Neurological Emergencies in Children and Adolescents
August 1, 2015
Reprints
Authors
Judith Toski Welsh, MD, Emergency Services Institute, Cleveland Clinic, Cleveland, OH
Purva Grover, MD, FACEP, Emergency Services Institute, Cleveland Clinic, Cleveland, OH
Peer Reviewer
Christopher J. Haines, DO, FAAP, FACEP, Chief Medical Officer, Children’s Specialized Hospital, New Brunswick, NJ; Associate Professor of Pediatrics and Emergency Medicine, Drexel University College of Medicine; Attending Physician, St. Christopher’s Hospital for Children, Philadelphia, PA
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Grover (author), Dr. Welsh (author), and Dr. Haines (peer reviewer) report no relationships with companies related to the field of study covered by this CME activity.
Executive Summary
- Simple febrile seizures are generalized seizures that occur once in a 24-hour period and last < 15 minutes.
- Antivirals should be considered in a child with febrile status epilepticus, focal febrile seizures, a focal neurologic deficit, or altered level of consciousness.
- A developmentally normal child with a nonfocal neurologic exam who has returned to his/her normal baseline after a brief first-time afebrile seizure does not need an emergent CT scan of the brain.
- In about 25% of children, an acute brain disorder (such as traumatic brain injury or meningitis) is cause for status epilepticus. One-third will have developmental delay or epilepsy, another quarter will have febrile seizure as the only cause, and about 10% will have no specific cause ever demonstrated for their prolonged seizure.
Neurological issues in children can take a very dramatic but relatively benign form, or can be subtle but representative of serious underlying illness. Differentiating between high- and low-risk presentations can be challenging, but a thorough understanding of pediatric practice guidelines can help emergency department (ED) physicians determine the most appropriate ED interventions and eliminate potential injury to a child from either excessive intervention or the sequelae of a missed diagnosis. This article will help ED physicians recognize and appropriately treat seizures in children, and provide advice to worried parents about their child’s potential for seizure recurrence. In addition, physicians will learn how to determine which patients require lumbar puncture and understand the risks of brain CT imaging in the pediatric population. Finally, the article will discuss how to know when to emergently or urgently refer children to pediatric neurology.
— Ann M. Dietrich, MD, Editor
Introduction
Neurologic issues in children are relatively common events and can present with symptoms frightening to parents and caregivers. When not treated expeditiously, some events, like status epilepticus, can lead to permanent impairment or cardiovascular collapse resulting in death. Simple febrile seizures, on the other hand, can look scary to parents but do not have high potential for permanent harm. Testing and intervening in the correct manner and at the right time is critical to preventing harm to children from either their underlying disease or medical treatment. Rapid recognition of high-risk historical and physical exam features can direct testing and therapy in an evidence-based manner.
Critical Decisions |
|
Case Presentations
Case One
An 18-month-old girl presents to the ED by ambulance after having a 2-minute episode of unresponsiveness and generalized shaking witnessed by her mother at home. The child had been fussy and went down for a nap earlier than her usual time. The mother felt the child was “warm” but did not take a temperature before laying the child down for a nap. The child did not fall or injure herself during the ictus. The child is up to date with her immunizations and has no significant past medical history, surgery, or hospitalizations. She attends daycare 3 days a week. The mother noted that the child recently had a runny nose. Vital signs upon ED admission include: rectal temperature of 39.5° C (103.1° F), HR 143, RR 28, and pulse ox 98% on room air. She resists the physical exam but is consolable in mother’s arms and happily accepts food and water. No specific focus of infection is obvious, and you cannot appreciate any signs of closed head injury present upon physical exam.
Case Two
A 7-year-old boy with long-standing developmental delay and a history of epilepsy is brought in by EMS with seizure from his school. A teacher witnessed him begin to have grand mal tonic clonic activity 25 minutes earlier while he was in class. EMS arrived and was unable to obtain an IV, so rectal diazepam was administered. The child continues to have seizure activity that has persisted despite the administration of diazepam at the scene and intranasal midzolam 10 minutes later in the ambulance. He is placed in the code room and a Broselow tape is placed beside him as he continues to shake uncontrollably. IV access is obtained, and lorazepam is administered based on his estimated weight on the Broselow tape. Setup for airway access is undertaken. His movements become less frequent, but do not cease entirely by the 30-minute mark. HR is 165 and regular, RR is 42, and rectal temperature is 37.5° C. Capillary refill is < 2 seconds. Another dose of lorazepam is given, but the child continues to seize. The ED pharmacist asks if she can be of service.
Case Three
A 15-year-old girl complains of headache for 1 week. The headache is fluctuating in intensity and emanates from both sides of her forehead. It radiates to the back of the head but she does not have a painful or stiff neck. She has not reported any recent injury or fevers. She has not had any nausea or vomiting, and has no difficulty with vision or balance. The headache is not getting worse, but it has not completely resolved despite daily doses of ibuprofen. Past medical history is significant for admission to the hospital at age 5 months for gastroenteritis. There is no family history of arteriovenous malformation, aneurysm, seizures, or strokes. The child is on no medications and does not smoke, drink, or use drugs. Vital signs are: HR 85, BP 102/65, RR 16, pulse ox 98% on room air. Her mother is concerned that her daughter has a brain tumor and says that their pediatrician referred them to the ED for a brain CT to rule this out.
Febrile Seizures
A febrile seizure is a seizure accompanied by fever (temperature ≥ 100.4° F or 38° C by any method), without central nervous system infection, that occurs in infants and children 6 months to 5 years of age.1 Most febrile seizures occur in children between 6 months to 5 years of age, and they are the most common reason for a seizure in children younger than 5. Febrile seizures are classified as either simple or complex. Simple febrile seizures are generalized seizures that occur once in a 24-hour period and last < 15 minutes. Occurrence of a simple febrile seizure does not increase a child’s risk of developmental delay or death, and is correlated with only a slightly increased risk of epilepsy compared to the general population. Complex febrile seizures are focal, multiple, or longer than 15 minutes in duration.
