Figure 9: Transverse Probe Placement for LP
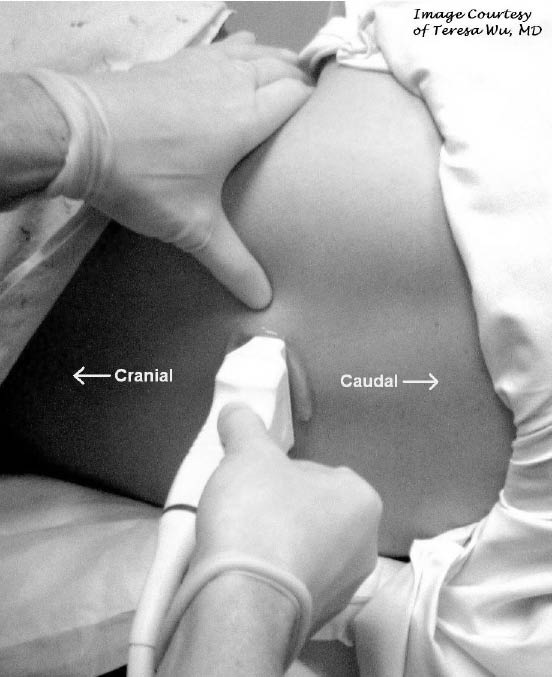
Defining midline by scanning in a transverse fashion perpendicular to the long axis of the spine
Scan from the patient's left to right until you find a spinous process. In this view, the spinous process will appear as a bright white, hyperechoic object casting a dark shadow far-field across the screen. (See Figure 10.)
Center the spinous process in the middle of the ultrasound screen. When the spinous process shadow is visualized in the middle of the screen, the corresponding spinous process is centered directly under the middle of the probe.
Use a sterile marker to identify this point as midline on the patient's back.
Scan and identify two more adjacent spinous processes. Extend a short line from cephalad to caudad, connecting the adjacent spinous processes you just mapped out. This will clearly outline the patient's spinal curvature and distinguish midline on the patient's back.
Once midline has been demarcated, rotate the transducer 90° so that it lies parallel to the spine. (Figure 11) Scan along the line demarcating midline along the patient's back.
Figure 11: Longitudinal Probe Placement for LP
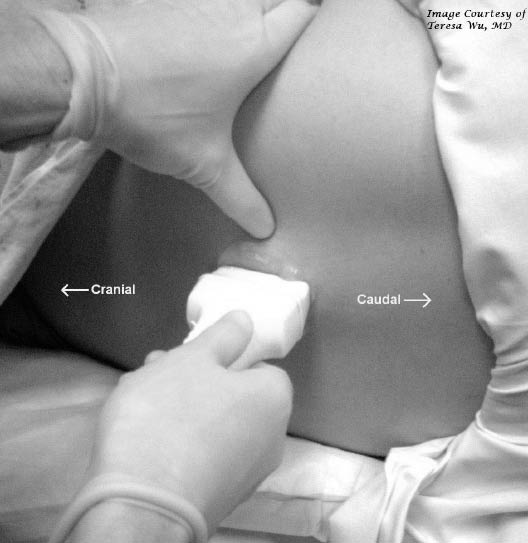
Scanning the spinous processes in a longitudinal fashion along the patient's midline
Figure 10: Spinous Process in a Transverse View
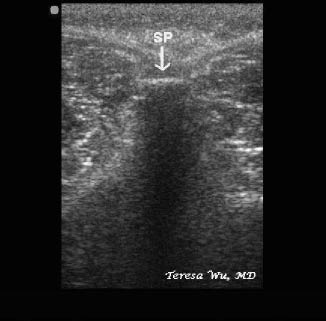
Ultrasound image of the spinous process in a transverse view of the spine
The spinous processes in this view will appear as hyperechoic curves casting dark shadows farfield to the transducer. (Figure 12)
Figure 12: Longitudinal View of Spinous Processes
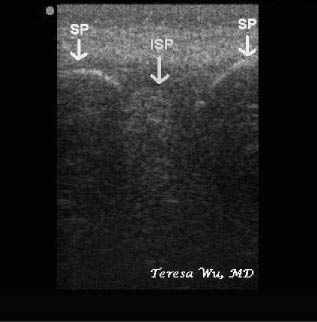
Longitudinal view of two adjacent spinous processes (SP) and the interspinous space (ISP)
Center the transducer over the spinous processes and try to capture two spinous processes simultaneously on the screen. Scan from cephalad to caudad along the midline until the interspinous space is in the middle of the screen.
