Pediatric Skin Infections
Pediatric Skin Infections
Authors:
Perry Stafford, MD, Professor of Surgery, Chief, Division of Pediatric Surgery, Robert Wood Johnson Medical School, University of Medicine and Dentistry of New Jersey, New Brunswick, NJ.
Terrence Curran, MD, Children's Hospital of Pittsburgh, PA.
Peer Reviewer:
Catherine A. Marco, MD, Professor, Department of Emergency Medicine, Program Director, Emergency Medicine Residency, University of Toledo College of Medicine, Toledo, OH.
The skin is a dynamic organ, accounting for 15-20% of total body weight, and exhibits many functions such as protection against thermal and mechanical insults and against pathogenic microorganisms. The skin is also responsible for many other functions, such as sensory, thermoregulation, as well as metabolic functions such as synthesizing vitamin D. This article reviews pediatric skin infections, common presentations, diagnosis, and treatment.
Ann M. Dietrich, MD, Editor
Infectious Conditions
Bacterial. Impetigo, Ecthyma, and Bacterial Intertrigo. Impetigo is a very common superficial skin infection seen among the pediatric population. It presents as moist, honey-colored crusts that originate as small vesicles. It usually presents on exposed areas, with the nose, face, and extremities being the most common sites. Impetigo is highly contagious, and overcrowding, poor sanitation, and poor hygiene contribute greatly to its spread. (See Figure 1.)
Figure 1. Impetigo
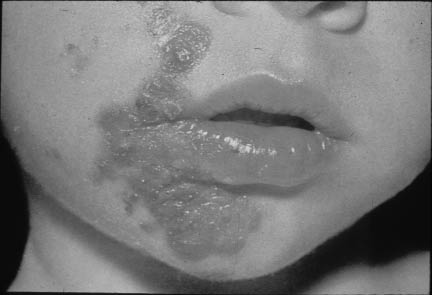
Ecthyma is a deeper form of impetigo that invades the dermis and is characterized by a vesiculopustule with an erythematous base and firmly adherent crust.
Bacterial intertrigo (see Figure 2) is an inflammatory response to infection in skin folds and areas that tend to be moist, such as axilla and interweb spaces of the toes, neck, and groin.
Figure 2. Intertrigo
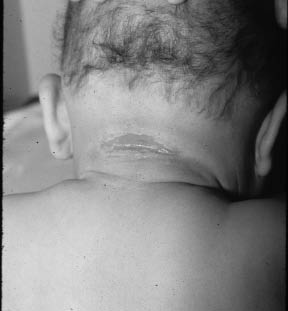
Image courtesy of Dr. Jonathan Singer
The typical pathogenesis of these infections is a minor trauma to the epidermis, such as a bug bite or scratching of dry skin and subsequent infection, most commonly with either Staphylococcus aureus or group A beta-hemolytic streptococcus (GABHS). Although S. aureus is the most common etiologic agent, methicillin-resistant Staphylococcus aureus (MRSA) is now recognized in 70-80% cases.1
Diagnosis can usually be made clinically, but there are other conditions that may mimic impetigo, such as herpes simplex infections, candidiasis, or contact dermatitis. Bacterial culture may be needed to confirm the diagnosis and may help tailor the treatment.
Treatment normally consists of a systemic antibiotic such as a first-generation cephalosporin or dicloxacillin. If MRSA is confirmed on culture, treatment should be tailored based on cultures, but trimethoprim/sulfamethoxazole or clindamycin should be considered as first-line therapies. Other choices may include fluoroquinolones, tetracyclines, or rifampin, but there may be increased resistance to these antibiotics.2
If there are frequent recurrences, one should consider the likelihood of carrier status. Cultures of the nares, axillae, etc., may confirm suspicions.
In addition, patients and family members should be advised of the importance of good hygiene, especially hand washing, and the importance of completing the full course of prescribed antibiotics. Children should not return to school until they have taken the antibiotics for at least 24 hours.
Cellulitis. Cellulitis is an inflammatory response to infection that presents with erythema, swelling, tenderness, and warmth of the skin. Systemic signs such as fever, chills, and fatigue may accompany it.3
The pathogenesis is usually a bacterial infection, most commonly pathogenic streptococci or Staphylococcus aureus, following a puncture wound, laceration, some form of trauma, or even a preceding viral infection.
Other less frequent causes of cellulitis include Pseudomonas aeruginosa cellulitis in patients with neutropenia or other predisposing conditions; Eikenella corrodens from a human bite; and Aeromonas hydrophila or Vibrio vulnificus from fresh or salt water lacerations, respectively. A thorough history of any preceding trauma may help in developing a list of probable pathogens.
Treatment of cellulitis should cover GABHS and S. aureus. In routine cases, oral outpatient therapy includes trimethoprim-sulfamethoxazole or clindamycin. In more serious cases, hospitalization for IV vancomycin may be needed.
Periorbital cellulitis requires special attention. If not treated aggressively, periorbital cellulitis may lead to orbital cellulitis, a condition that can lead to abscess formation and cavernous sinus thrombosis.4
Hospitalization for IV antibiotics is required, and a CT scan to exclude an abscess should also be strongly considered. A bluish tinge to the cellulitis should lead one to consider H. influenzae as the pathogen.
Other unique forms of cellulitis include perianal streptococcal dermatitis, erysipelas, and blistering dactylitis. (See Figures 3 and 4.)
Figure 3. Erysipelas
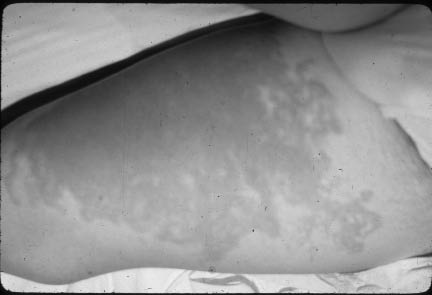
Image courtesy of Dr. Jonathan Singer
Figure 4. Dactylitis

Image courtesy of Dr. Jonathan Singer
Perianal dermatitis is a superficial infection localized to the perianal area. It most commonly presents in boys ages 6 months to 10 years, and many have a concomitant pharyngeal infection. Rectal pain with defecation, constipation, and blood-streaked stools are commonly associated with the infection.5 Perianal cellulitis may be confused with a rectal fissure that also causes severe pain with defecation. While Streptococcus pyogenes was once the major pathogen, there has been a shift in the epidemiology, and S. aureus is now more common.6
Penicillin V is considered the first choice for its effectiveness against GABHS. Alternatives in cases of penicillin allergy are erythromycin or macrolides. Additional topical therapy with antiseptic, chlorhexidine, clioquinol, or antibiotic ointments is widely used and may accelerate bacterial clearance.7
Erysipelas is a superficial form of cellulitis that is associated with marked lymphatic involvement usually secondary to infection with GABHS. (See Figure 3.) Although it can appear anywhere on the skin, the face, hands, and scalp are the most common sites of involvement. Penicillin or a macrolide is sufficient treatment, and most cases resolve without long-lasting sequelae.
