Pediatric Eye Infections
Pediatric Eye Infections
Authors:
Catherine A. Marco, MD, Professor, Department of Emergency Medicine, Program Director, Emergency Medicine Residency, University of Toledo College of Medicine, Toledo, OH.
Joanna L. Marco, BS, Brigham Young University, Provo, UT.
Peer Reviewer:
Alesia Fleming, MD, MPH, Assistant Professor of Pediatrics and Emergency Medicine, Emory University School of Medicine, Atlanta.
Eye infections are common among emergency department (ED) pediatric patients and can lead to significant morbidity if not properly managed. Specific attention to the physical examination is mandatory in the evaluation of pediatric eye infections, and should include an external examination, visual acuity, and pupillary reaction. Ocular motility, visual field testing, slit-lamp examination, fluorescein staining, intraocular pressure, and funduscopic examination should be conducted in select circumstances.
Following complete evaluation, many eye infections can be managed as outpatients with primary care or ophthalmologic follow-up. Certain eye infections warrant hospital admission or emergent ophthalmologic consultation, including orbital cellulitis, periorbital cellulitis, endophthalmitis, herpes infections, or any eye infection that may result in significant visual loss. Prompt evaluation, treatment, and referral are indicated to reduce incidence of visual loss.
Ann M. Dietrich, MD, Editor
Introduction/Epidemiology
Table 1. Differential Diagnosis of the Red Eye
Infections
- Conjunctivitis (viral, bacterial, fungal)
- Keratitis
- Iritis
- Periorbital cellulitis
- Orbital cellulitis
Ophthalmologic Conditions
- Acute angle-closure glaucoma
- Dry eye
- Blepharitis
- Nasolacrimal duct obstruction
- Uveitis
- Episcleritis
- Scleritis
Traumatic Conditions
- Corneal abrasion
- Foreign body
- Subconjunctival hemorrhage
- Trichiasis
- Thermal burns
Allergic Conditions
- Allergic conjunctivitis
Chemical Reactions
- Medication reactions
- Chemical burns
Intracranial lesions
- Malignancy
- Cavernous sinus thrombosis
- Intracranial abscess
The red eye is a common chief complaint in both primary care and emergency department settings. (See Table 1.) The red eye comprises approximately 6% of general medical visits and accounts for 15% of ophthalmologic consultations.1,2 Conjunctivitis accounts for approximately 30% of all eye complaints.3 Pediatric eye infections may include infections of the external eye structures, eyelids, conjunctiva, or the globe itself. Conjunctivitis is the most common nontraumatic eye complaint.
Prompt evaluation of the pediatric patient with an eye complaint includes history, physical examination, including visual acuity, and inspection. If trauma, foreign body, or significant eye disease is a possibility, fluorescein and slit-lamp examinations, and a funduscopic examination should also be performed. Although frequently a definitive diagnosis cannot be established in the ED, a differential diagnosis must be established, and non-infectious etiologies should be excluded, including trauma, allergic reactions, and connective tissue disorders.4 Eye infections may be caused by a variety of organisms, including viruses, bacteria, and fungi, and prompt definitive therapy should be instituted for the suspected infection.
The Clinical Evaluation/Diagnostic Tools
Examining the eye of a pediatric patient may pose a significant challenge. Most patients older than age 3 years can be successfully examined using interactive distracting techniques and parental assistance; rarely, a papoose board or sedation may be required for an adequate examination. After collecting a comprehensive history, the physical examination of the eye should include these elements: visual acuity, pupillary reactions, and external examination. In some cases, a more detailed examination is indicated, including ocular motility, visual field testing, slit-lamp examination, fluorescein staining, intraocular pressure, and funduscopic examination.6 Certain areas of a thorough eye examination are age specific, other areas are independent of age, and most depend on patient cooperation. Remember to perform the more uncomfortable portions of the exam last.
Visual acuity is considered to be the vital sign of the eye, and its measurement is essential in the evaluation of eye infections. Visual acuity in neonates, infants, and toddlers is performed by assessing pupillary reaction to light. A light source should be used 1-3 feet away; the ability to track and fixate on light determines adequate visual acuity. Steady fixation is considered roughly equivalent to 20/40, unsteady fixation is equivalent to 20/100, and inability to fixate is equivalent to 20/400. By the age of 2-3 years, normal development places visual acuity at 20/20. Formal visual acuity testing is performed using a Snellen chart, Allen chart (pictures), or rotating "E" chart at 20 feet. Testing should always be done with correction (if possible) or with a pin hole device if the patient is myopic. A pre-made pinhole device will correct most refractive errors to at least 20/30. If a pinhole device is not available, a quick alternative can be made using an 18-gauge needle and an index card, or a metal eye shield with multiple small holes can also be used. If a refractive error exists beyond 20/30, it should not be attributed to simple refractive error. When individuals are unable to read the fist line (20/200), shorten the distance to 10 feet and have them read the top line (10/200). Continued inability to read any letters will require the use of counting fingers and recording the distance (e.g., able to count 3 fingers at 3 feet). If the patient is unable to count fingers, then attempt to see if the patient can visualize gross hand motion or detect light perception.7,8
Pupil examination should include size, shape, symmetry, and reaction to light. Examination of the eye should include evaluation for an afferent pupillary defect. Normal pupils will constrict and accommodate equally when a bright light is shown on the pupil (direct) and when light is shown on the opposite pupil (consensual light reflex). If the light reflex is diminished, a swinging flashlight test will discriminate between an afferent (retina, optic nerve) injury or efferent (third nerve or papillary muscle) injury.
External examination of the eye includes observing for proptosis, enophthalmos, foreign bodies, erythema, swelling, or warmth of the eyelids and periorbital areas. The cornea, sclera, and conjunctiva should be examined by gross inspection as well as by slit-lamp examination. The cornea should be examined to rule out corneal infection. Evaluate the conjunctiva to detect inflammation, foreign bodies, or discharge.
