Intussusception and Midgut Volvulus
Authors
Jessica A. Stanich, MD, Resident Physician, Emergency Medicine, Mayo Clinic, Rochester, MN
M. Fernanda Bellolio, MD, MS, Assistant Professor of Emergency Medicine, Associate Research Chair, Department of Emergency Medicine, Mayo Clinic, Rochester, MN
Peer Reviewer
Tayrn R. Taylor, MD, FAAP, FACEP, Assistant Professor of Pediatrics and Emergency Medicine, Emory University School of Medicine, Atlanta, GA
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Dietrich (editor), Dr. Skrainka (CME question reviewer), Dr. Stanich (author), Dr. Bellolio (author), Dr. Taylor (peer reviewer), Ms. Coplin (executive editor), and Mr. Springston (associate managing editor) report no relationships with companies related to the field of study covered by this CME activity.
Abdominal pain is a common chief complaint in the pediatric emergency department (ED) and can be a diagnostic dilemma, as clinical presentation varies greatly depending on the child’s ability to communicate.1,2,3 In addition, the etiology of abdominal pain differs depending on the child’s age and so the differential diagnosis will vary.4,5 It is imperative for ED physicians to differentiate those with life-threatening pathology requiring immediate intervention from those with self-limiting causes of abdominal pain. Fortunately, most cases are nonthreatening and many children will be discharged home with minimal intervention. However, those with abdominal catastrophes require prompt diagnosis, as delays in diagnosis can prove to be fatal.
— Ann M. Dietrich, MD, Editor
This article will outline two common causes of abdominal pain in children younger than 2 years of age: intussusception and malrotation midgut volvulus. Intussusception refers to invagination or telescoping of a part of the intestine into itself, and malrotation volvulus is a congenital anomaly that results when the normal sequence of rotation and fixation of the bowel fails, which may result in intestinal obstruction.6,7 Identifying the cause of bowel obstruction may be as important as recognizing the obstruction itself, as delays in treatment significantly increase morbidity and mortality.4,8,9 Both can be challenging to identify and require astute diagnosis and prompt treatment since, ultimately, intestinal obstruction can lead to bowel ischemia, necrosis, perforation, sepsis, shock, and even death.
INTUSSUSCEPTION
Definition
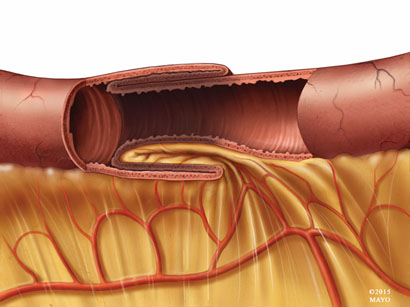
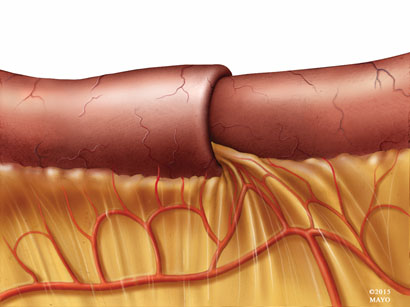
Intussusception refers to invagination or telescoping of a part of the intestine into itself (see Figure 1).6 It is a challenging diagnosis and its presentation varies from a well-appearing child with abdominal pain to one who is ill-appearing with altered mental status.
