Recognizing Human Trafficking Victims in the Emergency Department
March 1, 2015
Reprints
Author
Pinaki Mukherji, MD, FACEP, FAAEM, Assistant Professor of Emergency Medicine, Department of Emergency Medicine, Long Island Jewish Medical Center, New Hyde Park, NY.
Peer Reviewer
Kirsten Bechtel, MD, Section of Pediatric Emergency Medicine, Associate Professor Pediatrics, Yale School of Medicine, Co-Director, Injury Free Coalition for Kids, Yale-New Haven Children’s Hospital, New Haven, CT.
Executive Summary
- Human trafficking involves more than 20,000 victims, according to recent estimates. In addition to sexual exploitation, forced labor involving largely immigrants is most common.
- Victims are mostly female, but less than half are children. Men represent 20% of victims. Most are immigrants from Mexico or eastern Asia, in the United States illegally.
- Victims are likely to present with minor vague complaints, often with signs of physical trauma. Substance abuse, poverty, mental illness, and social isolation are common. Dental complaints are frequent. Look for tattoos of men’s names and bar codes at the nape of the neck.
- Victims younger than age 18 must be reported to Child Protective Services. Adults may receive help through the National Human Trafficking Resource Center at 1-888-373-7888.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Farel (CME question reviewer) owns stock in Johnson & Johnson. Dr. Schneider (editor) is employed by the American College of Emergency Physicians. Dr. Stapczynski (editor) owns stock in Pfizer, Johnson & Johnson, AxoGen, Walgreen Company, and Bristol Myers Squibb. Dr. Mukherji (author), Dr. Bechtel (peer reviewer), Mr. Landenberger (editorial director), and Ms. Mark (executive editor) report no financial relationships with companies related to the field of study covered by this CME activity.
This is a subject that has been discussed a lot in the news, and I must admit I was skeptical when we first discussed the topic. I was unsure how this related to our specialty. It seemed like a crime isolated to large urban areas and immigrants. But just this month, a ring of human traffickers were arrested in my old hometown of Rochester, New York! Human traffickers operate in large and small cities and rural areas.
Emergency physicians are all too familiar with the important public service role we play in identifying child abuse, domestic violence, and elder abuse. Identifying potential cases of human trafficking, therefore, is a natural extension of our role. Identifying these victims and mobilizing resources for the victim is an important part of our practice.
You may have seen a case of human trafficking and not recognized it. This article not only describes the crime, but also provides resources for you and the victims. In addition, it is hoped that the article will heighten awareness so you will watch for potential victims and provide them with help.
— Sandra Schneider, MD, Editor
Human trafficking affects up to 100 million people worldwide. Emergency physicians are uniquely positioned to encounter and identify this vulnerable group with increased awareness and attention to red flags.
Case 1. An 18-year-old Hispanic female presents to the emergency department (ED) with a two-day history of pelvic pain and vaginal bleeding. Her much older boyfriend accompanies her. The patient speaks some English, but looks to her boyfriend when asked questions. The man often answers for her, interjecting and addressing the provider directly. He states that her period began three days ago but that she has been complaining of cramping and heavier bleeding. The patient is seen in her street clothes and has several visible tattoos. The provider notes that the patient has normal vital signs, no focal abdominal tenderness, and a small amount of bleeding on bimanual exam. The boyfriend insists on being present during the bimanual exam, holding the patient’s hand. A urine pregnancy point of care test is performed, which is negative. Ibuprofen and outpatient follow-up are recommended for likely heavy menses.
Case 2. A 48-year-old Asian male presents to the ED with a painful reddened blister to his left forearm. The manager from the restaurant where the patient is employed accompanies him. The patient does not speak any English, and his manager explains that the patient burned his arm on a hot dishwasher. A history is obtained from the patient using the manager as translator, and the patient appears to answer questions in short, often one-word answers. The patient is registered at the bedside, and the manager provides the information, produces identification, and pays his copay. The patient remains fully clothed, but an old bruise and a small round healing burn are visible on his right forearm as well. A physician assistant working in the fast track area of the ED orders a tetanus booster, notes a linear parallel burn pattern with bullae, and dresses his second-degree burn with antibiotic ointment and sterile gauze. He is discharged, and the manager is given instructions to return for signs of infection.