Identify this spot with a marker or use a needle cap to gently indent the skin at this point. Use the sterile marker to draw a line across the patient's back at the level of the interspinous space, perpendicular to the probe.
Remove the ultrasound probe and note that the interspinous space lies directly under where the two lines intersect. (Figure 13)
Figure 13: LP Lines Cross Section
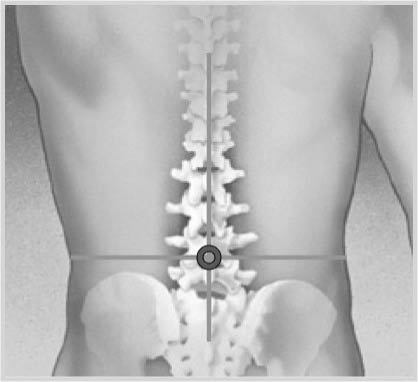
Insert your spinal needle where the two lines intersect along the patient's midline directly over the interspinous space.
Proceed with the lumbar puncture by directing the spinal needle toward the interspinous space identified.
An ultrasound-guided LP can be performed in a static or dynamic manner, depending on the number of personnel available to help with the procedure. Note that it is difficult to advance the spinal needle with one hand and hold the ultrasound probe with the other hand. If an assistant is available to hold the ultrasound probe in place, the procedure can be performed under direct ultrasound guidance in a dynamic fashion.
Pearls and Pitfalls.
Practice using ultrasound guidance to localize spinous processes on thin patients who are devoid of much subcutaneous fat first. Learning how to visualize the landmarks on thinner patients will maximize your chances of success when ultrasound guidance is required.
Many newer ultrasound machines have the capability and resolution to pick up the bright white, hyperechoic ligamentum flavum, which lies deep to the spinous processes and just superficial to the epidural space. If you are able to identify the ligamentum flavum during your scan, you can estimate the length of needle required to puncture through the ligamentum flavum into the spinal canal.
When attempting to visualize two adjacent spinous processes on the longitudinal view of the spine, start with the probe directly over the patient's midline. You may need to manipulate the cephalad or caudad portion of the probe by just a few millimeters to align both spinous processes on the screen simultaneously.
In the longitudinal view, it is important to keep the probe directly over midline. If you scan off to the side, you may visualize the adjacent transverse processes and mistake them as spinous processes.
Ultrasound-guided Regional Anesthesia
Indications. Regional anesthesia can be used during the reduction of fractures or dislocations, wound exploration, abscess drainage, laceration repair, minor surgical procedures, or to help ease localized pain (e.g., acute rib fractures, burns, etc.).28-30 Nerve blocks are traditionally performed using the landmark technique alone. The needle is inserted at a site that approximates the nerve location and course based on palpation and recognition of external anatomical landmarks. As technology has advanced, clinicians have discovered that they can use bedside ultrasound to visualize and localize the target nerve bundle and adjacent anatomical structures and vessels.29 Visualizing the target nerve and performing a nerve block under direct ultrasound guidance maximizes the chances of successfully infiltrating anesthesia around the nerve and minimizes the risk of neurovascular injury.29-31
Contraindications. There are no absolute contraindications to performing an ultrasound-guided nerve block, but there are some contraindications to performing the regional block itself. Before proceeding with the procedure, ensure that the patient does not have a compartment syndrome, ensure that he or she does not have an allergy to the chosen anesthetic, and that the target nerve is superficial enough to be accessed and anesthetized. Be careful when performing the procedure on patients who are coagulopathic. Do not puncture through skin that has overlying cellulitis, an abscess, or other signs of infection.
