Acute Shoulder Injury
April 1, 2015
Reprints
Authors
Brian L. Springer, MD, FACEP,
Associate Professor,
Wright State University,
Department of Emergency Medicine,
Dayton, OH
Deirdre Witte, MD,
Resident Physician,
Wright State University Emergency Medicine Residency Program,
Dayton, OH
Peer Reviewer
Steven M. Winograd, MD, FACEP,
St. Barnabas Hospital,
Clinical Assistant Professor,
Emergency Medicine,
New York College of Osteopathic Medicine,
Old Westbury, NY
Executive Summary
- Proximal fractures of the humerus tend to occur in older patients, most often female, and are most often from low-energy trauma. Those that involve 1-3 fracture segments can be managed conservatively.
- AC separations are most often caused by direct trauma or a fall onto the arm. They cause pain over the joint line on exam. Type 1 and 2 injuries have minimal displacement of the clavicle on X-ray and can be treated with a sling.
- Fractures of the clavicle nearly always occur in the middle or lateral aspect of the bone. Figure-of-eight dressings are no longer used; a simple sling will allow better healing and less discomfort.
- Suspect a rotator cuff tear in older patients (particularly diabetics) who have pain when actively abducting the arm past 120 degrees. Often they will have pain on palpation of the biceps tendon.
Acute Shoulder Injury
Introduction
Musculoskeletal injuries or pain complaints comprise a large portion of visits to emergency departments (EDs) every year. Recent estimates from the Centers for Disease Control and the National Hospital Ambulatory Medical Care Survey showed that of 136 million ED visits, 40 million were injury-related.1,2 Injuries to the shoulder are seen following occupational, recreational, and sports activities, and as a result of trauma and illness (such as seizures). The shoulder alone accounts for 8-13% of sports-related injuries, and shoulder injuries are a frequent reason for visits to the ED.3
The shoulder is the most mobile joint in the human body. The same mechanisms that allow for mobility also put the shoulder at risk for traumatic and overuse injuries. Patients suffering from an acute shoulder injury, or those with ongoing shoulder pain that impairs their athletic or daily activities, will seek help in the ED. Recognition and early management of chronic injury can facilitate recovery and return to activity. Occult fractures or dislocations can lead to poor outcomes if missed. Emergency physicians (EPs) are frequently confronted with individuals who have sustained traumatic dislocations and fractures to the shoulder, with patient ages spanning pediatric to elderly. Acute management of these injuries must be part of the EP’s skill set.
This article provides an overview of the common shoulder problems likely to present in the ED. Since shoulder dislocations were covered in detail in a recent issue, they will not be included. A careful history, physical exam, and working knowledge of basic shoulder orthopedics will help the physician get patients back to their activities sooner and safer. Additionally, familiarity with the shoulder will allow the emergency physician to recognize complex pathology and refer when appropriate.
Shoulder Anatomy
There are excellent online resources that review the anatomy of the shoulder. Among them is a YouTube video “Shoulder Anatomy Animated Tutorial” available at www.youtube.com/watch?v=D3GVKjeY1FM. The shoulder is a complex structure with a plethora of bones, muscles, and ligaments that allow for relative stability over a wide range of motion. In actuality, the shoulder is three joints: the glenohumeral joint, the acromioclavicular joint, and the sternoclavicular joint.4
The bones that form the shoulder include the proximal humerus, which is the insertion point for the majority of muscles that provide strength and mobility. The scapula is an oddly shaped bone whose acromion and coracoid process are the attachment sites for the majority of ligaments that provide stability. The clavicle, another uniquely shaped bone, guards vital blood vessels and nerves as they exit the thorax.
The shoulder ligaments are conveniently named for the bones that they connect, or for the shapes they resemble. Medially, the sternoclavicular joint is stabilized by the costoclavicular ligaments, infraclavicular ligaments, and the anterior and posterior portions of the sternoclavicular capsular ligaments. The medial aspect of the clavicle is connected by the interclavicular ligament. Laterally at the acromioclavicular (AC) joint, the coracoclavicular ligaments, the conoid, and the trapezoid are strong stabilizing tissues. The coracoacromial ligament functions somewhat like a seatbelt under which some muscles of the shoulder travel. Additionally, because it is a bridge between two portions of the scapula, it can remain intact and provide stability when other bones of the shoulder are compromised. The superior AC ligament provides lateral stability to the likewise named joint. Its counterpart, the inferior AC ligament, also provides stability but is thinner and less robust. The coracohumeral ligament, a broad connection between the coracoid and humerus, provides support to the superior glenohumeral joint. The glenohumeral ligaments, comprised of the superior, middle, and inferior portions, reinforce the glenoid capsule anteriorly by connecting the glenoid of the scapula to the head of the humerus. Finally, the glenoid ligament, also known as the glenoid labrum, is less of a ligament and more of a soft-tissue extension of the shallow “socket” portion of the “ball and socket” shoulder joint. It functions to create a deeper but more forgiving pocket for the humeral head. The labrum is important not only because it is part of what allows such diverse movement in the shoulder joint but also because its injury can be a source of pain and joint instability.5
The latissimus dorsi and pectoralis major muscles insert on the humerus, facilitating adduction and internal rotation of the shoulder. These muscles also affect injury patterns to the joint. For example, it is the overpowering forces from these larger muscles that cause posterior dislocations with seizures and electrocutions, and result in the inferior position of bone fragments after humeral fractures.4 The rotator cuff muscles are small but important. The supraspinatus, infraspinatus, teres minor, and subscapularis (SITS muscles) are dynamic stabilizers, keeping the humeral head within the glenoid fossa and facilitating abduction and internal/external rotation. Acute or chronic injury to the rotator cuff can lead to significant pain, decreased range of motion, and functional deficits.6 The biceps contributes to forward flexion, abduction, or adduction, depending on the degree of internal or external rotation of the shoulder. Because of the way both the short and long heads of the biceps traverse the glenohumeral joint, they also contribute to joint stabilization. The deltoid muscle provides an elegant cap to the glenohumeral joint, providing abduction as well as overlying the axillary nerve and vessels.
The largest vessels associated with the shoulder are the subclavian artery and vein. They exit the thorax under the protection of the clavicle and then branch off to smaller vessels. Similarly, the brachial plexus is also protected by the clavicle but then branches into the various nerves responsible for providing sensation and function for some of the shoulder and all of the arm and forearm.