Workup of Febrile Seizure in the ED. In a fully immunized child, ED management of simple febrile seizures is limited to a search for a source for the fever. In these children, routine CBC and blood cultures are not indicated.2 Urinary tract infection (UTI) should be considered in those children who present without an obvious source on exam. Ill-appearing children require immediate antibiotic therapy. In children with less severe illness, those at risk of UTI should have urinalysis and culture performed. Risk factors for UTI are:
- Female sex
- Uncircumcised male
- No other source of fever
- Fever ≥ 39° C
- In girls: white race, age < 12 months, and fever > 2 days
-
In boys: non-black race and
fever > 24 hours
Children without risk factors may be followed clinically without need for urinalysis and culture.3 A chest radiograph is appropriate in children with significant respiratory illness, white blood cell count > 20,000/mm³, or temperature > 39° C (102.2° F).4
Electrolytes, serum calcium, magnesium, or phosphorus and CT imaging of the brain are not routinely recommended for children with a simple febrile seizure.5 These tests may be indicated in special cases. Electrolytes may be helpful to determine severity of illness in a child with dehydration. A CT scan of the head may be considered in a child who was injured in a fall related to the seizure and who has stigmata of head injury. Abnormal test results are rare in the majority of children presenting with a simple febrile seizure.
Among unimmunized children with a fever > 39° C, the risk of occult bacteremia is as high as 10% when the white blood cell count is > 15,000/mm³. CBC and blood culture are recommended in this group, and children with WBC > 20,000/mm³ should also have chest radiography.6
Meningitis in the Child with a Febrile Seizure. Consideration of lumbar puncture must be made in the case of any child with a febrile seizure. Lumbar puncture is clearly indicated in a febrile child with meningsimus or persistently altered level of consciousness, or in a child who is inconsolable. It should be strongly considered in children with an incomplete vaccination history (particularly for Streptococcus pneumoniae and Haemophilus influenzae), in infants with a first febrile seizure between 6 and 12 months of age, and in children who have been pretreated with antibiotics. In children 12 months of age or older with a simple febrile seizure, however, multiple retrospective studies have not shown an increased risk of meningitis.
CT scanning is not indicated for most patients prior to performing lumbar puncture. Children who require imaging are those with focal deficits, altered level of consciousness suggesting cerebral herniation, or papilledema on physical exam. Postural abnormalities and cranial nerve abnormalities are present in most patients who are later found to have cerebral herniation associated with meningitis.
Children in septic shock also should not have lumbar puncture performed, but instead efforts should be concentrated on adequate resuscitation and administration of antibiotic therapy.7
Antibiotics should be started immediately in children with suspected meningitis, even before lumbar puncture is attempted if the child appears ill. Empiric coverage should include treatment for penicillin-resistant S. pneumoniae and Neisseria meningitidis. Cefotaxime 100 mg/kg, or ceftriaxone 100 mg/kg plus vancomycin 15 mg/kg, is suitable in children without contraindications. In a child with allergies or a complex medical history (i.e., ventriculoperitoneal shunt, immune suppressed for any reason, or recent neurologic surgery), emergent consultation with a pediatric infectious disease specialist and/or pediatric neurosurgeon is appropriate.
Management of Complex Febrile Seizures. No specific guidelines apply to the management of complex febrile seizures, making the evaluation more challenging. These children must be evaluated on a case-by-case basis. Focal convulsions can suggest the possibility of mass effect, encephalitis, or a brain abscess, especially in a child with a prolonged altered level of consciousness.8 Antivirals should be considered in a child with febrile status epilepticus, focal febrile seizures, a focal neurologic deficit, or altered level of consciousness. Herpes simplex is a rare, but potentially devastating, cause of complex febrile seizures in children.9 Rapid treatment of herpes simplex infection with acyclovir can reduce the risk of neurologic impairment or death.10
Even among children with complex febrile seizures, however, lumbar puncture has a low yield unless the child presents with other signs and symptoms suggestive of meningitis.11 CT imaging can be considered as well in appropriate patients with altered mental status or a focal neurological exam. A recent retrospective review of children with a first complex febrile seizure also demonstrated very few abnormal brain CT results in the absence of other concerning symptoms. In particular, children who met the complex febrile seizure criteria on the basis of multiple seizures in 24 hours are at particularly low risk of intracranial pathology.12
Febrile status epilepticus is a relatively rare but high-risk variant of complex febrile seizure. It rarely stops spontaneously, is medication-resistant, and is often a child’s first seizure. The prospective, multicenter FEBSTAT study noted that treatment delays were associated with increased duration of seizure activity, and that seizures lasting longer than 5 minutes tended to continue even if treated. Prehospital antiepileptic drug administration in this study was inconsistent due to local protocols and was variable by region. Ventilatory support was required more frequently in children whose seizures were long-lasting.13
Parental Counseling of Children with Febrile Seizures. Parents should be advised that after a first febrile seizure, about one in three children will have a recurrence. They should be told that noting the time at the onset is important, and that the child should be moved to a safe area free of injurious objects. In a prospective review of 428 children, four features predicted an increased risk of recurrence: patient age younger than 18 months or temperature < 40° C at onset, < 1 hour between fever and convulsion, and first-degree relative with febrile seizure.14 Administration of antipyretics can make a child feel better, but multiple studies have failed to demonstrate that prophylactic use of antipyretics reduces the risk of recurrent febrile seizure.15
Afebrile Seizures
By the time they are 14 years old, 1% of children will have an afebrile seizure, with most of those episodes occurring in children younger than 3 years of age. Seizure recurrence is variable, with estimates between 14% and 65%, with the overwhelming majority occurring within 2 years of the initial episode.16
Evaluation of Afebrile Seizures. The initial task to undertake is to determine whether the event was truly a seizure or a seizure mimic. Many conditions in children can be confused with seizures, including apnea, pallid syncope, reflux, benign sleep myoclonus, breath holding spells, rigors or chills, dystonia, or tics. Syncope should be considered if there is no postictal spell or if the child complains of palpitations. Breath holding spells occur most commonly in infants between 6 and 18 months of age, and often occur while the child is upset and crying. The child may become limp and appear ashen, and loss of consciousness can occur with or without clonus. These episodes are brief, lasting < 1 minute.
A comprehensive history and physical exam should be performed on all patients with suspected seizure activity. (See Table 1.) A report of the event from an eyewitness is one of the most helpful pieces of information. A verbal child also can provide helpful data.
