Sexually Transmitted Infections in Adolescents
July 1, 2017
Reprints
AUTHORS
Taryn Taylor, MD, Assistant Professor of Pediatrics and Emergency Medicine, Emory University School of Medicine, Atlanta, GA
Lauren Middlebrooks, MD, Emory University School of Medicine, Atlanta, GA
PEER REVIEWER
Catherine A. Marco, MD, Professor of Emergency Medicine, Wright State University Boonshoft School of Medicine, Kettering, OH
Executive Summary
- As defined by the United States Preventive Services Task Force, high-risk sexual behavior involves having multiple current sexual partners, having a new partner, using condoms inconsistently, having sex while under the influence of alcohol or drugs, or having sex in exchange for money or drugs.
- Sexually transmitted infections can be divided into two categories based on clinical presentation: genital ulcers and discharge syndromes. Genital ulcer syndromes may be painful, such as genital herpes simplex virus (HSV) and chancroid, or painless, such as syphilis. Discharge syndromes include gonorrhea, nongonococcal urethritis, chlamydia, mucopurulent cervicitis, Trichomonas vaginalis, and urethritis.
- Chlamydia is the most common sexually transmitted infection reported annually to the Centers for Disease Control and Prevention (CDC).
- HSV PCR and herpes culture are recommended for workup of active herpetic lesions, including genital ulcers. Although HSV PCR has a higher sensitivity, cultures are useful in distinguishing HSV-1 from HSV-2 infection.
- The CDC updated treatment guidelines for sexually transmitted infections in 2015 are noted in Table 3.
- Nucleic acid amplification tests (NAATs) are the most sensitive modality for detection of Chlamydia achomatis and are more sensitive than cultures for Neisseria gonorrhoeae. NAATs are most sensitive for the detection of T. vaginalis, detecting the infection three to five times more likely than wet-mount microscopy.
Unfortunately, adolescents are at increased risk for sexually transmitted infections secondary to high-risk sexual behavior, victims of commercial sexual exploitation, or sexual experimentation. The consequences can be devastating in the long term. Clinicians must maintain a high degree of suspicion and sensitivity (since most teenagers are reluctant to seek medical care and may not share all the information the clinician needs) to make this diagnosis, minimize complications, and optimize outcome for this vulnerable population.
— Ann M. Dietrich, MD, FAAP, FACEP
Sexually transmitted infections (STIs), known as venereal diseases, are bacterial, viral, or parasitic infections transmitted primarily through unprotected sexual contact with an infected person. The terms STI and STD (sexually transmitted disease) are interchangeable. STI has become increasingly favored among clinicians and public health officials to avoid the word “disease,” which suggests there would be the presence of signs or symptoms.1 Based on the Centers for Disease Control and Prevention’s (CDC) analyses, the most common STIs in the United States include chlamydia, gonorrhea, syphilis, human immunodeficiency virus (HIV), human papillomavirus (HPV), hepatitis B, herpes simplex virus (HSV), and trichomoniasis. Chancroid, lymphogranuloma venereum, Mycoplasma genitalium, and pubic lice are less common, but should be considered in a thorough STI evaluation.
STIs are transmitted through bodily fluids — blood, vaginal fluid, and semen — or by direct contact with open or infected skin lesions. Routes include oral, vaginal, or anal penetration and do not exclude sharing of sex toys, which also can be a vehicle for transmission contingent on the presence of fresh bodily fluid.1 Very rarely, transmission can occur through sharing damp towels or clothing.
The risk for STI transmission increases with age, community prevalence, and risky sexual behavior. As defined by the United States Preventive Services Task Force (USPSTF), high-risk sexual behavior involves having multiple current sexual partners, having a new partner, using condoms inconsistently, having sex while under the influence of alcohol or drugs, or having sex in exchange for money or drugs.2 Intravenous drug users and correctional facility inmates also are considered high-risk populations.
According to the CDC, there are about 20 million new cases of STIs in the United States each year, with about 50% of these cases affecting adolescents and young adults 15 to 24 years of age. Data suggest this group demographic most commonly is affected by chlamydia or gonorrhea.3 A 2005 Youth Risk Behavior Survey concluded that high school students commonly engaged in high-risk sexual behaviors. For example, 37% of students admitted to not using barrier contraception during sexual intercourse. More than half of these students never had been tested for HIV and, therefore, were unaware of their status.4 Adolescents now are identified as a new, at-risk cohort of patients. Not only do they engage in unprotected sexual activities more commonly, but teens also are found to have multiple sexual partners, are unlikely to speak openly about engaging in sexual intercourse, and have difficulty with resources such as transportation for doctors’ visits, which inevitably affects frequency of STI testing and treatment. Furthermore, their immune systems are not as mature as those of adults, and anatomically, the cervix of young, adolescent women contains more columnar epithelium, which also increases risk for infection.5
The USPSTF provides recommendations for STI testing with the expectation that patients would be screened routinely at well visits. However, it has been estimated that only 38% of adolescents receive preventive healthcare. Of those receiving preventive healthcare, only 40% spent time alone with their physician for counseling on topics such as sexuality, mental health, and substance use. Adolescents, who also are more likely to be uninsured than any other age group, commonly rely on the emergency department (ED) for primary care.6 Therefore, ED physicians have the potential to make a huge impact by following established testing guidelines for this age-specific population.
