Childhood Upper Extremity Trauma
Childhood Upper Extremity Trauma
Authors:
Ademola Adewale, MD, FAAEM, Assistant Program Director and Director of Research, Florida Hospital Emergency Medicine Residency Program, Orlando.
Michelle L. Rorich, DO, MBA, PGY-3 Resident, Florida Hospital Emergency Medicine Residency Program, Orlando.
Peer Reviewer:
Steven M. Winograd, MD, FACEP, New York Community Hospital, ED Attending, New York–Presbyterian Healthcare System, Weill Medical College of Cornell University.
Upper extremity injuries are common in childhood and typically present to the emergency department (ED) for acute management. The clinician must recognize the differences between injuries in the child and the adult, including anatomic and physiologic differences that alter injury patterns and affect management. Early recognition of the subtle variations in pediatric radiographic interpretation may facilitate management and impact outcome. The authors review common pediatric fractures and management.
The Editor
Introduction
Musculoskeletal injuries account for approximately 10-15% of all childhood injuries, with most occurring as a result of a fall, sports-related injury, motor vehicle trauma, or intentional physical abuse.1 In reviewing the most common orthopedic upper extremity injuries, it is important that the clinician have a strong clinical understanding of the significant differences between the adult and pediatric musculoskeletal system. The pediatric musculoskeletal system is constantly maturing and is composed of more cartilage and collagen than in adults. This inherent quality renders the bone more porous and, thus, easily bendable, resulting in minimal propagation of fractures, and the abundance of cartilage improves resilience, leading to more bowing, buckle, and greenstick injuries.1,2 (See Table 1.) Also unique to the immature musculoskeletal system is the presence of growth plates and their respective injuries.
Table 1. Fractures Unique to Children
|
Fracture |
Description |
|
Physeal fractures |
Fracture occurring at the growth plate |
|
Torus fractures/buckle fracture |
Compressive load causing buckling of cortex |
|
Greenstick fractures |
Incomplete fracture in which cortex remains intact on one side |
|
Bowing fractures/plastic deformity |
Bending fracture that exhibits bowing without disruption of periosteum |
The growth plate is essentially a transition zone, termed the physis or physeal plate, between the metaphysis and epiphysis. A rapidly changing metabolic area of the skeletal system that facilitates bone growth and remodeling and, if damaged, can result in deformity and abnormal growth.3-6 Overall, growth-plate fractures account for 15-20% of major long-bone fractures in childhood. The majority of growth-plate injuries heal without long-term complications. However, an estimated 30% will result in a growth disturbance, and up to 2% can result in a functional growth deformity.7 The Salter-Harris classification system classifies physeal fractures as types I through V. In general, the severity of injury to the growth plate generally increases with each Salter-Harris grade. The following mnemonic can be helpful to remember the different Salter-Harris types when the long bone is in a vertical orientation with the epiphysis at the bottom. The mnemonic refers to the fracture line and its relationship to the growth plate:
S ("Straight across") = Type I (low risk for growth plate injury);
A ("Above") = Type II;
L ("Lower" or "BeLow") = Type III;
T ("Two" or "Through") = Type IV;
E ("End") or ER ("ERasure of the growth plate") = Type V (high risk for growth plate injury);
R.8
Having gained appreciation for the differences in pediatric and adult musculoskeletal systems, it is also important to approach each pediatric injury systematically by obtaining a detailed history and performing a thorough physical examination. While obtaining the history, the clinician should be cognizant of the mechanism, timing, and situation surrounding the injury. A thorough physical exam entails removing all clothing, bandages, and splints. Following removal of all obscuring items, an inclusive physical exam should involve inspection of the skin for any obvious deformities, swelling, and ecchymosis. The patient should be asked to locate the area of maximal tenderness, and the clinician should proceed with palpation, range of motion, and neurovascular exam of the involved extremity, including assessment of the joints both proximal and distal to the suspected fracture.2
Following a thorough physical exam, radiological views of the area of maximal tenderness and the joints, both proximal and distal, should be obtained. In addition to obtaining appropriate imaging, the clinician will need to identify radiographic abnormalities, including subtle findings, appropriately treat and immobilize injuries, and decide on the need for immediate subspecialty consultation or referral. (See Table 2.)
Table 2. Upper Extremity Trauma that Requires Orthopedic Referral
- An open fracture
- Severely displaced fractures
- Major joint dislocation
- Fractures with neurovascular compromise
- Injuries involving the growth plate
- Fractures with potential for developing compartment syndrome
Traumatic Upper Extremity Injuries by Location
The Clavicle. The clavicle is the most frequently injured bone in children, with more than half occurring in children younger than 10 years of age.2 The majority of these fractures occur as a result of shoulder compression during child birth or a fall on an outstretched arm. Clinically, clavicle fractures can be divided into fractures of the shaft, the medial, and distal ends.
