Wide Rhythm in a Patient with Chest Pain
The ECG in the figure below was obtained from a 44-year-old man who presented to the ED with new-onset chest pain. He was hemodynamically stable at the time this tracing was recorded. If no other history was available, how would you interpret this ECG? What do you suspect is going on clinically?
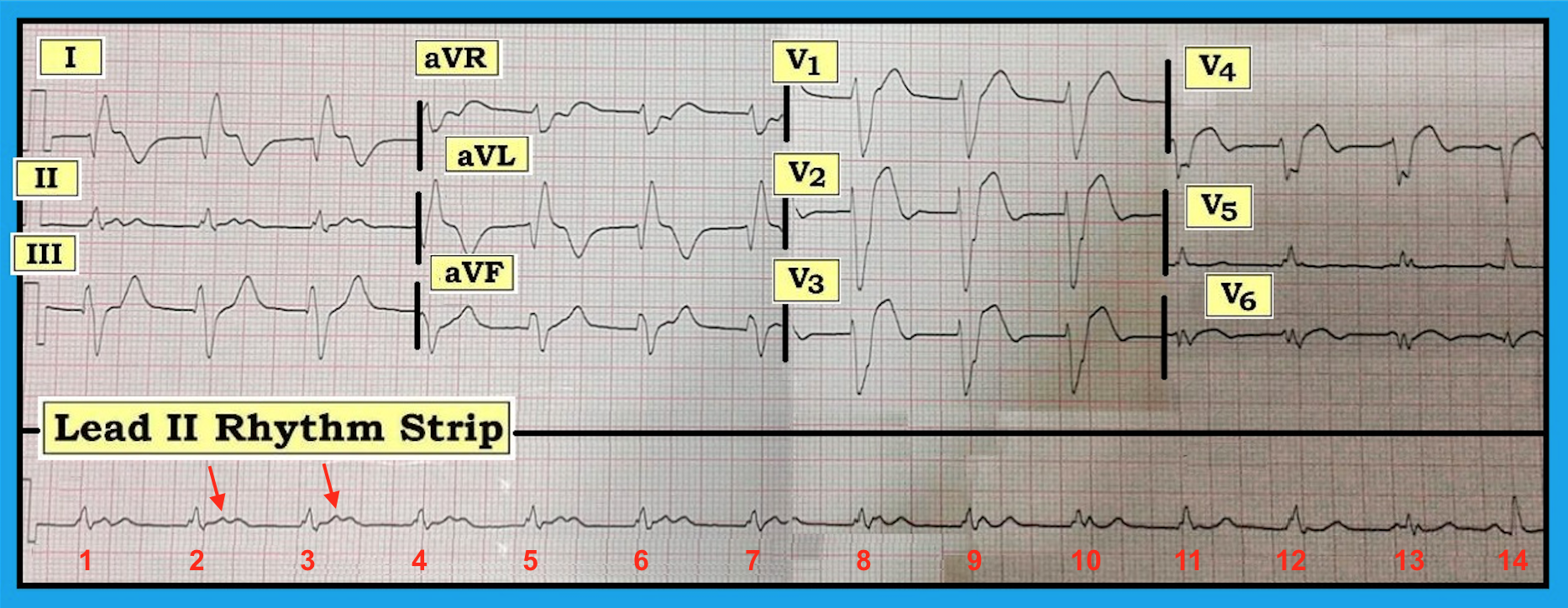
This is a challenging case. Quick perusal of the 12-lead ECG suggests that the QRS complex is markedly widened, at least in most leads on the tracing. The reason the QRS complex does not initially appear to be wide in lead II is that the terminal part of the QRS in this lead is nearly isoelectric to the baseline. That this is the case should be apparent from comparison of lead II with simultaneously recorded leads I and III. Thus, although the QRS complex does not appear to be wide in the long lead II rhythm strip at the bottom of this tracing, the QRS is wide. However, conducting sinus P waves are absent for all but the last two beats on the tracing. The presence of an almost regular wide-QRS rhythm at about 80/minute without sinus-conducted P waves defines these first 12 beats as accelerated idioventricular rhythm (AIVR).
- AIVR is an extremely common reperfusion rhythm in the setting of evolving acute ST elevation myocardial infarction (STEMI).
- On occasion, both Q waves and ST-T wave changes suggestive of ongoing ischemia/infarction may appear in ventricular beats or ventricular rhythms. This appears to be the case here, as there are Q waves, ST elevation, and deep T wave inversion in leads I and aVL beyond that expected for simple AIVR. Additionally, there are reciprocal changes in lead III, and disproportionate J-point ST elevation in leads V1, V2, and V3. In a patient with new chest pain, these findings suggest acute evolving STEMI, with probable reperfusion based on the presence of the AIVR rhythm.
- The other interesting finding relates to atrial activity. Early on, there is AV dissociation (red arrows). Eventually, sinus P waves resume prior to the QRS, with the result that the last beat on the tracing (beat #14) is a sinus-conducted “capture” beat. QRST appearance of this single sinus-conducted beat in simultaneously recorded lateral chest leads shows lack of r wave development by lead V4, and abnormal ST coving plus elevation in leads V4 and V6 that supports our conclusion of evolving STEMI.
For a further discussion of this case, please visit: http://bit.ly/2a2tvP9.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
