Legal Drugs of Abuse
Legal Drugs of Abuse
Authors:
Dan Quan, DO, Maricopa Medical Center, Department of Emergency Medicine, Division of Toxicology, Phoenix, AZ.
Daniel Haase, MD, Maricopa Medical Center, Emergency Medicine Residency, Phoenix, AZ.
Rachel Levitan, MD, Maricopa Medical Center, Emergency Medicine Residency, Phoenix, AZ.
Peer Reviewer:
Karen N. Hansen, MD, FACEP, Assistant Professor of Emergency Medicine, University of Maryland School of Medicine.
This issue might be subtitled "What will they think of next?" Getting high does not always require the purchase of illegal drugs, and all substances that alter sensorium, such as nutmeg, cannot be regulated. However, the emergency physician must remain aware of the latest fads of drug abuse, and should be able to recognize the symptoms they cause. Currently, those drugs are K2, Spice, "bath salts," and "plant food," along with some recycled favorites from the past nutmeg and canned air. Luckily, most of these cause time-limited changes in sensorium without major physiologic effects. Sedation and time generally are all that is needed for emergency treatment.
Sandra M. Schneider, MD, FACEP, Editor
Introduction
Drugs of abuse are all too commonly seen in the emergency department (ED), no matter where your practice is located. Most emergency physicians are comfortable dealing with alcohol intoxication, methamphetamine, cocaine, heroin, and other common "street drugs." This paper will discuss other common drugs that are perhaps less well known and considered "legal." We will present five different drugs, including synthetic tetrahydrocannabinol (THC), "bath salts," salvia, nutmeg, and canned air cleaners. Management of the intoxicants is discussed at the end.
Case 1
A 20-year-old college student is brought into the ED by his friend because the patient started to not feel well after smoking something at a party. The patient's friends state that they do not know what it was but it was legal. The patient's vital signs are: heart rate of 114 beats per minute; respiratory rate of 16 breaths per minute; blood pressure of 148/89 mmHg; oxygen saturation of 98% on room air; and an oral temperature of 37.2°C. He appears somewhat anxious and is mildly tremulous. He does not appear to be in any acute distress, but he is somewhat confused. He states he is slightly nauseated and feels his heart beating. He denies any visual disturbances, hallucinations, or pain. His physical examination is unremarkable.
The patient is placed on a cardiac monitor. One liter of IV 0.9% normal saline and 4 mg of IV ondansetron are administered. Laboratory tests are remarkable for a mild leukocytosis without an increase in bands, and a mildly elevated BUN/creatinine ratio. The chemistry panel, urine drug screen, ethanol, acetaminophen, and salicylate tests are negative. An ECG shows sinus tachycardia without any ST or T-wave abnormalities. QRS complexes are narrow, and QTc is within normal limits.
Two hours after presentation, the patient states that he wants to go home. He is alert, oriented, and no longer tremulous or anxious. His discharge vital signs have returned to normal. One of his friends is in the ED and is willing to take him home. The friend states that they were smoking "Spice."
Pathophysiology and Pharmacology
Tetrahydrocannabinol, or THC, is the principle active ingredient in marijuana. It is well known for its classic effects of relaxation, euphoria, and analgesia. It is also frequently used for its anti-emetic properties, which is the basis for its legal use in multiple U.S. states. However, in individuals who are naïve to THC, the opposite effects of anxiety, tachycardia, and nausea are often seen. There is a substantial amount of literature suggesting that heavy and chronic marijuana usage is associated with psychosis and schizophrenia.1,2
JWH-018 is probably the most studied synthetic cannabinoid. It has been found in multiple preparations and has been shown to be a potent cannabinoid receptor (CB) agonist.3 CB1 is the principal receptor thought to be most highly responsible for the euphoria and psychoactive effects of THC. The CB2 receptor resides mostly in the immune system but has some effect on pain control and mood regulation.1
Most individuals who smoke a synthetic cannabinoid typically do not present to the ED and report symptoms consistent with classic THC effects.2 However, there is an increased rate of adverse reactions associated with synthetic cannabinoids, as evidenced by the new phenomenon of patients presenting to the emergency department with synthetic cannabinoid intoxication. While reliable pharmacokinetic data do not exist on all the specific synthetic cannabinoids, clinical data in case reports suggest that adverse effects typically occur within 30 minutes, wane within 3-4 hours, and completely disappear by 6 hours.2,4-6
Clinical Features
Symptoms described with synthetic marijuana use are elevated heart rate, elevated blood pressure, palpitations, diaphoresis, tremulousness, anxiety, and agitation.4,5,7,8 Other physical findings may include mydriasis, although this finding is not consistent with intoxication. Psychosis with auditory and visual hallucinations is mentioned in rare circumstances, most commonly with individuals who have underlying psychiatric disorders.9,10 Seldom have seizures and arrhythmias been reported.1,2
Diagnostic Studies
Because the toxidrome of synthetic cannabinoid intoxication may be similar to that of sympathomimetic substances, a full toxicologic workup may be warranted, especially if the patient presents with severe alterations of vital signs, changes in mental status, or cannot give a history of synthetic cannabinoid use. Hypokalemia has been reported by some case reports4, but it is not a consistent finding across the literature in patients presenting with synthetic cannabinoid intoxication.4,5
Although there are structural similarities between synthetic marijuana and THC, commonly used urine drug screens are unable to detect the presence of synthetic cannabinoids in the urine. It is important to note that urine drug screens may be positive for THC weeks after use, and a positive test does not exclude the use of synthetic cannabinoids.11 Currently, there is no emergency department test that can confirm intoxication with synthetic cannabinoids and further testing is not useful in the acute management.
