Pediatric Appendicitis
Pediatric Appendicitis
Authors:
Jeffrey A. Holmes, MD, Clinical Instructor, Department of Emergency Medicine, Maine Medical Center, Portland, ME; Tufts University School of Medicine, Boston, MA.
Matthew DeLaney, MD, Attending Physician, Mercy Hospital, Portland, ME.
Peer Reviewer:
Julie Anderson-Suddarth, MD, FAAP, Attending Physician, Blank Children's Hospital Emergency Department, Adjunct Clinical Assistant Professor of Pediatrics, University of Iowa Carver College of Medicine, Associate Program Director, Blank Children's Hospital Pediatric Residency, Des Moines, IA.
Abdominal pain is an exceedingly common presentation in the emergency department. Every clinician fears missing the diagnosis of appendicitis. Children are particularly challenging since appendicitis is less common, and the history and physical may be subtle. The diagnostic use of CT is not without its risks and must be balanced against the potential risk of appendicitis in each individual patient. This article provides a comprehensive review of appendicitis in children.
The Editor
Introduction
Abdominal pain is one of the most common chief complaints for a child presenting to the emergency department (ED) or acute care facility. While not the cause of abdominal pain for the large majority of patients, appendicitis is the most common surgical etiology for children older than 2 years of age and is responsible for up to 13% of pediatric surgeries.1,2 Nationwide, there are 77,000 cases of appendicitis each year, with a total cost to the system of $680 million.3
Despite its prevalence, appendicitis is still difficult to diagnose in children. The rate of initial misdiagnosis ranges from 28-57% in children younger than 12 years, with the rate of initial misdiagnosis increasing to near 100% in children younger than 2 years.4 With high rates of initial misdiagnosis, the rate of appendiceal perforation remains significant in children with appendicitis. In a study of children younger than 4 years of age, appendiceal perforation occurred in the majority of cases, ranging from 80% to 100%. With high rates of initial misdiagnosis and subsequent delays in treatment, cases of missed appendicitis are a common source of malpractice claims.5-7
Appendicitis is most common in adolescent and teenage patients. For patients between the ages of 10-19 years, the rate of appendicitis is 23.3 per 10,000 population per year. There is a slight male to female predominance (1.4:1), with males aged 10-14 having a rate of 27.6 per 10,000 population per year and females aged 15-19 having rates of 20.6 per 10,000 population per year.6
Appendicitis is relatively rare in patients younger than 5 years of age, accounting for less than 5% of cases. Neonatal appendicitis is extremely rare, with only 141 cases reported in the past century.8 The relative rarity of this surgical disease in the very young likely contributes to rates of misdiagnosis and the increased likelihood of perforation. In neonates, mortality rates for appendicitis have been reported as high as 25%.9 Appendicitis in neonates typically occurs in conjunction with other pathology, notably in the setting of prematurity and in patients with inguinal hernias.10
Interestingly, appendicitis appears to have genetic, racial, and seasonal variations. Patients with a family history of appendicitis in a first-degree relative have a 3.5 to 10.0 times increase in relative risk compared to those who do not.4 Caucasian patients have a 1.5 times higher rate of appendicitis than non-caucasians. Additionally, there is an increase in the rates of appendicitis between May and September, which is thought to be secondary to increased rates of enteric infections during periods of warm weather.9,11-13
The appendix is a blind-ended tubular structure running from the cecum proximal to the ileocecal valve. The appendix can range in length from less than 5 cm in neonates to 25 cm in adults.14 While the base of the appendix has little anatomic variability, the remainder of the appendix can lie in various locations within the abdomen, including retrocecal, subcecal, retroileal, preileal, or in the pelvis itself.15 The range of lengths and the varied anatomic locations combine to create a wide variety of clinical symptoms, often with atypical features.
Appendicitis has been described as having five stages that typically occur over a time period of 24-36 hours. The first stage begins when the lumen of the appendix becomes obstructed and leads to distention. During the second stage, the distended appendix stimulates the visceral thoracic nerves in the T8-T10 distribution and causes peri-umbilical pain. In the third stage, as the appendix becomes more distended, there is an increase in intra-luminal pressure and a decrease in perfusion. This decrease in perfusion leads to tissue ischemia and compromises the integrity of the mucosal lining, allowing bacteria to invade the wall of the appendix. Stage four is characterized by transmural inflammation. In the final stage, the transmural inflammation spreads to the surrounding peritoneum, causing pain that is typically localized to the right lower quadrant.16
Differential Diagnosis
Patients with appendicitis have symptoms that are shared by a multitude of disease processes. Complaints of abdominal pain, vomiting, and diarrhea are very common and occur in nearly 20% of general and pediatric emergency department cases.17 A comprehensive list of differential diagnoses across all age groups for these complaints is lengthy and includes both abdominal and non-abdominal etiologies. In a study of more than 1,100 consecutive children ages 1-12 years old who presented to an ED or walk-in clinic, 5% had acute abdominal pain of less than three days duration.18 Almost 80% of the patients complaining of abdominal pain were diagnosed with upper respiratory tract infection, otitis media, pharyngitis, viral syndrome, abdominal pain of uncertain etiology, or gastroenteritis. Most likely due to the frequency of these diagnoses and the rarity of appendicitis, upper respiratory tract infections and gastroenteritis have been found to be the most common misdiagnoses in children who present with appendicitis.19 Pediatric patients often present with abdominal complaints. While not the most common source of these complaints, appendicitis often causes similar symptoms and should be considered in any patient who presents with abdominal pain, nausea, or vomiting.
