The Next Pandemic: Hospital Management
December 13, 2015
Reprints
Authors
Robert E. Falcone, MD, FACS, Vice President of Clinical Policy and Population Health, Ohio Hospital Association, Clinical Professor of Surgery, The Ohio State University, Columbus.
Andrew Detty, BA, Quality and Population Health Analyst, Ohio Hospital Association, Columbus.
Peer Reviewer
James J. Augustine, MD, FACEP, Clinical Professor of Emergency Medicine, Wright State University, Dayton, OH.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Farel (CME question reviewer) owns stock in Johnson & Johnson. Dr. Stapczynski (editor) owns stock in Pfizer, Johnson & Johnson, AxoGen, Walgreens Boots Alliance Inc., and Bristol Myers Squibb. Ms. Mark’s spouse (executive editor) works for a company that creates advertising for Uroplasty. Dr. Schneider (editor), Dr. Falcone (author), Mr. Detty (author), Dr. Augustine (peer reviewer), Leslie Coplin (executive editor), and Mr. Landenberger (editorial and continuing education director) report no financial relationships with companies related to the field of study covered by this CME activity.
Executive Summary
- The next major pandemic is likely to be due to influenza.
- In an infectious disease pandemic, the hospital resource most at risk for inadequate supply is staff.
- In an infectious disease pandemic, it is recommended that triage be established outside the hospital emergency department.
- Protocols should be developed to guide distribution of intensive care unit (ICU) beds and life-support equipment.
- Psychologic support may be necessary to staff during and after a pandemic event.
Introduction
The threat of pandemic infectious disease lurks quietly beneath the surface of everyday hospital operations and society at large. Moments of panic inspire waves of planning and preparedness activities as new pathogens and mutations pose transient threats. But in the wake of the immediate danger, these moments compete with full hospital beds, a 24/7 news cycle, and any number of demands for clinicians’ and administrators’ attention.
Pandemics are nebulously defined. Widespread geographic impact is the agreed upon hallmark; experts debate the role of factors such as severity and attack rates in classifying a pandemic, and even apply the label to behaviors and noninfectious diseases.1 In cases such as the 2009 H1N1 influenza outbreak, which the World Health Organization (WHO) labeled a “pandemic” but was ultimately of low severity, debate over the definition can crowd out discussion of planning and preparedness.2 However, the threat of pandemic infectious disease is real and overwhelming.
The potential scope and scale of pandemic influenza, in particular, could be immense. Using previous 20th-century pandemics as a guide, the Department of Health and Human Services (HHS) estimates that 90 million Americans could fall ill and 209,000 to 1,903,000 could die.3 Social disruption would be significant, and the resources of hospitals and emergency departments (EDs) would be stretched thin.
More than 5 years after the H1N1 pandemic of 2009, this paper examines the history of pandemics’ impact in the United States and worldwide, their likely impact in the near future, the current state of preparedness of United States hospitals, and special considerations for hospital operations during a pandemic.
Historical Perspective: Selected Pandemics of the Past
Pandemics have had devastating consequences for civilizations worldwide since antiquity. (See Table 1.) Two ongoing world pandemics include tuberculosis (TB) and HIV/AIDS. Mortality from tuberculosis, caused by Mycobacterium tuberculosis, has fallen 47% worldwide since 2000.4 However, it is now the infectious disease responsible for the most deaths worldwide annually. TB killed 1.5 million people (1.1 million HIV-negative people and 400,000 HIV-positive people) in 2014, compared to 1.2 million people killed by HIV/AIDS (including the 400,000 HIV-positive people in the TB death toll).4 An estimated 9.6 million new cases of TB occurred, including 480,000 new cases of multidrug-resistant TB.4 More than 1.2 million Americans are currently living with the HIV virus.5
Table 1. Major Non-Influenzal Infectious Disease Epidemics and Pandemics
|
Event |
Date |
Death Toll |
|
NOTE: Tuberculosis data are from WHO annual tuberculosis burden estimates, 1990-2014. All other death tolls are as of October 2014. SOURCES: National Geographic Staff. (2014, October 25). Graphic: As Ebola’s Death Toll Rises, Remembering History’s Worst Epidemics. Retrieved from http://news.nationalgeographic.com/news/2014/10/141025-ebola-epidemic-perspective-history-pandemic/ World Health Organization. (2015). WHO TB Burden Estimates. Retrieved from https://extranet.who.int/tme/generateCSV.asp?ds=estimates |
||
|
Plague of Justinian (bubonic plague) |
541-542 |
100,000,000 |
|
Black Death (bubonic plague) |
1346-1350 |
50,000,000 |
|
Great Plague of London |
1665-1666 |
100,000 |
|
First cholera pandemic |
1817-1823 |
110,000 |
|
Second cholera pandemic |
1829-1849 |
200,000 |
|
Typhus epidemic |
1847 |
20,000 |
|
Fourth cholera pandemic |
1863-1879 |
704,596 |
|
Fifth cholera pandemic |
1881-1896 |
981,899 |
|
Modern plague |
1894-1903 |
10,000,000 |
|
Sixth cholera pandemic |
1899-1923 |
1,500,000 |
|
HIV/AIDS |
1960-present |
39,000,000 |
|
Seventh cholera pandemic |
1961-present |
570,000 |
|
Tuberculosis (in era of WHO reporting) |
1990-present |
47,000,000 |
|
SARS |
2002-2003 |
774 |
|
West African meningitis outbreak |
2009-2010 |
1210 |
|
Congo measles epidemic |
2011-present |
4555 |
|
Haiti cholera epidemic |
2011-present |
6631 |
|
West African Ebola epidemic |
2014-present |
4877 |
The ongoing Ebola virus disease epidemic in West Africa has also captured the world’s attention, causing 28,607 cases and 11,314 deaths as of November 2015.6 Four cases have been confirmed in the United States, including two acquired abroad and two acquired domestically.7 The two domestic cases occurred in two nurses at Texas Health Presbyterian Hospital in Dallas, which faced criticism for its initial misdiagnosis and ineffective infection control protocols.8 Evidence suggests that Ebola may persist in the body fluids and tissues of survivors for many months after they are symptomatic.9,10 The publicized case of a nurse who suffered Ebola-related meningitis months after appearing to have recovered raises the possibility of Ebola as a chronic illness.11
Outbreaks of coronaviruses that caused severe acute respiratory syndrome (SARS) in 2003 and Middle East respiratory syndrome (MERS) from 2012 to present have also called attention to pandemic preparedness. However, the greatest pandemic threat remains the virus whose regularity belies the unpredictable threat that it poses: influenza.
Influenza Pathophysiology and History
There are three influenza virus types that infect humans: A, B, and C. Type A viruses’ natural reservoirs are in aquatic birds, and they affect a range of warm-blooded animals, including swine, horses, and other mammals. Type B and C viruses are nearly exclusively found in humans.12
Clinically, patients present with a sudden onset of fever, coryza, cough, headache, prostration, malaise, and upper respiratory tract and tracheal inflammation. These symptoms generally last for 7 to 10 days in nonfatal cases, although fatigue and weakness may persist for several weeks.12 The virus replicates in the epithelium of the respiratory tree. Nonfatal cases tend to involve the upper respiratory tract, while fatal infections generally are associated with primary viral or secondary bacterial pneumonia. Mortality is especially high in elderly individuals, infants, and people with comorbid chronic conditions. For a comprehensive description of the pathology of influenza A, see Taubenberger and Morens.12 Notably, the pathology of influenza appears consistent across seasonal and pandemic outbreaks, although patients with some emerging avian strains have had higher rates of associated conjunctivitis, diarrhea, abdominal pain, and vomiting.13
Regular seasonal influenza can be caused by type A or type B, while type C intermittently causes mild respiratory disease. Five percent to 20% of the population is infected in the annual seasonal epidemic cycle,13 with 200,000 hospitalizations and 24,000 deaths in the United States in a typical year.12,14 Type A viruses are also the primary pandemic threat. Type A viruses are divided into subtypes based on the characteristics of two surface proteins, hemagglutinin (H) and neuraminidase (N). Eighteen H subtypes and 11 N subtypes are currently known.15 These antigens can circumvent prior immunity in humans via antigenic drift (i.e., mutations over time that prevent antibody binding) or antigenic shift (i.e., reassortment between influenza A viruses, leading to a virus with new antigens or antigen combinations against which immunity has not been acquired).12 Influenza A viruses to which there is not widespread immunity can lead to pandemic flu.