Figure 1. Clavicle and Rib Fractures
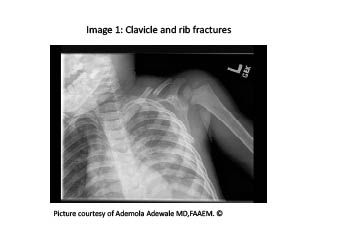
Clavicle shaft fractures (See Figure 1) result from direct trauma or from the transmission of indirect forces resulting from falling on an outstretched arm. A child will commonly present cradling the injured arm. In younger children, since their periosteum is thicker, fractures may be less displaced than older children, and clinical presentation may be delayed until the guardian detects a "knot" from the callus formation. In contrast, older children and adolescents typically sustain more significant injuries, resulting in noticeable lowering of the shoulder on the injured side, with localized swelling and tenderness and radiographic evidence of displacement and angulation.7 The treatment of nondisplaced or minimally displaced and angulated fractures, including those resulting from birth trauma, is primarily supportive. A figure-of-eight splint, sling and swathe, or shoulder harness can be used in older children and adolescents for 1 to 4 weeks for comfort, with instructions to refrain from participating in sports or related activities for 8 weeks.9 In any child with a significantly displaced fracture causing tenting of the overlying skin, an open fracture, or with bone impalement through the musculature, surgical evaluation and repair are indicated. In addition, clavicular shaft fractures associated with violent trauma or significant displacement should be evaluated closely for neurovascular injury, given the close proximity of both the brachial plexus and subclavian vessels.
Both medial and distal clavicular injuries commonly result from physeal separations. Pain and swelling in the proximity of the sternoclavicular joint is the common presenting complaint with medial epiphyseal injuries. Medial epiphyseal separations can be displaced either anteriorly or posteriorly, with the direction of displacement being determined by direct palpation. A clinical finding of posterior displacement is of particular concern, as compression of the trachea, subclavian vessels, or brachial plexus can occur, as well as involvement of the mediastinal structures.9 To determine the degree of displacement, multiple radiographic views and/or computed topography (CT) may be required.
Distal clavicular injuries tend to result from a direct blow to the shoulder, with increased pain while testing range of motion of the arm. Radiologically, such injuries can be mistaken for acromioclavicular separations. Treatment for both minor medial and distal fractures is supportive with a sling and progressive motion as the pain subsides.2 More serious injuries with or without neurovascular involvement require orthopedic evaluation.
The Scapula. Scapular fractures are very rare. However, when they do occur, they are usually the result of a high-energy trauma, such as a severe direct blow or from a motor vehicle accident. All scapular fractures are of a concern, as they are usually associated with multiple other fractures, including clavicle, ribs, thoracic vertebral, and humeral fractures.7 In addition, life-threatening injuries to the chest, neck, and head may also occur. Clinically, the diagnosis of a scapular fracture may be delayed secondary to the associated injuries.7 Plain radiographs may reveal fractures of the body or neck of the scapula, but a CT scan may be needed to delineate glenoid injuries.2 Treatment is conservative, with use of a sling or shoulder immobilizer for 2 weeks and progression to range of motion exercises. Fleisher et al recommend orthopedic consultation with any scapular fracture, given the rarity of the injuries.
The Shoulder. Shoulder dislocations in children are uncommon before physeal plate closure. Although rare in infants and children, it is occasionally seen in adolescents. As with adults, this dislocation may occur anteriorly, posteriorly, or inferiorly. The most consistent mechanism resulting in a traumatic dislocation is that of a significant direct force, with the majority displaced anteriorly. The child often presents with the injured arm held in abduction and external rotation, with the humeral head palpable anterior to glenoid fossa. Less than 3% of dislocations occur posteriorly in this age group and are commonly missed.10 Clinically, a posteriorly dislocated arm is typically held in adduction with slight internal rotation, appearing flat anteriorly with a coracoid process prominence. The rarest traumatic dislocation, luxatio erecta, or inferior dislocation, is likely if the patient presents with the involved shoulder maximally abducted and adjacent to his or her head. These injuries typically occur with enough force that results in an open injury with the humeral head being driven through the axilla.7 For any dislocation, special attention should be paid to a thorough neurovascular exam to identify any signs of an axillary nerve injury that may be present. Most dislocations can be diagnosed clinically; however, to determine the direction of displacement, customary views of the shoulder should be obtained, and these must include an anteroposterior, axial, and the Y-view.2,11
Although several reduction techniques exist, a detailed discussion is beyond the purview of this paper. Timely reduction of all acute dislocations is advised. Post-reduction imaging should be obtained to ensure reduction and the absence of glenoid fossa injury (Bankart's lesion) or posterolateral glenoid rim fracture (Hill-Sachs deformity). The integrity of the axillary nerve should be re-assessed post reduction as well. Patients should be placed in a sling or shoulder immobilizer for comfort and referred to an orthopedist for subsequent care.