Blistering dactylitis is an infection with group A beta-hemolytic Streptococcus or Staphylococcus aureus of the fingertips. (See Figure 4.) It results in painful tense blisters with an erythematous base on the volar surface of the distal phalanx. It may be confused with herpetic whitlow. It is most commonly associated with Streptococcus, but one should also consider S. aureus as the pathogen. Treatment should be directed at the above two pathogens.
Scarlet Fever. Scarlet fever is a rash that occurs secondary to infection from streptococci. It occurs most often in children 2-10 years of age and may present with a sore throat or a skin infection. Symptoms include sore throat, fever, chills, malaise, headache, abdominal pain, and vomiting.8 Signs include erythematous macules and papules that begin on the neck and spread down over the trunk and purulent tonsillitis. The patient may also have a strawberry tongue (see Figure 5) or Pastia's signs, lines of hyperpigmentation seen in the body folds such as the antecubital fossa, as well as significant lymphadenopathy. The syndrome is secondary to fever-producing exotoxins from the streptococci, which are released when the bacteria are infected with a virus.
Figure 5. Scarlet Fever

Image courtesy of Dr. Jonathan Singer
Scarlet fever may be confused with several viral syndromes, such as measles, rubella, or infectious mononucleosis, or allergic drug reactions.
Scarlet fever once produced feared sequelae such a rheumatic fever and acute glomerulonephritis, but prompt treatment can minimize these sequelae. Treatment should consist of a 10-day course of penicillin or erythromycin, and patients and parents should be counseled about the importance of completing the full course of antibiotics.
Folliculitis, Furunculosis. Folliculitis is an infection of the hair follicles, while furuncles are perifollicular abscesses that present as painful erythematous nodules.
Folliculitis tends to occur on the buttocks and extremities and is overwhelmingly the result of S. aureus infection. Superficial folliculitis can normally be treated with good hygiene and a topical antibiotic such as mupirocin.9
Hot Tub Folliculitis. Also known as pseudomonal folliculitis, hot tub folliculitis is caused by exposure to poorly chlorinated hot tubs, whirlpools, or swimming pools. Lesions usually appear 1-2 days after exposure and are erythematous follicular pustules and vesiculopustules. Lesions generally resolve spontaneously and no specific treatment is needed.
Furuncles and carbuncles generally need more invasive treatment with incision and drainage as well as antibiotics aimed at S. aureus. Antibiotic treatment should be aimed at S. aureus in areas where MRSA is prevalent; clindamycin or trimethoprim-sulfamethoxazole should be used empirically.
The differential diagnosis includes acne vulgaris, contact dermatitis, or cutaneous abscesses. As with all superficial bacterial infections, patients other family members should be advised of the importance of good personal hygiene as well. If there are recurrent infections, then further evaluation for immunodeficiency conditions or diabetes should be undertaken. There may also be a reservoir of bacteria, such as a family pet, that may facilitate repeated infections.
Cat Scratch Disease. Cat scratch disease occurs secondary to infection with Bartonella henselae, a gram-negative bacillus, and is normally transmitted by a scratch or bite from an infected cat or kitten.
It commonly presents as a benign but tender regional lymphadenopathy, but a good history usually recalls a small papule or nodule at the site of the injury inflicted by a cat. There is usually a two-week to two-month interval between the cat scratch and the appearance of the lymphadenopathy. Lymph nodes may remain enlarged for up to one year.10 Fever is seen in about one-third of patients, as well as generalized fatigue and headache.
Diagnosis is usually clinical since it is difficult to culture the bacteria, but diagnostic techniques have improved.11 Diagnostic modalities include Starry silver impregnation stain as well as molecular diagnostic tests.
Cat scratch disease may be confused with viral infections that cause prolonged lymphadenopathy, such as mononucleosis or HIV infection, or lymphoma or mycobacterial infections.
Treatment is not always necessary in the immunocompetent patient, but it is recommended for immunocompromised patients.12
Lyme Disease. Lyme disease is transmitted by tick bites, predominantly the deer tick, Ixodes dammini, and is caused by the bacteria Borrelia burgdorferi. The risk of acquiring Lyme disease in the United States varies with the distribution, density, and prevalence of infection in vector ticks. Although it is spread throughout the United States, most cases of Lyme disease occur in the northeastern and north-central states.13
Lyme disease is broken down into 3 stages. Stage 1 is called primary Lyme disease, stage 2 is called secondary Lyme disease or early-disseminated Lyme disease, and stage 3 is called tertiary Lyme disease or chronic persistent Lyme disease.
In primary disease, the earliest manifestation is a unique rash known as erythema chronicum migrans. (See Figure 6.) This can occur anywhere from 4-20 days after the tick bite, but many patients do not specifically remember the bite. Other associated symptoms with early Lyme disease include fatigue, fever, chills, headache, muscle and joint aches, and swollen lymph nodes.14
Figure 6. Lyme Disease Erythema Migrans
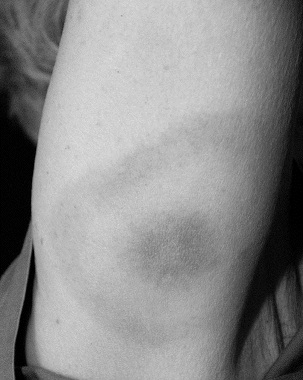
Source: CDC/James Gathany
If Lyme disease goes untreated, it will progress to stage 2 in 50-60% of patients and results in rheumatologic, dermatological, cardiac, and central nervous system symptoms such as additional ECM lesions on other areas of the body, neurological symptoms such as Bell's palsy and meningitis that may include changes in behavior and peripheral radiculopathies, rheumatologic symptoms such as monoarticular arthritis in large joints with a warm, swollen, and tender joint without associated erythema, and cardiac symptoms such as palpitations. A small percentage of patients can develop atrioventricular block or even a pericarditis.