History and Physical Exam
There are excellent online resources that review the examination of the shoulder. Among them is a YouTube video “Shoulder Examination — Orthopaedics” available at https://www.youtube.com/watch?v=g8xtOqZFTwo. In any patient who is presenting to the ED with an acute shoulder injury, search for associated life- or limb-threatening traumatic injuries. A brief assessment of the patient’s circulatory status, airway, breathing, and neurologic status should be conducted prior to more detailed evaluation of joint injury. Often, the emergency physician can quickly make this determination at the bedside by observing an injured but otherwise well-appearing patient. Should there be evidence of or concern for more significant trauma, the primary survey and appropriate interventions will take priority over any shoulder injury. Do not allow dramatic appearing orthopedic injuries to draw you away from critical elements of the trauma assessment.
Begin with a focused but complete history of the problem. (See Table 1.) Determine where the patient is experiencing pain, the duration of pain, and whether it is getting better or worse, what activity (if any) was occurring at the time pain began, what activities worsen or relieve the pain, and any associated symptoms. History of acute trauma should raise suspicion of dislocation, fracture, or AC separation. History of repetitive motion and overuse should raise suspicion for osteoarthritis, chronic rotator cuff tear (RCT), or subacromial impingement. Ask about any neurologic or vascular complaints such as numbness, weakness, or functional loss. A history of the arm going “dead” or feeling the shoulder slip during injury could indicate subluxation of the glenohumeral joint. A unilateral “dead” arm is also common with a stinger, which is an injury to the brachial plexus. Bilateral weakness or paresthesia should raise suspicion for cervical spine injury. Presence of fever should raise concern for septic arthritis.
Table 1. History of Shoulder Injury: Highlights
- Mechanism of injury; inquire about recent activities that may have resulted in injury, such as sport, recreation, or other physical activity
- Duration of pain
- Location of pain
- Exacerbating factors (especially overhand activity)
- Prior shoulder injury/pathology/surgery
- Associated symptoms (paresthesia, radicular pain)*
- Presence of night pain*
- Constitutional symptoms (fever, weight loss)*
* Presence of these features may indicate pathology such as cervical radiculopathy or neoplastic disease (although night pain is seen in rotator cuff tear/tendinopathy, and glenohumeral arthritis).
Shoulder pain may be referred from other organ systems. In age-appropriate patients, ask about associated symptoms such as chest pain or shortness of breath that may indicate angina. Peritoneal irritation from abdominal pathology may cause referred shoulder discomfort. Cholecystitis can present with referred pain to the right shoulder or scapula. Splenic enlargement or rupture may cause referred pain in the tip of the left shoulder (Kehr’s sign).
Past medical history can also give clues to etiology of shoulder pain. Adhesive capsulitis is more common in diabetics, those with thyroid disease, and individuals with cerebral or cardiac atherosclerotic disease.7 Individuals with prior shoulder dislocations are more susceptible to subsequent dislocation, or may present with anterior glenohumeral instability, RCTs, or labral tears.
In order to perform a proper inspection, the patient must be undressed. This is the only way to effectively evaluate for deformity, atrophy, skin changes and rash, abnormal range of motion (ROM), and neurologic function. (See Table 2.) It also enables the physician to examine the contralateral shoulder for comparison. Male patients should be examined shirtless; female patients may be examined in a tank top or brassiere, although a gown allows the easiest palpation of the entire shoulder girdle. Inspect the shoulder closely for any muscular asymmetry or scapular winging.
Table 2. Physical Examination of the Shoulder: Highlights
- Always perform a trauma-based primary survey before more detailed examination.
- Undress the patient to assess for atrophy or asymmetry; compare to contralateral side.
- Examine at least a joint above (cervical spine) and below (elbow) seeking referred pain or associated injury.
- Observe active range of motion while standing behind the patient, looking for abnormal movement.
- Check and document distal pulses and sensation over the deltoid (axillary nerve) before and after any procedural manipulation.
- Specialized tests for rotator cuff injury (Neer and Hawkins impingement tests, etc.) are neither sensitive nor specific on their own; combine them with a good history and thorough examination.
Palpate the bones for any areas of point tenderness or step-offs. Begin palpation with the SC joint and gradually work your way laterally along the clavicle, to the AC joint, humeral head, and humeral shaft. Feel for tenderness, crepitation, or deformity. Palpate the scapula from proximal to distal, as scapulothoracic injury and dysfunction can cause pain to the shoulder. Palpate the surrounding soft tissues of the upper back, scapulothoracic articulation, and about the proximal humerus. Palpate the infraspinatus, supraspinatus, rotator cuff insertion on the proximal humeral head, and the proximal biceps tendon. Tailor your exam to the patient; an acute fracture or dislocation may impair the patient’s ability to tolerate your exam. Prompt administration of appropriate analgesics will facilitate your assessment. As a general rule, inspect and palpate a joint above (cervical spine) and joint below (elbow) the shoulder.3
Check active and passive range of motion. Compare to the contralateral side. Range of motion testing should include abduction, forward flexion, cross-body adduction, and internal and external rotation. Observe abduction and flexion from behind so that any asymmetry in scapular movement can be noted. Active range of motion may be limited by pain or functional deficits, while passive range of motion is preserved in most injuries. Limitations of passive range of motion should raise suspicion for fracture, dislocation, or adhesive capsulitis.
Assess strength of the biceps, triceps, deltoid, and rotator cuff muscles. Resisted abduction with the arm angled 30 degrees anterior to minimize deltoid tests the supraspinatus; external rotation with elbow flexed at 90 degrees, rotating from midline against resistance, tests the infraspinatus and teres minor; internal rotation (patient places hand against the small of the back and pushes off against resistance) tests the subscapularis. Check distal pulses at the wrist. Suprascapular and radial nerve injury may result in rotator cuff weakness (particularly abduction) or impaired elbow and wrist extension. Axillary nerve injury may result in sensory deficits over the lateral deltoid.
Specialized physical exam tests for shoulder pathology are operator dependent, and lack sensitivity and specificity. No single test should be used to make a pathognomonic diagnosis. Combinations of testing along with an accurate history can help narrow the differential diagnosis.8,9,10 Test for subacromial impingement by passively forward flexing the shoulder with the thumb pointing down, internally rotating the humerus (Neer’s test), or by abducting the shoulder to 90 degrees and internally rotating (Hawkin’s test). Pain on either maneuver is considered a positive exam.
