Penetrating Chest Injury
September 1, 2017
Reprints
AUTHORS
Ademola Adewale, MD, FAAEM, Director of Research and Simulation, Assistant Program Director, Florida Hospital Emergency Medicine Residency Program, Orlando.
Kevin Goldman, MD, PGY-3, Emergency Medicine Chief Resident, Florida Hospital, Orlando.
PEER REVIEWER
Jay Menaker, MD, Associate Professor of Surgery, University of Maryland, Baltimore.
Financial Disclosure
Dr. Dietrich (editor in chief), Dr. Adewale (author), Dr. Goldman (author), Dr. Menaker (peer reviewer), Ms. Behrens (nurse planner), Ms. Mark (executive editor), Ms. Coplin (executive editor), and Ms. Hatcher (AHC Media editorial group manager) report no financial relationships with companies related to this field of study.
EXECUTIVE SUMMARY
- The shock index and MGAP (Mechanism, Glasgow coma scale, Age, and Arterial Pressure) score are tools to risk stratify trauma patients.
- A meta-analysis that reviewed 25 years of published data regarding the survival of emergency department (ED) thoracotomies found an overall survival rate of 7.4%.
- The Eastern Association for the Surgery of Trauma has guidelines specifying when ED thoracotomy is appropriate. The guidelines concluded that patients who present pulseless but with signs of life after penetrating thoracic injury should undergo an ED thoracotomy.
- Portable chest X-ray and thoracic ultrasonography (focused assessment with sonography in trauma [FAST] exam) are the modalities of choice in patients not stable enough to leave the ED.
- Stable patients with trans-mediastinal injuries should receive a cardiac FAST and CT angiogram to exclude life-threatening injuries (combined negative predictive value of 100%).
- The treatment of rib fractures is mostly supportive. Ensuring proper ventilation, via pain control, and/or noninvasive or invasive measures, is the highest priority, especially in the elderly population.
Penetrating trauma of the chest can have severe and devastating consequences. Advances in ultrasound and treatment therapies have improved survival. A high degree of suspicion is indicated to identify the more subtle injuries associated with penetrating trauma to the chest.
— Ann M. Dietrich, MD, Editor
Introduction
Across the United States, injuries due to trauma account for 41 million emergency department (ED) visits annually. Of these, 3.3 million require hospital admission and 192,000 patients succumb to their injuries.1 In the United States, trauma is the leading cause of death for those 1-46 years of age and the third leading cause of mortality across all age groups.2 Penetrating thoracic trauma, although less common than blunt trauma, portends a higher mortality. Nine percent of all trauma-related deaths are from thoracic injures, 33% of which are due to penetrating trauma.3 Although there is geographic variation, in the United States, firearms and stabbings account for most injures that involve the thoracic wall. Other less common mechanisms of penetrating thoracic trauma are impalement during industrial accidents, falls, collisions, and blast injuries. The prevalence of firearm and knife-related injuries is a burden to our communities, both fundamentally and economically. In 2014, initial hospitalizations for firearm-related injuries in the United States cost an average of $735 million per year and resulted in more than 33,700 deaths.4
To best understand the evaluation of penetrating trauma victims, it is important to have a basic knowledge of ballistics. The damage inflicted on a patient is proportional to the characteristics of the weapon, the energy of the object, and the tissue being penetrated. More specifically, the size of the penetrating object and the deformability and density of the tissue being penetrated all correlate with the extent of damage inflicted. For example, dense tissues sustain greater damage than less dense tissues do.5 Penetrating chest trauma can be broken down into two main categories based on the speed of the penetrating missile. There are low-velocity and high-velocity missiles. The most common low-velocity injury occurs when a patient sustains a stab wound. Low-velocity missiles refer to projectiles traveling at less than 350 m/s. The most common high-velocity injuries include bullets dispatched from firearms. (See Figure 1.) Firearms generally release bullets at speeds of 600-700 m/s. This is the speed at which explosive effects commonly are seen.6 Distinguishing between the two types is relevant in the evaluation of the trauma patient because high-velocity missiles cause injury to the structures adjacent to their path. In addition, the path of high-velocity missiles is not always straight. In penetrating chest trauma, specifically, the trajectory of the missile may be altered by structures within the thoracic cavity.
Figure 1. Penetrating Chest Trauma
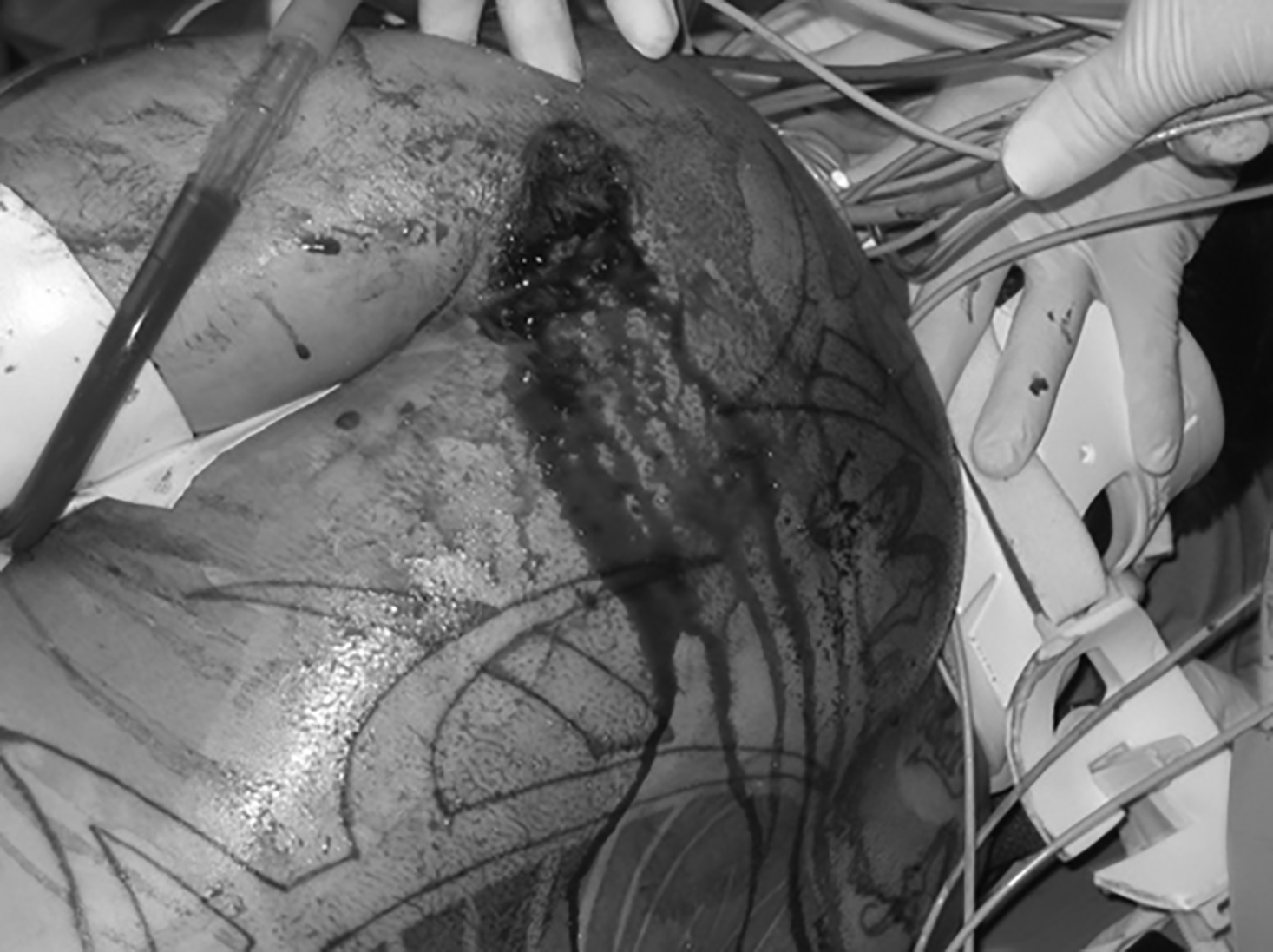
The above patient sustained a shotgun injury to the chest.