Ocular motility should be assessed and documented if trauma or anatomic abnormality is suspected. If a patient is unable to move the eye in a certain direction, concerns for entrapment of a muscle from an orbital blow-out fracture, direct muscle injury, or central nervous problem should be considered.
Visual field testing can be brief and involve the four major quadrants of vision; formal visual field testing can be done at a later time. Visual field testing is important to perform, especially if the history suggests the possibility of retinal detachment or vitreous hemorrhage (e.g., new floaters or flashes of light). Performing visual field testing is quick and easy. Have the patient cover one eye, position yourself at eye level, and hold your fingers halfway between yourself and the patient. Ask the patient to look at your nose while you slowly move your fingers from the outside in, making sure the patient does not look away from your nose and toward the fingers. Binocular visual field loss is typically neurological in nature and not an ophthalmologic issue.
A slit-lamp examination in older children is performed using the same technique as for adults. Younger children may feel more comfortable sitting on a parent's lap for the examination. Some tricks to having younger children be more cooperative with the exam are to coax them into seeing something fun in the slit lamp (e.g., favorite cartoon character). Have parents place their chin in the device first to reassure the child, and tell them that they will see a pretty blue light. When examining infants, have parents sit and support the child's bottom with one hand, while the other hand rests on the back of the infant's head. If the child is not cooperative, a Wood's lamp may be an alternative to diagnosing corneal defects; however, Wood's lamp examination does not allow the detail of inspection afforded by slit-lamp examination.
Intraocular pressure (IOP) evaluation is generally used to assess the possibility of glaucoma or significant eye injuries. IOP testing is contraindicated in suspected globe perforation, corneal abrasion, and foreign bodies. IOP can be measured with a portable tonometer or using slit-lamp applanation tonometry. Normal IOP is 12 mm Hg. Errors in tonometry can easily be made by placing too much pressure on the eye, blinking, or crying, all of which may artificially elevate IOP.
Finally, in order to view the posterior portions of the eye and retina, funduscopic examination may be indicated. To assist in good visualization of the optic nerve and retina, have lights in the room turned off and turn the intensity of the ophthalmoscope to its lowest setting and smallest aperture. Toddlers may be afraid of the ophthalmoscope, but allowing them to see it up close and possibly hold it may take away some anxiety. Another trick with toddlers is to ask them to look for their favorite cartoon character in the light as you are performing your exam. Ideally, funduscopic examination is best performed after dilation. Pupils should not be dilated if serial neurologic exams are to be performed or if acute angle closure glaucoma is suspected.
Extraocular Infections
Periorbital Cellulitis. Periorbital (preseptal) cellulitis is an infection of the eyelid and surrounding soft tissues anterior to the orbital septum, without involving the eye or orbit. Periorbital cellulitis is more common than orbital (septal) cellulitis. The most common predisposing conditions for periorbital cellulitis include conjunctivitis, infected wound or trauma, insect bites, and sinusitis.9 Periorbital cellulitis can also result more rarely from hematogenous spread, dental infection, upper respiratory tract infection, or endophthalmitis.10-12 The most commonly implicated organisms include Staphylococcus aureus, Streptococcus pyogenes, and Streptococcus pneumoniae. Since Haemophilus influenzae type B (HIB) vaccines have become routinely administered, HIB rarely causes periorbital cellulitis. Other causative organisms may include Acinetobacter species, Nocardia, Bacillus anthracis, Pseudomonas aeruginosa, Neisseria gonorrhea, and other species.
Common presenting complaints include fever, malaise, eye pain, and periorbital swelling. There may be erythema, chemosis, or conjunctivitis with discharge. Vision is typically not affected, except by discharge. Inflammation may extend over the superior orbital rim onto the brow. In contrast, in orbital cellulitis, the upward spread of inflammation is blocked by the orbital septum.
Distinguishing between periorbital cellulitis and orbital cellulitis has important treatment and disposition implications. Patients with proptosis, ophthalmoplegia, painful extraocular movement, periorbital edema, or an ANC of < 10,000 cells per microliter are at high risk for orbital cellulitis or abscess.13 These patients should receive prompt evaluation, imaging, and treatment.
Immunocompromised children, including children with diabetes, require an ophthalmology consult upon presentation with eyelid erythema. Redness may be an indication of mucormycosis, which generally requires surgical debridement.12
Periorbital cellulitis may be treated as an outpatient with oral antibiotics only for patients older than 1 year of age if orbital involvement is excluded, the child is afebrile and appears nontoxic, and follow-up is reliable.12 If the child appears toxic, or orbital cellulitis or abscess is suspected, then the child should be admitted and should receive imaging studies and parenteral antibiotics. If periorbital cellulitis occurs in the neonate (often due to dacryocystitis), then hospitalization and parenteral antibiotics are indicated.
For outpatient management, oral antibiotics such as amoxicillin/clavulanate, cefpodoxime, or cefdinir are appropriate. The typical duration of oral antibiotic use is 10-14 days, but if the patient does not improve after 48 hours of oral antibiotic therapy, inpatient treatment is indicated.
For children who are admitted, early consultation with an ophthalmologist is important. For inpatient antibiotic management, parenteral ceftriaxone or cefotaxime are appropriate antibiotic choices. Intravenous cefazolin or nafcillin are appropriate if there is a clear cutaneous entry site.