|
Figure 1. Diagram of Intussusception |
|
|
Epidemiology
Approximately 90% of the time, the diagnosis is made in children younger than 2 years of age and it is fairly uncommon in children less than 3 months.1,3 Intussusception is the most common cause of bowel obstruction in infants between 6-36 months of age.10-13 Most of the time, the child is healthy with no underlying medical problems, and intussusception tends to affect males slightly more often than females (3:2).13
Pathophysiology
The exact etiology is unclear, and 75-90% of the time it is deemed idiopathic.4,14 An infectious etiology has been investigated with conflicting results; a virus or bacteria may stimulate lymphatic tissue, resulting in hypertrophy of a Peyer’s patch, which can act as a lead point for invagination of the bowel. Theoretically, any pathology within the gastrointestinal (GI) tract may act as a lead point; Meckel’s diverticulum and polyps are common culprits.15-18 There is seasonal predilection associated with gastroenteritis and viral syndromes like upper respiratory tract infection, otitis media, and influenza.19 Patients with Henoch-Schönlein purpura have a higher incidence of intussusception, which has been proposed to be secondary to areas of intestinal wall hematoma that act as lead points for intussusception. Vaccines have also been postulated as a cause, which led to a previous form of rotavirus vaccine being taken off the market in 1999.20 Two relatively newer studies in 2014 suggest there remains an increase in the rate of occurrence after vaccination.20,21
Other causes in older children are: lymphoma, Peutz-Jeghers polyps, inversion of Meckel’s, hemangioma, carcinoid, juvenile polyposis coli, and ascaris lumbricoides, among others.
Intussusception occurs when the proximal part of the bowel telescopes into the more distal segment. This invagination can be between virtually any parts of the bowel; however, it occurs most frequently between the ileum and the colon (ileo-colic).1,14 The more proximal segment drags portions of the mesentery with it, which contains venous and lymphatic structures leading to congestion, swelling, inflammation, ischemia, necrosis, and eventually perforation.5
Clinical Features
Intussusception can be a challenging diagnosis depending on the age of the child and the clinical presentation. Board review books classically depict a young child with colicky abdominal pain, and parents will report currant jelly/red stools, although this is not most commonly seen.10 Typically, children will complain of severe abdominal pain that is intermittent. As the bowel peristalses and obstructs, children will experience severe abdominal pain followed by complete resolution of symptoms as the peristaltic obstruction is relieved.22 Later, if the obstruction persists, the bowel can become ischemic and children can become lethargic with an altered mental status. In fact, the differential diagnosis for an altered mental status in children younger than 5 years of age should include intussusception (see Table 1).13,23
|
Table 1. Differential Diagnosis for Pediatric Patients Presenting with Altered Mental Status |
|
|
Altered Mental Status |
|
|
E |
encephalopathy endocrinopathy |
|
I |
insulin (hypoglycemia) intussusception |
|
O |
opiates |
|
U |
uremia |
|
T |
trauma tumor thermal |
|
I |
infection intracranial pathology |
|
P |
psychogenic poisoning |
|
S |
seizure |
|
A |
alcohol acid/base metabolic |
Children can develop bilious emesis due to the obstruction, and up to 80% might have a mass in the right upper quadrant at the time of presentation. Some children might have fever.24 In the setting of perforation, the abdomen may be distended, rigid, and guarding, and/or rebound tenderness may be elicited.
Diagnostic Studies
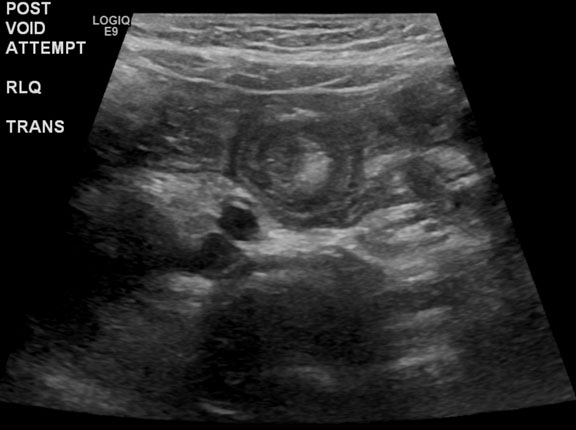
The diagnostic approach depends on how the child presents, which is influenced by the patient’s age and length of obstruction. More ambiguous cases in the setting of a very ill-appearing infant will certainly require broad testing, including labs and imaging such as ultrasound and a CT scan of the head and abdomen.25 However, when one suspects intussusception, labs are rarely useful in making the diagnosis.12,13 Ultrasound imaging is the gold standard diagnostic modality, and is nearly 100% sensitive and approximately 88-100% specific.13,26 A “target sign” can classically be seen on ultrasound as shown in Figure 2. Several studies suggest abdominal X-ray should not be used as a primary screening modality, and emerging data suggest emergency providers working in resource-limited settings may be able to make an accurate diagnosis with bedside ultrasound.4,16,24,26-28 Making the diagnosis at the bedside has potential to decrease ED length of stay, expediting management and leading hopefully to better outcomes. However, this is certainly speculative at this time. CT may be considered when ultrasound cannot delineate a true etiology, but it should not be performed routinely in patients with suspected intussusception.