There have been about a dozen flu pandemics since 1700,12 including three in the 20th century and one in 2009-2010. (See Table 2.) The 1918-1919 “Spanish” H1N1 flu pandemic was the deadliest of these last four, causing about 50 million deaths worldwide16 and close to 675,000 in the United States.17 This virus was unusually pathogenic and killed a disproportionate number of young adults compared to other years.12
Table 2. Characteristics of 20th and 21st Century Influenza Pandemics
|
Year(s) and Common Name |
Area of Origin |
Influenza A Virus Subtype |
Estimated Reproductive Number |
Estimated Case Fatality |
Estimated Attributable Excess Mortality Worldwide |
Age Groups Most Affected |
|
SOURCE: Adapted from World Health Organization. (2013). Pandemic Influenza Risk Management: WHO Interim Guidance. World Health Organization. Retrieved from http://www.who.int/influenza/preparedness/pandemic/GIP_PandemicInfluenzaRiskManagementInterimGuidance_Jun2013.pdf?ua=1 |
||||||
|
1918 “Spanish flu” |
Unclear |
H1N1 (unknown) |
1.2–3.0 |
2–3% |
20–50 million |
Young adults |
|
1957–1958 “Asian flu” |
Southern China |
H2N2 (avian) |
1.5 |
< 0.2% |
1–4 million |
All age groups |
|
1968–1969 “Hong Kong flu” |
Southern China |
H3N2 (avian) |
1.3–1.6 |
< 0.2% |
1–4 million |
All age groups |
|
2009–2010 “influenza A (H1N1) 2009” |
North America |
H1N1 (swine) |
1.1–1.8 |
0.02% |
100,000–400,000 |
Children and young adults |
The next pandemic occurred in 1957-1958, spreading from Asia and killing about 69,800 Americans, primarily the elderly.17 In 1968-1969, a third pandemic occurred, with its origins in Hong Kong. About 33,800 Americans died. This third pandemic may have been milder than the 1957-1958 pandemic in the United States due to partial immunity conferred by the similar 1957 virus, its peak during holiday vacation from school, and improved medical care.17
Miller et al identify five defining features of flu pandemics prior to the 21st century:
- shifts in virus subtypes;
- highest death rates shifting to younger populations;
- multiple successive pandemic waves;
- higher transmissibility than seasonal influenza; and
- different impact across different geographic regions.18
Although the characteristics of future pandemics cannot be predicted with certainty, evaluating the characteristics of past pandemics has allowed HHS to make planning assumptions for medical resource use during moderate and severe pandemic flu scenarios. (See Table 3.)
Table 3. HHS Planning Assumptions for Moderate and Severe Pandemic Influenza Scenarios
|
Characteristic |
Moderate (1958/68-like) |
Severe (1918-like) |
|
SOURCE: Adapted from U.S. Department of Health and Human Services. (2005). HHS Pandemic Influenza Plan. Washington, DC: U.S. Department of Health and Human Services. Retrieved from http://www.flu.gov/planning-preparedness/federal/hhspandemicinfluenzaplan.pdf |
||
|
Illness |
90 million (30%) |
90 million (30%) |
|
Outpatient medical care |
45 million (50%) |
45 million (50%) |
|
Hospitalization |
865,000 |
9,900,000 |
|
ICU care |
128,750 |
1,485,000 |
|
Mechanical ventilation |
64,875 |
742,500 |
|
Deaths |
209,000 |
1,903,000 |
The 2009-2010 H1N1 Pandemic
It appeared that planning assumptions might be put to the test during the first pandemic of the 21st century, the 2009-2010 H1N1 outbreak. The virus was quadruple-reassortant, with gene segments from North American swine flu,19 North American avian flu, human flu, and Asian and European swine flu. Emerging first in the United States and Mexico, the disease spread worldwide, killing an estimated 284,400 people, 201,200 due to respiratory issues and 83,300 due to cardiovascular issues (categories do not sum to total due to rounding).20 Eighty percent of deaths were in people younger than 65 years.20 In the United States, there were approximately 43 to 89 million cases and 8870 to 18,300 deaths; middle-aged people were disproportionately affected.17 On net, the 2009 H1N1 pandemic was far less deadly than those of the 20th century.
Deaths from H1N1, as in previous pandemics, have been linked to inadvertent host immunological responses in the lungs (i.e., “cytokine storms”).21 Monsalvo et al suggest that high levels of mortality among middle-aged adults (relative to children and the elderly) were the result of immune complex-mediated disease.22 Middle-aged adults had nonprotective antibodies that cross-reacted with the virus, whereas the elderly had immunity due to a previous H1N1 outbreak, and children’s immune systems were relatively naïve (leading to high incidence and low mortality). In a review, Singanayagam et al examined the 2009 H1N1 outbreak, identifying factors associated with severe infection, including: young age, pregnancy/postpartum, chronic lung disease, obesity, hypotension, tachycardia, multilobar chest radiograph involvement, elevated creatine kinase, elevated lactate dehydrogenase, and thrombocytopenia.23
Contemporary Global Response
The International Health Regulations (IHR, 2005) govern the international response to public health risks of potential worldwide significance. Under the IHR, 196 member states and non-member parties are obligated to detect, assess, notify, and report events that may constitute “public health emergencies of international concern” (PHEICs) to WHO; all cases of smallpox, wild-type polio, SARS, and human influenza caused by a new subtype must be reported.24 Bound states are also obligated to develop core capabilities for public health surveillance and response. WHO is required to determine whether a PHEIC exists and facilitate information sharing and dissemination, and may make a declaration of a pandemic.25
The 2009 pandemic was the first to occur after WHO had released pandemic preparedness guidance. At the time, WHO had a six-phase alert system for pandemics. The virus was isolated for the first time in April 2009, and WHO Director-General Margaret Chan declared a pandemic (phase 6) on June 11, 2009, when close to 30,000 cases had been confirmed in 74 countries.26 She declared that the world had entered the post-pandemic period on August 10, 2010.27
After the end of the pandemic, WHO convened a Review Committee on the Functioning of the International Health Regulations (2005) and on Pandemic Influenza (H1N1) 2009.28 The Committee’s conclusions and recommendations included the following, in addition to some praise and commendation:
- IHR parties lacked and should accelerate implementation of core capacities to detect, assess, and report public health threats;
- WHO should develop measures to assess the severity of influenza epidemics;
- Problematic communication with the media and the public, and failure to respond to criticism of the WHO, should be addressed through strategic communications management; and
- The pandemic preparedness guidance and six-phase structure should be simplified.28
The WHO came under particular fire due to the perception that it had overstated the seriousness of the pandemic, with some critics suggesting that its objective was to benefit vaccine makers.28
In response, the WHO released new interim guidance for pandemic influenza risk management in 2013, with four pandemic phases: Interpandemic, Alert, Pandemic, and Transition.25 More detailed descriptions of the phases and associated WHO actions are found in Table 4 and Figure 1. The guidance also recommends criteria for risk and severity assessments at the global (i.e., WHO), national, and local levels.
Additionally, the WHO Pandemic Influenza Preparedness (PIP) Framework became effective May 24, 2011.29
The WHO and its members’ new approach and obligations have not yet been put to the test by a second 21st-century flu pandemic. Time will tell whether they are better prepared to address the next crisis and communicate effectively with the media and the public.