A primary responsibility of the emergency physician when evaluating a child with abdominal complaints is to identify potentially life-threatening issues such as volvulus, infectious processes that require treatment such as urinary tract infection (UTI) or pneumonia, and other diseases like appendicitis that require acute surgical intervention. While the majority of cases of abdominal pain will not require surgery or emergent therapy, it is important to consider these emergent sources of pain when evaluating any patient with abdominal pain. A good starting point in evaluating a child with abdominal pain is to generate a differential that is both age- and gender-specific. For example, volvulus is most common in neonates, while intussusception is seen most frequently in toddlers. As female patients enter their teen years, diagnoses such as ectopic pregnancy and pelvic inflammatory disease should become part of the differential diagnosis. Once a differential diagnosis is generated, a detailed history and physical exam should be performed. Rather than being overly broad and all-inclusive, the history and physical should focus on signs and symptoms with enough predictive power to significantly affect the pretest probability of these diagnoses. Unfortunately, due to the inherently limiting and sometimes misleading factors in a pediatric patient, physicians are still left with doubt about the probability of a serious etiology. In these cases, further testing, repeat exams and consultation should be pursued to further narrow the differential diagnosis.
Exam and laboratory findings can be helpful in evaluating a patient but should be interpreted with caution, as patients with appendicitis have many findings in common with less emergent diagnoses. For example, in a patient who complains of abdominal pain with diarrhea, it is tempting to assume that the patient has gastroenteritis, a common cause of ED visits. Unfortunately, diarrhea is also seen in up to 40% of children 2 years or younger with appendicitis.20,21 Similarly, a patient's complaint of dysuria and urinary frequency may not be from a urinary tract infection, but instead from an inflamed appendix adjacent to the bladder or ureter. The presence of white or red blood cells in the urine in 16.5-30% of cases of appendicitis can also be misleading.22 Constipation is another common pediatric complaint and source of abdominal pain. Obtaining and finding the presence of stool on an X-ray cannot reliably be used to exclude the diagnosis of appendicitis.23,24
Clinical Presentation
When evaluating a pediatric patient, the history and physical exam are frequently limited by developmental issues, vague nonspecific symptoms, and physical exam findings that are difficult to obtain. Obtaining a history and examining a younger child can be vastly different from an adult or even an older child. Some children may be developmentally unable to describe or localize their symptoms and tend to be more apprehensive, making an adequate examination of the abdomen more difficult. Symptoms, such as nausea and vomiting, tend to be more nonspecific and found with a variety of disease processes. In addition, non-abdominal etiologies such as pneumonia and strep are well known to cause a "belly ache." Children may have difficulty accurately describing their symptoms, and emergency practitioners should not rely too heavily on the patient's history of present illness.25
These inherent difficulties in examining the young child require a different approach than that used for the adult or even the older child. Children with appendicitis frequently present with atypical symptoms. In addition, fear and apprehension can limit the yield of a physical exam. To overcome some of these obstacles, it is important to attempt to gain the child's trust before starting your exam. Offering a child a toy and discussing favorite cartoons can ease a child's fears and help gain his or her trust. Examine the fearful child in the caretaker's arms if necessary. Techniques such as palpating the abdomen while pretending to listen for bowel sounds can help overcome anticipatory guarding and can allow for a more accurate exam. Children often don't respond to direct questioning. Instead of asking a child "Does this hurt," watch for facial expressions and other nonverbal clues to obtain helpful information. A favorite trick is to turn the abdominal exam into a game by telling the child that you will try to guess what he or she had to eat with your "magic hands." Pizza and hamburger are reliable guesses, and the process of "figuring out their favorite food" can distract the patient and allow for a more thorough abdominal exam.26 Instead of assessing for rebound tenderness, challenge the patient to jump high enough to touch your hand, or ask him or her to run around the room. Given the prevalence of nonabdominal sources of pain, nausea, and vomiting, all exams should include an evaluation of the patient's lungs and genital area.
Table 1. "Can't Miss" Causes of Abdominal Pain
Neonate |
2 months - 2 years |
2-5 years |
> 5 years |
|
|
|
|
Before specifically reviewing the clinical features of appendicitis, it is worthwhile to emphasize that the purpose of the history and physical exam is to help determine the pretest probability of appendicitis. It is this probability that will drive the need for surgical consultation, discharge home with close follow-up, or further testing. For example, the 16-year-old male with a classic story of migratory abdominal pain to the right lower quadrant, with focal abdominal pain, vomiting, fever, and rebound tenderness has a high pretest probability of appendicitis and needs immediate surgical consultation. The afebrile 2-year-old who presents with emesis, diarrhea, and reassuring serial abdominal exams has a likely low pretest probability, and can be safely discharged with close follow-up. Further laboratory testing is unlikely to significantly affect the probability of appendicitis in either of these patients and may even lead to falsely positive or negative results. Patients determined to have an intermediate probability, however, require further diagnostic testing.
