Pediatric Seizures
June 1, 2016
Reprints
AUTHORS
Amber M. Morse, MD, Pediatric Emergency Medicine Fellow, University of Arkansas for Medical Sciences/Arkansas Children’s Hospital, Little Rock
Heather A. Heaton, MD, Instructor of Emergency Medicine, Department of Emergency Medicine, Mayo Clinic, Rochester, MN
PEER REVIEWER
Jeffrey Bullard-Berent, MD, Clinical Professor of Emergency Medicine and Pediatrics, UCSF School of Medicine, San Francisco, CA
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Dietrich (editor), Dr. Skrainka (CME question reviewer), Ms. Wurster (nurse planner), Dr. Morse (author), Dr. Heaton (author), Dr. Bullard-Berent (peer reviewer), Ms. Coplin (executive editor) and Ms. Mark (executive editor) report no relationships with companies related to the field of study covered by this CME activity.
EXECUTIVE SUMMARY
- The most common etiology of neonatal seizures is hypoxic-ischemic encephalopathy, usually manifesting within 48 hours of life. However, infection is an important trigger for seizures in this population and, therefore, providers should have a low threshold to initiate the workup for possible meningoencephalitis.
- Febrile seizures are the most common cause of seizures in the pediatric population between 6 months and 5 years of age.
- A simple febrile seizure consists of a patient between 6 months and 5 years of age; association with fever (temperature > 38.0º C); generalized tonic-clonic seizure activity, spontaneous cessation within 15 minutes, and only one episode in a 24-hour period; brief postictal period and absence of pre-existing neurological abnormality.
- The decision to perform a lumbar puncture should be driven by concerning clinical findings (i.e., meningeal signs, toxic appearance), missing or indeterminate immunization status, or recent antibiotic use that might mask signs and symptoms of meningitis.
- Most experts highlight multiple seizures, focal findings, young age, and high-risk medical history as reasons to have a higher threshold to obtain neuroimaging in the emergency department.
- Electroencephalography (EEG) should be performed within 24 to 48 hours in all patients with unprovoked (afebrile) first-time seizure activity to identify epileptogenic brain activity or pre-existing progressive neurologic abnormalities. Simple febrile seizures do not require EEG.
Seizures in the pediatric population are a common presentation in emergency departments. The astute emergency medicine clinician must have a good understanding of the various types of seizures in pediatric patients, as well as the most common etiologies associated with each type. Additionally, insight into seizure mimics in the pediatric patient is useful for emergency providers given the implications for treatment. Although benzodiazepines remain the first-line therapy for the patient having a seizure, awareness of next steps in therapy is necessary when caring for these patients in status epilepticus.
— Ann M. Dietrich, MD, FAAP, FACEP
DEFINITION OF THE PROBLEM
Pediatric seizures are the most common neurologic emergency of childhood. With significant distinctions in etiology based on age, and subsequent differences in diagnostic evaluation, pediatric seizures require the emergency medicine practitioner to have a clear understanding of both how to treat the patient and how to provide adequate education to those presenting with the child. Furthermore, a clear understanding of age-based seizure mimics is essential to not miss critical alternative diagnoses.
EPIDEMIOLOGY
Seizures affect 4-10% of children at some point during their lifetime, and approximately 150,000 children in the United States experience a new-onset seizure annually. Approximately 25,000 to 40,000 seizures will be an initial afebrile seizure.1,2 Of pediatric patients presenting with new-onset seizures, only 30,000 patients will subsequently develop epilepsy.1 Poorly controlled seizures are the primary risk factor for sudden unexpected death in epilepsy.3 Severity of seizures varies, ranging from self-limited to fatal in as many as 3-4% of patients.3,4
Approximately 10% of pediatric patients presenting to the emergency department (ED) with seizure activity are in status epilepticus, with an annual incidence of more than 80,000.5,6 Status epilepticus is most common in children younger than 2 years of age.6,7 Febrile seizures are the cause in approximately one-third of children in status epilepticus, making it the most common etiology of this event.4,8,9 The mortality rate for status epilepticus is 3-5%.10
ETIOLOGY
The etiology of a pediatric seizure should be considered first by age: neonatal vs. older children. Likewise, the causes differ between febrile seizures and afebrile seizures. Seizure etiology after the neonatal period is reviewed in Table 1.