Risks. Knowledge of the local anatomy is essential for performing the procedure. During the nerve block, patients are at risk for infiltration of anesthetic around the incorrect target nerve, vascular infiltration or injury, hematoma formation, ecchymosis, laceration of the target nerve, pain, or ineffective blockade. Patients are also at risk for local and systemic reactions to the anesthetic being utilized. Prior to performing a nerve block, it is prudent to determine if regional anesthesia will alter the patient's care after initial evaluation and management in the ED. When necessary, it is helpful to coordinate management options with requisite consultants to determine the timing and type of nerve block administered.
Benefits. Ultrasound guidance minimizes the risk of nerve laceration or vascular injury. Direct ultrasound guidance maximizes chances of successfully bathing the nerve and achieving a regional block.
How to Perform the Procedure.
Place the patient in a position of comfort.
Common sites for ultrasound-guided regional anesthesia include supraclavicular brachial plexus, infraclavicular brachial plexus, interscalene brachial plexus, axial brachial plexus, intercostal nerves, femoral nerve, sciatic nerve, popliteal nerve, saphenous nerve, radial nerve, median nerve, and ulnar nerve.
In the emergency department, extremity nerve blocks are the most common ones performed.32-34
Use the highest frequency linear array transducer available (13-10 MHz) if you are planning to anesthetize superficial nerve bundles. For deeper nerves, use the 5-2MHz curvilinear probe.
Assemble the needle of choice (insulated nerve block needles, long spinal needle, or shorter standard needles).
Prep and drape the patient and the ultrasound transducer in a sterile fashion.
Apply a copious amount of gel over the target area. Sterile packets of Surgilube® work well if other commercially available ultrasound gel packets are not readily available.
Turn down the overall gain of your image. The adjacent muscle should appear dim and dark compared to the hyperechoic nerve fibers coursing around them.
Remember that most nerves will course in between distinct muscular junctions. Use ultrasound to delineate muscle borders and the intermuscular space.
Look for your target nerve in the transverse fashion first. The proximal nerve bundle will appear as a honeycomb in cross-section. The hypoechoic componenets are the nerves themselves, surrounded by hyperechoic connective tissue. (See Figure 14.)35,36
Figure 14: Cross Sectional View of Median Nerve
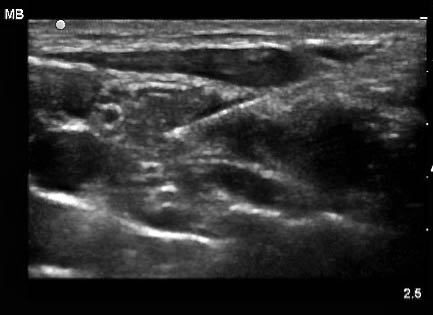
Cross sectional view of a hyperechoic needle approaching the median nerve. Note the honeycomb appearance of the hypoechoic nerves surrounded by hyperechoic connective tissue.
Note that tendons and nerves will appear very similar on ultrasound. When in doubt, trace the target structure with the probe and determine if it merges into a muscle proximally. Typically, tendons will eventually dive into a muscle, whereas nerves will course along the periphery.
Once you have located the target nerve in the transverse fashion, obtain a longitudinal view of the nerve.
In the long axis, a nerve will demonstrate internal echotexture consisting of continuous hypoechoic longitudinal elements (fascicle groups) interspersed with hyperechoic perineural connective tissues.
Once the target nerve has been localized, the region around it can be anesthetized with ultrasound guidance via the long-axis approach.
Insert the needle under the ultrasound probe and aim the needle tip at the target nerve. Before puncturing the nerve, inject the desired amount of local anesthetic to bathe the nerve completely. (See Figure 14.)
Figure 15: Ultrasound of a Normal Eye

Ultrasound image of a normal eye
Look for nerve sheath distension with hypoechoic fluid during anesthetic infiltration.
Scan proximally and distally along the target nerve to determine the extent of anesthetic spread.
Specific Nerve Blocks Commonly Used in the Emergency Department.
In the ED, regional anesthesia of the extremities is performed much more often than other types of nerve blocks.