Image courtesy of A. Adewale, MD.
General Emergency Department Approach
By definition, penetrating chest trauma requires a violation of the chest wall. The chest wall is made of soft tissue and bone. Skin, fasciae, and muscle overlay the rib cage and sternum. The major organs within the thorax are prone to injuries when the chest wall has been violated. The lungs, heart, great vessels, tracheobronchial tree, esophagus, and diaphragm can be injured individually or simultaneously during trauma. Each will be discussed in greater detail in the sections that follow.
The most common mechanisms by which a patient succumbs to early death include airway obstruction, loss of oxygenation or ventilation, exsanguination, cardiac failure, cardiac tamponade, and air embolism.7 In chest trauma, initial vital signs can be falsely reassuring. Scoring systems have been created to identify those trauma patients with compensated shock who may decompensate quickly. The shock index (heart rate/systolic blood pressure) is one example. Retrospective studies evaluating the ability of an abnormal shock index (> 0.9) to identify those potentially sick patients have shown this to be a useful tool in predicting mortality.9,10 As a prehospital triage tool, the shock index has led to earlier activation of trauma resources and, in turn, better outcomes for patients.
The MGAP score is a newer scoring system that seeks to improve the ability to risk stratify those patients who are likely to have worse outcomes. MGAP is an acronym for Mechanism, Glasgow coma scale, Age, and Arterial Pressure. Sartorius et al defined three groups of patients whose MGAP scores predict morbidity and mortality: The risk of death is low in patients with MGAP scores of 23-29, intermediate in patients with MGAP scores of 18-22, and high in patients with MGAP scores of 3-17.11 Although used less frequently than the shock index, a recent cross-sectional descriptive study showed this to be an effective prehospital and hospital scoring system for risk stratifying the potentially sick, multiple trauma patient.12
The Arresting Patient
Traumatic cardiac arrest is associated with very high mortality rates. Although statistics vary, overall survival seems to be between 0-17%.13 The physician in the trauma bay must predict which patients have the best chance of survival, and what procedures should and should not be performed during a trauma code. However, these questions do not have simple answers. Many would argue that in certain circumstances, resuscitation should not be initiated at all because of the very poor prognosis of patients in traumatic cardiac arrest. In 2013 Leis et al published a study that found a 6.6% survival rate in trauma patients who received advanced life support. They concluded, therefore, that advanced life support should be initiated at least in all traumatic cardiac arrest patients regardless of initial rhythm.14 However, the authors did not mention the role of closed chest compressions in their description of the resuscitation. Many have argued that closed chest cardiopulmonary resuscitation (CPR) in traumatic arrest patients not only is ineffective, but also takes away the physician’s ability to perform other potentially lifesaving procedures.15 The rationale is that in traumatic cardiac arrest, the patient most likely has arrested as a result of hemorrhagic shock (exsanguination) or obstructive shock (tension pneumothorax, pericardial tamponade), and closed chest CPR does not fix either problem. However, the data on this are scarce, and further research is required to guide management.
In patients with penetrating chest trauma with either witnessed cardiac arrest or unresponsive hypotension despite vigorous resuscitation, an ED thoracotomy often is indicated. Although it is a high-risk procedure in the resuscitation bay, and one that does not yield very high survival rates, it can be a lifesaving measure. A meta-analysis that reviewed 25 years of published data regarding the survival of ED thoracotomies found an overall survival rate of 7.4%. The outcome depends in large part on the mechanism and location of injury. Penetrating chest injuries had a better outcome than did blunt chest injuries, and stab wound victims had a better prognosis than did gunshot wound victims.16 Therefore, this procedure should be considered early in the arresting patient after a penetrating chest injury in a hospital with sufficient surgical backup.
Opening the chest in the ED, via an ED thoracotomy, allows the physician to perform several lifesaving procedures. The physician can release a pericardial tamponade, repair a cardiac injury, control hilar bleeding, cross clamp the aorta, or restart the heart. Since it was first described in 1950, the specific circumstances for which an ED thoracotomy is appropriate have been debated.17 The Eastern Association for the Surgery of Trauma (EAST) has guidelines specifying when this procedure is appropriate. The guidelines concluded that patients who present pulseless but with signs of life after penetrating thoracic injury should undergo an ED thoracotomy. The guidelines could only conditionally recommend resuscitative ED thoracotomy in patients who present pulseless without signs of life, due to more limited data.18
Although the procedure itself has not changed drastically over the years, most ED physicians do not perform it routinely. Before a resuscitative thoracotomy is performed, the patient should be intubated. Selectively intubating the right lung by advancing the endotracheal (ET) tube to a depth of 30 cm causes a collapse of the left lung, allowing for better visualization once the left chest is open. If the decision is made to perform CPR, do not halt compressions until just prior to making the initial incision. The physician should be clothed with sterile gloves, a gown, and mask. The left chest should be prepped antiseptically, and the patient’s left arm should be raised above the head to identify the landmarks better and to create a wider space between the ribs. An anterolateral incision at the fourth to fifth intercostal space with a no. 20 blade should be made. The incision should be extended past the posterior axillary line. Scissors are used to cut the intercostal muscles and expose the thoracic cavity. A rib spreader is placed between the ribs with the handle directed downward.19 Once the chest is opened, rapidly finding and controlling the site of injury is essential to the patient’s survival. The evaluation and management of each individual penetrating intrathoracic injury are discussed in more detail in the sections that follow.
The Unstable Patient
As in all critically ill patients, an algorithmic approach to the unstable trauma patient is essential for effective management. As highlighted in the Advanced Trauma Life Support (ATLS) guidelines set forth by the American College of Surgeons, starting with the ABCs (airway, breathing, and circulation) ensures that essential actions are not missed.20 The guidelines emphasize the dogma that the physician must not move to the next step until the prior one has been addressed. The diagnostic approach to the unstable trauma patient has changed as ultrasound equipment has become more available, portable, and higher in resolution. In the unstable patient who has sustained penetrating chest trauma, a CT scan may not be an option because of the risk of the patient decompensating. Portable chest X-ray and thoracic ultrasonography (focused assessment with sonography in trauma [FAST] exam) are the modalities of choice in patients not stable enough to leave the ED. In fact, studies have shown thoracic ultrasonography, in the hands of an experienced physician, to be far more sensitive than chest X-rays in diagnosing both pleural effusions and pneumothoraces.21
With regard to the unstable patient with suspected cardiac injury, transthoracic ultrasound has proven to be the diagnostic modality of choice as well. It is both sensitive and specific for identifying pericardial effusion and tamponade.22
In the unstable, bleeding patient, autotransfusion has become a topic of interest. Autotransfusion, also known as cell salvage, is the collection of blood from a bleeding site and the reinfusion of that blood into the same patient. Autotransfusion decreases the need for allogenic blood transfusions. This proves beneficial in patients with rare blood types, those at risk of infectious disease transmission, and those presenting at facilities with restricted homologous blood supply. In the penetrating chest trauma patient, the blood used for autologous transfusions is collected directly from the chest tube. Many chest tube collection systems have a port for an autotransfusion canister. Although intraoperative autotransfuser devices contain a filter and centrifuge, in the deteriorating patient, autologous blood can be reinfused into the patient up to six hours after collection without heparin.23 However, studies have shown that the hemoglobin concentration from the chest tube is, on average, 2 grams less than venous blood and that coagulation factors were significantly lower than in whole blood.23 Therefore, hesitation comes from the fear that autologous blood can lead to worsening coagulopathy via hemodilution and inflammation. However, in a study from 2015, Rhee et al showed autologous transfusions to be safe and cost effective.24
Fluid resuscitation in the trauma patient has been another topic of debate. Current literature has shown that large volume crystalloid or red blood cell-only fluid resuscitation leads to worsening outcomes by means of dilutional coagulopathy and the dislodgment of clots.25 In patients who are expected to require more than 10 units of red blood cells in 24 hours, the administration of blood products (red blood cells, platelets, and fresh frozen plasma) in combination rather than in isolation, termed massive transfusion protocol, has been shown to decrease mortality through improvement of coagulation parameters.26 The exact ratio at which these products should be administered, however, remains a subject of debate.