Introduction
Human trafficking is a global problem encompassing the realms of human rights, international law, federal statutes, organized crime, public health, and medicine. The most broadly accepted definition found in the United Nations Convention Against Transnational Crime1 focuses not just on transportation or harboring of victims, but on exploitation, which might include sexual exploitation, forced labor or servitude, or even (more common globally) human organ provision or recruitment of child soldiers. The number of victims appears to be immense, although there are issues with data gathering and reporting, which may underestimate the true scope of the problem.2 Globally, up to 900,000 people are transported across borders yearly for purposes of exploitation and slavery, with nearly 45,000 victims identified in 2013.3 The market for profiting from trading in humans explains the increasing estimates even during the past 15 years. Human trafficking was thought by the International Labor Organization to be a $32 billion industry in 2010 and is now estimated to have grown to $150 billion.5 While the illegal drug trade remains far and away the largest market, human trafficking is the second largest criminal industry in the world, surpassing the trading of illegal firearms and weapons.
The U.S. State Department estimates up to 20,000 persons are trafficked into the United States yearly, with most of them related to sexual exploitation. While many of these trafficked humans arrive via major international hubs such as Los Angeles, New York City, and Miami, there is evidence that these persons are also transported widely within borders of the United States, with victims identified in cities across all 50 states.6
While there is a great deal of attention given to international trafficking, significant domestic trafficking occurs, especially to vulnerable undomiciled children, runaways, or those in welfare or foster care.7 With the increasing growth of the trafficking trade, there is increased need for medical provider education in identifying and assisting victims.
Healthcare providers are a key element in the identification of human trafficking victims. These individuals commonly enter the health care system during periods of transportation, detainment, or exploitation. Interviews of trafficking survivors estimated that up to 50% had encountered a health care professional for acute complaints.8 Emergency physicians already function as front-line providers for the disenfranchised and vulnerable who may lack access to appropriate medical care. They are accustomed to encountering victims of partner violence, are tasked with screening for child and elder abuse, and are ideally positioned to care for and provide resources to victims of human trafficking. Yet, healthcare workers are rarely engaged or trained to recognize these patients, despite their potential opportunity to intervene. This review will summarize the scope of the problem, some typical patterns of health care utilization, the challenge of recognizing this entity in the ED setting, red flags in presentation that may prompt investigation, and strategies and resources to assist these patients.
Epidemiology
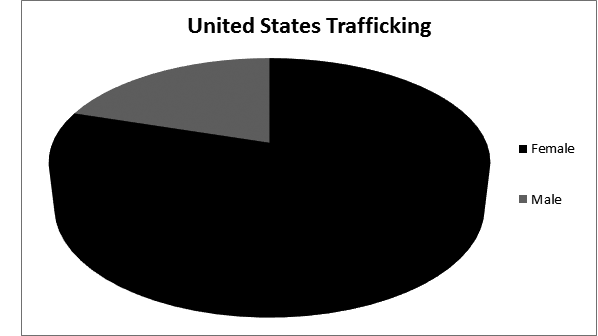
The two major categories of human trafficking are sexual exploitation and forced labor. Of all trafficked victims worldwide, about 78% are in forced labor and 22% are victims of sexual exploitation.9 Within the United States, however, approximately 75% of human trafficking victims are from sexual exploitation and 25% are from forced labor and servitude. While children are an at risk group, they represent just 26% of all victims globally, and within the United States nearly 40% of the total.3 A typical U.S. trafficking victim is much more likely to be female than male, but men still represent one out of every five patients seen, and children represent a minority within the group. This is in contrast to popular perceptions regarding trafficking and the stereotype that most victims are young female children. Research shows that male victims are also less commonly recognized, and more often criminalized or deported than female victims. This may lead to underreporting and the possibility that men represent a significantly larger proportion than the estimated 20% of trafficked humans.10
About 33% of human trafficking victims are English-speaking.11 Many people who are trafficked internationally may be transported within regional areas or continents.12 The majority of internationally trafficked victims who have been brought to the United States are from Mexico and countries in eastern Asia; the remainder are from Central America, southern Asia, Africa, and Europe.3 Victims are sometimes abducted, but can be lured with employment opportunities, study abroad programs, or promises of marriage. In some cases, smugglers who specialize in transporting people are enlisted voluntarily, but then the monies demanded suddenly balloon and victims are pushed into servitude to repay their “debts.” Poverty stricken families can even sell a child or intimate partner to a trafficker. Common risk factors identifying vulnerable populaces include poverty, substance use, mental illness, exposure to violence, social isolation, immigrant status (especially undocumented), and those who are migrants, refugees, and low-wage laborers. (See Figures 1 and 2.)