Instability is a common cause of acute and chronic shoulder pain in younger athletes, and may be unidirectional (most often anterior or inferior) or multidirectional. Application of anterior and posterior stress to the shoulder may reveal a palpable shift in the joint or may only elicit discomfort. If the examiner suspects the patient may have sustained an anterior subluxation or dislocation that has spontaneously reduced, duplicate the mechanism of injury by abducting the shoulder to 90 degrees, flexing the elbow, and externally rotating the glenohumeral joint. A sense of apprehension and impending dislocation is sensitive for anterior instability, whereas pain itself is nonspecific. Clinical testing for tears of the glenoid labrum is challenging. Specialized tests such as the O’Brien test and crank test may arouse clinical suspicion, but conclusive assessment often entails use of MRI.11,12
Imaging Modalities
The recommended approach to shoulder pain is a thorough history and physical exam. Time course, mechanism of injury, range of motion, joint appearance, and palpation of the joint are often very revealing. From there, imaging studies can identify many of the most common shoulder injuries, namely dislocations, humeral fractures, and clavicular fractures. This section is an overview of the various imaging modalities; recommendations for specific injuries are discussed in greater detail later. A reasonable approach to an injured shoulder is to start with a three-view series of radiographs including a true anteroposterior, trans-scapular lateral (Y-view), and axillary lateral view.4 If an acromioclavicular joint separation is suspected, it may be useful to image the contralateral shoulder to help assess the severity of the lesion.13
There is ongoing interest in eliminating unnecessary imaging, which can be both costly and time-consuming.14 One case in which the need for radiographs continues to be debated is in those with suspected anterior dislocation. Rates of concurrent fracture in younger patients are low, and it has been suggested that forgoing a pre-reduction shoulder radiograph in this age group could reduce imaging in those with anterior dislocations by up to 40%.15 Similarly, other studies have suggested that with the guidance of a seasoned EP, certain populations, specifically those with prior shoulder dislocations, may not need pre- or post-reduction films in the non-traumatic setting.14,16 Use caution, however. One prospective study demonstrated post-reduction films identified six fractures that were missed by pre-reduction films.17 It should be noted that in all of these studies, the identified fractures did not change management of the patient in the ED. The bottom line is that although the consensus agrees that EM physicians are excellent at identifying anterior shoulder dislocations with physical exam and history, there is not yet a significantly large prospective trial that definitively states shoulder dislocations can be managed without either a pre- or a post-reduction film.
Radiographs of the shoulder are not limited to the identification of fractures and dislocations. The presence of a superiorly displaced humeral head on X-ray can suggest a rotator cuff injury.6 Calcific tendinitis, which may present as acute pain and decreased range of motion, can often be identified on plain film.18 Ultrasound is becoming an increasingly used modality for evaluating soft-tissue injury of the shoulder. Ultrasound may be an ideal test for rotator cuff tendon injury. Although it is operator dependent, sensitivity of ultrasound approaches 98% for identifying rotator cuff tears. Acute, full-thickness tears are the easiest to identify as they are most likely to demonstrate a large pocket of fluid and absence of contiguous tendon.18 Despite the increasing use of ultrasound, many orthopedists still consider MRI to be the modality of choice for identifying soft-tissue injury.19 However, this is less likely to be available or useful for treatment in the emergency department. Computed tomography scans, with the exception of CT angiography to evaluate vasculature in severe thoracic trauma, are not typically used in the ED to evaluate shoulder injuries. Most often, it is used in the outpatient setting to further categorize fracture deformities perioperatively.20,21,22
Proximal Humerus Fractures
As the population ages, there has been a documented increase in the number of proximal humerus fractures. It has been postulated that this is related to the increased risk of falls as well as the increased number of those who suffer from osteoporosis, diabetes, and other comorbidities.23,24 Proximal humerus fractures account for approximately 6% of all adult fractures, making them the seventh most common fractures seen. They account for 5% of all fractures seen in the ED, and are the third most common fracture seen in the elderly.3 A recent study of U.S. emergency departments found that proximal humerus fractures appear to be more common in the United States than in other parts of the world.25 Regardless of the country, proximal humerus fractures are being seen increasingly often in the acute care setting.26 The majority of proximal humeral fractures are minimally or non-displaced, and will respond to conservative treatment with immobilization and early range of motion. Displaced fractures pose challenges to orthopedic surgeons and may result in associated neurological and vascular injury.
The most common mechanism of proximal humeral fractures in younger populations is motor vehicle crashes (MVCs) or other high-energy causes. In older populations, especially those older than age 60, proximal humeral fractures are most often due to low-energy injuries like falls from standing height. They are more common in women than men at this age, with a ratio of 3:1, making up almost half of the humeral fractures seen in the elderly. Therefore, a high index of suspicion, even in those with low-energy trauma, is important to ensure the timely diagnosis of this injury.24,25,27,28
A thorough history can help direct identification of proximal humerus fracture. Falling with an outstretched arm from a ground level height is the most common mechanism in the elderly. In younger patients, suspect the injury in cases of high-energy trauma to the lateral shoulder. Patients frequently hold the arm in adduction, and complain of increased pain with movement. Due to the surrounding musculature, obvious deformity may not be seen; tenderness over the affected area is usually present. If there is concern that the humerus could be fractured, conduct an in-depth examination of the affected limb including distal pulses, active and passive range of motion, and sensation. The axillary nerve is most commonly affected with proximal humerus fractures. Fortunately, these are usually traction or contusion injuries rather than complete nerve disruptions, and symptoms resolve with time. Fractures of the anatomic neck are in close proximity to the axillary artery and the anterior and posterior circumflex arteries and, although rare, vascular injury may occur. If there is apparent vascular compromise (pulse deficits, extremity pallor or coolness, or extensive extremity swelling) or an open fracture, an orthopedic surgeon should be involved immediately.29,30
Figure 1. Proximal Humerus Fracture
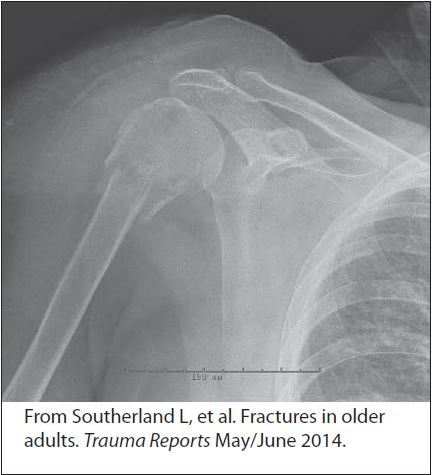
From Southerland L, et al. Fractures in older adults. Trauma Reports May/June 2014.