For example, it is often useful to perform an ulnar, radial, or median nerve block to explore a large hand wound, perform a laceration repair, or reduce a fracture
To anesthetize the ulnar nerve, identify the flexor carpi ulnaris and ulnar artery via ultrasound just proximal to the wrist crease. Remember that the flexor carpi ulnaris is the most medial tendon on the volar surface of the wrist with the hand in a supine position. The ulnar artery can be visualized just medial and dorsal to the tendon.
Anesthetize the ulnar nerve that lies between the ulnar artery and flexor carpi ulnaris tendon.
To anesthetize the median nerve, identify the flexor carpi radialis and palmaris longus tendons with ultrasound just proximal to the wrist crease. The median nerve can be visualized in between the palmaris longus and the flexor carpi radialis.
Anesthetize the median nerve at this site, remembering that the palmar branch of the median nerve is very superficial and may not be visible on bedside ultrasound.
To anesthetize the superficial radial nerve, it may be necessary to use an acoustic standoff pad to help visualize the nerve bundle. The radial nerve courses just above the styloid process of the radius in between the extensor palmaris brevis and longus tendons. Use ultrasound to help guide anesthetic injection in between the tendons just proximal to the anatomic snuff box.
Femoral nerve blocks are also routinely used to aid in pain management of lower extremity injuries.
Place the probe just below the inguinal ligament and locate the femoral artery and vein, the fascia iliaca, and the iliopsoas muscle. You should be able to visualize the femoral nerve coursing deep to the fascia iliaca and superficial to the iliopsoas muscle.
Using in-plane visualization, anesthetize the femoral nerve via a lateral approach. Note that you may see quadriceps twitching when the needle comes in contact with the nerve bundle.
Pearls and Pitfalls.
Although you may not be able to visualize some of the smaller nerve bundles on ultrasound, you can use ultrasound guidance to localize adjacent anatomical structures to help you map out the course of the target nerve.
Make sure you localize adjacent vascular structures that need to be avoided during the procedure.
Aim the ultrasound beams so they bisect the needle tip as it punctures the skin and approaches the target nerve. Utilize tissue movement and artifacts such as ring down to help you visualize the needle trajectory. (See Figure 7, "Basic Emergency Ultrasound-guided Procedures," Volume 32, Number 5, Feb. 14, 2011.) You may need to fan or slide the probe away from the puncture site to maintain visualization of the needle tip as you advance the needle deeper into the patient.
Note that lymph nodes can also look similar to nerve bundles in the transverse plane. When in doubt, trace the structure proximally and distally. Lymph nodes will be small, discrete nodules that terminate within a couple of centimeters, whereas nerves can be traced contiguously proximally and distally from the target site.
Emergency Ocular Ultrasonography
Indications. Bedside ocular sonography has been shown to be very useful in the evaluation and detection of ophthalmologic conditions such as retinal detachment, vitreous hemorrhage, lens dislocation, retrobulbar hematoma, globe rupture, and detection of ocular foreign bodies. Ultrasound can also be used to assess the optic nerve diameter as a marker for increased intracranial pressure. During an evaluation of the eye, consider using ultrasound as an adjunct to your physical examination.
Because it is a fluid-filled structure, the eye is remarkably easy to scan. The normal globe is an oblong structure that is roughly 23.5 mm high and 24 mm deep. It is separated into an anterior chamber, which consists of the lens and cornea, and a posterior chamber, which includes the vitreous body, the retina, and the choroid layers bound by the sclera. The anterior and posterior chambers are separated from each other by the iris. Behind the posterior globe, the hypoechoic optic nerve can also be visualized and evaluated for any abnormalities. In patients for whom a thorough ocular examination cannot be completed, bedside ocular ultrasonography can provide very useful diagnostic information.
Contraindications. There are no absolute contraindications to performing a bedside ocular ultrasound. Note that a water-based, non-irritating ultrasound gel should be utilized to examine the globe. If a globe rupture is suspected, care must be taken to minimize the amount of pressure placed on the globe during the scan. Applying a copious amount of gel, using an acoustic sound-off pad, or utilizing an ocular ultrasound shield can help minimize the amount of pressure applied.
