Long-Term Cognitive Decline and Coronary Artery Bypass Surgery (CABG)
Long-Term Cognitive Decline and Coronary Artery Bypass Surgery (CABG)
Abstract & Commentary
By John J. Caronna, MD, Professor of Clinical Neurology, Weill Cornell Medical College, New York, NY. Dr. Caronna reports no financial relationships relevant to this field of study. This abstract originally appeared in the July 2008 issue of Neurology Alert.
Synopsis: CABG does not increase the risk of long-term cognitive decline.
Source: Selnes OA, Grega MA, Bailey MM, et al. Cognition 6 years after surgical or medical therapy for coronary artery disease. Ann Neurol 2008;63:581-590.
Enthusiasm for coronary artery bypass grafting (CABG) as an intervention for cardiovascular disease has been tempered by concerns about postoperative cognitive decline. At one month after surgery, up to two-thirds of patients have cognitive decline.1 Those with subtle neurological injury improve to baseline over the first few months after CABG.2 The occurrence of late cognitive decline at 5 or more years after CABG has been reported but without appropriate control subjects.3
Selnes and colleagues conducted a 5-year observational study of patients with coronary artery disease who were treated at Johns Hopkins University Medical Center. Subjects included 152 CABG and 92 nonsurgical control patients treated medically or with percutaneous stents. Patients received baseline, 3-, 12-, 36-, and 72-month cognitive assessments with a comprehensive neuropsychological battery that included the Mini-Mental State Examination (MMSE)3 at all time points.
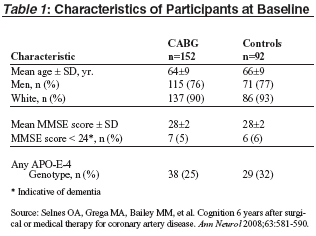
At baseline, the CABG group had lower mean scores for several of the neuropsychological tests but there were no statistically significant differences between the CABG group and the nonsurgical patients in the unadjusted raw scores. (See Table 1.) Both groups showed improvement in cognitive performance from baseline to 12 months. Therefore, to evaluate the amount of decline in cognitive test performance over time for the two groups, the investigators examined change from baseline to 72 months. To address the question of the magnitude of late decline, they compared degree of change in cognitive performance from 12 to 72 months.
 |
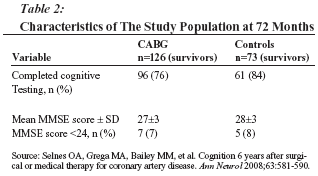
Mild late cognitive decline was observed in both study groups but there were no statistically significant differences between the CABG and control patients in the degree of change from 12 to 72 months for any cognitive domain. There also was no difference between groups in the degree of change from baseline to 72 months in the number of subjects with a MMSE score in the clinically impaired range. (See Table 2.)
 |
The investigators, therefore, concluded that although late cognitive decline does occur in patients who have undergone CABG surgery, the degree of this decline does not differ from that observed in age-matched, nonsurgical patients with coronary artery disease. Their results indicate that there is no syndrome of late cognitive impairment that is specific to the use of cardiopulmonary bypass.
Commentary
The subject of cognitive impairment following CABG surgery received media attention recently following an article in Vanity Fair that suggested Bill Clinton had suffered a personality change since his CABG operation in 2004. Friends were quoted as saying that he was not the same person after surgery. The findings of Selnes and associates should put to rest the worries of Bill Clinton's family and friends, as well as reassuring patients and physicians that there is no increased risk of dementia from CABG surgery. The study is important because it is one of the few to include a control or comparison group of nonsurgical patents. Nevertheless, as pointed out by Yaffe and Covinsky4 in their editorial comments, there was a high "lost-to-followup" rate of about 35% in both groups.
Although, for statistical analysis, one can assume that the lost-to-followup subjects are missing at random, it may be that these patients had more severe underlying disease, lower functional status, and a greater risk for poor cognitive outcome.
It also is disappointing that the study lacked brain MRI studies before surgery in CABG subjects and at baseline and 72 months in both groups. Perhaps additional studies involving neuroradiologists and in larger, more diverse cohorts may identify subgroups at greater risk for late cognitive decline and, therefore, in need of intervention in the form of more aggressive risk factor modification.
References
1. Hogue CW Jr, Palin CA, Arrowsmith JE. Anesth Analg. 2006;103:21-37.
2. Selnes OA, et al. Ann Thoracic Surg. 2003;75:1377-1384.
3. Newman MF, et al. N Engl J Med. 2001;344:395-402.
4. Yaffe K, Covinsky KE. Ann Neurol. 2008;63:547-548.
Enthusiasm for coronary artery bypass grafting (CABG) as an intervention for cardiovascular disease has been tempered by concerns about postoperative cognitive decline.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