In complicated or open fractures, imaging may include CT and CT angiography to elicit details of the fracture and to assess the extent of vascular insult. In closed fractures without evidence of significant neurovascular compromise, plain radiographs should be obtained. Obtain a true anterior-posterior view of the glenohumeral joint, a scapular-Y, and an axillary view. This will allow the provider to assess for shoulder dislocation, glenoid fracture, and proximal humeral fracture. Care should be taken to note if the patient is seated or supine, as an upright film may allow for more accurate depiction of displacement and alignment.29
Classification. There are many different classification schemes for proximal humerus fractures. Perhaps the two best known are the Neer and the AO classifications. (See Table 3.) Both systems were designed to help describe the nature of the injury to surgeons indicating the need for operative intervention and correct surgical approach.31,32 The guiding factors in both descriptive systems are injury severity, displacement, and vascular isolation (increased isolation equals increased risk of avascular necrosis.)33 The AO system is less commonly used. Both the Neer and AO systems are complex, and it should be noted that these classification systems do not often change the treatment in the ED, but may help the emergency physician better define the injury when consulting with orthopedics.
Table 3. Classification of Proximal Humerus Fractures
The Neer classification system defines proximal humerus fractures by the number of displaced segments, with additional categories for articular fractures and dislocations. Potential segments involved are the greater tuberosity, lesser tuberosity, articular surface, and humeral diaphysis. A segment is defined as displaced if there is > 1 cm separation or 45 degrees angulation.
One-Part Fracture: No fragments displaced. Fracture with no fragments displaced is defined as a one-part fracture regardless of actual number of fracture lines or their location.
Two-Part Fracture: Greater tuberosity, lesser tuberosity, or articular segment at anatomic or surgical neck is displaced.
Three-Part Fracture: Surgical neck is displaced, along with one tuberosity.
Four-Part Fracture: All four segments displaced, with articular segment displaced laterally from glenoid.
Risk of avascular necrosis increases depending on number of fragments and displacement. Neer also created separate categories for fracture dislocations and to describe articular surface injuries.
Adapted from: Carofino BC, Leopold SS. Classifications in brief: The Neer classification for proximal humerus fractures. Clin Orthop Relat Res (2013) 471:39–43.
Management. Proximal humerus fractures were found in a recent study to carry a 10% mortality, with the only independent predictor of survival being whether or not the patients lived in their own homes.27 Unless there is an associated vascular injury or open fracture, most patients can be managed with a sling immobilizer, analgesics, and follow-up as an outpatient. Consider admission for any patient, especially one who is elderly, in whom ability to perform activities of daily living and access to follow-up may be compromised.29
Although it is generally agreed that younger patients benefit from surgical intervention to preserve their native bone, multiple studies have demonstrated that in patients with minimally displaced fractures, especially in populations older than 75 years, conservative management allows for good mobility and quality of life.34 Patients with proximal humerus fractures that have 1-3 fracture parts with minimal angulation and/or displacement can expect to spend 1-4 weeks in a sling with strict precautions and guided rehabilitation. Those with 3- and 4-part fractures and with greater displacement and/or angulation are thought to be at greater risk for avascular necrosis and non-union, and are more likely to benefit from surgical repair.31,32 The length of time in an immobility sling as well as the types of surgical repair continue to be a topic of research and discussion among orthopedists. The treatment course after the diagnosis in the ED will be dependent on both the degree of injury and the habits of the orthopedic surgeon.
Acromioclavicular Separation
Injuries to the AC joint make up approximately 9% of all shoulder injuries. Almost half of these injuries occur in individuals in their 20s. AC joint injuries are five times more common in males, and are strongly linked to participation in contact sports. AC separations are among the most common injuries seen in hockey players, and among the most common shoulder injuries seen in football players.35
The AC joint is surprisingly mobile. It has a surrounding capsule enclosing synovial fluid and a cartilaginous articular surface, analogous to most joints. The joint capsule, along with the earlier mentioned coracoclavicular, acromioclavicular, and coracoacromial joints provide exceptional static stability to the joint, supplemented by active stabilization of the deltoid and trapezius muscles. The AC joint is capable of up to 30 degrees of motion in the vertical, horizontal, and frontal planes. This coupling of clavicular and scapular movement is essential to allow for full range of motion of the shoulder.
The most common method of injury to the AC joint is application of direct force from a fall or impact on the “point” of the shoulder with the arm adducted. The impact drives the scapula inferiorly, dislocating the AC joint and placing stress on the coracoclavicular ligaments, which may also be injured. The AC joint may also be injured indirectly by a fall on an outstretched arm or elbow, driving the humeral head superior into the acromion. These injuries tend to be less severe, affecting only the AC ligaments and sparing the CC ligaments.
On presentation, patients will complain of pain in the AC joint. Irritation of the subacromial space, lateral pectoral nerve, or suprascapular nerve may also result in referred pain to the anterior, lateral, or posterior shoulder.35 Swelling or obvious deformity may be present depending on the degree of injury. Examine the patient standing; the weight of the arm will stress the AC joint and may worsen pain and accentuate deformity. The patient’s shoulder will be tender to palpation along the AC joint. Motion typically is painful with abduction and flexion, but worse with cross-body adduction which generates compression forces within the joint. With the elbow flexed at 90 degrees and the shoulder internally rotated, gently abduct the arm to 90 degrees. Slowly adduct the arm across the body, keeping a hand on the AC joint. The maneuver will usually localize pain to the joint, and crepitation may be felt. Rotator cuff strength may be compromised due to pain.
Standard shoulder radiographs should be obtained to evaluate the integrity of the joint.36 Radiographic findings of AC separation include widening of the AC joint greater than 3 mm and an increase in the coracoclavicular distance greater than 13 mm. Obtaining weighted “stress views” of the affected shoulder is of limited clinical use and no longer recommended in the emergency department setting.3
AC Injury Classification. AC injuries are graded depending on the location and extent of ligament damage, as represented by radiographic findings following injury. Type I injury involves only a strain of the acromioclavicular ligaments. There may be mild widening of the AC joint but no change in the coracoclavicular (CC) space. A type II injury involves tear of the AC ligaments and disruption (but not a complete tear) of the CC ligaments. The AC joint will be widened, and the scapula may depress under weighted stress. A type III injury involves complete rupture of both ligaments. The distal clavicle will be prominent and may actually tent the skin. The scapula will be depressed inferiorly on plain films. Type IV, V, and VI injuries represent more severe injury to the joint and are classified according to the positioning and degree of displacement of the clavicle relative to the acromion. (See Table 4.)
Table 4. AC Separation Chart
AC separations are classified based on radiographic displacement, which correlates with extent of ligamentous injury.