The Humerus. Fractures involving the humerus are relatively more common in children than in adolescents and typically involve the shaft of the humerus. Proximal humeral fractures are rare and occur more in adolescents than in young children. Fractures occurring before adolescence are usually at the metaphysis, with Salter Harris type I injuries seen occasionally.2 During adolescence, the physeal region becomes more vulnerable due to rapid growth, and it is a common site of Salter Harris type II injuries.2 (See Figure 2.) Common mechanisms of injury include falls on an extended, adducted arm and direct blows to the shoulder. Patient presentations range from pain and mild swelling to obvious deformity and shortening of the arm. Routine anteroposterior and lateral radiographs should be obtained, with comparison views of the opposite arm if necessary to help differentiate normal variations in the epiphyseal line from a fracture. As with shoulder dislocations, close attention should be given to a thorough neurovascular exam. The remodeling capacity for proximal humeral fractures is ideal, even with 50-70 degrees of angulation in a pre-adolescent or with less than 50 degrees of angulation and 50% apposition in adolescents.2 As a result of this ability to remodel, the treatment often is conservative with a sling, sling and swathe, or hanging cast with orthopedic follow-up. Open fractures, fractures with neurovascular involvement, pathological fractures, and displaced fractures involving the articular surface in comparison require subspecialty consultation.
Figure 2. Shoulder Physeal Plate Injury in an 8-Year-Old Boy
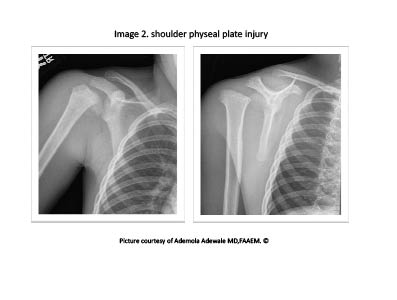
Humeral shaft fractures are the second most common fracture seen as a result of birth trauma, but overall they comprise a small percentage of all fractures in children and adolescents. (See Figure 3.) Occurring less frequently than those involving either the distal (see Figure 4) or proximal humerus, the majority of these fractures result from high-energy direct trauma, with the pattern of fracture emulating the likely mechanism of injury. For radiographic evaluation, a standard AP and lateral views should be obtained.
Figure 3. Humeral Shaft Fracture
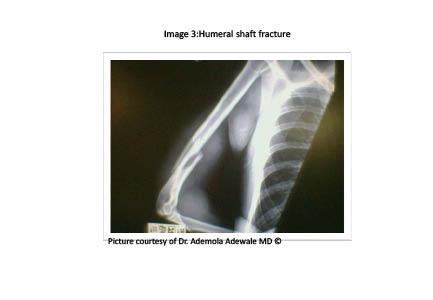
Figure 4. Distal Humerus Fracture
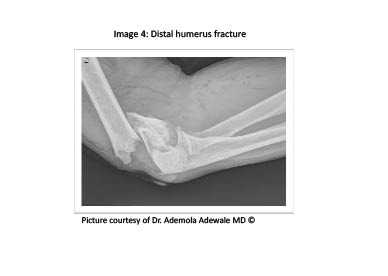
Transverse shaft fractures are usually the result of direct blows, whereas spiral fractures are typically caused by indirect twisting that may occur during a fall or as a result of nonaccidental trauma.2 The clinician must be mindful of children who present with an inconsistent mechanism of injury or history of minor trauma resulting in a humeral shaft fracture, as child abuse and pathological fractures must be considered. These injuries typically present with localized pain, swelling, and deformity. Special attention should be paid to ensure a complete neurovascular examination, as any fracture that involves the distal two-thirds of the humeral shaft has the propensity to result in radial nerve damage. Neurovascular examinations should include testing the function of the brachioradialis muscle, the wrist, and finger and thumb extension. In addition, the sensation to the dorsum of the hand and web space between the thumb and index fingers must be documented. Fortunately, even if a radial nerve palsy occurs, with appropriate fracture management, most resolve.2 Treatment is primarily conservative, with incomplete fractures being treated with sling and swathe. Complete, minimally displaced fractures can be managed with an upper-arm sugar-tong splint and sling. The alternative is a long-arm cast for older children and adolescents. Immediate orthopedic consultation is recommended for any completely displaced fracture that is angulated greater than 20 degrees in children, greater than 10 degrees in adolescents, overriding of fracture segments greater than 2 cm, significant rotation deformity, or any fracture with evidence of radial nerve involvement. All others can be stabilized and referred for orthopedic follow-up within 3-5 days.12
The Elbow. Injuries involving the pediatric elbow account for almost 15% of all pediatric fractures.2 Of all the pediatric injuries, those involving the elbow are the most challenging with respect to diagnosis, treatment, and possible complications. Thus, it is important for the clinician to have a good knowledge base of the normal anatomy and radiographic findings to avoid a missed or delayed diagnosis.
