EXECUTIVE SUMMARY
Results of a public health intervention promoting the use of free expedited partner therapy (EPT) indicate it substantially increased use of the medicine and might have cut rates of chlamydia and gonorrhea infection.
• Researchers randomly assigned 23 of 25 local health jurisdictions in Washington state to one of four study groups, rolled out the program sequentially at 6-8 month intervals, and compared outcomes between groups and within groups before and after the intervention.
• Twenty-eight states and the District of Columbia allow healthcare practitioners to provide at least some sexually transmitted infection (STI) treatment for the partner of a patient diagnosed with an STI without first examining the partner. Six states allow treatment for all or most STIs, while 22 states and the District of Columbia permit treatment for specific STIs.
Results of a Washington state public health intervention promoting the use of free expedited partner therapy (EPT) indicate it substantially increased use of the medicine and might have cut rates of chlamydia and gonorrhea infection.1
Researchers randomly assigned 23 of 25 local health jurisdictions in Washington to one of four study groups, rolled out the program sequentially at 6-8 month intervals, and compared outcomes between groups and within groups before and after the intervention. Heterosexual individuals with gonorrhea or chlamydial infection were eligible. The study made free patient-delivered partner therapy available to clinicians and provided public health partner services based on clinician referral. The main study outcomes were chlamydia test positivity among women ages 14-25 in 219 sentinel clinics and incidence of reported gonorrhea in women, both measured at the community level.1
Study results indicate that the percentage of persons receiving EPT from clinicians increased from 18% to 34% (p less than 0.001) and the percentage receiving partner services rose from 25% to 45% (p less than 0.001). Chlamydia test positivity and gonorrhea incidence in women decreased over the study period, from 8.2% to 6.5% and from 59.6 to 26.4 per 100,000, respectively. After adjusting for temporal trends, scientists state the intervention was associated with an approximately 10% reduction in chlamydia positivity and gonorrhea incidence, though the confidence bounds on these outcomes both crossed 1 chlamydia positivity prevalence ratio = 0.89, 95% confidence interval [CI] 0.77-1.04, p = 0.15; gonorrhea incidence rate ratio = 0.91, 95% CI 0.71-1.16, p = 0.45).1
“Given existing evidence and guidelines in support of EPT, we believe that continued and expanded use of the intervention is warranted, and that the design of our program can be a model for health departments seeking to increase EPT use,” the researchers state.
EPT for sexually transmitted infections (STIs) has been in existence for some time. In 2006, the Centers for Disease Control and Prevention (CDC) recommended that healthcare providers who treat patients for chlamydia and gonorrhea also provide treatment for the patient’s partner, even if he or she has not been seen by the provider. However, it has taken time for state laws and regulations to be amended to permit such action.
According to a February 2015 review from the Guttmacher Institute, most state policies follow the CDC guidelines and recommend this course of treatment for gonorrhea and chlamydia infections. In other cases, states allow EPT for the treatment of all STIs or only for specific infections, such as gonorrhea, chlamydia or trichomoniasis. Several of these states encourage or require the healthcare practitioner to provide information about STIs to the patient to give to their partner, the review notes.2
Where do states stand when it comes to EPT? According to the Guttmacher Institute review, 28 states and the District of Columbia allow healthcare practitioners to provide at least some STI treatment for the partner of a patient diagnosed with an STI without first examining the partner. Six states allow treatment for all or most STIs, while 22 states and the District of Columbia permit treatment for specific STIs.2 (To see where states stand, see graphic.)
