Evaluation and Management of Abscesses in the Emergency Department
May 15, 2017
Reprints
AUTHORS
Jonathan Thornton, MD, Emergency Medicine Resident, Mayo Clinic, Rochester, MN
Thomas Hellmich, MD, Emergency Medicine Consultant, Department of Emergency Medicine, Division of Pediatric and Adolescent Emergency Medicine, Mayo Clinic, Rochester, MN
PEER REVIEWER
Jeffrey Bullard-Berent, MD, Clinical Professor of Emergency Medicine and Pediatrics, UCSF School of Medicine, San Francisco, CA
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Farel (CME question reviewer) owns stock in Johnson & Johnson. Ms. Light (nurse planner) reports that she is a retained consultant for Bard Medical. Brian Hocum, PharmD, (pharmacist reviewer) reports that he is an employee of United Therapeutics. Dr. Schneider (editor), Dr. Stapczynski (editor),Dr. Thornton (author), Dr. Hellmich (author), Dr. Bullard-Berent (peer reviewer), Ms. Mark (executive editor), and Ms. Coplin (executive editor) report no financial relationships with companies related to the field of study covered by this CME activity.
EXECUTIVE SUMMARY
- Methicillin-resistant Staphylococcus aureus (MRSA) is the most common isolate from cutaneous abscesses in the United States.
- Bedside ultrasound increases the certainty of abscess diagnosis and localization.
- The majority of cutaneous abscesses can be treated with incision and drainage alone.
- Loop drainage and primary closure following drainage are two reasonable options to traditional incision and drainage.
- Routine culture is not indicated in healthy patients with uncomplicated cutaneous abscesses.
- It is a reasonable option to prescribe oral trimethoprim-sulfamethoxazole after the incision and drainage procedure.
Introduction
Abscesses are common skin and soft tissue infections (SSTI), and their incidence has risen substantially over the years.1-4 Despite the number of patients with abscesses presenting to the emergency department (ED), the management of abscesses varies widely between care providers.5 This article reviews the current management options for simple cutaneous abscesses in patients, including review of the epidemiology, differential diagnosis, diagnostic studies, and changing practice of wound cultures and antibiotic therapy. In addition, this article outlines the essential steps of abscess management, informing practitioners of current best practice options as evidenced by current literature or expert opinion.
Definition/Epidemiology
An abscess is a localized collection of pus resulting from the disintegration of tissue and influx of leukocytes in the dermis and deeper skin tissues. The overlying epidermis may be normal or inflamed in appearance. Cellulitis is an infection of the dermis and subcutaneous tissues. Cellulitis may be purulent (pus producing) or nonpurulent. The overlying skin in a cellulitis infection is warm and erythematous, with indistinct edges as the inflammation spreads from involved tissue to normal tissue. Erysipelas is a variant of nonpurulent cellulitis, with markedly distinct or sharp edges to the erythema and prominent lymphatic involvement. There is variation in the use of these terms and, in some countries, erysipelas is used synonymously with cellulitis.6 Abscesses are thought to begin as a superficial cellulitis that leads to cell liquefaction and debris collection in the dermis with subsequent loculation and abscess formation.6
SSTIs including abscesses are common presentations in the ED. The 2013 National Hospital Ambulatory Medical Care Survey: Emergency Department identified 2.69 million ED visits due to cellulitis and abscess (2.1% of all ED visits in 2013), with incision and drainage procedures reported in 1.16 million (0.9% of all ED visits in 2013).2 The incidence of pediatric abscesses has risen considerably in the past 20 years; Lopez et al found that hospitalizations secondary to SSTIs doubled from 1997-2009.7 SSTIs, especially in children, most frequently are caused by Staphylococcus aureus or Streptococcus pyogenes, together accounting for more than 90% of cases.8 Staphylococcus and Streptococcus are also the primary cause of cutaneous abscesses, but enteric bacteria and anaerobic and Gram-negative organisms are not uncommon depending on the anatomic location. Along with the increasing numbers of cutaneous abscesses, the percentage due to methicillin-resistant S. aureus (MRSA) also is rising.3,9 The incidence of community-acquired MRSA (CA-MRSA) varies by location, race, and age, and is the most common offending agent in many communities, even in patients with no apparent risk factors.1,10-12
Clinical Features
Skin abscesses typically manifest as a focal raised or indurated area that is tender and often fluctuant, with overlying and possibly spreading erythema, warmth, and edema that may or may not have a pustule. (See Figure 1.) Signs of systemic illness are rare with simple abscesses and should prompt a more thorough diagnostic evaluation, including the possibility of bacteremia. Abscesses can be difficult to differentiate from other SSTIs. Marin et al found that the reliability of diagnosis based on clinical exam alone was poor and was not a reliable determinant for the management of abscesses in children.13 Other adjuncts, such as ultrasound, should be used to aid in diagnosis.
Differential diagnosis for a simple abscess includes cellulitis, erysipelas, folliculitis, carbuncles, hidradenitis suppurativa, sebaceous cysts, sporotrichosis, and other soft tissue disorders. Skin abscesses often occur in healthy patients with no apparent risk factors. However, individuals at increased risk for skin abscesses include immunocompromised patients, intravenous drug users, those living in close contact with people with skin infections, those in crowded living conditions, and those with any skin barrier breakdown such as cuts or insect bites.6,14 A history of any skin breakdown or puncture, such as bites, preceding the infection should be elicited, as it may indicate the source of infection and require more targeted therapy.