The best way to determine pretest probability is to focus on those signs and symptoms that are most likely to affect the probability of the diagnosis ideally those with helpful likelihood ratios. Likelihood ratios combine both sensitivity and specificity, making it applicable to each patient before the physician knows whether disease is present or absent. Bundy et al performed a review of the English language literature from 1996 to 2007 to assess the precision and accuracy of symptoms, signs, and basic laboratory testing for children aged 18 years or younger with abdominal pain. (See Table 2.) Findings found most helpful included the presence of a fever (LR 3.4 [95% CI 2.4-4.8]) and rebound tenderness (LR 3.0 [95% CI 2.3-3.9]). Independently they both tripled the odds of appendicitis. A history of mid-abdominal pain migrating to the right lower quadrant at least doubled the risk (LR range 1.9-3.1). The major limitation of this review was that it found most studies lacked child-specific, age-stratified data.27
Table 2. The Precision and Accuracy of Symptoms and Signs for Children Age 18 Years or Younger with Abdominal Pain
Sign/Symptom |
Positive Likelihood Ratio |
Negative Likelihood Ratio |
Adapted from: Bundy DG, Byerley JS, Liles EA, et al. Does this child have appendicitis? JAMA 2007;298:438-451. |
||
Fever |
3.4 [95% CI 2.4-4.8] |
0.32 [95% CI 0.16-0.64] |
Rebound tenderness |
3.0 [95% CI 2.3-3.9] |
0.28 [95% CI 0.14-0.55] |
Migratory pain to right lower quadrant |
1.9-3.1 |
0.41-0.72 |
In children younger than 2 years, appendicitis is rare, has variable presentations, and is difficult to diagnose. This, unfortunately, leads to routine delayed diagnosis and high rates of perforation. The most common symptoms include vomiting (85-90%), pain (35-77%), diarrhea (18-46%), and fever (40-60%). Localized right lower quadrant tenderness is noted in less than 50% of cases.4
Appendicitis in preschool-aged children from 2 to 5 years is also rare, but these children tend to be developmentally more able to describe and localize their symptoms. As children age, they tend to have more "typical" symptoms of appendicitis. Rothrock found that abdominal pain (89-100%), vomiting (66-100%), and fever (80-87%) are the most common symptoms associated with appendicitis in this age group.4 Unlike in infants, the presence of right lower quadrant tenderness (58-85%) and involuntary guarding (85%) in this age group was more common.28,29 It is unclear whether abdominal pain precedes vomiting in the majority of patients. Vomiting is the first symptom; however, given the age range, the progression of symptoms is somewhat difficult to verify. In any event, patients in this age group with appendicitis can present with vomiting as their sole symptom.19
School-aged children and adolescents have increased incidence of appendicitis, thus a higher starting pretest probability and more reliable clinical features. One study prospectively evaluated the signs and symptoms of 377 children aged 2 to 16 years old presenting with abdominal pain. The authors found 97% (28/29) of children with appendicitis had at least two of the following four clinical features: vomiting, right lower quadrant pain, abdominal tenderness, or guarding.30 Despite these more typical features, this age can still frequently present atypically. Becker et al performed a prospective study of children and adolescents with suspected appendicitis. Among patients with appendicitis, the most notable atypical features included apyrexia (83%), absence of rebound pain (52%), lack of anorexia (40%), and lack of migration to the right lower quadrant (50%).31 Overall, a significant portion of children with appendicitis will have atypical symptoms. As children age and approach adulthood, the presence of classic signs of appendicitis becomes more prevalent; however, the presence or absence of various symptoms cannot be used to reliably diagnose or exclude appendicitis.
Diagnostic Evaluation
White Blood Cell. When evaluating pediatric patients for possible appendicitis, the history and physical are frequently not sufficient, and more information is needed to reliably make a diagnosis. The use of laboratory testing in the work-up of possible appendicitis has been widely studied, and the utility of various laboratory findings is a source of continued debate. The white blood cell count (WBC) is readily available and is commonly used in the work-up of abdominal pain. In a systematic review, Bundy et al examined several studies that used a threshold WBC of 10,000/µL and found summary likelihood ratio (LR) of 2.0 in patients with an elevated WBC. The sensitivities ranged from 0.8-0.92, with specificities ranging from 0.29-0.76. Increasing the threshold WBC did not improve likelihood ratios and caused a significant decline in sensitivity.32
The presence of a left shift or more than 80% polymorphonuclear cells and bands on a cell differential in the setting of an elevated WBC has been shown to have significant predictive power. In a retrospective analysis of pediatric patients with nontraumatic abdominal pain, Wang et al reported a likelihood ratio of 3.4 in patients with an elevated WBC count and 5.9 in patients with a left shift. When patients had both an elevated WBC count and a left shift, the likelihood ratio increased to 9.8.33
The lack of WBC elevation can help improve diagnostic accuracy in patients with abdominal pain. In a prospective study of children with suspected appendicitis, Kharbanda et al found that patients with a WBC < 8850/µL and an absolute neutrophil count < 6750 had a likelihood ratio of 0.06.34 While a normal WBC cannot completely exclude the diagnosis of appendicitis, it can be suggestive of an alternative diagnosis.
Other Biomarkers. Multiple other biomarkers have been used in conjunction with the WBC to evaluate patients with abdominal pain. As a marker of inflammation, C-reactive protein (CRP) has shown wide ranges in sensitivity and specificity. In a recent prospective study, Kwan et al used a threshold value of 3 mg/dL and found that patients with an elevated CRP and a WBC greater than 12,000/µL were 7.75 times more likely to have appendicitis (OR 7.75).35 Patients with a normal CRP have an LR of 0.44-0.47 and are half as likely to have appendicitis.12 Procalcitonin has been used as a marker of infection and has been found to be specific for perforated appendicitis, yet it lacks the sensitivity needed to be widely used. In general, the presence or absence of an elevated white blood cell count lacks the diagnostic accuracy to be used as a single marker for appendicitis. In summary, the utility of a white blood cell count increases significantly when seen with the presence of a left shift or an elevated CRP.