Even without treatment, many of these symptoms will resolve over a period of weeks to months, but nearly 60% of patients with untreated infection may experience recurrent bouts of severe arthritis, with large joints, particularly the knees, being affected most commonly. Up to 5% of untreated patients may develop chronic neurological complaints months to years after infection that include shooting pains, numbness or tingling in the hands and feet, and problems with short-term memory.
Erythema chronicum migrans may be misdiagnosed as a tinea infection, but it does not violate the epidermis, whereas a tinea infection does. If the classic ECM rash is seen, a diagnosis of Lyme disease may be made and treatment instituted. If a patient presents with symptoms of later stages, then serology should be sent for IgM, and a Western blot may be done as well.
Treatment of Lyme disease for children older than the age of 8 years is oral doxycycline twice daily for three weeks. Doxycycline is relatively contraindicated in children younger than 8 years of age. Antibiotics recommended for children younger than 8 years are amoxicillin or cefuroxime axetil.15
Prophylaxis is controversial in instances of tick bites. The American Academy of Pediatrics does not recommend it, while the Infections Diseases Society of America guidelines recommend it only in specific circumstances.15-17
Patients should be educated in methods of tick repellent and avoidance of high-risk areas; the importance of completing the full course of antibiotics to avoid complications should be stressed.
Viral Rashes
Viral infections are a large portion of pediatric practice and can be thought of as those that primarily affect the skin, such as herpes, molluscum contagiosum, or warts, and those that are systemic but have dermatologic manifestations.
Primary Localized Skin Infection
Herpes Simplex. Herpes simplex virus 1 (HSV-1) and HSV-2 are both part of the larger family of herpesviruses that include Epstein-Barr virus, cytomegalovirus, varicella zoster virus, and human herpesviruses 6-8.
Herpes simplex infection can present in variety of ways. Herpetic gingivostomatitis and herpetic whitlow are the more common presentations seen in children, but other forms of herpes simplex infection include genital herpes (likely to be seen in adolescents), herpes labialis, herpetic keratoconjunctivitis, cutaneous herpes and eczema herpeticum, and neonatal herpes.
HSV-1 infections are extremely prevalent, with an estimated 18-35% of children being infected by the age of 5 years, and nearly 90% of adults having antibodies to HSV-1. HSV-2 infections are commonly acquired by sexual contact, although the strict separation between the two sites is changing.
Herpetic gingivostomatitis is most commonly seen in children ages 1-5 years. It presents with perioral vesicles on an erythematous base that evolve into painful, shallow, gray ulcerations. The lesions often involve the palate, tongue, and gingivae, and may be seen around the mouth, chin, lips, and cheeks in up to 75% of patients. Fever, drooling, irritability, and avoidance of eating and drinking are common.
Herpes simplex infection tends to be self-limiting over 10 days to two weeks, but some patients may need hospitalization for treatment of dehydration due to poor oral intake. Some advocate treatment with acyclovir, which seems to reduce the time to healing and is most effective if started within three days of the outbreak, but the FDA has not approved any antiviral agent for initial primary gingivostomatitis.18
Herpes labialis is the most common type of recurrent herpes infection and appears on the lips, normally around the vermillion border. Patients may report several days of tingling, itching, or burning in the area prior to eruption of the lesion. Topical or oral antiviral agents are helpful in treating this form of herpes if started within 1-2 days of the outbreak.
Herpetic keratoconjunctivitis is an infection of the eye that can result in severe purulent conjunctivitis with edema, erythema, and vesiculation with superficial erosion or ulceration of the cornea. Patients present with pain, blurry vision, swelling, and conjunctivitis. An ophthalmology consult is indicated, and treatment with topical and oral antiviral agents generally leads to resolution within two weeks without permanent damage.
Genital herpes is extremely prevalent, and it is estimated that about 1 in 6 Americans between the ages of 14 and 49 years is infected with HSV-2. HSV-2 is a lifelong and incurable infection that can cause recurrent and painful genital sores.19 Risk factors include race, age, years of sexual activity, number of partners, lower socioeconomic standing, and the presence of other sexually transmitted diseases.
Genital herpes presents with painful vesicles clustered on an erythematous base and may be distributed throughout the genital area. The vesicles eventually rupture and leave painful erosions or ulcers that may be associated with itching, dysuria, vaginal or urethral discharge, and tender inguinal lymphadenopathy.20 These symptoms usually resolve over the period of a week, and the cutaneous lesions heal over 2 to 4 weeks.
The choice of antiviral therapy can include oral acyclovir, famciclovir, or valacyclovir, all of which improve the time of healing. Long-term therapy for frequent recurrent infections can help to reduce both the intensity and frequency of infections.
Patients should be counseled about the contagious nature of the lesions. The CDC recommends that persons with genital herpes should abstain from sexual activity with uninfected partners when lesions or other symptoms of herpes are present. It is important to know that even if a person does not have any symptoms, he or she can still infect sex partners. Sex partners of infected persons should be advised that they may become infected and they should use condoms to reduce the risk. Sex partners can seek testing to determine if they are infected with HSV.21
Cutaneous herpes can occur anywhere on the body. It may be confused with other infections of the skin such as impetigo or herpes zoster.
Eczema herpeticum is a severe disseminated HSV infection that occurs in children with atopic dermatitis and other chronic skin conditions. Patients present with abrupt onset of fever, malaise, and widespread eruption of vesicles and erosions.22
Complications of eczema herpeticum include secondary bacterial infection, herpetic keratoconjunctivitis, dehydration, and viremia. Treatment should include IV hydration and IV antiviral therapy as well as treatment of secondary complications.
Molluscum Contagiosum. Molluscum contagiosum is a common viral infection in children that presents as discrete, dome-shaped, waxy or pearl-like lesions on the skin. It most commonly presents in young children and young adults and spreads in a variety of ways. Direct physical contact is a common way and there are reports of epidemics related to public swimming pools. The incubation period can be anywhere from two to eight weeks.