Orbital Cellulitis. Orbital (septal) cellulitis is an infection of the orbit posterior to the orbital septum. The infection may involve any of the orbital structures, including the eye, as well as its supporting muscles and nerves. Most cases of orbital cellulitis result from secondary spread from paranasal sinusitis (often ethmoid sinusitis, as the ethmoid sinus is only separated from the orbit by the thin lamina papyracea). Other common causes include hematogenous spread, penetrating trauma, or dental abscess. Prompt diagnosis and definitive treatment are crucial to prevent potential complications, including visual loss, meningitis, abscess, or mortality.13,14
Staphylococcus is the most common species cultured in pediatric orbital cellulitis, and 73% of S. aureus isolates are methicillin-resistant. Streptococcal species may also cause orbital cellulitis. Other organisms are rarely implicated, including Haemophilus influenzae, non-spore-forming anaerobes, Eikenella corrodens, Aeromonas hydrophila, Pseudomonas aeruginosa, and other fungal and mycobacterial organisms.15 Since the introduction of the HIB vaccine, H. influenzae is less commonly implicated as a cause of orbital cellulitis. Surgical aspirations are most likely to yield a positive culture, but because of its invasive nature, nasal swabs or cultures of ocular discharge may be preferred. Blood cultures are unlikely to have a positive yield.15 Past recommendations for blood cultures, based on H. influenzae's common complications, may no longer be indicated today. In choosing antibiotic coverage, consider obtaining cultures through ocular discharge or nasal swabs.15
Orbital cellulitis usually presents with unilateral symptoms, which may include proptosis, swollen and erythematous eyelid, chemosis, impaired or painful eye movement, double vision, visual loss, and resistance to retropulsion of the globe. Papilledema, vomiting, severe headache, or meningeal signs may signify further spread of the infection to the meninges or the cavernous sinus.
Other diagnoses that should be considered in the differential diagnosis of orbital cellulitis include malignancies, scleritis, granulomatous disease, trauma, allergic reactions, or abscess.16
When orbital cellulitis is suspected, CT is indicated, preferably with axial and coronal thin cuts of the sinuses and orbits. Imaging may also distinguish cellulitis from malignancies, such as neuroblastoma or retinoblastoma.4 MRI may be useful if cavernous sinus thrombosis is suspected, and may provide further details into soft-tissue involvement. Ultrasound is unlikely to provide sufficient visualization of the posterior orbit to be of use.10 Emergent ophthalmology consultation is indicated for patients with confirmed or suspected orbital cellulitis. If imaging studies indicate sinus involvement, obtain an otolaryngology consult as well.12
Children with orbital cellulitis should be admitted for IV antibiotics and close monitoring. Aggressive medical management is usually appropriate initially, and patients should receive broad-spectrum antibiotics as soon as possible. Vancomycin should be administered empirically if methicillin-resistant S. aureus (MRSA) is suspected. An additional agent, such as ampicillin/sulbactam, ceftriaxone, or cefotaxime, or a fluoroquinolone such as ciprofloxacin or levofloxacin, should be added to cover other pathogens.12,17 The antibiotic choice may be narrowed following culture results. Although medical management may be preferable, if there is no improvement after 48 hours of IV antibiotics, or if there are signs such as a large abscess, blindness, or progressing orbital signs, surgical intervention may be indicated.18 If the infection has progressed to subperiosteal orbital abscess, surgical drainage is indicated.11
Hordeolum. Hordeolum is an acute staphylococcal infection of either the meibomian gland (internal hordeolum) or the zeisian gland (external hordeolum). It usually presents as a tender, red nodule at the margin of the lid, and may have associated lid edema or purulent discharge.4 Conservative management with warm compresses is advised. Topical antibiotics do not speed recovery of hordeolum, but they may help prevent the spread of the infection to neighboring areas. Surgical drainage may be indicated in severe or chronic cases.12
Chalazion. Chalazion is a firm, localized, lipogranulomatous inflammation of the eyelid. Although it is typically caused by obstructed meibomian glands, not bacterial infection, it may occur as a consequence of infection. There is typically no pain or discharge. Warm compresses may also be helpful, and topical antibiotic ointment should be prescribed when there are signs of infection. Definitive management may include a single intralesional triamcinolone acetonide injection followed by lid massage, which is nearly as effective at treating chalazia as incision and curettage.19
Blepharitis. Blepharitis is a chronic inflammation of the eyelids, often associated with staphylococcal infection.5 Blepharitis presents with scaling around the eyelashes, eyelid inflammation, discomfort, itching, and conjunctival hyperemia. Severe cases that involve the cornea make up 5% of the total disease spectrum.20
Proper eye hygiene is crucial for managing blepharitis. Patients should keep the lids clean by lightly scrubbing the base of the eyelashes with a cotton swab dipped in diluted baby shampoo, and warm compresses may provide additional relief. For acute cases of staphylococcal blepharitis, topical antibiotics such as bacitracin or erythromycin may be appropriate. For moderate to severe acute cases, tobramycin/dexamethasone ophthalmic suspension 0.3%/0.05% has been shown to be more effective than azithromycin.21
Ocular Infections
Conjunctivitis. Acute conjunctivitis is conjunctival inflammation typically resulting from infection or allergy. It is the most frequent ophthalmologic complaint among children seen in the ED.22 Conjunctivitis may have bacterial, viral, or noninfectious etiologies. Noninfectious etiologies include chemical conjunctivitis, allergic conjunctivitis, phlyctenular conjunctivitis, Kawasaki disease, ligneous conjunctivitis, and giant papillary conjunctivitis.23 Although this article will focus on the infectious etiologies, consider noninfectious etiologies in the differential diagnosis when appropriate.
Distinguishing between the different forms of conjunctivitis can be helpful in determining the most appropriate treatment, as well as in detecting possible complications. The age of the child as well as the characteristics of the discharge, conjunctival injection, and other symptoms are useful in clinically determining etiology. (See Table 2.)