Supracondylar Fractures. Supracondylar fractures account for more than half of all pediatric fractures and commonly occur between the ages of 3 and 10 years.13-15 (See Figure 5.) The peak incidence for these fractures is between the ages of 5-7 years, with an average age of 7.9 years.7 Supracondylar fractures are typically divided into two different classification subsets: extension- and flexion-type fractures. The extension-type fractures are responsible for almost 95% of all supracondylar fractures and most commonly occur when a child falls on an outstretched hand with a hyperextended elbow. Clinically, these children present with localized tenderness and swelling over the injured elbow, with a depression over the proximal triceps.7
Figure 5. Supracondylar Fracture
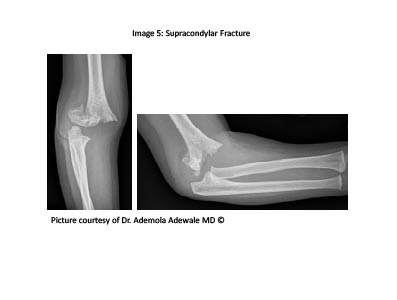
The less common flexion-type fractures account for about 5% of supracondylar injuries and often result from a direct trauma to the posterior aspect of a flexed elbow, which subsequently leads to an anterolateral movement of the entire condylar complex.7
Initial evaluation of both types of fractures includes a thorough history and physical exam that includes assessment of skin color, temperature, capillary refill, palpation of brachial artery, distal pulses, as well as the sensory and motor components of the median, radial, and ulnar nerves. If the degree of swelling is significant or any displacement is seen, close attention must be paid to a complete neurovascular exam and the thorough documentation of findings because of the risk for vascular compromise as well as subsequent development of compartment syndrome.16 Prompt orthopedic evaluation and treatment are recommended for any suspicion of neurovascular compromise.
Radiographic imaging should be obtained in any child presenting with localized tenderness or swelling of the elbow or a history consistent with a possible elbow fracture.7 At a minimum, an anteriorposterior view in extension and a lateral view at 90 degrees of flexion should be obtained. If no obvious fracture is identified, the practitioner should then review the radiograph systematically to identify subtle abnormalities that may suggest an occult fracture. Three elements that require particular attention include: the presence or absence of fat pads, the anterior humeral line, and the location and appearance of the ossification centers.17
Figure 6. Posterior Fat Pad
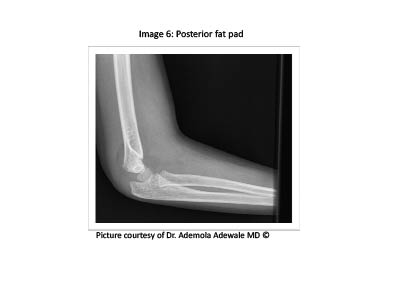
A lateral projection of the elbow should be assessed for the presence of both anterior and posterior fat pads.18 (See Figure 6.) The presence of a fat pad is a nonspecific marker of hemorrhage, joint effusion, or occult fracture. A narrow radiolucent strip superior to the radial head and anterior to the distal humerus can be a normal finding; however, if the anterior fat pad is wide, also known as a "sail sign," there should be a high index of suspicion for an occult fracture. In contrast, any radiolucency posterior to the distal humerus and adjacent to the olecranon fossa, a posterior fat pad, is highly indicative of occult fracture. (See Figure 6.)
The lateral view should also be assessed for the position of the anterior humeral line. The normal anterior humeral line can be traced along the anterior cortex of the humerus and will intersect at least one-third of the capitellum anteriorly. There is high probability of a supracondylar fracture if the anterior humeral line intersects less than one-third of the capitellum. When using this element for identification of subtle elbow fractures, the practitioner must keep in mind the age of the child and the variability with partial ossification of the capitellum.
The varying stages of the appearance and maturation of the ossification centers of the pediatric elbow make imaging interpretations unusually challenging. Utilizing the acronym CRITOE (capitellum, radial head, internal epicondyle, trochlea, olecranon, lateral epicondyle), and recalling that the capitellum ossifies at approximately 1 year of age with each of the following occurring in a two-year progression (i.e., 1, 3, 5, 7, 9 and 11 years of age), can aid in accurate imaging evaluation.7
Acute management includes adequate pain control and splint application for comfort. Further definitive management is dependent on the degree of displacement and angulation based on interpretation of the radiographs. Injuries without obvious radiographic injury but with history and clinical findings suspicious for fracture should still be placed in a posterior long-arm splint applied with the elbow flexed to 90 degrees with the forearm in a neutral position and with arrangement for appropriate orthopedic follow-up within 24 hours. Non-displaced fractures without any neurovascular involvement can be managed similarly. Caregivers should be educated on the signs of neurovascular comprise or compartment syndrome and advised to return to the ED immediately if any such signs or symptoms develop.
Any fractures with components of angulation and/or displacement, whether extension- or flexion-type, require orthopedic evaluation to determine the most appropriate treatment (i.e., closed reduction or percutaneous pinning) and hospitalization for continued neurovascular assessments.7 Pain should be managed similarly to all other fractures, and a posterior noncircumferential splint applied with the elbow at 110 degrees of flexion.