Risks. Few studies are available evaluating the risks of prolonged exposure of the aqueous and vitreous humor to high-frequency sound waves. In 2001, Silverman and colleagues evaluated the effects of 30 minutes of exposure to a very high frequency (50MHz) scan of the cornea and lens of rabbits. They found no tissue changes on slit lamp or light microscopy in their study population.37 Other human studies have shown small rises in intraocular temperature with high-frequency pulsed Doppler scans.38 Because the literature is scant on this topic, it is prudent to minimize the amount of exposure by limiting the duration of the scan as much as possible. Patients should be instructed to keep their eyes closed for the duration of the scan. Inadvertent ocular exposure to ultrasound gel can cause some mild conjunctival irritation.
Benefits. Patients may present with eyelid edema, photophobia, confusion, pain, or cooperation issues that preclude a thorough and complete ocular and fundoscopic exam. Bedside ultrasound can provide useful diagnostic data in a safe and efficient manner. In addition to evaluating intraocular structure, bedside ultrasound can be used to assess for swelling or fluid-filled collections around or behind the globe.
How to Perform the Procedure.
Place the patient in a position of comfort.
Use a clean, high-frequency, linear array transducer (13-5MHz).
Instruct the patient to keep his or her eyelid closed for the duration of the entire procedure.
Apply a copious amount of gel over the patient's closed eyelid.
Turn up the gain on the ultrasound machine. Increasing the gain will brighten the image at the expense of resolution, but will allow you to see subtle ocular abnormalities like small hemorrhages or detachments.
Float the probe gently over the gel on top of the patient's eyelid. Hold the probe with your first, second, and third digits while using your fourth and fifth fingers to stabilize your hand on the patient's face and forehead.
Adjust the depth of the image on the ultrasound screen so that you can visualize the entire globe. (See Figure 15.)
Assess the globe for symmetry and systematically evaluate each portion of the eye. Determine if the lens is in the proper location just behind the iris. Evaluate the vitreous body for any hyperechoic artifacts or echogenic material floating in the posterior chamber that may suggest a vitreous hemorrhage. (See Figure 16.)
Figure 16: Vitreous Hemorrhage
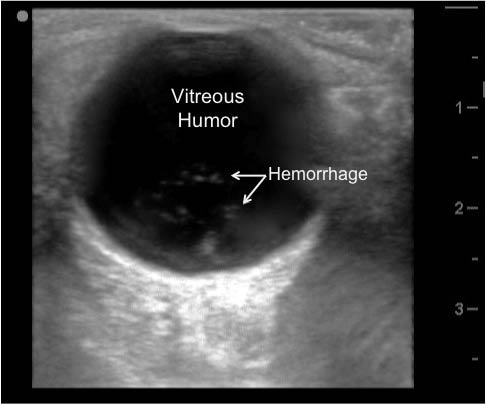
Ultrasound image of echogenic material in the vitreous humor suggesting a vitreous hemorrhage.
An acute vitreous hemorrhage will appear as speckled, hyperechoic material floating in the vitreous humor. Have the patient look in all four directions with the eyelid closed. You will see swirling of the vitreous hemorrhage within the posterior chamber.
As the hemorrhage ages, it will appear more like a "cobweb" secondary to blood coagulation and membrane formation. Older vitreous hemorrhages may not be as mobile under dynamic visualization.
Evaluate the retina for any signs of detachment. When the retina detaches from the retinal pigment epithelium and choroid, it can be seen as a thin, hyperechoic, floating membrane on bedside ultrasound. (See Figure 17.) When the patient moves the eye, the membrane will undulate within the vitreous humor.
Figure 17: Detached Retina
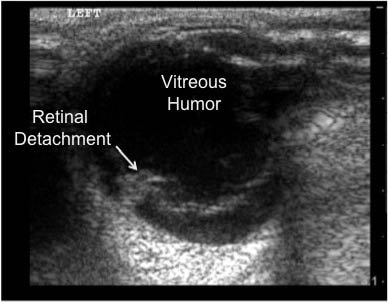
Ultrasound image of the thin, hyperechoic retinal membrane detached and floating in the vitreous humor.