TABLE 1. COMMON ETIOLOGIES OF SEIZURES AFTER THE NEONATAL PERIOD 4,8,9,11-13,15-16 |
|
|
Febrile |
|
|
Afebrile |
|
|
Status epilepticus |
|
|
Source: Author adapted. |
|
Neonatal Seizures. The neonatal period is defined as birth to 28 days of life. The most common etiology of neonatal seizures is hypoxic-ischemic encephalopathy (HIE), usually manifesting within 48 hours of life.11 From an emergency medicine standpoint, infection is an important trigger for seizures in this population and, therefore, providers should have a low threshold to initiate the workup for possible meningoencephalitis in neonates presenting with seizure activity. The most common organisms in this age group include group B streptococci, herpes simplex virus, Escherichia coli, and Listeria. However, infections also can be congenital or acquired in early life, including toxoplasmosis, rubella, and cytomegalovirus.12
Intracranial hemorrhage accounts for 10% of neonatal seizures, usually related to birth or non-accidental trauma.12 Congenital intracranial abnormalities, such as tuberous sclerosis, pachygyria, or lissencephaly, may manifest as seizures in this age group as well.13 Metabolic derangements, including hypoglycemia, hypocalcemia, hypomagnesemia, hypernatremia, and hyponatremia, may cause seizures and can result from a variety of conditions ranging from inborn errors of metabolism to errors with mixing of infant formula.12
Febrile Seizures
Febrile seizures are the most common cause of seizures in the pediatric population.14 Occurring in 2-5% of the U.S. pediatric population, with peak incidence at 18 months, febrile seizures occur in infants and children between 6 months and 5 years of age.15 The etiology of febrile seizures remains unclear, with theories ranging from the rate of increase of the fever vs. the peak temperature. Furthermore, there might be a genetic predisposition, as 25-40% of patients have a family history of febrile seizures.15,16
Afebrile Seizures
An afebrile pediatric patient who presents with seizures has a vast differential to consider. The seizure might be a de novo presentation of epilepsy or could be a symptom of another process, such as an intracranial tumor or infection, metabolic derangement, ingestion, neurocutaneous syndrome, or non-accidental trauma.
Status Epilepticus
For patients presenting in status epilepticus, a broad differential must be considered. Keeping in mind that approximately one-third of these presentations relate to a fever, additional etiologies include central nervous system infections, trauma, and ingestions.4,8,9
PATHOPHYSIOLOGY
Seizures are convulsions or involuntary muscle contractions coupled with alteration in mental status.17,18 Generalized seizures arise from the bilateral hemispheres of the cerebral cortex. In contrast, focal seizures arise from one region or hemisphere of the brain.17,19 Aberrant electrical activity and subsequent manifestation of the seizure may range from subtle, nonconvulsive events to stereotypic movements to dramatic generalized convulsions. Neonatal seizures are typically more subtle than seizures in older children and adults, given the immature nervous system of the neonate.12
CLINICAL FEATURES
Generalized seizures cause loss of consciousness along with full-body tonic (sustained)-clonic (interrupted) movements, atonia, and/or myoclonic jerking. In contrast, focal seizures can manifest as disturbances in motor/sensory/autonomic function, emotional state, cognition, behavior, or memory with or without alteration in consciousness.17,19 Also of note, focal seizures can progress into generalized seizures at any time. At the cessation of seizure activity, the patient will enter the postictal period, characterized by confusion, fatigue, lethargy, and/or irritability. If the seizure continues unabated for longer than 5 minutes or if there are repetitive seizures without return to baseline consciousness, then the patient has progressed to status epilepticus.18 Any patient who exhibits seizure activity at time of presentation to the ED should be treated as status epilepticus.
Approximately 50% of neonatal seizures present with subtle findings, such as ocular movement or lip smacking; additionally, seizures can be the etiology of abnormal vital signs, such as hypertension, in this patient population.13
Non-convulsive status epilepticus can present in several different ways, including altered mental status, mild confusion, and subtle physical movements and should be considered in patients with inexplicable, sudden changes in mental status or delayed recovery after a seizure.20-22
A focused history will provide valuable information in the child with seizure activity as well. The history should include information about the events preceding the seizure, seizure duration, number of seizures in the past 24 hours, description of the seizure and whether it has any focal aspects (i.e., unilateral movements, eye deviation, head turning), and how the patient acted following cessation of seizure activity. Other pertinent information includes a history of seizures in the patient or family members, anticonvulsant use and recent dosing practices, developmental abnormalities, ventricular shunt or other neurosurgical procedure, recent illness, recent trauma, recent immigration after years in a developing country, and possible exposures.17,19
The initial physical exam focuses on possible causes of the seizure and may be somewhat limited due to active seizure activity or the postictal state. Vital signs should be obtained upon arrival, and include temperature, as elevated temperature may indicate an underlying infectious origin. Other vital signs and physical characteristics, including heart rate, blood pressure, sweating, flushing, and cyanosis, may indicate a toxic exposure or ingestion. Pupil size, symmetry of convulsive movements, and other seizure characteristics should be noted. A head-to-toe investigation of the skin and musculoskeletal system may indicate trauma or physical abuse as a possible cause. However, a normal exam does not obviate the need for concern in the pediatric patient. If there are notable neurological deficits or posturing, they should be evaluated and treated immediately.17,19 In the neonatal population, providers might find clues to the etiology of the seizure from the physical exam. Fevers, a bulging fontanelle, or dysmorphic features may point to the cause of the event.