Table 2. Characteristics of Pediatric Conjunctivitis
|
Bacterial |
Viral |
Allergic |
|
|
Adapted from: Teoh DL, Reynolds S. Diagnosis and management of pediatric conjunctivitis. Pediatr Emerg Care 2003;19:48-55. |
|||
|
Common etiologies |
Staphylococcus aureus Streptococcus pneumonia Neisseria gonorrhea Chlamydia trachomatis Pseudomonas aeruginosa Moraxella catarrhalis |
Adenovirus HSV HZV Enterovirus Coxsackie Epstein-Barr |
Allergens Pollens |
|
Prevalent age |
All ages, especially neonates to toddlers |
All ages, especially school age to adults |
Late childhood to early adulthood |
|
Character of discharge |
Purulent |
Watery |
Mucoid |
|
Amount of discharge |
Copious |
Moderate |
Mild to moderate |
|
Injection |
Severe |
Moderate |
Mild to moderate |
|
Lymphadenopathy |
Occasional |
Common |
None |
|
Associated signs |
Papillary response |
Follicular response |
Chemosis |
|
Associated conditions |
Otitis media |
URI, pharyngitis |
Rhinitis, asthma, eczema |
Bacterial Conjunctivitis. Bacterial conjunctivitis is extremely common in the United States. In 2005, there were approximately four million cases in the United States. The estimated cost of treating these cases is approximately $589 million annually.25 Bacterial conjunctivitis is characterized by injected conjunctiva, episcleral vessels, and papillae in the palpebral conjunctiva. It is often accompanied by thick, purulent discharge and eyelash matting. Findings are often unilateral, although bilateral bacterial conjunctivitis may occur. Preauricular adenopathy may be present. The finding of photophobia, which is not a feature of bacterial conjunctivitis, should raise suspicion for iritis or herpetic keratoconjunctivitis. The examination should include slit-lamp examination in contact lens wearers to exclude corneal ulcer.
The most common organisms cultured are S. aureus, S. pneumoniae, Pseudomonas aeruginosa (particularly in contact lens wearers), Moraxella catarrhalis, and Chlamydia trachomatis. In severe cases, Neisseria gonorrhoeae should be considered. Care should be taken to identify N. gonorrhoeae, as penetration of the cornea is possible in these cases.12
Bacterial conjunctivitis is usually self-limited and should be managed conservatively. Topical antibiotic treatment is indicated, as distinction between viral and bacterial etiologies may not be possible in the ED. Antibiotic treatment may slightly decrease the duration of the infection. Some authors advocate that antibiotic use should be delayed by several days. Compared to immediate prescribing, delayed prescribing does not affect the severity of symptoms and only marginally increases the duration of symptoms, but it reduces unnecessary antibiotic use.26-28 However, this approach may not be practical in the ED environment, where compliance and follow-up may be less than ideal. In most cases, it is appropriate to give the parents a prescription for topical antibiotics that can be filled in 48 hours if symptoms have not improved. Supportive care, including frequent eye irrigation with sterile water, warm compresses, decongestants, and artificial tears, may be helpful. Contact lens wearers should discontinue use until treatment has been completed. Conjunctivitis may be highly contagious, and patients should be educated about hand-washing and infection-control techniques.
Appropriate antibiotic selection should include a broad-spectrum topical antibiotic ointment or drops.29 Ointment may be preferable for children because of longer duration and decreased frequency of administration. Consider factors such as cost, patient compliance, and risk of adverse effects when selecting an antibiotic.
Appropriate antibiotic medications include erythromycin ointment, sulfacetamide ophthalmic drops, or polymyxin/trimethoprim drops. Besifloxacin ophthalmic solution 0.6%, given three times daily for seven days, is another effective and safe treatment.30-32 Azithromycin 1.5% eye drops given twice daily for three days have been shown to be effective, and the ease of use may increase patient compliance.33,34 Moxifloxacin 0.5% ophthalmic solution, administered three times daily for three days, is also effective and is better tolerated than azithromycin.35,36 Levofloxacin eye drops 0.5%, given three times daily for five days, are also useful.37,38 Some widely used drugs, such as sulfacetamide and neomycin, tend to cause sensitization and should be prescribed with caution.39 (See Table 3.)
Table 3. Selected Topical Ophthalmic Antibiotics40,41
|
Agent |
Formulation |
Comments |
|
Erythromycin |
0.5% ointment |
Effective against gram-positive organisms and atypical microbes |
|
Tobramycin |
0.3% solution, 0.3% ointment |
Effective against gram-negative organisms and some gram-positive organisms; may cause sensitization |
|
Gentamicin |
0.3% solution |
Effective against gram-negative organisms and some gram-positive organisms; may cause sensitization |
|
Trimethoprim sulfate |
Solution, ointment; available in combination with Polymyxin B as Polytrim |
Broad-spectrum coverage, including MRSA and H. influenzae |
|
Azithromycin |
1% solution |
Broad-spectrum coverage; approved for over 1 year of age |
|
Sulfacetamide sodium |
10%, 15%, 30% solution, 10% ointment |
Broad-spectrum coverage; high allergic potential; rarely causes Stevens Johnson syndrome |
|
Chloramphenicol |
0.5% solution, 1% ointment |
|
|
Bacitracin/Polymyxin B |
Ointment; available in combination with trimethoprim as Polytrim |
Effective against most gram-positive and gram-negative organisms in combination |
|
Ciprofloxacin |
0.3% solution or 0.3% ointment |
Broad-spectrum activity, including against Pseudomonas aeruginosa |
|
Levofloxacin |
0.5% solution, 1.5% solution |
Broad-spectrum activity, including against Pseudomonas aeruginosa |
|
Moxifloxacin |
0.5% solution |
Broad-spectrum activity, including against Pseudomonas aeruginosa; improved activity against gram-positive organisms |
|
Besifloxacin |
0.6% solution |
Broad-spectrum activity |
|
Neomycin |
Solution, ointment |
High incidence of sensitivity reactions; potentially toxic to corneal epithelium |
|
*This list is representative samples and not all-inclusive. According to The Medical Letter experts, most topical antibiotics are effective for the treatment of uncomplicated conjunctivitis. |
||
Gonococcal conjunctivitis requires special consideration and management. Gonococcal conjunctivitis should be suspected in cases of severe conjunctivitis with profuse purulent discharge, erythema, irritation, local tenderness, chemosis, periorbital edema, and preauricular adenopathy. This diagnosis in a child older than 1 month of age raises the suspicion of sexual abuse.23 Because of the high risk of ocular complications, including keratitis, perforation, and visual loss, inpatient treatment with intravenous antibiotics, such as ceftriaxone or cefotaxime, is indicated.