Table 4. World Health Organization Pandemic Phases
|
Phase Name |
Description |
|
SOURCE: World Health Organization. (2013). Pandemic Influenza Risk Management: WHO Interim Guidance. World Health Organization. Retrieved from http://www.who.int/influenza/preparedness/pandemic/GIP_PandemicInfluenzaRiskManagementInterimGuidance_Jun2013.pdf?ua=1 |
|
|
Interpandemic Phase |
|
|
Alert Phase |
|
|
Pandemic Phase |
|
|
Transition Phase |
|
Figure 1. Continuum of Pandemic Phases with Indicative WHO Actions
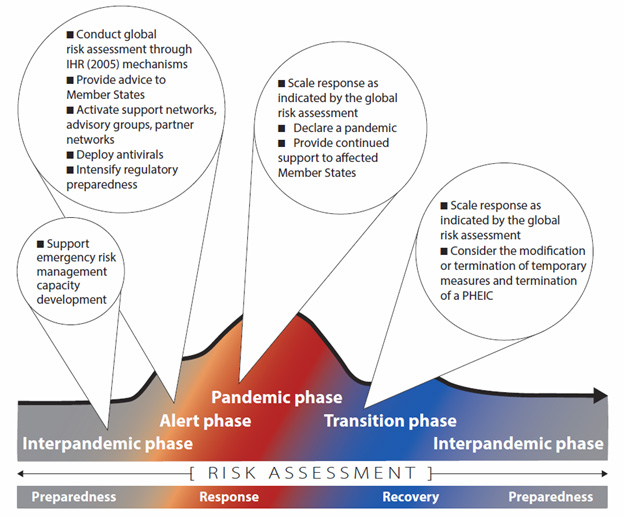
SOURCE: Reprinted with permission from World Health Organization. (2013). Pandemic Influenza Risk Management: WHO Interim Guidance. World Health Organization. Retrieved from http://www.who.int/influenza/preparedness/pandemic/GIP_PandemicInfluenzaRiskManagementInterimGuidance_Jun2013.pdf?ua=1
Contemporary U.S. Response
The United States has its own framework for addressing pandemic influenza. The federal National Strategy for Pandemic Influenza and associated implementation plan are centered on three pillars: preparedness and communication; surveillance and detection; and response and containment.30,31 The HHS Pandemic Influenza Plan serves as a blueprint for HHS preparedness and response, and includes guidance for states and localities.3
Like the WHO, the Centers for Disease Control and Prevention (CDC) revised its framework for pandemic planning in the wake of the 2009 H1N1 outbreak. In 2014, the CDC released a six-interval framework aligned with the four WHO phases to serve as reference points, replacing the stages outlined in the national implementation plan: two pre-pandemic intervals (Investigation and Recognition) and four pandemic intervals (Initiation, Acceleration, Deceleration, and Preparation).32 The framework is described in more detail in Table 5 and Figure 2. The U.S. government has also adopted risk and severity assessment tools (the Influenza Risk Assessment Tool and the Pandemic Severity Assessment Framework, respectively).32
Table 5. WHO and CDC Preparedness and Response Framework for Novel Influenza A Virus Pandemics
|
World Health Organization Phases |
CDC Intervals |
Federal Indicators for CDC Intervals |
State/Local Indicators for CDC intervals |
|
SOURCE: Adapted from Holloway R, Rasmussen SA, Zaza S, et al. Updated Preparedness and Response Framework for Influenza Pandemics. Morbid Mortal Wkly Rep 2014;63(RR06):1–9. |
|||
|
Interpandemic phase: Period between influenza pandemics |
Investigation: Investigation of novel influenza A infection in humans or animals |
Identification of novel influenza A infection in humans or animals anywhere in the world with potential implications for human health |
Identification of novel influenza A infection in humans or animals in the United States with potential implications for human health |
|
Alert phase: Influenza caused by a new subtype has been identified in humans |
|||
|
Recognition: Recognition of increased potential for ongoing transmission of a novel influenza A virus |
Increasing number of human cases or clusters of novel influenza A infection anywhere in the world with virus characteristics, indicating increased potential for ongoing human-to-human transmission |
Increasing number of human cases or clusters of novel influenza A infection anywhere in the world with virus characteristics, indicating increased potential for ongoing human-to-human transmission |
|
|
Pandemic phase: Global spread of human influenza caused by a new subtype |
Initiation: Initiation of a pandemic wave |
Confirmation of human cases of a pandemic influenza virus anywhere in the world with demonstrated efficient and sustained human-to-human transmission |
Confirmation of human cases of a pandemic influenza virus in the United States with demonstrated efficient and sustained human-to-human transmission |
|
Acceleration: Acceleration of a pandemic wave |
Consistently increasing rate of pandemic influenza cases identified in the United States, indicating established transmission |
Consistently increasing rate of pandemic influenza cases identified in the state, indicating established transmission |
|
|
Deceleration: Deceleration of a pandemic wave |
Consistently decreasing rate of pandemic influenza cases in the United States |
Consistently decreasing rate of pandemic influenza cases in the state |
|
|
Transition phase: Reduction in global risk, reduction in response activities, or progression toward recovery actions |
Preparation: Preparation for future pandemic waves |
Low pandemic influenza activity but continued outbreaks possible in some jurisdictions |
Low pandemic influenza activity but continued outbreaks possible in the state |
Figure 2. Preparedness and Response Framework for Pandemic Influenza—CDC Intervals
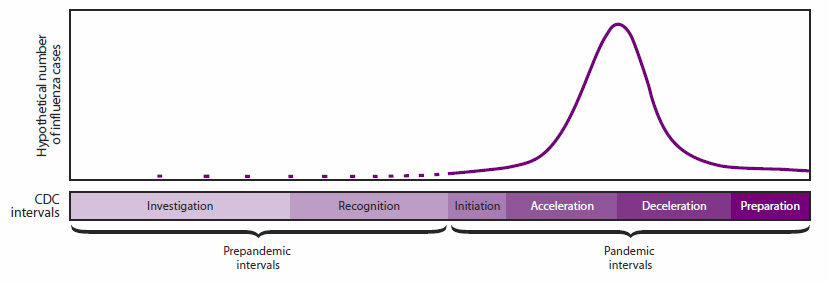
SOURCE: Reprinted with permission from Holloway R, Rasmussen SA, Zaza S, et al. Updated Preparedness and Response Framework for Influenza Pandemics. Morbid Mortal Wkly Rep 2014;63(RR06): 1–9.
The U.S. government’s actions during the 2009 pandemic are illustrative of the levers at its disposal for addressing pandemic flu. Perhaps most importantly, following the isolation of the H1N1 virus in April 2009, initial Food and Drug Administration (FDA) approval of an H1N1 vaccine occurred in September 2009.19
In addition, the CDC maintains a Strategic National Stockpile (SNS) that contains supplies of medicine and medical supplies for distribution in the event of public health emergencies. After the federal government declared a public health emergency in April 2009, the SNS began to release 25% of its influenza-related supplies to states, including antiviral drugs and personal protective equipment (PPE), and announced plans to bolster its supply of antivirals.19 In a retrospective review of the government’s response, HHS suggested that the overall supply of antiviral medications was adequate, but the supply for pediatric populations was not. Tracking of medication that reached states was a challenge, as was coordination with the commercial supply chain.33 It is also possible that a more severe outbreak would have strained the supply.
The federal government took legal and regulatory action, as well. Under Section 1135(b) of the Social Security Act, the HHS Secretary may waive or modify participation requirements for Medicare, Medicaid, and the Children’s Health Insurance Program (CHIP), including certain Emergency Medical Treatment and Labor Act (EMTALA) requirements, Health Insurance Portability and Accountability Act (HIPAA) requirements, and in-state licensing requirements for clinicians. During the 2009 pandemic, the HHS Secretary issued such a waiver.34 Notably, the waiver allowed for direction or relocation of patients from hospitals to other locations to receive medical screening under a state preparedness plan, or transfer of an individual who has not been stabilized if necessary, as is generally prohibited under EMTALA. Sixteen requests were made by 13 states to operate under the waiver; six were approved, and the rest were addressed under current law and regulation.33
The HHS Secretary also took legal action to expand access to antiviral medications. The neuraminidase inhibitors oseltamivir (Tamiflu®) and zanamivir (Relenza®) were largely effective during the 2009 outbreak, despite limited reports of resistance to oseltamivir.19 In April 2009, the FDA issued Emergency Use Authorizations (EUAs) allowing expanded use of oseltamivir in hospitalized patients and infants and dispensing of both drugs by an expanded array of health care workers, including volunteers. In October 2009, the FDA issued an EUA allowing the use of a new investigational neuraminidase inhibitor, intravenously administered peramivir, in some hospitalized patients. In both cases of EUAs, Public Readiness and Emergency Preparedness (PREP) Act liability protection was extended to the additional uses.33 Peramivir eventually received formal FDA approval in December 2014, joining enterically administered oseltamivir and orally inhaled zanamivir in the neuraminidase inhibitor arsenal.35 The FDA also used EUAs to authorize 18 new diagnostic tests to meet demand, although none were point-of-care tests, and only one was available during peak testing demand.33
Finally, the federal government used www.flu.gov as a centralized repository for flu information, including algorithms for triage upon presentation, in relation to influenza-like illness (ILI), for adults and children.36,37 Many resources were available to consumers in English and Spanish, and an electronic self-triage tool discussed further below was provided.
Ultimately, the impact of these federal efforts flowed down to the states and, in turn, to U.S. hospitals.
Contemporary Hospital Response
The 2009-2010 pandemic impacted demand for hospital services. ED visits increased by 18% over baseline in 2005-2008.38 Overall, there was no corresponding surge in all-cause admissions, although there was a 42% increase in pneumonia and influenza admissions. In hospitals that experienced a high surge in admissions, patients with stroke and acute myocardial infarction (AMI) had a significant increase in mortality risk compared to those at no-surge hospitals; notably, those hospitals also had higher mortality for those conditions in the year prior to the pandemic.38
Increased demand was felt more acutely at individual hospitals and health systems. Even fear alone could drive demand higher. A study of one 18-hospital system showed that ED visits increased dramatically (driven mainly by pediatric visits) when public concern about H1N1 was high but disease prevalence was low.39 The experiences of several hospitals illustrate creative approaches to managing a surge in demand.
At Children’s Hospital of Philadelphia, portions of the lobby were converted into an auxiliary ED waiting room for patients determined to be of lower acuity on initial triage.40 A hospital-based outpatient unit was used in the evenings and on weekends to provide care to non-urgent ED patients. Attending physicians from the Department of Pediatrics (without training in pediatric emergency medicine) provided physician surge capacity. Repurposing of rehabilitation unit beds and temporary conversion of single rooms to double rooms provided adequate surge capacity for inpatients. One unforeseen challenge involved ensuring that hospital information systems were prepared to account for alternative use of hospital space. Notably, the rate of inpatient admission was relatively low among ED visitors; in a pandemic with greater severity, greater experience may be required among clinicians responding to the surge.40
At Lincoln Medical and Mental Health Center in the South Bronx, pre-triage staging permitted rapid identification of patients with and without ILI, masking of those with ILI, and monitoring of patient flow.41 Separate clinical tracks were established for patients with and without ILI. Walkout rates did not increase significantly from the prior year, despite a 93.6% increase in mean ED visits and just a 26% increase in physician staffing.41
At Texas Children’s Hospital in Houston, a mobile pediatric emergency response team (MPERT) was established in a parking lot close to the ED entrance. The open-air environment permitted social distancing and rapid evaluation, treatment, and discharge of low-acuity children presenting with symptoms of H1N1.42 In the years since the pandemic, Stanford researchers have simulated a “drive-through” clinic model that allows social distancing and rapid evaluation of patients during a pandemic.43
The Minnesota Department of Health collaborated with health plans and hospital systems that had existing nurse triage telephone lines (NTLs) to establish a coordinated NTL network, called the MN FluLine.44 Using a standardized triage protocol, registered nurses advised callers on when and where to seek care, and offered prescriptions to high-risk individuals advised to stay at home. The Department of Health estimates that the hotline may have prevented close to 11,000 face-to-face health care encounters.44 Partnering with the Association of State and Territorial Health Officials (ASTHO) and the National Association of County and City Health Officials (NACCHO), among others, the CDC has launched the Nurse Triage Line project to examine the feasibility of a national coordinated network of nurse triage lines.45
These are just a few examples of hospital response to the 2009-2010 pandemic, but they demonstrate the innovative approaches to managing pandemics that began to emerge.