Differential Diagnosis
In patients who present with severe synthetic cannabinoid intoxication, sympathomimetic intoxication should be considered, especially in those patients with abnormal vital signs. Sympathomimetic substance intoxication with methamphetamines, "bath salts," cocaine, ecstasy, etc., should be considered. In individuals presenting with psychosis, phencyclidine (PCP) intoxication should also be entertained.
Adulterated marijuana or synthetic THC should be considered in the differential diagnosis. PCP can be dissolved into a solvent and then allowed to permeate a marijuana cigarette (known as "Sherm"). Patients with PCP-laced marijuana will frequently present with symptoms of psychosis, agitation, and violent behavior. Typically, patients who are intoxicated with PCP alone do not necessarily have elevated heart rate or blood pressure; however, the psychomotor agitation associated with PCP intoxication can secondarily promote both tachycardia and hypertension. Cocaine-adulterated marijuana use, called "dusting" or "snow-capping," may present with similar symptoms. Both PCP and cocaine may be detected in some urine drug screens.
Background and Epidemiology
Synthetic cannabinoids, more popularly known as "K2" or "Spice," have become a new phenomenon in the United States within the last 18 months. Synthetic marijuana analogues first became available in the United States in 2006, but did not start becoming a widespread "legal" drug of abuse until early 2010.
According to the American Association of Poison Control Centers (AAPCC), there were 13 calls to poison centers in 2009 regarding exposure to synthetic cannabinoids, but in 2010 there were 2,915 documented calls.12 As of May 31, 2011, there were already 2,476 calls to poison centers regarding synthetic cannabinoid exposure.7
The widespread availability of the drug is one of the most concerning aspects in this new drug of abuse. Because synthetic cannabinoids are marketed as incense or potpourri, they have been sold virtually everywhere. The statement, "not intended for human consumption," is printed on these products so the products avoid Food and Drug Administration (FDA) regulation. Ubiquitous in head shops and tobacco shops, synthetic marijuana has been sold in gas stations, convenience stores, and even grocery stores.
Synthetic cannabinoids obtained the mainstream media's attention in June 2010 after an Iowa teenager with no past medical history of depression or other psychiatric illness committed suicide while intoxicated with K2. According to the police investigation, the teenager began to "freak out," according to his friends. Next, he got his parents' rifle and shot himself in the head, ending his life.13 Later, investigations suggested the patient might have had an underlying depression. Iowa, as well as several other states, went on to pass bans of synthetic cannabinoids.
In November 2010, the Drug Enforcement Agency (DEA) placed a 12-month ban on the sale of products containing five of the most prevalent synthetic THC analogues: JWH-018, JWH-073, JWH-200, CP-47,497, and cannabicyclohexanol. The ban took effect on March 1, 2011. The DEA news release bans the substances, "for at least one year while the DEA and the United States Department of Health and Human Services (DHHS) further study whether these chemicals and products should be permanently controlled."8
During the one-year ban, these compounds will be restricted as schedule I substances, which are highly abused and serve no medical benefit. The DEA also has the option to extend their emergency ban up to an additional six months while studying whether or not to permanently ban the substances.
Despite the aggressive DEA ban, new synthetic cannabinoids have already been popping up on the Internet. Because the DEA only bans five distinct substances, new cannabinoid analogs circumvent the ban by altering the original molecular make-up of JWH-018. The exact structure of these new compounds has not been detailed.14
In Germany, a new synthetic cannabinoid, JWH-122, has been isolated. Marketed as "Lava Red," side effects of elevated heart rate, blood pressure, agitation, and psychosis have been noted.15 Even more concerning, seizures, cardiac arrhythmias, and loss of consciousness requiring intubation have been reported with this drug, though rarely.16 JWH-122 has been shown to be a very potent cannabinoid (CB) receptor agonist and is similar in structure to its parent compound, JWH-018.15 This suggests that even minor alterations in the chemical structure can have profound changes in clinical effect. While chemists attempt to avoid the restrictions of governmental agencies, they are creating potentially hazardous, and even lethal, new compounds.
Most of the brands of synthetic cannabinoids have a variety of scents or flavors available. There is also considerable concern that the additives to the synthetic cannabinoids may be, at least in some part, responsible for the variability in side effects seen with these products. These additives are not listed on the packages because they are labeled as "not for human consumption."
Case 2
Staff and hospital security are wrestling with a man who is yelling, swearing, agitated, and combative. He appears to be delusional. He has a heart rate of 125 beats per minute, a blood pressure of 160/100 mmHg, a respiratory rate of 22, oxygen saturation of 96% on room air, and temperature of 38.2°C. IV access is established, and the patient is placed on a cardiac monitor including continuous pulse oximetry. He is sedated with benzodiazepines and is given IV fluids. Both rapid blood glucose and ECG are normal. The basic blood work, serum alcohol level, acetaminophen level, aspirin level, urinalysis, and urine drug screen are unremarkable. After several hours, he is calm. You can carry out a reasonable conversation, and he admits to snorting and injecting "bath salts" with his friends.
Pathophysiology and Pharmacology
These products known as "bath salts" or "plant food" contain stimulant compounds such as 3,4-methylenedioxypyrovalerone (MDPV) or 4-methylmethcathinone (mephedrone). The products are being ingested, snorted, and injected.
