Bronchiolitis
Authors
Daniel Migliaccio, MD,
Stanford/Kaiser Residency Program,
Stanford, CA
Daniel Imler, MD,
Assistant Professor,
Pediatric Emergency Medicine,
Pediatric Hospital Medicine,
Stanford School of Medicine,
Stanford CA
N. Ewen Wang, MD,
Associate Professor Surgery (Emergency Medicine),
Associate Director Pediatric Emergency Medicine,
Stanford School of Medicine,
Stanford CA
Peer Reviewer
Aaron Leetch, MD,
Assistant Professor,
Departments of Emergency Medicine and Pediatrics;
Associate Program Director,
Emergency Medicine/Pediatrics Residency,
University of Arizona,
Tucson, AZ
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Dietrich (editor), Dr. Skrainka (CME question reviewer), Dr. Migliaccio (author), Dr. Imler (author), Dr. Wang (author), Dr. Leetch (peer reviewer), Ms. Coplin (executive editor), and Ms. Hamlin (managing editor) report no relationships with companies related to the field of study covered by this CME activity.
Executive Summary
">Bronchiolitis is a common clinical condition encountered by practitioners. In 2014 the American Academy of Pediatrics endorsed and updated the clinical practice guideline for the diagnosis, testing, and management of bronchiolitis with significant changes in recommendations for the evaluation and treatment of these children. The authors present a thorough review of these guidelines to assist the practicing clinician with an understanding of the current national standard for care of these patients.
— Ann M. Dietrich, MD, Editor
Case: A 10-month-old female presents to the emergency department (ED) with a fever, cough, and copious rhinorrhea. She has been febrile to 38.5° C (101.3° F). Oxygen saturation is 89% on room air while asleep. On physical exam she has significant rhinorrhea. Auscultation of the lungs demonstrates diffuse wheezes and crackles. Chest X-ray shows increased atelectasis in the lower lobes.
What evaluation is necessary? Is laboratory testing or a urinalysis needed? Are pediatric bronchiolitis algorithms useful in determining the course of evaluation? Is a chest X-ray indicated? What treatments work? What should we consider trying in the ED? Which patients should be admitted? Is there a subset of patients at risk for apnea?
Definition and Etiology
Bronchiolitis is an acute inflammatory process of the lower respiratory system occurring mostly in children between the ages of 1 month and 2 years. The most commonly implicated pathogen is the respiratory syncytial virus (RSV). However, multiple other pathogens can lead to the same constellation of symptoms, including adenovirus, bocavirus, human metapneumovirus, influenza virus, and parainfluenza virus.1
Epidemiology
Bronchiolitis is the most common cause of hospitalization among infants during the first year of life. Approximately 100,000 bronchiolitis admissions occur annually in the United States.2 According to the Centers for Disease Control and Prevention, almost all children will have an RSV infection by the time they are 2 years old, with 25-40% demonstrating signs or symptoms of respiratory illness.3 Bronchiolitis most commonly affects children younger than 2 years of age. However, adults — especially the elderly, immunocompromised, and adults with lung disease — can be infected with RSV and demonstrate a range of illness from simple upper respiratory symptoms to pneumonia and respiratory failure.4
A prospective, population-based study found an average RSV hospitalization rate of 5.2 per 1000 children younger than 24 months of age between the years 2000-2005, with age being the most important risk factor for hospitalization.5 The highest age-specific rate of RSV hospitalization occurred between 30 days and 60 days of age (25.9 per 1000 children). The admission rate was found to be similar in term vs preterm infants (< 37 weeks’ gestational age), although for extreme preterm infants (< 32 weeks’ gestational age), there was an inverse relationship between gestational age and hospital admission (13.9% vs 4.4% for infants born at ≤ 26 weeks’ gestation vs those born at 30-32 weeks’ gestation, respectively).