Febrile Seizures
Febrile seizures are a recognized seizure type. A simple febrile seizure exhibits the following characteristics:
- Patient age between 6 months and 5 years
- Association with fever (temperature > 38.0º C)
- Predominantly generalized tonic-clonic seizure activity
- Spontaneous cessation of convulsion within 15 minutes and only one convulsion in a 24-hour period
- Brief postictal period
- Absence of pre-existing neurological abnormality.14,18
A simple febrile seizure is characterized as a complex febrile seizure if the seizure lasts longer than 15 minutes, if there are recurrent seizures in a 24-hour period, or if there is evidence of focality. The classification of febrile seizures is unique in definition and treatment in comparison to afebrile seizures; continuous febrile seizures are characterized as complex after 15 minutes, whereas afebrile seizures are considered status epilepticus when the event continues beyond 5 minutes.
DIAGNOSTIC STUDIES
Diagnostic studies are directed by the patient's age and clinical presentation. Particularly in the neonatal population, while stabilization of the patient occurs, obtaining a glucose level is imperative. For both nonfebrile and febrile seizure patients, laboratory analysis is of low yield unless the history of present illness or medical history suggests specific diagnostic testing.
Laboratory Analysis: Febrile Seizures
In the vast majority of patients, simple febrile seizures require no more evaluation than that of a child with a fever. Laboratory analysis should be directed by the patient age, history, and physical exam; however, it is frequently unnecessary. The risk of bacteremia, urinary tract infection, and meningitis are similar between children presenting with a simple febrile seizure and those presenting with a fever but no seizure activity.23-26 Hardasmalani et al had no positive blood cultures or positive urine cultures in any of their patients with complex febrile seizures.27 There are similar results recorded by Boyle and Sturm, who showed no positive blood cultures in their population and positive urine cultures in only 4% of patients.28 For children presenting with complex febrile seizures, it is important for emergency medicine providers to know that bacterial meningitis does not typically present with an isolated fever and single seizure.29
Laboratory Analysis: Afebrile Seizures
Traditionally, laboratory analysis, especially blood glucose checks and electrolyte evaluation, has been a common practice when evaluating seizure patients presenting to the ED. Recent studies have shown that laboratory testing is not necessary in children whose consciousness levels have returned to baseline, physical exam findings are normal, and history does not indicate a possible underlying cause.30 In the study by Strobel et al, laboratory studies were obtained in 87% of their study group, with five out of 81 patients exhibiting clinically significant laboratory values. In each of the significant cases, medical history and seizure characteristics would have indicated the need for laboratory testing.31 Consider drawing a blood glucose and electrolyte panel in patients who do not return to baseline; further testing should be directed by the patient’s history and exam.
Lumbar Puncture
Lumbar puncture is not routinely indicated for most seizure patients.19 Most recent studies assessing the need for lumbar puncture have evaluated patients with febrile seizures. In this patient population, meningitis or positive cerebrospinal cultures have varied between zero and 1.8%.14,27,28,32 Since the introduction of the Haemophilus influenzae type b and Streptococcus pneumoniae vaccines, the incidence of bacterial meningitis has dramatically decreased.32 Thus, the decision to perform a lumbar puncture should be driven by concerning clinical findings (i.e., meningeal signs, toxic appearance), missing or indeterminate immunization status, or recent antibiotic use that might mask signs and symptoms of meningitis. Febrile status epilepticus does carry increased risk of meningitis compared to those with simple febrile seizures; lumbar puncture should be strongly considered in this patient population.4,33
Neuroimaging
It is postulated that 8-31% of children presenting to the ED with a first-time nonfebrile seizure will have abnormalities on neuroimaging.34 Acute neuroimaging in the ED is most frequently computed topography (CT), due to its ease of use and availability. However, since CT exposes children to substantial radiation and magnetic resonance imaging (MRI) often is difficult to obtain in the ED, investigators recently have explored neuroimaging abnormalities in patients with first-time seizure to define whether neuroimaging changes ED management or disposition. In other words, they have sought to delineate when neuroimaging is emergent in the ED setting and when a patient can safely obtain outpatient CT or MRI to evaluate for abnormalities contributing to seizure activity. Dayan et al found that 0.8% (3/341) of patients had abnormalities considered emergent/urgent on CT or MRI and only one of the 341 patients required neurosurgery.34 Aprahamian et al showed similar findings with 4.1% (13/319) of patients having emergent/urgent CT or MRI, with only one of the 319 requiring immediate intervention.35 With the low number of abnormalities causing a change in emergency management, certain risk factors have been cited to better guide emergency medicine providers in identifying relevant abnormalities. Most experts highlight multiple seizures, focal findings, young age, and high-risk medical history as reasons to have a higher threshold to obtain neuroimaging in the ED.34-36 Risk factors for abnormal imaging indicating intracranial pathology are listed in Table 2.2,19,37,38