Epidemiology
It is important for healthcare providers to recognize the increased rate of sexually transmitted infections, particularly in this vulnerable patient population. In the United States, the average age of reported sexual debut, defined as vaginal sex, is 14.4 years.7 Approximately 7% of these young people report their first sexual encounter as before the age of 13 years. Previous studies have determined that the prevalence of sexually transmitted infections in sexually active females aged 14 to 19 years is one in four.8 The etiology of this increased rate is multifactorial. However, the rise in young men who have sex with men (YMSM) as well as at-risk youth who engage in exchange-sex (i.e., sex in exchange for money, drugs, or other needs) are significant contributing factors.
Chlamydia
Chlamydia is the most common sexually transmitted infection reported annually to the CDC. According to the 2015 CDC Sexually Transmitted Disease Surveillance study, despite the transient decrease in rates of chlamydia during 2011-2013, the rate of reported infections increased 5.9% during 2014-2015.9 Females ages 15 to 19 years are among the highest age-specific group of reported cases. In 2015, the incidence was four per 100,000 females, representing an increase of 1.5% from the previous year. This is particularly concerning because of increased risk of transmission of the bacteria Chlamydia trachomatis during adolescence due to cervical ectopy. Cervical ectopy is a physiologic process that occurs during puberty and involves the columnar cells. These cells typically are located within the cervical canal, but during puberty are located on the outer surface of the cervix and, therefore, are more susceptible to infection. There is an increased rate of the infection among males as well. In 2015, among males aged 15 to 19 years, the rate of reported cases was 767.6 cases per 100,000 males, representing an increase of 6.3% from the previous year.9
Gonorrhea
Gonorrhea, which is caused by Neisseria gonorrhoeae, is the second most commonly reported notifiable sexually transmitted disease in the United States.9 Along with C. trachomatis, infections from N. gonorrhoeae are the primary cause of pelvic inflammatory disease (PID) in the United States. Similar to chlamydia, in 2013, there was a transient decrease in the rate of gonorrhea, which has increased gradually among both males and females since. Unlike chlamydia, however, the rate of increase of gonorrhea in 2014-2015 was higher among males. In 2015, there was a total increase of reported gonorrhea cases of 12.8% from the previous year. This rate of reported cases was 123.9 per 100,000 population. Unfortunately, as the rate of cases of gonorrhea rises, so does its resistance to antimicrobials, leading to changes in CDC treatment guidelines, which will be discussed later in this article. In 2015, the second highest rate of gonorrheal cases was among young women aged 15 to 19 years. Among males of the same age, there was an increase in the rate of infections of 10.1% from the previous year.
Syphilis
Treponema pallidum is the bacterium that causes syphilis, a genital ulcerative disease. In 2000 and 2001, national rates of syphilis were at an all-time low of 2.1 cases per 100,000 population.9 Over the subsequent years, the gradual rise of primary and secondary syphilis was attributable to an increase in reported cases among men who have sex with men (MSM). However, in 2015, the reported cases of primary and secondary syphilis showed an increase of 18.1% in men and 27.3% in women from the previous year, which includes a rate increase of 10.2% in youth ages 15 to 19 years. Similar to chlamydia and gonorrhea, syphilis infections are associated with a high rate of HIV co-infection. Further, as the rates of primary and secondary syphilis rise in women, so do the rates of congenital syphilis.
Chancroid
Haemophilus ducreyi is the bacterium noted to cause chancroid, which is characterized by painful ulcers and inguinal lymphadenopathy called buboes. Rates of this disease have declined steadily, and only 11 cases were reported in 2015.9 However, it is important to note that this bacteria is difficult to culture; therefore, cases may go unreported because of underdiagnosis.
Human Papillomavirus
While HPV infection is not a reportable condition, HPV is the most common sexually transmitted infection in the United States.10 The prevalence of HPV types 6, 11, 16, and 18 has decreased in females aged 14 to 19 years since 2009, likely because of HPV vaccine benefits in this age group.
Herpes Simplex Virus
Similar to HPV, HSV infections are not nationally reportable. HSV type 1 (HSV-1) infections are generally orolabial, while HSV type 2 (HSV-2) infections are usually genital. HSV-1 infections usually occur during childhood; however, recent epidemiologic studies have reported an increased rate of these infections in teens and young adults. An increase in oral sexual behavior has been thought to be a contributory factor. Data obtained from the National Disease and Therapeutic Index reports a gradual increase in visits to physician offices for HSV genital infections.11
Human Immunodeficiency Virus
More than 1.2 million persons in the United States are infected with HIV, and while the number of new cases has trended downward, there is a rise in new HIV infection among certain patient populations, including YMSM, intravenous drug users, African Americans, and Hispanics/Latinos.12 Adolescents and young adults ages 13 to 24 years accounted for 26% of all new HIV infections; however, approximately 60% of HIV-positive adolescents are unaware of their status. In 2006, the CDC recommended routine HIV screening for all adolescents and adults (13 to 64 years) in high-prevalence areas, particularly those who are seeking treatment for tuberculosis or STIs, as early detection is found to be critical to decreasing transmission.5 (See Table 1.)