Complications that may arise from supracondylar fractures vary widely. The most commonly seen are neurovascular injuries, compartment syndrome and a long-term varus deformity, also known as cubitus varus. The most commonly injured neurovascular structures include the median, radial, and ulnar nerves in succession. The radial and brachial arteries may also be involved.15,19,20 Any vascular injury can manifest with the development of compartment syndrome in the volar forearm within 12 to 24 hours of injury. The suspicion of compartment syndrome mandates immediate intracompartmental pressure measurement and emergent orthopedic consultation. Any untreated patient may be at risk for the development of Volkmann's ischemic contracture, which is a fixed flexion of the elbow, pronation of the forearm, flexion at the wrist, and extension at the metacarpal-phalangeal joint.14,15
Radial Head Subluxation (Nursemaid's Elbow). Nursemaid's elbow results from traction on a pronated forearm with an extended elbow and typically occurs when a child sinks toward the ground while being held by the wrist, or from a sudden pull on the arm. The resultant longitudinal traction causes entrapment of the radial head distal to the annular ligament. Most subluxations occur in children 1 to 4 years of age and are rare after the age of 7 years. Patients classically present with a stationary flexed and pronated arm. The diagnosis is primarily based on the history and physical exam; imaging in the majority of cases is not warranted unless the history is unclear or if the physical exam suggests otherwise. Reduction of the subluxation can be accomplished by using one of two techniques. The first involves holding the elbow while supinating the wrist and simultaneously flexing the elbow. The second method requires holding the affected elbow while hyperpronating the forearm. Studies have shown the success rate with the two methods ranges from 80.4-92% and 97.5%, respectively.7 Most children will resume normal use of the affected arm within 15 minutes of reduction.9 If this does not occur, the clinician must consider the reduction unsuccessful or entertain an alternative diagnosis. Immobilization is unnecessary in simple subluxations, and parents should be advised to avoid further episodes of sudden traction on the child's arm.
Fractures of the Lateral Epicondyle. Fractures of the lateral epicondyle are the second most common elbow fractures in children21,22 and typically result from a fall on an outstretched hand with the elbow extended and the forearm supinated. Patients present with tenderness and swelling around the lateral aspect of the elbow. Suspected injuries should be evaluated with a minimum of three radiographic views: anteroposterior, lateral, and oblique. The radiographic finding that is synonymous with this fracture is the Thurston-Holland fragment, which is the presence of a posteriorly displaced metaphyseal fragment.7 Treatment is dependent upon the degree of displacement, which is best appreciated in the oblique view. Minimal displacements less than 2 mm can be treated with splinting with the elbow flexed and wrist pronated and dorsiflexed. Fractures with greater than 2 mm of displacement require orthopedic evaluation for possible open reduction or closed reduction with pinning. Since most lateral epicondyle fractures are intra-articular and transphyseal, they have the propensity to carry some degree of complications. Some of the commonly seen complications are: cubitus varus, lateral spur formation, delayed union, nonunion, and a possible growth arrest.
Fractures of the Medial Epicondyle. Fractures of the medial epicondyle usually result from either an avulsion fracture occurring at the growth plate or in association with elbow dislocations about 50% of the time. The medial epicondyle serves as the insertion point for the ulnar collateral ligament and the muscles responsible for the flexion of the forearm. The proximity of the ulnar nerve to the epicondyle results in an injury to this nerve in about 10-16% of these fractures. The presence of ulnar paresis on presentation should alert the practitioner to potential injury to the nerve. Acute or chronic valgus stress may produce an avulsion fracture, typically from overuse or repeated use, as seen with young baseball pitchers. These children present with pain and swelling localized to the medial aspect of the elbow. Recommended imaging and treatment are the same as for suspected lateral epicondylar fractures.
Elbow Dislocations. Dislocations of the elbow are unusual in the pediatric population. Contact sports and falls account for the majority of injuries, with most occurring in the older child or teenager. Dislocations tend to occur with a fall on an extended or partially flexed arm with supination of the forearm. (See Figure 7.) Patients present with an obvious deformity of the involved elbow, swelling, a shortened forearm, and fullness in the antecubital fossa.2 A neurovascular exam is paramount, as ulnar, median, and radial nerve injuries have been documented and warrant early recognition and intervention. As with adults, the most common dislocations occur posteriorly and are associated with fractures of the medial epicondyle, coronoid process, olecranon, and proximal radius. Treatment involves closed reduction, posterior splinting with post-reduction imaging, and a thorough post-reduction neurovascular exam. (See Figure 7.)