Resource Utilization and Social Disruption
The potential consequences of a pandemic are not exclusively medical. Resource utilization and social disruption could be significant. In 1999, Meltzer et al estimated that, independent of disruptions to commerce and society, the economic impact of a pandemic could be $71.3 billion to $166.5 billion.46 The Congressional Budget Office, meanwhile, has suggested that a pandemic due to a highly virulent (i.e., 1918-like) flu strain could lead to a short-term economic impact comparable to a postwar recession.47
SARS, which led to fewer than 1000 deaths but had a high case fatality rate, caused significant economic disruption in affected countries, especially Hong Kong, China, Canada, and Singapore. Gross domestic product (GDP) losses were seen in Hong Kong ($3.7 billion), Canada ($3.2-6.4 billion), and Singapore ($4.9 billion).48 GDP growth slowed in all four countries, and additional losses were seen in exports and trade, as well as the tourism, food, and travel industries.48 In a pandemic, with higher incidence and greater mortality, the economic impact would be multiplied significantly.
During the 1918 flu pandemic, social disruption was immense. Government and media messaging downplayed the threat of disease, in part to keep morale up during the ongoing World War, eroding the public trust.49 With much of the health care workforce abroad at war, resources were strained.50 Broader worker shortages were compounded by absenteeism. Distrust and fear led to a state of panic among the public. The American experience during the 1918 pandemic serves as a warning of the societal consequences of understaffed hospitals and a lack of transparency in messaging.
Projections for the Near Term Future
Potential Chokepoints. The relevant question with respect to the next influenza pandemic is not “if,” but “when.” Flu remains the most potent pandemic disease threat. It is therefore useful to identify potential resource “chokepoints” that could arise during the next event.
Among the most significant is vaccine production. As discussed above, during the 2009 H1N1 pandemic, 5 months elapsed between the first isolation of the flu strain and FDA approval of a vaccine. For the first 3 months of its availability, most state and local health departments targeted specific population groups for vaccination, until there was sufficient supply to ease those restrictions.19 Most vaccine development still occurs through a time-consuming egg-based process.51 In 2012, the FDA approved a cell-based production process that still begins with vaccine virus growth in eggs, but then allows viruses to replicate in cultured mammalian cells. This approach cuts some development time.51 In 2013, the FDA approved an entirely egg-free process in which a hemagglutinin protein from the vaccine virus is combined with a virus that is subsequently grown in insect cells. This approach could cut production time and mitigate the vaccine bottleneck if it becomes more widely adopted.
Availability of intensive care unit (ICU) beds and ventilators presents another potential chokepoint. A 2010 study estimated the supply of full-feature mechanical ventilators in U.S. acute care hospitals to be 62,188,52 just less than one ventilator for each ICU bed in the country.53 Mean hourly ICU occupancy nationally is 68.2%; 29.0% of all ICU beds are filled by patients on ventilators.53 Meltzer et al note that peak ventilator need in a pandemic could vary greatly depending on clinical attack rate, severity, and the shape of the epidemiological curve. They estimate peak need for ventilators among pandemic influenza patients to be 7000 to 140,000, depending on these factors.54 Based on these estimates, existing supply could be completely adequate; alternatively, it could be less than half of the number needed in a worst-case scenario.
Allocation of critical care resources among regions and individual institutions is another area of major concern. Carr et al estimate that if 0.04% of the population experienced sudden critical illness, critical care need would exceed bed supply in more than 90% of the nation’s hospital referral regions.55
Other potential chokepoints could include: the drug development and clinical trial process, which has posed challenges in responding to fast-moving diseases like Ebola in West Africa;56 staffing to cope with increased demand for health services; potentially inadequate antiviral supplies; and addressing a significant number of bodies of the deceased.57
Although pandemic severity is unpredictable, there are measures at the governmental and hospital level that can potentially mitigate these bottlenecks.
Mitigation Strategies. Hospital preparedness and planning are discussed in more detail below, but disease surveillance and vaccination warrant special mention as mitigation strategies. Surveillance activities offer the opportunity to anticipate an impending pandemic and set into motion the often time-consuming processes to combat it.25
In addition, the CDC engages in five levels of flu surveillance:
- virologic surveillance at public health and clinical laboratories, with novel influenza A virus as a nationally notifiable condition;
- surveillance of outpatient visits for ILI, through the U.S. Outpatient Influenza-like Illness Surveillance Network (ILINet);
- mortality surveillance through the National Center for Health Statistics, city mortality reporting systems, and nationally notifiable influenza-associated pediatric mortality;
- surveillance of hospitalizations with laboratory-confirmed influenza through the Influenza Hospitalization Surveillance Network (FluSurv-NET); and
- weekly reports of influenza activity from state and territorial epidemiologists.58
Another chief preventive measure is vaccination. As discussed above, new cell-based production methods may expedite the process of vaccine production and approval. However, vaccination of target populations — particularly health care workers — is a separate challenge. During the 2009-2010 pandemic, just 61.9% of health care personnel had received seasonal flu vaccination, and 37.1% had received a 2009 H1N1 vaccination by 2010.59 Coverage with both vaccines was 34.7%. Just 17.3% of those not vaccinated against 2009 H1N1 cited non-availability of the vaccine; most indicated concern about side effects or that they “[didn’t] need it.”
The evidence base for mandatory vaccination policies for health care workers is mixed. A 2013 Cochrane systematic review found that for individuals older than 60 years in long-term care institutions, health care worker vaccination had no effect on laboratory-confirmed influenza, lower respiratory tract infection (or associated deaths), or hospitalization.60 A 2014 CDC meta-analysis examining long-term care and hospital settings did not find statistically significant decreases in all-cause hospitalization or laboratory-confirmed influenza associated with health care worker vaccination, but did find significant decreases in all-cause mortality and influenza-like illness.61
Low vaccine take-up among health care workers can be attributed in part to the murky evidence and in part to concerns over violation of workers’ autonomy.62,63 As of November 2014, three states required hospitals to ensure that their employees were vaccinated against influenza, and 10 required hospitals to offer the vaccine.64 Some hospitals have independently implemented mandatory vaccine requirements, although in several cases, employees and nurse unions have sued hospitals over the requirements.65,66 These requirements and concerns apply primarily to seasonal influenza, but they carry implications for pandemic flu, in which transmission patterns may be unanticipated and concerns could be compounded by uncertainty over vaccine effectiveness and availability.
Current State of Preparedness
A major challenge of preparing for a flu pandemic is the inherent uncertainty over its attack rate, its severity, and, to some degree, its clinical profile. This uncertainty contributed to public perceptions of WHO’s overestimation of the 2009-2010 pandemic’s severity. However, HHS has prepared planning assumptions that roughly approximate the range of outcomes of a moderate (1958/1968-like) or severe (1918-like) pandemic. (See Table 3.)
The severe pandemic estimates are particularly relevant given the highly pathogenic strains of avian influenza that have begun to emerge. Since 2003, 844 confirmed cases of avian influenza A (H5N1) have been reported to WHO, and 449 of those infected have died, for a case fatality rate of 53%.67 In addition, avian influenza A (H7N9), which was first detected in 2013 in China, had infected 571 people as of February 2015, killing 212, for a case fatality rate of 37%. This strain has not shown evidence of sustained transmission among humans to date, but some limited human-to-human transmission has not been ruled out.68
Triage Guidelines. As discussed above, there is a significant possibility that demand for health care services, particularly intensive care and mechanical ventilation, will exceed supply during a severe pandemic. For this reason, effective triage is needed to optimize limited resources.
One level of triage may be needed upon initial presentation at the ED (or, if possible, prior), to ensure that patients are directed to an appropriate level of care and cohorted, if necessary, based on their flu status. Some innovative approaches were described above. The experience of Montefiore Medical Center in the Bronx during the 2009 H1N1 pandemic is also instructive. The hospital developed a guideline to triage patients with ILI for testing, isolation, and treatment.69 The guideline was implemented by the hospital’s Antibiotic Stewardship Program, in partnership with other departments.
Self-triage off-site is an option that was explored, as well. Just prior to the 2009 H1N1 pandemic, an interdisciplinary group including clinicians and public health experts developed an algorithm called Strategy for Off-Site Rapid Triage (SORT) to direct patients for treatment of ILI.70 After the pandemic began, the tool was refined and validated. Versions were adopted and posted online by the CDC for use by clinicians and call center staff. In addition, a self-triage tool for adults based on SORT was posted on websites supported by HHS and Microsoft. The websites were used for self-assessment about 650,000 times.70
A subsequent study of a self-triage tool for parents of children with ILI based on SORT found that the test was highly sensitive but had low specificity in determining whether ED care was necessary.71 If self-triage is to become a viable tool for managing patient surge, a delicate balance will be necessary to minimize false positives while avoiding false negatives.