Other children at risk for hospitalization from acute bronchiolitis include children with congenital heart disease, as well as those with chronic lung disease, as both populations have diminished pulmonary reserve.6 Children with compromised immune function are also more likely candidates for hospital admission from bronchiolitis.7
Pathophysiology
Although the most common virus implicated in bronchiolitis is RSV, more than 30% of patients will have multiple pathogens identified.8,9 The disease process typically begins with an acute upper respiratory tract infection and spreads to the lower airways within a few days. The infection results in small airway inflammation, edema, increased mucus production, and eventual epithelial cell necrosis. This response causes airflow obstruction and atelectasis leading to an increased work of breathing along with the symptoms of wheezing, crackles, and/or rales.10
RSV was first isolated in 1956 from a chimpanzee and was initially known as the chimpanzee coryza agent; it came to be known as RSV to reflect the giant cells or syncytia that formed among respiratory cells infected with the virus. However, humans are the only known reservoir of the virus.11 Human RSV is an enveloped RNA virus and is a member of the family Paramyxoviridae. Infection is normally confined to the respiratory mucosa, as the virus has a predilection for respiratory cells. The virus is spread primarily via person-to-person contact (with respiratory secretions) and can live on environmental surfaces for up to 8 hours. Immunity to reinfection, even with the same strain of RSV, is incomplete and short-lived, with re-infections from antigenically similar strains occurring throughout life.12 Secondary RSV infections tend to be milder, which suggests at least partial immunity.13 However, severe disease can still occur in young children from a secondary RSV infection, indicating that age is the most important factor in disease severity.14
An unsuccessful attempt to create a vaccine against RSV occurred in the 1960s, using a formalin-inactivated-RSV (FI-RSV) vaccine. Children who were inoculated with the FI-RSV vaccine had an exaggerated immune response and had a far higher incidence of severe disease, with two deaths occurring secondary to vaccination.15 Recently palivizumab, a genetically engineered humanized monoclonal antibody, has been used for passive immunization in certain populations. It is crucial to note that while prophylaxis decreases the risk of hospitalization with RSV in these children, significant disease can still occur.16
Apnea occurs in a small number of children with RSV, with a rate of approximately 3%.17 Apnea usually occurs within the first 2-3 days after the onset of typical upper respiratory infection symptoms, such as rhinorrhea and cough.18 However, the cause of apnea remains unknown. Proposed mechanisms include local pulmonary neurotransmitters19 as well as disruptions in the neural control pathways.20 The risk of apnea in children with RSV is related to age. In a retrospective study, Willwerth et al developed certain clinical risk criteria to seek out those infants who are at risk of apnea and require admission.18 The criteria they used to determine high risk for apnea include 1) born at full term and were younger than 1 month, 2) born preterm and younger than 48 weeks post-conception, or 3) the child’s parents or a clinician had already witnessed an apnea episode with this illness before inpatient admission. They found that 19 of 691 patients had apnea during hospitalization and all were identified by the above risk criteria (100% sensitivity; 1-sided 97.5% confidence interval 82% to 100%), with a 100% negative predictive value, as none of the infants considered low risk for apnea went on to develop apnea. Apnea, in turn, has been associated with increased risk for prolonged hospitalization, intensive care admissions, and mechanical ventilation.21
Clinical Course
The typical progression of bronchiolitis consists of a viral prodrome with rhinitis, fever, and cough. Subsequently, the child develops increased respiratory effort secondary to the lower airway edema and mucus obstruction. This can present as audible grunting, nasal flaring, and/or intercostal/subcostal retractions. On physical exam, these children typically have varying degrees of tachypnea, hypoxemia, wheezing, and crackles. These symptoms typically peak within 3-4 days of symptom onset. Mean resolution of fever is 5 days and cough between days 5-15 (90% resolved by day 21). The mean resolution of symptoms is about 12 days, with the last symptom to dissipate being the excess mucus production.22 Symptoms of bronchiolitis are dynamic and are largely due to mucus plugging and inflammation of the airways. Thus, children need continued pulmonary toilet and reassessment in the ED. The dynamic nature of the illness can explain why it has been difficult to correlate pulse oximetry readings to disease severity.23 In fact, pulse oximetry in the clinical assessment of children has actually led to increased hospital length of stay without being able to predict clinical outcomes.24 However, most emergency medicine physicians believe it is reasonable to admit infants with oxygen saturation that is persistently below 88% while asleep and 90% while awake after observation in the ED.
Fortunately, severe adverse clinical outcomes, such as respiratory failure requiring intubation and mechanical ventilation, are rare and range from 3 to 5 per 100,000 children.25,26,27
Diagnostic Studies
The American Academy of Pediatrics (AAP) endorses that the diagnosis of bronchiolitis is purely clinical. The AAP updated the clinical practice guideline for the diagnosis, testing, and management of bronchiolitis in 2014.28 The use of chest X-ray is common in the workup of bronchiolitis, but it is not recommended by the AAP, as they do not correlate with disease severity and do not guide management (see Figure 1).29 Shuh et al found that performing a chest X-ray in children with bronchiolitis made physicians more likely to treat with antibiotics.30 Atelectasis, which is common in viral bronchiolitis, may be misinterpreted as consolidation and treated as pneumonia (see Figure 2). However, a chest X-ray may be indicated when the diagnosis of bronchiolitis is uncertain or the presentation is atypical/the patient is very ill (respiratory failure). Specifically, a chest X-ray is useful when there is no prodromal history or there is concern for a foreign body aspiration.