Figure 1. Global Trafficking Victims
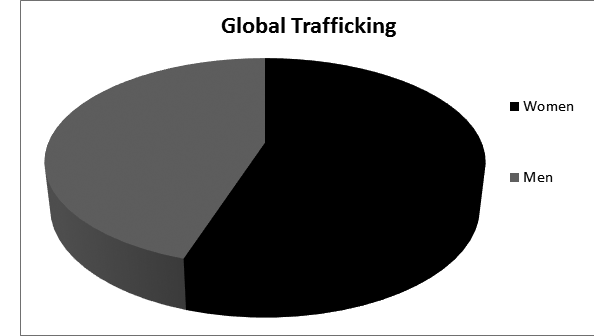
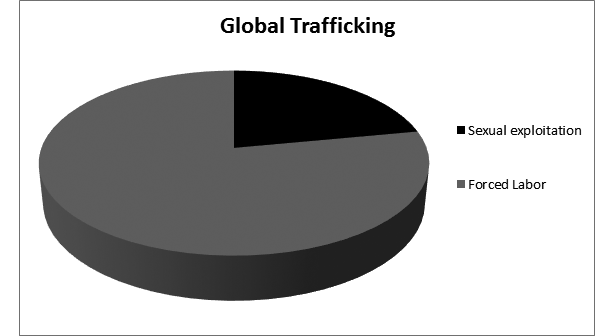
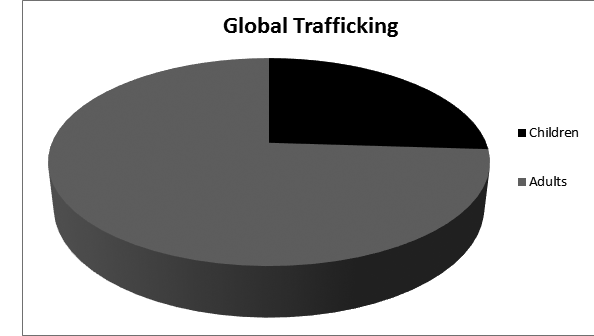
Figure 2. U.S. Trafficking Victims
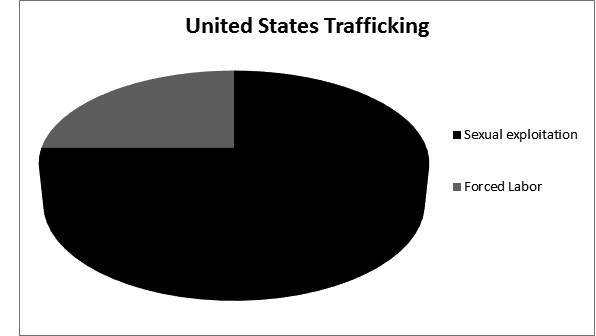
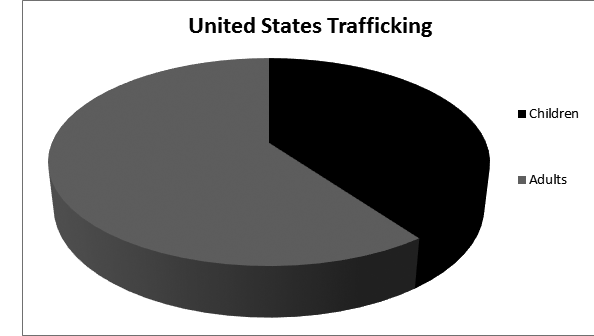
Presenting Complaints
Acute medical complaints seen in these patients are varied and multifactorial. Lack of nutrition, sleep deprivation, physical violence and injury, and mental health complaints due to extreme stresses are commonly seen. As with many of our disadvantaged members of society, they may also present with chronic diseases at advanced stages as they are systematically denied access to medical care by traffickers. While many of these patients can present with vague, minor, and nonspecific complaints, there are common secondary complaints of which emergency medicine practitioners should be aware.
Table 1. Common Presenting Complaints to the Emergency Department
- Back pain
- Headaches
- Fractures
- Contusions
- Burns
- Dental complaints
- Vaginal bleeding
- Pelvic pain
- Sexually transmitted infections
- Unwanted pregnancy
- Anxiety
- Depression
- Suicidal ideation
- Somatization
- Substance use
- HIV
- Hepatitis
Trauma/Musculoskeletal Pain
A very high number of trafficking survivors report physical injuries (57%), injuries caused by weapons or instruments (40%), and nearly all report either sexual assault or physical violence (95%).13 Repeated physical abuse and torture resulting in fractures, contusions, and burns are common. Injuries around the head, mouth, or genital area, as well as wounds that appeared self-inflicted are warning signs. Wounds or burns caused by tools of myriad kinds leaving a pattern, injuries of varying ages, and on separate areas of the body are red flags, just as in evaluating possible abuse or domestic violence cases. In addition to acute injuries, more vague chronic complaints are common, with headaches and back pain reported at 82% and 68%, respectively.14 These chronic chief complaints commonly coexist with psychiatric secondary complaints.