Patients typically present complaining of the appearance of the rash, but may also complain of itching or soreness associated with the lesions. The most common location in children is in the axillae, side of the trunk, lower abdomen, thighs, and face. Widespread cutaneous infection may occur in immunosuppressed individuals or those with pre-existing skin conditions.
This condition nearly always resolves spontaneously in individuals with competent immune systems and patients should be counseled to stay out of heated swimming pools and hot tubs, as well as to take showers as opposed to baths. If further treatment is needed, a variety of topical treatments, such as tretinoin cream, benzoyl peroxide, or imiquimod, are efficacious.
Viral Exanthems
Measles. Despite a very active immunization program within the United States, measles has not been eradicated. It is at its lowest prevalence in history, but during 2008, more measles cases were reported than in any other year since 1997. More than 90% of those infected had not been vaccinated or their vaccination status was unknown.23
Measles has an incubation period of 9 days to 2 weeks, which is then followed by a high fever, a barking cough that may be confused with croup, rhinitis, and conjunctivitis. Cervical lymphadenopathy is usually present, as is preauricular adenopathy. The cutaneous eruption is preceded by intense erythema of the mucous membranes that is speckled with white spots known as Koplik spots. The cutaneous morbilliform eruption begins on the forehead and spreads to the face, trunk, and extremities.
Even in previously healthy children, measles can be a serious illness requiring hospitalization. Measles can be complicated in up to 30% of cases. Pneumonia, which occurs in up to 5% of cases, is the complication that is most often the cause of death in young children. Bacterial otitis media occurs in about 10% of cases and can lead to permanent hearing loss. Diarrhea is reported in about 8% of cases. These complications are more common among the extremes of age, with children younger than 5 years of age and adults older than 20 years being most at risk. About 1 child in every 1,000 who get measles will develop encephalitis that can lead to permanent cognitive problems and death. For every 1,000 children who get measles, 1 or 2 will die from it.
There is no specific treatment for measles except for supportive therapy and antibiotic therapy for bacterial infectious complications. If given within 6 days of exposure, measles immune globulin may prevent or mollify the course of the disease. Additionally, vitamin A supplementation in children 1 year old or older may help prevent complications.
Patients and their family members should be advised of the very contagious nature of measles, and any case of measles should be reported to the health authorities.24
Rubella. Rubella is also known as German measles and may be confused with measles. Rubella exposure in utero during the first trimester leads to a syndrome that includes neonatal purpura and petechiae secondary to thrombocytopenia. Other effects of congenital rubella include deafness, congenital heart disease, cataracts, retinopathy, glaucoma, growth retardation, behavioral disorders, meningoencephalitis, and psychomotor retardation.25
The clinical syndrome may be entirely asymptomatic in up to 50% of cases. In general, the child appears well, and in young children, there is generally no fever. Adolescents may present with fever, especially when arthritic symptoms are present. The dermatological manifestations may be preceded by suboccipital and posterior auricular lymphadenopathy.
The exanthem is a faintly erythematous macular eruption that starts on the face and then spreads to the trunk and proximal extremities. Within two days, this rash resolves and the distal extremities become involved.
There is a constellation known as STAR (sore throat, arthritis, and rash) that is sometimes seen in conjunction with rubella, most often in adolescent girls.
There is no specific treatment for postnatally acquired rubella outside of symptomatic treatment aimed at fever and arthritis, but it important to ensure that the patient has not come in contact with pregnant women. Patients may be contagious from 2 days prior to the eruption of the exanthem until 7 days afterward. During this time, the child should be kept away from pregnant women.
Roseola. Roseola occurs predominantly as the result of infection with either human herpesvirus (HHV) 6 or 7 in children younger than 2 years old. It is sometimes the result of an infection with echovirus 16.
There is a predictable pattern of three days of fever, which then resolves and leads to an eruption of a pink, morbilliform rash predominantly on the trunk that fades within 24 hours. The fever may be high enough to result in seizures, although the exact incidence of fevers in roseola is unknown. Associated findings may include mildly edematous eyelids and posterior cervical lymphadenopathy. Occasionally, the fever may be accompanied by a cough and otitis media.
Roseola is distinguished from other similar rashes by the high fever associated with roseola that lasts for three days. HHV 6 or 7 can be identified in cultures of peripheral leukocytes, by serodiagnosis, or using molecular sequencing of the skin lesions, but often the clinical presentation is enough to make the diagnosis.
There is no specific treatment since most cases are self-limiting. Supportive care should be aimed at control of fever with antipyretic medications and baths, as well as anti-inflammatory medications for arthritis. The exception to this is in immunosuppressed patients who can develop encephalitis as a result of HHV 6 or 7 reactivation or infection. They should be treated with antiviral medications.27
Parvovirus. Human parvovirus B19 infection leads to fifth disease, so called because it was the fifth childhood disease characterized by a rash to be identified. Fifth disease starts as an intense erythema of both cheeks (which is why the disease is also referred to as "slapped cheek disease") after an incubation period of 4-14 days. The rash normally lasts 3-5 days and then resolves, but may return for up to 4 months and is exacerbated by vigorous exercise, overheating, and sun exposure. The rash may also involve other parts of the body such as the extremities, trunk, and abdomen.
The infection may also result in the STAR syndrome, as described in the section on rubella. Parvovirus B19 infection can also present as acute arthritis, which can be mistaken for acute rheumatoid arthritis. Arthritis involving the hands, wrists, or knees occurs and normally resolves in 1-2 months and should be treated symptomatically with nonsteroidal anti-inflammatory drug (NSAID) pain relievers. Parvovirus B19 IgM, rash, and familial history can help to distinguish parvovirus arthritis from acute rheumatoid arthritis.28
The feared complication of parvovirus infection is nonimmune hydrops fetalis (NIHF). It is estimated that parvovirus infection is responsible for 15–27% of all cases of NIHF.29 Parvovirus infects red blood cell precursors, which stops their maturation and can lead to severe anemia in the fetus producing nonimmune hydrops fetalis. Other patient populations who are at risk of severe complications of parvovirus infection include immunosuppressed patients and those with hemolytic anemias such as sickle cell disease.