If a foreign body is suspected, scan through the anterior and posterior chambers and the surrounding tissue. Remember that foreign bodies can be very difficult to visualize directly on ultrasound and you may need to infer their presence by looking for acoustic shadowing far-field to the suspected object.39,40
Once you have evaluated the globe, increase the depth of the scan to evaluate the region and structures posterior to the orbit.
If the patient has a retrobulbar hematoma, it will appear as a dark, anechoic or hypoechoic structure just posterior to the orbit. (See Figure 18.) Hematomas will become less hypoechoic and less distinct as they mature. Older hematomas may blend into the echogenicity of the surrounding tissue.
Figure 18: Retrobulbar Hematoma
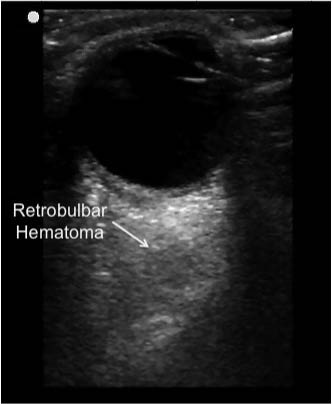
Ultrasound image of a dark, hypoechoic retrobulbar hematoma visualized behind the orbit.
Find the optic nerve that runs perpendicular to the posterior retina. Measure the optic nerve diameter 3 mm behind the globe. (See Figure 19.) The normal optic nerve diameter is < 5 mm in adults, < 4.5 mm in children older than 1 year of age, and < 4 mm in children younger than 1 year of age.41 Increased optic nerve diameter has been associated with increased intracranial pressures.42
Figure 19: Dilated Optic Nerve Sheath
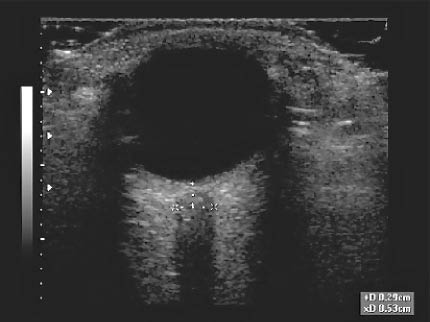
Measuring the optic nerve diameter of a dilated optic nerve sheath 3 mm behind the globe. Note the dilated optic nerve sheath at 5.3 mm.
Ultrasound can also be used to diagnose a globe rupture at the bedside.43 Gently float the transducer over a bed of gel applied over the patient's closed and swollen eyelid. Look for a flattened or irregular anterior chamber, scleral buckling around the edges, or hyperechoic blood mixed with the vitreous humor in the posterior chamber. (See Figure 20.)
Figure 20: Ruptured Globe
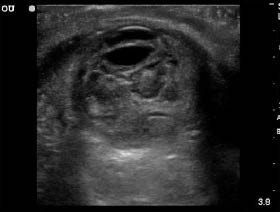
Ultrasound image of a globe rupture. Note the irregular shaped and flattened anterior chamber and buckling of the sclera along the perimeter of the eye.
Once you have finished scanning the patient's orbit, wipe off the remaining gel with a warm, wet washcloth and evaluate the eye for any signs of irritation after the scan.
Pearls and Pitfalls.
Bedside ultrasound can provide extremely useful data when a comprehensive ocular and fundoscopic exam is difficult to obtain.
Minimize the amount of pressure applied to the orbit at all times.
Most ocular ultrasounds should be performed with the transducer oriented in a horizontal or transverse fashion across the patient's eye. Prominent frontal bones can preclude optimal probe contact and subsequent visualization of the orbit in the vertical or longitudinal orientation.
Measuring the optic nerve diameter is a quick and noninvasive way to assess for increased intracranial pressure. Record the average of multiple measurements taken of the optic nerve sheath where the wall of the optic nerve is visualized best. This is typically at 3 mm posterior to the globe.
Conclusion
Bedside ultrasound provides a safe, inexpensive, and efficient way of analyzing patient anatomy and mapping out the best course to proceed with various procedures. In trained hands, ultrasound can be used to maximize the chances of success while minimizing the inherent risks involved with any procedure. Prior to performing any invasive procedure, utilize bedside ultrasound to map out the target structure and all of the adjacent organs and vessels that should be avoided. With ultrasound guidance, you can improve patient satisfaction, decrease the time required to successfully perform a procedure, and minimize complications.