|
Figure 1. Radiograph of Infant with Bronchiolitis |
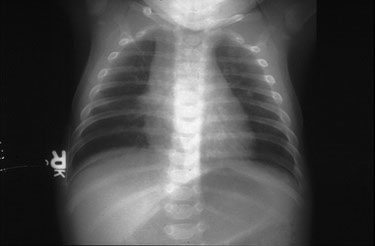 |
|
Figure 2. Radiograph of Infant with Bronchiolitis and Atelectasis |
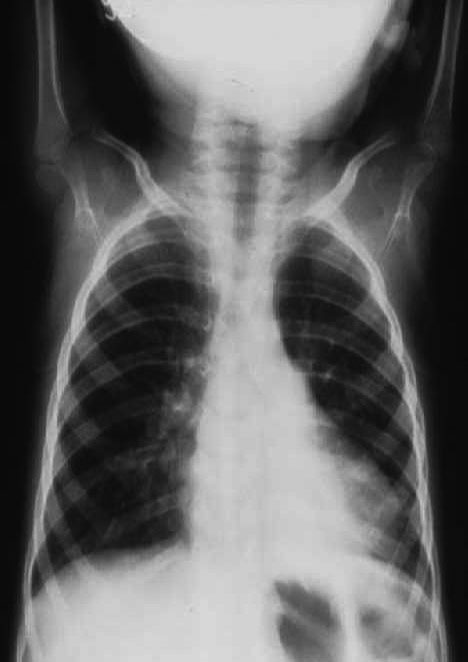 |
In contrast, testing for serious bacterial infection concomitant with bronchiolitis still remains controversial. It is well-accepted that infants younger than 30 days of age with fever necessitate a full septic workup (including a lumbar puncture) and empiric antibiotics, as the risk of serious bacterial illness (SBI) in this population is substantial.31 Infants older than 60 days of age with bronchiolitis may have a decreased risk of concomitant serious bacterial infection and may not warrant cultures and extensive testing.32 Levine et al found an overall decreased risk of SBI in RSV-positive infants as compared to RSV-negative infants. However, the workup of infants who presented between 30-60 days of life remains in the “gray zone.”33,34 The most implicated infection that has been associated with RSV bronchiolitis has been urinary tract infections (UTIs).35 Kuppermann et al found a 2% prevalence of urinary tract infection with concomitant RSV infection. However, this is similar to the baseline rate of culture-positive urine in asymptomatic children under the age of 3 years, randomly selected for testing.36 Similarly, Ralston et al found the rate of UTI to be 1% in children with bronchiolitis.37
In addition, the AAP endorses that viral serology testing is not routinely recommended in the workup of children with bronchiolitis, as it does not alter clinical management.23,38 A recent Cochrane review found that immunofluorescence or polymerase chain reaction (PCR) did not lead to changes in antibiotic use, ED length of stay, or clinically relevant changes in outcomes.39 In addition, the children who are thought to have bronchiolitis will require isolation regardless of the virus involved. However, a positive viral test is useful in admitted infants; the probability of bacterial infection is decreased and, in theory, this would reduce the incidence of unnecessary antibiotics.40 If diagnostic studies are to be conducted, respiratory virus PCR testing for common pathogens provides the greatest sensitivity, specificity, and convenience (see Table 1).41 Further, the AAP states that infants who are receiving monthly palivizumab prophylaxis and are hospitalized should be tested, as a breakthrough RSV infection would lead to discontinuation of the drug.
|
Table 1. Testing for Common Pathogens |
|||||
|
Test |
Sensitivity |
Specificity |
Optimal Timing |
Advantages |
Disadvantages |
|
RT- PCR |
72-94% |
95-100% |
Within 1 week |
More rapid/sensitive than viral cultures, 1-2 days. |
High limits of detection |
|
Direct fluorescent antibody testing (DFA) |
80% |
94-99% |
Within 1 week |
Results within 30- 60 minutes |
Not readily available Human error, fading of dyes |
|
Viral culture |
40-60% |
100% |
Within 4 days |
Very specific |
Low sensitivity, 7-10 day delay between specimen collection and diagnosis |
|
Adapted from: Current Best Practices for Respiratory Virus Testing41 |
|||||
|
Rapid antigen direct tests (RADTs) |
50-98% |
93-99% |
Within 3 days |
Results within 15-30 minutes |
Lower sensitivity than RT-PCR |
Clinical Prediction Rules for Disease Severity and Admission
Children’s hospitals across the nation have adopted different scoring systems in an attempt to streamline decision making in the management of bronchiolitis. Namely, they attempt to quantify respiratory distress utilizing such parameters as respiratory rate, accessory muscle use, wheezing, cyanosis, and oxygen saturation. The AAP does not endorse any particular scoring system, as studies attempting to determine scoring system validity have failed to demonstrate significant construct validity.42,43 For instance, McCallum et al present 15 different scoring systems, only five of which had any validation, limited to inter-rater agreement. Table 2 includes an example of the scoring system used at Stanford University Hospital with the acronym W.A.R.M. (Wheeze, Air Exchange, Respiratory rate, Muscle use) and it will be used in the disposition algorithm presented in this paper.44,45
|
Table 2. W.A.R.M. Score |
|||
|
Variable |
0 Points |
1 Point |
2 Points |
|
Air Exchange (assess all 4 chest areas; left/right front and left/right back) |
Normal |
One area decreased |
More than one area decreased |
|
Respiratory rate |
|||
|
≤ 2 months |
≤ 60 |
> 60 |
|
|
2-12 months |
≤ 50 |
> 50 |
|
|
1-2 years |
≤ 40 |
> 40 |
|
|
Muscle Use/Retractions |
None |
Subcostal or intercostal |
2 of the following: subcostal, intercostal, substernal OR nasal flaring, trachial tugging, or abdominal breathing |
|
Adapted from: Cincinnati Children’s Hospital and clinical pathway from curbsideup.com 44,45 |
|||
|
Wheeze |
None |
End expiratory |
Entire expiratory/any inspiratory |
Management