Figure 1: Chemical Structure of THC and Synthetic Analogues
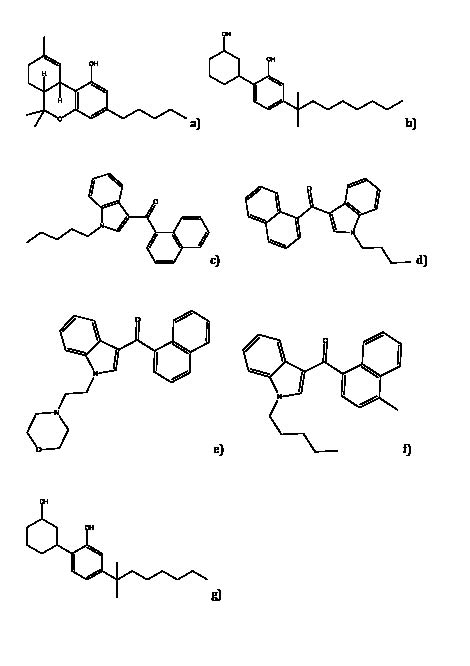
a) THC b) Cannabicyclohexanol c) JWH-018 d) JWH-073 e) JWH-200 f) JWH-122 g) CP-47,497
Bath salts are structurally similar to cathinones. (See Figure 2.) There are multiple synthetic derivatives of cathinones. One of the longest known and most studied compounds in this class comes from the Khat (quat or gat) (Catha edulis) shrub that grows in eastern and central Africa. This plant has long been used by native people for its stimulant properties. The fresh leaves or stems are chewed or brewed into tea. The plant releases cathinones and the less toxic cathines, which are used to boost energy and suppress appetite. It is believed that cathinones act by inhibiting monamine transporters for dopamine, serotonin, and norepinephrine within the central nervous system (CNS).17-20 Cathinone and its derivative compound cathine are controlled substances in the United States (Schedule I and IV, respectively).20 Cathinones are similar to amphetamine in chemical appearance and clinical effects.
Figure 2: Chemical Structures
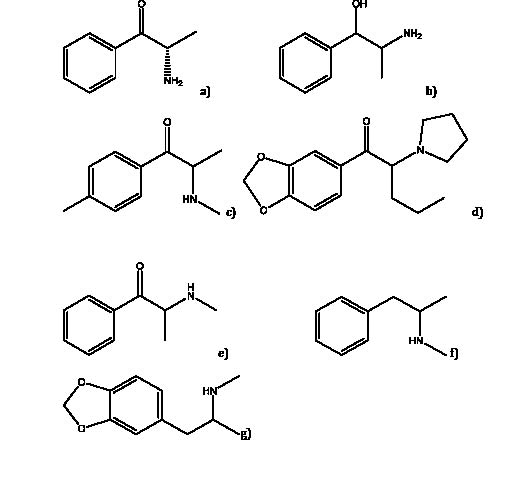
Chemical structures of a) cathinone b) cathine c) mephedrone d) MDPV e) methcathinone f) methamphetamine g) MDMA.
Although human studies with mephedrone are limited, rat studies showed a relationship between 3,4-methylenedioxymethamphetamine (MDMA or ecstasy), mephedrone, and amphetamines. This study looked at the effects of mephedrone on the nucleus accumbens of rats. It was found that mephedrone had similar neurochemical and functional properties to MDMA. Both chemicals caused a rapid increase in serotonin levels. There was a similar effect in dopamine release and elimination from mephedrone that resembled that of amphetamines. Mephedrone appears to have properties of both MDMA and amphetamine on the brain's reward system, which may account for its use as a designer drug of abuse.21
Clinical Features
The clinical presentation of this ingestion is similar to other stimulant/sympathomimetic compounds. The patient's clinical presentation is most consistent with methamphetamine or cocaine intoxication: Hypertension, tachycardia, hyperthermia, agitation, tremor, seizure, delusions, hallucinations, paranoia, and mydriasis may occur. There is no readily available test that detects bath salt intoxications. Standard ED urine drug screens do not detect its use.
Differential Diagnosis
Patients presenting with bath salt ingestion will appear to have a sympathomimetic intoxication. The differential diagnosis should include methamphetamines, cocaine, ecstasy, PCP, and others. Co-ingestion or multidrug abuse should also be considered.