A second, more ethically challenging level of triage relates to allocation of scarce critical care resources. In a clinical review, Challen et al72 suggest that a critical care triage framework in a pandemic should:
- Identify patients who will require higher-level care at some stage;
- Recognize patients who are too unwell to benefit from critical care;
- Be consistently applicable by health care workers and professionals from diverse backgrounds and scalable to reflect varying levels of need and capacity; and
- Be disease nonspecific, to allow comparisons across patients with and without influenza.
The authors emphasize two potentially contradictory aspects of triage in a pandemic situation. On the one hand, the weighty ethical and legal implications of the decision-making process require consideration at a senior level and consistent application. At the same time, the overwhelming of resources will require physicians outside of critical care, as well as other health professionals lacking critical care expertise, to make triage decisions. A careful balance between advanced planning and incorporation of accumulating evidence about the disease is needed to ensure that a triage system is understood and implemented consistently.72
A variety of scoring tools have been studied for their ability to allocate critical care resources during an influenza epidemic, including: CURB-65 (confusion, uremia, respiratory rate > 30/min, systolic blood pressure < 90 mmHg, and age > 65), UK Department of Health severity scoring, and the Sequential Organ Failure Assessment (SOFA).23,73-75 None have proven consistently reliable for making allocation decisions.
As such experience demonstrates, there may not be a single algorithm that applies to every hospital and every situation. However, hospitals will benefit from advance discussion of the principles that will guide their triage processes, rather than waiting for a pandemic to strike.
Recommendations for Preparedness Planning. Preparation is vital to ensure that hospitals are equipped for a pandemic, in terms of organization, staffing, and supplies. The CDC has developed a free tool that allows hospitals to estimate the number of hospitalizations and deaths caused by an influenza pandemic of a user-specified length and severity, and compares estimated hospitalizations, ICU admissions, and ventilator need with existing hospital capacity.76 FluSurge 2.0 is available to download at www.cdc.gov/flu/pandemic-resources/tools/flusurge.htm.
In preparation for a pandemic, hospitals should address the elements of the National Incident Management System (NIMS), including the preparation of Hazard Vulnerability Analysis (HVA) plans; an Incident Management System (IMS); a Hospital Emergency Incident Command System (HEICS); understanding of local, regional, state, and national resources; education; and drills. For more information on NIMS in relation to natural disasters, see Falcone and Detty.77 Although an IMS is useful for all-hazards planning, Daugherty et al identify roles specific to epidemic and pandemic illness that may be useful to hospitals, including a medical control chief and situational assessment chief.78
Toner and Waldhorn recommend the following pandemic planning measures for hospitals:
- employment of a full-time incident coordinator;
- use of a pandemic preparedness committee with clinical, support, and senior administrative representation;
- participation in a regional hospital coordinating group, with mutual aid agreements;
- use of FluSurge and HHS planning assumptions to guide planning for moderate and severe pandemics;
- ability to make 30% of licensed bed capacity available for flu patients within 1 week; and
- collaboration in regional plans to make 200% of licensed bed capacity available for flu within 2 weeks.79
They estimate that the cost of preparedness for the average 164-bed hospital is $1,000,000 ($200,000 for a pandemic plan, $160,000 for staff education and training, $400,000 for stockpiling minimal personal protective equipment [PPE], and $240,000 for stockpiling basic supplies).79
Education and Drills. Education and training exercises can improve clinicians’ knowledge of pandemic influenza.80 Drills can expose staff and administrators to the unique challenges of working in a pandemic, including the use of uncomfortable PPE, more time-consuming tasks, more difficult communication, and increased waste production.81 They can also draw attention to gaps in hospitals’ preparedness.
The Occupational Safety & Health Administration (OSHA) recommends that the following elements be included in staff education and training in health care facilities:
- recommended infection control precautions, including contact and droplet precautions;
- reporting pandemic influenza to hospital and public health officials;
- planning strategies for nosocomial surveillance;
- proper use of PPE and hand hygiene;
- provision of respiratory etiquette educational materials;
- training of infection control monitors;
- “tabletop” simulation exercises; and
- risk communication materials.13
A number of training materials are available for health care professionals and workers. HHS has assembled an extensive set of instructional and training resources on pandemic influenza in its Disaster Lit collection, available at http://disasterlit.nlm.nih.gov/search/?search=Search&PubTypeID%5b%5d=45&searchTerms=%28Influenza%20OR%20flu%29.
The CDC has released a “Pan Flu Scramble Exercise,” which is a tabletop exercise for communities and health care stakeholders, and can be accessed at www.cdc.gov/phpr/healthcare/panfluscramble.htm.
Yale New Haven Health’s Center for Emergency Preparedness and Disaster Response also has two courses on pandemic influenza planning response for health care workers and clinicians, which are available at http://ynhhs.emergencyeducation.org/.
Equipment and Supply Caches. As mentioned previously, the CDC’s SNS is meant to mitigate supply shortages in the event of a public health emergency. As with other preparedness and planning considerations, stockpiling is made more challenging by flu’s unpredictability. Given that supply is likely to be limited in a pandemic, even taking the SNS into account, hospitals may also wish to create their own caches of supplies and medication.
Although there may be lag time between the discovery of a pandemic flu strain and the development of an effective vaccine, HHS intends to collaborate with the pharmaceutical industry to produce and stockpile up to 20 million doses of vaccine against any circulating virus with the potential to become a pandemic. Doses will likely be earmarked for health care workers with direct patient contact, and hospitals should be prepared to secure vaccine supplies when they become available.13
Given hospitals’ tight budgets and reliance on “just-in-time” supply chains, stockpiling of antivirals may appear to be an uncertain economic prospect. Notably, due to viral resistance, only the neuraminidase inhibitors (not the adamantane class, which includes adamantine and rimantadine) are recommended to treat recently circulating flu strains.82 Even the effectiveness of the neuraminidase inhibitors against a given strain is not certain.13 However, Balicer et al estimate that stockpiling of oseltamivir for therapeutic use in high-risk patients is ultimately cost-saving not only for the broader economy, but also for the health care system.83 Stockpiling for therapeutic use in all patients, or for post-exposure short-term prophylaxis among patient contacts, is estimated to be cost-saving only for the economy at large. Worldwide supply could pose a challenge to hospital stockpiling of oseltamivir, but it is worthwhile for hospitals to investigate.
Antibiotics and pulmonary medications to treat secondary infections and pneumonia present additional options for stockpiling, as does PPE. Toronto’s experience during the SARS outbreak of 2003 is worthy of consideration. One 1300-bed hospital reported daily PPE use during the peak of the outbreak as including 3000 disposable isolation gowns, 14,000 pairs of gloves, 18,000 N95 respirator masks, 9500 ear loop masks, and 500 pairs of goggles.84 Due to the potential increase in PPE use during a pandemic, HHS recommends stockpiling disposable N95 respirators and surgical masks, face shields, gowns, and gloves.13
Radonovich et al relay a thoughtful approach to stockpiling for a Veterans Integrated Service Network in Florida, which addresses key planning assumptions, expected demand, prioritization and compromise due to limited resources, and storage considerations.85
Special Considerations
Staffing During a Pandemic. There are several potential barriers to hospital staffing during a pandemic. Although there is little evidence that health care workers are at greater risk of contracting influenza than the general public,86 hospitals can nonetheless expect significant absenteeism due to illness. Federal estimates suggest that employers can expect 40% absenteeism at the height of the pandemic wave due to illness, care for family members, canceled school, and other flu-related reasons.31 A significant percentage of workers may be unwilling to report to hospitals during a pandemic due to fear of contracting illness;87 one recent survey suggested that 18% would be unwilling to report if reporting were required, and 28% would be unwilling to report voluntarily.88 Concern over personal and family safety, as well as dependent child care needs at home, are the most commonly cited barriers.89 Compensation issues may also arise, due to the risk inherent in treating patients with influenza.13
Offering workers and their families preferential access to antivirals and PPE may mitigate unwillingness to report to work, as may offering transportation to those who need it.89 Toner and Waldhorn propose the following to make the most of a limited workforce during a pandemic:
- rapid testing for staff available 24/7, with initiation of antiviral treatment within six hours of symptom onset;
- providing in-home childcare for well children using screened volunteers;
- offering medical daycare to sick family members;
- open, honest, and transparent planning;
- transitioning clinical staff to high-need areas;
- bolstering clinical staff with nontraditional personnel; and
- coordinating with other hospitals on recruiting and using volunteers.79
In addition to volunteers, medical students, nursing students, and retired or out-of-state health care workers may be used to reinforce hospital staffing. Legal considerations around such actions are considered below.