Gynecologic
Gynecologic complaints, including genital pain, vaginal bleeding, and complications of pregnancy, are common among victims of sex trafficking. Sexually transmitted infections (STIs) are also common, presenting as vaginal discharge (70%) and pelvic pain (59%).13 HIV, in particular, has been linked to trafficking victims, both globally and domestically.15 One review reported HIV prevalence as ranging between 22.7% and 45.8% globally among victims of sex trafficking.16 Pregnancy is a major risk for sex trafficking victims, and multiple elective abortions are common. Repeated visits to providers, previous treatment of STIs, pelvic inflammatory disease, and signs of trauma to the genitourinary area from sexual assault are all potential warning signs of sexual exploitation. Retained foreign bodies may cause rectal or vaginal injury, and sponges and absorptive materials are sometimes used to allow menstruating women to continue to “work.”17 As up to 80% of victims of sex trafficking in this country are women and girls, the American College of Obstetricians and Gynecologists put forth a committee opinion to encourage awareness of this problem among practitioners.18
Psychologic
Human trafficking victims are subjected to a wide range of coercive tactics that reinforce the traffickers’ ability to control and exploit them. They are often deprived of sleep and food, which weakens their ability to resist demands and creates rewards for compliance. They are isolated from human interaction as much as possible, both physically with confinement, and mentally, keeping them from making social connections, and using language barriers to keep them dependent on the trafficker. Close monitoring of behavior, enforcement of trivial demands, and degradation make the victim feel watched at all times and fearful of reprisal for even minor transgressions. These stressors directly put victims at risk for serious mental health problems.19
Poor mental health is widely reported among all trafficking victims. Anxiety disorder, depression, suicidal ideation, and posttraumatic stress disorder (PTSD) have all been described in these patients. Symptoms of hostility, paranoia, and hopelessness are common. One European study found 57% of victims of human trafficking had symptoms diagnostic for PTSD.13 Mental illness may be caused by the circumstances of trafficking, but may also be a risk factor. A study describing U.S. victims found that 30% of victims had a pre-existing diagnosis of major depression.20 These may be the presenting symptoms to an emergency department setting and may also be offered as secondary after a somatic complaint of headache, back pain, dizziness, and generalized weakness.
Substance Use
Substance use and addiction make victims vulnerable to traffickers, and can be negative coping strategies during a stressful experience. Forced or coerced use of drugs and alcohol can also be used to isolate a victim and integrate them into their exploitation. An addicted individual becomes easier to control and may further avoid seeking law enforcement for fear of prosecution of illegal drug use. Substance use can also increase rates of self-harm and mental illness, and increases exposure to needle-related infectious disease (HIV, hepatitis) and participation in high-risk sexual activities. Patients may present to the ED with overdose, intoxication, or withdrawal symptoms. Presence of substance abuse also correlated highly with the presence of mental illness in younger victims of human trafficking, with estimates of 75-90% of substance users having comorbid psychiatric diagnoses.21
Dental
Dental professionals are another front-line group of providers who are likely to encounter trafficking victims with acute complaints. Victims may present with dental trauma and loss of teeth from violent acts. Injuries to the face and mouth area are common in abuse cases, and the potential for tooth involvement is high. More insidious problems arise as well, including caries from poor nutrition and lack of primary care, infectious complications due to HIV, and even oral cancers or gingival disease due to substance use. Like emergency physicians, dental clinics likely come unwittingly into contact with this group and have the opportunity to identify these victims.8 In 2012 the first U.S. dentist attempted to raise awareness of trafficking victims in dental care settings,22 and since then others have called for an increased awareness of potential victims of human trafficking by oral health care providers.23
Skin
Bruises and contusions in potential victims of human trafficking should not be dismissed as minor injuries. Bruising in areas that are unusual for accidental injury include the cheek, neck, trunk, and buttocks.24 Any repeated symmetrical injuries (some of which represent bite marks), patterns that may have been made with tools, including belts, cords, shoes, or kitchen utensils, and linear or circular burns are cause to investigate abusive injury.25 Multiple ecchymoses of varying ages, scarring, and signs of poorly cared for previous wounds should raise the concern for repeated inflicted injury.
Tattoos are of particular interest, as they have been reported in human trafficking to be used to designate property as humans are traded and sold. Tattoos of names, especially when not the victim’s name, or multiple names can indicate ownership. Some tattoos are numbers or barcodes, meant to be identifying marks or prices, and are sometimes hidden by hair at the nape of the neck. These markings have been adopted by many and stylized such that their presence is certainly not specific for trafficking activity and may be applied for purely decorative purposes. Tattoos should be explored with patients, and signs of other signs of human trafficking noted.