Figure 1. Subcutaneous Abscess
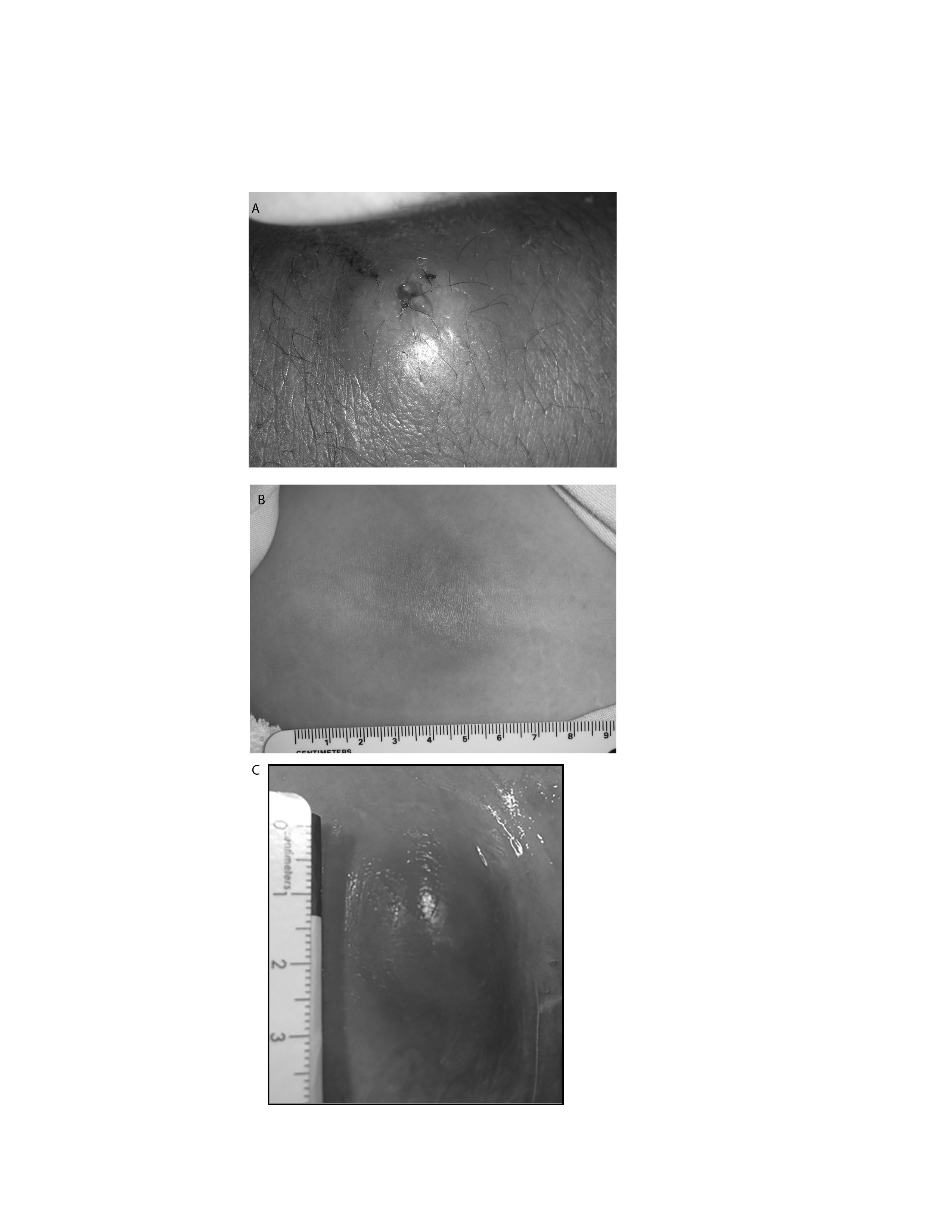
Image A: Cutaneous abscess on dorsum of wrist with seropurulent drainage;
Image B: Cutaneous abscess on buttock with overlying and spreading erythema and edema; Image C: Cutaneous abscess with overlying erythema
Images A and B courtesy of J.S. Stapczynski, MD; Image C used with permission of Mayo Foundation of Medical Education and Research. All rights reserved.
Diagnostic Studies
Diagnosis is based primarily on history and physical exam; however, as mentioned above, exam alone is often unreliable, and adjuncts can be used to ensure the correct diagnosis. Bedside ultrasound is a quick, inexpensive imaging study that can improve the accuracy of diagnosis.15-18 An abscess will be represented by a hypoechoic or anechoic area of fluid collection. (See Figure 2.) Ultrasound also can be helpful prior to incision and drainage (I&D) to identify the best place for incision to ensure that the entire abscess will be drained. Ultrasound after I&D also can be used to ensure that the entire abscess was drained and there are no remaining loculations with persistent fluid collections. With the continued advancement of ultrasound use in the ED, it is becoming best practice to evaluate and confirm abscesses with ultrasound.
When MRSA first emerged as a problem in the 1990s, it was considered reasonable to obtain culture and sensitivities to help guide treatment. Now studies have shown that abscess cultures and sensitivities are less relevant in simple uncomplicated skin abscess, even those with MRSA.19 The 2014 Infectious Diseases Society of America (IDSA) guidelines recommend culture with sensitivities of purulent moderate abscesses defined as having associated signs of systemic illness. Simple or mild abscesses do not necessarily need a culture with sensitivities.4
The American College of Emergency Physicians (ACEP) “Choosing Wisely” campaign recommends against obtaining wound cultures after incision and drainage of uncomplicated skin and soft tissue abscesses with adequate follow-up because the results generally will not alter treatment.20 Culture and sensitivities can be helpful if there is abscess recurrence or antibiotic failure; however, routine collection is not necessary and should be collected only when results may alter the treatment plan. Laboratory studies and blood cultures typically are not recommended or required for simple abscess evaluation. If the patient has signs of systemic illness or is immunocompromised, consider additional laboratory tests (CBC, chemistry panel, lactate) to evaluate for occult sepsis and blood cultures to check for bacteremia.