Personal Protective Equipment. Hospitals can be sites of significant disease transmission during an outbreak. During the SARS outbreak, the majority of cases in Taiwan and Canada were the result of in-hospital exposures.13 Flu is spread primarily through droplets, although there is some evidence to support airborne transmission, and special caution should be taken during aerosol-generating procedures. There is ongoing debate about the role of airborne transmission of flu and, consequently, debate about whether surgical masks or respirators are most appropriate for health care workers in various settings.90 If respirators are to be used, proper fit testing is essential. OSHA has prepared extensive guidance on the use of respirators, gloves, isolation gowns, and eye and face protection in the event of pandemic influenza.13
Ensuring an adequate supply of PPE should be an integral consideration in hospitals’ preparedness efforts and stockpiling. Given the uncertain transmission patterns in a potential pandemic, adaptation of approaches to PPE may be necessary as evidence emerges on the ground.
Appropriate PPE also should be used in caring for the deceased. Splashes and droplet contamination remain a risk, and for patients who died during the infectious period, the potential presence of the virus in the lungs necessitates respiratory protection during procedures on the lungs and aerosol-generating procedures.91
Medico-Legal Concerns. Pandemic influenza may raise ethical and legal issues that challenge everyday notions of individual liberty and allocation of resources. Some of the legal issues are discussed above in relation to the 2009 H1N1 pandemic, and consideration of additional issues follows.
An Agency for Healthcare Research and Quality (AHRQ) publication outlines the potential for altered standards of care in a mass casualty event.92 The authors point to potential legal issues that could arise during such an event, including: expansion of scope-of-practice standards and associated credentialing; credentialing of retired or out-of-state clinicians; ceding of hospital authority to participate in a broader incident management system; and changes to standards for privacy, confidentiality, and documentation of care.
The authors also note that clinical decisions and policy decisions may require coordination in the move to any altered standard of care. Hospital decisions require the support of local, state, and/or federal policy makers. The authors point to the Model State Emergency Health Powers Act, developed by The Center for Law and the Public’s Health, and Colorado’s draft executive orders for use in disaster emergencies as examples of potential legal frameworks supporting altered standards of care.92 The Institute of Medicine has issued guidance for states developing standards of care for use in disasters when institutions have reached “crisis capacity,” as described by Hicks et al.93,94
The Ethics Subcommittee of the Advisory Committee to the CDC suggests that during an influenza pandemic, the priority of preserving functioning of society may outweigh prevention of serious complications in terms of allocation of resources (e.g., vaccines and antiviral medication). The evaluation of which members of society are essential to its preservation is inevitably challenging, requiring transparency, consistency, and active recognition of diverse perspectives and historical abuses.95
Managing a pandemic also raises the prospect of infringing on personal liberty in the interest of the greater society. Quarantine, isolation, and “social distancing” are measures particularly relevant to hospitals, and should be approached with a careful eye toward evidence of their effectiveness and their broader societal impact.95 Recent experience with Ebola is instructive. When health care workers returned to the United States during the West African Ebola outbreak of 2014, some states imposed mandatory 21-day quarantine periods. Experts questioned not only the evidence base for such measures, but also their chilling effect on the willingness of health care workers to respond to the Ebola crisis.96
Psychological Effects on the Health Care Worker and Community. Pandemic influenza also may have a significant psychological impact on health care workers, patients, and the surrounding community. Data on the psychological effects of a pandemic are limited, but experience with natural disasters suggests that stress reactions could be common, and human service workers may have a high risk of post-traumatic stress disorder.97
The effects of the 2003 SARS outbreak provide some lessons. At a Canadian hospital, quarantine caused fear, anger, loneliness, and boredom among isolated patients, and the fear of becoming infected and restrictions on activity caused discomfort for uninfected patients.98 Health care workers expressed fear and resentment in the face of the danger of infection and constantly changing information; social isolation exacerbated their anxiety, as did concern about infecting loved ones. Stigma was a major issue for health care workers, as was lack of restorative sleep.98
In a Taiwan hospital, 11% of nurses were found to have developed SARS-related stress reaction syndrome (i.e., anxiety, depression, hostility, or somatization).99 Researchers found that among health care workers in Hong Kong hospitals, stress levels persisted for a year after the SARS outbreak, and levels of depression and anxiety were higher among workers who had a high risk of exposure to the virus.100 Availability of psychiatric services and greater availability of information from the hospital may mitigate psychological impact on health care providers.101 Although most people will need minimal psychological support, its availability to staff and potentially to family members should be a consideration in hospital preparedness.13,31
Lessons Learned
- While a number of pathogens have led to worldwide epidemics and pandemics throughout the course of human civilization, the next major pandemic will most likely be due to influenza.
- The United States has a National Strategy for Pandemic Influenza and an associated implementation plan centered on three pillars: preparedness and communication; surveillance and detection; and response and containment.
- World (WHO) and national preparedness centers on the rapid identification and preparation of appropriate vaccines, and national stockpiles of drugs and supplies. The local hospital response must be tailored to the community.
- The most critical potential “chokepoint” for hospital pandemic preparedness is a shortage of staff. Other potential chokepoints include: shortages of vaccines, shortages of antivirals, shortages of PPE, shortages of ICU beds, and shortages of ventilators.
- Mitigation strategies include: local, regional, and national surveillance; vaccination, including for health care workers; and local stockpiles of antivirals and supplies.
- Triage should begin outside of the ED if possible. A number of novel solutions are available for consideration.
- Triage decisions regarding limited critical care beds and equipment should be developed ahead of time and based on local resource projections.
- Disaster planning should be coordinated through the existing HEICS process, but should be specific to pandemic flu.
- Drills and tabletop exercises should occur on a regular basis as part of disaster planning and preparedness.
- Hospital staffing during a true pandemic may be compromised, and those staff members who do work may require psychological support.
REFERENCES
- Morens DM, Folkers GK, Fauci AS. What is a pandemic? J Infect Dis 2009;200:1018–1021.
- Doshi P. The elusive definition of pandemic influenza. Bull WHO 2011;89:532–538.
- U.S. Department of Health and Human Services. (2005). HHS Pandemic Influenza Plan. Washington, DC: U.S. Department of Health and Human Services. Retrieved from www.flu.gov/planning-preparedness/federal/hhspandemicinfluenzaplan.pdf
- World Health Organization. (2015). Global Tuberculosis Report 2015 (20th Edition). Geneva: World Health Organization. Retrieved from http://apps.who.int/iris/bitstream/10665/191102/1/9789241565059_eng.pdf?ua=1
- Centers for Disease Control and Prevention. HIV in the United States: At A Glance. Retrieved from http://www.cdc.gov/hiv/statistics/overview/ataglance.html. Sept. 29, 2015.
- World Health Organization. (2015). Ebola virus disease outbreak. Retrieved from http://www.who.int/csr/disease/ebola/en/.
- Centers for Disease Control and Prevention. (2015, November 9). 2014 Ebola Outbreak in West Africa. Retrieved from http://www.cdc.gov/vhf/ebola/outbreaks/2014-west-africa/index.html
- Sack K. Downfall for hospital where Ebola spread. The New York Times. Oct. 15, 2014.
- Centers for Disease Control and Prevention. Possible Sexual Transmission of Ebola Virus — Liberia, 2015. Morbid Mortal Wkly Rep 2015;64:479–481.
- Deen GF, Knust B, Broutet N, et al. Ebola RNA persistence in semen of Ebola virus disease survivors — Preliminary report. N Engl J Med 2015;
- BBC News. Ebola nurse Pauline Cafferkey “has made full recovery.” BBC News. Retrieved from http://www.bbc.com/news/uk-scotland-34791692. Nov. 12, 2015.
- Taubenberger JK, Morens DM. The pathology of influenza virus infections. Ann Rev Pathol 2008;3:499–522.
- Occupational Safety and Health Administration. (2009). Pandemic Influenza Preparedness and Response Guidance for Healthcare Workers and Healthcare Employers (No. OSHA 3328-05R). Washington, DC: Occupational Safety and Health Administration, U.S. Department of Labor.
- Centers for Disease Control and Prevention. (2010). Estimates of Deaths Associated with Seasonal Influenza — United States, 1976-2007. Morbid Mortal Wkly Rep 2010;59(33):1057–1062.
- Centers for Disease Control and Prevention. Types of Influenza Viruses. Retrieved from http://www.cdc.gov/flu/about/viruses/types.htm. Aug. 19, 2014.
- Taubenberger JK, Morens DM. 1918 Influenza: The mother of all pandemics. Emerg Infect Dis 2006;12:15–22.
- U.S. Department of Health and Human Services. (n.d.). Pandemic Flu History. Retrieved from http://www.flu.gov/pandemic/history/
- Miller MA, Viboud C, Balinska M, et al. The signature features of influenza pandemics — Implications for policy. N Engl J Med 2009;360:2595–2598.
- Centers for Disease Control and Prevention. (2010, June 16). The 2009 H1N1 Pandemic: Summary Highlights, April 2009-April 2010. Retrieved from http://www.cdc.gov/h1n1flu/cdcresponse.htm
- Dawood FS, Iuliano AD, Reed C, et al. Estimated global mortality associated with the first 12 months of 2009 pandemic influenza A H1N1 virus circulation: a modelling study. The Lancet Infectious Diseases 2012;12:687–695.
- Gao R, Bhatnagar J, Blau DM, et al. Cytokine and Chemokine Profiles in Lung Tissues from Fatal Cases of 2009 Pandemic Influenza A (H1N1). Am J Pathol 2013;183:1258–1268.