Case Resolutions
Case 1. The patient seen for heavy bleeding during menses returns to the ED with the older man, who then leaves after the patient is registered. She is febrile, in severe pain, and is bleeding heavily. She gives a history to the provider using a translator and gives her own information on this visit. She gives a different date of birth than on her previous visit record and is found to be 15 years old rather than 18. She states that the older man would accompany her to different locations where she would have sex with others while he collected money. She is unsure of the location where she slept, but indicates that she has been there for approximately four months. She states that she was thought to be pregnant and that someone attempted to perform an abortion on her, after which she was brought to the ED for her first visit.
The patient is changed into a gown and examined. She is found to have a tender lower abdomen, a blood saturated makeup sponge with clots in the vaginal vault, severe pain to bimanual exam, and heterogeneous material seen on ultrasound in the uterus. It is noted during her physical exam that she has multiple tattoos, including a tattoo on her breast with a man’s name; it is not the name of the man who accompanied her. She is also found to have multiple bruises to her neck, back, and abdomen of varying sizes and colors. She is admitted to the gynecology service, administered IV antibiotics for presumed sepsis following an attempted abortion by her captors, and for possible dilatation and curettage (D+C).
This patient’s previous visit history is reviewed and the previous provider interviewed. While the medical care described in the chart seems reasonable to reviewers, in retrospect, the fact that the “boyfriend” appeared to be much older than the patient may have been the earliest red flag. His actions in not allowing the patient to speak, answering questions for her, and never leaving her side were all concerning for controlling behavior. The breast tattoo and multiple bruises would have raised concerns if the patient was fully undressed. The history taken from the patient on this second visit paints a very different picture.
The provider gains the patient’s trust and offers to notify the National Human Trafficking Resource Center (NHTRC) to find local resources and ensure a safe shelter. Because the patient is younger than 18 years of age, the clinician is mandated to make a report to child protective services.26 While this call and others to law enforcement or federal agencies may be made anonymously from either the provider or the patient, it is advisable for the provider to obtain the patient’s permission, as the victim cannot be forced to report criminal activity, and the patient or their family may be at risk of reprisal if they do so.27 As a physician, the safety of the patient and their loved ones must be a moral obligation and professional priority.
Case 2. A 48-year-old Asian man returns to the ED where he was seen one week prior. He is alone and a history is obtained via translator phone. The patient states that he was being held in a basement but was able to escape and returned to the ED, as this was the only place he had been able to locate. He informs providers that he answered an advertisement for restaurant employment, but was offered a job in a distant city and told that he would have to depart on a bus immediately if he wanted the position. Upon being offered a salary and living quarters, he agreed to go, intending to send money back to his family and eventually bring them to live in the new locale. After a long ride, he was taken to a restaurant, told to put his possessions in a locker and begin work. His belongings were removed from the locker, including his identification and cash, and he was told that he would have to pay a “job-finding fee” and that the cost of his transportation, food, and lodging would also be deducted from his pay. After two months, the patient had received no payment, and had been beaten or burned with cigarettes if he refused to work. Upon visiting the ED the week prior, the medical bill was added to his debt. Seeing no end to his servitude and feeling that his health was failing, he decided to risk harm to his person and attempt to escape. He gives his name and date of birth, but can produce no identification. He states that he has been living in the United States. for four years but admits to having entered the country illegally.
The patient is changed into a gown and examined, and in addition to a healing second-degree burn that was his chief complaint on a previous visit, he is found to have multiple cigarette burns on his upper arms and abdomen. There are also several large bruises to his legs and buttocks, which have a similar size and well circumscribed, linear edges. These injuries are recorded in the medical record and photographed with the patient’s permission. These skin findings could aid further investigations or legal prosecution.28 Blood is drawn and laboratory values are notable for potassium of 2.8, albumin of 2.5, and glucose of 282. The patient states that he is given only one meal per day and ran out of his prescription medications. He is given intravenous fluid, his potassium is corrected, and he resumes his chronic diabetes medication.
When the ED provider offers to report the situation to authorities, the patient refuses, saying he wishes to speak to a social worker or try to get transportation back to his home. Reticence in reporting crimes of this nature are quite common when a victim is undocumented, as deportation is a great concern. Since this is an adult patient, the clinician is not mandated to make any official report without the patient’s consent.26 After discussing the matter with the patient, he is referred to a social worker but also given the number for a referral line to the NHTRC. The patient is given access to a translator phone and a safe private space in the ED where he is able to anonymously call the line to ask pertinent questions regarding his situation. He is offered a certification process that may be able to provide him with documentation to stay in the United States legally and also access to federal and state services including health care, translation, and legal representation. He provides details of his situation that may lead to prosecution of this trafficking case and potentially assist other victims. The patient agrees to apply for certification, which may provide him access to a trafficking, or “T” visa. It is important for the provider to be aware that an undocumented immigrant in this situation cannot be guaranteed that a visa will be provided, or that he or she will not be deported.29
Discussion
These cases are two of the more common types of human trafficking. When they first presented to the ED, their complaints were assumed to be minor, and the signs of trafficking were overlooked. In each case, the medical care was appropriate to the facts of the case obtained. But each case had red flags for human trafficking that were missed which may have prompted earlier investigation and management.