It is important to first consider the ABCs (airway, breathing, and circulation) in children who have respiratory symptoms. Once the diagnosis of bronchiolitis is established, the AAP clinical guidelines have given clear recommendations regarding treatment. The therapeutic interventions that have been used in the past are many and include bronchodilators, corticosteroids, antibiotics and antivirals, hypertonic saline, and nasal suction. The AAP emphasizes supportive care, including suctioning, oxygenation, and hydration in their newly published guidelines.28 The management pathway presented in this paper is adopted from Dr. Dan Imler, pediatric emergency medicine physician at the Lucille Packard Children’s Hospital pediatric department. Lastly, it is important to provide materials at discharge, including thorough return precautions and techniques for suctioning the child at home. These instructions should stress adequate hydration and monitoring of the child’s work of breathing. One technique that can be offered is to utilize 2-3 drops of warm water placed in each nostril prior to bulb suctioning and repeat multiple times.
I. Bronchodilators
It has been common practice to provide a “trial” of albuterol in children with suspected bronchiolitis. However, the 2014 AAP guidelines discourage the use of albuterol in patients diagnosed with bronchiolitis. Multiple meta-analyses and systematic reviews have demonstrated that while bronchodilators may improve clinical symptom scores, they do not affect disease resolution, need for admission to the hospital, or length of stay (LOS).1,46 As per the AAP, “Although it is true that a small subset of children with bronchiolitis may have reversible airway obstruction resulting from smooth muscle constriction, attempts to define a subgroup of responders have not been successful to date.” The AAP holds strongly to the principle of bronchiolitis being a clinical diagnosis, and does not recommend a trial of albuterol as a diagnostic test. A recent Cochrane review of the available data on the use of beta-agonists for children with recurrent wheezing presenting with bronchiolitis demonstrated no clear benefit in this population.47 Of note, children with severe disease were often excluded from these trials. In these patients, treatment with beta-agonists may be indicated depending on the clinical scenario.
II. Racemic Epinephrine
Multiple meta-analyses have found no evidence to support the use of epinephrine in the treatment of bronchiolitis.48 This is further supported by large randomized, controlled trials, and the AAP endorses against utilization of epinephrine in the treatment of bronchiolitis.48,49
II. Corticosteroids
The use of steroids in children diagnosed with bronchiolitis seems intuitive considering the largely inflammatory nature of bronchiolitis. In fact, two recent studies have shown a decreased LOS with administration of steroids.50,51 Moreover, in children with preexisting asthma/recurrent wheezing, limited evidence demonstrates a decreased LOS.51 However, in large studies and reviews, systemic glucocorticoids and combination bronchodilators-glucocorticoids do not improve hospitalization rates or disease progression.52,53 Thus, their use is not recommended by the AAP.
III. Nebulized Hypertonic Saline
The relative cost and safety of nebulized hypertonic saline has made it a topic of recent debate. In theory, hypertonic saline breaks up the mucus and pulls fluid in from the vascular system, thinning secretions while also irritating the airways and stimulating coughing.54 A Cochrane review performed by Zhang et al found a significantly reduced LOS (by 1.2 days) and improved clinical severity score.55 However, there are numerous other studies that demonstrate that it does not improve hospitalization rates or disease progression.56,57 Therefore, its use is not recommended by the AAP guidelines in the emergency department, but it may be considered in the inpatient setting.
IV. Antibiotics/antivirals
As previously mentioned, the risk of SBI, such as bacteremia, meningitis, and urinary tract infection, is rare in children diagnosed with bronchiolitis.37,58 Therefore, the AAP strongly recommends against the use of antibiotics in these children. Antibiotics are only indicated if a concomitant bacterial infection is suspected utilizing features in the patient history and physical exam.59,60 However, children who present with severe bronchiolitis and are critically ill, such as those in respiratory failure, may warrant empiric antibiotics.61 Similarly, the AAP recommends against the use of ribavirin in children, as research regarding the efficacy of the drug on positive clinical outcomes remains ambiguous.62
V. Special Populations
Morbidity and mortality in bronchiolitis are highest in premature infants and children with underlying medical illnesses. These children may warrant a trial of the aforementioned treatments depending on the clinical scenario. Moreover, some of these children may benefit from passive immunization with palivizumab. However, its cost and need for monthly injections make it inopportune to use in the general population.