Background and Epidemiology
Bath salts conjure up an image of a luxurious bathtub overflowing with bubbles, aromatherapy, perhaps a glass of wine, and relaxation. The term "bath salts" now has a much more sinister connotation. These "bath salts" are not sold in expensive packaging from bath and beauty supply stores as inorganic salts used for bathing. Bath salts containing mephedrone and other related compounds now connote a new sort of designer drug of abuse. Sold as "bath salts" or "plant food" and labeled "not for human consumption," this new type of designer drug can be bought at grow shops, head shops, convenience stores, gas stations, and online for recreational drug use. They are sold under such names as "Vanilla Sky," "Ivory Wave," and many others.22,23
Bath salts first made their appearance as a designer drug of abuse in the end of the first decade of the 21st century in Western Europe. The first case of confirmed toxicity associated with mephedrone use comes from the United Kingdom in 2010.24 A 22-year-old man ingested and injected 4 g of mephedrone powder and then presented to a U.K. emergency department with palpitations, blurred vision, chest pressure, diaphoresis, anxiety, and delusions of mercury poisoning. He was tachycardic and hypertensive on presentation. His physical examination and labs, including mercury level, were otherwise normal. He was treated with benzodiazepines and discharged. Liquid chromatography and mass spectrometric detection were used on a serum sample and revealed mephedrone. Gas chromatography/mass spectroscopy (GC/MS) toxicology screen did not reveal any other drugs of abuse.24
Bath salts also have been reported to cause a number of fatalities. Four deaths related to mephedrone were reported in April 2011 in the United Kingdom.25 In this case series, four fatalities were linked to mephedrone by femoral venous blood analysis using high-performance liquid chromatography (HPLC). Each of the four patients was found to have levels of mephedrone on autopsy. One case involved a 49-year-old woman who inhaled some of the drug and was found dead, with coronary artery disease and myocardial fibrosis being a contributing cause of death. A second case involved a 19-year-old man who suffered cardiopulmonary arrest after using mephedrone. A third case involved a 55-year-old woman who was found dead after a night of drug use. A fourth case involved a 17-year-old boy who was involved in a fatal motor vehicle collision after being high on mephedrone.25
MDPV has also been used as a designer drug of abuse. It has also been found in patients who have ingested bath salts.26 It is not licensed for medical use in the United States.27 In Finland, it has been a drug of abuse and concern since 2008. Since the autumn of 2009, blood screens of intoxicated drivers have included an assay for MDPV, which has been found to be positive in 5.7% of intoxicated drivers (not alcohol only) both alone and in combination of other substances of abuse.28
Methcathinone is another synthetic derivative of cathinone. It was first seen in Russia and the former Soviet Union in the late 1980s and 1990s. Several cases of methcathinone (otherwise known as "Cat") toxicity were reported in the rural Midwest in the early 1990s. These patients presented in a similar fashion, with a sympathomimetic toxidrome of agitation and hallucinations.29
Bath salts were first described in a published article as a drug of abuse in the United States in May 2011. A Michigan ED reported a case series of 35 patients from November 13, 2010 to March 31, 2011. During this period, many cases were reported and presented to the local emergency department with symptoms consistent with bath salt intoxication. One death was reported.26
The American Association of Poison Centers released its first clinical statement on these toxins in December 2010.30 Recent preliminary Poison Center data show 303 calls in 2010 and already 3,740 calls as of July 7, 2011, in regard to bath salts.31
Several states are taking a stand and passing legislature to make bath salts illegal. Governor Bobby Jindal of Louisiana was one of the first to make the sale of these drugs illegal.32 Many other states, including Illinois and Florida, are taking similar steps to regulate these substances. The DEA has listed bath salts as a drug of concern. It is currently under investigation.33
Case 3
A 21-year-old man presents to the ED for hallucinations. His girlfriend states that the patient smoked "Seer's sage" approximately 15 minutes prior to arrival. She says he smoked it in the past, but his hallucinations are worse today. He is having a "bad trip" and "demons are trying to get him."
The patient's vital signs are a heart rate of 105 beats per minute, respiratory rate of 16 breaths per minute, blood pressure of 127/79 mmHg, oxygen saturation of 98% on room air, and an oral temperature of 37.2°C.
By the time you see the patient, he is calm, lying in bed, and requesting to go home. He is alert and oriented, and he denies visual or auditory hallucinations. He has not had a "trip" like that before, and he denies any other co-intoxicants. After a period of observation, the patient is discharged home.
Pharmacology and Pharmacokinetics
The principle psychoactive ingredient in Salvia divinorum is salvinorin A, a molecule that was first isolated in the early 1980s. Its exact mechanism of action was not well understood until 2002, well after it became commercially available. Salvia acts as a K-opioid receptor agonist, as opposed to the serotonin or 5-HT receptor, which is the main receptor targeted by classic hallucinogens such as lysergic acid diethylamide (LSD) and mescaline. The K-opioid receptor is widely distributed throughout the brain, spinal cord, and peripheral nerves. K-opioid agonists typically cause dissociation and delirium. It also appears that salvinorin A has significant dopamine (D2) receptor action, similar to LSD and mescaline.34
The most interesting aspect of salvinorin A pharmacology is its short duration of action. When smoking salvia, the onset of action is virtually immediate, with the duration of action typically cited between 20-30 minutes. There is mild variation depending on whether it is smoked or if the vaporized salvia was extract, leaf, or pure salvinorin A. Hallucinogens, such as LSD, can cause "trips" that last 6-12 hours depending on quantity consumed and the patient's tolerance. Mescaline's effect can last 12 hours or more.35-37