|
Figure 2. Ultrasound Depicting Intussusception |
|
Source: Mayo Clinic |
Differential Diagnosis
The differential diagnosis for children with abdominal pain will vary depending on age and clinical presentation (see Table 2). Intussusception and incarcerated hernia have been found to be the most common causes of acute non-traumatic abdominal pain in children younger than 1 year of age.1 However, for any child presenting with altered mental status and abdominal pain, ED physicians must consider intussusception (see Table 1). Appendicitis is more commonly found in children older than 1 year of age. Also, one should consider testicular torsion in male patients with unexplained abdominal pain and inspection of the genitalia should always be performed.
|
Table 2. Differential Diagnosis of Acute Abdominal Pain by Age4,5 |
|
|
|
|
< 2 years of age |
2-5 years |
Management
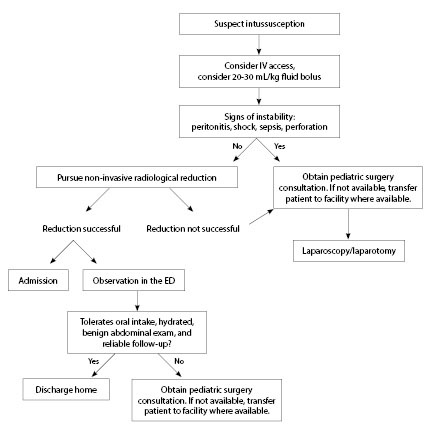
Up to 90% are fixed and do not reduce spontaneously, requiring reduction (see Figure 3). Intravenous access should be considered early, as hypovolemia is common and many will require aggressive fluid resuscitation (20-30 mL/kg isotonic fluid).29 Once the diagnosis is made, a non-invasive radiological reduction should be considered, usually using fluoroscopic guidance with air or contrast. Emerging data suggest radiation-free sonography-guided hydrostatic reduction has a good success rate, although presently it is not standard practice.28,30,31 Peritonitis, shock, sepsis, or radiologic evidence of perforation is a contraindication to non-invasive reduction.5 The American College of Radiology currently recommends that non-invasive reduction only be performed with a surgeon readily available onsite; however, there have been no large studies validating this recommendation.32,33 This information is important for ED providers because following this guideline transfer should be considered promptly once the diagnosis is made if surgical resources are not closely available. A study by Nguyen et al at a large tertiary care children’s hospital suggests presence of onsite surgeons may not be necessary, as complications after non-invasive reduction are rare. However, the provider should be comfortable performing percutaneous needle decompression and managing hemodynamic instability, and be able to arrange surgical care if needed. Surgery is performed if non-invasive radiologic reduction is unsuccessful or contraindicated. Reduction can usually be performed laparoscopically, with open laparotomy uncommonly required.
|
Figure 3. Intussusception Management Algorithm |
 |
Disposition
Admission is indicated if the patient requires surgical intervention, is critically ill, or has contraindications for non-invasive reduction. However, after successful radiologic reduction, disposition becomes slightly less apparent or universal. Recurrence rates are approximately 10%, and recurrence itself is not associated with a significant increase in morbidity or mortality.34,35 Several recent studies suggest patients can be safely discharged with reliable outpatient follow-up following non-invasive radiologic reduction.36-38 For adequately hydrated patients with easily completed non-invasive reduction, observation in the ED for pain recurrence and oral intake is appropriate. If the patient is pain free and can tolerate oral intake, he or she could be discharged home with reliable caregivers. Follow-up and return instructions should be clearly outlined.
If the patient continues to have pain, does not appear adequately hydrated, or if radiologic reduction is difficult, consultation to a pediatric surgeon should be pursued and admission considered.