Table 1. Major Sexually Transmitted Infections |
|||
STI |
Clinical Presentation |
Diagnostic Testing |
Treatment |
|
Chlamydia |
Mucopurulent genital discharge, dysuria, genital burning and itching |
First-catch urine nucleic acid amplification test (NAAT) |
Azithromycin or doxycycline |
|
Gonorrhea |
Greenish-yellow genital discharge, dysuria, pelvic inflammatory disease |
First-catch urine NAAT |
Ceftriaxone + azithromycin |
|
Trichomonas |
Mucopurulent genital discharge, dysuria, genital burning and itching |
Nucleic acid amplification test from urine, vaginal, endocervical, or urethral specimens |
Metronidazole or tinidazole |
|
Human Papillomavirus |
Asymptomatic or genital warts |
During routine PAP smear |
Procedural treatment or topical imiquimod cream |
|
Herpes Simplex Virus |
Painful vesicles in genital-anal area; vesicles rupture into ulcers |
HSV PCR and herpes culture |
Acyclovir |
|
Syphilis |
Painless papule/ulcer in or around genitals |
Venereal Disease Research Laboratory or rapid plasma reagin tests |
Benzathine penicillin G |
|
Human Immunodeficiency Virus |
Asymptomatic or acute retroviral syndrome |
4th-generation ELISA test |
Truvada + raltegravir OR dolutegravir |
Clinical Presentation and Complications
A useful approach to evaluating STIs in adolescents is based on the pattern of symptom presentation. This generally can be divided into genital ulcer and discharge syndromes. Genital ulcer syndromes can be divided further into those that are painful, such as genital HSV and chancroid, and those that are painless, such as syphilis. Discharge syndromes include gonorrhea, nongonococcal urethritis, chlamydia, mucopurulent cervicitis, Trichomonas vaginalis, and urethritis.
Genital Ulcer Syndromes
Syphilis. Syphilis is divided into four stages — primary, secondary, latent, and tertiary. The predominant symptom of primary syphilis is a skin lesion that begins as a papule on or around the genitals, around the anus, in the rectum, or in or around the mouth. Infection is transmitted by direct contact with the syphilitic chancre. (See Figure 1.) This lesion gradually erodes into a painless, indurated ulcer with smooth firm borders. This highly infectious lesion heals by itself in three to six weeks; however, the bacteria continue to grow in the body if not treated. Symptoms of secondary syphilis usually appear two to eight weeks after the initial infection and represent hematogenous dissemination of spirochetes. Clinical manifestations during this stage include a generalized rash that involves the palms and soles.
Figure 1. Primary Syphilis Chancres |
|
|
|
|
|
SOURCE: Centers for Disease Control and Prevention. Sexually Transmitted Diseases (STDs). STD Clinical Slides. Available at: https://www.cdc.gov/std/training/clinicalslides/default.htm. Accessed May 30, 2017. |
|
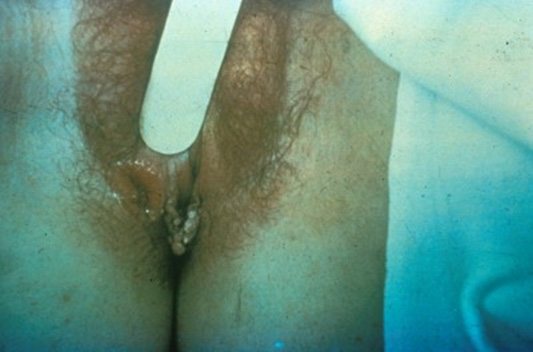
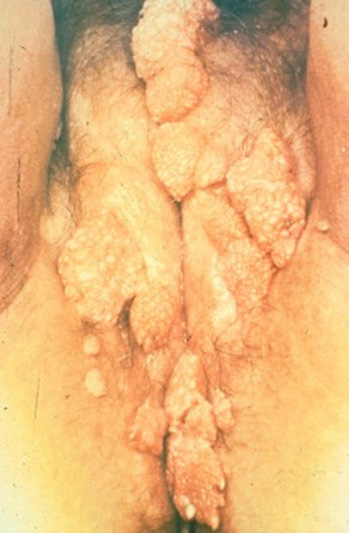