Table 1. Valuable Historical Data to Consider in Seizure Patients |
|
A full physical exam should start with careful evaluation of vital signs, including blood pressure. ED physicians should look for signs of injury, especially evidence of head trauma. Although children with mild head injury are no more at risk of seizure than the general population, up to 57% of children with abusive head trauma will have seizures.17 A full neurological exam should be performed, including an assessment of gait if developmentally appropriate, as well as a skin exam to look for signs of a neurocutaneous disorder. Even if a fever is not present, a stiff neck or other meningeal signs may signal the need for lumbar puncture. Symptoms of a toxidrome may be present in a poisoned child. A bulging fontanel in an infant suggests increased intracranial pressure.
Laboratory analysis of electrolytes and magnesium can be helpful in children younger than 6 months of age with a first seizure, since they are at increased risk of an undiagnosed metabolic abnormality. Excessive dilution of formula can cause hyponatremia, and the effect of excess free water is more severe in smaller infants. Children with the highest pretest probability of abnormal lab values were those who presented to the ED with active seizures, were hypothermic (< 36.5° C), or were younger than 1 month of age.18 Laboratory workup is indicated in children who present with a prolonged first seizure; have a history of a metabolic disorder, dehydration, or suspected excessive free water ingestion; or who have a depressed level of consciousness. An extensive lab workup, including lumbar puncture, is not necessary in a child who is neurologically normal and recovers uneventfully from a brief first seizure. Lumbar puncture should be performed in children with a lengthy postictal period or any symptoms suggestive of meningitis, encephalitis, or subarachnoid hemorrhage.
Neuroimaging in Children with First Seizure. Parents frequently inquire about whether their child with a first seizure should have CT imaging. A developmentally normal child with a nonfocal neurologic exam who has returned to his/her normal baseline after a brief ictus does not need an emergent CT scan of the brain. Brain CT can be helpful in patients who are at high risk for abnormal imaging results. These include patients listed in Table 2.
Table 2. Indications for CT in Children with Afebrile Seizure |
|
|
Adapted from: Sharma S, et al. The role of emergent neuroimaging in children with new-onset afebrile seizures. Pediatrics 2003;111:1-5. |
Risks of CT Imaging in Children. When clinically appropriate, CT is a relatively safe procedure in children. The major risks of performing a CT on a child include the increased risk of cancer from ionizing radiation and those risks associated with the need for sedation in younger or fearful children.
|
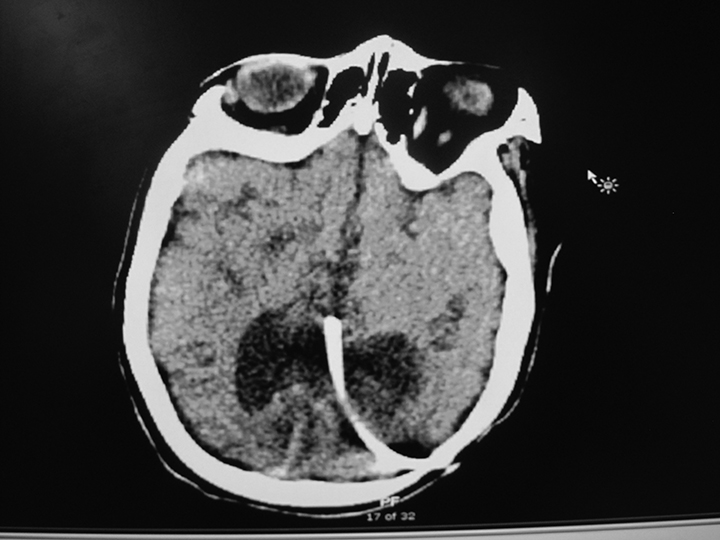
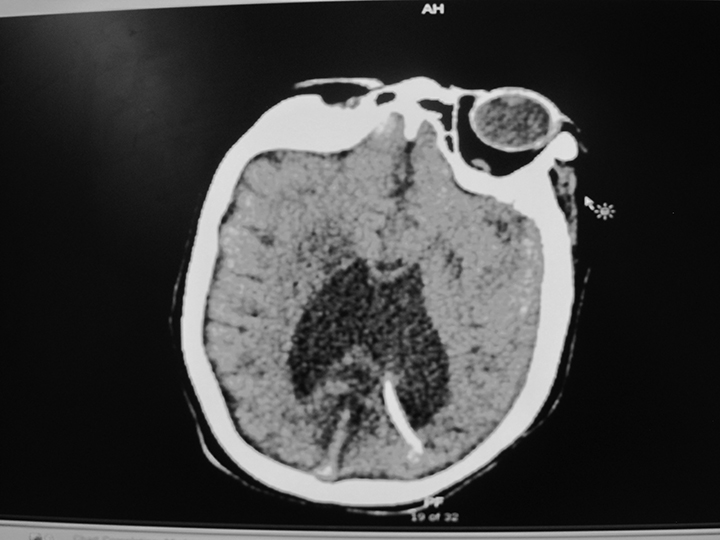
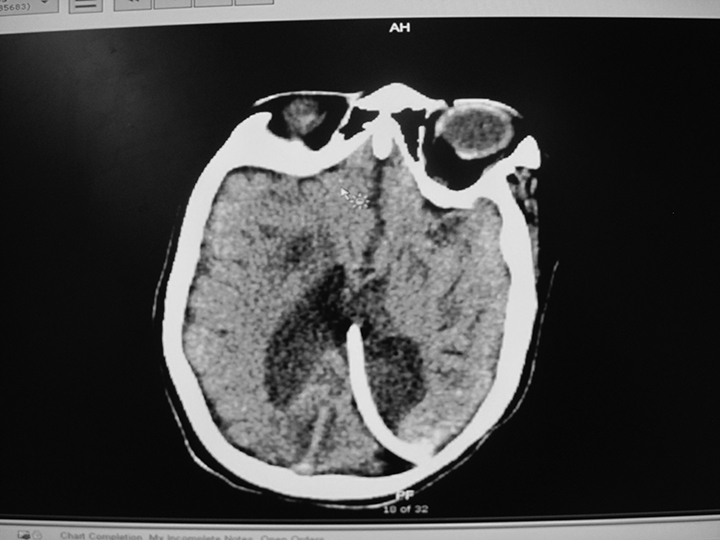
Figure 1. Ventriculoperitoneal shunt failure with hydrocephalus |
|
Child with history of seizures, developmental delay now with increased seizure frequency and gait disturbance |
|
|
Depending on the technique used, one CT of the brain can expose a child to anywhere from 4 to 8 months of background radiation in a single dose. Solid organ cancer risk from one CT scan of the brain is 1.1 to 2.4 cases per 10,000 CT scans. More than 4 million CT scans are performed on children each year in the United States, equating to thousands of potentially avoidable cancers in children annually.19 Although the risk to an individual is small, the cumulative risk to the population is high given the large number of scans performed. Reducing the effective radiation dose, as well as eliminating medically unnecessary, duplicative, and repeat scans, all can mitigate the risk of ionizing radiation on children. As many as one-third of CT scans performed in the United States are not medically necessary or could be supplanted by observation or an alternative imaging method.20 Guidelines should be implemented properly to appropriately guide performance of CT — to both capture positive findings in children at high risk of clinically significant abnormalities, as well as to avoid injury to children who are at low risk of a positive scan.