MALROTATION MIDGUT VOLVULUS
Definition
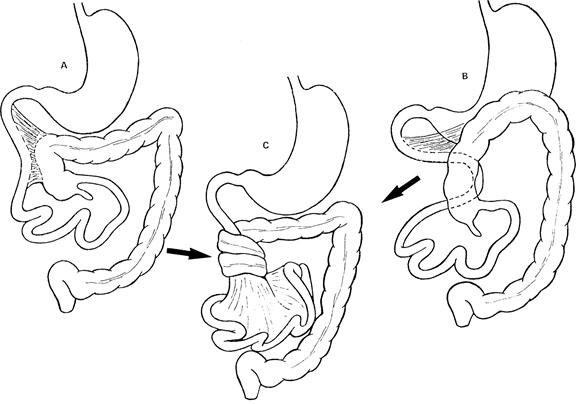
Intestinal malrotation is a congenital anomaly that results when the normal sequence of rotation and fixation of the bowel fails.7,39 Midgut volvulus is a complication of malrotation when the bowel twists around a fixed point usually mesentery that has adhesed to the bowel causing obstruction (see Figure 4).8,40
|
Figure 4. Malrotation Midgut Volvulus |
|
Source: Courtesy of Dr. Mark Mannenbach, Mayo Clinic |
Epidemiology
Malrotation is uncommon, and its prevalence in children younger than 1 year of age is 3.9/10,000 live births; however, it can lead to irreversible intestinal necrosis, which can be fatal, and so one must have a high index of suspicion to make the diagnosis.13,41,42 Most children present within the first month of age and the majority within the first year of life.39 Morbidity and mortality largely depend on the extent of bowel ischemia, which has been largely attributed to a delay in diagnosis.7,9 Males are slightly more affected than females (2:1).3,43
Pathophysiology
During normal embryologic development a counterclockwise turn of both the proximal and midgut portions of the intestine occurs around the fourth to tenth week of gestation, prior to the intestine retracting into the abdomen.13 Abnormalities of rotation physiology result in excessive mobility and compression of the bowel, leading to twisting or volvulus. Mesentery can stick to the bowel and act as a fixed point that the intestine can rotate around, or the bowel may not be fixated correctly to the posterior abdominal wall, which allows the whole midgut to lie free within the abdomen.39 Any part of the intestine may twist and become obstructed, resulting in midgut, cecal, or duodenal volvulus.
Clinical Features
Classically, malrotation with obstruction presents with bilious vomiting, but overall presentation varies.43 Bilious emesis indicates obstruction below the ampulla of Vater, which is a common place for obstruction to occur in the setting of malrotation; although bilious emesis is not pathognomonic for volvulus, it is important to emphasize midgut volvulus should be highly considered in the neonate presenting with bilious emesis.9 The age of the infant affects appearance of disease. Neonates may be fussy and parents may complain of feeding difficulties, intermittent apnea, or even failure to thrive. Older infants may appear to have abdominal pain and diarrhea with or without hematochezia and vomiting. Physical exam findings are non-specific; peritoneal signs indicative of perforation that can lead to sepsis and shock are late signs and indicate a poor prognosis.