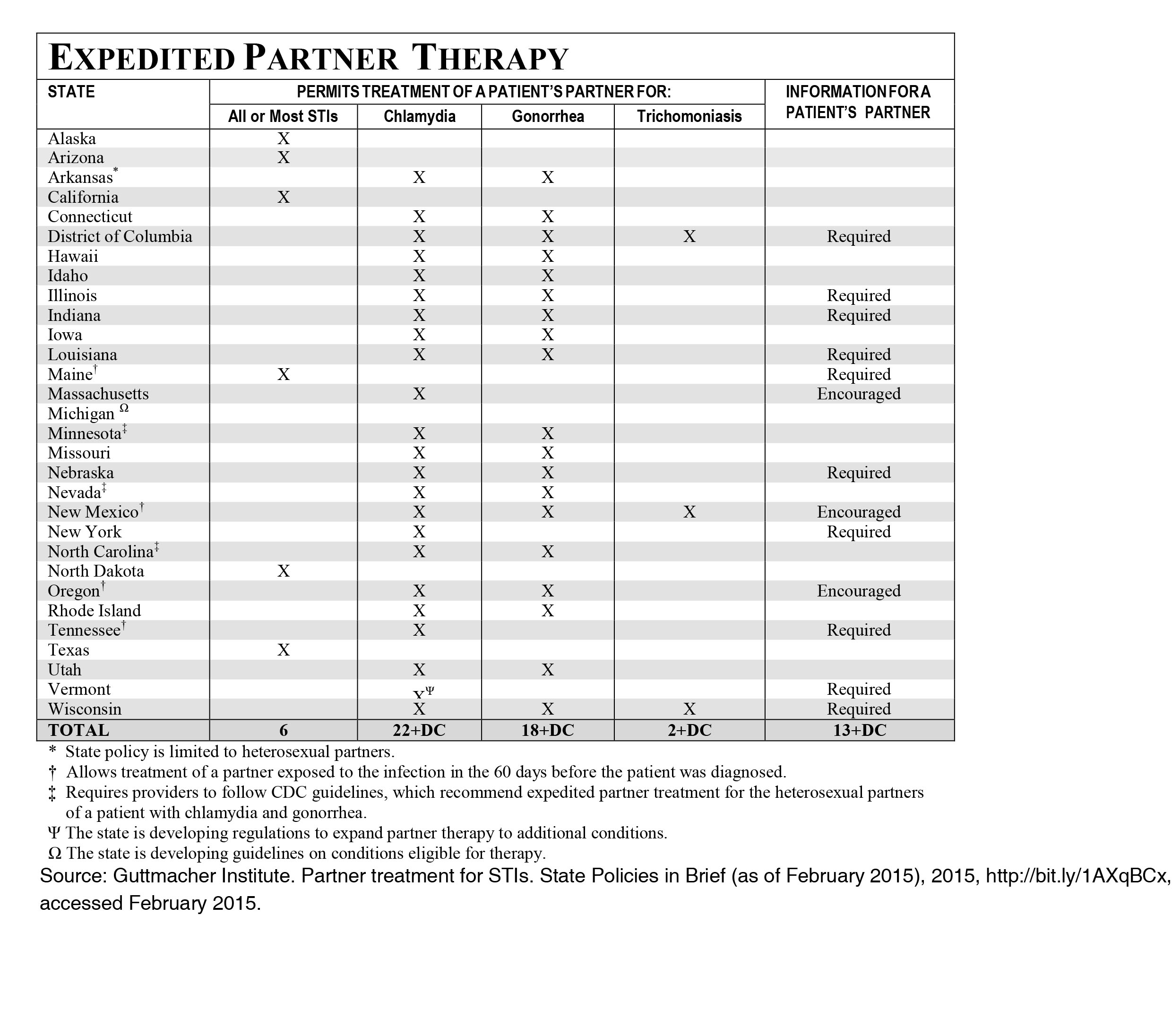
The Guttmacher Institute review notes 22 states and the District of Columbia allow treatment for chlamydia. Eighteen states and the District of Columbia allow treatment for gonorrhea. New Mexico, Wisconsin, and the District of Columbia permit treatment for trichomoniasis. Thirteen states and the District of Columbia encourage or require healthcare practitioners to provide patients with information about STIs to give to their partner.2
Results from a 2013 study showed that in states where laws and policies explicitly authorize EPT, receipt of EPT was significantly higher than where the law simply makes EPT permissible by default.3 When states have laws allowing EPT, 13.3% of patients reported receiving such therapy, compared to 5.4% where there were no pertinent laws and EPT was permissible, and 1% where there were no EPT laws and EPT potentially was allowable.3
In 2014, Michigan joined the ranks of states that allow EPT, while Alabama passed legislation authorizing Alabama Department of Public Health clinics to allow such therapy, says Stephanie Arnold Pang, director of policy and communications at the National Coalition of STD Directors. The District of Columbia issued legislation in early 2014 to authorize EPT. EPT advocates in West Virginia are moving to reintroduce EPT legislation in 2015 after similar legislation was vetoed in 2014 due to technicalities, Pang notes.
-
Golden MR, Kerani RP, Stenger M, et al. Uptake and population-level impact of expedited partner therapy (EPT) on Chlamydia trachomatis and Neisseria gonorrhoeae: The Washington State Community-Level Randomized Trial of EPT. PLoS Med 2015; doi: 10.1371/journal.pmed.1001777.
-
Guttmacher Institute. Partner Treatment for STIs. Accessed at http://bit.ly/1AXqBCx.
-
Cramer R, Leichliter JS, Stenger MR, et al. The legal aspects of expedited partner therapy practice: Do state laws and policies really matter?” Sex Transm Dis 2013; 40(8):657-662.