TABLE 2. RISK FACTORS FOR INTRACRANIAL PATHOLOGY ON CT/MRI AFTER FIRST SEIZURE2,19,37-38 |
|
Medical Conditions |
History or Physical Exam Findings |
|
Bleeding disorders |
Anticoagulation therapy Hemophilia von Willebrand's disease |
|
Cerebrovascular disease |
Focal seizure or new focal deficit |
|
Cysticercosis |
Emigrated from an endemic area |
|
HIV/AIDS |
Persistent altered mental status |
|
Hydrocephalus or recent shunt surgery |
Persistent postictal period |
|
Neurocutaneous disorders |
Prolonged seizure (>15 minutes) |
|
Sickle cell disease |
Recent head trauma |
|
Malignancy |
Recent travel to areas endemic with Taenia solium, the pork tapeworm |
|
Source: Author adapted. |
|
Electroencephalography (EEG)
EEG should be performed in all patients with unprovoked (afebrile) first-time seizure activity to identify epileptogenic brain activity or preexisting progressive neurologic abnormalities. Simple febrile seizures do not require EEG. If possible, EEG should be performed within 24 to 48 hours after the seizure, as EEG done in this time frame has a higher yield of significant abnormalities.39 Like neuroimaging, EEG does not necessarily need to be done in the ED, however, and actually may be difficult to obtain in the ED due to ordering policies, EEG technician staffing, and epileptologist reading hours. Emergent EEG is indicated and most helpful in unexplained and prolonged altered level of consciousness, nonconvulsive status epilepticus, and ongoing seizure activity in a pharmacologically paralyzed or comatose patient.19,39,40
DIFFERENTIAL DIAGNOSIS
Idiopathic epilepsy is usually diagnosed after one or more unprovoked seizure episodes that do not have another underlying cause and exhibit abnormal synchronous electrical activity of the brain. The differential diagnosis of seizure disorders is broad, not only because jerking or convulsive non-seizure episodes can mimic seizure activity, but also because seizures can be a manifestation of many underlying abnormalities. Common episodes that can mimic seizure activity are listed in Table 3.17-19,41-43
TABLE 3. SEIZURE MIMICS17-19,41-43 |
|
Event |
Characteristics |
|
Neonatal reflexes |
Startle reflex is frequently mischaracterized as seizure activity |
|
Hyperekplexia |
Marked startling at sudden sounds or touch seen in infants can be so intense it results in total body stiffening and apnea |
|
Spasmus nutans |
Presents with pendular nystagmus, head nodding, and head tilt or abnormal head positioning and can be seen in infants 4 months to 12 months of age |
|
Gastroesophageal reflux |
Associated with feeding; usually presents as arching of back and crying in the conscious child |
|
Breath holding spells |
Preceded by crying or upset child and results in limpness, loss of consciousness, and occasional posturing; typically seen between ages 6 months and 5 years |
|
Shuddering attacks |
Rapid shivering of the head, shoulder, and trunk; can start in infancy and persist through early childhood |
|
Sleep disorders |
Sleep myoclonus includes myoclonic movements that do not disturb or wake the child; sleep terrors can also mimic seizures in young children; narcolepsy can mimic “drop” seizures |
|
Daydreaming |
Reported to have altered responsiveness, but maintains posture and head control and can be interrupted by calling name or touch |
|
Syncopal episode |
Preceded by lightheadedness, dizziness, diaphoresis, palpitations, blurred vision, and/or pallor |
|
Psychogenic |
Keeps eyes tightly closed, avoids painful stimuli, has haphazard limb movements, and has rapid return to normal level of consciousness. May present in early adolescence. Typically female with psychiatric comorbidities. |
|
Panic attack |
Complains of chest pain, shortness of breath, numbness/tingling in hands/feet, and/or contractions of extremities |
|
Post-traumatic seizure |
Jerking or twitching after trauma to the head |
|
Tic disorders |
Repetitive twitching, blinking, or head shaking |
|
Opsoclonus-myoclonus-ataxia syndrome |
Rare syndrome associated with neuroblastoma; repeated, random and rapid eye movements in both horizontal and vertical directions (opsoclonus); unsteady gait (ataxia); brief, repeated, shock-like spasms of several muscles within the arms, legs (myoclonus). Extreme irritability, reduced and fragmented sleep (insomnia), rage attacks, difficulty articulating speech (dysarthria), or inability to speak (mutism), decreased muscle tone (hypotonia), and vomiting are common. |
|
Source: Author adapted. |
|
MANAGEMENT
The goal of the ED team in managing the child with seizure activity is to perform initial stabilization, terminate the seizure, and evaluate and treat any underlying etiologies.
Initial Stabilization
Initial stabilization should utilize Pediatric Advanced Life Support guidelines and focus on airway, breathing, and circulation to provide adequate respiratory and hemodynamic support. Vital signs should be obtained immediately, and the patient should be placed on a full monitor with heart rate, respiratory rate, blood pressure, and pulse oximetry information. One can also consider adding end-tidal CO2 monitoring to better evaluate ventilation status.