Language barriers existed that prevented a full history from being taken. Emergency staff translators or translator phones were not used. Even when these patients are able to speak to providers, they have often been coached and given fabricated histories to provide to medical providers by their traffickers.17 Inconsistent histories between the patient and those accompanying them, or evolving histories given by the patient, may give a provider a reason to ask further questions. Under federal and state laws, patients with limited English proficiency have a right to language assistance in accessing health care services. Not every facility will have access to a translator or translator phone and, thus, any bilingual person accompanying the patient may be used for expediency. This is a potentially dangerous practice that can put the history in question even when issues such as trafficking are not a concern, and there is some evidence that it leads to increased medical errors.30
Patients accompanied by a partner who is significantly older (greater than 10 years has been suggested) may be misrepresenting the relationship. When those claiming to be partners, family members, or boyfriends appear dismissive of the patient, discourage them from speaking for themselves, or are unwilling to leave the patient alone, the provider should attempt to separate them and take a history privately. Both the patient’s and the partner’s body language and affect may convey concern for controlling behavior and a potential abusive or trafficking situation.
In cases where any concerns are raised regarding a potential trafficking situation, the provider is likely to encounter resistance from the patient even when a private interview is performed in the patient’s primary language. It is incumbent upon the provider to establish a rapport and overcome barriers to trust. Some trafficking victims have encountered law enforcement or other officials to their detriment prior to their accessing health care. Authority figures in general are likely to be mistrusted, especially when documentation status is a concern. When attempting to take a history from such patients, it is recommended that the provider ask screening questions about the situation directly and non-judgmentally. (See Table 2.)
Table 2. Questions to Ask to Help Identify a Trafficking Victim
- What type of work do you do?
- Are you free to come and go?
- What is it like where you work?
- Are you paid for your work?
- Where do you sleep and eat?
- Are there locks on doors and windows so you cannot go out?
- Where are your friends or family?
- Have you or your family been threatened? Hurt?
- Has you identification or documentation been taken from you?
Patients who are not in possession of their own passport or identification documents should prompt concern. Patients who cannot provide their own address or place of residence but defer to a companion may have had this information deliberately hidden from them to reduce the likelihood of escape or reporting to authorities. Often, the primary provider is not the staff member who is requesting this information, so an alarm may not be raised. It may be wise to educate your registration staff to identify and report this type of behavior.
Physical exam findings were present in each case that raised concern for violence and abuse. Because each patient had very focused treatment, was not undressed completely, and was not questioned about other injuries or complaints, these findings were not documented until the second visit. Contusions, burns, or wounds on the extremities may be the result of accidental injuries, but their presence may prompt questioning and a more extensive exam. The presence of injuries to the head, mouth, neck, trunk, buttocks, or genital area would be less likely to be accidental. Both patients had symmetrical or repeated patterns of injury that are much more likely to be concerning for abuse and documentation of these is important for a forensic medical record. The documentation of tattoos possibly representing ownership would have been noted with a full exam.
Resources
The Victims of Trafficking and Violence Protection Act of 2000 (TVPA) was the first in a series of legislative acts enacted in 2003, 2005, and 2008 that increased the available tools to combat trafficking globally and domestically.31 The TVPA classified trafficking as a federal crime, established tracking tools such as the Trafficking in Persons Report (TIPS) and a federal task force to coordinate anti-trafficking efforts, and created protections for victims to avoid being criminalized. While these acts have provided invaluable resources, victims, law enforcement officials, and health care providers are not aware of their existence. There exists a large gap between the existence of these tools and their utilization.
After screening for and identifying trafficking victims, the clinician is better able to assist the patient. Different trafficking victims are likely to require very different resources, and may even refuse assistance. If the victim is younger than 18 of age, mandatory reporting is required to Child Protective Services, and law enforcement officials may be involved as well. For adult victims, in most cases, the patient must agree to a referral. They may refuse, fearing for their safety, or not wish to leave their situation, believing they have no better alternatives. Involving a social worker or justice advocate may be an appropriate intervention. Like domestic violence cases, pushing the patient to escape may not be welcomed and may not even be safe.32 If the patient is amenable, giving a referral number for the NHTRC or other local groups is encouraged. Offering this referral or a local hotline is helpful even if the victim does not utilize it immediately, as these patients may interact with the health care system again and receive a repeated message of potential aid. A number of telephone and online resources exist for both providers and patients. The NHTRC is likely the broadest phone referral for patients, and the Rescue and Restore Campaign from the Department of Health and Human Services, the most encompassing resource for front-line providers. (See Table 3.)