Figure 2. Ultrasound Appearance of Cutaneous Abscesses
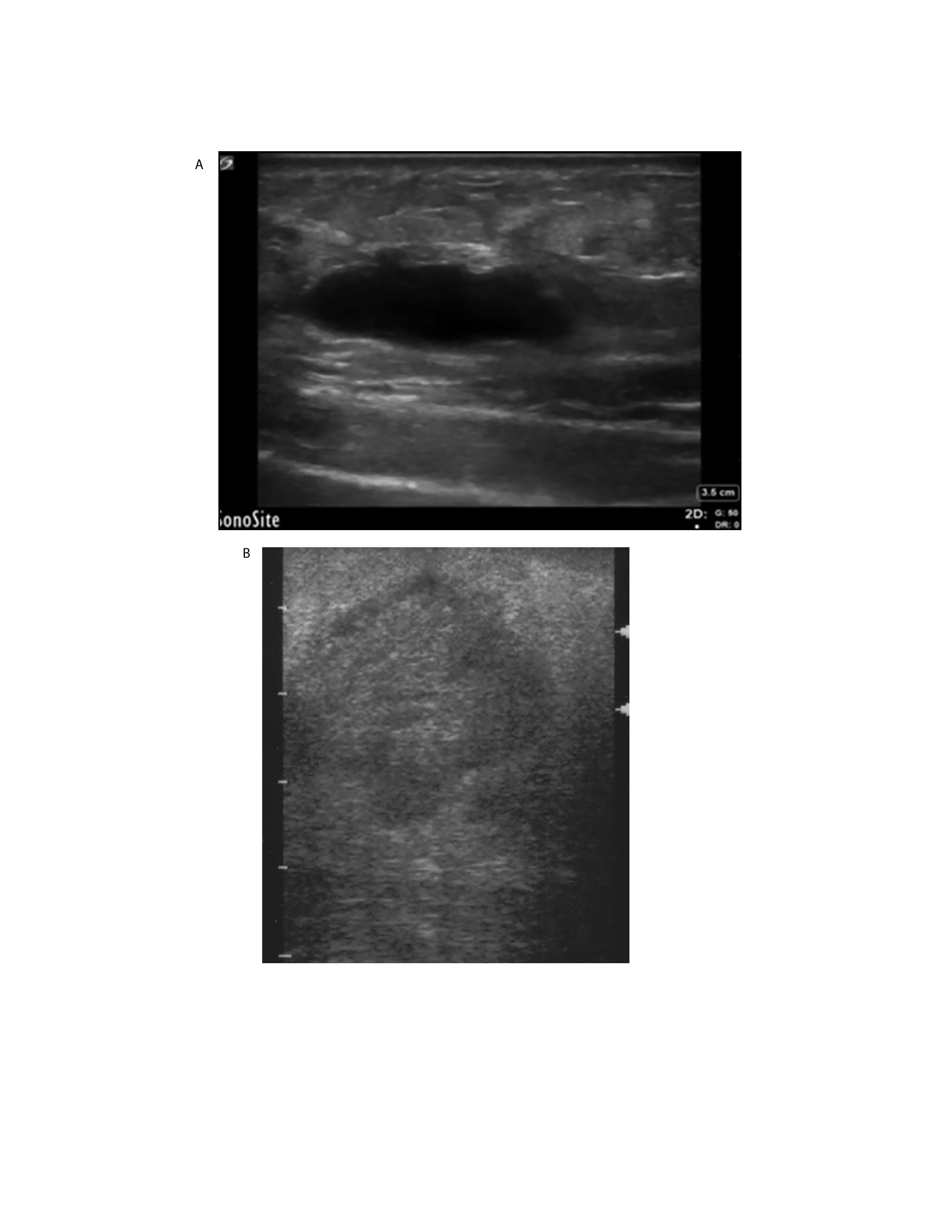
Image A: Ultrasound of abscess with clear anechoic fluid collection
Image B: Ultrasound of buttock abscess with hypoechoic fluid collection showing internal echoes consistent with purulent debris
Image A used with permission of Mayo Foundation for Medical Education and Research. All rights reserved. Image B courtesy J.S. Stapczynski, MD.
Management
Surveys of physicians have found that the management of simple cutaneous abscesses varies widely and is based mostly on personal experience and anecdotal evidence.21 Historically, there have been three major options for the management of the simple abscess: I&D alone, I&D plus antibiotics against methicillin-sensitive S. aureus (MSSA), or I&D plus antibiotics with coverage for MRSA. Physician preference for these three options can be quite split when presented with a case in which all of these options may be reasonable.5
Needle aspiration is also an option, but is used infrequently and generally is not recommended for simple cutaneous skin and soft tissue abscesses. It is also quite common for the clinician to be faced with early abscess-like SSTI with erythema, induration, no fluctuance, and an ultrasound that is negative for a fluid collection. In cases of a suspected evolving abscess — often referred to as “not ripe abscess” — supportive care, including warm compresses, analgesia, and close follow-up, is recommended.
Antibiotics Are Not Necessary
Historically, studies of I&D alone compared to I&D followed by post-procedure oral antibiotics have shown no difference in outcome.22-25 Thus, in immunocompetent patients without other significant comorbidities and a single simple cutaneous abscess that has not been previously treated, it is reasonable to treat with I&D alone.
The studies from which the I&D alone approach is supported primarily come from an era before the increase in MRSA as a cause for cutaneous abscess. Thus, I&D alone may not be relevant given the prevalence of MRSA as a cause for skin abscesses. Small, observational studies did not find a benefit to oral antibiotic coverage after I&D of simple cutaneous abscesses when MRSA was present.25,26
However, in 2016, a large (1,247 intention-to-treat patients), multisite (five U.S. EDs), randomized trial comparing oral trimethoprim-sulfamethoxazole (320 mg and 1,600 mg, respectively, twice daily, for 7 days) with placebo in patients 12 years of age and older after I&D of a cutaneous abscess was published.27 In patients who completed the protocol, clinical cure occurred in 92.9% of the trimethoprim-sulfamethoxazole group vs. 85.7% of the placebo group. The number needed to treat to increase this beneficial outcome by one individual was about 14 patients (95% confidence interval; 9-31 patients). Trimethoprim-sulfamethoxazole was superior to placebo with most secondary outcomes, such as lower rates of subsequent surgical drainage procedures, skin infections at new sites, and infections in household members 7 to 14 days after the treatment period. Of note, 45.3% of the study participants had wound cultures that were positive for MRSA.