Airway and Breathing
- Position the head to ensure airway patency. Consider a nasopharyngeal airway if obstruction is present.
- Suction secretions as needed.
- Place non-rebreather mask to supply 100% oxygen.
- Consider bag-mask ventilation if there are signs of inadequate ventilation and oxygenation. These include inadequate chest rise, poor air movement on auscultation, poor respiratory effort, central cyanosis, and/or oxygen saturation less than 90%.
-
Consider endotracheal intubation in the following situations:
- Severe hypoxia (bradycardia, hypotension, poor perfusion);
- Failure of bag-mask ventilation to provide adequate ventilation;
- Concern for raised intracranial pressure;
- Refractory status epilepticus.
Circulation
- Obtain vascular access to administer anticonvulsants and give fluids to support circulating volume. If an intravenous (IV) line is unsuccessful, then an intraosseous route should be used.18
Termination of Seizures. The antiepileptic drugs (AEDs) found to be the most effective as first-line treatment for seizures are benzodiazepines. They control seizure activity in 63-73% of patients presenting to the ED.44 Historically, lorazepam has been the benzodiazepine of choice in the United States, but comparison of IV lorazepam to IV midazolam and diazepam has found that they are all equally effective in seizure cessation.45 Of note, seizures caused by inborn errors of metabolism in the neonatal population are poorly responsive to conventional therapy.46
Home Care
- The only FDA-approved drug recommended for breakthrough seizures for families and caretakers in the United States at this time is rectal diazepam gel.47
- Other transmucosal routes (buccal, nasal) for benzodiazepines are being studied for their effectiveness, as families and affected children report that they would prefer these routes over rectal diazepam due to ease of use and avoidance of the embarrassment of rectal administration.48
Pre-hospital/EMS Care
- Traditionally, IV lorazepam has been used by paramedics and EMTs for patients with seizure activity. IVs can be difficult to start or take longer than expected, delaying the AED needed for seizure cessation. The delay in medication is an important factor, as the time from seizure onset to AED initiation is significantly related to shorter seizure duration.49 Multiple studies, including the RAMPART and GRADE studies, have investigated various routes and types of benzodiazepines because of this phenomenon.50-52
- Intranasal, buccal, and intramuscular midazolam have been compared to IV diazepam and IV lorazepam and have been found to be as effective in seizure cessation.50-55 In addition, midazolam has a much better shelf life, which is more practical for EMS crews.51
Seizure activity that continues despite benzodiazepines requires a second-line AED. There is less evidence on the preferred second-line medication, as there are no large prospective, randomized, controlled trials to guide treatment.56 However, common second-line medications include phenytoin/fosphenytoin, valproic acid, levetiracetam, and phenobarbital.44,57,58 Each medication has advantages and disadvantages. Valproic acid can cause serious toxicity in children with underlying metabolic disorders and children younger than 2 years of age, while phenobarbital can cause respiratory depression, hypotension, and severe sedation in an already compromised, seizing child.57 Levetiracetam is well-tolerated and has minimal side effects, but experience is still relatively limited. The response to phenytoin, which is perhaps the most commonly used second-line AED, is statistically significantly worse compared to other medications in multiple trials and is particularly ineffective in febrile seizures.57,59 Overall, the choice of second-line, and potentially third-line, treatment is based on patient characteristics, availability at the institution, and consultant recommendation.
Administering continuous infusions and anesthetic medications is considered after failure of traditional second-line AEDs. Even less data exist on these medications or therapies, although almost one-third of seizure patients will enter this stage of refractory status epilepticus.44,57 Like second-line AEDs, many of these agents will be started based on consultant recommendations and institutional traditions. Furthermore, once status epilepticus has continued beyond 24 hours, the patient is considered to be in the super-refractory epilepticus stage, with recommendations based purely on case studies.44
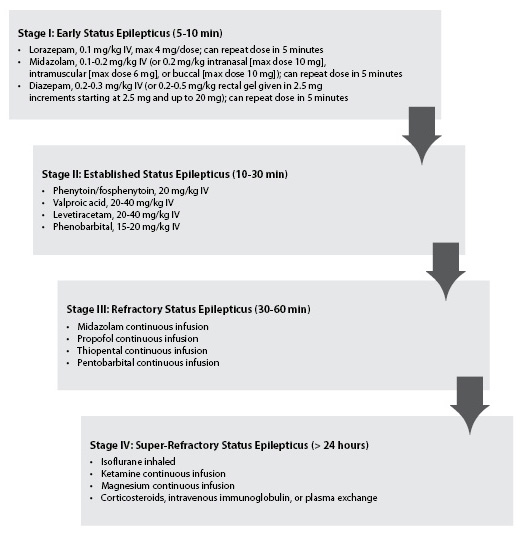
In the ED, most practitioners will be charged with treating Stage I (5 to 10 minutes of seizure activity) and Stage II (10 to 30 minutes of seizure activity) status epilepticus, while only occasionally delving into the realm of Stage III (30 to 60 minutes of seizure activity). Figure 1 delineates treatment options from Stage I of status epilepticus to Stage IV status epilepticus.18,44,60
FIGURE 1. TREATMENT OPTIONS FOR STATUS EPILEPTICUS18,44,58,60 |
 |
|
Source: Author created. |
Several unique therapies exist to treat refractory epilepsy in the pediatric population. The only implantable device currently approved for use in the United States is the vagal nerve stimulator, which delivers a stimulus to terminate seizures when a small magnet is held directly over the device.61 Additionally, some patients may present on a ketogenic diet, in which a starvation state is used to induce ketosis. Occasionally, complications from this, including dehydration, hypoglycemia, and metabolic derangements, might precipitate in a presentation to the ED; providers must be careful when correcting these patients, as in some cases correcting the derangements might worsen seizure activity.62 Providers must be aware of the complications in patients in whom seizure activity is so severe that experimental therapies are used. Although surgery might be beneficial in some of these patients, the complications of bleeding, hematoma formation, and obstructive hydrocephalus must be considered with presentation to the ED.