The Stable Patient
In the stable trauma patient, an algorithmic approach prevents missing devastating injuries. In the penetrating chest trauma patient, special attention should be given to identifying all penetrating wounds and evidence of retained fragments of the penetrating missile, including rolling the patient. In gunshot victims, an even number of wounds often suggests the missile entered and exited the patient. The diagnostic studies used in a stable patient, unlike in the unstable patient, involve additional modalities. CT scan has become the gold standard for evaluating stable penetrating trauma patients. Ultrasound is a valuable modality that can identify and assist with triage and definitive diagnostic testing.
Disposition of the Stable Penetrating Trauma Patient
A key point is the issue of disposition. Deciding whether a penetrating thoracic trauma patient can be discharged home safely is important. In an era when hospital resource utilization is monitored closely, discharging low-risk patients is advantageous for both the patient and the hospital.
In a prospective study, Seamon et al sought to answer this question. They categorized low-risk patients as those who did not have an initial pneumothorax on CT or any indication for going to the operating room. They found that a three-hour repeat chest X-ray was sufficient for ruling out serious thoracic injuries.27 The authors noted that some of these initially low-risk patients developed delayed pneumothoraces within the first three hours of injury, but none developed a pneumothorax after that time period. Therefore, the authors concluded that low-risk patients with a negative three-hour chest X-ray are safe to discharge home.
Rib Fractures and Flail Chest
The ribs are one of the most commonly injured structures in the thorax. Although rib fractures initially may appear more benign than other types of penetrating chest trauma injuries, patients with multiple rib fractures have poor overall outcomes. In one study, 34% of patients with multiple rib fractures were discharged to a long-term care facility and 12% of those died of complications.28 The National Trauma Data Bank notes a 10% mortality rate and a 13% complication rate with rib fractures.29 The hospital course of these patients often is complicated by injuries from the initial assault and/or the sequelae of poor inspiratory effort. Pneumonia, pulmonary effusion, aspiration, acute respiratory distress syndrome (ARDS), pulmonary embolism, and atelectasis all are seen in hospitalized patients who have sustained rib fractures.30
A close evaluation of the location and number of ribs fractured can give insight into the possibilities of associated injuries. In patients with fractures of the upper ribs (1-2), the great vessels are prone to injury secondary to their anatomic location. Because of the protection provided by the bony and muscular framework of the upper limb, injuries to the first two ribs generally require great force. Mortality rates in blunt and penetrating traumatic upper rib fractures have been noted as high as 30%.28 Injuries to ribs 4-9 occur commonly in blunt trauma and in penetrating trauma. Penetrating injuries in this part of the chest wall often are associated with pneumothoraces, hemothoraces, and lung contusions.20 These injuries occur via two possible mechanisms. Either the penetrating missile itself or the subsequently broken ribs puncture the lung parenchyma. Fractures of the lower ribs (9-12) can be accompanied by injuries to the intra-abdominal organs. The spleen, liver, and kidneys are vulnerable to penetrating trauma because of their anatomic location.31
Flail chest occurs when a segment of the rib cage becomes detached from the chest wall. Two or more adjacent ribs break in two or more places, leaving a segment that paradoxically moves with inspiration and expiration. The morbidity from flail chest is not from the paradoxical chest wall movement, but occurs, instead, from the associated injury to the lung parenchyma and the splinting that results in poor inspiratory effort.32
The initial evaluation of a penetrating chest trauma victim in whom a rib fracture is suspected should aim specifically at locating the fracture and evaluating for associated injuries. Crepitus, subcutaneous emphysema, pulsatile bleeding, or any obvious deformities can be indications of additional intrathoracic trauma. Patients who are hypoxic, who show signs of shock, or who have multiple injuries require immediate intubation. Bedside ultrasound and portable chest X-ray can be used initially to evaluate for rib fractures and associated intrathoracic organ injury but should not delay definitive management. However, CT scan remains the gold standard for evaluation of most intrathoracic injuries.33
The treatment of rib fractures is mostly supportive. Ensuring proper ventilation, via pain control, and/or noninvasive or invasive measures, is the highest priority, especially in the elderly population. Poor inspiratory effort leads to the sequelae of in-hospital complications. A shift in the therapeutic regimens for pain control has taken place, and now often involves a multimodal approach. Multimodal pain therapy combines opioid analgesics with non-opioid medications. Studies have proven scheduled intravenous nonsteroidal anti-inflammatory drugs (NSAIDs) (i.e., ketorolac) lead to lower opioid requirements and improved pain scores.34 Catheter-based analgesia, however, has shown mixed benefits. In a meta-analysis published by EAST, epidural catheter-based pain management showed lower pain scores at 24 and 48 hours, but not at 72 hours after intervention.35 Therefore, the EAST guidelines only conditionally recommend epidural anesthesia because of limited evidence of its effectiveness. On the other hand, other catheter-based interventions (paravertebral nerve blocks, continuous intrapleural infusions, and continuous intercostal infusions) did not show significant differences in pain scores over other modalities.35 Operative stabilization in patients with flail chest, the most invasive intervention suggested, has been shown to be associated with shorter ventilator duration, shorter ICU stay, and decreased risk of developing pneumonia.36
The disposition for patients with rib fractures depends on the extent of the injuries and other organs involved. Patients with isolated rib fractures can be discharged home safely with analgesia and an incentive spirometer. However, the morbidity and mortality associated with rib fractures in the pediatric and geriatric populations is exponentially higher than in the adult population. In fact, studies have shown that for each additional rib fracture in a geriatric trauma patient, mortality increases by 19%.37 The pediatric skeleton is more pliable and takes greater force to fracture. Therefore, the presence of rib fractures should alert the practitioner to more severe injuries. (See Figure 2.) Therefore, geriatric and pediatric patients with multiple rib fractures often require admission to the ICU for close monitoring. Additionally, a lack of rib fractures cannot predict the absence of intrathoracic injury.