If a child with bacterial conjunctivitis experiences pain, headache, photophobia, decreased vision, nausea, or any degree of corneal ulceration, or if he or she wears contact lenses, immediately obtain an ophthalmology consultation.42-44 Hyperacute cases and cases without improvement after 24 hours of antibiotic treatment should also be referred to an ophthalmologist.43
Viral Conjunctivitis. Viral conjunctivitis is most commonly caused by adenovirus, but it may also be caused by herpes, varicella, or, less commonly, coxsackievirus or Epstein-Barr.4 Viral etiology is more likely in patients older than age 5 years presenting in April through November, with bilateral symptoms, minimal discharge, or watery discharge.44
Adenovirus is associated with four different clinical presentations, which vary slightly based on the virus serotype, but which all generally include such features as redness, watery discharge, and eyelid edema. The four main clinical presentations include nonspecific follicular conjunctivitis (NFC), pharyngeal conjunctival fever (PCF), epidemic keratoconjunctivitis (EKC), and acute hemorrhagic conjunctivitis (AHC).47 PCF occurs more often in children and is associated with fever, sore throat, follicular conjunctivitis, and sometimes punctuate keratitis that will stain with fluorescein. EKC is more clinically obvious and is characterized by conjunctival injection, chemosis, and keratitis. Patients with EKC often develop subepithelial stromal infiltrates approximately one week after the onset of symptoms. Because conjunctival hemorrhage and punctuate corneal epithelial defects are risks with adenovirus infection, patients must be examined with a slit lamp. It is possible to obtain viral cultures, but as delayed culture results are unlikely to affect treatment, cultures are of limited value in the ED. If a pseudomembrane is present, remove it with wet cotton-tipped forceps.
The primary treatment of viral conjunctivitis is patient education and supportive care. Patients should be aware that viral conjunctivitis may worsen for the first 4 to 7 days from onset, and may take two weeks or longer to fully heal.23 Instruct parents to keep their children home from school until there is no more discharge. Instruct children and family not to share towels or clothing and to practice frequent hand washing. Artificial tears, cold compresses, and topical vasoconstrictors may provide symptomatic relief. Contact lens wearers should discontinue use until treatment is completed.
Because definitive diagnosis of a viral etiology may not be possible, many cases of conjunctivitis are appropriately managed with topical antibiotics, as described above. Specific medical management of viral conjunctivitis is limited. Cidofovir has been successful in some cases of adenoviral conjunctivitis, but some cases of toxicity have been reported.48 A povidone/iodine 0.4%/0.1% ophthalmic suspension may also be effective in treating adenoviral conjunctivitis, although more research is required.49 These drugs may be moderately effective in treating adenovirus infections, but there are few, if any, effective antivirals for other nonherpetic viral etiologies.45
Herpetic Viral Conjunctivitis. Herpes simplex virus (HSV) is another cause of viral conjunctivitis, and requires specific antiviral treatment. It should be considered as a possibility and excluded in cases that appear to be adenoviral conjunctivitis. Herpetic conjunctivitis presents with typical viral conjunctival signs and symptoms, such as red eye, itching, watery discharge, or enlarged preauricular nodes. Telltale features of HSV conjunctivitis that distinguish it from adenoviral conjunctivitis include pain, associated herpetic skin lesions, and the well-known dendritic corneal ulcer pattern. Although the classic dendritic ulcer pattern of HSV keratitis is not always visible, its presence can help to confirm the diagnosis. For this reason, fluorescein staining and slit-lamp examination should be performed. Diagnosis can be confirmed with a viral culture. HSV conjunctivitis often carries the risk of corneal ulceration or loss of vision. Because the diagnosis may be difficult in some cases, ophthalmology consultation is recommended.10
Common antiviral agents used to treat HSV conjunctivitis include topical acyclovir, trifluridine, valacyclovir, ganciclovir, or oral acyclovir.45,50 Topical combination agents (an antibiotic together with a corticosteroid) are not recommended due to risk of worsening existing bacterial ulcer or HSV keratitis.45,47 The fact that some cases of HSV conjunctivitis may be indistinguishable from adenoviral conjunctivitis warrants caution in the use of ophthalmic corticosteroids. Treatment should be initiated in conjunction with ophthalmologic consultation.
Keratitis. Keratitis refers to inflammation of the cornea. Keratitis may be infectious in etiology, and may co-exist with conjunctivitis as keratoconjunctivitis. Patients typically experience significant pain. Common etiologies include viral and bacterial pathogens. Topical antibiotic therapy is indicated with an agent to cover common bacterial pathogens. (See Table 3.) Concomitant iritis may cause significant pain and should be treated with cycloplegics, such as homatropine 2% drops (a single dose will last 24-72 hours). Viral keratitis should be treated in conjunction with ophthalmology consultation. Bacterial keratitis can be vision-threatening and also requires ophthalmologic consultation.