The preferred route of salvia administration is inhalation or vaporization. It is rarely chewed and swallowed because of the gastrointestinal deactivation of salvinorin A.38
Clinical Effects
Salvia is principally abused for its hallucinogenic and psychogenic effects. In one survey, the most frequent effects were "increased insight," "improved mood," "calmness," "increased connection with the universe or nature," "weird thoughts," and "things seeming unreal." Approximately 93% of those who responded to the survey reported smoking or vaporizing as forms of abuse, with a minority masticating the leaves. The majority used concentrated leaf extract as opposed to dried leaves. A very small percentage use pure salvinorin A (1.3%).36
The most commonly cited adverse reactions include "increased swelling," "lightheadedness," "drowsiness," "dizziness," and "lack of coordination," with almost all being noted about 20% of the time.36
Background and Epidemiology
Salvia divinorum, more frequently referred to as salvia, the plant's genus name, is known for its psychoactive and dissociative effects. It also carries the street names "Seer's Sage," "Diviner' Sage," "hierba Maria," and "SD." Salvia was originally used by the Mazatec Indians in the Sierra Mazatec Oaxaca, Mexico. Predominantly used by the Mazatec shamans to help produce visions during religious ceremonies, the plant has become an increasingly popular legal drug of abuse during the past decade.39
Figure 3: Chemical Structures of Salvinorin A, LSD, Mescaline
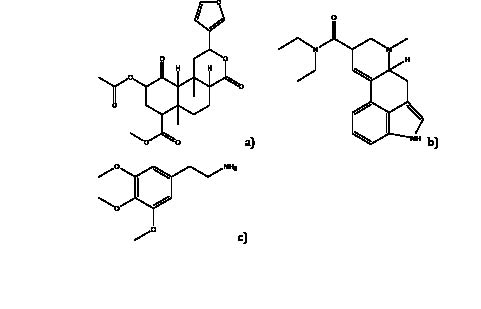
Chemical structure of a) salvinorin A b) LSD c) mescaline
Salvia became commercially available in the late 1990s, mostly available through Internet sales. Since that time, the substance has been banned by about a dozen U.S. states, but has managed to escape federal regulation by the DEA. Salvia divinorum is a controlled substance in multiple European countries, and recently became regulated in Canada in early 2011.40
Results from the 2006 National Survey on Drug Use and Health, a survey sponsored by the Substance Abuse and Mental Health Services Administration, suggest that 1.2 million Americans have tried salvia during their lifetime, with approximately 750,000 individuals having used it that year.41 The 2009 survey did not specifically address salvia use, but based on increased media attention and governmental legislation, some have estimated the number of individuals using salvia well into the millions per year.42
Case 4
A 19-year-old woman is brought from the local college campus by EMS with altered mental status. They state that she is nauseated and acting "bizarre." On arrival, her vital signs are: heart rate of 128 beats per minute, blood pressure of 108/68, respiratory rate of 20 breaths per minute, oxygen saturation of 98% on room air, and a temperature of 36°C. She feels like she is "soaring" but is very anxious. She has paresthesias and feels like she needs to urinate but is unable to do so. On physical examination, she is altered, her face is mildly flushed, her mouth is dry, and she is gagging. Her pupils are 4 mm and sluggishly reactive. She has mild ataxia. An IV is established with a normal saline infusion. The basic laboratory results include CBC, basic metabolic panel, beta-hCG, urinalysis, urine drug screen, ethanol, aspirin and acetaminophen levels are all normal. An ECG is unremarkable. She receives an antiemetic and a benzodiazepine for anxiolysis. She admits to ingesting three whole nutmeg ground into a milkshake to obtain a "fresh, safe, natural high."
Pharmacology and Pharmacokinetics
Nutmeg oil may be extracted from the nut of the evergreen tree Myristica fragrans. Clinical intoxication is usually seen after ingestion of 1-3 whole nuts (5-15 g) or 1-2 tablespoons (7-14 g) of ground nutmeg.43 (See Figure 4.) A single jar contains approximately 75 g of nutmeg.44 The spice is commonly mixed in other liquids, such as beer or juice, and ingested as a drink. There are reports of people injecting or inhaling nutmeg. Nutmeg contains approximately 5-15% volatile oils. These oils are considered to be the primary component leading to toxic effects. It is widely believed that myristicin and elemicin, alkylbenzene derivatives, are the toxicologically active compounds.45,46 Myristicin has been shown to inhibit monoamine oxidase and is thought to be converted to the amphetamine derivative 3-methoxy-4,5-methylene dioxyamphetamine, leading to its clinical effects. Elemicin is thought to have anticholinergic and psychotropic properties. The combination of these effects leads to hallucinations, an anticholinergic-type toxicity, and other variable symptoms.43-48 There is a case report of one patient who developed non-specific T-wave changes on his ECG, which resolved once intoxication resolved.49
Figure 4: Whole Nutmeg and Ground Nutmeg

Clinical Effects
Nutmeg intoxication may appear clinically as feelings of euphoria, hallucinations, paranoia, fatigue, tachycardia, nausea, vomiting, nonspecific neurologic complaints, or other alterations. Many patients will complain of dry mouth. There are a large number of patients who report a feeling of "soaring" or other types of movement hallucinations.
Background and Epidemiology
Nutmeg is typically used for flavoring in fresh-baked breads, pies, or cookies. Nutmeg is not something that immediately comes to mind when thinking about drug abuse. However, using the spice as a drug is not a novel use for this compound. Nutmeg has been used to treat stomach and skin ailments, to induce hallucinations, and as an abortifactant since the Middle Ages.43 Many case reports of nutmeg intoxication are in the literature scattered throughout the past 200 years. There are intervals of time when it is more abundant, such as during the 1960s and 1970s. Certain demographic groups are more predisposed to present with nutmeg intoxication, including adolescents, college students, and prisoners. Reasons for this include the low cost and availability of nutmeg.
Nutmeg intoxication, while not new, is certainly not common. An 11-year retrospective review of the California Poison Center revealed only 119 single-substance exposures to nutmeg.50 A review of calls placed to the Poison Information Center of Erfurt revealed that seven cases of nutmeg intoxication were reported from 1996-1998, with no cases reported from 1994-1995.45 One reason for the low number of reports may include ingestion of a large amount of fairly non-palatable substance in order to have the psychotropic and hallucinogenic effects. The "high" is variable, with significant negative side effects.