Urinalysis. A urinalysis can be a misleading test in the work-up of appendicitis. Other sources of abdominal pain, such as a urinary tract infection, can be diagnosed using a urinalysis. There are no findings in urinalysis, however, that are reliable enough to confirm or exclude the diagnosis of appendicitis. Tundidor et al found that one-third of patients with appendicitis reported dysuria or flank pain, and 15% of patients had pyuria.36
Laboratory results must always be interpreted with the patient's clinical picture in mind. In the early stages of appendicitis, patients may have normal laboratory values, as the inflammation and infection detected by the biomarkers have not yet become detectable. It has been suggested that laboratory values increase in diagnostic value as the patient's duration of symptoms increases. In a patient with a reassuring clinical exam after several days of symptoms, normal laboratory values may be somewhat reassuring. Conversely, in a patient with a worrisome exam, abnormal laboratory values may increase the likelihood that the patient has appendicitis. Ultimately, lab results should be interpreted with caution with the knowledge that it is possible to have appendicitis with completely normal laboratory results.4
Diagnostic Imaging
Pediatric appendicitis is notable for its often atypical presentation, a fact that is underscored by the significant number of cases that are seen by multiple providers before the correct diagnosis is made. Imaging, whether with ultrasound or computed tomography (CT) scan, is frequently used to evaluate patients when the clinical picture is less than clear. Plain films are not useful in the work-up of appendicitis. Heller et al performed a retrospective analysis of 821 patients who were admitted with suspected appendicitis. Seventy-eight percent of the patients had positive radiographic findings on plain films. Only 10% of those findings were suggestive of specific conditions, and in those patients with suggestive findings, the final diagnosis correlated with the suggestion only 43% of the time. Traditional teaching maintains that the presence of calcified appendicolith on plain films is suggestive of appendicitis, yet in this study, that finding was present in only 10% of patients. Overall, the authors found plain films to be misleading and were unable to identify any specific radiographic finding that was sensitive or specific for appendicitis.37
Ultrasound has become a popular imaging modality in the work-up of appendicitis. Benefits of ultrasound include reduced cost, speed of testing, the ability to evaluate appendiceal compressiblity, and a lack of ionizing radiation. The presence of operator variability is a limitation of ultrasound. In addition, scans can be equivocal when the appendix is unable to be fully visualized secondary to factors such as body habitus, gender, and anatomic location of the appendix. In patients with certain clinical or anatomic characteristics, the rate of equivocal scans and misdiagnosis is significantly increased. Schuh et al found a significant increase in both equivocal scans and misdiagnosis in children with a body mass index greater than the 85th percentile. In addition, patients with a low clinical suspicion of appendicitis had a rate of misdiagnosis of around 40%.38 An equivocal scan does not provide enough information to exclude appendicitis and often results in additional testing for the patient.
Ultrasound has a reported specificity that ranges from 88% to 99%, with a range of sensitivities from 50% to 100%.39 Overall, ultrasound tends to be more effective at identifying patients with appendicitis rather than excluding the disease with a negative result or equivocal result. Howell et al examined several studies involving the diagnostic accuracy of ultrasound. While 43% of the included studies reported negative likelihood ratios less than 0.1, 71% of studies had positive likelihood ratios greater than 10.40 In patients with a clinical presentation that is suggestive of appendicitis, an equivocal finding on ultrasound should not be used to exclude the disease.
Figure 1. Ultrasound of Acute Appendicitis
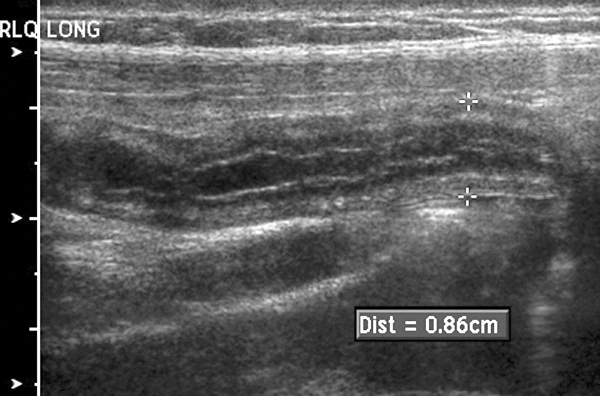
Acute appendicitis. Longitudinal sonogram of a child with right lower quadrant pain shows an enlarged appendix (cursors) measuring 8.6 mm. The appendix was non-compressible. No appendicolith or abscess was present.
Historically, the primary and most specific ultrasound criteria for diagnosing appendicitis has been an appendiceal maximal outer diameter (MOD) greater than 6 mm. Secondary criteria such as a lack of compressibility, fat stranding, and fluid collections are strongly suggestive of appendicitis. (See Figure 1.) In a recent retrospective analysis, Goldin et al found that using traditional criteria of MOD > 6 mm would have only identified 84% of appendicitis and resulted in 26 unnecessary surgeries and seven cases of missed appendicitis. In the same set of patients, using revised criteria of MOD > 7 mm or a wall thickness of > 1.7 mm led to the correct diagnosis in 97% of cases. This revised criteria, with a sensitivity and specificity of 99% and 95%, would have resulted in one case of missed appendicitis and led to only six unnecessary operations. In this study, adjusting for age, weight, or the presence of secondary signs did not improve the diagnostic accuracy.41
CT scans continue to be the most consistent and accurate imaging modality. The reported sensitivities of CT scans range from 66–100%, with the specificities ranging from 87-100%.42-45 The criteria for diagnosing appendicitis on CT scan include the presence of an abnormally thickened appendix with a diameter greater than 6 mm, the presence of surrounding inflammatory changes or abscess formation, or the presence of a calcified appendicolith.46 (See Figure 2.) The use of contrast and the potential risk from exposure to ionizing radiation are two potential drawbacks to CT scans, and are also areas of ongoing research and debate.
Figure 2. CT of Acute Appendicitis
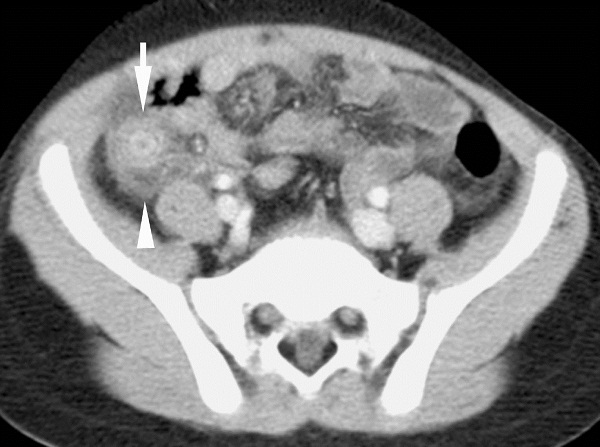
Contrast-enhanced CT image shows a enlarged appendix (arrow) with a thick enhancing wall and associated inflammatory changes in the periappendiceal fat (arrowhead).