DISPOSITION
Children with simple febrile seizures can be discharged home safely. Caregivers frequently ask questions regarding risk of recurrence. The risk of febrile seizure recurrence is approximately 33%, with increased risk seen in children younger than 18 months of age, a family history of febrile seizures, a short duration of fever onset before the seizure, and lower temperature at onset of seizure.15,63
Patients with a first-time seizure who present to the ED and have no additional seizure activity and a normal neurological exam also can be discharged home. The decision to place patients with a first-time seizure on an AED is often individualized to an institution or is made in conjunction with a neurology consultant. However, studies have shown that delaying therapy has no bearing on seizure control, unless the child has known abnormalities on EEG or neuroimaging.19 Families should be counseled that outpatient evaluation likely will include additional studies. A timely outpatient EEG is critical, as this is likely the best predictor of recurrence of the seizure.63,64 The overall afebrile seizure recurrence rate is about 54%, with most having a second episode within 2 years of the initial seizure.65,66
Patients with epilepsy who present with infrequent breakthrough seizures can be discharged home safely if they have returned to baseline mental status.18
Children who have received a dose of lorazepam or a long-acting AED should be admitted to the hospital for observation, as they are at increased risk of recurrent seizure activity and/or continued status epilepticus. Those patients with refractory status epilepticus, persistent alterations in consciousness, or dependence on mechanical ventilation (i.e., intubated in the ED) will require admission to the intensive care unit for continuous monitoring and care. These patients often require consultation with neurology to acquire continuous EEG monitoring and to obtain recommendations on preferred treatment for refractory status epilepticus.18
SUMMARY
Seizures are major neurological emergencies that affect many children presenting to the ED. Age, seizure type, and historical features will guide diagnostic workup and treatment options. The ED practitioner’s role in treating the child with seizure activity is to stabilize airway/breathing/circulation, identify underlying precipitants, and abort the seizure activity with antiepileptic medications. Furthermore, understanding the disposition needs of each type of seizure is pertinent knowledge for the ED provider.
REFERENCES
- Hauser WA. The prevalence and incidence of convulsive disorders in children. Epilepsia 1994;35(Suppl 2):S1-S6.
- Hirtz D, Ashwal S, Berg A, et al. Practice parameter: Evaluating a first nonfebrile seizure in children: Report of the quality standards subcommittee of the American Academy of Neurology, The Child Neurology Society, and The American Epilepsy Society. Neurology 2000;55:616-623.
- Nesbitt V, Kirkpatrick M, Pearson G, et al. Risk and causes of death in children with a seizure disorder. Dev Med Child Neurol 2012;54:612-617.
- Chin RF, Neville BG, Peckham C, et al. Incidence, cause, and short-term outcome of convulsive status epilepticus in childhood: Prospective population-based study. Lancet 2006;368:222-229.
- Singh RK, Stephens S, Berl MM, et al. Prospective study of new-onset seizures presenting as status epilepticus in childhood. Neurology 2010;74:636-642.
- Roberts MR, Eng-Bourquin J. Status epilepticus in children. Emerg Med Clin North Am 1995;13:489-507.
- Prasad AN, Seshia SS. Status epilepticus in pediatric practice: Neonate to adolescent. Adv Neurol 2006;97:229-243.
- Haafiz A, Kissoon N. Status epilepticus: Current concepts. Pediatr Emerg Care 1999;15:119-129.
- Lewena S, Pennington V, Acworth J, et al. Emergency management of pediatric convulsive status epilepticus: A multicenter study of 542 patients. Pediatr Emerg Care 2009;25:83-87.
- Raspall-Chaure M, Chin RF, Neville BG, et al. Outcome of paediatric convulsive status epilepticus: A systematic review. Lancet Neurol 2006;5:769-779.
- Minchom P, Niswander K, Chalmers I, et al. Antecedents and outcome of very early neonatal seizures in infants born at or after term. Br J Obstet Gynaecol 1987;94:431-439.