While this well-done study was supportive of routine trimethoprim-sulfamethoxazole after I&D, the historical cure rates of cutaneous abscesses and those seen in the antibiotic studies (including this one) justify that the I&D approach is still reasonable in many ED patients.25,26
There is potential for transient bacteremia to be induced by the I&D procedure. In immunocompetent patients, this transient bacteremia is handled by the immue system and is of no practical clinical consequence, similar to the transient bacteremia associated with dental cleaning procedures. In patients with structural cardiac conditions who are at increased risk for endocarditis (e.g., prosthetic cardiac valve), pre-procedure antibiotic prophylaxis is recommended by the American Heart Association to reduce the risk of the transient bacteremia developing into infective endocarditis.28
The IDSA 2014 guidelines for the management of SSTI abscesses4 recommend I&D, Gram stain and culture of exudate, and use of antibiotics based only on the signs of systemic infection (fever, tachypnea, tachycardia, leukocytosis). (See Figure 3.) Recurrent abscesses should be treated similarly; however, recurrence should prompt evaluation for an underlying condition, and treatment should be directed based on culture and sensitivity results.
As already discussed above, the ACEP “Choosing Wisely” campaign also has concluded that antibiotics are not necessary for simple abscesses in healthy individuals, and cultures should be obtained only if results will alter management. Antibiotics are indicated only for patients with severe or extensive disease, rapid progression in the presence of cellulitis, signs and symptoms of systemic illness (temperature > 38º C), tachycardia, tachypnea, abnormal white blood cells (WBCs), associated comorbidities or immunosuppression, extremes of age, abscesses in areas difficult to drain, associated septic phlebitis, or prior lack of response to incision and drainage.22 (See Table 1.) Figure 3 outlines a basic algorithm to follow for treatment of a simple cutaneous abscess.
Figure 3. Simple Cutaneous Abscess Management Algorithm
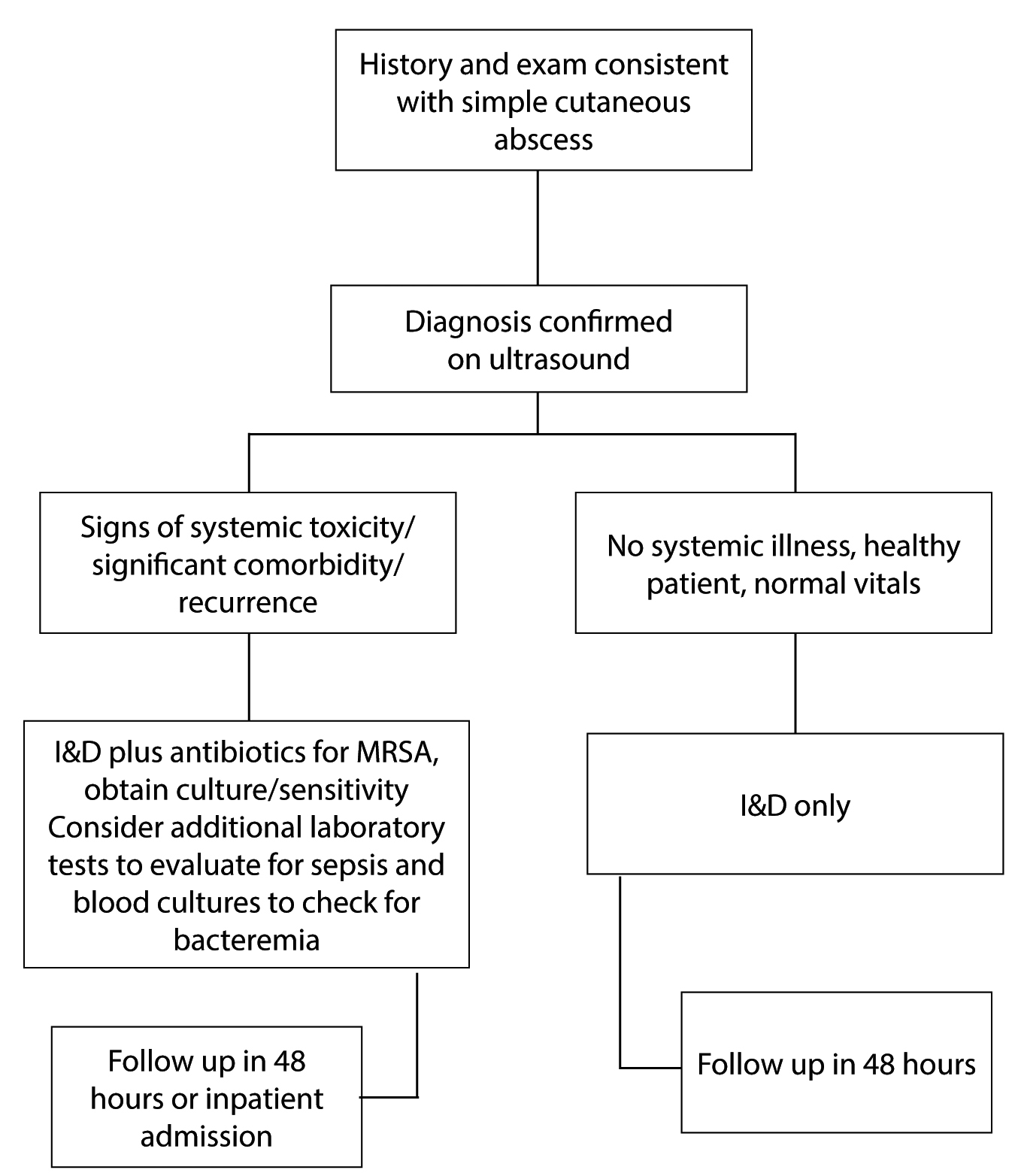
Table 1. Indications for Antibiotics
|
Severe or extensive disease |
|
Rapid progression with cellulitis |
|
Signs of systemic illness:
|
|
Associated comorbidities or immunosuppression |
|
Extremes of age |
|
Abscess difficult to drain |
|
Associated septic phlebitis |
|
Prior treatment failure |
Incision and Drainage
I&D is the ultimate definitive treatment for any simple skin and soft tissue abscess. After clinical diagnosis suggests an abscess, bedside ultrasound is recommended to confirm the fluid collection, determine its size and nature (e.g., loculations), and locate any possible surrounding vascular structures or foreign bodies. Several factors should be addressed when determining whether a particular abscess is amenable to drainage in the ED.