Figure 2. Pediatric Ribs and Clavicle Fracture
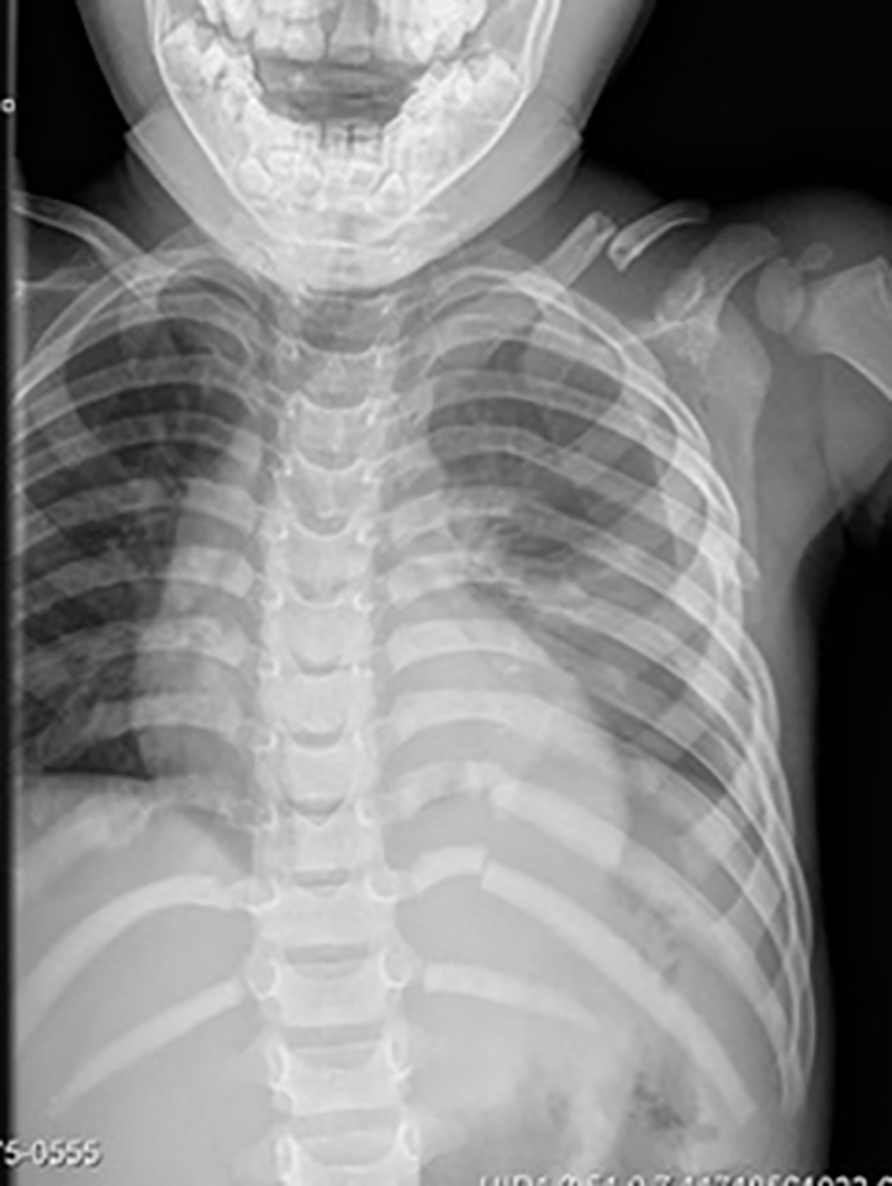
The above chest radiograph shows multiple left-sided rib fractures along with a left clavicle fracture.
Image courtesy of A. Adewale, MD.
Pneumothorax
A traumatic pneumothorax is one of the most common injuries sustained following penetrating thoracic trauma. A pneumothorax is the presence of air between the parietal and visceral pleura. It occurs from injuries sustained either to the lung parenchyma or the tracheobronchial tree. Pneumothoraces result in ventilation-perfusion mismatches via shunting; blood continues to perfuse areas of the lung that are poorly oxygenated. Air within the enclosed intrathoracic space, analogous to blood within the skull in traumatic intracranial hemorrhages, applies pressure to the lung, which ultimately can lead to its collapse. Pneumothoraces can be divided into several categories: simple pneumothorax, open pneumothorax, and tension pneumothorax. A simple pneumothorax is defined as one that is non-expanding. An open pneumothorax, often colloquially called a sucking chest wound, is seen commonly in penetrating traumas and is an unsealed opening in the chest wall. (See Figure 3.) This creates complications through its alteration of the vacuum normally present within the pleural cavity, which prevents the lungs from fully expanding.
Figure 3. Open Pneumothorax
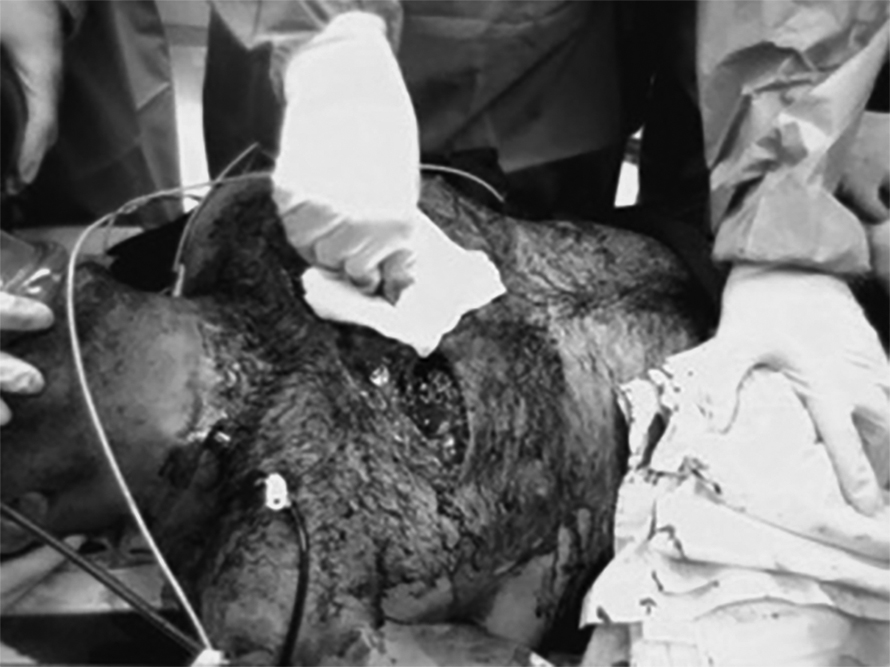
This image shows an open chest and sucking open pneumothorax after impalement.
Image courtesy of A. Adewale, MD.
A tension pneumothorax, the most life-threatening of the three, presents a true emergency. When the pressure in the thoracic cavity becomes high enough to shift the mediastinal contents and cause insufficient blood return to the heart, the patient is at high risk of rapid decompensation.
Diagnosing a pneumothorax often can be accomplished by physical exam alone. In an unstable patient with unilateral absent breath sounds or a sucking chest wound, the physician should not wait for imaging before intervening. However, in unstable patients in whom the diagnosis is less clear, ultrasound has become the modality of choice. Although in the past a chest X-ray was considered the best tool for diagnosing pneumothorax in the trauma bay, a paradigm shift has taken place. In an evidence-based review, Wilkerson et al found thoracic ultrasound to be superior to chest X-ray for detecting pneumothorax. They found an 86-98% sensitivity and 97-100% specificity as compared to chest X-ray, which had a much lower sensitivity of 28-75%.38
The bedside lung ultrasound in emergency (BLUE) protocol for assessing the patient in acute respiratory failure highlights the techniques for diagnosing a pneumothorax on ultrasound.39 Using a high-frequency probe, the practitioner looks through the ribs for the presence or absence of lung sliding. In a normal patient, lung sliding signifies the parietal and visceral pleura sliding past each other. On the other hand, the absence of lung sliding represents a pneumothorax. A very specific finding, one named the lung point, represents the point at which the inflated lung meets the pneumothorax. The ultrasound’s M mode can be a useful tool as well in looking for motion at one point. In this mode, the “bar code” sign represents the lack of normal lung sliding.40 Despite convincing data, if the patient is stable enough, CT scan still is considered the gold standard for diagnosing a pneumothorax.