References
1. Pepi M, Muratori M. Echocardiography in the diagnosis and management of pericardial disease. J Cardiovasc Med 2006;7(7):533-544.
2. Tsang TS, Oh JK, et al. Diagnostic value of echocardiography in cardiac tamponade. Herz 2000;25(8):734-740.
3. Vayre F, Lardoux H, et al. Subxiphoid pericardiocentesis guided by contrast two-dimensional echocardiography in cardiac tamponade: Experience of 110 consecutive patients. Eur J Echocardiogr 2000;1(1):66-71.
4. Ozer HO, Davutoglu V, et al. Echocardiography-guided pericardiocentesis with the apical approach. Turk Kardiyol Dern Ars 2009;37(3):177-181.
5. Choo TL, Wong KY, Chen CK, et al. Successful drainage of a traumatic haemopericardium with pericardiocentesis through an intercostal approach. Emerg Med Australas 2010;22(6):565-567.
6. Tsang TS, Freeman WK, Barnes ME, et al. Rescue echocardiographically guided pericardiocentesis for cardiac perforation complicating catheter-based procedures. The Mayo Clinical Experience. J Am Coll Cardiol 1998;32(5):1345-1350.
7. Levitov A, Mayo PH, Slonim, H. Critical Care Ultrasonography. McGraw-Hill, 2009: 317-320.
8. Roberts JR, Hedges JR, et al. Clinical Procedures in Emergency Medicine. Philadelphia, PA, W.B. Saunders. 2004:171-186, 305-322, 552-590, 841-859, 1197-1222, 1371-1392.
9. Ma OJ, Mateer JR. Emergency Ultrasound. NY, NY, McGraw Hill. 2008;449-462, 495-552.
10. Rozycki GS, Pennington SD, et al. Surgeon-performed ultrasound in the critical care setting: Its use as an extension of the physical examination to detect pleural effusion. J Trauma 2001:50(4):636-642.
11. Jones PW, Moyers JP, et al. Ultrasound-guided thoracentesis: Is it a safer method? Chest 2004:123(2):418-423.
12. Liu YH, Lin YC, et al. Ultrasound-guided pigtail catheters for drainage of various pleural diseases. Am J Emerg Med 2010:28(8):915-921.
13. Mayo PH, Goltz HR, et al. Safety of ultrasound-guided thoracentesis in patients receiving mechanical ventilation. Chest 2004:125(3):1059-1062.
14. Josephson T, Nordenskjold CA, Larsson J, et al. Amount drained at ultrasound-guided thoracentesis and risk of pneumothorax. Acta Radiol 2009;50(1):42-47.
15. Feller-Kopman D. Therapeutic thoracentesis: The role of ultrasound and pleural manometry. Curr Opin Pulm Med 2007:13(4):312-318.
16. Runyon BA. Paracentesis of ascitic fluid. A safe procedure. Arch Intern Med 1986:146(11):2259-2261.
17. Lin CH, Shih, FY, Ma MH, et al. Should bleeding tendency deter abdominal paracentesis? Dig Liver Dis 2005;37(12):946-951.
18. Grabau CM, Crago SF, Hoff LK, et al. Performance standards for therapeutic abdominal paracentesis. Hepatology 2004;40(2):484-488.
19. Von Kuenssberg JD, Stiller G, Wagner D. Sensitivity in detecting free intraperitoneal fluid with the pelvic views of the FAST exam. Am J Emerg Med 2003;21(6):476-478.
20. Nazeer SR, Dewbre H, et al. Ultrasound-assisted paracentesis performed by emergency physicians vs. the traditional technique: A prospective, randomized study. Am J Emerg Med 2005:23(3):363-367.
21. Irshad AS, Ackerman J, et al. Can the smallest depth of ascitic fluid on sonograms predict the amount of drainable fluid? J Clin Ultrasound 2009:37(8):440-444.
22. Strony R. Ultrasound-assisted lumbar puncture in obese patients. Crit Care Clin 2010;26(4):661-664.
23. Nomura JT, Leech SJ, Shenbagamurthi S, et al. A randomized controlled trial of ultrasound-assisted lumbar puncture. J Ultrasound Med 2007;26(10):1341-1348.