There have been two fatalities from nutmeg reported in the literature. The first case is from 1887 and involved an 8-year-old boy who is reported to have ingested two nutmegs and was found altered. He died approximately 24 hours later. Whether the death was from nutmeg ingestion or other causes (such as the treatment with injection of ammonia, brandy, and other compounds) is unclear.46,51 A more recent fatality was reported in Germany in 2000. In this case, myristicin (4 µg/mL) was detected in serum during a post-mortem examination of a 55-year-old woman. A nutmeg-like smell was noted on the autopsy examination of the stomach contents, so a myristicin level was ordered. The concentration was twice as high as previously reported. It was concluded that nutmeg ingestion, along with flunitrazepam, contributed to her death.45
Case 5
A concerned parent brings his 13-year-old son to the ED. He has been acting "funny" since his father got home about one hour ago. The patient is complaining of an abnormal sensation in his chest, as well as palpitations. Since arriving 10 minutes ago, the boy has returned to his baseline mental status. Vital signs are as follows: heart rate 106 beats per minute, blood pressure 114/68 mmHg, respiratory rate of 16, temperature 36.8°C, and oxygen saturation of 97% on room air. He is placed on a monitor, an IV is established with a liter bolus of normal saline, and laboratory testing is obtained. An ECG shows a prolonged QTc of 495 milliseconds. The laboratory work is normal. The urine drug screen is negative. The patient's mother arrives, bringing a can of generic "compressed dust remover" for computer keyboards. She found the can underneath the patient's bed.
Pathophysiology and Pharmacology
It is believed that inhalation of volatile hydrocarbons, such as the common component of canned air, 1,1-difluoroethane, exert their clinical effects via stimulation of gamma-aminobutyric acid (GABA) receptor complexes. The enhanced GABA receptor increases chloride permeability, which leads to hyperpolarization of the cell membrane and then inhibits excitability. This is similar to the way ethanol inhibits GABA. This effect explains why patients who are high on inhalants may also appear to be drunk. It is thought that inhaled hydrocarbons inhibit N-methyl-D-aspartate (NMDA) receptors and interfere with glutamate-mediated excitatory neurotransmission.52,53
One of the most feared complications of inhalant abuse is called "sudden sniffing death."54 This is an acute, fatal cardiotoxicity associated with hydrocarbon inhalation. Sudden death occurs immediately after use of the compound and the onset of physical activity or stress. Witnessed examples of this phenomenon include running away after abuse with the shock of being caught by parents or police. Hydrocarbon inhalation sensitizes the myocardium by blocking potassium current and prolonging repolarization. Sudden activity or a catecholamine surge produces a fatal dysrhythmia.55
Clinical Effects
Patients may present to the ED with signs and symptoms of alcohol intoxication with primarily CNS effects such as euphoria, giddiness, agitation, ataxia, and dizziness. Hypoxic injury and respiratory arrest may occur when the patient abuses inhalants in a closed space where oxygen is displaced with CO2 and the volatile substance. Occasionally, evidence of what was ingested may be seen around the mouth and on mucus membranes, such as in the case of inhaled spray paint. There may be signs of mucosal irritation such as sneezing, tearing, etc. Frostbite may occur on the fingertips and lips from the container, which chills as it empties.
Cardiac complaints such as palpations may present with dysrhythmias from premature beats, atrial fibrillation, and supraventricular tachycardia. Cardiac arrest can occur in those with sudden sniffing death.
Long-term inhalant abusers may develop long-term sequelae, including liver and kidney disease. Chronic solvent abusers have been found to have significantly more brain abnormalities on MRI than abusers of other drugs such as cocaine.54
Continuous cardiac monitoring is of utmost importance in these patients. Obtaining a chest X-ray is worthwhile because an ARDS-like lung injury or aspiration pneumonitis may develop. Avoid a noisy environment and sympathetic stimulation to reduce the risk for sudden sniffing death. Patients should be monitored for a few hours in the ED with oxygen therapy until their symptoms resolve.
Background and Epidemiology
Inhalant abuse is recreational exposure to inhaled vapors to obtain a sensation of being high.56 Many compounds can be inhaled to obtain a high, such as spray paint and gasoline. One item commonly abused is computer keyboard cleaner that contains a halogenated hydrocarbon, difluoroethane. (See Figure 5.) Many reports in the mainstream media have discussed the dangers of inhaling these types of compounds. Inhalation abuse can take several forms: "sniffing" or "snorting" fumes from their containers; spraying the aerosol directly into one's nose or mouth; "bagging," which is inhaling fumes of a substance that is sprayed into a plastic or paper bag; and "huffing," which is placing a soaked rag or cloth with the substance around the nose and mouth.57
Figure 5: 1,1-difluoroethane
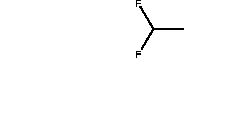
There are multiple case reports of deaths due to inhalation abuse. Data obtained from national and state surveys suggest that inhalant abuse is most common among 7th through 9th graders. Another national survey from 2003-2004 found that 2.5% of 4th graders had used inhalants at least once in the year prior to being surveyed.57
Although any volatile compound can be used, cleaning sprays such as the air compounds used to clean computer keyboards are some of the most common. Many companies have come under scrutiny for their products; Phil Lapin, president and CEO of Falcon Safety Products (manufacturer of common cleaning product Dust-Off), has made significant efforts to raise public awareness about safety and the potential for misuse of the products.58
Inhalation of volatile hydrocarbons has been reported in many deaths. A report from Japan in 2011 describes three cases of 1-1-difluoroethane inhalation-related deaths. In each case, a significant level of this chemical was found in the patient's system.59 Inhalational volatile hydrocarbons have also been associated with sudden cardiac death from dysrhythmia.60 Sudden cardiac death has also been associated with these compounds.
Management
Management for all of these intoxications is primarily supportive. Patients should be placed on a cardiac monitor with continuous pulse oximetry, and intravenous fluids may be given, especially for those who appear fluid depleted or are tachycardic. In those patients with alterations in mental status, point of care blood glucose measurement should be performed as soon as possible.