Endophthalmitis. Endophthalmitis is inflammation of the aqueous or vitreous humor of the eye, usually caused by infection. Endophthalmitis is rare in the pediatric population. Exogenous endophthalmitis results from direct inoculation by trauma or surgery, while endogenous endophthalmitis results from hematogenous spread. In pediatric patients, lethargy, unilateral eyelid swelling and erythema, conjunctival injection, and sometimes fever may occur.51 Hypopyon, an infection of the anterior chamber, may present as visible purulence layering in the anterior chamber. Common etiologic organisms include Staphylococcus aureus, streptococcal species, and other gram-positive and gram-negative organisms.52 As this is an ophthalmologic emergency with potentially devastating permanent effects on vision, ophthalmology should be consulted for diagnosis, admission, and surgical treatment of suspected endophthalmitis cases.53
Uveitis. Uveitis, sometimes known as intraocular inflammation, involves inflammation of the iris and ciliary body (with anterior uveitis) or the choroid (with posterior uveitis). Although it typically results from idiopathic or autoimmune causes, up to 13% of pediatric uveitis cases may result from infection, often from TORCH organisms (Toxoplasmosis, Other, (Syphilis), Rubella, Cytomegalovirus, and Herpes simplex virus).54 Anterior uveitis may be diagnosed in the ED. Patients with anterior uveitis may present with a wide range of complaints, typically, but not necessarily, including eye pain, conjunctival erythema, diminution of visual acuity, photophobia, and headache.27 Exclude glaucoma by measuring intraocular pressure. Scleral injection, cells in the anterior chamber, and flare help confirm the diagnosis of anterior uveitis. Although diagnosis of anterior uveitis is possible in the ED, diagnosis of intermediate or posterior uveitis remains difficult. For any cases of uveitis, ophthalmology should be consulted for diagnosis confirmation and treatment.53
Ophthalmia Neonatorum. Ophthalmia neonatorum (ON) refers specifically to conjunctivitis within the first four weeks of life.23 Infants are likely to develop conjunctivitis from different causes than older children, and may require different treatment therapies. The most frequent cause of ON is chemical conjunctivitis resulting from prophylactic silver nitrate drops, which occurs in 10% of neonates. Although silver nitrate has caused problems in the past, erythromycin ointment is more commonly used today and rarely causes chemical conjunctivitis. Chemical conjunctivitis in the neonate is typically mild, with bilateral hyperemia, mild inflammation, transient tearing, and little or no purulent discharge. This condition is self-limited and typically resolves without treatment in one to three days.
Figure 1. Differential Diagnosis of the Red Eye
Gonococcal ON. In neonates, the most critical organism to diagnose is Neisseria gonorrhoeae. The complications may be severe, as untreated gonococcal infection could result in corneal ulceration and, possibly, permanent loss of vision. Although previously the leading cause of blindness in the newborn period, recognition and treatment have reduced its incidence. The typical presentation of gonococcal ON includes bilateral purulent discharge, hyperemia, chemosis, and eyelid edema appearing in the first week after birth. (See Figure 2.) In some cases, symptoms may not appear until the second week of life.55 Obtain a Gram stain and culture to confirm suspected cases of gonococcal conjunctivitis, but when there is a high suspicion, laboratory results should not delay the prompt initiation of treatment.12
Figure 2. Gonococcal Ophthalmia Neonatorum
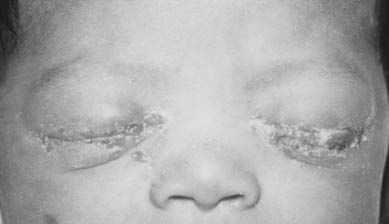
Reprinted from the Centers for Disease Control Public Health Image Library.
For cases of suspected gonococcal ON, an ophthalmology consult should be obtained immediately.12 Hospitalization and intravenous antibiotic therapy are indicated. Begin therapy with ceftriaxone or cefotaxime.54 Frequent eye irrigation with saline is important in removing purulent discharge and minimizing corneal inflammation. Test for concomitant infections, namely Chlamydia trachomatis and HSV. Until chlamydial cultures are negative, treat with oral erythromycin. This may treat existing chlamydial ON and help to prevent chlamydial pneumonitis.12 Topical treatment for gonococcal ON is unnecessary. Consider a full septic workup. Evaluate and treat the mother and her sexual contacts for gonorrhea and other sexually transmitted infections.24
Chlamydial ON. Chlamydia trachomatis is the most common cause of infectious ON. Symptoms include mucopurulent or purulent discharge, hyperemia, chemosis, and lid edema. Compared to gonococcal ON, chlamydial ON is less hyperacute, is less severe, and begins slightly later (at 5-10 days, compared to 2-7 days for N. gonorrhoeae infection).56 Diagnosis may be confirmed by positive identification of cytoplasmic inclusion bodies in the corneal epithelium, culture, direct immunofluorescence assay, ELISA, or PCR.6,10
Exclude other causes of conjunctivitis. Chlamydial ON generally does not require hospitalization.4 In infants, chlamydial conjunctivitis is accompanied by concomitant infection at other sites in more than 50% of cases. To prevent pneumonitis or other complications from chlamydial infection, systemic antibiotics are required. Oral erythromycin for at least 14 days is recommended.23 Treatment with sulfonamides is an alternative to erythromycin therapy. Close follow-up with the infant and outpatient evaluation of the mother and her sexual partners for STI are indicated. Although untreated cases may cause permanent scarring, chlamydial ON generally heals well with treatment.