Outpatient Management and Discharge Counseling. The American Academy of Neurology published a practice parameter regarding appropriate treatment of children with a first unprovoked seizure. The authors examined evidence and made recommendations regarding appropriate management of this condition. They suggested that the risks and benefits be weighed when making the decision to treat with antiepileptic drugs after a first seizure. Many of the medications used to treat epilepsy have cognitive and behavioral side effects. Although treatment after a first seizure reduces the risk of a second seizure, treatment after the first seizure does not make any difference in the likelihood a child will achieve a 1- or 2-year remission. The American Academy of Neurology guidelines recommend a routine EEG for all children with a first afebrile seizure.21 Stable children who are discharged from the ED should be given neurology follow-up.
Parents and children should be counseled regarding “seizure precautions”: reduction of risk of injury or death in the event of a recurrent seizure. Children should wear helmets when riding a bicycle, and should always ride on the sidewalk. Showering rather than bathing, swimming with a buddy (or avoiding swimming altogether), and not climbing (on ladders, up a tree) all are reasonable restrictions. Sudden death of a child during a seizure is a rare event, and usually is the consequence of a serious underlying neurological problem.
Convulsive and Nonconvulsive Status Epilepticus
Status epilepticus is seizure activity that lasts longer than 30 minutes, or intermittent seizure activity without recovery of consciousness between seizures. It is a true emergency, with risk of permanent neurological damage and death. Appropriate treatment of status epilepticus has reduced the death rate in children to between 1% and 5%. Due to the high risk associated with suboptimal treatment of status epilepticus, any seizure lasting longer than 5 minutes should be treated aggressively. Status epilepticus can present as the convulsive type, with obvious motor activity, or as nonconvulsive status. A diagnosis of nonconvulsive status epilepticus should be considered if a child has muscle jerking or twitching, abnormal ocular movements, or deviation of the eyes. Persistently impaired level of consciousness can be the result of a postictal state or from medication administration, but subtle nonconvulsive status epilepticus should be considered as well if the child fails to return to his or her neurologic baseline. Electroencephalography should be ordered in children with long-lasting depressed consciousness or in children who require ongoing neuromuscular paralysis to tolerate invasive ventilation.22
In children, the most common cause of status epilepticus is febrile illness, but the differential diagnosis is listed in Table 3.
Table 3. Differential Diagnosis of Status Epilepticus |
|
ED Management of Status Epilepticus. As with any critically ill patient, the initial goals of management are securing an airway, providing supplemental oxygen, and rapid placement of IV access. Stabilization of the cervical spine is appropriate if trauma cannot be ruled out. Termination of the ictus is also a high priority. Assessment of blood glucose and treatment of symptomatic hypoglycemia should be undertaken as quickly as possible. D10 solution should be used in newborns (dose 5-10 mL/kg) and D25 should be given to children older than 2 months of age (dose 2-4 mL/kg). Ketogenic diets are often used in children with intractable epilepsy. It is unclear how the diets work to control seizures, but studies have demonstrated efficacy. Empiric treatment with glucose is not recommended in children on a ketogenic diet.23
In a child without hypoglycemia, the initial drug class of choice is a rapid-acting benzodiazepine. (See Table 4.) Lorazepam, diazepam, and midazolam are frequently used. Midazolam can be administered intranasally and many EMS protocols include this drug and route of administration, which can be considered as an alternative in patients with difficult to obtain IV access. Careful consideration of prehospital medication administration is important to avoid airway loss due to excessive benzodiazepine dosing. Administration of more than two doses of benzodiazepine is associated with increased risk of airway loss in children with status epilepticus; it is unclear if this is the result of drug administration or more severe disease.24 Children whose care is compromised by prehospital or ED failure to adhere to guidelines are more likely to be admitted to pediatric critical care, particularly when there was either a delay in administering antiepileptic drugs or inadequate doses were provided.25
Table 4. Medications to Treat Seizures in Children |
|||
|
Drug |
Dose and Route |
Maximum Dosage |
Cautions |
|
Midazolam |
0.1 mg/kg IV bolus 2 mcg/kg/min infusion 0.2 mg/kg intranasal 0.5 mg/kg buccal |