- Zupanc ML. Neonatal seizures. Pediatr Clin North Am 2004;51:961-978, ix.
- Bernes SM, Kaplan AM. Evolution of neonatal seizures. Pediatr Clin North Am 1994;41:1069-1104.
- Teran CG, Medows M, Wong SH, et al. Febrile seizures: Current role of the laboratory investigation and source of the fever in the diagnostic approach. Pediatr Emerg Care 2012;28:493-497.
- Shinnar S, Glauser TA. Febrile seizures. J Child Neurol 2002;17(Suppl 1):S44-S52.
- Blumstein MD, Friedman MJ. Childhood seizures. Emerg Med Clin North Am 2007;25:1061-1086, vii.
- Fleisher GR, Ludwig S. Textbook of Pediatric Emergency Medicine. 6th ed. Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins Health; 2010.
- Sasidaran K, Singhi S, Singhi P. Management of acute seizure and status epilepticus in pediatric emergency. Indian J Pediatr 2012;79:510-517.
- Wilden JA, Cohen-Gadol AA. Evaluation of first nonfebrile seizures. Am Fam Physician 2012;86:334-340.
- Galimi R. Nonconvulsive status epilepticus in pediatric populations: Diagnosis and management. Minerva Pediatr 2012;64:347-355.
- Chang AK, Shinnar S. Nonconvulsive status epilepticus. Emerg Med Clin North Am 2011;29:65-72.
- Greiner HM, Holland K, Leach JL, et al. Nonconvulsive status epilepticus: The encephalopathic pediatric patient. Pediatrics 2012;129:e748-755.
- Teach SJ, Geil PA. Incidence of bacteremia, urinary tract infections, and unsuspected bacterial meningitis in children with febrile seizures. Pediatr Emerg Care 1999;15:9-12.
- Colvin JM, Jaffe DM, Muenzer JT. Evaluation of the precision of emergency department diagnoses in young children with fever. Clin Pediatr (Phila) 2012;51:51-57.
- Shah SS, Alpern ER, Zwerling L, et al. Low risk of bacteremia in children with febrile seizures. Arch Pediatr Adolesc Med 2002;156:469-472.
- Trainor JL, Hampers LC, Krug SE, et al. Children with first-time simple febrile seizures are at low risk of serious bacterial illness. Acad Emerg Med 2001;8:781-787.
- Hardasmalani MD, Saber M. Yield of diagnostic studies in children presenting with complex febrile seizures. Pediatr Emerg Care 2012;28:789-791.
- Boyle DA, Sturm JJ. Clinical factors associated with invasive testing and imaging in patients with complex febrile seizures. Pediatr Emerg Care 2013;29:430-434.
- Green SM, Rothrock SG, Clem KJ, et al. Can seizures be the sole manifestation of meningitis in febrile children? Pediatrics 1993;92:527-534.
- Chen CY, Chang YJ, Wu HP. New-onset seizures in pediatric emergency. Pediatr Neonatol 2010;51:103-111.
- Strobel AM, Gill VS, Witting MD, et al. Emergent diagnostic testing for pediatric nonfebrile seizures. Am J Emerg Med 2015;33:1261-1264.
- Najaf-Zadeh A, Dubos F, Hue V, et al. Risk of bacterial meningitis in young children with a first seizure in the context of fever: A systematic review and meta-analysis. PLoS One 2013;8:e55270.
- Chin RF, Neville BG, Scott RC. Meningitis is a common cause of convulsive status epilepticus with fever. Arch Dis Child 2005;90:66-69.
- Dayan PS, Lillis K, Bennett J, et al. Prevalence of and risk factors for intracranial abnormalities in unprovoked seizures. Pediatrics 2015;136:e351-360.
- Aprahamian N, Harper MB, Prabhu SP, et al. Pediatric first time non-febrile seizure with focal manifestations: Is emergent imaging indicated? Seizure 2014;23:740-745.
- Bautovich T, Numa A. Role of head computed tomography in the evaluation of children admitted to the paediatric intensive care unit with new-onset seizure. Emerg Med Australas 2012;24:313-320.
- Warden CR, Brownstein DR, Del Beccaro MA. Predictors of abnormal findings of computed tomography of the head in pediatric patients presenting with seizures. Ann Emerg Med 1997;29:518-523.
- Sharma S, Riviello JJ, Harper MB, et al. The role of emergent neuroimaging in children with new-onset afebrile seizures. Pediatrics 2003;111:1-5.
- Yigit O, Eray O, Mihci E, et al. The utility of EEG in the emergency department. Emerg Med J 2012;29:301-305.
- Ricardo JA, Franca MC Jr, Lima FO, et al. The impact of EEG in the diagnosis and management of patients with acute impairment of consciousness. Arq Neuropsiquiatr 2012;70:34-39.
- Alam S, Lux AL. Epilepsies in infancy. Arch Dis Child 2012;97:985-992.