Type I: AC ligaments sprained but intact; coracoclavicular ligaments uninjured
Type II: AC ligaments disrupted, coracoclavicular ligaments sprained but intact
Type III: AC and coracoclavicular ligaments disrupted
Type IV: AC and coracoclavicular ligaments disrupted; distal clavicle displaced posteriorly through the trapezius muscle
Type V: AC and coracoclavicular ligaments disrupted; muscle attachments disrupted; significant inferior displacement of acromion
Type VI: AC and coracoclavicular ligaments disrupted; clavicle displaced inferior to coracoid process and posterior to biceps and coracobrachialis tendon
Management. The end goal of AC injury management is establishing full, pain-free range of motion of the shoulder. Type I and II injuries can be treated conservatively. Initial management in the ED is focused on pain control. Ice, NSAIDs, and (if needed) a brief course of opioid analgesics are appropriate. To facilitate pain control, consider the use of direct joint injection with several cc’s of local anesthetic. This technique is used frequently on the sidelines of contact sports to facilitate return to play and appears to be safe. Caution should be advised, however, as individuals have exacerbated existing injury by returning to sport following local injection.37 Traditional sling immobilization is a useful pain-control adjunct, with gradual progression of range of motion initiated over the next 1-2 weeks. Heavy lifting, which directly stresses the AC joint, should be avoided for 2-3 months. If the patient is an athlete involved in a contact sport, additional padding will be required to protect the joint and the patient should be referred to their certified athletic trainer. With type III AC injury, treatment (operative versus conservative) remains controversial, and these individuals should receive outpatient referral to an orthopedic surgeon.38 ED management with sling immobilization and analgesics is indicated. Type IV, V, and VI injuries represent high-energy injuries with a greater degree of tissue disruption, and most are treated operatively. Immobilize the injured shoulder in a sling, administer analgesics, and consult with orthopedics to facilitate appropriate inpatient or outpatient follow-up.
Clavicle Fractures
Clavicle fractures constitute approximately 35-44% of all fractures of the shoulder girdle and from 2.6-5% of all fractures. Unlike many other shoulder injuries, clavicular fractures are more common in younger populations, with incidence decreasing after the first decade of life and not increasing again until the eighth decade. This is also one of the few fractures that is more common in men than in women, being about three times more likely in the male population. The mechanism of injury helps account for this difference; often clavicle fractures are the result of high-energy mechanisms such as falls while horseback riding or bicycling, or from motor vehicle collisions. In the elderly population, a fall from standing is the most likely mechanism. In all age groups, the injury occurs when patients fall directly onto an unprotected shoulder, either with or without an outstretched hand.28,39
Figure 2. Clavicle Fracture
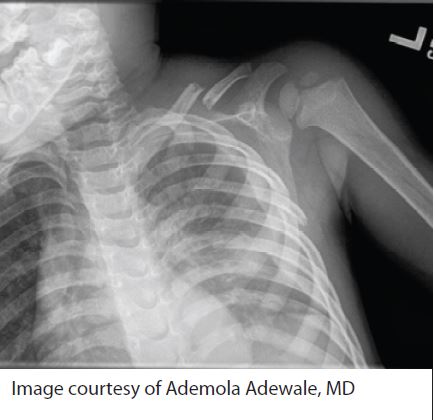
Image courtesy of Ademola Adewale, MD
When assessing clavicle fractures, it is important to understand the bone is divided into three parts: medial, mid-shaft, and lateral. Almost all clavicle fractures are mid-shaft fractures, accounting for 81-88%, depending on the age group. Medial clavicle fractures are by far the rarest, accounting for less than 2% of clavicle fractures and may be associated with mediastinal injury. The lateral third of the clavicle is fractured roughly 19% of the time, and may be associated with AC joint injury.39 There are a variety of classification systems including the Neer, the Edinburgh, and the Allman. In the emergency department, one does not need a specific classification scheme to provide optimal care. The provider needs only to identify which third of the clavicle is fractured and whether it is displaced or non-displaced.
After ensuring stability with a trauma primary survey, obtain a good history with a focus on mechanism and symptoms. Perform a careful physical exam looking for obvious deformities first. Clavicular fractures are often easily visualized and will be point-tender over the fracture line. Mild skin tenting may be present; compromise of the overlying tissue is grounds for surgical intervention.39 The clavicle protects neurovascular structures running from the neck to the arm, so a thorough neurovascular exam should be done. Assess for swelling, pallor, and pulse deficits in the affected arm. In significantly displaced or comminuted fractures, checking blood pressures from side to side can help ascertain if there is vascular injury to the subclavian vessels. Pulse deficits or blood pressure differentials should raise suspicion for this injury and prompt vascular imaging. The brachial plexus may also be injured by bone fragments from comminuted clavicle fractures. Carefully assess the distal limb for strength and sensation. As the clavicle sits on the anterior and superior thorax, consider the possibility of underlying chest injury such as pneumo- or hemothorax.40 Auscultate the chest carefully and have a low clinical threshold for obtaining imaging of the chest.
Imaging. Simple AP views of the clavicle (true AP and a 45 degree cephalic tilt AP) are often all that is needed to assess for injury. Be sure to assess the lung apex to look for pneumothorax, upper rib fractures, or other complications. If a patient arrives and is dyspneic, and does not have apparent clavicular fracture on X-ray but has a story with a concerning mechanism, a CT scan may be helpful to assess for possible medial clavicular fracture with posterior displacement.39 This is a rare complication of clavicle fracture but can cause compression of major vessels in the chest and should be considered.
Management. Barring significant neurovascular complications or open fractures, almost all clavicle fractures can be managed conservatively. Historically, even patients with displaced fractures were managed entirely without surgical intervention. Recently, there has been interest in surgically repairing comminuted and displaced fractures, as their rates of non-union have been higher in more current studies. The debate continues, and study outcomes on surgical versus nonsurgical treatment remain mixed. Depending on both classification of the injury and need for rapid return to function, delayed surgery may be an option.41,42
Regardless of whether the patient ultimately goes to surgery, initial treatment recommendations are generally uniform. The patient should be given adequate analgesics and be placed in a sling. Traditionally, a figure-of-eight sling was thought to facilitate healing. Recent studies show no benefit to a figure-of-eight sling over a traditional sling, and that a figure-of-eight sling may actually increase patient discomfort, risk of brachial plexus injury, and fracture non-union.39 The patient should be encouraged to wear the sling only as needed for comfort, and begin moving the shoulder as soon as he or she can comfortably do so.35 Provide sufficient outpatient pain medications and a referral to orthopedic surgery. Patients should be advised to return should they develop distal extremity pain or weakness, or should they notice any breakdown of skin overlying the fracture sight.