- Monsalvo AC, Batalle JP, Lopez MF, et al. Severe pandemic 2009 H1N1 influenza disease due to pathogenic immune complexes. Nature Medicine 2011;17:195–199.
- Singanayagam A, Singanayagam A, Wood V, et al. Factors associated with severe illness in pandemic 2009 influenza a (H1N1) infection: Implications for triage in primary and secondary care. J Infection 2011;63:243–251.
- World Health Organization. (2009). Frequently asked questions about the International Health Regulations (2005). World Health Organization. Retrieved from http://www.who.int/ihr/about/FAQ2009.pdf?ua=1
-
World Health Organization. Pandemic Influenza Risk Management: WHO Interim Guidance. World Health Organization. Retrieved from
http://www.who.int/influenza/preparedness/pandemic/GIP_PandemicInfluenzaRiskManagementInterimGuidance_Jun2013.pdf?ua=1 - Chan M. (2009, June 11). World now at the start of 2009 influenza pandemic. Retrieved from http://www.who.int/mediacentre/news/statements/2009/h1n1_pandemic_phase6_20090611/en/
- Chan M. (2010, August 10). H1N1 in post-pandemic period. Retrieved from http://www.who.int/mediacentre/news/statements/2010/h1n1_vpc_20100810/en/
- Review Committee on the Functioning of the International Health Regulations (2005) and on Pandemic Influenza (H1N1) 2009. (2011). Strengthening Response to Pandemics and Other Public-Health Emergencies: Report of the Review Committee on the Functioning of the International Health Regulations (2005) and on Pandemic Influenza (H1N1) 2009. Geneva: World Health Organization. Retrieved from http://apps.who.int/iris/bitstream/10665/75235/1/9789241564335_eng.pdf?ua=1
- World Health Organization. (2011). Pandemic influenza preparedness framework for the sharing of influenza viruses and access to vaccines and other benefits. World Health Organization. Retrieved from http://apps.who.int/iris/bitstream/10665/44796/1/9789241503082_eng.pdf
- Homeland Security Council. (2005, November). National Strategy for Pandemic Influenza. The White House. Retrieved from http://www.flu.gov/planning-preparedness/federal/pandemic-influenza.pdf
- Homeland Security Council. (2006, May). National Strategy for Pandemic Influenza: Implementation Plan. The White House. Retrieved from http://www.flu.gov/planning-preparedness/federal/pandemic-influenza-implementation.pdf
- Holloway R, Rasmussen SA, Zaza S, et al. Updated Preparedness and Response Framework for Influenza Pandemics. Morbid Mortal Wkly Rep 2014;63(RR06):1–9.
- U.S. Department of Health and Human Services. (2012). An HHS Retrospective on the 2009 H1N1 Influenza Pandemic to Advance All Hazards Preparedness. Washington, DC: U.S. Department of Health and Human Services. Retrieved from http://www.phe.gov/Preparedness/mcm/h1n1-retrospective/Documents/h1n1-retrospective.pdf
- Sebelius K. (2009, October 27). Waiver or Modification of Requirements Under Section 1135 of the Social Security Act. Department of Health and Human Services. Retrieved from https://www.cms.gov/About-CMS/Agency-Information/H1N1/downloads/1135WaiverSigned_H1N1.pdf
- Lowes R. (2014, December 22). FDA Approves Peramivir (Rapivab) for Influenza. Retrieved October 29, 2015, from http://www.medscape.com/viewarticle/837028
- Centers for Disease Control and Prevention. (2009, October 27). 2009-2010 Influenza Season Triage Algorithm for Adults (older than 18 years of age) With Influenza-Like Illness. Retrieved from http://www.cdc.gov/h1n1flu/clinicians/pdf/adultalgorithm.pdf
- Centers for Disease Control and Prevention, & American Academy of Pediatrics. (2009). 2009-2010 Influenza Season Triage Algorithm for Children (≤18 years) With Influenza-Like Illness. Retrieved from http://www.cdc.gov/h1n1flu/clinicians/pdf/childalgorithm2.pdf
- Rubinson L, Mutter R, Viboud C, et al. Impact of the Fall 2009 Influenza A(H1N1)pdm09 Pandemic on US Hospitals. Medical Care 2013;51(3), 259–265.
- McDonnell WM, Nelson DS, Schunk JE. Should we fear “flu fear” itself? Effects of H1N1 influenza fear on ED use. Am J Emerg Med 2012;30:275–282.
- Scarfone RJ, Coffin S, Fieldston ES, et al. Hospital-based pandemic influenza preparedness and response: Strategies to increase surge Capacity. Pediatr Emerg Care 2011;7:565–572.
- Waseem M, McInerney JE, Perales O, et al. Impact of operational staging to improve patient throughput in an inner-city emergency department during the novel H1N1 influenza surge: A descriptive study. Pediatr Emerg Care 2012;28:39–42.
- Cruz AT, Patel B, DiStefano MC, et al. Outside the box and into thick air: Implementation of an exterior mobile pediatric emergency response team for North American H1N1 (Swine) influenza virus in Houston, Texas. Ann Emerg Med 2010;55:23–31.
- Weiss EA, Ngo J, Gilbert GH, et al. Drive-through medicine: A novel proposal for rapid evaluation of patients during an influenza pandemic. Ann Emerg Med 2010;55:268–273.
- Spaulding AB, Radi D, Macleod H, et al. Design and implementation of a statewide influenza nurse triage line in response to pandemic H1N1 influenza. Public Health Reports 2012;127:532–540.
- Koonin LM, Hanfling D. Broadening Access to Medical Care During a Severe Influenza Pandemic: The CDC Nurse Triage Line Project. Biosecur Bioterror 2013;11:75–80.
- Meltzer MI, Cox NJ, Fukuda K. The economic impact of pandemic influenza in the United States: Priorities for intervention. Emerg Infect Dis 1999;5:659–671.
- Arnold R, De Sa J, Gronniger T, et al. (2006). A Potential Influenza Pandemic: Possible Macroeconomic Effects and Policy Issues. Washington, DC: Congressional Budget Office. Retrieved from https://www.cbo.gov/sites/default/files/109th-congress-2005-2006/reports/12-08-birdflu.pdf
- Keogh-Brown MR, Smith RD. The economic impact of SARS: How does the reality match the predictions? Health Policy 2008;88:110–120.
- Knobler SL, Mack A, Mahmoud A, et al. (2005). The Threat of Pandemic Influenza: Are We Ready? Workshop Summary. Washington, DC: National Academies Press. Retrieved from http://www.ncbi.nlm.nih.gov/books/NBK22156/pdf/Bookshelf_NBK22156.pdf
- Schoch-Spana M. “Hospital’s full-up”: The 1918 influenza pandemic. Public Health Rep 2001;116(Suppl 2):32–33.
- Centers for Disease Control and Prevention. (2015, January 6). How Influenza (Flu) Vaccines Are Made. Retrieved from http://www.cdc.gov/flu/protect/vaccine/how-fluvaccine-made.htm
- Rubinson L, Vaughn F, Nelson S, et al. Mechanical ventilators in US acute care hospitals. Disaster Medicine and Public Health Preparedness 2010;4:199–206.
- Wunsch H, Wagner J, Herlim M, et al. ICU Occupancy and Mechanical Ventilator Use in the United States. Crit Care Med 2013;41:2712–2719.
- Meltzer MI, Patel A, Ajao A, et al. Estimates of the Demand for Mechanical Ventilation in the United States During an Influenza Pandemic. Clin Infect Dis 2015;60(suppl 1), S52–S57.
- Carr BG, Addyson DK, Kahn JM. Variation in critical care beds per capita in the United States: Implications for pandemic and disaster planning. JAMA 2010;303:1371–1372.
- Helland K. (2015, October 26). MERS, Ebola, bird flu: Science’s big missed opportunities. Reuters. Retrieved from http://www.reuters.com/article/2015/10/26/us-health-epidemic-research-insight-idUSKCN0SK0P020151026
- Osterholm MT. Preparing for the Next Pandemic. N Engl J Med 2005;352:1839–1842.
- Centers for Disease Control and Prevention. (2015, October 13). Overview of Influenza Surveillance in the United States. Retrieved from http://www.cdc.gov/flu/weekly/overview.htm
- Centers for Disease Control and Prevention. Interim Results: Influenza A (H1N1) 2009 Monovalent and Seasonal Influenza Vaccination Coverage Among Health-Care Personnel — United States, August 2009 — January 2010. Morbid Mortal Wkly Rep 2010;59:357–362.
- Thomas RE, Jefferson T, Lasserson TJ. Influenza vaccination for healthcare workers who care for people aged 60 or older living in long-term care institutions. Cochrane Database Syst Rev 2013;(7).
- Ahmed F, Lindley MC, Allred N, et al. Effect of influenza vaccination of healthcare personnel on morbidity and mortality among patients: Systematic review and grading of evidence. Clin Infect Dis 2014;58:50–57.
- Stewart AM. Mandatory vaccination of health care workers. N Engl J Med 2009;361:2015–2017.
- Born K, Ikura S, Laupacis A. The evidence, ethics and politics of mandatory health care worker vaccination. J Health Services Research & Policy 2015;20:1–3.