The utility of contrast enhancement in CT scans for appendicitis remains unclear. Noncontrast scans can be performed more quickly, are cheaper, and avoid any potential complications from the use of contrast material. Various authors have promoted the use of contrast in children in an attempt to enhance visualization of the appendix and increase the diagnostic accuracy of CT scans.47 When compared to adults, children have less periappendiceal fat, which can limit the ability to see the appendix and can also mask the presence of secondary signs. IV contrast tends to be used most commonly, with various protocols adding oral or, less commonly, rectal contrast.48 In a recent meta-analysis, Hlibzcuk et al reported a sensitivity of 93%, a specificity of 96%, and a false-negative rate of 7.3% in adults who underwent noncontrast scans while being evaluated for appendicitis. These numbers compare favorably to results found in various studies that used contrast.49 In a retrospective study of pediatric patients with suspected appendicitis, Kaiser et al found that noncontrast-enhanced CT scans had a sensitivity of 66%. With the addition of IV contrast, the sensitivity of the scan increased to 90%, leading the authors to recommend the use of IV contrast in the evaluation of pediatric patients.50 In a recent study, Kharbanda et al found that the use of rectal contrast in addition to IV contrast did not result in any significant increase in sensitivity, specificity, or decrease in equivocal scans.51 The use of oral contrast has several limitations, including increased wait time prior to scanning and difficulty administering oral contrast due to nausea and vomiting. In a recent study, Laituri et al found that in patients given oral contrast, 30% did not have any visible contrast in the point of interest at the time of scanning. There was no significant increase in diagnostic accuracy in the group with visible contrast, leading the authors to conclude that oral contrast was not a necessary adjunct to IV contrast.52 While IV contrast seems to improve diagnostic accuracy in CT scans, the use of rectal and oral contrast material does not seem to offer a significant benefit.
Despite the use of contrast agents, nonvisualization of the appendix on CT scan is a continued problem in children. In a retrospective analysis, Garcia et al evaluated the diagnostic value of an equivocal CT scan in children where the appendix is not visualized. Out of 156 patients with a nonvisualized appendix on CT scan, two patients went on to be diagnosed with appendicitis, resulting in a false-negative rate of 1.3%. The negative predictive value of a normal CT with a nonvisualized appendix was 98.7%.53 In contrast to ultrasound, failure to visualize the appendix or other indirect signs of appendicitis on CT scan appears to offer a reasonable negative predictive value.
During the past several years, there has been a significant increase in the number of CT scans performed.54 This has led to an increased awareness of the associated radiation exposure, one of the most significant risks associated with CT scans. Radiation exposure can alter DNA and RNA, which alters cellular replication and can lead to a malignant transformation.55 The ability of radiation to induce malignancy has been theorized for more than a century, yet the majority of the data regarding radiation risk comes from data collected from the survivors of the atomic bombings of Hiroshima and Nagasaki during World War II. A long-term cohort study of more than 100,000 survivors revealed three disconcerting features about radiation-induced malignancy (RIM) that are especially pertinent when examining the potential exposure from CT scans:
Patients exposed to radiation experience a higher rate of malignancy.
A large single exposure is more dangerous than cumulative exposure to lower doses over time.
Younger patients, especially females, have an increased risk of developing RIM.56
Children are theoretically at higher risk of acquiring RIM for three reasons. First, they have a larger number of replicating cells, which are more susceptible to damage. Children also have significantly less soft tissue than adults to shield their organs, which leads to an increased effective organ dose of radiation. Finally, RIM tends to be a time-dependent disease process, and since children undergoing CT scans are exposed at a young age, they theoretically have a much longer timeframe during which they could develop a malignancy.
Brenner at al compared data from the atomic bomb survivors to radiation exposure from CT scans and attempted to calculate the increased lifetime risk of fatal radiation-induced malignancy. In a 1-year-old child, the lifetime risk of a fatal RIM increased by 0.18%. For every 555 1-year olds who were scanned, one would develop a fatal malignancy directly as a result of the diagnostic work-up. When the same data were applied to 15-year-olds, the increased risk of a fatal RIM was 0.11%. While the rate of malignancy decreases with age, in 15-year-olds undergoing one CT scan of the abdomen, 1 in 1000 will develop a fatal malignancy.57 Given the prevalence of appendicitis and the increased use of CT scans, the risk of radiation-induced malignancy is significant, and the risk of exposure from a CT scan should always be balanced with the potential diagnostic benefit to the patient.
Due in part to the risks of CT scans, many EDs have developed staged protocols that use ultrasound as the initial diagnostic test and proceed to CT scan in patients who have equivocal findings on ultrasound (defined as the nonvisualization of the appendix and the lack of alternate radiographic diagnosis). A recent retrospective study in a pediatric ED found that using a staged protocol increased accuracy and significantly reduced the use of CT scans. Krishanmoorthi et al employed the graded compression technique and used traditional ultrasound criteria. A positive scan was defined by visualization of a noncompressible appendix with an MOD > 6 mm. A negative scan involved a fully visualized, compressible appendix < 6 mm or the identification of an alternate diagnosis. Patients with equivocal findings then went on to CT scan. The staged protocol produced a sensitivity of 98.6% and a specificity of 90.6%. Notably, there was a 52.7% reduction in the number of CT scans.58
While ultrasound has limitations, its ease of use and lack of risk to the patient make it a reasonable first test in children with probable appendicitis who require imaging. CT scans remain a good imaging choice in patients with equivocal ultrasounds or when significant diagnostic uncertainty remains.