The definitive management for pneumothorax is a tube thoracostomy. The urgency with which it should be placed, and whether the pneumothorax will resorb without one, depends on the percent volume involved. In patients with less than a 20% pneumothorax, treatment with 100% oxygen and close monitoring often leads to resolution.20 On the other hand, a tension pneumothorax requires emergent intervention. In the prehospital setting, the management for a tension pneumothorax is still needle decompression. However, multiple studies have highlighted the pitfalls of this procedure. For example, in the obese population, a conventional catheter often does not reach the thoracic cavity.41 Inaba et al evaluated the optimal positioning for emergent needle thoracostomy. Contrary to common practice, they found that the success rate was highest at the fifth intercostal space, not the second, with an equally low complication rate (cardiac, lung, aorta, liver injury).42 For simple pneumothoraces, Kulvatunyou et al showed that a 14F pigtail catheter was sufficient. They found smaller catheters to have the same efficacy with reduced pain.43 Lastly, for open pneumothoraces, the prehospital treatment is a sterile occlusive dressing taped on three sides. A completely occlusive dressing risks an open pneumothorax becoming a tension pneumothorax. As in the other types, definitive treatment for an open pneumothorax is the placement of a tube thoracostomy. (See Figure 4.)
Figure 4. Bilateral Pneumothoraces With Chest Tube Placement
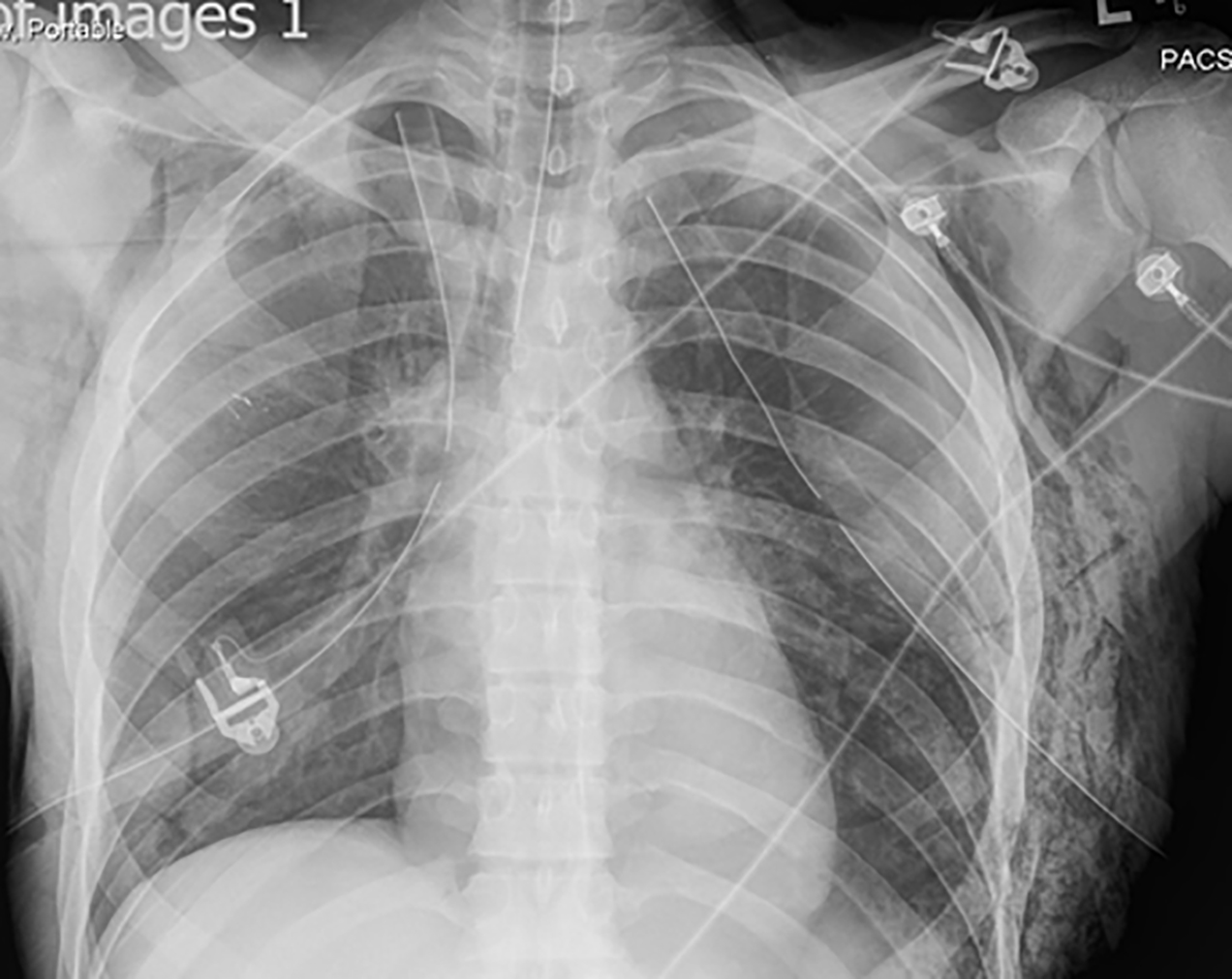
The chest radiograph shows bilateral pneumothoraces with bilateral tube thoracostomies. Note the subcutaneous emphysema seen bilaterally, worse on the left.
Image courtesy of A. Adewale, MD.
Hemothorax
A hemothorax is an accumulation of blood within the thoracic cavity. It is caused by injury to the intercostal vessels, the lung parenchyma, the internal mammary artery, or the great vessels.20 Much like a pneumothorax, a hemothorax limits the lungs’ ability to expand, leading to a ventilation-perfusion mismatch. Because the hemithorax can hold up to four liters of volume, patients rapidly bleeding into this cavity can exsanguinate. As a result, patients who sustain penetrating injuries to the great vessels often succumb to their injuries in the field. On the other hand, injury to the smaller vessels causes blood to accumulate slowly within the thoracic cavity, leading to the typical symptoms of pain, dyspnea, and tachypnea. (See Figures 5 and 6.)