Sternoclavicular Injuries
The sternoclavicular (SC) joint is it the only true joint connecting the upper limb and the axial skeleton. It has only a shallow articulation between the clavicle and the sternum, relying heavily on its surrounding ligaments rather than a deep joint pocket for stability.43,44 Despite this, the SC joint is rarely dislocated. SC dislocations make up only about 3% of shoulder girdle dislocations, the majority of which are the result of high-energy injuries from MVCs and sports such as rugby or football.45 Similar to other high-energy injuries, they are most common in young males.5
SC injuries may be categorized as type 1-3 or as mild, moderate, and severe. The mild (type 1) injury is not a dislocation but rather a sprain of the joint’s surrounding ligaments. Movement of the shoulder will elicit pain, and the joint may be tender and swollen. A moderate (type 2) injury is a partial thickness tearing of one or more surrounding ligaments, and may present with a greater degree of pain, swelling, and dysfunction. Some subluxation of the joint may be felt with manual stress. In either mild or moderate injury, both the exam and radiographs reveal that the joint is in proper anatomic position at baseline and does not fully dislocate. A severe (type 3) injury is a complete anterior or posterior dislocation of the joint.35,45,47 Patients will have severe pain worsened by shoulder movement. Deformity will be noted when compared to the contralateral shoulder, with either prominence (anterior dislocation) or absence (posterior dislocation) of the joint on observation.
Severe SC injuries are described as anterior or posterior based on whether the head of the clavicle lies anterior or posterior to the sternum. Anterior dislocations are far more common than posterior ones, with an incidence of between 5-27% of SC injuries.46 If a severe SC injury is suspected, a radiograph of the chest using the serendipity view (patient supine, with X-ray tube tilted 40 degrees and pointed at the manubrium) can be helpful in verifying the location of the clavicle head. If a posterior dislocation is suspected, CT may be preferable because soft tissue can be better visualized, and the use of contrast can highlight associated vascular injuries.43,44
Mild and moderate SC injuries may be treated with ice, analgesics, and sling immobilization for comfort.45,47 Active individuals and those with any degree of SC joint instability on exam should be referred to an orthopedic surgeon for outpatient follow-up. If an anterior dislocation is identified, attempting reduction in the ED is reasonable, given that many SC dislocations are treated successfully with closed reduction and conservative management.46 Before attempting this, the patient should be informed that the clavicle may spontaneously dislocate immediately or subsequently post-reduction. Place the patient supine with a towel roll between the shoulder blades, and apply gentle pressure to the anteromedial clavicle until reduced. If the joint remains reduced, place the patient in a figure-of-eight brace (the patient will need to remain braced for 4 to 8 weeks). If reduction is not successful, place him or her in a sling for comfort. In either case, provide adequate analgesics, and refer the patient to an orthopedic surgeon for outpatient follow-up.35,43,45
Posterior SC dislocations are considered surgical emergencies because of the potential for damage to underlying structures such as the esophagus, the vagus and phrenic nerves, the trachea, and innominate artery and vein.43,48 Posterior dislocation should be considered if a patient sustains injuries to the chest or shoulder from a high-energy mechanism. Exam findings such as dysphagia, dysphonia, edema, or venous congestion of the arm and/or neck of the ipsilateral limb may all be suggestive of a posterior SC dislocation. If the injury is suspected or seen on plain radiographs, obtain a CT scan with IV contrast. While emergent reduction with a towel clamp is often described in the literature, posterior dislocations should undergo closed reduction in the operating room under general anesthesia, with a vascular or cardiothoracic surgeon available due to risk of damage to underlying structures. Rarely, open operative reduction will be required.43,45
Rotator Cuff Injuries
Rotator cuff injuries are a common cause of shoulder pain in all age groups, and they encompass a spectrum of injuries. The true incidence of rotator cuff tears secondary to acute trauma is unknown; complete tears in the young are relatively uncommon and associated with a higher energy mechanism of injury such as a significant fall, MVC, or shoulder dislocation. With even minor trauma, tears occur more frequently in patients older than age 50. Overuse injuries are most commonly seen in athletes and active individuals, and increase in frequency after age 40. Mechanical irritation of the rotator cuff in the subacromial space may create “impingement syndrome” with resultant strain, tendinopathy, and subacromial bursitis.3,49,50
Differentiating rotator cuff injury from other pathology such as simple strains, contusions, or bursitis can be challenging. Diagnosis ultimately is made based on history of the injury, physical findings, and imaging studies, and often will not be confirmed in the ED. Patients with rotator cuff injury will often localize pain to the lateral deltoid. Pain is made worse with overhead activities, and night ache is a common complaint. Historically, patients may recall a direct blow or traction injury to the shoulder. In overuse, they may not recall a specific injury but may have engaged in repetitive activity such as cleaning or moving boxes. Overhand sporting activities such as swimming, tennis, baseball, or softball may precipitate or worsen injury. Patients may report a history of painful clicking or popping in the shoulder.
Tenderness to palpation of the relatively deep muscles of the rotator cuff may be difficult to elicit. Palpate the long head of the biceps tendon in the bicipital groove to determine biceps involvement. Biceps tendinopathy rarely exists alone; it is estimated that more than 90% of cases of biceps tendinopathy are associated with tears of the rotator cuff or labrum.51 In patients older than 50 years or in patients with pain radiating past the elbow, perform a careful cervical spine examination to rule out radicular symptoms. Patients will most likely have painful “arc of motion” with active abduction beyond 120 degrees, and in significant tears may be unable to fully abduct the shoulder. Observe ROM from behind, looking for asymmetric movements or muscular atrophy. Neer and Hawkins tests may be positive if impingement is present. While no single physical exam test is specific enough to rule in a tear, the combination of trauma history, painful/limited arc of motion, and advanced age highly correlates with the presence of rotator cuff pathology.3,8,9,52
Imaging. Radiographs of the shoulder should be performed to exclude fracture or dislocation. Obtain AP and axillary views. This allows the examiner to also look for signs of AC or glenohumeral arthritis, calcific tendinosis of the supraspinatus, and spurring of the acromion that may contribute to narrowing of the subacromial space. As noted earlier, superior displacement of the humeral head may be seen in rotator cuff tears, but in most cases plain films are nondiagnostic.3,6 Confirmation of rotator cuff tears is most often accomplished through outpatient MRI, although ultrasound use is increasing, and may be even more sensitive than MRI when performed by an experienced operator.52,53 If the patient has full range of motion, further imaging studies can be safely deferred to allow a trial of conservative treatment.