The pre-procedure plan should evaluate pain and sedation needs, identify availability of adequate resources to perform the procedure appropriately in the allotted time, and ensure that there are no significant contraindications to performing the procedure in the ED, such as abscesses that are extremely large or deep, in sensitive areas, or in close proximity to blood vessels or nerves. If all of these issues cannot be addressed, then surgical consultation may be necessary. Table 2 outlines the essential steps of I&D; certain details may need to be tailored to specific needs of the patient on a case-by-case basis.
Table 2. Incision and Drainage Guideline for Simple Cutaneous Abscess29
- Assemble required equipment including personal protective equipment, cleansing agent, local anesthetic, syringe and needle, gauze, scalpel, hemostat, saline, and materials for dressing.
- Obtain informed consent and discuss risks and benefits with the patient or family member(s).
- Ensure tetanus immunization is up to date.
- Treat with prophylactic antibiotics if high-risk cardiac lesions.
- Wear personal protective equipment including face mask with eye shield, gown, and gloves. The procedure is not sterile; however, protect yourself from bodily fluids as contents of abscesses can sometimes be under considerable pressure.
- Clean the identified area thoroughly with chlorhexidine or similar agent.
- Administer systemic analgesia/anxiolysis/sedation.
- Inject local anesthetic generously to include the subcutaneous areas around the abscess as well as deeper tissues. Consider a regional block, if applicable.
- Make a linear incision parallel to Langer or tension lines, if possible, to improve wound healing and scar formation using the scalpel. Incision should be large and deep enough to explore the entire abscess and allow spontaneous drainage of purulent material. Gentle pressure around the abscess can be applied to expel as much purulent material as possible.
- Consider wound culture.
- Insert hemostat into the abscess and bluntly dissect any loculations. Consider bedside ultrasound to ensure adequate drainage.
- Irrigate the wound with normal saline.
- Consider packing wound depending on size.
- Consider post-procedure antibiotics.
- Dress the wound.
- Review final disposition.
Factors to Consider for I&D
Pain control during I&D is a major issue, as this is a very painful procedure. A survey of both patients and practitioners identified abscess I&D as the second most painful ED procedure — second only to nasal intubation.30 Local anesthetics often are not adequate for pain control. Depending on the location, a regional block may be helpful. A regional block proximal to the abscess avoids the limiting effects of the acidic nature of the abscess and may negate the need for repeat dosing of anesthetic as the procedure progresses.
In children, procedural sedation should be considered in addition to local/regional anesthetics. Appropriate sedation will ensure pain and anxiety control, facilitating proper exploration and drainage of the abscess by the practitioner performing the procedure. A frank discussion with parents and/or patients regarding all of the possible treatment options is recommended, as well as utilizing shared decision-making to come up with the best plan of action for each individual patient. At a minimum, oral analgesia is recommended.
Irrigation/Packing
Irrigation of the wound after I&D generally is recommended to help remove debris from the wound; however, there is little evidence to support this practice. Packing the wound after I&D is highly variable among physicians, although the majority of practitioners still pack the wound.21 Packing is believed to ensure that the wound stays open to allow adequate drainage and healing by secondary intention. Several studies have shown that the practice of wound packing is unnecessary, with no increase in recurrence without packing, and may actually increase pain.31-33
Packing should be considered for problematic cases, such as pilonidal abscesses and abscesses > 5 cm. If packing is placed, it can be assessed for removal in 24 to 48 hours. Packed wounds that are still draining at 48 hours can be repacked and re-evaluated again in 48 hours. If the wound has stopped draining after 48 hours, the packing can be removed and the wound allowed to heal by secondary intention with routine follow-up.
Healing
Secondary intention — the process of leaving the wound open and allowing it to heal naturally — is common practice in the management of abscesses after I&D. Allowing the wound to heal by secondary intention facilitates ongoing drainage and is thought to decrease the risk of abscess re-accumulation, but it increases the risk of scarring and the time for wound closure compared to primary closure.
Several randomized trials have shown that primary closure with sutures has similar failure and recurrence rates compared to healing by secondary intention and would provide better cosmetic results.34,35 Primary closure should be considered for very large abscesses and those abscesses in locations that are cosmetically sensitive. Primary closure after abscess I&D is infrequent in the United States, but based on published experience primarily in other countries, primary closure can be a reasonable option.
Other Techniques
Although conventional I&D is the most common and widely accepted technique for drainage of a simple abscess, other techniques have been proposed and have the potential to be less invasive and less painful with quicker healing times. The loop technique has been shown in multiple studies to be an effective technique with similar outcomes to conventional I&D.36,37
This technique involves making a small stab incision on each side of the abscess, followed by wound exploration, irrigation, and drainage. Afterward, a vessel loop drain is introduced through one incision and pulled out the other, tied to itself, and left in place until drainage stops and the loop can be removed. (See Figure 4.) This is a promising technique that has been shown to be effective in small studies and is standard of practice in some places. Appropriate follow-up with a provider comfortable with assessing and removing the drain would be important prior to considering this technique.