Counseling of pregnant women who become exposed during pregnancy is important. Overall, only 50% of women are susceptible. Of those exposed, approximately 30% become infected. Then, approximately 25% of exposed fetuses become infected, and approximately 10% of infected fetuses die. Consequently, the risk of fetal death in a woman with known exposure to parvovirus B19 is approximately 0.4%. If the woman is seropositive, the risk approximates zero; if she is seronegative, the risk is about 0.8%.29 There is no specific treatment for parvovirus, and patients should be treated symptomatically. Immunoglobulin may help immunosuppressed patients.
Infectious Mononucleosis. Infectious mononucleosis is most often the result of infection with the Epstein-Barr virus (HHV 4) and is most often seen in the adolescent population. It presents with fatigue in nearly all patients, with fever, generalized lymphadenopathy, exudative tonsillitis, headache, and splenomegaly in most.
A pink transient morbilliform rash may be present in 15% of patients, but in those treated with antibiotics aimed at the sore throat, the incidence of the rash increases to nearly 80%. The antibiotic-associated rash may persist for 7-10 days.
Urticaria may also be present, and urticaria in response to cold has been described. Other symptoms include palmar erythema and neurologic symptoms, such as signs of encephalitis; meningitis and Guillain-Barré syndrome may also accompany the rash.
Diagnosis of mononucleosis is best done with the Paul-Bunnell test (heterophil), but in children younger than 4 years, EBV-IgM serology is preferred because of the high percentage of false negatives in this age group.
Antiviral treatment with acyclovir has not been shown to be effective, and antibiotics should not be given to avoid worsening of the exanthem.
Patients should be educated about the rare but potential risks of splenic rupture and should be advised to avoid contact sports or vigorous activity that might increase this risk. They should also be advised of the possible neurologic complications and the need to seek prompt medical care if this occurs.
Gianotti-Crosti Syndrome. Gianotti-Crosti syndrome is a benign, self-limiting condition with a distinct rash known as papular acrodermatitis that is characterized by groups of large, flat-topped nonpuritic papules that characteristically appear on the cheeks, buttocks, and extremities, with particular prominence on the elbows, knees, and hands.
The large majority of patients are younger than 3 years of age, and the eruption persists for 2-8 weeks. A low-grade rash and an upper respiratory tract infection may precede the rash. Some children may develop a generalized lymphadenopathy and, occasionally, a hepatosplenomegaly may appear.
In Europe, acrodermatitis is frequently associated with hepatitis B, but this is rarely seen in the United States. Epstein-Barr virus (EBV) is the virus most often associated with acrodermatitis, but cytomegalovirus, coxsackieviruses, parainfluenza virus, respiratory syncytial virus (RSV), and some live virus vaccines have also been associated with the disorder.
Gianotti-Crosti syndrome may be confused with many skin disorders, such as contact dermatitis, lichen planus, or severe pruritus. Diagnosis may include hepatitis virus serology or hepatitis B surface antigen, liver function tests, screening for EBV antibodies, serum zinc level, and a skin biopsy.
There is no specific treatment for acrodermatitis. Patients and parents should be counseled about the prolonged nature of the rash.
Varicella Infection. Infection with human herpesvirus-3 results in what is commonly known as chickenpox. It presents as a sudden onset of pale, erythematous macules that transition into edematous papules and finally become vesicles within 24-48 hours. These vesicles eventually crust over and shed, leaving superficial erosions. Over the next 2-5 days, successive waves of lesions may appear so that there are lesions of varying stages at any one time. The number of lesions that appear can have a very wide range, even among members of the same family.
Associated symptoms, such as fever, are usually mild but the disease is highly contagious from 1-2 days before to 5-6 days after the appearance of lesions. Complications of the infection include secondary bacterial infection of the lesions, often with S. aureus, occasionally pneumonia, and Reye's syndrome. Varicella infection in immune-compromised patients can produce high fever, encephalitis, pneumonia, and even disseminated intravascular coagulation.
The introduction of universal varicella vaccination in 1995 has substantially reduced varicella-related morbidity and mortality in the United States. One dose of varicella vaccine was 84.5% effective in preventing all varicella and 100% effective in preventing severe varicella. Post-exposure administration is highly effective in preventing or modifying varicella.30 However, it remains unclear whether vaccine-induced immunity fades over time, which may lead to susceptibility later in life, when the risk of serious complications may be greater than in childhood.31 Therefore, varicella should remain part of a differential diagnosis even if the child or adolescent has had the varicella vaccine.
Varicella can be confused with hand, foot, and mouth disease, as well as disseminated HSV. A Tzanck smear of a vesicle will help differentiate the HSV from varicella.
In an otherwise healthy child, no specific therapy is needed. Salicylates should be avoided to prevent Reye's syndrome. In immunosuppressed patients who are exposed, zoster immune globulin administered within 72 hours may reduce symptoms. If the lesions are secondarily infected, antibiotic treatment should be aimed at S. aureus, with consideration of the possibility of MRSA infection.
A recurrence of varicella infection results in herpes zoster that begins as macules and papules that progress to vesicles along contiguous dermatomes.
Anywhere from 1 to 5 days prior to the rash, there may be pain, itching, or tingling in the area where the rash eventually develops. Associated symptoms may include fever, headache, chills, and an upset stomach.
Post-herpetic neuralgia is the most common complication of herpes zoster. Additionally, shingles may lead to serious complications involving the eye and, very rarely, shingles can also lead to pneumonia, hearing problems, blindness, brain inflammation (encephalitis), or death.
Acyclovir, valacyclovir, and famciclovir are approved for the treatment of shingles. These antivirals will help shorten the length and severity of the outbreak, but they must be started as soon as possible after the rash appears. Analgesics may help relieve the pain caused by shingles, while wet compresses, calamine lotion, and colloidal oatmeal baths may help relieve some of the itching.