Figure 7. Elbow Dislocation and Relocation
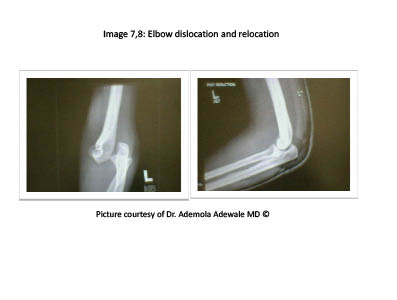
Forearm. Forearm fractures can be classified anatomically as occurring proximally, distally, or along the shaft of one or both bones. Fractures of the shaft of the radius or ulna account for 10-45% of pediatric fractures, occurring most commonly in early adolescence during the pubertal growth spurt.23-27 Forearm fractures vary considerably, as they may involve one or both bones and may be complete or incomplete fractures. Additionally, they may have considerable angulation and displacement with overriding segments. Most fractures result from a fall on an outstretched hand or direct trauma.26,28 Clinically, findings can vary from subtle findings to obvious deformities with swelling and point tenderness. The former tend to be buckle, greenstick, or plastic deformities, with the latter being the more common displaced fractures. If careful examination of the injured forearm reveals any puncture or open wound, orthopedic consultation is warranted for possible operative intervention. A minimum of two radiographs should be obtained to aid the clinician in determining the degree of angulation and displacement. Such fractures are classified according to location, completeness, angulation, and displacement. If radiographs exhibit a single bone fracture, additional views that include the wrist and elbow should be obtained to exclude Monteggia or Galeazzi fractures. Surgical intervention is usually only indicated for irreducible fractures, open fractures, and those with evidence of vascular injury. All others can be managed with closed reduction and immobilization. Potential complications include delayed union and nonunion, compartment syndrome, and synostosis.25,26
Figure 8. Monteggia Fracture
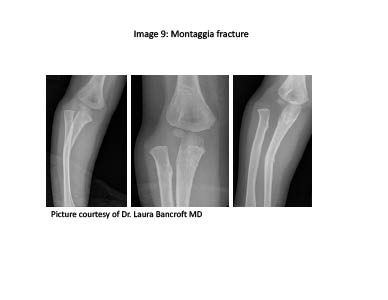
Monteggia Fracture. By definition, this injury includes radial head dislocation in combination with a fracture of the proximal third of the ulna. (See Figure 8.) Patients commonly present with obvious deformity to both the elbow and forearm following a fall on an outstretched hand. The clinician should be attentive during a thorough exam of the injured extremity, noting the presence or absence of any radial, medial, or posterior interosseous nerve involvement or evidence of an open fracture. The proximity of the radial head to both radial and median nerves increases the propensity of this fracture to produce nerve palsies; clinical significance cannot be underestimated. As previously mentioned, radiographs of the wrist, elbow, and forearm should be obtained, with special attention given to the anatomical position of the radius in all views. Any deviation of the proximal radius' alignment with the capitellum should trigger the clinician to consider a Monteggia fracture.29 Although most can be treated with closed reduction and immediate immobilization, surgical intervention is indicated in cases of unsuccessful closed reduction, inability to maintain alignment with closed reduction, or in cases of an open fracture. Patients should additionally be monitored for the development of compartment syndrome. Long-term complications of treated fractures include recurrent radial head dislocations, neuropraxias, malunion, and development of Volkmann's ischemic contracture.30
Distally occurring fractures account for 75% to 85% of all pediatric forearm fractures.23,26 These types of fractures result from a fall on an outstretched hand, with the resultant displacement dependent upon the position of the wrist at the time of impact. (See Figure 9.) Low-impact injuries result in buckle or torus fractures, and higher-impact injuries result in metaphyseal, physeal, greenstick, and Galeazzi fractures. Localized tenderness and swelling can help guide imaging interpretation and help the clinician recognize minor irregularities in the cortex consistent with frequently overlooked torus or buckle fractures.
Figure 9. Distal Forearm Fracture
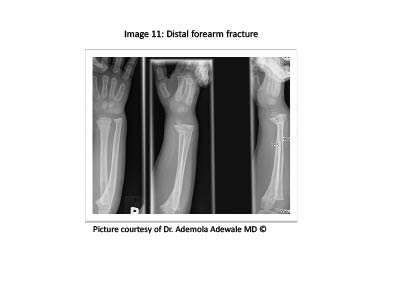
Metaphyseal fractures commonly involve a complete radial fracture with either a complete (see Figure 10), greenstick, styloid avulsion fracture, or plastic deformity of the ulna.7 Distal radial physeal injuries are classified according to the Salter Harris classification system. Except type III and IV injuries or intra-articular fractures, all other radial physeal injuries can be managed with closed reduction and have a high potential for remodeling. Type III and IV injuries require surgical intervention for definitive repair. Greenstick fractures can be managed with closed reduction and immobilization in neutral position.23,31
Figure 10. Distal Radius and Ulna Fracture
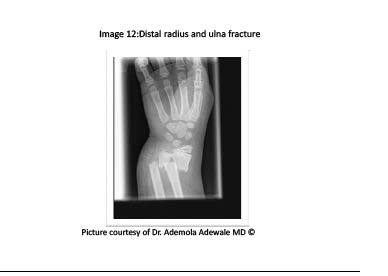
A relatively uncommon fracture in children, the Galeazzi fracture-dislocation involves a fracture of the radial shaft in association with a distal radioulnar dislocation. (See Figure 11.) This injury is usually the result of a fall on an outstretched hand with the forearm in pronation. The physical exam usually reveals prominence of the distal ulna and joint instability, with the patient unable to fully pronate or supinate his or her forearm. Treatment involves orthopedic consultation, closed reduction, and immobilization.