Bacterial ON Nongonococcal, Nonchlamydial. Beyond N. gonorrhoeae and C. trachomatis infection, other bacterial etiologies of ON must be considered as well. H. influenzae, S. aureus, and S. pneumoniae are all common causes of bacterial ON and present with typical bacterial conjunctivitis symptoms, including red eye, lid edema, and purulent discharge. Because conjunctival infection from many different organisms can present with extremely similar symptoms, clinical evaluation is usually nondiagnostic. Gram stain and culture, with the possibility of other laboratory exams, are indicated to make a definitive diagnosis. Pseudomonas aeruginosa is rare but may lead to corneal ulceration and loss of vision. Pseudomonal ON may present with edema, erythema, discharge, pannus formation, or endophthalmitis. Gram-negative rods suggest the presence of Pseudomonas, and culture can confirm. If Pseudomonas is found, consult ophthalmology. Systemic and topical antibiotics will be required, and subconjunctival injections may be necessary as well. If Pseudomonas, gonococcus, and Chlamydia are all eliminated as possibilities, then infants with bacterial ON may receive the same outpatient treatment options as older children.24
Herpetic ON. In infants, any non-purulent conjunctivitis or keratitis should raise suspicion of HSV infection. Without treatment, 30-40% of infants with skin, eye, and mouth herpetic disease go on to develop neurological complications. With treatment, only 5% of infected infants develop neurological impairments.56 Herpetic conjunctivitis in the neonate typically occurs between one and two weeks after birth. Symptoms include a non-purulent conjunctivitis, vesicles on the skin or around the eyes, keratitis, or even cataracts.56 PCR or culture can confirm the diagnosis.
Neonates with confirmed HSV infection should receive systemic acyclovir for 2-3 weeks. They should also receive topical antibiotic therapy to prevent secondary bacterial infection. Good options include 1% trifluridine eye drops or 3% vidarabine ointment.4
References
1. Granet D. Allergic rhinoconjunctivitis and differential diagnosis of the red eye. Allergy Asthma Proc 2008;29:565-574.
2. Seth D, Khan FI. Causes and management of red eye in pediatric ophthalmology. Curr Allergy Asthma Rep 2011;11:212-219.
3. Silverman MA. Emergent treatment of acute conjunctivitis. Available at: http://emedicine.medscape.com/article/797874-overview. Accessed July 27, 2011.
4. Erogul M, Shah BR. Ophthalmology. In: Shah BR, Lucchesi M. Atlas of Pediatric Emergency Medicine. New York, NY: McGraw-Hill, Medical Publishing Division; 2006:361-403.
5. Cronau H, Kankanala RR, Mauger T. Diagnosis and management of red eye in primary care. Am Fam Physician 2010;81:137-144.
6. Handler JA, Ghezzi KI. General ophthalmologic examination. Emerg Med Clin North Am 1995;13:521-538.
7. Datner EM, Jolly T. Pediatric ophthalmology. Emerg Med Clin North Am 1995;13:669-679.
8. Ervin-Mulvey LD, Nelson LB, Freely DA. Pediatric eye trauma. Pediatric Clin North Am 1983;30:1167-1183.
9. Rimon A, Hoffer V, Prais D, et al. Periorbital cellulitis in the era of Haemophilus influenzae type B vaccine: Predisposing factors and etiologic agents in hospitalized children. J Pediatr Ophthalmol Strabismus 2008;45(5): 300-304.
10. Sethuraman U, Kamat D. The red eye: Evaluation and management. Clinical Pediatrics 2009;48(6):588-600.
11. Soon VT. Pediatric subperiosteal orbital abscess secondary to acute sinusitis: A 5-year review. Am J Otolaryngol 2011;32(1):62-68.
12. Prentiss KA, Dorfman DH. Pediatric ophthalmology in the emergency department. Emerg Med Clin N Am 2008:26; 181-198.
13. Rudloe TF, Harper MB, Prabu SP, et al. Acute periorbital infections: Who needs emergent imaging? Pediatrics 2010;125:e719-e726.
14. Osguthorpe JD, Hochman M. Inflammatory sinus diseases affecting the orbit. Otolaryngol Clin North Am 1993;26:657.
15 McKinley SH, Yen MT, Miller AM, et al. Microbiology of pediatric orbital cellulitis. Am J Ophthalmol 2007;144:497.
16 Agarwal M, Biswas J, Shanmugam MP: Retinoblastoma presenting as orbital cellulitis: Report of four cases with a review of the literature. Orbit 2004;23:93.
17. Preseptal (periorbital) and orbital cellulitis. UpToDate. Available at: http://www.uptodate.com/contents/preseptal-periorbital-and-orbital-celloulitis?source=search_results&selectedTitle=1%7E10#H1. Accessed July 27, 2011.
18. Starkey CR, Steele RW. Medical management of orbital cellulitis. Pediatr Infect Dis J 2001;20:1002-1005.
19. Goawalla A, Lee V. A prospective randomized treatment study comparing three treatment options for chalazia: Triamcinolone acetonide injections, incision and curettage and treatment with hot compresses. Clinical and Experimental Ophthalmology 2007;35:706-712.
20. Gupta N, Dhawan A, Beri S, et al. Clinical spectrum of pediatric blepharokeratoconjunctivitis. J Am Assoc Peditaric Ophthalmol Strabismus 2010;14:527-529.
21. Torkildsen GL, Cockrum P, Meier E, et al. Evaluation of clinical efficacy and safety of tobramycin/dexamethasone ophthalmic suspension 0.3%/0.05% compared to azithromycin ophthalmic solution 1% in the treatment of moderate to severe acute blepharitis/blepharoconjunctivitis. Curr Med Res Opin 2011;27:171-178.
22. Buznach N, Dagan R, Greenburg D. Clinical and bacterial characteristics of acute bacterial conjunctivitis in children in the antibiotic resistance era. Pediatr Infect Dis J 2005;24:823-828.
23. Richards A, Guzman-Cottrill JA. Conjunctivitis. Pediatrics in Review 2010:31;196-208.
24. Teoh DL, Reynolds S. Diagnosis and management of pediatric conjunctivitis. Pediatr Emerg Care 2003;19:48-55.
25. Smith AF, Waycaster C. Estimate of the direct and indirect annual cost of bacterial conjunctivitis in the United States. BMC Ophthalmol 2009;9:13.