24 mcg/kg/min 10 mg Intranasal 10 mg Buccal |
IM midazolam not indicated by FDA for treatment of seizures Preferred benzodiazepine if BP is unstable |
|
Diazepam "> |
0.2 mg/kg IV, IO 0.5 mg/kg rectal |
5 mg IV(< 5 years old), 10 mg IV (5 and up) 20 mg PR |
Administer IV dose slowly to reduce risk respiratory depression |
|
Phenytoin |
20 mg/kg IV, IO |
Max rate 50 mg/min in older children and adults 1 mg/kg/min in younger children |
Bradycardia, arrhythmia, hypotension risk with rapid infusion Small difference between toxic and therapeutic doses |
|
Fosphenytoin |
20 Phenytoin Equivalents (PE)/kg IV/IM |
1.5-3 mg/kg/min, |
Cardiovascular monitoring still recommended during infusion |
|
Phenobarbital |
15-20 mg/kg IV |
500 mg |
Apnea and hypotension Gangrene if injected intra-arterially |
|
Propofol |
1 mg/kg IV bolus 2-4 mg/kg/hr infusion |
10 mg/kg |
Increased risk of lactic acidosis, rhabdomyolysis, and cardiovascular collapse |
|
Levetiracetam |
25-50 mg/kg IV |
100 mg/min |
Not currently included in U.S. guidelines for status epilepticus treatment |
|
IV = intravenous; IM = intramuscular; IO = intraosseous |
|||
|
Adapted from: Friedman JN; Canadian Pediatric Society, Acute Care Committee. Emergency manangement of pediatric patient with generalized status epilepticus. Paediatric Child Health 2011;16:91-97. |
|||
|
Lorazepam |
0.1 mg/kg IV |
4 mg |
Respiratory depression with repeated dosing |
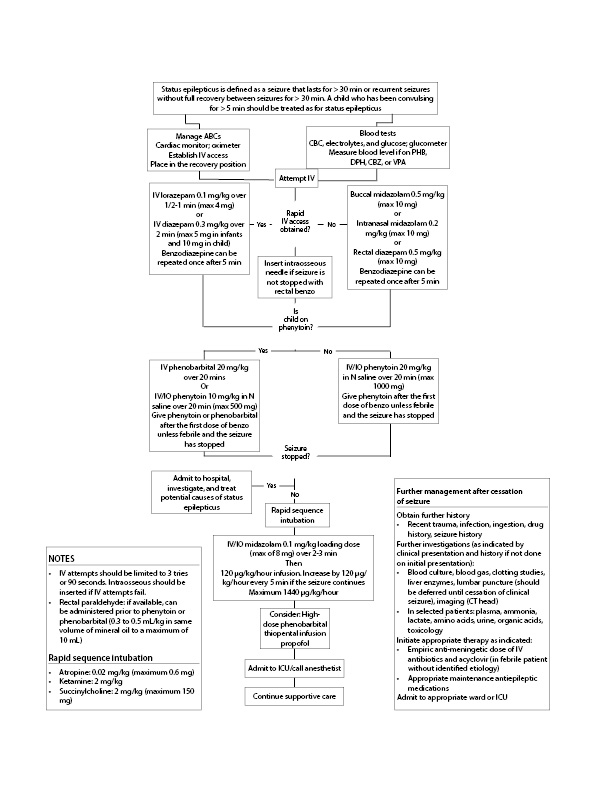
Following administration of a fast-acting benzodiazepine, a longer-acting antiepileptic drug should be administered. Fosphenytoin is preferred over phenytoin since it can be given more quickly and with less risk of cardiac arrhythmias, hypotension, and bradycardia.26 If the seizure continues, a third-line agent must be chosen. Traditionally, phenobarbital was used (loading dose 20 mg/kg at a rate of 2 mg/minute). Phenobarbital causes significant respiratory depression, especially with benzodiazepines present. Levetiracetam and valproic acid are treatment alternatives that may not put the child at as high a risk of airway loss. If seizures persist after the third-line medication is administered, another third-line medication should be used or pharmacologic coma induced. Propofol or midazolam can be loaded then continuously infused for ongoing seizure management (see Figure 2).27
|
Figure 2. Management of Convulsive Status Epilepticus in Infants and Children |
 |
Evaluation of Status Epilepticus. Following stabilization of the patient, workup of the underlying etiology of the seizure can occur. The causes of status epilepticus in children are variable but have a significant influence on the ED workup. (See Table 5.) Younger children are more likely to have febrile or symptomatic causes for their status epilepticus, while older children are more likely to have a history of seizures in the past or developmental delays.28 In about 25% of children, an acute brain disorder (such as traumatic brain injury or meningitis) is cause for status epilepticus. One-third will have developmental delay or epilepsy, another quarter will have febrile seizure as the only cause, and about 10% will have no specific cause ever demonstrated for their prolonged seizure.29
Table 5. Causes of Status Epilepticus in Children |
|
|
Acute brain insult |
25% |
|
Epilepsy, preexisting neurologic problems, or developmental delay |
33% |
|
Febrile seizures without other source |
25% |
|
Idiopathic |
10% |
|
Adapted from: Lee J, Huh L, Korn P, Farrell K. Guideline for the management of convulsive status epilepticus in infants and children. BCMJ 2011;53:279-285. |
|
In general, a search for the cause of the seizure in the ED includes laboratory workup and imaging. Laboratory evaluation should include electrolytes, including magnesium and phosphorus. Brain CT is helpful to rule out hemorrhage, stroke, or other structural lesion predisposing to status epilepticus. Lumbar puncture should be considered in immunocompromised children or those with recent fever. The ED physician should have a low threshold to perform lumbar puncture in patients with status epilepticus.
Headaches in Children and Adolescents
Headaches are common among children. In one epidemiologic study, more than 90% of children reported ever having a headache in their lifetimes.30 A recent study of the National Hospital Ambulatory Medical Care Survey revealed an estimate of 250,000 ED visits annually for children aged 5-18 years with headache-related complaints.31
Headaches are described as “primary” or “secondary.” Primary (migraine, cluster, and tension) headaches are diagnosed based on symptom complaints and patterns of occurrence. Secondary headaches are generally acute onset and due to an underlying disease process and have identifiable causes (sinusitis, brain tumor, intracranial hemorrhage, meningitis). In contrast to primary headaches, secondary headaches frequently present with abnormal physical findings.