Hand, Foot, and Mouth Disease (HFM). Enterovirus 71 and numerous types of the coxsackievirus can lead to the development of HFM disease. Enterovirus 71 is associated with outbreaks in China and Vietnam and, although rare, is more commonly associated with severe symptoms and mortality. In the United States, coxsackievirus A16 is the most common causative agent.32
The typical presentation is that of a young child, most commonly ages 1-4 years, with fever, malaise, and an exanthem and enanthem. The exanthem consists of grey-white vesicular lesions on the palms of the hands and the soles of the feet. The enanthem presents as vesicles and shallow ulcers of the tongue, buccal mucosa, and the palate. These lesions can be very painful, leading to aversion of oral intake and, subsequently, dehydration. Lymphadenopathy may also be present occasionally around the cervical and submandibular regions.
The course is generally benign, and supportive therapy with fluids, pain control, and antipyretics are the mainstays of treatment. Hospitalization is occasionally required for IV fluids and pain control. Although it is rare, HFM disease can be associated with meningitis, encephalitis, and polio-like paralysis, so any neurological symptoms must be taken seriously. This is more common when the causative agent is enterovirus-71.33,34
Potentially Fatal Conditions
Meningococcemia. Neisseria meningitidis infection is the leading cause of bacterial meningitis in children and can present with a wide range of symptoms from transient fever to severe meningitis. Transmission is secondary to inhalation of nasopharyngeal secretions infected with the bacteria Neisseria meningitidis.35
Patients present with a nonspecific prodrome of cough, headache, and sore throat that is followed by very rapid onset of fever with chills, arthralgias, and myalgias. Meningitis can accompany meningococcemia and results in headache, neck stiffness, lethargy, and drowsiness.
Up to two-thirds of patients manifest dermatologic lesions that most commonly include a petechial rash on the skin and mucous membranes, but may also include macular, urticarial, or morbilliform macules and papules.
The speed of progression of this disease cannot be emphasized enough. In fulminant meningococcemia, cardiovascular collapse occurs within a few hours, with rapid enlargement of petechiae and purpuric lesions, as well as a consumptive coagulopathy. These progressive lesions, termed purpura fulminans, represent cutaneous hemorrhage and necrosis.
Treatment should not be delayed, as time is of the most importance. Penicillin G is the treatment for meningococcal disease, but at the time of presentation, ceftriaxone is often used until the diagnosis is confirmed. Blood, urine, sputum, and CSF cultures should be obtained. Respiratory isolation and monitoring in an ICU setting are also appropriate.
Staphylococcal Scalded Skin Syndrome (SSSS). SSSS is the result of infection with Staphylococcus aureus and describes a blistering skin disease that is the result of toxins produced by S. aureus. The toxins, which are epidermolytic, target desmoglein 1, which is a cell-cell adhesion molecule.
SSSS presents initially as a local infection of the conjunctivae, oral region and nares, perineum, or umbilicus,36 and previous infection is often a preceding event. SSSS should be distinguished from TEN, which is most reliably done by skin biopsy.
Treatment is aimed at resuscitation, treatment of infection, pain control, and skin care. Penicillin and intravenous penicillinase-resistant penicillin should be commenced at high doses as soon as blood cultures have been taken.37
Neonates, infants, and severe cases in children should be treated in an ICU setting and consideration should be given to transferring the patient to a burn unit.
Fungi
Dermatophytes are fungi that invade the outer layer of the epidermis and proliferate. They may also invade the hair and the nails. These infections increase in prevalence with age and are more common in hot, humid climates and crowded living conditions as seen in urban areas. Different organisms can be responsible for the same clinical presentation, and treatment needs to be tailored to the organism to ensure the condition resolves.
Tinea Capitis. Tinea capitis is a dermatophyte infection of the scalp by one of several organisms. In the United Kingdom, United States, Jamaica, and Brazil, T. tonsurans is shown to represent 60-90% of tinea capitis infections, whereas M. canis is more prevalent in central and southern Europe, Saudi Arabia, and Puerto Rico.38
Tinea capitis presents as six different clinical forms: black dot, grey patch, moth eaten, kerion, diffuse scale, and pustular.38
Black dot ringworm is a noninflammatory stage that occurs when hairs break off at the follicle and leave small dark hairs in the follicles.39
The grey patch and moth-eaten presentations contain patchy hair loss with an erythematous scalp, patchy alopecia, and may last from 1 month to several years. The diffuse scale type may be confused with a generalized dandruff. The pustular type is difficult to diagnose and can be secondarily infected with bacteria or other fungi. This form results in boggy pus-containing kerions that can be complicated by scarring with alopecia even if appropriately treated.
Diagnosis of tinea capitis can be done with a Woods lamp, potassium hydroxide examination, or fungal culture. Woods lamp examination will diagnose M. canis but does not pick up T. tonsurans, so it cannot be used to exclude infection.
Potassium hydroxide examination is difficult to perform, but, if prepared properly, hyphae and spores may be seen within the hair shaft. Fungal culture is considered the gold standard and is the most reliable method of diagnosing tinea capitis. Consider culturing family members, since almost 50% of family members will be positive as well.
T. tonsurans should be treated with oral griseofulvin for a minimum of 4 weeks, but 2-3 months is often needed to completely resolve the infection. An additional treatment option is terbinafine. Topical antifungals are not effective. M. canis should be treated with griseofulvin as well, and an antifungal shampoo used twice weekly may also hasten the resolution of the infection. Antibiotics and steroids are not necessary.
Parents and patients should be counseled not to share combs, brushes, or head wear. Inquiry should also be made about household pets that may serve as a reservoir of dermatophytes, and efforts should be made to treat the animal as well to prevent recurrent infections.
Tinea Corporis. Tinea corporis occurs as a result of dermatophyte infection of the skin on various areas of the body and appears as a pruritic, circular, erythematous, scaly patch that spreads outward. The most common dermatophytes responsible for tinea corporis are M. canis, T. mentagrophytes, T. tonsurans, T. verrucosum, M. gypseum, Epidermophyton floccosum, and T. rubrum. Epidemics as a result of T. gladiatorum infection have been seen in wrestlers.
Tinea corporis that is misdiagnosed as eczema and treated with steroids will lose its characteristic appearance. Scaling will not be seen, and the annular border will be obscured. This is known as tinea incognito.
Tinea corporis generally responds well to the daily application of topical antifungals. For severe cases, patients who are severely immunocompromised, or in those patients who have failed topical treatment, a systemic agent may be preferable.