A. Prematurity — According to the AAP, monthly palivizumab prophylaxis should be given to infants born before 29 weeks’ gestation, as the risk for hospitalization equalizes after that age.63
B. Congenital heart disease/chronic lung disease — Although there is limited evidence regarding the benefit of prophylaxis in children with congenital heart disease, the AAP recommends its use in children with “hemodynamically significant heart disease.”16 In addition, it recommends prophylaxis for infants younger than 1 year of age who develop chronic lung disease of prematurity.
C. Other conditions — There is insufficient research to endorse use of prophylaxis in children with Down syndrome,64 cystic fibrosis,65 neuromuscular disease,66 or children who are immunocompromised.67 The decision to provide prophylaxis in these children should be reviewed on a case-by-case basis.
Disposition
Many scoring criteria have been created to facilitate the decision to discharge or admit children with bronchiolitis similar to that proposed in the pathway (see Figure 3, which displays a summary of various criteria used by Hospital for Sick Children, Cincinnati’s Children’s Hospital Medical Center, Lucille Packard’s Children’s Hospital, and the AAP).68,69,70 It is extremely important to assess the ability of the child to feed and maintain good hydration. If there is continued difficulty in being able to stay well-hydrated after therapy, intravenous fluid therapy and hospitalization should be considered. Similarly, the physician needs to assess the ability of the family to care for the child and return for further care. (See Table 3.)
|
Figure 3. Scoring Criteria to Discharge or Admit Children with Bronchiolitis44,45 |
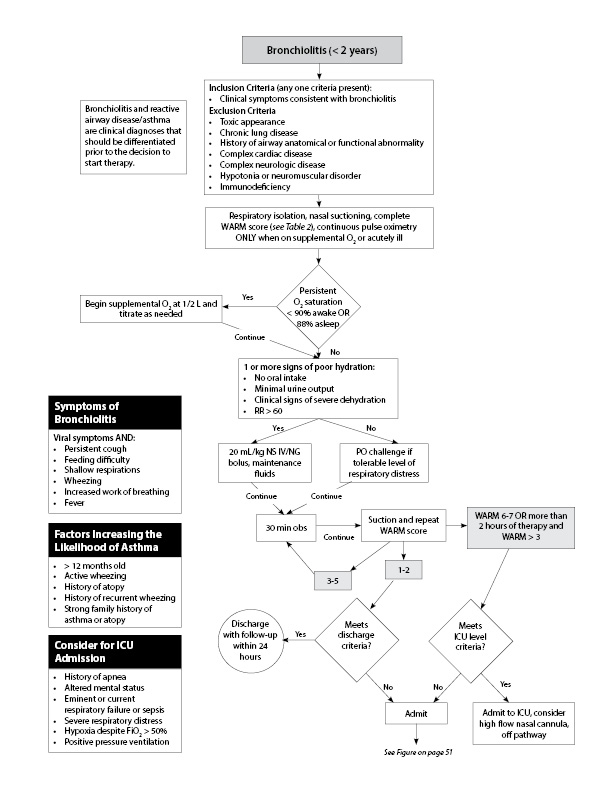 |
|
Figure 3. Scoring Criteria to Discharge or Admit Children with Bronchiolitis44,45 (cont.) |
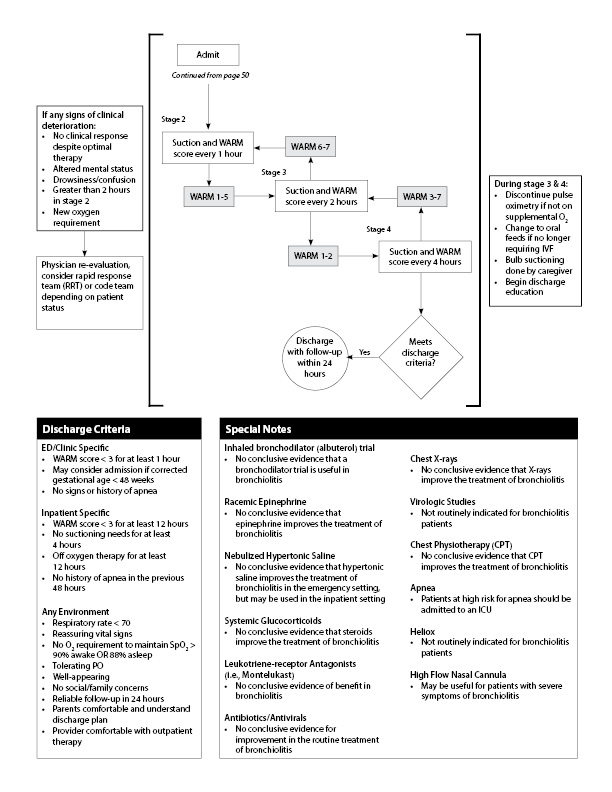 |
|
Table 3. Guide to Disposition of Bronchiolitis Patients |
|
|
Consider hospitalization |
|
|
Consider critical care admission |
|
Conclusion
Indeed, the evaluation and treatment of bronchiolitis continues to differ significantly among practitioners. However, adherence to the AAP clinical practice guideline can minimize unnecessary diagnostic testing and unproductive and sometimes costly treatments. Following the path set out by the AAP ensures the use of evidence-based practice in the management of children with bronchiolitis.