Figure 11. Galeazzi Fracture
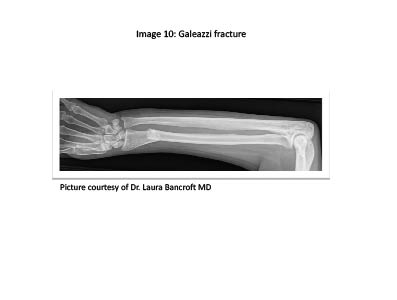
Wrist. Fractures of the pediatric carpal bones are fairly uncommon due to the lack of ossification until adolescence. The peak incidence of carpal fractures is seen at 12 years of age, with the scaphoid being the most commonly injured.32 The most common mechanism of injury is a fall on a outstretched hand with the wrist hyperextended. Unlike adults, scaphoid fractures in adolescents tend to be nondisplaced, located at the distal scaphoid, and involve a single cortex.33 Physical exam findings consistent with a possible scaphoid fracture include snuffbox tenderness, pain with supination against resistance, and pain with longitudinal compression of the thumb.7 As with adults, initial radiographic imaging may not demonstrate a fracture. If physical findings are suggestive of a scaphoid injury, the patient should be placed in a thumb spica splint for 2 weeks and orthopedic follow-up arranged.
The Hand. Hand injuries occur commonly in children and follow a bimodal distribution, with distal phalanx injuries occurring more commonly around 1 year of age and most phalangeal and metacarpal injuries occurring around 12 years of age.34-36 In general, most pediatric hand fractures are uncomplicated and can be adequately treated with immobilization; however, there are a few that require more definitive care.
Most distal phalanx injures result from a crush-type injury to the fingertip and involve the nail and nailbed. The nail and nailbed should be thoroughly evaluated for any trauma and repaired accordingly. These types of injures are considered open fractures; however, they can be managed with splinting, oral antibiotics to prevent osteomyelitis, and orthopedic follow-up.37
In general, almost all proximal and middle phalanx fractures can be managed with closed reduction and splinting. All closed, single metacarpal fractures can be managed with a splint and supportive care. However, any single metacarpal fracture with significant angulation, malrotation, or displacement will require open reduction and possible fixation.7 Malrotation is best tested by having the patient flex his or her fingers touching the palmar aspect of the hand. All fingers should point in the same direction; if there is malrotation, overlapping of the involved fingers will be noted.2 Additionally, the involvement of multiple metacarpals renders an injury unstable, and open reduction with pinning is usually required.
Conclusion
Upper extremity trauma in the pediatric population is a common presentation to the ED. The stark differences in the musculoskeletal system when compared to that of adults make the evaluation more challenging. The components of their bony structures (preponderance of cartilage) produce unique types of injury patterns. In addition, depending on the child's age, obtaining pertinent history of events prior to injury might be difficult. Regardless, inconsistent injury patterns to the long bones should warrant detailed investigation to exclude abuse as the cause of injury.
Radiographic evaluation of the pediatric bony structures creates challenges because of the physeal structures. Consequently, it may be necessary to obtain contralateral radiographic studies for comparison to identify subtle abnormalities. Attention must be given to physeal injuries to avoid a missed or delayed diagnosis that may result in a complication such as incomplete union, nonunion, or growth plate arrest. Another potential pitfall to avoid is to ensure complete documentation of neurovascular findings before and after manipulation of the injury. In addition, parents should be educated as to what the healing expectations are and also on how to identify potential complications such as compartment syndrome early. When in doubt, it is always wise to immobilize by splinting, ensure documentations of conversations with the orthopedist, and mandate 12- to 24-hour follow-up on injuries that are concerning.
References
1. Frost HM, Schonau E. The muscle unit in children and adolescents: A 2000 overview. J Pediatr Endocinol Metab 2000;13:571-90.
2. Fleisher GR, Ludwig S, et al, eds. Textbook of Pediatric Emergency Medicine, 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2010: 1335-1356.
3. Iannotti JP. Growth plate physiology and pathology. Orthop Clin North Am 1990;21:1-17.
4. Mizuta T, Benson WM, Foster BK, et al. Statistical analysis of the incidence of physeal injuries. J Pediatr Orthop 1987;7:518-523.
5. Johari AN. Remodeling of forearm fractures. J Pediatr Orthop Part B 1999;8:84-87.
6. Murray DW, Wilson-MacDonald J, Morscher E, et al. Bone growth and remodeling after fracture. J Bone Joint Surg Br 1996;78B:42-50.