Figure 5. Hemothorax With Pulmonary Contusion
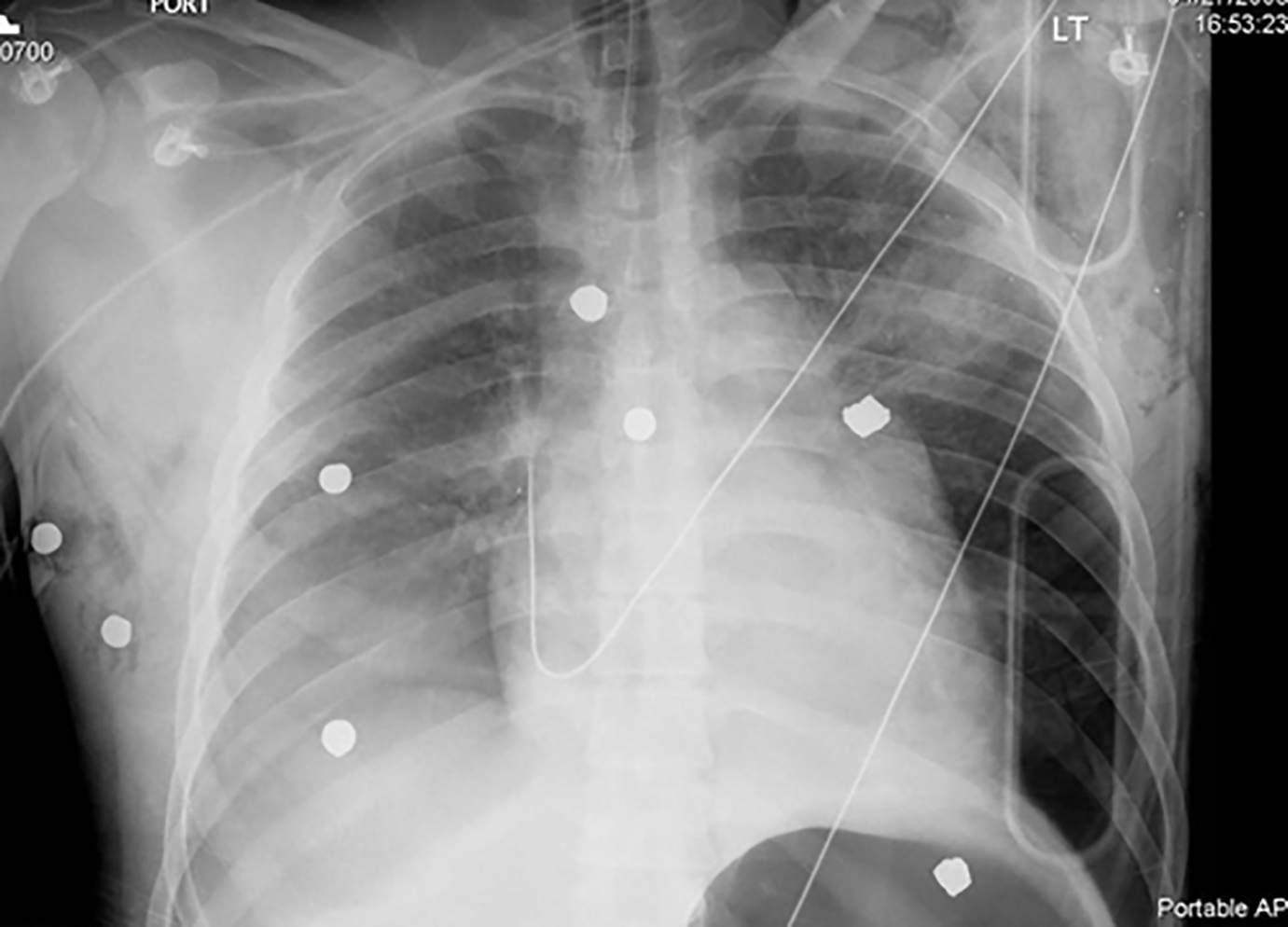
The chest radiograph above shows a male patient after a gunshot wound to the thorax with associated retained bullet fragments, right-sided hemothorax and pulmonary contusion, and subcutaneous emphysema.
Image courtesy of A. Adewale, MD.
Figure 6. Hemopneumothorax
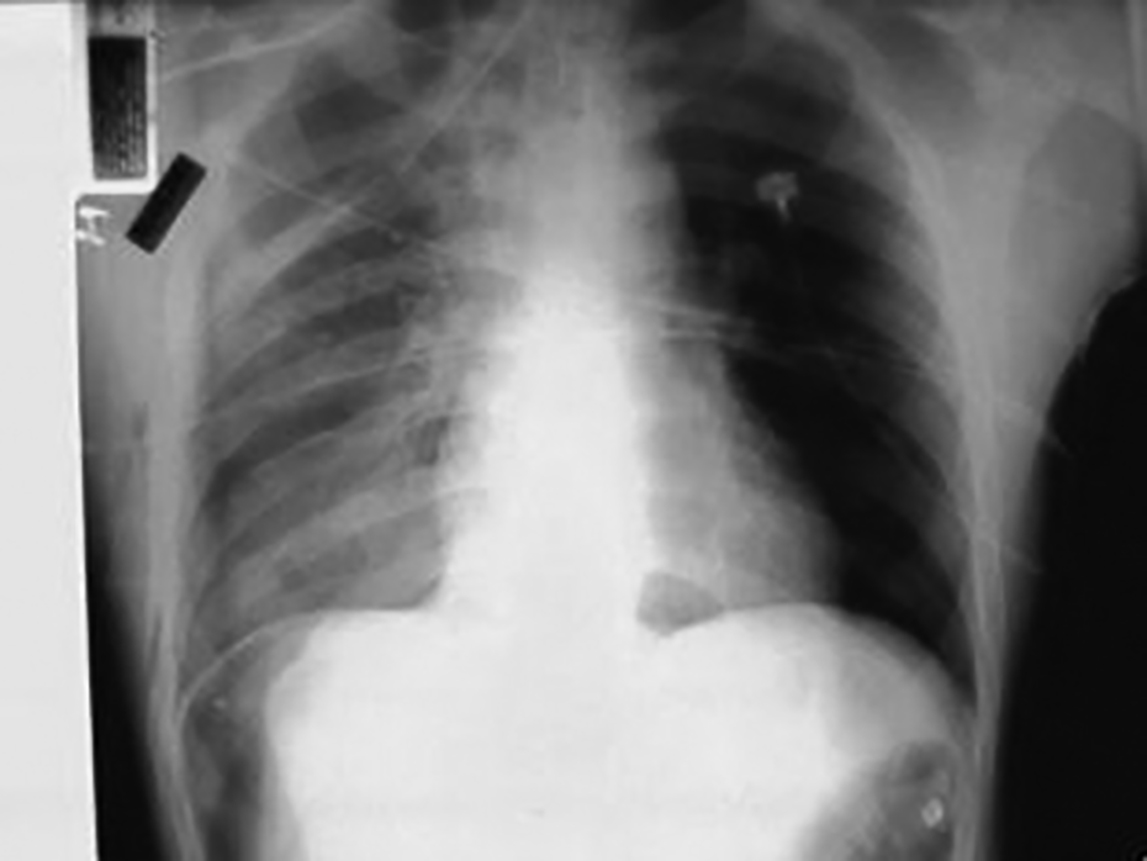
The above chest radiograph shows a deep sulcus sign with hemopneumothorax on the right after a gunshot wound to the chest.
Image courtesy of A. Adewale, MD.
The thoracic duct is another structure prone to injury in penetrating thoracic traumas. It is located within the left hemithorax and collects most of the lymph that circulates throughout the body. Injury to this structure leads to an entity called a chylothorax, which is the accumulation of this lymphatic fluid within the thorax. The symptoms are indistinguishable from a hemothorax, and the diagnosis most often is made when the milky appearing chyle drains from the chest tube.