Table 3. Resources/Referrals
-
For patients: National Human Trafficking Resource Center:
1-888-373-7888 - Department of Justice Human Trafficking Office: 1-888-428-7581
-
National Center for Missing and Exploited Children’s hotline:
1-800-843-5678 (1-800-THE-LOST) - For providers: U.S. Department of Health and Human Services, Campaign to Rescue and Restore Victims of Human Trafficking: http://www.acf.hhs.gov/programs/orr/resource/rescue-restore-campaign-tool-kits
General information
- U.S. Department of State, Office to Monitor and Combat Trafficking in Persons: http://www.state.gov/g/tip
-
U.S. Department of Justice, Office of Justice Programs:
http://ovc.ncjrs.gov/humantrafficking/ - Federal Bureau of Investigation, Investigative Programs, Crimes Against Children: http://www.fbi.gov/hq/cid/cac/crimesmain.htm
-
National Center for Missing and Exploited Children:
http://ncmec.org - United Nations Office on Drugs and Crime: http://www.unodc.org/unodc/en/human-trafficking/what-is-human-trafficking.html
Summary
Human trafficking is a rapidly growing global health and human rights problem. Trafficking can involve men, women, and children in just about every country in the world. It exists within U.S. borders and has been identified in all 50 states. Women and girls are at risk groups within the United States. While sex trafficking is more common domestically and healthcare providers are more aware of sexual exploitation, it is forced labor that is globally predominant. Even in the United States, the extent of forced labor trafficking may be more widespread than estimated and may be identified in restaurants, factories, hotels, housekeeping, cleaning services, construction, food processing, and virtually any low-wage labor force. Since the passage of the TVPA in 2000, there is increased legal protection for these victims, but a gap still exists in identifying and assisting them. Because there is no easy method to identify victims, there is a need for enhanced training for front-line professionals who may come into contact with these patients.33 A recent paper called for integrating this training into graduate medical education.34 Professionals in public health, social services, and nursing have now been joined by multiple medical organizations including the American College of Obstetricians and Gynecologists, the Christian Medical & Dental Associations, the American Academy of Pediatrics, and the American Medical Association?Medical Student Section in a call to action.35,36 Emergency medicine is ideally suited to leading this call. Just as recognizing and assisting victims of domestic violence has become an aspect of emergency assessment, so too should emergency providers learn how to identify and aid trafficking cases. Health care providers are afforded access to patients who are otherwise systematically isolated and prevented from having contact with authority figures. Being aware of the existence of these cases will improve sensitivity to screening. Being able to connect victims to the resources that are available at federal levels can be lifesaving. Emergency providers are trained to save lives and have the opportunity to intervene and truly impact the safety and medical care of this vulnerable population.
References
- 1.United Nations. (2004) United Nations Conventions against Transnational Crime and the Protocols Thereto. (United Nations Office on Drugs and Crime). New York, NY.
- 2.Loff B, Sanghera J. Distortions and difficulties in data for trafficking. Lancet 2004;363:566.
- 3.US State Department. Trafficking In Persons Report (TIPS) 2014. Available from: http://www.state.gov/j/tip/rls/tiprpt/2014/index.htm.
- 4.King G. Woman, Child For Sale: The New Slave Trade in the 21st Century. New York: Penguin Group; 2004.
- 5.International Labor Organization 2015. http://www.ilo.org/global/topics/forced-labour/lang--en/index.htm. Accessed 2/10/2015.
- 6.Coalition to Abolish Slavery and Trafficking. http://www.castla.org/key-stats. Accessed 2/4/2015.
- 7.Fong R, Cardoso J. Child human trafficking victims: Challenges for the child welfare system. Eval Program Plann 2010;33:311-316.
- 8.Baldwin S, Eisenman D, et al. Identification of human trafficking victims in health care settings. Health Hum Rights 2011;13:E36-E49.
- 9.International Labour Organization (ILO). ILO global estimate of forced labour 2012: Results and methodology. Geneva: ILO; 2012. Available at: http://www.ilo.org/washington/WCMS_182004/lang--en/index.htm.
- 10.Rosenberg R. Trafficking of adult men in the Europe and Eurasia region: Final report. Washington (DC): Creative Associates International; 2010. Available from http://pdf.usaid.gov/pdf_docs/Pnadw368.pdf.
- 11.U.S. Department of Justice. Characteristics of Suspected Human Trafficking Incidents, 2008-2010. April 2011 Available at: http://www.bjs.gov/content/pub/pdf/cshti0810.pdf.