- Centers for Disease Control and Prevention. (2014, November 19). State Immunization Laws for Healthcare Workers and Patients: Immunization Administration Requirements For Hospital Employees (Influenza). Retrieved from http://www2a.cdc.gov/vaccines/statevaccsApp/AdminbyVaccineandPatientType.asp?PatientTypetmp=Hospital%20Employees&Vaccinetmp=Influenza#21
- Freyer FJ. Nurses union sues to block proposed flu-shot mandate at Brigham and Women’s Hospital. The Boston Globe. Sept. 25, 2014. Retrieved from https://www.bostonglobe.com/metro/2014/09/24/nurses-union-sues-block-proposed-flu-shot-mandate-brigham-and-women-hospital/SQBXdxd1OQwTie5Fyg1d1J/story.html
- Associated Press. (2014, June 5). Nurse who refused flu shot wins lawsuit against Hackettstown Regional Medical Center. Lehighvalleylive.com. Retrieved from http://www.lehighvalleylive.com/warren-county/express-times/index.ssf/2014/06/nurse_who_refused_vaccine_wins.html
- World Health Organization. (2015, October 15). Cumulative number of confirmed human cases for avian influenza A(H5N1) reported to WHO, 2003-2015. World Health Organization. Retrieved from http://www.who.int/influenza/human_animal_interface/EN_GIP_20151015cumulativeNumberH5N1cases.pdf?ua=1
- World Health Organization. (2015, February 23). WHO Risk Assessment of Human infections with Avian Influenza A(H7N9) Virus. World Health Organization. Retrieved from http://www.who.int/influenza/human_animal_interface/influenza_h7n9/RiskAssessment_H7N9_23Feb20115.pdf?ua=1
- Ahmad H, Guo Y, Yaghdjian V, et al. Hospital Emergency Response to Novel Influenza A (H1N1) Pandemic in a Large New York City Hospital: An Opportunity for Antimicrobial Stewardship. Hospital Pharmacy 2012;47:532–537.
- Kellermann AL, Isakov AP, Parker R, et al. Web-based self-triage of influenza-like illness during the 2009 H1N1 influenza pandemic. Ann Emerg Med 2010;56(3), 288–294.e6.
- Anhang Price R, Fagbuyi D, Harris R, et al. Feasibility of web-based self-triage by parents of children with influenza-like illness: A cautionary tale. JAMA Pediatrics 2013;167:112–118.
- Challen K, Bentley A, Bright J, et al. Clinical review: Mass casualty triage — pandemic influenza and critical care. Critical Care 2007;11:212.
- Christian MD, Hawryluck L, Wax RS, et al. Development of a triage protocol for critical care during an influenza pandemic. CMAJ 2006;175:1377–1381.
- NYS Workgroup on Ventilator Allocation in an Influenza Pandemic, New York State Department of Health, & New York State Task Force on Life & the Law. (2007, March 15). Allocation of Ventilators in an Influenza Pandemic: Planning Document (Draft for Public Comment). New York State Department of Health. Retrieved from https://www.health.ny.gov/diseases/communicable/influenza/pandemic/ventilators/docs/ventilator_guidance.pdf
- Khan Z, Hulme J, Sherwood N. An assessment of the validity of SOFA score based triage in H1N1 critically ill patients during an influenza pandemic. Anaesthesia 2009;64:1283–1288.
- Zhang X, Meltzer MI, Wortley P. (2005). FluSurge2.0: A manual to assist state and local public health officials and hospital administrators in estimating the impact of an influenza pandemic on hospital surge capacity (Beta test version). Atlanta: Centers for Disease Control and Prevention, U.S. Department of Health and Human Services. Retrieved from http://www.cdc.gov/flu/pandemic-resources/tools/downloads/flusurge2.0_manual_060705.pdf
- Falcone R, Detty A. Natural disasters: Hospital management. Emerg Med Rep 2015;36:273–288.
- Daugherty EL, Carlson AL, Perl TM. Planning for the inevitable: Preparing for epidemic and pandemic respiratory illness in the shadow of H1N1 influenza. Clin Infect Dis 2010;50:1145–1154.
- Toner E, Waldhorn R. What hospitals should do to prepare for an influenza pandemic. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 2006;4:397–402.
- Leiba A, Dreiman N, Weiss G, et al. The effectiveness of an educational intervention on clinicians’ knowledge of pandemic influenza. Israel Med Assoc J 2010;12:460–462.
- Phin NF, Rylands AJ, Allan J, et al. Personal protective equipment in an influenza pandemic: A UK simulation exercise. J Hospital Infect 2009;71:15–21.
- Centers for Disease Control and Prevention. (2015, September 16). Influenza Antiviral Drug Resistance. Retrieved from http://www.cdc.gov/flu/about/qa/antiviralresistance.htm
- Balicer RD, Huerta M, Davidovitch N, et al. Cost-benefit of stockpiling drugs for influenza pandemic. Emerg Infect Dis 2005;11:1280–1282.
- Friesen S. The impact of SARS on healthcare supply chains. Logistics Quarterly Magazine 2003;9(2). Retrieved from http://logisticsquarterly.com/issues/9-2/article1.html.
- Radonovich LJ, Magalian PD, Hollingsworth MK, et al. Stockpiling supplies for the next influenza pandemic. Emerg Infect Dis 2009;15:e1–e1.
- Kuster SP, Coleman BL, Raboud J, et al, behalf of the Working Adult Influenza Cohort Study Group. Risk factors for influenza among health care workers during 2009 pandemic, Toronto, Ontario, Canada. Emerg Infect Dis 2013;19:606–615.
- Irvin CB, Cindrich L, Patterson W, et al. Survey of hospital healthcare personnel response during a potential avian influenza pandemic: Will they come to work? Prehospital Disaster Med 2008;23:328–335.
- Balicer RD, Barnett DJ, Thompson CB, et al. Characterizing hospital workers’ willingness to report to duty in an influenza pandemic through threat- and efficacy-based assessment. BMC Public Health 2010;10:436.
- Garrett AL, Park YS, Redlener I. Mitigating absenteeism in hospital workers during a pandemic. Disaster Med Public Health Preparedness 2009;3(Supplement S2):S141–S147.
- Killingley B. Respirators versus medical masks: evidence accumulates but the jury remains out. Influenza and Other Respiratory Viruses 2011;5:143–145.
- World Health Organization. (2007, May 10). Avian Influenza, Including Influenza A (H5N1), in Humans: WHO Interim Infection Control Guideline for Health Care Facilities. World Health Organization. Retrieved from http://www.wpro.who.int/emerging_diseases/documents/docs/AI_Inf_Control_Guide_10May2007.pdf
- Health Systems Research Inc. (2005). Altered Standards of Care in Mass Casualty Events (AHRQ Publication No. 05-0043). Rockville: Agency for Healthcare Research and Quality. Retrieved from http://archive.ahrq.gov/research/altstand/altstand.pdf
- Altevogt BM, Stroud C, Hanson SL, et al. (2009). Guidance for Establishing Crisis Standards of Care for Use in Disaster Situations: A Letter Report. Washington, DC: Institute of Medicine. Retrieved from http://www.nap.edu/catalog/12749/guidance-for-establishing-crisis-standards-of-care-for-use-in-disaster-situations
- Hick JL, Barbera JA, Kelen GD. Refining surge capacity: conventional, contingency, and crisis capacity. Disaster Med Public Health Preparedness 2009;3(2 Suppl):S59–67.
- Kinlaw K, Levine R. (2007). Ethical Guidelines in Pandemic Influenza. Ethics Subcommittee of the Advisory Committee to the Director, Centers for Disease Control and Prevention. Retrieved from http://www.cdc.gov/od/science/integrity/phethics/panFlu_Ethic_Guidelines.pdf
- Drazen JM, Kanapathipillai R, Campion EW, et al. Ebola and quarantine. N Engl J Med 2014;371:2029–2030.
- Center for the Study of Traumatic Stress. (n.d.). Mental Health and Behavioral Guidelines for Response to a Pandemic Flu Outbreak: Background on the Mental Health Impact of Natural Disasters, including Epidemics. Bethesda: Center for the Study of Traumatic Stress. Retrieved from http://www.sitemason.com/files/dE4JTG/CSTS_mental_health_behavioral_guidelines_response_to_.pandemic_flu_outbreak.pdf
- Maunder R, Hunter J, Vincent L, et al. The immediate psychological and occupational impact of the 2003 SARS outbreak in a teaching hospital. CMAJ 2003;168:1245–1251.
- Chen CS, Wu HY, Yang P, et al. Psychological distress of nurses in Taiwan who worked during the outbreak of SARS. Psychiatric Services 2005;56:76–79.
- McAlonan GM, Lee AM, Cheung V, et al. Immediate and sustained psychological impact of an emerging infectious disease outbreak on health care workers. Canadian Journal of Psychiatry 2007;52:241–247.
- Matsuishi K, Kawazoe A, Imai H, et al. Psychological impact of the pandemic (H1N1) 2009 on general hospital workers in Kobe. Psychiatry and Clinical Neurosciences 2012;66:353–360.
More than 5 years after the H1N1 pandemic of 2009, this paper examines the history of pandemics’ impact in the United States and worldwide, their likely impact in the near future, the current state of preparedness of United States hospitals, and special considerations for hospital operations during a pandemic.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