Primary Headache Syndromes. Migraine headache is second only to viral illness as a cause of headaches in children presenting for emergency care. Migraines are characterized by intermittent, throbbing headache pain associated with photophobia, nausea, vomiting, abdominal pain, and relief with sleep. Migraine headaches can occur even in the youngest children. In toddlers, parents will relate a history of decreased activity, pale skin, and vomiting. Migraine pain in children is frequently bilateral, and an adult pattern of unilateral headache does not start until adolescence.32
American Academy of Neurology guidelines state that strong evidence supports the use of ibuprofen and intranasal sumatriptan for migraine treatment in children and adolescents, and acetaminophen is a good treatment alternative. Little evidence supports the use of oral or subcutaneous triptans in pediatric patients.33 Dopamine antagonists prochlorperazine and metoclopramide are commonly used in ED treatment of pediatric patients, despite the lack of literature to support their use in this environment. A recent retrospective database review of ED migraine treatment in pediatric patients suggests that prochlorperazine is superior to metoclopramide in preventing a return to the ED within 72 hours, and that use of diphenhydramine is associated with an increased risk of revisit. The authors of this study could not determine if the use of diphenhydramine was prophylactic or the result of side effects from dopamine antagonist drugs. They did note that although the use of triptans is supported by research, they are very infrequently used in the ED.34
Recent research into pediatric migraines headaches has lent additional insight into this condition. Although a relatively common practice with migraine patients, administering intravenous fluids alone did not provide a statistically significant improvement in pain at 30 minutes into the course of ED treatment.35 A recent association between childhood migraine and a history of infantile colic has been established. A case-control study of 208 children showed that children who were colicky as infants were significantly more likely to have migraines between 6 and 12 years of age. Tension headaches were not associated with colic symptoms in infancy.36 School-related stress and anxiety is a common trigger for headaches in pediatric patients, and nationally, headache visits peak in January and September, the same months in which children return to school from vacation. Headache visits do not tend to trend down significantly in summer, leading the authors of this study to conclude that school itself is not the problem, but rather changes in sleep patterns and the transition from vacation to school.31
Tension headaches are as common in children as migraine headaches. They are characterized by pressure or a squeezing sensation of pain, and can last from minutes to days. There is overlap between symptoms of tension headaches and migraines, and although photophobia and phonophobia occur more commonly in migraines, some patients with tension headaches will complain of these symptoms as well. Nausea and vomiting are fairly uncommon with tension headaches, and generally patients with tension headaches will not complain of worsened symptoms with activity. Patients with tension headaches may have some muscular soreness on exam, but will be neurologically intact. Tension-type headaches are often associated with psychological stress.37
Like migraines, tension headaches should be treated with both pharmacologic and nonpharmacologic interventions. Non-narcotic medications such as ibuprofen should be administered as first-line treatment. Relaxation techniques, including cognitive behavioral therapy, biofeedback, and stress management, are generally recommended as an effective part of treatment,38 but to date no large randomized, controlled trials have been undertaken to determine efficacy of these interventions in an ED setting.
Cluster headaches are rare in children younger than 10 years of age, but can be seen in adolescents. They are characterized by unilateral pain and cranial autonomic symptoms. These include: lacrimation, rhinorrhea, facial sweating or flushing, ptosis, miosis, or periorbital edema. High-flow oxygen is the first-line agent to treat cluster headaches in the ED. Usually, the pain dissipates over 3 hours, but they can recur in “clusters” or paroxysms of pain over hours to days. Cluster headaches tend to be more severe and lancinating than migraines, although the distinction between the two entities can be difficult to make in an ED.39
Secondary Headache. Secondary headaches are caused by an underlying medical condition. The most common cause of secondary headache in children is acute febrile illness. Viral infections, colds, and sinusitis frequently present this way. Other causes of secondary headache in children to consider as part of a differential diagnosis include:
- Medications (SSRIs, oral contraceptives)
- Brain tumors
- Meningitis
- Intracranial hemorrhage
- Acute, severe systemic hypertension
- Idiopathic intracranial hypertension (pseudotumor cerebri)
- Hydrocephalus
History and physical exam help narrow down the differential diagnosis. Specific questioning about high-risk features should be part of the history. In particular, asking about sudden onset of pain, or a “thunderclap” nature, suggests a need to look for intracranial hemorrhage. A headache that awakens a child from sleep or an occipital location of pain suggests a need to search for a brain tumor. (See Table 6.) Occipital headache is rare in children and its presence suggests a significant underlying disease.
Table 6. Headache Features Commonly Associated with Tumors |
|
|
Adapted from: Lanphear J, Sarnaik S. Presenting symptoms of pediatric brain tumors diagnosed in the emergency department. Pediatr Emerg Care 2014;30:77-180. |
Pain that is chronic in nature but is worsening acutely in frequency or intensity is high-risk due to the association of this kind of pain with mass-occupying lesions. A child’s past medical history of immunodeficiency (see Figure 3), ventriculoperitoneal shunt, malignancy, sickle cell disease, bleeding disorders, or cyanotic heart disease increase the risk of life-threatening intracranial disease. Physical exam should be complete, including vital signs with accurate blood pressure and temperature measurements, and a careful neurologic examination.
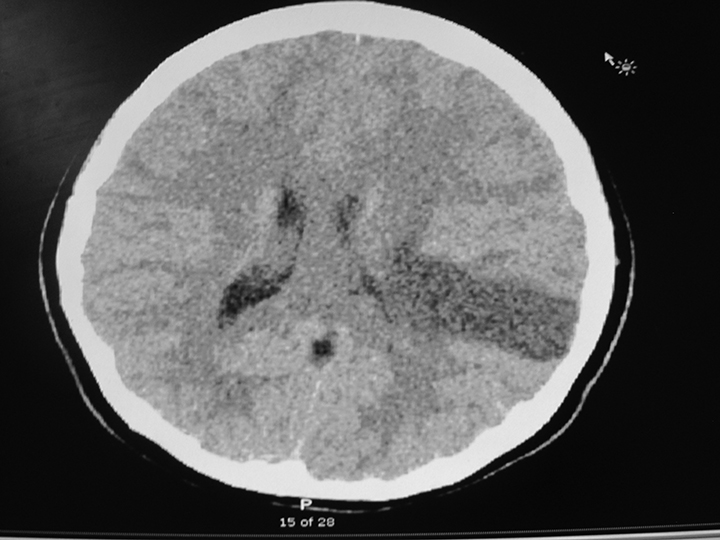
Figure 3. MCA Infarction |
|
Patient: 15-year-old female with "migraine." Had viral myocarditis 3 years ago, underwent heart transplant. Currently on immune suppression. Ongoing headaches for 1 month. Day of evaluation had gradual onset of headache that became progressively worse and then was associated with altered mental status in ED. Diagnosed with MCA infarction, possibly related to septic embolism.
|
Confusion or lethargy may be the result of intracranial hemorrhage, infection, hypertensive encephalopathy, or increased intracranial pressure from mass effect. Abnormal eye movements or papillary response also suggests a need to search for an intracranial mass, as does focal weakness or ataxic gait. Some children with migraines can develop focal neurologic deficits, but a deficit should not be attributed to a benign cause without a thorough workup.