Traditionally, MRI has not been widely used in the diagnosis of appendicitis. Benefits of MRI include the ability to obtain high resolution images without significant exposure to radiation. Drawbacks to MRI include an increase in cost and the length of time needed to obtain an adequate scan. In addition, the availability of an MRI for emergent studies varies from hospital to hospital. Initial studies of MRI use to rule out appendicitis in pregnancy were promising, and recent studies of nonpregnant adults have yielded sensitivities and specificities that compare favorably to CT scans.59,60 While initial studies involving MRI are promising, more research into the use of MRI needs to take place before it becomes the test of choice for children with possible appendicitis.
Several studies have questioned the usefulness of imaging in general and have suggested that a greater emphasis be placed on physical exam and clinical impression. Kosloske et al evaluated the clinical impression of a pediatric surgeon without the use of imaging and reported a sensitivity of 99%, a specificity of 93%, and a diagnostic accuracy of 97%. While these results compare favorably to the use of imaging, their study used patients who had been pre-screened by other providers who then asked for a surgical evaluation for possible appendicitis.61 Wong et al report that over a 10-year period, ultrasound use to diagnose appendicitis increased by 50% and CT scan use increased by 35%. Despite the increased utilization of this technology, there was no decline in the time to diagnosis, the severity of appendicitis at the time of surgery, or the rate of perforation.62 In younger children in whom the physical signs and symptoms are often atypical, the increased use of imaging has not led to improved outcomes. In 1980, Graham et al reported a perforation rate of 63% for preschool-aged children.63 In 2007, despite an 80% increase in the use of imaging, Colvin et al found that the perforation rate remained at 53%.64 While imaging can be a useful component of an evaluation, the patient's clinical history and physical exam continue to have a significant value.
Clinical Scoring Systems
During the past several years, various clinical scoring systems have been developed to help aid in diagnosing appendicitis while limiting the use of imaging. The Alvarado score and the Pediatric Appendicitis Score (PAS) are the most commonly used scoring systems.65,66 The aim of both scores is to establish a threshold that determines whether a patient should go to surgery or undergo observation. The scores are made up of various clinical features and laboratory findings and do not incorporate any imaging modalities. Prospective attempts to validate these scores have shown sensitivities ranging from 76-94%, with specificities ranging from 62-98% and positive predictive values from 54-76%. The sensitivities of both scores are increased for males. One significant issue with both systems is the limited scope of the scores.67
Both systems are designed to identify patients with a high likelihood of appendicitis who can be taken directly to the operating room without undergoing further testing. To date, no system has been developed to identify patients who are low risk enough to be discharged without further imaging or observation. In patients with a high likelihood of appendicitis, the scoring systems may facilitate a prompt surgical disposition; however, they should not be used to rule out appendicitis or otherwise risk stratify patients with abdominal pain.
Patients with a high suspicion of appendicitis need an emergent surgical evaluation. The traditional treatment for acute appendicitis is an appendectomy.
Management of Appendicitis
In patients with uncomplicated appendicitis, the use of antibiotics does not seem to offer any significant benefit and can result in an increase in side effects.68 In children with perforated appendicitis with abscess formation, the traditional treatment has involved intravenous antibiotics, abscess drainage, and delayed appendectomy. St. Peter et al compared this interval approach to an approach that featured an early appendectomy. Both groups of patients had similar rates of complication and recurrent abscesses, leading the authors to question the benefit of the traditional delayed appendectomy.69
Nonperforated appendicitis is typically managed laparoscopically. A relatively new surgical technique employs a single incision at the umbilicus, which reduces the amount of abdominal scarring. A recent case series found that this technique involved a slightly longer operative time but could otherwise be used safely in children as young as 19 months.70
Recent studies have evaluated a conservative nonsurgical treatment of appendicitis involving intravenous antibiotics and monitoring. A significant limitation to this conservative approach is the rate of recurrence, which can be as high as 35%.71 While there is some evidence that a portion of patients can be effectively managed with antibiotics alone, to date the available studies have yet to be prospectively validated.72
Appendicoliths are a recognized cause of appendicitis; however, the presence of an appendicolith without other signs of appendicitis presents a clinical dilemma. In children with abdominal pain, the presence of an appendicolith on CT has a reported sensitivity of 65% and specificity of 86% for appendicitis, yet appendicoliths are an incidental finding in up to 13% of children undergoing a CT scan. Lowe et al found that 14% of children undergoing CT scans for appendicitis had an appendicolith without other evidence of appendicitis. Of this group, 83% failed to develop appendicitis after further monitoring.73 The presence of an appendicolith without further signs of appendicitis should not necessarily mandate an appendectomy; however, in a patient with abdominal pain, these findings should not be interpreted as "normal." These patients need close follow-up or inpatient observation.
Summary
Abdominal pain is a frequent ED complaint. In children, the history and physical exam may be challenging. Excluding the diagnosis of appendicitis is critical. A careful history, physical examination, and judicious use of diagnostic imaging will help identify cases of appendicitis in an expeditious manner.
References
1. Scholer SJ, Pituch K, Orr DP, et al. Clinical outcomes of children with acute abdominal pain. Pediatrics 1996;98:680.
2. Reynolds SL, Jaffe DM. Diagnosing abdominal pain in a pediatric emergency department. Pediatr Emerg Care 1992;8:126.
3. Guthery SL, Hutchings C, Dean JM, et al. National estimates of hospital utilization by children with gastrointestinal disorders: Analysis of the 1997 kids' inpatient database. J Pediatr 2004;144(5):589–594.
4. Rothrock SG, Pagane J. Acute appendicitis in children: Emergency department diagnosis and management. Ann Emerg Med 2000;36:39.
5. Alloo J, Gerstle T, Shilyansky J, et al. Appendictitis in children less than 3 years of age: A 28-year review. Ped Surg Int 2004;19:777-779.
6. Luckmann R, Davis P. The epidemiology of acute appendicitis in California: Racial, gender and seasonal variation. Epidemiol 1991;2:323-330.
7. Horwitz J, Gursoy M, Jaksic T, et al. Importance of diarrhea as a presenting symptom of appendicitis in very young children. Am J Surg 1997;173:80-82.
