EDs grapple with record-breaking number of drug shortages
EDs grapple with record-breaking number of drug shortages
Communications, long-term planning critical to optimizing patient care
Hospitals have been accustomed to dealing with sporadic drug shortages for more than a decade, but now both pharmacists and clinicians are scrambling to keep up with a problem that has proven to be unpredictable and challenging. "Each year has been a record-breaking year," explains Erin Fox, PharmD, manager of the Drug Information Service at the University of Utah Hospitals and Clinics in Salt Lake City, UT. The service has been tracking drug shortages nationally since 2001, and supplying that information to the Bethesda, MD-based American Society of Health-System Pharmacists (ASHP) so that it can be conveyed to practitioners via the organization's public web site. (See Resource Box for links to ASHP web site,below.)
The issue prompted President Obama to issue an executive order instructing the Food and Drug Administration to broaden reporting of potential drug shortages, speed regulatory reviews, and evaluate whether drug shortages are leading to price gouging.
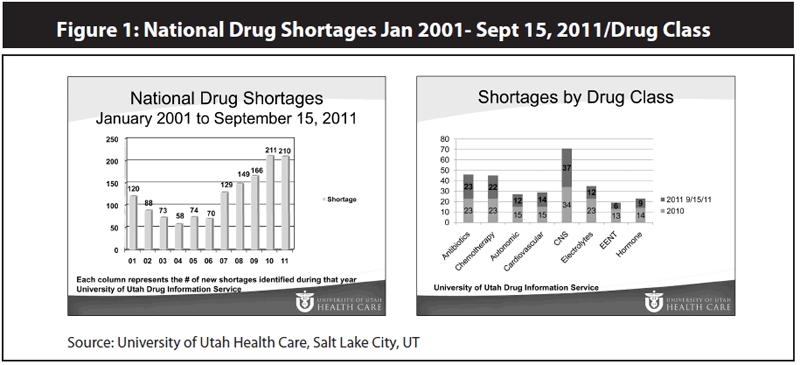
By late September of this year, Fox says there were already 213 documented drug shortages — more than what occurred in all of 2010, with a quarter of the year left to go. In contrast, there were only 70 documented drug shortages in 2006, says Fox. (See Figure 1, below.) "We have just seen this huge explosion in the number of shortages," she says. "And that just makes things very difficult if you are always trying to chase down some form of a drug that might be available."
The drug shortages are impacting all areas of health care, but EDs in particular, with their reliance of quick decision-making, are finding that they need to stay one step ahead of the problem to insure that they have alternatives if a key drug that they routinely rely on is suddenly unavailable.
Be cognizant of safety challenges
"There is usually very short notice that a medication isn't available or a certain formulation isn't available, so we have to notify practitioners of what is available and what isn't, and what the alternatives are," says Michael Argus, MD, medical director, Mercy Hospital Anderson, in Cincinnati, OH. "We have regular meetings that go over what [shortages] are anticipated versus when we are sure that there will be a shortage of a medication. We get the information out via email and direct communications."
With drugs sometimes coming from different makers and in different formulations, ED practitioners must spend more time thinking through how they administer medication, explains Argus. "We need to work more closely with our pharmacy to make sure that we've got the right medication at the right time," he says. "And at times, it means that we have to go to alternative medications in the same class to provide the same symptom relief."
While drug shortages and drug substitutions can certainly interfere with the kind of quick decision-making that is critical when treating trauma patients, Argus suggests that emergency personnel may be more accustomed to making these kinds of adjustments than practitioners in other specialties. "If you are someone who is inclined to doing the same thing over and over, there are some theoretical risks [associated with the drug shortages]," he says. "We are used to responding to the changing climate."
However, most experts agree that with more drug substitutions and other work-arounds, the potential for delays and errors increases. And these problems have already led to patient deaths, according to an anonymous survey carried out by ASHP. In addition, a report from Alabama attributed the deaths of nine patients to an IV solution that was contaminated with bacteria. The IV solution was made by a local pharmacy when supplies from the pharmaceutical manufacturer ran short. In fact, hospitals are increasingly turning to local suppliers when critical medicines are unavailable, according to the Institute for Safe Medication Practices in Horsham, PA.