Diagnostic Studies
The diagnostic studies performed largely depend on the clinical appearance of the child. A broad net with respect to testing is needed in the toxic-appearing infant. Upper gastrointestinal (UGI) contrast study to assess the third and fourth part of the duodenum is the gold standard to make the diagnosis.39 A classic “corkscrew” appearance in the volvulus can be identified with sensitivity of 96%.44
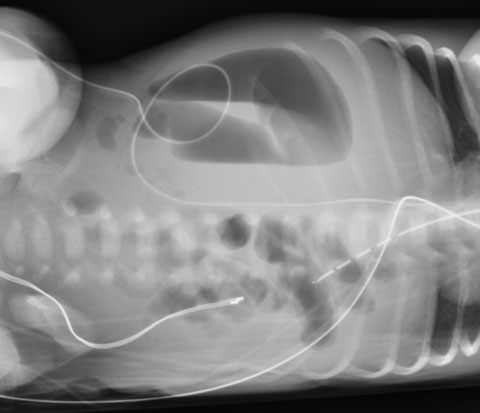
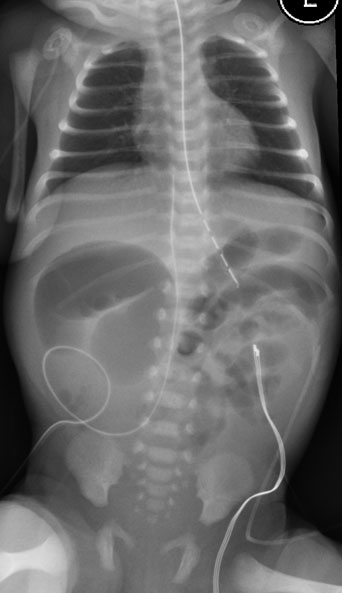
Figure 5 shows the X-ray of a newborn presenting with bilious vomiting. The flat and decubitus X-ray shows asymmetry of the bowel gas with distended loops of bowel in the right side and left side of the abdomen. This patient had malrotation with midgut volvulus.
|
Figure 5. Decubitus (A) of Neonate with Midgut Volvulus |
|
Asymmetry of the bowel gas with a moderately distended loop of bowel in the right and left side of the abdomen. This newborn has midgut volvulus. A Decubitus view Source: Courtesy of Dr. Mark Mannenbach, Mayo Clinic |
|
Figure 5. X-ray flat (B) of Neonate with Midgut Volvulus |
|
Asymmetry of the bowel gas with a moderately distended loop of bowel in the right and left side of the abdomen. This newborn has midgut volvulus. B Flat view Source: Courtesy of Dr. Mark Mannenbach, Mayo Clinic |
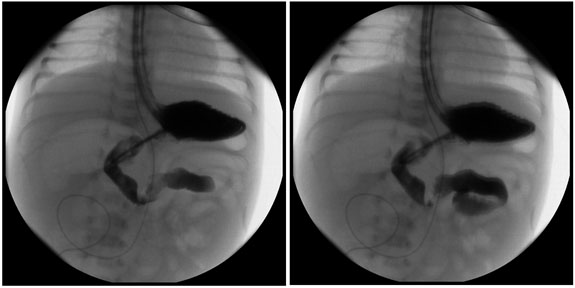
Figure 6 is an upper gastrointestinal study depicting midgut volvulus in a newborn; the study shows that the duodenal jejunal junction crossed to the left of midline but did not extend superiorly as expected, and there was no peristalsis identified within the stomach or duodenum.
|
Figure 6. Upper Gastrointestinal Study Depicting Midgut Volvulus in a Newborn |
|
The duodenal jejunal junction crossed to the left of midline but did not extend superiorly as expected, and there was no peristalsis identified within the stomach or duodenum. |
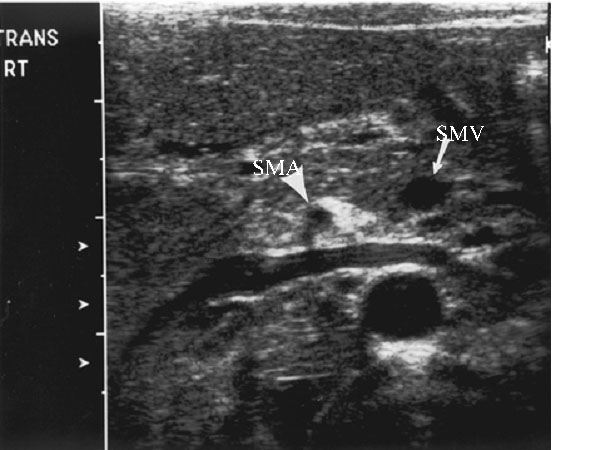
Ultrasound of the mesenteric vessels can also be obtained looking for a “whirlpool sign,” which is a swirling shape seen when the superior mesenteric vein (SMV) and mesentery encompass the superior mesenteric artery (SMA),45 or for “reversal sign.” Figure 7 is an ultrasound showing SMV/SMA reversal sign in midgut volvulus. The sensitivity and specificity of ultrasound are slightly lower than UGI contrast studies, and, as such, ultrasound usually is used as an adjunct.46
|
Figure 7. Ultrasound Showing SMV/SMA Reversal Sign in Midgut Volvulus |
|
Source: Courtesy of Dr. Mark Mannenbach, Mayo Clinic |
Unstable neonates with sepsis, severe metabolic acidosis, or systemic shock presenting with bilious emesis and abdominal distension should likely forgo imaging and proceed with surgical exploration. CT scanning is not routinely performed unless the child’s presentation is ambiguous or an alternative pathology, such as intra-abdominal mass, is high in the differential.
