Executive Summary
The latest national statistics show that long-acting reversible contraceptives (LARCs) now follow the Pill, sterilization, and condoms as the most common methods used by U.S. women.
-
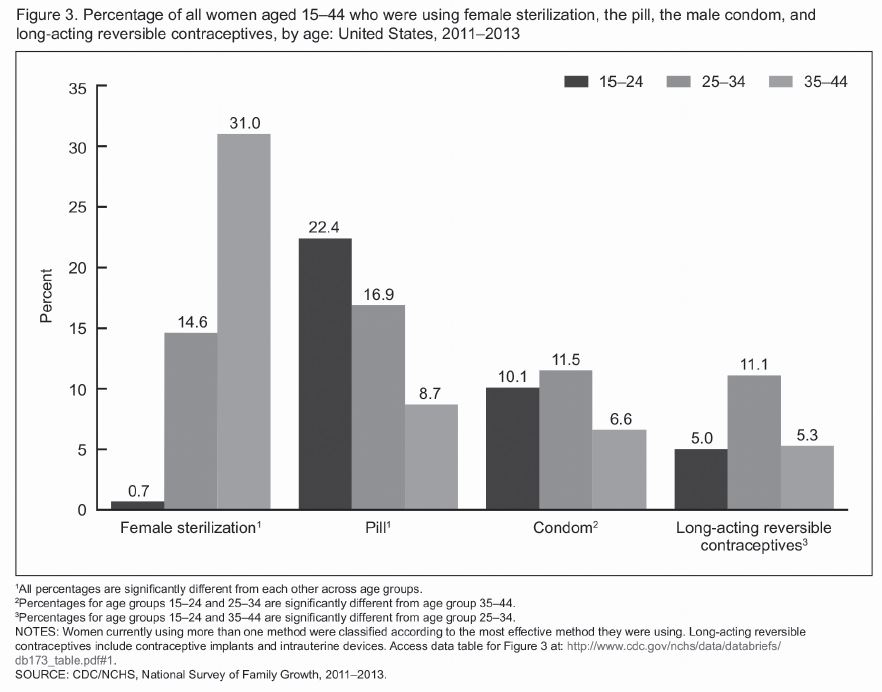
When looking at use by age, data from the current report indicate use of LARCs was higher among women ages 25-34 (11.1%) compared with women ages 15-24 (5.0%) and ages 35-44 (5.3%).
-
Use Of Oral Contraceptives Was Higher Among Younger Women, Data Reflect. Almost One Woman Out Of Four Ages 15-24 (22.4%) Was Using The Pill Compared With About One Woman In 12 Ages 35-44 (8.7%).
The latest national statistics show that long-acting reversible contraceptives (LARCs) now follow the Pill, sterilization, and condoms as the most common methods currently used by women in the United States.1 However, with 51% of pregnancies unintended in the United States,2 advocates are pushing to improve access to such effective birth control.
This new data represent good news from the Centers for Disease Control and Prevention’s National Center for Health Statistics (NCHS), says Andrew Kaunitz, MD, University of Florida Research Foundation professor and associate chairman of the Department of Obstetrics and Gynecology at the University of Florida College of Medicine — Jacksonville. More U.S. women have access to and have chosen to use highly effective reversible contraceptives, he notes.
“Building on this progress will depend, among other things, on reimbursement policies minimizing out-of-pocket cost for women considering the implant or intrauterine devices [IUDs],” states Kaunitz. “As more of our patients choose IUDs and implants, we can look forward to fewer unintended pregnancies and induced abortions.”
To prepare the current report, statisticians used data from the 2011–2013 National Survey of Family Growth on contraceptive use in the month of the interview to provide a snapshot of current contraceptive status among U.S. women ages 15-44. Their analysis indicates that in 2011-2013, 61.7% of the 60.9 million U.S. women ages 15-44 were using contraception. The most common contraceptive methods being used were the Pill (16.0%), female sterilization (15.5%), male condoms (9.4%), and LARCs (7.2%).
In the previously prepared report, which looked at use from 2006-2010, analysts did not present a subtotal for LARCs, states Kimberly Daniels, PhD, lead author of the current report. Although not shown, that percentage for LARCs was 3.8% for 2006-2010 among women ages 15-44, compared with the 7.2% shown in the new report for 2011-2013. That increase is statistically significant, she notes.
When looking at use by age, data from the current report indicates use of LARCs was higher among women ages 25-34 (11.1%) compared with women ages 15-24 (5.0%) and ages 35-44 (5.3%). (See the overview chart on p. 27.)