For patients in whom a history is unreliable or cannot be obtained, laboratory studies may include chemistries, total creatinine-kinase, acetaminophen, salicylate and ethanol levels, and a urine drug screen. An electrocardiogram should also be considered, with specific attention looking for ischemic changes, dysrhythmias, and QRS widening or QT prolongation. For patients who are febrile and altered, consider lumbar puncture and cerebral spinal fluid studies. Imaging of the brain, such as with a CT scan, may also be considered. It is important to remember that salvia, LSD, bath salts, nutmeg, inhaled hydrocarbons, and mescaline will not be detected on a standard urine drug screen.
In patients who have severe anxiety and/or psychomotor agitation, benzodiazepines should be the mainstay of therapy for all of these ingestions. Protecting staff from a potentially combative, agitated patient through the use of medications such as benzodiazepines is of utmost importance. Patients who exhibit sympathomimetic toxicities should be physically restrained with caution due to the risk of rhabdomyolysis and self injury. In the case of synthetic cannabinoid intoxication, the agitation and anxiety seem to be fairly short-lived,9-11 and shorter-duration benzodiazepines, such as midazolam, may be an appropriate choice. Antipsychotics may be considered in those individuals who present with severe psychosis or agitation with a normal QT. Patients may require sedation and mechanical ventilation if agitation is severe and prolonged.
Avoid the use of beta-antagonist medications in patients with severe tachycardia and hypertension because of concern for concomitant intoxication with sympathomimetic agents such as cocaine.
It is important to keep in mind that these drugs are often synthesized in clandestine, unregulated laboratories, raising concern for contaminants, other additives, and incorrectly synthesized products. Polysubstance abuse is a common problem and should always be considered on the differential diagnosis.
Consultation with a poison control center or a toxicologist may assist in patient management in cases of an uncertain diagnosis or moderate to severe clinical symptoms. Any patient who remains altered, from whom a reliable history cannot be obtained, or with metabolic or other abnormalities should be considered for admission and further management.
References
1. Wells DL, Ott CA. The "new" marijuana. Ann Pharmacotherapy 2011;45:414-417.
2. Seely KA, et al. Marijuana-based drugs: innovative therapeutics or designer drugs of abuse? Molecular Interventions 2011;11:36-51.
3. Atwood BK, et al. JWH018, a common constituent of "Spice" herbal blends, is a potent and efficacious cannabinoid receptor agonist. Br J Pharmacology 2010;160:585-593.
4. Vearrier D, Osterhoudt KC. A teenager with agitation: Higher than she should have climbed. Ped Emerg Care 2010;26:462-465.
5. Schneir AB, et al. "Spice" girls: Synthetic cannabinoid intoxication. J Emerg Med 2011;40:296-299.
6. Johnson LA, et al. Spice: A legal marijuana equivalent. Military Med 2011;176:718-720.
7. Synthetic Marijuana Data. American Association of Poison Control Centers. Press Release. 6/28/2011.
8. DEA moves to Emergency Control Synthetic Marijuana. DEA Public Affairs Press Release. 10/24/2010.
9. Every-Palmer S. Synthetic cannabinoid JWH-018 and psychosis: An explorative study. Drug and Alcohol Dependence 2011 In press.
10. Muller H, et al. The synthetic cannabinoid Spice as a trigger for an acute exacerbation of cannabis induced recurrent psychotic episodes. Schizophrenia Research 2010;118:309-310.
11. Hudson S, Ramsey J. The emergence and analysis of synthetic cannabinoids. Drug Testing and Analysis 2011.
12. Wehrman J. Fake marijuana spurs more than 4,500 calls to U.S. Poison Centers. American Association of Poison Control Centers. Press Release. 5/15/2011.
13. Gay M. Synthetic marijuana spurs state bans. The New York Times 7/10/2010.
14. Burdi J. Synthetic marijuana is back, despite Federal ban and new state law. The Sun Sentinel 6/26/2011.
15. Ernst L, et al. Identification and characterization of JWH-122 used as new ingredient in "Spice-like" herbal incenses. Forensic Science International 2011;208:e31-e35.
16. Synthetic cannabinoids in herbal products. United Nations Office on Drugs and Crime; April 2011.
17. Brenneisen R, Fisch HU, Koelbing U, et al. Amphetamine-like effects in humans of the khat alkaloid cathinone. Br J Clin Pharmacol 1990;30:825-828.
18. Kalix P. Pharmacological properties of the stimulant khat. Pharmacol Ther 1990;48:397-416.
19. Widler P, Mathys K, Brenneisen R, et al. Pharmacodynamics and pharmacokinetics of khat: A controlled study. Clin Pharmacol Ther 1994;55:556-562.
20. Auerbach P. Toxic plant ingestions. In: Wilderness Medicine, 5th ed.
21. Kehr J, et al. Mephedrone compared to MDMA (ecstasy) and amphetamine, rapidly increases both dopamine and serotonin levels in nucleus accumbens of awake rats. Br J Pharm Accepted Article. doiL 10.1111/j.1476-5381.2011.011499.x
22. Officials fear bath salts becoming the next big drug menace. Washington Post January 23, 2011 http://www.washingtonpost.com/wp-dyn/content/article/2011/01/22/AR2011012203854.html. Accessed July 16, 2011.
23. http://www.aapcc.org/dnn/Portals/0/prrel/BathSalts11811.pdf. Accessed July 16, 2011.
24. Wood, D, Davies S, et al. Recreational use of mephedrone (4-methylmehthcathinone, 4-MMC) with associated sympathomimetic toxicity. J Med Toxicol 2010;6:327-330.