Differential Diagnosis
The differential diagnosis for malrotation largely depends on the age of the child, although many will present with abdominal pain (see Table 2.) Malrotation volvulus usually presents in children younger than 1 month of age, so the differential diagnosis will include illnesses more common in this age group. However, one should suspect malrotation midgut volvulus in a child of any age presenting with bilious vomiting and abdominal pain.
Necrotizing enterocolitis should be considered if the child is premature and presents with changes in feeding and abdominal distention. Older infants presenting with signs of intestinal obstruction and altered mental status should raise concern for intussusception.4 Pyloric stenosis can present with vomiting; however, vomiting is always non-bilious. It is important to note that malrotation volvulus can present in children of any age and has been diagnosed in adults as well.47
Management
Malrotation volvulus is a surgical emergency and requires a laparotomy. Intravenous access should be obtained promptly and aggressive fluid resuscitation started. Nasogastric tube should be placed and antibiotics initiated to cover gram-positive, gram-negative, and anaerobes. Immediate surgical consultation, perhaps even prior to obtaining imaging, may be indicated if the patient is unstable and malrotation volvulus suspected. Morbidity and mortality increase if the obstruction is not treated within 24 hours.3 Surgery is performed to correct the obstruction and minimize risk of future volvulus; the surgery will not correct the actual malpositioning of the bowel. The surgical approach, laparotomy or laparoscopic, does not affect length of stay or the complication rate.48 If bowel necrosis is found, bowel resection will occur, placing the patient at risk for short bowel syndrome, again, emphasizing the need for prompt diagnosis and treatment. The longer the bowel stays obstructed the more likely ischemia and necrosis ensue.
Disposition
Children diagnosed with malrotation volvulus require admission at a facility with pediatric surgical resources. Transfer should be considered even prior to diagnosis if malrotation volvulus is suspected.
Summary
Intussusception is usually diagnosed in children younger than 2 years of age. It affects males slightly more often than females. The exact etiology is unclear; however, there is an association with gastroenteritis and viral syndromes such as upper respiratory tract infection, otitis media, and influenza. Most frequently, the intussusception occurs between the ileum and the colon. Children can present with intermittent abdominal pain, vomiting, and currant jelly or red stools; however, the latter is a late sign. Intussusception should be considered in a child presenting with altered mental status. Non-invasive radiological reduction should be attempted; however, if the child appears critically ill, pediatric surgery should be consulted promptly.
Malrotation midgut volvulus most commonly presents in children younger than 1 month of age. Bilious emesis in a neonate should be considered a surgical emergency until proven otherwise. Patients can present with irritability, feeding difficulties, failure to thrive, and abdominal pain. The diagnosis can be challenging and delays in diagnosis increase morbidity and mortality significantly. Signs of bowel ischemia, such as hematochezia or sepsis, indicate a poor prognosis. UGI contrast study is the gold standard diagnostic modality, and pediatric surgical consultation is required since an operation is required.
Overall, children presenting to the ED with abdominal pain can be challenging to diagnose. ED physicians are charged to differentiate between self-limited pathology and more life-threatening surgical emergencies. Intussusception and malrotation midgut volvulus both can present with abdominal pain, vomiting, and irritability. Both can be fatal if the diagnosis is delayed or missed, and so one must have a high index of suspicion.
References
1. Tseng YC, Lee MS, Chang YJ, Wu HP. Acute abdomen in pediatric patients admitted to the pediatric emergency department. Pediatr Neonatol 2008;49:126-134.