Other symptoms include lymphadenopathy, fever, myalgias, and joint pain. Sores, called mucous patches, can develop in or around the mouth, vagina, or penis. Genital warts, called condyloma acuminata, also may develop during this stage. (See Figure 2.) The symptoms of secondary syphilis usually resolve within two to 10 weeks, even if left untreated. Untreated syphilis proceeds to the latent phase, during which there are no visible signs or symptoms of syphilis. Tertiary syphilis is rare, even in individuals who have been untreated. It can occur anywhere from 10 to 30 years after the primary infection. The disease can cause multi-organ system damage to the central nervous system (neurosyphilis) and the cardiovascular system (causing aneurysms and valve disease).12
Figure 2. Condyloma Acuminata |
|
Condyloma acuminata, vulva |
Condyloma acuminata, meatal |
 |
 |
|
SOURCE: Centers for Disease Control and Prevention. Sexually Transmitted Diseases (STDs). STD Clinical Slides. Available at: https://www.cdc.gov/std/training/clinicalslides/default.htm. Accessed May 30, 2017. |
|
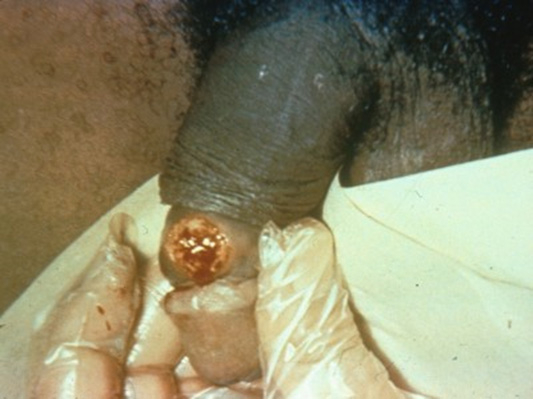
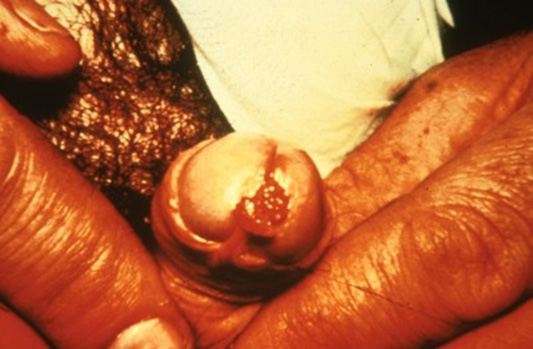
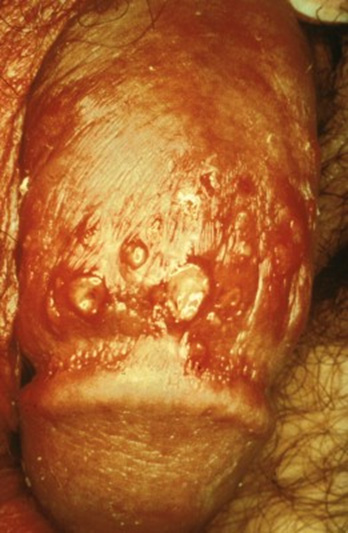
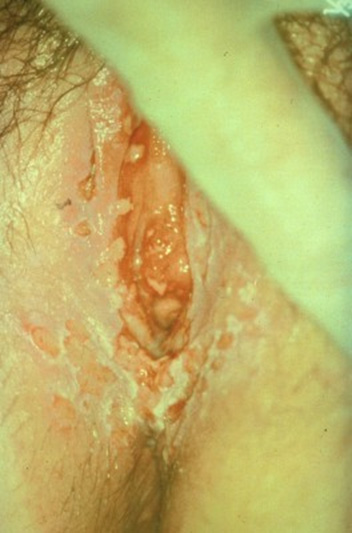
Genital Herpes Simplex. Genital herpes can be caused by HSV-1 and HSV-2 strains. The average incubation period for primary genital herpes infection is three to seven days. Systemic symptoms include fever, headache, malaise, and myalgias, as well as local lymphadenopathy. Painful herpetic vesicles develop in the genital-anal area and rupture into ulcerative lesions that can cause cervicitis, proctitis, dysuria, and urethritis. Crusting and reepithelialization occur within four to 15 days. (See Figure 3.) Genital herpes has a frequent reactivation rate, and recurrent infections usually are preceded by tenderness, pain, and burning at the site of eruption. Systemic symptoms are uncommon, and the genital lesions usually heal within seven to 10 days.13
Figure 3. Primary Herpes |
|
Primary herpes, male |
Primary herpes, female |
 |
 |
|
SOURCE: Centers for Disease Control and Prevention. Sexually Transmitted Diseases (STDs). STD Clinical Slides. Available at: https://www.cdc.gov/std/training/clinicalslides/default.htm. Accessed May 30, 2017. |
|
Haemophilus Ducreyi. As previously discussed, reported infections caused by H. ducreyi are becoming less common. Transmission of the bacteria is via skin-to-skin contact, and symptoms usually appear within four to 10 days of infection. Similar to genital herpes, this ulcerative lesion is very painful and can appear on the genitalia, cervix, and anus. Unlike the chancre in syphilis, this lesion is not indurated and often is referred to as “soft.”
Discharge Syndromes
Gonorrhea. Gonorrhea is transmitted through sexual contact with an infected person. Although the majority of infected women are asymptomatic, when present, symptoms will include greenish-yellow vaginal discharge, dysuria, and vulvitis. If untreated, PID can result. PID is a bacterial infection of the female reproductive organs that causes fever, abdominal pain, and cramping and dyspareunia. Diagnosis is based on clinical findings (discussed in screening techniques), and complications include infertility, ectopic pregnancy, and long-term pelvic pain. Hospitalization of females with PID should be considered in individuals who meet the following criteria: tubo-ovarian abscesses; pregnancy; severe illness, nausea, and vomiting or high fever; unable to follow or tolerate an oral outpatient regimen; and no clinical response to oral antimicrobial therapy.