Data were analyzed by level of educational attainment. Current use of female sterilization declined with greater educational attainment; 27.0% of women with a high school diploma or general equivalency diploma (GED) were using female sterilization, compared with 10.3% of women with a bachelor’s degree or higher. Current pill use was more common with greater educational attainment. One in five women (21.5%) with a bachelor’s degree or higher was using the Pill. Statistics show fewer than one woman in 20 (3.6%) without a high school diploma or GED was using an oral contraceptive. Similar percentages of women across education groups were using condoms (8%–11%) or LARCs (8%–10%).1
Use of oral contraceptives was higher among younger women, data reflect. Almost one woman out of four ages 15-24 (22.4%) was using the Pill, compared with about one woman in 12 ages 35-44 (8.7%). Similar percentages of women ages 15-24 (10.1%) and 25-34 (11.5%) were using condoms; use was lower among women ages 35-44 (6.6%), researchers report.1
Statisticians also analyzed current contraceptive method use by race/ethnicity. Current use of LARCs was higher among Hispanic (8.7%) and non-Hispanic white (7.4%) women compared with non-Hispanic black women (5.0%), figures show. Current use of female sterilization was higher among non-Hispanic black women (21.3%) compared with non-Hispanic white women (14.0%).
When looking at pill use, statistics suggest current use was higher among non-Hispanic white women (19.0%) than among Hispanic (10.9%) and non-Hispanic black (9.8%) women. Current condom use was similar across the three Hispanic origin and race groups shown, which was about 9%, data indicate.
How to improve access
The American College of Obstetricians and Gynecologists is recommending 18 policies and practices that will increase availability of the full range of contraceptive methods and will remove existing and potential barriers.
According to a newly released Committee Opinion, contraception is an essential part of preventive care, and all women should have unhindered and affordable access to all contraceptives approved by the Food and Drug Administration (FDA).3
A key focus of this Committee Opinion is informing clinicians across the board about access issues to the various methods of contraception in general and informing them that all women should have access, states Wanda Kay Nicholson, MD, professor of obstetrics and gynecology at the University of North Carolina at Chapel Hill. Henderson serves as chair of the College’s Committee on Health Care for Underserved Women, which compiled the recommendations.
The new recommendations call for the following:
-
full implementation of the Affordable Care Act (ACA) requirement that new and revised private health insurance plans cover all FDA-approved contraceptives without cost sharing, including non-equivalent options from within one method category (for example, both levonorgestrel and copper intrauterine devices);
-
easily accessible alternative contraceptive coverage for women who receive health insurance through employers and plans exempted from the contraceptive coverage requirement;
-
Medicaid expansion in all states, an action critical to the ability of low-income women to obtain improved access to contraceptives;
-
the right of women to receive prescribed contraceptives or an immediate informed referral from all pharmacies;
-
inclusion of all contraceptive methods, including LARC, on all payer and hospital formularies;
-
over-the-counter access to oral contraceptives with accompanying full insurance coverage or cost supports;
-
payment and practice policies that support provision of three- to 13-month supplies of combined hormonal methods to improve contraceptive continuation.3
“We can prevent unintended pregnancy and help ensure that women have the contraceptive care necessary to have healthy families if and when they want to,” says Nicholson. “But we must remove barriers and promote access for all American women, and we must support policies that will increase and improve utilization of contraceptives.”
Robert Hatcher, MD, MPH, professor emeritus of gynecology and obstetrics at Emory University School of Medicine in Atlanta, says, “The near-to-doubling of the use of LARC methods, from 3.8% to 7.2%, in the two time periods referred to in the NCHS studies is certainly in the right direction. However the use of LARC methods by just over 75% of the 9,256 women in the St. Louis Contraceptive CHOICE Project suggests that all hoping to increase use of IUDs and implants carefully study the counseling techniques employed by the CHOICE Project.”4
Now that the ACA is covering all the contraceptive costs of an ever-increasing number of women, more and more women can receive LARC methods at no cost, says Hatcher.
-
Daniels K, Daugherty J, Jones J. Current contraceptive status among women aged 15-44: United States, 2011–2013. NCHS data brief, no 173. Hyattsville, MD: National Center for Health Statistics. 2014.
-
Finer LB, Zolna MR. Shifts in intended and unintended pregnancies in the United States, 2001-2008. Am J Public Health 2014; 104(Suppl 1):S43-48.
-
Committee opinion no. 615: Access to contraception. Obstet Gynecol 2015; 125(1):250-255.
-
Madden T, Mullersman JL, Omvig KJ, et al. Structured contraceptive counseling provided by the Contraceptive CHOICE Project. Contraception 2013; 88(2):243-249.