References
- Wainwright C. Acute viral bronchiolitis in children — a very common condition with few therapeutic options. Paediatr Respir Rev 2010;11:39-45; quiz 45.
- Hasegawa K, Tsugawa Y, Brown DF, et al. Trends in bronchiolitis hospitalizations in the United States, 2000-2009. Pediatrics 2013;132:28-36.
- Centers for Disease Control and Prevention. Respiratory Syncytial Virus Infection [press release]. 2014.
- van Asten L, van den Wijngaard C, van Pelt W, et al. Mortality attributable to 9 common infections: Significant effect of influenza A, respiratory syncytial virus, influenza B, norovirus, and parainfluenza in elderly persons. J Infect Dis 2012;206:628-639.
- Bueno SM, Gonzalez PA, Cautivo KM, et al. Protective T cell immunity against respiratory syncytial virus is efficiently induced by recombinant BCG. Proc Natl Acad Sci U S A 2008;105:20822-20827.
- Ricart S, Marcos MA, Sarda M, et al. Clinical risk factors are more relevant than respiratory viruses in predicting bronchiolitis severity. Pediatr Pulmonol 2013;48:456-463.
- Prescott WA, Jr., Hutchinson DJ. Respiratory syncytial virus prophylaxis in special populations: Is it something worth considering in cystic fibrosis and immunosuppression? J Pediatr Pharmacol Ther 2011;16:77-86.
- Brand HK, de Groot R, Galama JM, et al. Infection with multiple viruses is not associated with increased disease severity in children with bronchiolitis. Pediatr Pulmonol 2012;47:393-400.
- Stempel HE, Martin ET, Kuypers J, et al. Multiple viral respiratory pathogens in children with bronchiolitis. Acta Paediatr 2009;98:123-126.
- Choi J, Lee GL. Common pediatric respiratory emergencies. Emerg Med Clin North Am 2012;30:529-563, x.
- Collins PL, Graham BS. Viral and host factors in human respiratory syncytial virus pathogenesis. J Virol 2008;82:2040-2055.
- Lambert L, Sagfors AM, Openshaw PJ, Culley FJ. Immunity to RSV in early-life. Front Immunol 2014;5:466.
- Hall CB, Walsh EE, Long CE, Schnabel KC. Immunity to and frequency of reinfection with respiratory syncytial virus. J Infect Dis 1991;163:693-698.
- Ohuma EO, Okiro EA, Ochola R, et al. The natural history of respiratory syncytial virus in a birth cohort: The influence of age and previous infection on reinfection and disease. Am J Epidemiol 2012;176:794-802.
- Murata Y. Respiratory syncytial virus vaccine development. Clin Lab Med 2009;29:725-739.
- Hampp C, Kauf TL, Saidi AS, Winterstein AG. Cost-effectiveness of respiratory syncytial virus prophylaxis in various indications. Arch Pediatr Adolesc Med 2011;165:498-505.
- Ralston S, Hill V. Incidence of apnea in infants hospitalized with respiratory syncytial virus bronchiolitis: A systematic review. J Pediatr 2009;155:728-733.
- Willwerth BM, Harper MB, Greenes DS. Identifying hospitalized infants who have bronchiolitis and are at high risk for apnea. Ann Emerg Med 2006;48:441-447.
- Balzamo E, Joanny P, Steinberg JG, et al. Mechanical ventilation increases substance P concentration in the vagus, sympathetic, and phrenic nerves. Am J Resp Crit Care Med 1996;153:153-157.
- Kawashima H, Kashiwagi Y, Ioi H, et al. Production of chemokines in respiratory syncytial virus infection with central nervous system manifestations. J Infect Chemother 2012;18:827-831.
- Wang EE, Law BJ, Stephens D. Pediatric Investigators Collaborative Network on Infections in Canada (PICNIC) prospective study of risk factors and outcomes in patients hospitalized with respiratory syncytial viral lower respiratory tract infection. J Pediatr 1995;126:212-219.