Males with gonorrheal infections can present with a greenish-yellow discharge from the penis, or dysuria. Untreated infection increases their risk for development of epididymo-orchitis and infertility. Symptoms of rectal infections in both males and females include rectal discharge, anal itching, bleeding, and painful bowel movements.
Adolescents who have high-risk sexual behaviors are more likely to develop disseminated gonococcal infections (DGI). There are two presentation patterns that are common to patients with DGI. The first is referred to as the arthritis-dermatitis syndrome and involves tenosynovitis, dermatitis, and polyarthralgias without purulent arthritis. In a second pattern, patients may present with purulent arthritis without associated skin lesions. Other rare complications of DGI include endocarditis, meningitis, and osteomyelitis.13
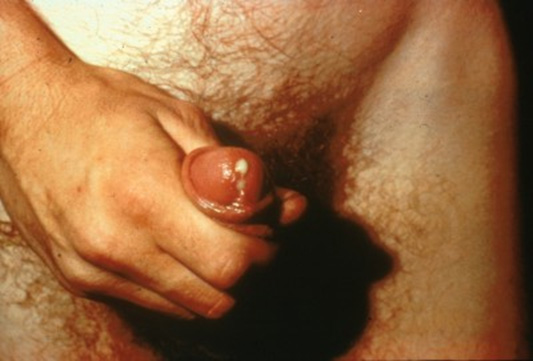
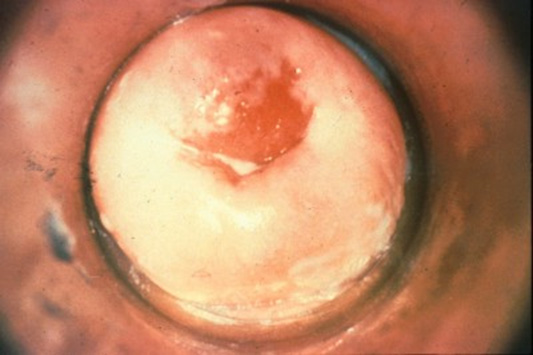
Nongonococcal Urethritis, Mucopurulent Cervicitis, and Vaginitis. Sexually transmitted nongonococcal urethritis (NGU) is caused most commonly by C. trachomatis; however, it also can be caused by T. vaginalis. It is transmitted via direct mucous membrane contact with an infected person. Symptoms include dysuria, discharge from the penis, as well as burning and itching of the genitals. In women, chlamydia is a common cause of mucopurulent cervicitis and vaginitis, resulting in vaginal discharge and dysuria. Chlamydia infections also can lead to PID, and co-infections with gonorrhea are common. (See Figure 4.)
Figure 4. Gonococcal Urethritis and Gonococcal Cervicitis |
|
Gonococcal urethritis |
Gonococcal cervicitis |
 |
 |
|
SOURCE: Centers for Disease Control and Prevention. Sexually Transmitted Diseases (STDs). STD Clinical Slides. Available at: https://www.cdc.gov/std/training/clinicalslides/default.htm. Accessed May 30, 2017. |
|
T. vaginalis is a parasite that can be transmitted via sexual contact. Infections most often are asymptomatic; however, when symptomatic, the infection causes similar symptoms of genital discharge, burning, itching, and dysuria.13
Human Papillomavirus. HPV is transmitted via direct contact with infected genital skin or mucosa. Condom use is only about 70% effective in preventing HPV transmission because there is still contact with genital skin.10 Individuals with a low viral load may be asymptomatic. High viral load infections of low-risk strains may result in genital warts, while those of high-risk strains may result in cervical cancer. Genital warts are highly infectious and once treated usually clear within six months. HPV types 16 and 18 cause 70% of cervical cancers and precancerous lesions. Vaccinations against these two types have been developed, and are offered to both male and female adolescents.