24. Furness G, et al. An evaluation of ultrasound imaging for identification of lumbar intervertebral level. Anesthesia 2002;57:277-280.
25. Stiffler KA, Jwayyed S, et al. The use of ultrasound to identify pertinent landmarks for lumbar puncture. Am J Emerg Med 2007:25(3):331-334.
26. Ferre RM, Sweeney TW, et al. Ultrasound identification of landmarks preceding lumbar puncture: A pilot study. Emerg Med J 2009;26(4):276-277.
27. Ferre RM, Sweeney TW. Emergency physicians can easily obtain ultasound images of anatomical landmarks relevant to lumbar puncture. Am J Emerg Med 2007;25(3):291-296.
28. Abrahams MS, Horn JL, Noles LM, et al. Evidence-based medicine: Ultrasound guidance for truncal blocks. Reg Anesth Pain Med 2010;35(2):S36-S42.
29. Walker KJ, McGrattan K, Aas-Eng K, et al. Ultrasound guidance for peripheral nerve blockade. Cochrane Database Syst Rev 2009;7(4):CD006459.
30. Shah M, Blackmore M. The role of ultrasound in regional anesthesia. Br J Hosp Med 2010;71(12):718-727.
31. Orebaugh Sl, Williams BA, Vallejo M, et al. Adverse outcomes associated with stimulator-based peripheral nerve blocks with versus without ultrasound visualization. Reg Anesth Pain Med 2009;34(3):251-255.
32. Otto L, et al. Feasibility of forearm ultrasonography-guided nerve blocks of the radial, ulnar, and median nerves for hand procedures in the emergency department. Ann Emerg Med 2006;48(5):558-562.
33. Redborg KE, et al. Ultrasound improves the success rate of a tibial nerve block at the ankle. Reg Anesth Pain Med 2009;34(3):256-260.
34. Stone MB, Price D, Wang R. Ultrasound guided supraclavicular block for the treatment of upper extremity fractures, dislocations, and abscesses in the ED. Am J Emerg Med 2007;25(4):472-475.
35. Bianchi S, Martinoli C. Ultrasound of the Musculoskeletal System. Springer Berlin Heidelberg, New York. 2007;97-103.
36. Beekman R, Visser LH. High resolution sonography of the peripheral nervous system: A review of the literature. Eur J Neurol 2004;11:305-314.
37. Silverman RH, Lizzi FL, Ursea BG, et al. Safety levels for exposure of cornea and lens to very high-frequency ultrasound. J Ultrasound Med 2001;20(9):979-986.
38. Cucevic V, Brown AS, Foster FS. Thermal assessment of 40 MHz pulsed Doppler ultrasound in human eye. Ultrasound Med Biol 2005;31(4):565-573.
39. Jurgens C, Geitz W, Tost FH. Use of high frequency ultrasound for foreign body imaging in chronic conjunctivitis due to microtrauma. Klin Monbl Augenheilkd 2008;225(7):660-662.
40. Vander JF, Gault JA. Ophthalmology secrets. Mosby, New York. 2007;40-46.
41. Kimberly HH, Shah S, Marill K, Noble V. Correlation of optic nerve sheath diameter with direct measurement of intracranial pressure. Acad Emerg Med 2008;15(2):201-204.
42. Tsung JW, Blaivas M, Cooper A, et al. A rapid noninvasive method of detecting elevated intracranial pressure using bedside ocular ultrasound: Application to 3 cases of head trauma in the pediatric emergency department. Pediatric Emerg Care 2005;21(2):94-98.
43. Wu TS, Dommer P, Pearson TC. Trauma patient with right eye pain and swelling. Ann Emerg Med 2010. [Epub ahead of print].
You are nearing the end of a busy shift in your emergency department (ED) when pre-hospital providers arrive with your next patient. They bring in a 69-year-old male with a chief complaint of headache and chest pain. Emergency medical services (EMS) activated him as a "code STEMI" in the field. He is hypertensive, diaphoretic, and complaining of a headache and chest pain on arrival.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