- Petruzella FD, Gorelick MH. Duration of illness in infants with bronchiolitis evaluated in the emergency department. Pediatr 2010;126:285-290.
- Mansbach JM, Piedra PA, Teach SJ, et al. Prospective multicenter study of viral etiology and hospital length of stay in children with severe bronchiolitis. Arch Pediatr Adolesc Med 2012;166:700-706.
- Schroeder AR, Marmor AK, Pantell RH, Newman TB. Impact of pulse oximetry and oxygen therapy on length of stay in bronchiolitis hospitalizations. Arch Pediatr Adolesc Med 2004;158:527-530.
- Thompson WW, Shay DK, Weintraub E, et al. Mortality associated with influenza and respiratory syncytial virus in the United States. JAMA 2003;289:179-186.
- Chan PW, Lok FY, Khatijah SB. Risk factors for hypoxemia and respiratory failure in respiratory syncytial virus bronchiolitis. Southeast Asian J Trop Med Public Health 2002;33:806-810.
- Mansbach JM, Piedra PA, Stevenson MD, et al. Prospective multicenter study of children with bronchiolitis requiring mechanical ventilation. Pediatrics 2012;130:e492-500.
- Ralston SL, Lieberthal AS, Meissner HC, et al. Clinical practice guideline: The diagnosis, management, and prevention of bronchiolitis. Pediatrics 2014;134:e1474-1502.
- Swingler GH, Hussey GD, Zwarenstein M. Randomised controlled trial of clinical outcome after chest radiograph in ambulatory acute lower-respiratory infection in children. Lancet 1998;351:404-408.
- Schuh S, Lalani A, Allen U, et al. Evaluation of the utility of radiography in acute bronchiolitis. J Pediatr 2007;150:429-433.
- Bilavsky E, Shouval DS, Yarden-Bilavsky H, et al. A prospective study of the risk for serious bacterial infections in hospitalized febrile infants with or without bronchiolitis. Pediatr Infect Dis J 2008;27:269-270.
- Levine DA, Platt SL, Dayan PS, et al. Risk of serious bacterial infection in young febrile infants with respiratory syncytial virus infections. Pediatr 2004;113:1728-1734.
- Purcell K, Fergie J. Concurrent serious bacterial infections in 2396 infants and children hospitalized with respiratory syncytial virus lower respiratory tract infections. Arch Pediatr Adolesc Med 2002;156:322-324.
- Liebelt EL, Qi K, Harvey K. Diagnostic testing for serious bacterial infections in infants aged 90 days or younger with bronchiolitis. Arch Pediatr Adolesc Med 1999;153:525-530.
- Kuppermann N, Bank DE, Walton EA, et al. Risks for bacteremia and urinary tract infections in young febrile children with bronchiolitis. Arch Pediatr Adolesc Med 1997;151:1207-1214.
- Kaluarachchi D, Kaldas V, Roques E, et al. Comparison of urinary tract infection rates among 2- to 12-month-old febrile infants with RSV infections using 1999 and 2011 AAP diagnostic criteria. Clin Pediatr 2014;53:742-746.
- Ralston S, Hill V, Waters A. Occult serious bacterial infection in infants younger than 60 to 90 days with bronchiolitis: a systematic review. Arch Pediatr Adolesc Med 2011;165:951-956.
- Bordley WC, Viswanathan M, King VJ, et al. Diagnosis and testing in bronchiolitis: a systematic review. Arch Pediatr Adolesc Med 2004;158:119-126.
- Stollar F, Alcoba G, Gervaix A, Argiroffo CB. Virologic testing in bronchiolitis: does it change management decisions and predict outcomes? Eur J Pediatr 2014;173:1429-1435.
- Ferronato AE, Gilio AE, Ferraro AA, et al. Etiological diagnosis reduces the use of antibiotics in infants with bronchiolitis. Clinics 2012;67:1001-1006.
- Doan Q, Enarson P, Kissoon N, et al. Rapid viral diagnosis for acute febrile respiratory illness in children in the emergency department. Cochrane Database System Rev 2012;5:CD006452.
- McCallum GB, Morris PS, Wilson CC, et al. Severity scoring systems: are they internally valid, reliable and predictive of oxygen use in children with acute bronchiolitis? Pediatr Pulmonol 2013;48:797-803.
- Destino L, Weisgerber MC, Soung P, et al. Validity of respiratory scores in bronchiolitis. Hosp Pediatr 2012;2:202-209.
- Imler D. Bronchiolitis 2015; Available at: http://curbsideup.com/path.asp?pathID=27.
- WARM Respiratory Scoring Tool [press release]. Available at: http://www.cincinnatichildrens.org/WorkArea/DownloadAsset.aspx?id=878872010.