HIV. Adolescents who previously have had a sexually transmitted disease are at an increased risk for acquiring HIV. Newly diagnosed teens commonly present with candidal pneumonia, esophagitis or vaginitis, parotitis, varicella zoster, and herpes simplex recurrences. Between 30-70% of teens may present with acute retroviral syndrome. This syndrome usually presents two to six weeks after infection and is characterized by a mononucleosis-like syndrome with fever, sore throat, lymphadenopathy, malaise, anorexia, rash, myalgias, and fatigue. Because the differential diagnosis for these presenting symptoms is broad, clinicians must have a high index of suspicion and consider incorporating the HEADSS assessment while gathering the history. (See Table 2.) The clinical stages of HIV infection can be seen in Table 3.14
Table 2. HEADSS Psychosocial Risk Assessment |
HEADSS |
|
Home Education Activities Drug use and abuse Sexual behavior Suicidality and depression |
|
Adapted from: Cohen E, Mackenzie RG, Yates GL. HEADSS, a psychosocial risk assessment instrument: Implications for designing effective intervention programs for runaway youth. J Adolesc Health 1991;12:539-544. |
Table 3. WHO Clinical Staging of HIV Disease for Adults and Adolescents with Confirmed HIV |
|
|
Primary HIV infection |
|
|
Clinical Stage 1 |
|
|
Clinical Stage 2 |
|
|
Clinical Stage 3 |
|
|
Clinical Stage 4 |
|
|
SOURCE: U. S. Department of Health and Human Services . (2014, April). Guide for HIV/AIDS Clinical Care. AIDS National Education Training Centers National Coordinating Research Center. Available at: https://aidsetc.org/guide/hiv-classification-cdc-and-who-staging-systems. Accessed Feb. 23, 2017. |
|
Screening Recommendations
The USPSTF recommends targeting three populations for STI testing: 1) non-pregnant women; 2) pregnant women; and 3) men.2 Within each group, the risk status of current sexual practices and age should be considered. One also should take into account demographics. For example, many Southern states have higher rates of STIs, and some communities have higher prevalence of specific STIs compared to others.2 Therefore, it is critical for physicians to maintain awareness of STI prevalence in their specific location of practice.
Given that women are at higher risk for STI-related complications as discussed above, all sexually active women younger than 25 years of age should be tested annually for chlamydia, gonorrhea, and HIV, even if high behavioral risk factors are not present. Pregnant women should be screened for chlamydia, HIV, hepatitis B, and syphilis early in pregnancy, given risks posed to the unborn child.2 Pregnant women who engage in high-risk sexual practices also should be screened for gonorrhea. YMSM who identify as gay or bisexual should be screened at least annually for chlamydia, gonorrhea, HIV, and syphilis. YMSM are not considered high risk based on sexual preference alone, and just as with other populations, risky behaviors and demographics should play a role in the decision to screen more frequently, specifically increased frequency of HIV testing. A summary of screening recommendations as provided by the CDC can be found in Table 4.16
Table 4. CDC Screening Recommendations for Sexually Transmitted Infections |
|
STI |
Population |
|
Chlamydia |
Non-pregnant Women
Pregnant Women
Men
|
|
Gonorrhea |
Non-pregnant Women
Pregnant Women
Men
|
|
HIV |
Non-pregnant Women
Pregnant Women
Men
|
|
MSM: men who have sex with men; STI: sexually transmitted infections SOURCE: 2015 Sexually Transmitted Diseases Treatment Guidelines. (2017, January 25). Available at: https://www.cdc.gov/std/tg2015/default.htm. Accessed Feb. 19, 2017 . |
|
Table 4. CDC Screening Recommendations for Sexually Transmitted Infections (continued) |
|
STI |
Population |
|
Syphilis |
Non-pregnant Women
Pregnant Women
Men
|
|
HPV |
Non-pregnant and Pregnant Women
Men
|
|
HSV |
Non-pregnant Women
Pregnant Women
Men
|
|
Hepatitis B |
Non-pregnant Women
Pregnant Women
Men
|
|
Trichomonas |
Non-pregnant and Pregnant Women
Men
|
|
MSM: men who have sex with men; HPV: human papillomavirus; HSV: herpes simplex virus; SOURCE: 2015 Sexually Transmitted Diseases Treatment Guidelines. (2017, January 25). Available at: https://www.cdc.gov/std/tg2015/default.htm. Accessed Feb. 19, 2017. |
|
Testing Modalities
Chlamydia
Nucleic acid amplification tests (NAATs) are the most sensitive modality for detection of chlamydia trachomatis.16 First-catch urine specimens, the first part of the urine stream, can be collected easily from both men and women. Preferably, women should avoid cleaning the labial area prior to giving the sample.17 Self-collected or provider-collected swabbed specimens from the endocervix or vagina in women, or of the urethral meatus in men, also are acceptable. Oropharyngeal and rectal swabs can be sent on those specific anatomic sites of sexual contact.18
Gonorrhea
NAATs are more sensitive than cultures of N. gonorrhoeae, and often have a quicker turnaround time.17 Most commonly, NAATs are first-catch urine specimens; however, many labs also have the resources to run endocervical, vaginal, and urethral swabs. Cultures for detection include fluid samples from the oropharyngeal, endocervical, urethral, rectal, and ophthalmic sites. One benefit of culture is its ability to be sent for antibiotic sensitivities — this is of great importance given rapid resistance patterns of this specific bacteria.17
Pelvic Inflammatory Disease
The clinical diagnosis of PID has a high positive predictive value, which increases in patients with high-risk profiles.19 Women presenting with lower abdominal or pelvic pain and at least one of the following on pelvic examination should be treated presumptively for PID16:
- uterine tenderness, or
- cervical motion tenderness, or
- adnexal tenderness.