Tinea Faciei. Tinea faciei most often occurs in young children. The most common organism is M. canis, while others include T. rubrum and T. mentagrophytes in both typical and atypical forms. It typically appears as single or multiple blemishes and circular erythematous-scaling patches with central clearing. Atypically, it may appear as a more severe inflammatory reaction with ill-defined borders, central scaling, and the presence of follicular papules and vesicle-pustules instead of clearing, with occasional edema and hyperpigmentation.40
Tinea faciei often mimics other illnesses such as lupus erythematosus, polymorphous light eruption, rosacea, seborrhoeic dermatitis, atopic dermatitis, contact dermatitis, perioral dermatitis, pityriasis alba, bacterial infections, and herpes simplex.41
Treatment with topical antifungals usually suffices, but cases that are not responsive or complicated by the immune status of the patient may need systemic therapy.
Tinea Cruris. Tinea cruris is a dermatophyte infection of the groin region. It is commonly seen in adolescent males. The primary causative fungal agents of tinea cruris include Epidermophyton floccosum and Trichophyton rubrum, with Trichophyton mentagrophytes, Trichophyton verrucosum, and Trichophyton interdigitale less commonly involved.42
Tinea cruris often can be cured using topical antifungal medications. Systemic medication is used in patients who have a hypersensitivity to topical treatment or who have resistant or extensive disease.
Patient education plays an important role in the eradication of the disease. Good hygiene is a must in controlling the infection. Proper drying of the area after bathing, avoidance of tight garments, and proper application of the topical medications are essential in resolving the infection.
If a concurrent superficial fungal infection is present on any other area, especially the feet, separate towels for each region should be used after bathing. Putting on socks before undergarments or using disposable gloves when cleaning the feet also can be helpful techniques to decrease the spread of infection to the groin. Antifungal powders are useful, as they have the added benefit of drying affected regions.42
Tinea Versicolor. Tinea versicolor is another dermatophyte infection of the stratum corneum in which multiple oval, scaly macules are found on the trunk, neck, face, and upper arms in children and adolescents.
Skin scrapings with potassium hydroxide examination reveal numerous hyphae and circular spores. A biopsy of the lesion will also show hyphae and spores within the stratum corneum.
The organism responsible for tinea versicolor is Malassezia furfur, which thrives in hot, humid environments. Treatment is with antifungal solutions or fluconazole shampoo. A single dose of fluconazole or itraconazole may be enough in some cases, but in tropical or subtropical regions, a full two-week course of once-daily oral ketoconazole may be needed.
Candidiasis. Candidiasis is the result of infection by pathogenic yeast, most commonly Candida albicans, in areas of the body predisposed to warmth and moisture. Its appearance is distinct depending on which area of the body it colonizes. In the oral cavity, white plaques are seen on an erythematous base, while in the diaper region, it presents as a beefy erythema with elevated margins and satellite plaques.
Candidiasis can also present on the fingertips, i.e. paronychia, and is commonly a result of thumb sucking. It can also present in the folds of the neck, axilla, and inguinal folds and is commonly seen in obese individuals in these areas. Vulvovaginal candidiasis appears as a cheesy white discharge from the vagina with white plaques on an erythematous base on the vaginal walls and occurs most commonly in adolescent females.
Candidiasis may be confused with a variety of diseases depending on the location of the infection. In the mouth, herpes simplex, burns, and epidermolysis bullosa all have similar presentations. In the groin, bacterial intertrigo, burns, and even maceration may be confused for a candidiasis infection. Vulvovaginal candidiasis may be confused with a variety of sexually transmitted diseases, including Trichomonas and gonorrhea.
Topical treatment with anti-yeast agents is usually enough to clear the infection from topical areas.
Diaper dermatitis is frequently caused by candidiasis, but a number of etiologies should be considered. Secondary bacterial infection after disruption of the skin barrier by maceration, exogenous irritants from diaper wipes or over-the-counter topical products, nonaccidental burns, and tinea inguinalis are all among potential causes of diaper dermatitis.43 Determining the correct etiology of diaper dermatitis is the most important step in treating it.
Parents should be informed of the importance of good hygiene and keeping the area dry. All potential irritants, such as commercial wipes and topical lubricants, should be stopped. Zinc oxide ointment is a proper protective agent that may also help with wound healing. If a yeast infection is diagnosed, antifungal treatment with nystatin ointment or ciclopirox cream may be helpful. A follow-up examination about a week after treatment should be conducted to ensure clearance of the infection.
Antifungal Medications. Azoles and allylamines are the two main classes of antifungal medications.
Azoles work by inhibiting the enzyme lanosterol 14a-demethylase, which reduces the formation of ergosterol, a critical component of fungal cell walls. Membrane damage leads to a fungistatic effect. Examples of azole antifungals include ketoconazole, econazole, oxiconazole, clotrimazole, and miconazole.
Allylamines inhibit the enzyme squalene epoxidase that generates ergosterol from squalene, leading to fungicidal buildup of toxic levels of squalene in the cells. Terbinafine and naftifine are allylamine treatment options, whereas butenafine is a benzylamine antifungal agent that is structurally similar to allylamines.
Ciclopirox olamine is another effective antifungal medication that is recommended for twice daily use for four weeks. It works by disrupting iron-dependent enzyme systems and intracellular membranes.42
Conclusion
In summary, the diagnosis of infectious skin lesions in children is challenging. Bacterial, viral, and fungal infections share many common presenting features, and it is important to distinguish between them so the correct treatment can be provided.
References
1. Weston L. Morelli Color Textbook of Pediatric Dermatology, 4th edition. Elsevier; 2007: 63.
2. Hansra NK, Shinkai K. Cutaneous community-acquired and hospital-acquired MRSA. Dermatologic Therapy 2011;24:263–272.
3. Cellulitis. ADAM Medical Encyclopedia. Available at: http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001858/. Accessed October 2011.
4. Paller AS, Mancini AJ. Hurwitz Clinical Pediatric Dermatology, 3rd edition, Elsevier ; 2006: 327-328.
5. Schachner LA, Hansen RC. Pediatric Dermatology, 3rd edition. Mosby; 2003: 998.
6. Heath C, Desai N, Silverberg NB. Recent microbiological shifts in perianal bacterial dermatitis: Staphylococcus aureus predominance. Pediatric Dermatology 2009;26:696–700.