Figure 4. Loop Technique36
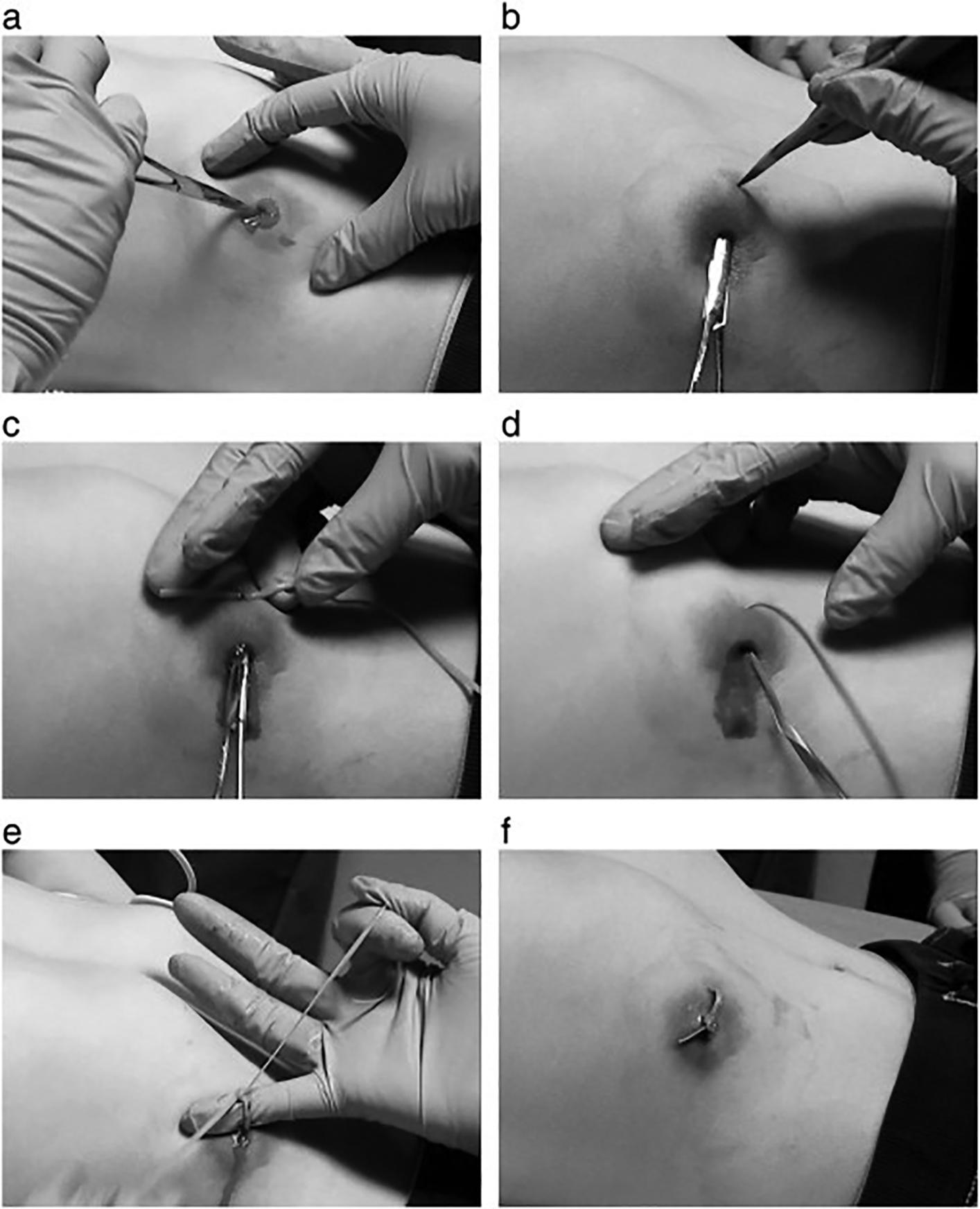
Reprinted from: Ladde JG, Baker S, Rodgers CN, et al. The loop technique: A novel incision and drainage technique in the treatment of skin abscesses in a pediatric ED. Am J Emerg Med 2015;33:272, with permission from Elsevier.
Another technique is ultrasound-guided needle aspiration of an abscess, which is potentially less invasive and painful with decreased cosmetic concerns. However, prospective studies have shown that this technique is not reliable for obtaining any purulent material despite ultrasound guidance and, in general, is not a recommended treatment option.38
Expert Consultation
Most cutaneous abscesses can be managed in an office or ED setting; however, surgical consultation may be necessary in certain cases. Consider consultation for abscesses that are very large, complex, or in sensitive areas such as the hands, face, or breasts. Ultrasound should be used to ensure that there are no critical structures such as vessels or nerves around the abscess that may complicate drainage in the ED.
Pilonidal abscesses often are drained in the ED for symptomatic pain relief but recurrent episodes may need referral to surgery for excision of sinus tracts. (See Figure 5.) Abscesses in the rectal area should be evaluated for fistula and may require surgical consultation. Provider comfort level with the procedure, as well as discussion with the patient or family, always should be used to guide treatment.
Figure 5. Pilonidal Abscess
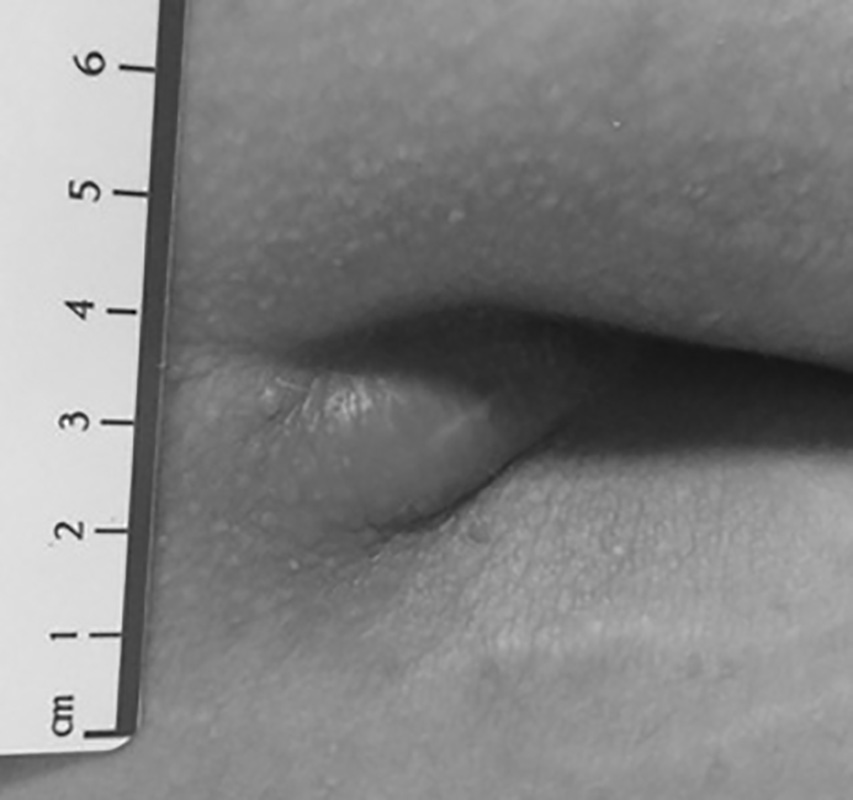
Used with permission of Mayo Foundation for Medical Education and Research.