Hepatitis B
Serologic testing is necessary to diagnose hepatitis B. A combination of the patient’s hepatitis B surface antigen, surface antibody, and core antibody can lead to the confident diagnosis of acute, previous, or chronic infection, and can identify immunity.16
Human Papillomavirus
Routine HPV screening is not indicated in women younger than 25 years of age, nor in sexual partners of women infected with the virus.16 There are a variety of tests for HPV detection; however, the most common screening assessment involves cytological scraping during routine Papanicolaou smear. If positive, a confirmation test is required in the form of colposcopy, biopsy, or DNA technique.20
Human Immunodeficiency Virus
Screening for HIV infection through ELISA is the most appropriate initial test that can be performed. The combined antigen/antibody (fourth generation) test is preferred over the antibody tests alone, given that it can detect the virus as soon as three weeks after exposure. Second- or third-generation antibody-only tests may take up to 12 weeks for enough antibodies to be made and then detected. Although ELISA has a high sensitivity, particularly fourth-generation testing, it can yield false-positive results.21 Rapid immunoassays screen for antibodies from finger pricks or oral swabs and provide results within 20 minutes, but are slower to detect infection and, therefore, can yield false-negative results. All positive screening results should be followed up with an HIV-1/HIV-2 antibody differentiation assay, Western blot, or indirect immunofluorescence assay. Western blot is used most commonly.
Herpes Simplex Virus
HSV PCR and herpes culture are recommended for workup of active herpetic lesions, including genital ulcers. HSV PCR has a higher sensitivity; however, cultures are useful in distinguishing HSV-1 from HSV-2 infection. Cytologic assessments, such as Tzanck smear, are insensitive.16
Syphilis
Treponema pallidum is best identified by visualization on dark field microscopy by a well-trained, experienced microscopist. Given that multiple factors depend on the success of this test, including volume and thickness of the specimen used, the diagnoses of syphilis can be made using both a non-treponemal test and treponemal test.16 CDC-approved non-treponemal tests include Venereal Disease Research Laboratory test or rapid plasma reagin test. These are best used for screening purposes and, if reactive, a treponemal test should follow. Fluorescent treponemal antibody absorbed (FTA-ABS) tests, the T. pallidum passive particle agglutination (TP-PA) assay, various enzyme immunoassays (EIAs), chemiluminescence immunoassays, immunoblots, and rapid treponemal assays are options, and can detect presence of antibodies sooner than non-treponemal tests.22
Trichomonas
NAATs are most sensitive for the detection of T. vaginalis, detecting the infection three to five times more likely than wet-mount microscopy. The NAAT, APTIMA has a sensitivity of 95.3-100% and specificity of 95.2-100%. Specimens can be sent from urine, vagina, endocervix, or urethra. Cultures and wet preparations are decreasing in popularity because of lower sensitivities.16
Treatment Recommendations
Treatment of STIs is not only important to decrease evolution of the infection into a sexually transmitted disease process, but also to decrease transmission among partners. The CDC established treatment guidelines that were updated in 2015 to incorporate new guidelines addressing gonococcal resistance. Providers should bear the responsibility of arranging treatment for their patients’ sexual partners through their state’s health department.
Treatments for common STIs have been adapted from the CDC and are reflected in Table 5.16
Table 5. Treatment Guidelines for Common STIs |
||
Infection |
Treatment |
Dose/Route |
|
Trichomonas |
|
|
|
Chlamydia |
Urogenital or rectal
|
|
|
Gonorrhea |
|
|
|
Syphilis |
|
|
|
Human Immuno-deficiency Virus23 |
Post-exposure prophylaxis: Give within 72 hours of exposure; patients ≥ 13 years. Refer to package insert for age-/weight-based dosing in pediatrics
|
|
|
Human Papillomavirus |
Patient administered:
Physician administered:
|
|
|
Herpes Simplex Virus |
|
|
|
Pelvic Inflammatory Disease |
|
|
|
*Preferred ‡For cefotetan/doxycycline and cefoxitin/doxycycline regimen, may transition to PO doxycycline 24-48 hours after clinical improvement to complete the 14 day course. Source: 2015 Sexually Transmitted Diseases Treatment Guidelines. (2017, January 25). Available at: https://www.cdc.gov/std/tg2015/default.htm. Accessed Feb. 19, 2017. |
||
Summary
The rate of STIs in the United States continues to rise gradually. Adolescents often engage in high-risk sexual behavior, are reluctant to seek medical care, and have limited resources, which makes them an extremely vulnerable cohort of the population. It is important to recognize the pattern of symptom presentation — generally either genital ulcer or discharge syndromes. Accurate diagnosis may require NAATs, ELISA, and serologic testing. Treatment of the patients and their partners, along with education of safe sex practices, is imperative.
REFERENCES
- American Sexual Health Association. STDs/STIs. Available at: http://www.ashasexualhealth.org/stdsstis/. Accessed Feb. 27, 2017.
- Meyers D, Wolff T, Gregory K, et al. USPSTF Recommendations for STI Screening. Available at: https://search.uspreventiveservicestaskforce.org/search?q=STI+screening&entqr=0&output=xml_no_dtd&proxystylesheet=USPSTF_frontend&client=USPSTF_frontend&site=USPSTF_Collection&x=0&y=0. Accessed Feb. 21, 2017.