7. Jongen J, et al. Perianal streptococcal dermatitis: An important differential diagnosis in pediatric patients. Dis Colon & Rectum 2008;51:584-587.
8. Scarlet fever. ADAM Medical Encyclopedia. Available at: http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001969/. Accessed October 2011.
9. Paller AS, Mancini Hurwitz AJ. Clinical Pediatric Dermatology, 3rd edition. Elsevier; 2006: 368-369.
10. Weston WL, Lane AT, Morelli JG. Color Textbook of Pediatric Dermatology, 4th edition. Mosby; 2007: 73.
11. Florin TA, Zaoutis TE, Zaoutis LB. Beyond cat scratch disease: Widening spectrum of Bartonella henselae infection. Pediatrics 2008;121;e1413.
12. Cat scratch disease. ADAM Medical Encyclopedia. Available at: http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0002581/. Accessed October 2011.
13. Marques AR. Lyme disease: A review. Curr Allergy Asthma Rep 2010;10:13-20.
14. Centers for Disease Control and Prevention. Lyme Disease. CDC web site. Available at: http://www.cdc.gov/lyme/signs_symptoms/index.html. Accessed October 2011.
15. Wormser GP, et al. IDSA Guidelines: The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: Clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis 2006;43:1089-1134.
16. Committee on Infectious Diseases. Prevention of Lyme disease. Pediatrics 2000;105:142-147.
17. Response of the Infectious Diseases Society of America Lyme Disease Review Panel to Johnson and Stricker. Clin Infect Dis 2010;51(9):1110–1111.
18. Cunningham A, Griffiths P, Leone P, et al. Current management and recommendations for access to antiviral therapy of herpes labialis. J Clin Virol 2011; Sept. 1, epub ahead of print.
19. Centers for Disease Control and Prevention. Press release: CDC study finds herpes rates remain high. March 9, 2010. CDC web site. Available at: http://www.cdc.gov/nchhstp/newsroom/hsv2pressrelease.html. Accessed October 2011.
20. Paller AS, Mancini Hurwitz AJ. Clinical Pediatric Dermatology, 3rd edition. Elsevier 2006; 399.
21. Centers for Disease Control and Prevention. Genital herpes CDC Fact Sheet. CDC web site. Available at: http://www.cdc.gov/std/herpes/stdfact-herpes.htm. Accessed October 2011.
22. Paller AS, Mancini Hurwitz AJ. Clinical Pediatric Dermatology, 3rd edition. Elsevier 2006; 400.
23. Centers for Disease Control and Prevention. Measles outbreaks. CDC web site. Available at: http://www.cdc.gov/measles/outbreaks.html. Accessed October 2011.
24. Centers for Disease Control and Prevention. Summary of notifiable diseases United States, 2009. Morbid Mortal Wkly Rep MMWR 2011;58; May 13, 2011. Available at: http://www.cdc.gov/mmwr/PDF/wk/mm5853.pdf. Accessed October 2011.
25. Weston WL, Lane AT, Morelli JG. Color Textbook of Pediatric Dermatology, 4th edition. Mosby; 2007: 116.
26. Hardie D, Yeats J. Calling the shots: Postexposure prophylaxis against virues. Main Topic 2003;21:322-330. Available at: http://www.ajol.info/index.php/cme/article/viewFile/43899/27418. Accessed October 2011.
27. Razonablea RR, Zerrb DM, and the AST. HHV-6, HHV-7 and HHV-8 in solid organ transplant recipients. Am J Transplantation 2009;9 (Suppl 4): S97–S103.
28. Yamao S, Yamaguchi K, Matsui Y, et al. Parvovirus arthritis mimicking early rheumatoid arthritis. J Allergy Clin Immunol 2011;127 Supplement:AB226.
29. Fisher RG, Boyce TE. Moffet's Pediatric Infectious Diseases: A Problem-Oriented Approach. 2004; Chapter 19; 631.
30. Seward JF, Marin M, Vázquez M. Varicella vaccine effectiveness in the US vaccination program: A review. J Infect Dis 2008;197 (Supplement 2):S82-S89.
31. Chaves SS, et al. Loss of vaccine-induced immunity to varicella over time. N Engl J Med 2007;356:1121-1129.
32. Centers for Disease Control and Prevention. About hand, foot, and mouth disease. CDC web site. Available at: http://www.cdc.gov/hand-foot-mouth/about/index.html. Accessed October 2011.
33. Centers for Disease Control and Prevention. Hand, foot, and mouth disease complications. CDC web site. Available at: http://www.cdc.gov/hand-foot-mouth/about/complications.html. Accessed. October 2011.
34. World Health Organization. Hand, foot, and mouth disease: Overview. WHO web site. Available at: http://www.wpro.who.int/health_topics/hfmd. Accessed October 2011.
35. Paller AS, Mancini AJ. Hurwitz Clinical Pediatric Dermatology, 3rd edition. Elsevier; 2006: 373.
36. Paller AS, Mancini AJ. Hurwitz Clinical Pediatric Dermatology, 3rd edition. Elsevier; 2006: 375.
37. Blyth M, Estela C, Young AE. Severe staphylococcal scalded skin syndrome in children. Burns 2008;34:98-103.
38. Patel GA, Schwartz RA. Tinea capitis: Still an unsolved problem? Mycoses 2011;54:183-188.
39. Weston WL, Lane AT, Morelli JG. Fungal and yeast infections of the skin. Color Textbook of Pediatric Dermatology, 4th edition. Mosby; 2007: 81.
40. Aste N, Atzori L, Aste N, et al. A 20-year survey of tinea faciei. Mycoses 2010;53:504–508.
41. Aste N, Atzori L, Aste N, et al. A 20-year survey of tinea faciei. Mycoses 2010;53:504–508.
42. Patel GA, Wiederkehr M, Schwartz RA. Tinea cruris in children. Cutis 2009;84:133-137.
43. Schachner LA, Hansen RC. Pediatric Dermatology. New York: Mosby; 2003: 95-96.
The skin is a dynamic organ, accounting for 15-20% of total body weight, and exhibits many functions such as protection against thermal and mechanical insults and against pathogenic microorganisms.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