25. Maskell P, De Paoli G, Seneviratne C, Pounder D. Mephedrone (4-methylmethcathinone)-related deaths. J Ann Toxicol 2011;35:188-191.
26. Centers for Disease Control and Prevention. Emergency department visits after use of a drug sold as "bath salts" Michigan, November 13, 2010-March 31, 2011. MMWR Morb Mortal Wkly Rep 2011 May 20;60(19):624-627.
27. http://www.aapcc/org.dnn/Portals/0/prrel/may122011bathsalts.pdf. Accessed July 16, 2011.
28. Kriikku P, Wilhelm L, Schwarz O, Ritatalo J. New designer drug of abuse: 3,4-Methylenedioxypyrovalerone (MDPV). Findings from apprehended drivers. For Sci Int 2011;10:195-200.
29. Emerson TS, Cisek J. Methcathinone: A Russian designer amphetamine infiltrates the rural Midwest. Ann Emerg Med 1993;22:1897-1903.
30. http://www.aapcc.org/dnn/Portals/0/prrel/bathsalts-final.pdf. Accessed July 17, 2011.
31. http://www.aapcc.org/dnn/Portals/0/Bath%20Salts%20Data%20for%20Website%207.07.2011.pdf. Accessed July 18, 2011.
32. http://www.nola.com/politics/index.ssf/2011/06/louisiana_lawmakers_approve_ba.html. Accessed July 15, 2011.
33. http://www.cbsnews.com/stories/2011/02/01/earlyshow/health/main7305536.shtml. Accessed July 21, 2011.
34. Roth BL, Baner K, et al. Salvinorin A: A potent naturally occurring non-nitrogenous kappa opioid selective agonist. Proc Natl Acad Sci 2002;99:11934-11939.
35. Lange JE, et al. Salvia divinorum: Effects and use among YouTube users. Drug and Alcohol Dependence 2010;108:138-140.
36. Baggott M, Erowid E, Erowid F. A survey of Salvia divinorum users. Erowid Extracts 2004;6:12-14.
37. Kelly BC. Legally tripping: A qualitative profile of Salvia divinorum use among young adults. 2011;43:46-54.
38. Pichini S, et al. Quantification of the plant-derived hallucinogen Salvinorin A in conventional and non-conventional biological fluids by gas chromatography/mass spectrometry after Salvia divinorum smoking. Rapid Communications in Mass Spectrometry 19 (12):1649–1656.
39. Valdes LJ, Diaz JL, Paul AG. Ethnopharmacology of ska maria pastora. J Ethnopharmacology 1983;7:287-312.
40. http://www.erowid.org/plants/salvia/. Accessed on 7/19/2011.
41. Substance Abuse and Mental Health Services Administration. (2007). Results from the 2006 National Survey on Drug Use and Health: Volume I. Summary of National Findings.
42. Substance Abuse and Mental Health Services Administration. 2010. Results from the 2009 National Survey on Drug Use and Health: Volume I. Summary of National Finding.
43. Chapter 42. In: Goldfrank's Toxicologic Emergencies, 8th ed. 2006.
44. Mack RB. Toxic encounters of the dangerous kind. NC Med J 1982;43:439.
45. Stein U, Greyer H, Hentschel H. Nutmeg (myristicin) poisoning report on a fatal case and a series of cases recorded by a poison information centre. Forensic Sci Int 2001;118:87-90.
46. BC, Chiang W. Toxicology of nutmeg abuse. J Toxicol Clin Toxicol 2000;38:671-678.
47. Abernethy MK, Becker LB. Acute nutmeg intoxication. Am J Emerg Med 1992;10:429-430.
48. Kalbhen DA. Nutmeg as a narcotic. Angew Chem Internat Edit 1971;10: 370-374.
49. McKenna A, Nordt SP, Ryan J. Acute nutmeg poisoning. Eur J Emerg Med 2004;11:240-241.
50. Carstairs S, Cantrell FL. The spice of life: An analysis of nutmeg exposures in California. Clin Tox 2011;49:177-180.
51. Demetriades AK, Wallman PD, McGuiness A, Gavalas MC. Low cost, high risk: Accidental nutmeg intoxication. Emerg Med J 2005;22:223-225.
52. Nelson LS. Toxicologic myocardial sensitization. J Toxicol Clin Toxicol 2002;40:867-879.
53. Chapter 79. Goldfrank's Toxicologic Emergencies, 8th ed. 2006.
54. http://archives.drugabuse.gov/NIDA_notes/NNVol17N4/Chronic.html. Accessed July 23, 2011.
55. Bass M. Sudden sniffing death. JAMA 1970;212:2075-2079.
56. Section 5, Chapter 32. In: Basic and Clinical Pharmacology, 11th ed. 2009.
57. http://teens.drugabuse.gov/facts/facts_inhale1.php. Accessed July 23, 2011.
58. http://www.falconsafety.com/images/dust_off/.
59. Sakai K, Maruyama-Maebashi K, Takatsu A, et al. Sudden death involving inhalation of 1,1-difluoroethane (HFC-152a) with spray cleaner: Three case reports. Forensic Sci Int 2011;206(1-3):e58-61. Epub 2010 Sept. 26.
60. Avella J, Wilson JC, Lehrer M. Fatal cardiac arrhythmia after repeated exposure to 1,1-difluoroethane (DFE). Am J Forensic Med Pathol 2006;27:58-60.
This issue might be subtitled "What will they think of next?" Getting high does not always require the purchase of illegal drugs, and all substances that alter sensorium, such as nutmeg, cannot be regulated. However, the emergency physician must remain aware of the latest fads of drug abuse, and should be able to recognize the symptoms they cause.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