- Centers for Disease Control and Prevention. 2015 Sexually Transmitted Disease Surveillance: STIs in Young Adolescents and Adults. (2016, October 18). Available at: https://www.cdc.gov/std/stats15/adolescents.htm. Accessed Feb. 27, 2017.
- Branson BM, Handsfield HH, Lampe MA, et al. Revised Recommendations for HIV Testing of Adults, Adolescents, and Pregnant Women in Health-Care Settings. Available at: http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5514a1.htm. Accessed Feb. 23, 2017.
- Centers for Disease Control and Prevention. Sexually Transmitted Diseases. CDC Fact Sheet: Information for Teens and Young Adults: Staying Healthy and Preventing STDs. Available at: https://www.cdc.gov/std/life-stages-populations/stdfact-teens.htm. Accessed Feb. 23, 2017.
- Minniear TM, Gilmore B, Arnold SR, et al. Implementation of and barriers to routine HIV screening for adolescents. Pediatrics 2009;124:1076-1084.
- Outlaw AY, Phillips G 2nd, Hightow-Weidman LB, et al. Age of MSM sexual debut and risk factors: Results from a multisite study of racial/ethnic minority YMSM living with HIV. AIDS Patient Care STDS 2011;25(Suppl 1):S23-S29.
- Forhan SE, Gottlieb SL, Sternberg MR, et al. Prevalence of sexually transmitted infections among female adolescents aged 14 to 19 in the United States. Pediatrics 2009;124:1505-1512.
- Centers for Disease Control and Prevention. Sexually Transmitted Disease Surveillance: STDs 2015. Available at: https://www.cdc.gov/std/stats15/std-surveillance-2015-print.pdf. Accessed Feb. 23, 2017.
- Juckett G, Hartman-Adams H. Human papillomavirus: Clinical manifestations and prevention. Am Fam Physician 2010;82:1209-1214.
- National Disease and Therapeutic Index. IMS Health, Integrated Promotional Services™. IMS Health Report 1966–2014.
- Lukehart S. A Journey through Syphilis: How does Treponema pallidum cause such a complex disease? – CDC STD Prevention Science Series Webinar. June 2, 2016.
- Toney J, Bachmann L. Common Sexually Transmitted Diseases: STD 101 for Clinicians. (2012) Available at: https://www.cdc.gov/std/training/std101/presentations-2012/std-common-clinicians.pdf. Accessed Feb. 5, 2017.
- World Health Organization. WHO Case Definitions of HIV for Surveillance and Revised Clinical Staging and Immunologic Classification of HIV-Related Disease in Adults and Children. Available at: http://www.who.int/hiv/pub/guidelines/HIVstaging150307.pdf?ua=1. Accessed Feb. 9, 2017.
- Centers for Disease Control and Prevention. HIV in the United States: At a Glance. Dec. 2, 2016. Available at: https://www.cdc.gov/hiv/statistics/overview/ataglance.html. Accessed Feb. 2, 2017.
- Centers for Disease Control and Prevention. 2015 Sexually Transmitted Diseases Treatment Guidelines. Available at: https://www.cdc.gov/std/tg2015/default.htm. Accessed Feb. 19, 2017.
- Brocail M. Gonorrhea: Definition, Symptoms and Testing Information. Available at: https://www.stdcheck.com/blog/everything-about-gonorrhea-and-gonorrhea-testing/. Accessed Feb. 18, 2017.
- American Association for Clinical Chemistry. Lab Tests Online. Chlamydia and Gonorrhea NAAT Screening Method Endorsed by CDC. Available at: https://labtestsonline.org/news/140521naat/. Accessed Feb. 20, 2017.
- Centers for Disease Control and Prevention. 2010 STD Treatment Guidelines. Pelvic Inflammatory Disease. Available at: https://www.cdc.gov/std/treatment/2010/pid.htm. Accessed Feb. 18, 2017.
- Dixit R, Bhavsar C, Marfatia YS. Laboratory diagnosis of human papillomavirus virus infection in female genital tract. Indian J Sex Transm Dis 2011;32:50-52.
- American Sexual Health Association. STDs/STIs. Available at: http://www.ashasexualhealth.org/stdsstis/. Accessed Feb. 21, 2017.
- Centers for Disease Control and Prevention. Syphilis - CDC Fact Sheet (Detailed). Feb. 13, 2017. Available at: https://www.cdc.gov/std/syphilis/stdfact-syphilis-detailed.htm. Accessed Feb. 23, 2017.
- Centers for Disease Control and Prevention. Updated guidelines for antiretroviral post exposure prophylaxis after sexual, injection drug use, or other nonoccupational exposure to HIV—United States, 2016. Available at: https://stacks.cdc.gov/view/cdc/38856. Accessed Feb. 24, 2017.
Unfortunately, adolescents are at increased risk for sexually transmitted infections secondary to high-risk sexual behavior, victims of commercial sexual exploitation, or sexual experimentation. The consequences can be devastating in the long term. Clinicians must maintain a high degree of suspicion and sensitivity (since most teenagers are reluctant to seek medical care and may not share all the information the clinician needs) to make this diagnosis, minimize complications, and optimize outcome for this vulnerable population.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.