Which Children with Headache Require Emergent Imaging? Most children presenting to the ED with headache and a normal neurologic exam do not need labs drawn or any imaging performed. (See Table 7.) Studies show a low yield of CT and MRI in this population, varying from 0.9% to 1.2%.40 Practice guidelines established by the American Academy of Neurology and endorsed by the American Academy of Pediatrics and the American College of Radiology recommend that children presenting with uncomplicated headaches should not receive imaging of the brain. Despite the national recommendations, CT scanning remains common in pediatric settings including EDs.41 Pediatricians who were surveyed about their patients’ and families’ expectations of treatment commonly indicated that they believed that ruling out a brain tumor was the parents’ primary goal, while only 2% of the surveyed parents indicated that this was their primary concern.42
Table 7. When Neuroimaging Is Required |
|
The goal of neuroimaging is to detect a lesion that requires a change in management, including operative intervention. Cranial infections, congenital or vascular malformations, hemorrhage, cancers, or hydrocephalus all require emergent neurosurgical consultation and potential intervention. CT imaging is frequently considered prior to lumbar puncture, and should be done when considering subarachnoid hemorrhage as a diagnosis in a child with a thunderclap headache. In children with focal neurologic deficits or altered mental status, a CT is an appropriate intervention before performing lumbar puncture. Neuroimaging of children with severe pain and a first-degree relative with an arteriovenous malformation or aneurysm is also appropriate given the genetic potential of these disease processes. CT angiography or MRI with MRA of the neck can detect arterial dissection causing headache. Dissection should be considered in any patient with pain and a neurologic deficit, and should be emergently evaluated.
Case Resolutions
Case One
The child underwent urinary catheterization and her urinalysis was positive for leukocyte esterase and nitrate. A microscopic analysis showed > 30 WBC/hpf. Urine culture was sent to the lab and later grew > 100,000 cfu of Escherichia coli. The child normalized her vital signs after administration of ibuprofen and appeared well upon discharge. She was discharged to home with oral antibiotics and scheduled follow-up the next day with her pediatrician.
Case Two
After two doses of lorazepam, this child’s seizure continued. Although the clonic movements slowed somewhat, he continued to twitch and did not regain his normal level of consciousness. The ED pharmacist confirmed the dose of 20 phenytoin equivalents per kg, and advised the nurses as to the appropriate infusion rate. Following the infusion, he continued with the same low-frequency epileptic movements, and started to have some respiratory depression. At that time, he was intubated and a full set of vital signs was obtained, including a rectal temperature of 38.7° C. Ceftriaxone and vancomycin were ordered empirically, and the ED pharmacist went to obtain the medications. The child was taken for a CT of the brain and the pediatric neuroradiologist read it as unchanged from baseline in real time. Subsequently, a lumbar puncture was performed, suggesting viral meningitis. The child was transferred to the local pediatric tertiary care center PICU via critical care transport team. The team reported a few days later to say that the child was extubated and just about ready to transition care to the pediatric inpatient floor.
Case Three
A full neurologic exam was performed on this child. She had normal cranial nerves, normal station and gait, and no focal cerebellar signs. Reflexes, motor strength and tone, and cognition were all normal for age. There was normal vision and no visual field cuts detected on exam.
Her mother was advised that the risk of CT imaging was not insignificant and was medically unnecessary in the ED. Given her normal neurologic exam and chronic intermittent history of headache, it was decided that she would not have a CT done in the ED, but that an urgent neurologist visit would be appropriate. If the specialist felt that imaging was warranted, this could be pursued as an outpatient. The child was given a dose of ibuprofen with resolution of symptoms 1 hour later.
Summary
Neurological problems in children are relatively common and can present dramatically, with frightened children and worried parents. Fortunately, the vast majority of pediatric patients with seizures and headaches will not suffer any ill effects as a consequence of their symptoms.
All patients with emergent neurologic presentations need a thorough physical exam, searching for signs of toxicity, trauma, and infection. A detailed neurologic exam can be performed in minutes and can render insight into a potentially high-risk condition. CT imaging should be reserved for children with a moderate or high pretest probability of an intracranial lesion, and not part of a routine evaluation in low-risk children. Parents should be advised as to the risk of recurrence of neurologic symptoms. Parents should be given a treatment and follow-up plan that clearly explains the criteria for re-evaluation, and referred to general pediatrics or neurology as appropriate.
Pearls and Pitfalls |
|
Pearls |
|
|
Pitfalls |
|
REFERENCES
- Clinical Practice Guideline – Febrile Seizures: Guideline for the neurodiagnostic evaluation of the child with a simple febrile seizure. Pediatrics 2011;127:389-394
-
Rudinsky SL, Carstairs KL, Reardon JM, et al. Serious bacterial infections in febrile infants in the post-pneumococcal conjugate vaccine era. Acad Emerg Med 2009;16:585-590.
"> -
Subcommittee on Urinary Tract Infection. Urinary tract infection: Clinical practice guideline for the diagnosis and management of the initial UTI in febrile infants and children 2 to 24 months. Pediatrics 2011;128:595-610.
-
American College of Emergency Physicians Clinical Policies Committee. Clinical policy for children younger than three years presenting to the emergency department with fever. Ann Emerg Med 2003;42:530-545.
-
Clinical Practice Guideline – Febrile Seizures: Guideline for the neurodiagnostic evaluation of the child with a simple febrile seizure. Pediatrics 2011;127:392.
-
American College of Emergency Physicians. Clinical policy for children younger than three years presenting to the emergency department with fever. Ann Emerg Med 2003;42:530-545.
-
Oliver WJ, Shope TC, Kuhns LR. Fatal lumbar puncture: Fact versus fiction — an approach to a clinical dilemma. Pediatrics 2003;112:e174-e176.
-
Teng D, Dayan P, Hesdorffer D, et al. Risk of intracranial pathologic conditions requiring emergency intervention after a first complex febrile seizure episode among children. Pediatrics 2006;117:304-308.
-
Hofert S, Burke MG. Nothing is simple about a complex febrile seizure: Looking beyond fever as a cause for seizures in children. Hosp Pediat 2014;4:181-187.
-
Ward KN, Ohrling A, Bryant NJ, et al. Herpes simplex serious neurological disease in young children: Incidence and long-term outcome. Arch Dis Child 2012;97:162-165.