The diagnosis of a hemothorax in penetrating chest trauma initially is based on the history and physical exam. The first diagnostic modality of choice remains a chest X-ray. However, it must be noted that chest radiographs can miss up to 1,000 mL of blood in the supine patient.44 As with a pneumothorax, ultrasound has been used as a modality for diagnosing hemothorax as well. Although not as sensitive in diagnosing a hemothorax as a pneumothorax, studies have shown ultrasound to be more effective than chest X-ray in diagnosing small amounts of fluid within the thoracic cavity.45 However, CT imaging remains the modality of choice because of its high sensitivity and specificity for diagnosing a hemothorax.46
The management of hemothorax after a penetrating wound involves a tube thoracostomy. Inaba et al evaluated whether the size of the chest tube affects complication rates. When comparing 28F chest tubes to 40F tubes, they found a similar rate of complications, a similar efficacy of drainage, and a similar level of pain, leading them to conclude that size does not matter.47 As mentioned earlier, another additional approach to dealing with an exsanguinating trauma patient with a hemothorax is early autologous fresh whole blood transfusion.24 It is important to note that once the chest tube is placed, there are indications to convert to a thoracotomy either in the ED or in the operating room. Rapid exsanguination from the chest tube, defined as more than 1,500 mL immediately returned, is an indication to perform a thoracotomy in the ED. If the chest tube drainage remains 200 to 250 mL/hour for more than four to five hours, a thoracotomy in the operating room to locate and ligate the bleeding vessel should be considered strongly.20
Pulmonary Contusion
Pulmonary contusions can be seen in both penetrating and blunt trauma. Unlike many of the other previously discussed pathologies, the sequelae of pulmonary contusions often develop over days rather than minutes. Pulmonary contusions occur from direct force to the chest wall. This results in damage to the lung parenchyma with associated hemorrhage and edema involving the alveoli. Extravasation of fluid into the alveoli and interstitial spaces leads to a worsening V/Q mismatch via shunting. Pulmonary contusions (see Figure 5) can lead to severe complications such as ARDS, respiratory failure, atelectasis, and pneumonia.48
The modalities for diagnosing a pulmonary contusion, like those of the other penetrating chest trauma injuries, are chest X-ray and CT scan. It is important to maintain a high suspicion for this injury because the patient’s initial images may appear benign. It often takes 24 to 48 hours after the initial injury to show the full sequelae of the disease process. Patients with poor PaO2/FiO2 ratios initially and with no overt signs of lung injury must be treated as having a pulmonary contusion until proven otherwise. Studies have shown a correlation between low PaO2/FiO2 ratios and greater volume of contused lung on follow-up CT scans.49
The management of pulmonary contusions depends on the severity, the presence of associated injuries, and the comorbid conditions of the patient. Again, because the full effect of pulmonary contusions does not develop until 24 to 48 hours after initial injury, it is important to monitor these patients closely. The mainstays of treatment are preventing respiratory failure and ensuring adequate blood oxygenation. Large contusions are challenging to manage.50 Noninvasive positive pressure ventilation can be useful for keeping collapsed alveoli open. However, patients with significant respiratory distress or those who are altered from other injuries require intubation. Injured lungs are prone to becoming stiff; therefore, high pressure settings on the ventilator often are required. The ARDS protocol was created to manage patients such as these. It allows for appropriate oxygenation in stiff and injured lungs.50 Although the physician must take care to avoid excessive volume resuscitation, the EAST guidelines gave a level 2 recommendation against excessive fluid resuscitation of patients with pulmonary contusions. The guidelines recommend resuscitating with isotonic crystalloid or colloid solution until there are signs of adequate tissue perfusion. Once the patient is properly resuscitated, however, the guidelines recommend against unnecessary fluid administration. As in patients with multiple rib fractures, the guidelines also emphasize the use of optimal analgesia and aggressive chest physiotherapy to decrease the likelihood of respiratory failure.51
Transmediastinal Injury
The mediastinum contains many vital structures. It can be divided into the superior and inferior mediastinum. The superior mediastinum contains the thymus, brachiocephalic veins, superior vena cava, azygous vein, aortic arch, pulmonary arteries, vagus nerve, and phrenic nerves. The inferior mediastinum is subdivided further into anterior, middle, and posterior. The anterior mediastinum contains the caudal thymus gland and sternopericardial ligaments. The middle mediastinum contains the heart and great vessels along with the phrenic nerves. The posterior mediastinum contains the descending aorta, esophagus, thoracic duct, sympathetic chains, vagus nerves, and hemiazygos vein. In penetrating chest trauma, great vessel injuries (superior vena cava, inferior vena cava, pulmonary arteries, pulmonary veins, and the aorta) often cause rapid hemorrhagic shock. As mentioned previously, these injuries have a very high mortality, and patients often exsanguinate before arriving in the ED.52
The diagnostic approach to trans-mediastinal injuries has changed over the years. As always, unstable patients need definitive and rapid intervention with the trauma surgeon in the operating room. The arresting patient often requires an ED thoracotomy. Traditionally, stable patients have received a very extensive evaluation, including an endoscopy, contrast swallow, angiography, and echocardiography. However, recent data have shown that a cardiac FAST exam and a CT angiogram are sufficient to rule out life-threatening injuries safely. When combined, they have a negative predictive value of 100%.53 A patient with penetrating chest trauma and a positive cardiac FAST needs intervention in the operating room. If the FAST is negative, the patient should have a CT angiogram performed. If there is obvious injury, the patient will require an interventional radiologist or surgeon to correct it definitively. If the scan is equivocal, the provider should perform the traditional, more extensive method for evaluation, which includes a bronchoscopy, angiography, esophagogastroduodenoscopy (EGD), and a swallow study.
The decision to perform an ED thoracotomy must be made within minutes. The goal, specifically in penetrating mediastinal injuries, is to locate and control great vessel or cardiac bleeding. In the ED setting, great vessel bleeds must be found and repaired using non-absorbable sutures. In patients who are exsanguinating, and in whom an intra-thoracic bleed cannot be located, cross clamping the aorta may be necessary as a temporary measure to shunt blood toward the body’s two most vital organs, the heart and brain. Although often difficult to identify, the aorta can be found lying anterior to the vertebral body and posterior to the esophagus. Once identified, a vascular clamp is used to occlude the descending aorta and obtain temporary hemostasis.19 In all cases of trans-mediastinal injuries, the physician must make decisions quickly because these patients have a propensity to deteriorate rapidly.
Cardiac Injuries
The prehospital mortality for penetrating cardiac injuries is approximately 86%.54 Cardiac injury should be suspected when the penetrating missile traverses “the precordial box.” The precordial box is the anatomic area within the thorax defined superiorly by the clavicles and sternal notch, laterally by the nipple line, and inferiorly by the xyphoid. In penetrating cardiac injuries, as opposed to blunt injuries, tamponade is less common because a laceration of the pericardium allows the blood to be released from the pericardial sac. (See Figure 7.) It remains important, however, to keep this differential diagnosis in mind in any unstable trauma patient. The physician should look for components of Beck’s triad, which can raise suspicion for cardiac tamponade. This triad consists of hypotension, jugular venous distention, and muffled heart sounds.
Ultrasound has become one of the most valuable tools in diagnosing cardiac injuries, particularly cardiac tamponade. The physician should keep in mind, however, that the absence of a pericardial effusion in patients with penetrating thoracic trauma does not rule out cardiac injuries, for the reasons stated above.55 Therefore, any violation to the precordial box requires a thorough workup, which includes a CT scan and a formal echocardiogram.