All rights reserved.
Antibiotics
As discussed, antibiotics generally are not required for the management of a simple cutaneous abscess. Antibiotics should be considered for patients with severe or extensive disease, rapid progression in the presence of cellulitis, signs and symptoms of systemic illness (temperature > 38º C), tachycardia, tachypnea, abnormal WBCs, associated comorbidities or immunosuppression, extremes of age, abscess in areas difficult to drain, associated septic phlebitis, or prior lack of response to incision and drainage. If antibiotics are prescribed, an antibiotic with activity against MRSA should be used empirically, then tailored according to culture sensitivity results. (See Table 3.) Local antibiotic resistance also should be considered when choosing antibiotics.
Table 3. Antibiotics with MRSA Coverage
Antibiotic |
Dose |
Comments |
|
TMP/SMX |
Pediatrics: 4-6 mg/kg/dose (TMP component) PO twice daily Adults: 320/1,600 mg (two DS tablets) PO twice daily |
Does not cover Streptococcus. First-line oral therapy is not recommended for women in the third trimester of pregnancy and for children younger than 2 months of age. |
|
Doxycycline |
Pediatrics: 2 mg/kg/dose (max dose 100 mg) PO twice daily Adults: 100 mg PO twice daily |
Not recommended for children younger than 8 years |
|
Clindamycin |
Pediatrics 10-13 mg/kg/dose PO/IV every 6-8 h (max dose 40 mg/kg per day) Adults: 300-600 mg PO every 8 h |
Check local resistance rates; use only if local resistance < 10-15%. The medication has a bad taste; adherence may be difficult |
|
Vancomycin |
1 month-11 years old: 10-15 mg/kg/dose IV every 6-8 h (max dose 1 g) 12-16 years old: 10-15 mg/kg/dose IV every 12 h Adults: 10-15 mg/kg/dose IV every 8-12 h |
IV treatment choice |
|
Linezolid |
< 5 years: 10 mg/kg/dose 3 times daily IV/PO > 5 years: 10 mg/kg/dose 2 times daily IV/PO, |
May cause myelosuppression |
Disposition
Typically in healthy individuals, outpatient treatment with primary care follow-up is sufficient. If antibiotic coverage is deemed necessary for a simple, uncomplicated skin and soft tissue abscess, outpatient oral antibiotics usually are adequate. Patients should follow up with their primary care physician, an urgent-care type clinic, or return to the ED within 48 hours to ensure appropriate response. If packing was placed, it can be evaluated for removal or removal and replacement at that time. If symptoms are resolving and no packing is in place, the patient can follow up in approximately one week for final exam to ensure resolution.
After packing is removed, patients should be given instructions for frequent soaking of the abscess in warm, soapy water. Patients also should be counseled on adequate pain control as an outpatient. Nonsteroidal anti-inflammatory drugs or acetaminophen may be sufficient for smaller abscesses; however, short-term opioid prescriptions may be necessary for larger abscesses in painful areas.
Patients with systemic disease or underlying comorbidities may require parenteral antibiotics and admission to the hospital. Decolonization may be considered for recurrent MRSA infections, but the success of durable MRSA eradication is controversial. These regimens often include applying mupirocin ointment to the nares and/or chlorhexidine scrubs or dilute bleach baths.39,40
Summary
In summary, abscesses are a very common presentation in the ED. MRSA is the most common isolate of these abscesses, regardless of risk factors. History and physical exam combined with ultrasound should be used to diagnose abscesses. I&D is the ultimate treatment with careful attention to pain and anxiety control during the procedure. Antibiotics should be used only in the setting of systemic illness or with patients who have other medical comorbidities and should cover MRSA. Follow up should be obtained within 48 hours to ensure appropriate resolution of the abscess.
REFERENCES
1. Singer AJ, Talan DA. Management of skin abscesses in the era of methicillin-resistant Staphylococcus aureus. N Engl J Med 2014;370:1039-1047.
2. National Hospital Ambulatory Medical Care Survey: 2013 Emergency Department Summary Tables. Found at https://www.cdc.gov/nchs/data/ahcd/nhamcs_emergency/2013_ed_web_tables.pdf. Accessed April 29, 2017.
3. Pallin DJ, Egan DJ, Pelletier AJ, et al. Increased US emergency department visits for skin and soft tissue infections, and changes in antibiotic choices, during the emergence of community-associated methicillin-resistant Staphylococcus aureus. Ann Emerg Med 2008;51:291-298.
4. Stevens DL, Bisno AL, Chambers HF, et al; Infectious Diseases Society of America. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis 2014;59:e10-e52.
5. Hammond SP, Baden LR. Management of skin and soft-tissue infection — polling results. N Engl J Med 2008;359:e20.
6. Kelly EW, Magilner D. Chapter 152. Soft Tissue Infections. In: Tintinalli JE, et al. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 8th ed. New York: McGraw-Hill Education; 2016.
7. Lopez MA, Cruz AT, Kowalkowski MA, et al. Trends in resource utilization for hospitalized children with skin and soft tissue infections. Pediatrics 2013;131:e718-725.
8. Darmstadt GL. Oral antibiotic therapy for uncomplicated bacterial skin infections in children. Pediatr Infect Dis J 1997;16:227-240.
9. Taira BR, Singer AJ, Thode HC Jr, et al. National epidemiology of cutaneous abscesses: 1996 to 2005. Am J Emerg Med 2009;27:289-292.