8. Selbst SM, Friedman MJ, Singh SB. Epidemiology and etiology of malpractice lawsuits involving children in US emergency departments and urgent care centers. Pediatr Emerg Care 2005;21:165–169.
9. Karaman A, Cavusoglu YH, Karaman I, et al. Seven cases of neonatal appendicitis with a feview of the English-language literature. Pediatr Surg Int 2003;19: 707–709.
10. Jancelewicz T, Kim G, Miniati D. Neonatal appendicitis: A new look at an old zebra. J Pediatr Surg 2008;43:e1-5.
11. Humes DJ, Simpson J. Acute appendicitis. BMJ 2006; 333:530-534.
12. Bundy DG, Byerley JS, Liles EA, et al. Does this child have appendicitis? JAMA 2007;298:438-451.
13. Addiss D, Shaffer N, Fowler B, et al. The epidemiology of appendicitis and appendectomy in the United States. Am J Epidem 1990;132:910-925.
14. Buschard K, Kjaeldgaard A. Investigation and analysis of the position, fixation, length and embryology of the veriform appendix. Acta Chir. Scand 1973;139:293-298.
15. Guidry S, Roole G. The anatomy of appendicitis. Am Surg 1994;60:68-71.
16. Birnbaum BA, Wilson SR. Appendicitis at the millennium. Radiology 2000;215: 337-348.
17. Rothrock SG, Green SM, et al. Plain abdominal radiography in the detection of acute medical and surgical disease in children: A retrospective analysis. Ped Emerg Care 1991;7:280-285.
18. Scholer SJ, Pituch K, Orr DP, et al. Clinical outcomes of children with acute abdominal pain. Pediatrics 1996;98: 680-685.
19. Rothrock SG, Skeach G, Rush JJ, et al. Clinical features of misdiagnosed appendicitis in children: Emergency department diagnosis and management. Ann Emerg Med 1991;20:45-51.
20. Horwitz JR, Gursoy M, Jaksic T, et al. Importance of diarrhea as a presenting symptom of appendicitis in very young children. Am J Surg 1997;173:80-82.
21. Alloo J, Gerstle T, Shilyansky J, et al. Appendicitis in children less than 3 years of age: A 28-year review. Pediatr Surg Int 2004;19:777-779.
22. McLario D, et al. Understanding the varied presentaiton and management of children with acute abdominal disorders. Ped Emerg Med Rep 1997.
23. Bewley A, Clancy MJ, Hall JRW. The erroneous use by an accident and emergency department of plain radiographs in the diagnosis of constipation. Arch Emerg Med 1989;6:257-258.
24. Campbell JPM, Gunn AA. Plain abdominal radiographs and acute abdominal pain. Br J Surg 1988;75:554-556.
25. Scholer SJ, Pituch K, Orr DP, et al. Clinical outcomes of children with acute abdominal pain. Pediatrics 1996;98: 680-685.
26. Brown L, Jones J. Acute abdominal pain in children: "Classic" presentations vs. reality. Emerg Med Practice December 2000;2.
27. Bundy DG, Byerley JS, Liles EA, et al. Does this child have appendicitis? JAMA 2007;298:438-451.
28. Williams N, Kapila L. Acute appendicitis in the preschool child. Arch Dis Child 1991;66:1270-1272.
29. Wilson D, Sinclair S, McCallion WA, et al. Acute appendicitis in young children in the Belfast urban area: 1985-1992. Ulster Med J 1994;63:3-7.
30. Reynolds SL, Jaffe DM. Diagnosing abdominal pain in a pediatric emergency department. Pediatr Emerg Care 1992;8:12-128.
31. Becker T, Kharbanda A, Bachur R. Atypical clinical features of pediatric appendicitis. Acad Emerg Med 2007;14:124.
32. Bundy D, Byerley J. Does this child have appendicitis? JAMA 2007;298(4): 438-451.
33. Wang LT, Prentiss KA, Simon JZ, et al. The use of white blood cell count and left shift in the diagnosis of appendicitis in children. Pediatr Emerg Care 2007;23:69-76.
34. Kharbanda A, Taylor G, Fishman S, et al. A clinical decision rule to identify children at low risk for appendicitis. Pediatrics 2005;116:709-716.
35. Kwan K, Nager A. Diagnosing pediatric appendicitis: Usefulness of laboratory markers. Am J Emerg Med 2010;28: 1009-1015.
36. Tundidor AM, Amado JA, Montes de Oca JL. Urological manifestations of acute appendicitis. Arch Esp Urol Apr 2005;58:207-212.
37. Heller RM, Hernanz-Schulman M. Applications of new imaging modalities to the evaluation of common pediatric conditions. J Pediatr 1999;135:632-639.
38. Schuh S, Man C, Cheng A et al. Predictors of non-diagnostic ultrasound scanning in children with suspected appendicitis. J Pediatr 2011;158:112-
39. Taylor GA. Suspected appendicitis in children: In search of the single best diagnostic test. Radiology 2004;231:293-295.
40. Howell JM, Eddy OL, Lukens TW, et al. Clinical Policy: Critical issues in the evaluation and management of emergency department patients with suspected appendicitis. Ann Emerg Med 2010;55:71-116.
41. Goldin AB, Khanna P, Thapa M, et al. Revised ultrasound criteria for appendicitis in children improve diagnostic accuracy. Pediatr Radiol 2011;41:993-999.
42. Lowe LH, Penney MW, Stein SM, et al. Unenhanced limited CT of the abdomen in the diagnosis of appendicitis in children: comparison with sonography. Am J Roentgenol 2001;176:31-35.
43. Sivit CJ, Applegate KE, Stallion A, et al. Imaging evaluation of suspected appendicitis in a pediatric population: Effectiveness of sonography versus CT. Am J Roentgenol 2000;175:977-980.