Make use of clinical pharmacists
"We have been hit from every angle [by the drug shortages], both in general care and specialty care," says Michael O'Neal, DPh, the manager of pharmaceutical procurement at Vanderbilt University Medical Center, a campus that includes an adult hospital, a children's hospital, and a psychiatric facility, in Nashville, TN. For example, O'Neal says the medical center has struggled with multiple shortages in oncology, surgery, and emergency care. "A lot of the emergency syringes that we use in our code carts and with our first responders in our ambulances [have experienced shortages], and we haven't been able to get our hands on certain antibiotics that are first-line treatments for a lot of different infections," he says. "We stay in crisis mode, and we have become less surprised by shortages and more anticipatory of them."
O'Neal says at one point the ED was hit with multiple shortages of basic pain medications such as morphine injections. "We had to shift our ED from using the 10 milligram injections to using the 4 milligram injections, but it was operationally a struggle because the volume they use in the ED is so great, and they had to use basically twice as much ... or two and a half times more," he says. "In these high-stress, high-output areas, change is never good, especially unanticipated change where you haven't had time to implement a good change-management plan."
O'Neal acknowledges that it is tough not having much lead time in knowing what drugs are going to be in short supply, but he manages the problem by staying in constant consultation with practitioners so that they always have an alternative plan in place if a drug they use routinely is not available. "We use our clinical pharmacists. We depend on them a lot because they are out there on the floor and are very relational with the physicians," he says. "We have established communications with our clinical staff where we can get information out quickly."
Practitioners don't always agree with a specific alternative plan, says O'Neal, and he may agree that it is not the best situation, but he stresses that it is frequently all that can be done at that moment.
Prioritize resources
Fox says this type of communication can go a long way toward helping hospitals prioritize their resources in a way that is best for patients. "As soon as pharmacists realize that they can't get [a particular drug] in ... and the shortage is going to last for a few weeks, they should be having a conversation with their providers," she says. "That way, everyone can make a plan together on what is the best way to handle the shortage."
The providers may conclude, for example, that if a drug is in short supply, they only want to use it to treat a particular subset of patients who have high need for that particular drug. This approach may enable the hospital to use the drug for a longer period of time on these select patients who really need it, explains Fox. Alternatively, it may make more sense to simply use a drug until it is no longer available, and then switch to an agreed upon alternative.
Either way, the approach enables practitioners and pharmacists to make thoughtful decisions about what is in the best interests of patient care, says Argus. "As much as you can get people prepared ahead of time, the better your care is going to be," he says.
Sources/Resources
- For the latest information on current and anticipated drug shortages collected by the Drug Information Service at the University of Utah Hospitals and Clinics in Salt Lake City, UT, visit the web site of the American Society of Health-System Pharmacists at www.ashp.org/shortage.
- For more information about legislation focused on relieving problems related to shortages of critical drugs, visit the web site of the American Society of Health-System Pharmacists at www.ashp.org/menu/Advocacy/FederalIssues/DrugShortages.aspx.
- Michael Argus, MD, Medical Director, Mercy Hospital Anderson, Cincinnati, OH. Email: [email protected].
- Jeff Beeson, DO, medical director, MedStar Emergency Medical Services, Fort Worth, TX. Email: [email protected].
- Raymond Fowler, MD, FACEP, Chief of EMS Operations, BioTel EMS System, University of Texas Southwestern Medical Center in Dallas, TX. E-mail: [email protected].
- Erin Fox, PharmD, Manager, Drug Information Service, University of Utah Hospitals and Clinics, Salt Lake City, UT. E-mail: [email protected].
- Michael O'Neal, DPh, Manager of Pharmaceutical Procurement, Vanderbilt University Medical Center, Nashville, TN. Email: [email protected].
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