2. Graff LG 4th, Robinson D. Abdominal pain and emergency department evaluation. Emerg Med Clin North Am 2001;19:123-136.
3. McCollough M, Sharieff GQ. Abdominal pain in children. Pediatr Clin North Am 2006;53:107-137, vi.
4. Yang WC, Chen CY, Wu HP. Etiology of non-traumatic acute abdomen in pediatric emergency departments. World J Clin Cases 2013;1:276-284.
5. van Heurn LW, Pakarinen MP, Wester T. Contemporary management of abdominal surgical emergencies in infants and children. Br J Surg 2014;101:e24-33.
6. Lin LH. Perspectives on intussusception. Pediatr Neonatol 2013;54:143-144.
7. Shalaby MS, Kuti K, Walker G. Intestinal malrotation and volvulus in infants and children. BMJ 2013;347:f6949.
8. Lampl B, Levin TL, Berdon WE, Cowles RA. Malrotation and midgut volvulus: A historical review and current controversies in diagnosis and management. Pediatr Radiol 2009;39:359-366.
9. Lee HC, Pickard SS, Sridhar S, Dutta S. Intestinal malrotation and catastrophic volvulus in infancy. J Emerg Med 2012;43:e49-51.
10. Weihmiller SN, Buonomo C, Bachur R. Risk stratification of children being evaluated for intussusception. Pediatrics 2011;127:e296-e303.
11. Punnoose AR, Kasturia S, Golub RM. JAMA patient page. Intussusception. JAMA 2012;307:628.
12. Lochhead A, Jamjoom R, Ratnapalan S. Intussusception in children presenting to the emergency department. Clin Pediatr 2013;52:1029-1033.
13. Shah S. An update on common gastrointestinal emergencies. Emerg Med Clin North Am 2013;31:775-793.
14. Mandeville K, Chien M, Willyerd FA, et al. Intussusception: Clinical presentations and imaging characteristics. Pediatr Emerg Care 2012;28;842-844.
15. Takahashi T, Miyano G, Kayano H, et al. A child with colo-colonic intussusception due to a large colonic polyp: Case report and literature review. Afr J Paediatr Surg 2014;11:261-263.
16. Stolz LA, Kizza H, Little K, Kasekende J. Intussusception detected with ultrasound in a resource-limited setting. Lancet 2013;381:2054.
17. Mirza B. Inverted Meckel’s diverticulum simulating pedunculated polyp as a lead point for ileoileal intussusception in a child. APSP J Case Rep 2013;4:6.
18. Asaumi Y, Miyanaga T, Ishiyama Y, et al. Pediatric ileoileal intussusception with a lipoma lead point: A case report Gastroenterol Rep 2014;2:70-72.
19. Minney-Smith CA, Levy A, Hodge M, et al. Intussusception is associated with the detection of adenovirus C, enterovirus B and rotavirus in a rotavirus vaccinated population. J Clin Virol 2014;61:579-584.
20. Yih WK, Lieu TA, Kulldorff M, et al. Intussusception risk after rotavirus vaccination in U.S. infants. N Engl J Med 2014;370:503-512.
21. Weintraub ES, Baggs J, Duffy J, et al. Risk of intussusception after monovalent rotavirus vaccination. N Engl J Med 2014;370:513-519.
22. Territo HM, Wrotniak BH, Qiao H, Lillis K. Clinical signs and symptoms associated with intussusception in young children undergoing ultrasound in the emergency room. Pediatr Emerg Care 2014;30:718-722.
23. Pumberger W, Dinhobl I, Dremsek P. Altered consciousness and lethargy from compromised intestinal blood flow in children. Am J Emerg Med 2004;22:307-309.
24. Losek JD, Fiete RL. Intussusception and the diagnostic value of testing stool for occult blood. Am J Emerg Med 1991;9:1-3.
25. Daneman A, Navarro O. Intussusception. Part 1: A review of diagnostic approaches. Pediatr Radiol 2003;33:79-85.
26. Halm BM, Boychuk RB, Franke AA. Diagnosis of intussusception using point-of-care ultrasound in the pediatric ED: A case report. Am J Emerg Med 2011;29:354.e1-3.