- Zorc JJ, Hall CB. Bronchiolitis: Recent evidence on diagnosis and management. Pediatr 2010;125:342-349.
- Chavasse R, Seddon P, Bara A, McKean M. Short acting beta agonists for recurrent wheeze in children under 2 years of age. Cochrane Database System Rev. 2002(3):CD002873.
- Skjerven HO, Hunderi JO, Brugmann-Pieper SK, et al. Racemic adrenaline and inhalation strategies in acute bronchiolitis. N Engl J Med 2013;368:2286-2293.
- Wainwright C, Altamirano L, Cheney M, et al. A multicenter, randomized, double-blind, controlled trial of nebulized epinephrine in infants with acute bronchiolitis. N Engl J Med 2003;349:27-35.
- Garrison MM, Christakis DA, Harvey E, et al. Systemic corticosteroids in infant bronchiolitis: A meta-analysis. Pediatr 2000;105:E44.
- Alansari K, Sakran M, Davidson BL, et al. Oral dexamethasone for bronchiolitis: A randomized trial. Pediatr 2013;132:e810-816.
- Fernandes RM, Bialy LM, Vandermeer B, et al. Glucocorticoids for acute viral bronchiolitis in infants and young children. Cochrane Database System Rev 2013;6:CD004878.
- Corneli HM, Zorc JJ, Mahajan P, et al. A multicenter, randomized, controlled trial of dexamethasone for bronchiolitis. N Engl J Med 2007;357:331-339.
- Ralston S, Hill V, Martinez M. Nebulized hypertonic saline without adjunctive bronchodilators for children with bronchiolitis. Pediatr 2010;126:e520-525.
- Zhang L, Mendoza-Sassi RA, Wainwright C, Klassen TP. Nebulized hypertonic saline solution for acute bronchiolitis in infants. Cochrane Database System Rev 2008(4):CD006458.
- Wu S, Baker C, Lang ME, et al. Nebulized hypertonic saline for bronchiolitis: a randomized clinical trial. JAMA Pediatr 2014;168:657-663.
- Grewal S, Klassen TP. The tale of 2 trials: Disentangling contradictory evidence on hypertonic saline for acute bronchiolitis. JAMA Pediatr 2014;168:607-609.
- Farley R, Spurling GK, Eriksson L, Del Mar CB. Antibiotics for bronchiolitis in children under two years of age. Cochrane Database System Rev 2014;10:CD005189.
- Pinto LA, Pitrez PM, Luisi F, et al. Azithromycin therapy in hospitalized infants with acute bronchiolitis is not associated with better clinical outcomes: a randomized, double-blinded, and placebo-controlled clinical trial. J Pediatr 2012;161:1104-1108.
- McCallum GB, Morris PS, Chang AB. Antibiotics for persistent cough or wheeze following acute bronchiolitis in children. Cochrane Database System Rev 2012;12:CD009834.
- Levin D, Tribuzio M, Green-Wrzesinki T, et al. Empiric antibiotics are justified for infants with respiratory syncytial virus lower respiratory tract infection presenting with respiratory failure: a prospective study and evidence review. Pediatr Crit Care Med 2010;11:390-395.
- Ventre K, Randolph AG. Ribavirin for respiratory syncytial virus infection of the lower respiratory tract in infants and young children. Cochrane Database System Rev 2007(1):CD000181.
- Hall CB, Weinberg GA, Blumkin AK, et al. Respiratory syncytial virus-associated hospitalizations among children less than 24 months of age. Pediatr 2013;132:e341-348.
- Megged O, Schlesinger Y. Down syndrome and respiratory syncytial virus infection. Pediatr Infect Dis J 2010;29:672-673.
- Robinson KA, Odelola OA, Saldanha IJ, McKoy NA. Palivizumab for prophylaxis against respiratory syncytial virus infection in children with cystic fibrosis. Cochrane Database System Rev 2013;6:CD007743.
- Giusti R. North American synagis prophylaxis survey. Pediatric Pulmonol 2009;44:96-98.
- El Saleeby CM, Somes GW, DeVincenzo JP, Gaur AH. Risk factors for severe respiratory syncytial virus disease in children with cancer: The importance of lymphopenia and young age. Pediatr 2008;121:235-243.
- Clinical Practice Guideline. Management of Bronchiolitis in Infants. [press release]. 2011.
- Cincinnati Children’s Hospital Medical Center: Evidence-based care guideline for management of bronchiolitis in infants 1 year of age or less with a first time episode, Bronchiolitis Pediatric Evidence-Based Care Guidelines [press release]. 2010.
- Lucille Packard’s Children’s Hospital. Bronchiolitis Guidelines. [press release]. 2009.
MONOGRAPH: A thorough review of guidelines to assist in the care of patients with this debilitating condition.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