- 12.Zimmerman C, Kiss L, Houssain M, et al. Trafficking in persons: A health concern? Cien Saude Colet 2009;14(4):1029-1035.
- 13.CdeBaca L, Sigmon J. Combating trafficking in persons: A call to action for global health professionals. Glob Health Sci Pract 2014;2:261-267.
- 14.Zimmerman C, Hossain M, Yun K, et al. The health of trafficked women: A survey of women entering posttrafficking services in Europe. Am J Public Health 2008;98(1):55-59.
- 15.United Nations Development Programme (2006-2007). Migration gone wrong: Linkages between trafficking and HIV. Accessible at: http://www.childtrafficking.com/Docs/undp_07_mig_wro_0108.pdf.
- 16.Oram S, StÖckl H, Busza J, et al. Prevalence and risk of violence and the physical, mental and sexual health problems associated with human trafficking: A systematic review. PLoS Med 2012;9(5): e1001224.
- 17.Munoz J. Red flags: Identifying sex trafficking victims in the ED. Emergency Physicians Monthly. Nov. 18, 2012. Accessed 1/15/15 at http://www.epmonthly.com/features/red-flags-identifying-sex-trafficking-victims-in-the-ed-/.
- 18.[No authors listed.] Committee opinion no. 507: Human trafficking. Obstet Gynecol 2011;118:767-770.
- 19.Baldwin S, Fehrenbacher AE, Eisenman DP. Psychological coercion in human trafficking: An application of Biderman’s Framework. Qual Health Res 2014; November 4 [Epub ahead of print].
- 20.Well M, Mitchell KJ, Ji K. Exploring the role of the internet in juvenile prostitution cases coming to the attention of law enforcement. J Child Sex Abus 2012;21:327-342.
- 21.Grella CE, Hser YI, Joshi V, et al. Drug treatment outcomes for adolescents with comorbid mental and substance use disorders. J Nerv Ment Dis 2001;189(6):384-392.
- 22.O’Callaghan MG. Human trafficking and the dental professional. J Am Dent Assoc 2012;143(5):498-504.
- 23.Nuzzolese E. Human trafficking: Role of oral health care providers. J Forensic Odontostomatol 2014;32(1):1-8.
- 24.Harris T. Bruises in children: Normal or child abuse? J Ped Health Care 2010;24(4):216-221.
- 25.Maguire S, Mann MK, Sibert J, et al. Are there patterns of bruising in childhood which are diagnostic or suggestive of abuse? A systematic review. Arch Dis Child 2005;90(2):182-186.
-
26.Becker H, Bechtel K. Recognizing victims of human trafficking in the pediatric emergency department. Pediatr Emerg Care 2015;(31)2:
144-147. - 27.Dovydaitis T. Human trafficking: The role of the health care provider. J Midwifery Womens Health 2010;55(5):462-467.
- 28.Alempijevic D, Jecmenica D, Pavlekic S, et al. Forensic medical examination of victims of trafficking in human beings. Torture 2007;17(2):117-121.
- 29.U.S. Department of Health and Human Services. Administration for Children and Families. Office of Refugee Resettlement. National Human Trafficking Resource Center. The campaign to rescue and restore victims of human trafficking. Fact Sheet: Certification for adult victims of trafficking. Available from: www.acf.hhs.gov/trafficking/about/cert_victims.html.
- 30.Flores G, Abreu M, Barone CP, et al. Errors of medical interpretation and their potential clinical consequences: A comparison of professional versus ad hoc versus no interpreters. Ann Emerg Med 2012;60(5):545-553.
- 31.U.S. Department of State. U.S. Laws on Trafficking in Persons. Available at: http://www.state.gov/j/tip/laws/.
- 32.Rhodes KV, Frankel RM, Levinthal N, et al. “You’re not a victim of domestic violence are you?” Provider patient communication about domestic violence. Ann Intern Med 2007;147(9):620-627.
- 33.Isaac R, Solak J, Giardino AP. Health care providers’ training needs related to human trafficking: Maximizing the opportunity to effectively screen and intervene. J Applied Research on Children 2011;2(1): article 8.
- 34.Grace AM, Ahn R, Macias Konstantopoulos W. Integrating curricula on human trafficking into medical education and residency training. JAMA Pediatr 2014;168(9):793-794.
- 35.Sabella D. The role of the nurse in combating human trafficking. Am J Nurs 2011;111(2):28-37.
- 36.Macy R, Graham LM. Identifying domestic and international sex-trafficking victims during human service provision. Trauma Violence Abuse 2012;13:59-76.
You may have seen a case of human trafficking and not recognized it. Emergency physicians can play a role in identifying victims and mobilizing resources for them.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