Treatment. Patients with suspected rotator cuff pathology in the ED should be treated with ice, analgesics, and a sling for comfort. Appropriate referral to an orthopedist or sports medicine specialist should be given. Advise patients of all ages to institute gentle range-of-motion as soon as tolerated. Young, active individuals with acute traumatic tears are more likely to have surgical intervention. Active patients with partial tears due to overuse and degenerative changes are likely to respond to aggressive rehabilitation and rotator cuff strengthening. Surgical tendon repair and decompression of the subacromial space are considered in recalcitrant cases. In older patients, surgery remains controversial, as many patients with full thickness tears are asymptomatic. That is contrasted by concerns that in symptomatic patients, tendon repair becomes increasingly difficult when surgery is delayed.50 Once again, the mainstay of treatment in the ED is conservative management to include analgesia, range of motion, and close follow-up.
Adhesive Capsulitis
Adhesive capsulitis or “frozen shoulder” is characterized by insidious onset of pain and loss of range of motion of the joint. The exact mechanism of the disease is poorly understood. Pathologically, it results from contraction of the glenohumeral joint capsule and adherence to the humeral head. The incidence of adhesive capsulitis is approximately 3% in the general population. Women are more often affected than men, with a peak incidence between 40 and 70 years of age. Individuals with insulin-dependent and non-insulin dependent diabetes, and meeting criteria for prediabetes are at significantly increased risk. Approximately 20% of diabetics will develop adhesive capsulitis, as compared to 2-5% of the general population.3 Less commonly associated conditions include hypo- and hyperthyroidism, Parkinson’s disease, hypoadrenalism, cardiac disease, and stroke.54 While adhesive capsulitis may be diagnosed as idiopathic or “primary,” underlying shoulder pathology such as rotator cuff tendinopathy or tear, subacromial bursitis, biceps tendinopathy, or recent shoulder surgery or trauma may exist and probably is a greater contributor to disease risk than previously thought.
Adhesive capsulitis has been classically described as having three sequential stages: painful stage, freezing stage, and recovery stage. There is no evidence to validate this classification, as pain and limited range of motion may occur in all phases of the disease. Pain and decreased range of motion can persist for years, and 10% of patients never regain full range of motion.55
History and Physical Exam. Patients will complain of poorly localized, deep aching pain and diminished range of motion. Progressive difficulty in reaching forward, overhead, and (especially) behind the back will be present. Be sure to ask about the presence of fever, night sweats, weight loss, or neuropathic symptoms in the extremity that may indicate presence of other disease processes such as cervical radiculopathy or neoplasm. Additional differential diagnosis considerations include glenohumeral osteoarthritis, rotator cuff and biceps tendinopathy, acromioclavicular arthropathy, and autoimmune disease (lupus, rheumatoid arthritis). As noted, these etiologies may occur alongside adhesive capsulitis, making the diagnosis challenging. Adhesive capsulitis can often be differentiated from other diseases by limitation in passive range of motion.3 Loss of motion with forward flexion, abduction, and external and internal rotation should raise suspicion for adhesive capsulitis. Compare these maneuvers on the affected and unaffected sides to accurately assess deficits.
The gold standard for diagnosis of adhesive capsulitis is direct visualization under surgery, although other imaging modalities such as MRI are being used increasingly to supplement the history and physical exam.54,55 In the ED, it is prudent to obtain plain radiographs to assess for tumors, pathologic fractures, severe osteoarthritis, and calcific tendinitis.
Management of adhesive capsulitis is controversial, and good data for any of the common treatment modalities is lacking. These include NSAIDs, corticosteroids (oral and injected), physical therapy, and acupuncture. Some patients with severe and recalcitrant symptoms may benefit from joint manipulation under general anesthesia or surgical capsular release.55 These decisions will ultimately be made as an outpatient, and the EP should refer any suspected cases of adhesive capsulitis to an orthopedic surgeon. ED treatment should include pain control (NSAID, acetaminophen, and a brief course of opioid analgesics if warranted) and instructions to avoid immobilization and institute early range-of-motion exercises. Consider oral prednisone, starting at 40-60 mg and tapering down by 10 mg every 4-7 days, as this may provide a short-term (6 weeks) improvement in pain and range of motion.56 Ensure underlying medical issues such as diabetes or thyroid disease are well controlled. Remember that if you do elect to treat with steroids, hyperglycemia will be worsened. If the patient does not have a preexisting diagnosis of diabetes, it is reasonable to refer the patient to his or her primary care physician for outpatient screening.
References
- National Hospital Ambulatory Medical Care Survey: 2011 Emergency Department Summary Tables. http://www.cdc.gov/nchs/data/ahcd/nhamcs_emergency/2011_ed_web_tables.pdf.
- FastStats-Emergency Department Visits. www.cdc.gov/nchs/fastats/emergency.department.htm.
- Malik S, Chiampas G, Leonard H. Emergency evaluation of injuries to the shoulder, clavicle, and humerus. Emerg Med Clin N Am 2010;28:739-763.
- Daya M, Nakamura Y. Shoulder. In: Marx JA, et al (eds.) Rosen’s Emergency Medicine: Concepts and Clinical Practice, 7th edition. Philadelphia, PA: Mosby/Elsevier; 2010.
- Simoni P, et al. Imaging of superior labral anterior to posterior (SLAP) tears of the shoulder. J Sports Med Phys Fitness 2012;52(6):622-630.
- Roy A. Rotator cuff disease. Available at http://emedicine.medscape.com/article/328253-overview. June 2009.
- Ewald A. Adhesive capsulitis: A review. Am Fam Physician 2011;83(4):417-422.
- Hermans J, et al. Does this patient with shoulder pain have rotator cuff disease? JAMA 2013;310(8):837-847.
- Which physical exam tests provide clinicians the most value when examining the shoulder? Br J Sports Med 2012;46(14):964-978.
- Luime JJ, et al. Does this patient have an instability of the shoulder or a labrum lesion? JAMA 2004;292(16):1989-1999.
- Edwards SL, et al. Nonoperative treatment of superior labrum anterior posterior tears: Improvements in pain, function, and quality of life. Am J Sports Med 2010;38(7):1456-1461.
- Guanche CA, Jones DC. Clinical testing for tears of the glenoid labrum. Arthroscopy 2003;19(5):517-523.
- Kim AC. Acromioclavicular joint injuries and reconstructions: A review of expected imaging findings and potential complications. Emerg Radiol 2012;19(5):399-413.
- Hendey GW, Chally MK, Stewart VB. Selective radiography in 100 patients with suspected shoulder dislocation. J Emerg Med 2006;31:23–28.
- Orloski J, et al. Do all patients with shoulder dislocations need prereduction x-rays. Am J Emerg Med 2011;29(6):609-612.