26. Visscher KL, Hutnik CML, Thomas M. Evidence-based treatment of acute infective conjunctivitis. Can Fam Physician 2009;55:1071-1075.
27. Mueller JB, McStay CM. Ocular infection and inflammation. Emerg Med Clin N Am 2008;26:57-72.
28. Everitt HA, Little PS, Smith PW. A randomized controlled trial of management strategies for acute infective conjunctivitis in general practice. BMJ 2006;333:321.
29. Cavuoto K, Zutshi D, Karp CL, et al. Update on bacterial conjunctivitis in South Florida. Ophthalmology 2008;115:51-56.
30. Chang MH, Fung HB. Besifloxacin: A topical fluoroquinolone for the treatment of bacterial conjunctivitis. Clin Ther 2010;32:454-471.
31. Carter NJ, Scott LJ. Besifloxacin ophthalmic suspension 0.6%. Drugs 2010;70: 83-97.
32. Karpecki P, Depaolis M, Hunter JA. Besifloxacin ophthalmic suspension 0.6% in patients with bacterial conjunctivitis: A multicenter, prospective, randomized, double-masked, vehicle-controlled, 5-day efficacy and safety study. Clin Ther 2009;31:514-526.
33. Denis F, Chaumeil C, Goldschmidt P, et al. Microbiological efficacy of 3-day treatment with azithromycin 1.5% eye-drops for purulent bacterial conjunctivitis. Eur J Ophthalmol 2008;18:858-868.
34. Bremond-Gignac D, Mariani-Kurkdjian P, Beresniak A, et al. Efficacy and safety of azithromycin 1.5% eye drops for purulent bacterial conjunctivitis in pediatric patients. Pediatr Infect Dis J 2010;29:222-226.
35. Granet DB, Dorfman M, Stroman D, et al. A multicenter comparison of polymyxin B sulfate/trimethoprim ophthalmic solution and moxifloxacin in the speed of clinical efficacy for the treatment of bacterial conjunctivitis. J Pediatric Ophthalmol Strabismus 2008;45:340-349.
36. Granet D, Lichtenstein SJ, Onofrey B, et al. An assessment of the tolerability of moxifloxacin 0.5% compared to azithromycin 1.0% in DuraSite. Clin Ophthalmol 2007;1:519-525.
37. Szaflik J, Szaflik JP, Kaminska A. Clinical and microbiological efficacy of levofloxacin administered three times a day for the treatment of bacterial conjunctivitis. Eur J Ophthalmol 2009;19:1-9.
38. Lichtenstein SJ, Rinehart M. Efficacy and safety of 0.5% levofloxacin ophthalmic solution for the treatment of bacterial conjunctivitis in pediatric patients. J AAPOS 2003;7:317-324.
39. Drugs for some common eye disorders. Treatment Guidelines from the Medical Letter. 2010;8(89):1-8.
40. Ophthalmic azithromycin. Med Lett 2008;1279:11.
41. Bacterial conjunctivitis. Emedicine/Medscape. Available at: http://emedicine.medscape.com/article/1191730-medication#2. Accessed July 27, 2011
42. Gold RS. Treatment of bacterial conjunctivitis in children. Pediatric Annals 2011;40:95-105.
43. Tarabishy AB, Jeng BH. Bacterial conjunctivitis: A review for internists. Cleve Clin J Med 2008;75:507-512.
44. Magauran B. Conditions requiring emergency ophthalmologic consultation. Emerg Med Clin N Am 2008;26: 233-238.
45. Skevaki CL, Galani IE, Pararas MV, et al. Treatment of Viral Conjunctivitis with Antiviral Drugs. Drugs 2011;71:331-347.
46. Meltzer JA, Kunkov S, Crain EF. Identifying children at low risk for bacterial conjunctivitis. Arch Pediatr Adolesc Med 2010;164:263-267.
47. O'Brien TP, Jeng BH, McDonald M, et al. Acute conjunctivitis: Truth and misconceptions. Curr Med Research and Opinions 2009;25:1953-1961.
48. Skevaki CL, Galani IE, Pararas MV, et al. Treatment of viral conjunctivitis with antiviral drugs. Drugs 2011;71:331-347.
49. Pelletier JS, Stewart K, Trattler W, et al. A combination povidone-iodine 0.4%/dexamethasone 0.1% ophthalmic suspension in the treatment of adenoviral conjunctivitis. Adv Ther 2009;26(8):776-83.
50. Wilhelmus KR. Therapeutic interventions for herpes simplex virus epithelial keratitis. Cochrane Database Syst Rev 2008; CD002898.
51. Wagner RS. Complications of strabismus surgery. In: Wilson M, Saunders RA, Trivedi RH. Pediatric Ophthalmology: Current Thought and Practical Considerations. Berlin: Springer-Verlag; 2009:227-241.
52. Han DP, Wisniewski SR, Wilson LA, et al. Spectrum of susceptibilities of microbiologic isolates in the Endophthalmitis Vitrectomy Study. Am J Ophthalmol 1996;122:1.
53. Magauran B. Conditions requiring emergency ophthalmologic consultation. Emerg Med Clin N Am 2008;26: 233-238.
54. Madigan WP, Raymond WR, Wroblewski KJ, et al. A review of pediatric uveitis: Part I. Infectious causes and the masquerade syndromes. J Pediatr Ophthalmol Strabismus 2008;45:140-149.
55. MacDonald N, Mailman T, Desai S. Gonococcal infections in newborns and in adolescents. Adv Exp Med Biol 2008;609:108-130.
56. Kimberlin DW, Lin CY, Jacobs RF, et al. Natural history of neonatal herpes simplex virus infections in the acyclovir era. Pediatrics 2001;108:223-229.
Eye infections are common among emergency department (ED) pediatric patients and can lead to significant morbidity if not properly managed.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