10. Fridkin SK, Hageman JC, Morrison M, et al. Methicillin-resistant Staphylococcus aureus disease in three communities. N Engl J Med 2005;352:1436-1444.
11. Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med 2006;355:666-674.
12. Magilner D, Byerly MM, Cline DM. The prevalence of community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA) in skin abscesses presenting to the pediatric emergency department. N C Med J 2008;69:351-354.
13. Marin JR, Bilker W, Lautenbach E, et al. Reliability of clinical examinations for pediatric skin and soft-tissue infections. Pediatrics 2010;126:925-930.
14. Gordon RJ, Lowy FD. Bacterial infections in drug users. N Engl J Med 2005;353:1945-1954.
15. Tayal VS, Hasan N, Norton HJ, et al. The effect of soft-tissue ultrasound on the management of cellulitis in the emergency department. Acad Emerg Med 2006;13:384-388.
16. Squire BT, Fox JC, Anderson C. ABSCESS: Applied bedside sonography for convenient evaluation of superficial soft tissue infections. Acad Emerg Med 2005;12:601-606.
17. Iverson K, Haritos D, Thomas R, et al. The effect of bedside ultrasound on diagnosis and management of soft tissue infections in a pediatric ED. Am J Emerg Med 2012;30:1347-1351.
18. Marin JR, Dean AJ, Bilker WB, et al. Emergency ultrasound-assisted examination of skin and soft tissue infections in the pediatric emergency department. Acad Emerg Med 2013;20:545-553.
19. Schmitz GR. How do you treat an abscess in the era of increased community-associated methicillin-resistant Staphylococcus aureus (MRSA)? J Emerg Med 2011;41:276-281.
20. American College of Emergency Medicine. [press release] Choosing Wisely: Five things physicians and patients should question. Dallas, TX: American College of Emergency Medicine; 2013. Available at: http://www.choosingwisely.org/societies/american-college-of-emergency-physicians/. Accessed Dec. 5, 2015.
21. Schmitz G, Goodwin T, Singer A, et al. The treatment of cutaneous abscesses: Comparison of emergency medicine providers’ practice patterns. West J Emerg Med 2013;14:23-28.
22. Duong M, Markwell S, Peter J, et al. Randomized, controlled trial of antibiotics in the management of community-acquired skin abscesses in the pediatric patient. Ann Emerg Med 2010;55:401-407.
23. Hankin A, Everett WW. Are antibiotics necessary after incision and drainage of a cutaneous abscess? Ann Emerg Med 2007;50:49-51.
24. Llera JL, Levy RC. Treatment of cutaneous abscess: A double-blind clinical study. Ann Emerg Med 1985;14:15-19.
25. Rajendran PM, Young D, Maurer T, et al. Randomized, double-blind, placebo-controlled trial of cephalexin for treatment of uncomplicated skin abscesses in a population at risk for community-acquired methicillin-resistant Staphylococcus aureus infection. Antimicrob Agents Chemother 2007;51:4044-4048.
26. Lee MC, Rios AM, Aten MF, et al. Management and outcome of children with skin and soft tissue abscesses caused by community-acquired methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis J 2004;23:123-127.
27. Talan DA, Mower WR, Krishnadasan A, et al. Trimethoprim-sulfamethoxazole versus placebo for uncomplicated skin abscesses. N Engl J Med 2016;374:823.
28. Wilson W, Taubert KA, Gewitz M, et al. Prevention of infective endocarditis: Guidelines from the American Heart Association: A guideline from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anesthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation 2007;116:1736-1754.
29. Fitch MT, Manthey DE, McGinnis HD, et al. Videos in clinical medicine. Abscess incision and drainage. N Engl J Med 2007;357:e20.
30. Singer AJ, Richman PB, Kowalska A, et al. Comparison of patient and practitioner assessments of pain from commonly performed emergency department procedures. Ann Emerg Med 1999;33:652-658.
31. O’Malley GF, Dominici P, Giraldo P, et al. Routine packing of simple cutaneous abscesses is painful and probably unnecessary. Acad Emerg Med 2009;16:470-473.
32. Kessler DO, Krantz A, Mojica M. Randomized trial comparing wound packing to no wound packing following incision and drainage of superficial skin abscesses in the pediatric emergency department. Pediatr Emerg Care 2012;28:514-517.
33. Leinwand M, Downing M, Slater D, et al. Incision and drainage of subcutaneous abscesses without the use of packing. J Pediatr Surg 2013;48:1962-1965.
34. Singer AJ, Thode HC Jr, Chale S, et al. Primary closure of cutaneous abscesses: A systematic review. Am J Emerg Med 2011;29:361-366.
35. Singer AJ, Taira BR, Chale S, et al. Primary versus secondary closure of cutaneous abscesses in the emergency department: A randomized controlled trial. Acad Emerg Med 2013;20:27-32.
36. Ladde JG, Baker S, Rodgers CN, et al. The loop technique: A novel incision and drainage technique in the treatment of skin abscesses in a pediatric ED. Am J Emerg Med 2015;33:271-276.
37. Tsoraides SS, Pearl RH, Stanfill AB, et al. Incision and loop drainage: A minimally invasive technique for subcutaneous abscess management in children. J Pediatr Surg 2010;45:606-609.
38. Gaspari RJ, Resop D, Mendoza M, et al. A randomized controlled trial of incision and drainage versus ultrasonographically guided needle aspiration for skin abscesses and the effect of methicillin-resistant Staphylococcus aureus. Ann Emerg Med 2011;57:483-941.
39. Kaplan SL, Forbes A, Hammerman WA, et al. Randomized trial of “bleach baths” plus routine hygienic measures vs routine hygienic measures alone for prevention of recurrent infections. Clin Infect Dis 2014;58:679-682.
40. Finnell SM, Rosenman MB, Christenson JC, et al. Decolonization of children after incision and drainage for MRSA abscess: A retrospective cohort study. Clin Pediatr 2015;54:445-450.
This article reviews the current management options for simple cutaneous abscesses in patients, including review of the epidemiology, differential diagnosis, diagnostic studies, and changing practice of wound cultures and antibiotic therapy.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