44. Acosta R, Crain EF, Goldman HS. CT can reduce hospitalization for observation in children with suspected appendicitis. Pediatr Radiol 2005;35:495-500.
45. Kharbanda AB, Taylor GA, Bachur RG. Suspected appendicitis in children: Rectal and intravenous contrast-enhanced versus intravenous contrast-enhanced CT. Radiology 2007;243:520-526.
46. Balthazar EJ, Megibow AJ, Siegel SE, et al. Appendicitis: Prospective evaluation with high-resolution CT. Radiology 1991;180:21-24.
47. Mullins ME, Kircher MF, Ryan DP, et al. Evaluation of suspected appendicitis in children using limited helical CT and colonic contrast material. Am J Roentgenol 2001;176:37–41.
48. Hill BC, Johnson SC, Owens EK, et al. CT scan for suspected abdominal process: Impact of combinations of IV, oral and rectal contrast. World J Surg 2010;34:699-703.
49. Hlibczuk V, Dattara JA, Jin Z, et al. Diagnostic accuracy of noncontrast computed tomography for appendicitis in adults: A systematic review. Ann Emerg Med 2010;55:51-59e1.
50. Kaiser S, Finnbogason T, Jorulf HK, et al. Suspected appendicitis in children: Diagnosis with contrast-enhanced versus nonenhanced helical CT. Radiology 2004;231:427-433.
51. Kharbanda AB, Taylor GA, Bachur RG. Suspected appendicitis in children: Rectal and intravenous contrast-enhanced versus intravenous contrast-enhanced CT. Radiology 2007;243:520-526.
52. Laituri CA, Fraser JD, Aguayo P, et al. The lack of efficacy for oral contrast in the diagnosis of appendicitis by computed tomography. J Surg Res 2011;170: 100-103.
53. Garcia K, Hernanz-Schulman M, Bennett DL, et al. Suspected appendicitis in children: diagnostic importance of normal abdominopelvic CT findings with nonvisualized appendix. Radiology 2009;250:531-537.
54. Frei SP, Bond WF, Bazuro RK, et al. Appendicitis outcomes with increasing computed tomographic scanning. Am J Emerg Med 2008;26:39-44.
55. Sale K, Wallace D, Girod D, et al. Radiation-induced malignancy of the head and neck. Otolaryngol Head Neck Surg 2004;131:643-645.
56. Hall EJ. Lessons we have learned from our children: Cancer risks from diagnostic radiology. Pediatr Radiol 2002;32: 700-706.
57. Brenner DJ. Estimating cancer risks from pediatric CT: Going from qualitative to quantitative. Pediatr Radiol 2002;32: 228-231.
58. Krishnamoorthi R, Ramarajan N, Wang N et al. Effectiveness of a staged US and CT protocol for the diagnosis of pediatric appendicitis: Reducing radiation exposure in the age of ALARA. Radiology 2011;259:231-239.
59. Pedrosa I, Zeikus EA, Levine D, et al. MR imaging of acute right lower quadrant pain in pregnant and nonpregnant patients. Radiographics 2007;27:721-743; discussion 743-753.
60. Singh AK, Desai H, Novelline RA. Emergenc MRI of acute pelvic pain: MR protocol with no oral contrast. Emerg Radiol 2009;16:133-141.
61. Kosloske A, et al. The diagnosis of appendicitis in children: Outcomes of a strategy based on pediatric surgical evaluation. Pediatrics 2004;113:29-34.
62. Wong K, Cheung T, Tam P. Diagnosing acute appendicitis: Are we overusing radiologic investigations? J Pediatr Surg 2008;43:2239-2241.
63. Graham JM, Pokorny WJ, Harberg FJ. Acute appendicitis in preschool age children. Am J Surg 1980;139:247-250.
64. Colvin J, Bachur R, Kharbanda A. The presentation of appendicitis in pre-adolescent children. Pediatric Emerg Care 2007;23:849-854.
65. Alvarado A. A practical score for the early diagnosis of acute appendicitis. Ann Emerg Med 1986;15:557-564.
66. Samuel M. Pediatric appendicitis score. J Pediatr Surg 2002;37:872-881.
67. Mandeville K, Pottker T, Bulloch B. Using appendicitis scores in the pediatric ED. Am J Emerg Med 2010;April:1-6.
68. Gorecki WJ, Grochowski JA. Are antibiotics necessary in nonperforated appendicitis in children? A double blind randomized controlled trial. Med Sci Monit 2001;7:289-292.
69. St. Peter SD, Aguayo P, Fraser JD, et al. Initial laparoscopic appendectomy versus initial nonoperative management and interval appendectomy for perforated appendicitis with abscess: A prospective, randomized trial. J Pediatr Surg 2010;45:236-240.
70. Oltmann SC, Garcia NM, Ventura B, et al. Single-incision laparoscopic surgery: Feasibility for pediatric appendectomies. J Pediatr Surg 2010;45:1198-1202.
71. Hansson J, Korner U, Khorram-Manesh A, et al. Randomized clinical trial of antibiotic therapy versus appendicectomy as primary treatment of acute appendicitis in unselected patients. Br J Surg 2009;96:473-481.
72. Turhan AN, Kapan S, Kutukcu E, et al. Comparison of operative and non operative management of acute appendicitis. Uls Travma Acil Cerrahi Derg 2009;15:459-462.
73. Lowe LH, Penney MW, Scheker LE, et al. Appendicolith revealed on CT in children with suspected appendicitis: How specific is it in the diagnosis of appendicitis? Am J Roentgenol 2001;175:981-984.
Abdominal pain is an exceedingly common presentation in the emergency department. Every clinician fears missing the diagnosis of appendicitis. Children are particularly challenging since appendicitis is less common, and the history and physical may be subtle. The diagnostic use of CT is not without its risks and must be balanced against the potential risk of appendicitis in each individual patient. This article provides a comprehensive review of appendicitis in children.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