27. Gingrich AS, Saul T, Lewis RE. Point-of-care ultrasound in a resource-limited setting: Diagnosing intussusception. J Emerg Med 2013;45:e67-70.
28. Bekdash B, Marven SS, Sprigg A. Reduction of intussusception: Defining a better index of successful non-operative treatment. Pediatr Radiol 2013;43:649-656.
29. McDougall RJ. Paediatric emergencies. Anaesthesia 2013;68(Suppl 1):61-71.
30. Menke J, Kahl F. Sonography-guided hydrostatic reduction of ileocolic intussusception in children: Analysis of failure and success in consecutive patients presenting timely to the hospital. Eur J Pediatr 2015;174:307-316.
31. Ocal S, Cevik M, Boleken ME, Karakas E. A comparison of manual versus hydrostatic reduction in children with intussusception: Single-center experience. Afr J Paediatr Surg 2014;11:184-188.
32. Nguyen HN, Kan JH, Guillerman RP, Cassady CI. Intussusception revisited: Is immediate on-site surgeon availability at the time of reduction necessary? AJR Am J Roentgenol 2014;202:432-436.
33. Kaiser AD, Applegate KE, Ladd AP. Current success in the treatment of intussusception in children. Surgery 2007;142:469-475; discussion 475-477.
34. Hsu WL, Lee HC, Yeung CY, et al. Recurrent intussusception: When should surgical intervention be performed? Pediatr Neonatol 2012;53:300-303.
35. Gray MP, Li SH, Hoffmann RG, Gorelick MH. Recurrence rates after intussusception enema reduction: A meta-analysis. Pediatrics 2014;134:110-119.
36. Beres AL, Baird R, Fung E, et al. Comparative outcome analysis of the management of pediatric intussusception with or without surgical admission. J Pediatr Surg 2014;49:750-752.
37. Chien M, Willyerd FA, Mandeville K, et al. Management of the child after enema-reduced intussusception: Hospital or home? J Emerg Med 2013;44:53-57.
38. Gilmore AW, Reed M, Tenenbein M. Management of childhood intussusception after reduction by enema. Am J Emerg Med 2011;29:1136-1140.
39. Millar AJ, Rode H, Cywes S. Malrotation and volvulus in infancy and childhood. Semin Pediatr Surg 2003;12:229-236.
40. Laurence N, Pollock AN. Malrotation with midgut volvulus. Pediatr Emerg Care 2012;28:87-89.
41. Durkin ET, Lund DP, Shaaban AF, et al. Age-related differences in diagnosis and morbidity of intestinal malrotation. J Am Coll Surg 2008;206:658-663.
42. Schulman J, Edmonds LD, McClearn AB, et al. Surveillance for and comparison of birth defect prevalences in two geographic areas--United States, 1983-88. MMWR CDC Surveill Summ 1993;42:1-7.
43. Nehra D, Goldstein AM. Intestinal malrotation: Varied clinical presentation from infancy through adulthood. Surgery 2011;149:386-393.
44. Applegate KE. Evidence-based diagnosis of malrotation and volvulus. Pediatr Radiol 2009;39(Suppl 2):S161-S163.
45. Zhou H, Yan Y, Li C. The whirlpool sign: Midgut volvulus. Emerg Med J 2014;31:1015.
46. Orzech N, Navarro OM, Langer JC. Is ultrasonography a good screening test for intestinal malrotation? J Pediatr Surg 2006;41:1005-1009.
47. Haak BW, Bodewitz ST, Kuijper CF, de Widt-Levert LM. Intestinal malrotation and volvulus in adult life. Int J Surg Case Rep 2014;5:259-261.
48. Stanfill AB, Pearl RH, Kalvakuri K, et al. Laparoscopic Ladd’s procedure: Treatment of choice for midgut malrotation in infants and children. J Laparoendosc Adv Surg Tech A 2010;20:369-372.
MONOGRAPH: It is imperative for ED physicians to differentiate children with life-threatening pathology requiring immediate intervention from the rest.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.