-
Tibussek D, Karenfort M, Mayatepek E, et al. Clinical reasoning: Shuddering attacks in infancy. Neurology 2008;70:
e38-41. - Selbst SM, Clancy R. Pseudoseizures in the pediatric emergency department. Pediatr Emerg Care 1996;12:185-188.
- Trinka E, Hofler J, Leitinger M, et al. Pharmacotherapy for status epilepticus. Drugs 2015;75:1499-1521.
- Gathwala G, Goel M, Singh J, et al. Intravenous diazepam, midazolam and lorazepam in acute seizure control. Indian J Pediatr 2012;79:327-332.
- Ficicioglu C, Bearden D. Isolated neonatal seizures: When to suspect inborn errors of metabolism. Pediatr Neurol 2011;45:283-291.
- Pellock JM, Seinfeld S. Is there a need for further trials for the treatment of prolonged seizures? Epileptic Disord 2014;16(Spec No 1):S103-107.
- Chin RF. What are the best ways to deliver benzodiazepines in children/patients with prolonged convulsive seizures? Epileptic Disord 2014;16(Spec No 1):S50-58.
- Seinfeld S, Shinnar S, Sun S, et al. Emergency management of febrile status epilepticus: Results of the FEBSTAT study. Epilepsia 2014;55:388-395.
- Silbergleit R, Lowenstein D, Durkalski V, et al; Neurological Emergency Treatment Trials I. RAMPART (Rapid Anticonvulsant Medication Prior to Arrival Trial): A double-blind randomized clinical trial of the efficacy of intramuscular midazolam versus intravenous lorazepam in the prehospital treatment of status epilepticus by paramedics. Epilepsia 2011;52(Suppl 8):45-47.
- Silbergleit R, Lowenstein D, Durkalski V, et al. Lessons from the RAMPART study — and which is the best route of administration of benzodiazepines in status epilepticus. Epilepsia 2013;54(Suppl 6):74-77.
- Shah MI, Macias CG, Dayan PS, et al. An evidence-based guideline for pediatric prehospital seizure management using GRADE methodology. Prehosp Emerg Care 2014;18(Suppl 1):15-24.
- Javadzadeh M, Sheibani K, Hashemieh M, et al. Intranasal midazolam compared with intravenous diazepam in patients suffering from acute seizure: A randomized clinical trial. Iran J Pediatr 2012;22:1-8.
- Thakker A, Shanbag P. A randomized controlled trial of intranasal-midazolam versus intravenous-diazepam for acute childhood seizures. J Neurol 2013;260:470-474.
- Tonekaboni SH, Shamsabadi FM, Anvari SS, et al. A comparison of buccal midazolam and intravenous diazepam for the acute treatment of seizures in children. Iran J Pediatr 2012;22:303-308.
- Langer JE, Fountain NB. A retrospective observational study of current treatment for generalized convulsive status epilepticus. Epilepsy Behav 2014;37:95-99.
- Sanchez Fernandez I, Abend NS, Agadi S, et al. Gaps and opportunities in refractory status epilepticus research in children: A multicenter approach by the Pediatric Status Epilepticus Research Group (pSERG). Seizure 2014;23:87-97.
- Riviello JJ, Jr., Claassen J, LaRoche SM, et al. Treatment of status epilepticus: An international survey of experts. Neurocrit Care 2013;18:193-200.
- Ismail S, Levy A, Tikkanen H, et al. Lack of efficacy of phenytoin in children presenting with febrile status epilepticus. Am J Emerg Med 2012;30:2000-2004.
- Taketomo CK. Pediatric & Neonatal Dosage Handbook. Hudson, OH: Lexi-Comp Inc.; American Pharmacists Association.
- Kotagal P. Neurostimulation: Vagus nerve stimulation and beyond. Semin Pediatr Neurol 2011;18:186-194.
- Rubenstein JE, Kossoff EH, Pyzik PL, et al. Experience in the use of the ketogenic diet as early therapy. J Child Neurol 2005;20:31-34.
- Berg AT, Shinnar S, Darefsky AS, et al. Predictors of recurrent febrile seizures. A prospective cohort study. Arch Pediatr Adolesc Med 1997;151:371-378.
- Shinnar S, Kang H, Berg AT, et al. EEG abnormalities in children with a first unprovoked seizure. Epilepsia 1994;35:471-476.
- Shinnar S, Berg AT, Moshe SL, et al. The risk of seizure recurrence after a first unprovoked afebrile seizure in childhood: An extended follow-up. Pediatrics 1996;98:216-225.
- Stroink H, Brouwer OF, Arts WF, et al. The first unprovoked, untreated seizure in childhood: A hospital based study of the accuracy of the diagnosis, rate of recurrence, and long term outcome after recurrence. Dutch study of epilepsy in childhood. J Neurol Neurosurg Psychiatry 1998;64:595-600.
Although benzodiazepines remain the first-line therapy, awareness of next steps in therapy is necessary.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