-
Kimia A, Ben-Joseph EP, Rudloe T, et al. Yield of lumbar puncture among children who present with their first complex febrile seizure. Pediatrics 2010;126:62-69.
-
Kimia AA, Ben-Joseph EP, Prabhu S, et al. Yield of emergent neuroimaging among children presenting with a first complex febrile seizure. Pediat Emerg Care 2012;28:316-321.
-
Seinfeld S, Shinnar S, Sun S, et al; FEBSTAT Study Team. Emergency management of febrile status epilepticus: Results of the FEBSTAT study. Epilepsia 2014;55:388-395.
-
Berg AT, Shinnar S, Darefsky AS, et al. Predictors of febrile seizures. A prospective cohort study. Arch Pediatr Adolesc Med 1997;151:371-378.
-
Van Esch A, Van Steensel-Moll HA, Steyerberg EW, et al. Antipyretic efficacy of ibuprofen and acetaminophen on children with febrile seizures. Arch Pediatr Adolesc Med 1995;149:632-637.
-
Hirtz D, Berg A, Bettis D, et al. Practice parameter: Treatment of the child with a first unprovoked seizure. Report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology 2003;60:166-175.
-
Hasbani DM, Topjian AA, Friess SH, et al. Nonconvulsive electrographic seizures are common in children with abusive head trauma. Pediatr Crit Care Med 2013;14:709-715.
-
Scarfone RJ, Pond K, Thompson K, Fall I. Utility of laboratory testing on infants with seizures. Pediatr Emerg Care 2000;16:309-312.
-
Miglioretti DL, Johnson E, Williams A, et al. The use of computed tomography in pediatrics and the associated radiation exposure and estimated cancer risk. JAMA Pediatr 2013;167:700-707.
-
Brenner DJ, Hall EJ. Computed tomography—an increasing source of radiation exposure. N Engl J Med 2007;357:2277-2284.
-
Hirtz D, Berg A, Bettis D, et al. Practice parameter: Treatment of the child with a first unprovoked seizure: Report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Subcommittee of the Child Neurology Society. Neurology 2003;60;166-175.
-
Lee J, Huh L, Korn P, Farrell K. Guideline for the management of convulsive status epilepticus in infants and children. BC Med J 2011;53:279-285.
-
Neal EG, Chaffe H, Schwartz RH, et al. The ketogenic diet for the treatment of childhood epilepsy: A randomised controlled trial. Lancet Neurol 2008;7:500-506.
-
Bosson N, Khodabakhsh D, Kaji A, et al. Risk factors for apnea in children presenting with out-of-hospital seizure. Pediatr Emerg Care 2014;30:617-620.
-
Chin RFM, Verhurst L, Neville BG, et al. Inappropriate emergency management of status epilepticus in children contributes to need for intensive care. J Neurol Neurosurg Psychiatry 2004;75 1584-1588.
-
Fischer JH, Patel TV, Fischer PA. Fosphenytoin: Clinical pharmacokinetics and comparative advantages in the acute treatment of seizures. Clin Pharmacokinet 2003;42:33-58.
-
Marx J, Hockberger R, Walls R. Rosen’s Emergency Medicine: Concepts and Clinical Practice, 8th ed. Chapter 175: Neurologic Disorders. Philadelphia: Elsevier Saunders; 2013.
-
Shinnar S, Pellock JM, Moshé SL, et al. In whom does status epilepticus occur: Age-related differences in children. Epilepsia 1997;38:907-914.
-
Lee J, Huh L, Korn P, Farrell K. Guideline for the management of convulsive status epilepticus in infants and children. BCMJ 2011;53:279-285.
-
Barea LM, Tannhauser M, Rotta NT. An epidemiologic study of headache among children and adolescents of southern Brazil. Cephalalgia 1996;16:545-549.
-
Kedia S, Ginde AA, Grubenhoff JA, et al. Monthly variation of United States pediatric headache emergency department visits. 2014;34:473-478.
-
Headache Classification Committee of the International Headache Society (IHS). The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia 2013;33:629-808.
-
Lewis D, Ashwal S, Hershey A, et al. Practice parameter: Pharmacologic treatment of migraine headache in children and adolescents. Neurology 2004;63:2215-2224.
-
Bachur R, Monuteaux MC, Neuman MI. A comparison of acute treatment regimens for migraine in the emergency department. Pediatrics 2015;135:232-238.
-
Richer L, Craig W, Rowe B. Randomized controlled trial of treatment expectation and intravenous fluid in pediatric migraine. Headache 2014;54:1496-1505.
-
Romanello S, Spiri D, Marcuzzi E, et al. Association between childhood migraine and history of infant colic. JAMA 2013;309:1607-1612.
-
Anttila P. Tension-type headache in childhood and adolescence. Lancet Neurol 2006;5:268-274.
-
Rains JC, Penzien DB, McCrory D, Gray RN. Behavioral headache treatment: History, review of the empirical literature, and methodological critique. Headache 2005;45(Suppl 2):S92-S109.
-
Ozge J, Termine C, Antonaci F, et al. Overview of diagnosis and management of paediatric headache. Part I: Diagnosis. J Headache Pain 2011;12:13-23.
-
American College of Radiology. ACR Appropriateness Criteria 2012. Child – Headache. Avaliable at: https://acsearch.acr.org/docs/69439/Narrative/. Accessed Oct. 4, 2014.
-
DeVries A, Young PC, Wall E, et al. CT scan utilization patterns in pediatric patients with recurrent headache. Pediatrics 2013;132:e1-e8.
-
Raieli V, Compagno A, Pandolfi E, et al. Headache: What do children and mothers expect from pediatricians? Headache 2010;50:290-300.
Neurological issues in children can take a very dramatic but relatively benign form, or can be subtle but representative of serious underlying illness. Differentiating between high- and low-risk presentations can be challenging, but a thorough understanding of pediatric practice guidelines can help emergency department physicians determine the most appropriate ED interventions and eliminate potential injury to a child from either excessive intervention or the sequelae of a missed diagnosis. This monograph will help ED physicians recognize and appropriately treat seizures in children, and provide advice to worried parents about their child’s potential for seizure recurrence. In addition, physicians will learn how to determine which patients require lumbar puncture and understand the risks of brain CT imaging in the pediatric population. It also covers how to know when to emergently or urgently refer children to pediatric neurology.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.