- Shuster M, et al. Prospective evaluation of a guideline for the selective elimination of pre-reduction radiographs in clinically obvious anterior shoulder dislocation. CJEM 2002;4:257–262.
- Kahn JH, Mehta SD. The role of post-reduction radiographs after shoulder dislocation. J Emerg Med 2007;33:169-173.
- Ostlere S. Imaging the shoulder. Imaging 2007;19:191-200.
- Vazquez, J, Kassarjian, A. MRI of shoulder trauma. Semin Musculoskel Radiol 2006;10(4):268-283.
- Merchant N, Scalea T, Stein D. Can CT angiography replace conventional bi-planar angiography in the management of severe scapulothoracic dissociation injuries? Am Surgeon 2012;78(8):875-882.
- Reynolds A. Imaging of the injured shoulder. Radiologic Technology 2012;83(3):261-282.
- Hao YD, et al. Evaluation of the clinical significance of classification of traumatic anterior shoulder instability using double contrast computed tomography arthrography. J Int Med Research 2011;39:424–434.
-
Dimai HP, et al. Epidemiology of proximal humeral fractures in Austria between 1989 and 2008. Osteoporos Int 2013;24:
2413–2421. - Christian B, et al. Trends in epidemiology and patho-anatomical pattern of proximal humeral fractures. International Orthopaedics 2014;38:1697–1704.
-
Iyengar JJ, et al. Nonoperative treatment of proximal humerus fractures: A systematic review. J Orthop Trauma 2011;25(10):
612-617. - Court-Brown CM, Garg A, McQueen MM. The epidemiology of proximal humeral fractures. Acta Orthop Scand 2001;72(4):365–371.
-
Clement ND, et al. The outcome of proximal humeral fractures in the elderly: Predictors of mortality and function. The Bone and Joint Journal 2014;96-B(7):
970-977. - Court-Brown CM, Caesar B. Epidemiology of adult fractures: A review. Injury 2006;37(8):691–697.
- Jo MJ, Gardner MJ. Proximal humerus fractures. Curr Rev Musculoskelet Med 2012;5(3):192–198.
- Anglen JO, et al. Avoiding complications in the treatment of humeral fractures. J Bone Joint Surg Am 2008;90(7):1580-1589.
- Carofino BC, Leopold SS. Classifications in brief: The Neer classification for proximal humerus fractures. Clin Orthop Relat Res 2013;471(1):39-43.
- Handoll HG, Ollivere BJ, Rollins KE. Interventions for treating proximal humeral fractures in adults. Cochrane Database Syst Rev 2012;12;12: CD000434.
- Frankle MA. Proximal humerus fractures. http://emedicine.medscape.com/article/1261320. April 2013.
- Torrens C, et al. Functional and quality-of-life results of displaced and nondisplaced proximal humeral fractures treated conservatively. J Orthop Trauma 2011;25(10):581-587.
- Bontempo NA, Mazzocca AD. Sternoclavicular, clavicular, and acromioclavicular injuries. In: O’Connor F, et al (eds.) ACSM’s Sports Medicine: A Comprehensive Review 2013 American College of Sports Medicine:323-346.
- Kim AC, et al. Acromioclavicular joint injuries and reconstructions: A review of expected imaging findings and potential complications. Emerg Radiol 2012;19(5):399-413.
- Orchard JW, et al. Long-term safety of using local anesthetic injections in professional rugby league. Am J Sports Med 2010;38(11):2259-2266.
- Smith TO, et al. Operative versus non-operative management following Rockwood grade III acromioclavicular separation: A meta-analysis of the current evidence base. J Orthop Traumatol 2011;2(1):19–27.
- Kashif Khan LA, Bradnock TJ, Scott C, et al. Fractures of the clavicle. J Bone Joint Surg Am 2009;91(2):447-460.
- Mouzopoulos G, et al. Complications of clavicle fracture and acromioclavicular: What the general surgeon should know. Chirurgia 2008;103(5):509-512.
- McKee MD, et al. Deficits following nonoperative treatment of displaced midshaft clavicular fractures. J Bone Joint Surg Am 2006;88:35-40.
- Virtanen KJ, et al. Operative and nonoperative treatment of clavicle fractures in adults: A systematic review of 1,190 patients from the literature. Acta Orthop 2012;83(1):65–73.
- Bontempo NA, Mazzocca AD. Biomechanics and treatment of acromioclavicular and sternoclavicular joint injuries. Br J Sports Med 2010;44(5):361.
- Deren ME, et al. Posterior sternoclavicular dislocations: A brief review and technique for closed management of a rare but serious injury. Orthopedic Reviews 2014;6(1):10-14.
- Balcik BJ, Monseau AJ, Krantz W. Evaluation and treatment of sternoclavicular, clavicular, and acromioclavicular injuries. Orthopedics, Primary Care: Clinics in Office Practice 2013;40(4):911-923.
- Glass ER, et al. Treatment of sternoclavicular joint dislocations: A systematic review of 251 dislocations in 24 case series. Journal of Trauma-Injury Infection and Critical Care 2011;70(5):1294-1298.
- Bicos J, Nicholson GP. Treatment and results of sternoclavicular joint injuries. Clin Sports Med 2003;22:359–370.
- Groh GI, Wirth MA. Management of traumatic sternoclavicular joint injuries. J Am Acad Orthopedic Surgeons 2011;19(1):1-7.
- Sorensen AK, et al. Acute rotator cuff tear: Do we miss the early diagnosis? A prospective study showing a high incidence of rotator cuff tears after shoulder trauma. J Shoulder Elbow Surg 2007;16(2):174-180.
- Quillen DM, Wuchner M, Hatch RL. Acute shoulder injuries. Am Fam Physician 2004;70(10):1947-1954.
- Churgay CA. Diagnosis and treatment of biceps tendinitis and tendinosis. Am Fam Physician 2009;80(5):470-476.
- O’Kane JW, Toresdahl BG. The evidence based shoulder evaluation. Curr Sports Med Rep 2014;13(5):307-313.
- Matthieu JC, et al. Detection of rotator cuff tears: The value of MRI following ultrasound. Eur Radiol 2010;20(2):450–457.
- Harris G, et al. Adhesive capsulitis: Review of imaging and treatment. J Med Imaging Radiation Oncol 2013;57(6):633–643.
- Buchbinder R, et al. Oral steroids for shoulder pain (adhesive capsulitis). Cochrane Database 2009; www.cochrane.org/CD006189/MUSKEL_oral-steroids-for-shoulder-pain-adhesive-capsulitis.
MONOGRAPH: Musculoskeletal injuries or pain complaints comprise a large portion of visits to EDs every year.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