7. Carson S, Woolridge, DP, Colletti J, et al. Pediatric upper extremity injuries. Pediatric Clin North Am 2006;53:41-67.
8. Tandberg D, Sherbring MSO. A mnemonic for the Salter-Harris classification. Am J Emerg Med 1999;17:321.
9. Baren JM, Rothrock SG, Brennan JA, et al. Pediatric Emergency Medicine. Philadelphia: Saunders; 2008:172-179.
10. Bishop, JY. Pediatric shoulder trauma. Clin Orthop 2005;432:41-48.
11. Raby N, Berman L, de Lacy G. Accident & Emergency Radiology: A Survival Guide, 2nd ed. Philadelphia: Elsevier; 2005:90-107.
12. Musgrave DS, Mendelson SA. Peditaric orthopedic trauma: Principles in management. Crit Care Med 2002;30:S431-S443.
13. Della-Giustina K, Della-Giustina DA. Emergency department evaluation and treatment of pediatric orthopedic injuries. Emerg Med Clin North Am 1999;17:895-922.
14. Wu J, Perron AD, Miller MD, et al. Orthopedic pitfalls in the ED: Pediatric supracondylar humerus fractures. Am J Emerg Med 2002;20:544-9.
15. Villarin LA, Beck KE, Freid R. Emergency department evaluation and treatment of elbow and forearm injuries. Emerg Med Clin North Am 1999;17:844-858.
16. Simon RR, Koeingsknecht SJ, editors. Emergency Orthopedics: The Extremities. Stamford (CT): Appleton & Lange; 1987:122-129.
17. Noonan KJ, Price CT. Forearm and distal radius fractures in children. J Am Acad Orthop Surg 1998;6:146-156.
18. Shrader MW. Pediatric supracondylar fractures and pediatric physeal elbow fractures. Orthop Clin North Am 2008;39;163-171.
19. Lyons ST, Quinn M, Stanitski CL. Neurovascular injuries in type III humeral supracondylar fractures in children. Clin Orthop 2000;376:62-67.
20. Brown, IC, Zinar DM. Traumatic and iatrogenic neurological complications after supracondylar humerus fractures in children. J Pediatr Orthop 1995;15:440-443.
21. Skaggs D, Pershad J. Pediatric elbow trauma. Pediatric Emerg Care 1997;13:425-434.
22. Mirsky EC, Karas JR, Weiner LS. Lateral condyle fractures in children: Evaluation of classification and treatment. J Orthop Trauma 1997;11:117-120.
23. Boyer BA, Overton B, Schrader W, et al. Position of immobilization for pediatric forearm fractures. J Pediatr Orthop 2002;22:185-187.
24. Jones K, Weiner DS, The management of forearm fractures in children: A plea for conservatism. J Pediatr Orthop 1999;19:811-825.
25. Luhmann SJ, Schootman M, Schoenecker PL, et al. Complication and outcomes of open pediatric forearm fractures. J Pediatr Orthop 2004;24:1-6.
26. Rodriguez-Merchan EC. Pediatric fractures of the forearm. Clin Orthop 2005;432:65-72.
27. Schimittenbecher PP. State-of-the-art treatment of forearm fractures. Injury 2005;36 (Suppl A):S25-34.
28. Vorlat P, De Boweck H. Bowing fractures of the forearm in children: A long-term follow-up. Clin Orthop 2003;413:233-237.
29. Kay RM, Skaggs DL. The pediatric Monteggia fracture. Am J Orthop 1998;27:606-609.
30. Stein F. Grabias SL, Deffer PA. Nerve injuries complicating Monteggia lesions. J Bone Joint Surg Am 1983;53A:1432-1436.
31. Herring JA, Tachdjian MO, editors. Tachdjian's Pediatric Orthopedics, 3rd edition. Philadelphia: WB Saunders; 2002:2115-2252.
32. Light TR. Carpal injuries in children. Hand Clin 2000;16:513-522.
33. Fabre O, De Boeck H. Fractures and nonunions of the carpal scaphoid in children. Acta Orthop Belg 2001;67:121-125.
34. Bhende MS, Dandrea LA, Davis HW. Hand injuries in children presenting to a pediatric emergency department. Ann Emerg Med 1993;22:1519-1523.
35. Fetter-Zarzeka A, Joseph MM. Hand and fingertip injuries in children. Pediatr Emerg Care 2002;18:341-345.
36. Ljungberg E, Rosberg HE, Dahlin LB. Hand injuries in young children. J Hand Surg Br 2003;28:376-380.
37. Nofsinger CC, Wolfe SW. Common pediatric hand fractures. Curr Opin Pediatr 2002;14:42-45.
Musculoskeletal injuries account for approximately 10-15% of all childhood injuries, with most occurring as a result of a fall, sports-related injury, motor vehicle trauma, or intentional physical abuse.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