Definitive treatment for the crashing or arresting patient in whom a cardiac injury is suspected is an ED thoracotomy. Once the thoracic cavity is open and can be visualized, the area should be evaluated for injuries. If tamponade is present or suspected, a pericardiotomy should be performed to release fluid from the pericardial sac. When making the initial incision through the pericardium, care should be taken to avoid injury to the phrenic nerve. The phrenic nerve should be identified first and an incision should be made anterior and parallel to it. For penetrating wounds to the myocardium, a finger can be placed over the defect while awaiting definitive care. Another temporary measure is placing a Foley catheter through the wound to control bleeding. (See Figure 7B.) The balloon is inflated and the defect is occluded by pulling pressure. Penetrating myocardial injuries are closed definitively with surgical staples or with non-absorbable sutures. Although less common in penetrating trauma than blunt trauma, patients in a lethal arrhythmia can be resuscitated via internal defibrillation while the thorax is open. Internal paddles are placed on the anterior and posterior aspects of the heart, and a shock is administered directly to the myocardium. In an arresting patient, direct cardiac compressions can be performed in an open thorax as well.19
Figure 7A and 7B. Penetrating Cardiac Injury From Stab Wound
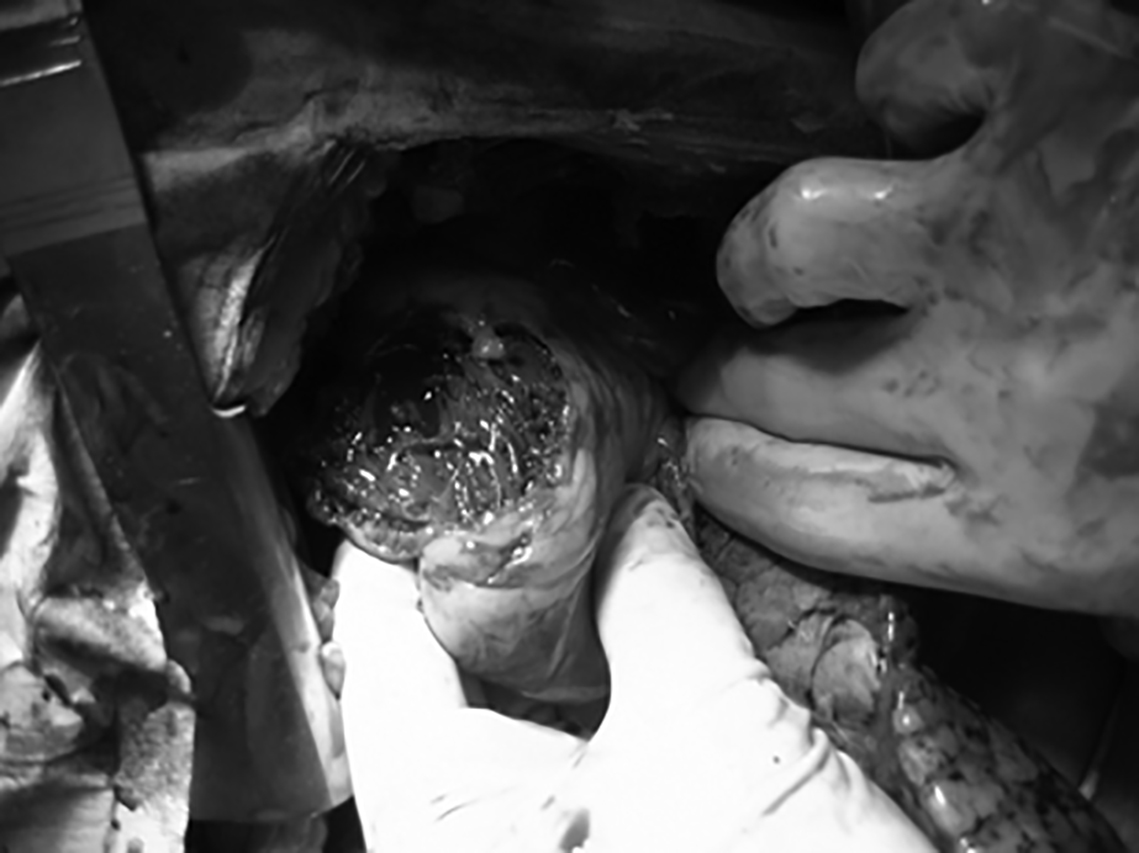
A. This image shows a ruptured myocardium after a stab wound to the anterior chest.

B. Rapid repair of ruptured myocardium with staples and Foley catheter tamponade before definitive operating room repair.
Images courtesy of A. Adewale, MD.
Tracheobronchial Injury
Tracheobronchial injuries include lacerations to the trachea or bronchi. Injuries to these structures allow air to accumulate within the pleural cavity, the mediastinum, and soft tissues. Although only seen in about 0.5% of trauma patients, the mortality rates remain very high.56 Complete lacerations to the trachea or bronchi lead to asphyxiation from an inability to keep the lung inflated. In about 30% of injuries that penetrate the tracheobronchial network, esophageal and major vascular injuries occur as well. Therefore, keeping a high suspicion for associated injuries is essential.57 Patients complaining of dyspnea, stridor, or hemoptysis after a penetrating thoracic or neck trauma must have tracheobronchial injuries included in their differential diagnosis. On physical exam, a crunching sound heard around the heart, referred to as Hamman’s crunch, and crepitus in the subcutaneous tissues are often present.58
Diagnosing tracheobronchial injuries can be difficult, and they often are missed initially if a high index of suspicion is not maintained. Although nonspecific, the first diagnostic modality of choice is a chest X-ray. Pneumomediastinum, subcutaneous air, and a pneumothorax that persists despite tube thoracostomy should increase the suspicion for this injury. CT scans are the best noninvasive modality for diagnosis, but they miss up to 10% of tracheobronchial injuries.59 Therefore, if the CT scan is equivocal, further imaging is required with tracheobronchoscopy, which remains the gold standard.60
The initial goals in treating tracheobronchial injuries include stabilizing the airway and defining the extent of the injury.59 Care must be taken because positive pressure ventilation and/or the placement of an endotracheal tube itself can convert a partial injury into a complete transection.59 Because these injuries often present as a pneumothorax, a chest tube should be placed. The presence of a persistent air leak is highly suggestive of tracheobronchial injury.61 In patients who are not improving, selective intubation of the non-injured lung has been shown to lead to better outcomes.20 Although minor injuries often heal without surgical intervention, patients who do not improve with intubation and chest tube placement may need more definitive repair. Definitive surgical intervention includes performing a thoracotomy or median sternotomy to either suture or resect the injured structure. A delay in diagnosis and treatment has been shown to influence outcomes negatively.62
Esophageal Injury
Esophageal injuries often are difficult to diagnose because they are not associated with a specific clinical sequela. The clinical picture may include painful swallowing; throat, neck, or chest pain; cough; hematemesis; dyspnea; and/or subcutaneous emphysema. Although esophageal injury is rare, one should maintain a high clinical suspicion for it in patients with a penetrating trauma that traverses the mediastinum with a left hemothorax or pneumothorax without a rib fracture, the presence of particulate matter in chest tube drainage, or the presence of pneumomediastinum.63
Definitive diagnosis can prove difficult because even with a high clinical suspicion, CT scan with IV contrast alone often can miss esophageal injuries. As mentioned in the section above, if there is no evidence that a penetrating object traversed the mediastinum on CT scan, no further imaging is required. However, if the CT scan is equivocal, further imaging is necessary because a missed esophageal injury portends a poor prognosis.63 An esophagram can be performed using a water-soluble contrast to detect injuries initially missed on CT. A flexible esophagogastroduodenoscopy is valuable because it directly visualizes the esophagus, but it should be used with caution in the acute setting because of the risk of additional injury.64
Initial ED management, as in all trauma patients, should include airway protection and fluid resuscitation. Early initiation of broad-spectrum antibiotics should be implemented in the ED as well. The definitive management for esophageal injuries depends on injury severity and the American Association for the Surgery of Trauma Organ Injury Severity Score (AAST-OIS) for the esophagus.65 The AAST-OIS score considers the circumferential size of the laceration and the amount of devascularization present. In patients who require operative management, an open surgery is the most common approach. The mortality for these injuries remains high, so early recognition and consultation for definitive management leads to the best outcomes.66
Diaphragm Injury
The diaphragm is a muscular structure essential mechanically for normal ventilation and anatomically for separating the negatively pressured thorax from the peritoneal cavity. Therefore, injuries to the diaphragm can lead to significant respiratory compromise or bowel injury. During normal respirations, the diaphragm spans T4 to T12; consequently, a high index of suspicion must be maintained with any injury for which the penetrating missile traverses this area. Diaphragmatic injuries are more common in isolation on the left because it is protected by the liver on the right.
Because of the difficulty in diagnosis, the incidence of occult diaphragmatic injuries has been measured as high as 24%.67 Diaphragmatic injuries may not be visualized on many imaging modalities. Complications of even small injuries include a nonfunctioning respiratory cavity or intra-abdominal contents herniating into the thorax, causing compression of the lung and/or bowel strangulation.68 (See Figure 8.)
Figure 8. Herniation of Colon
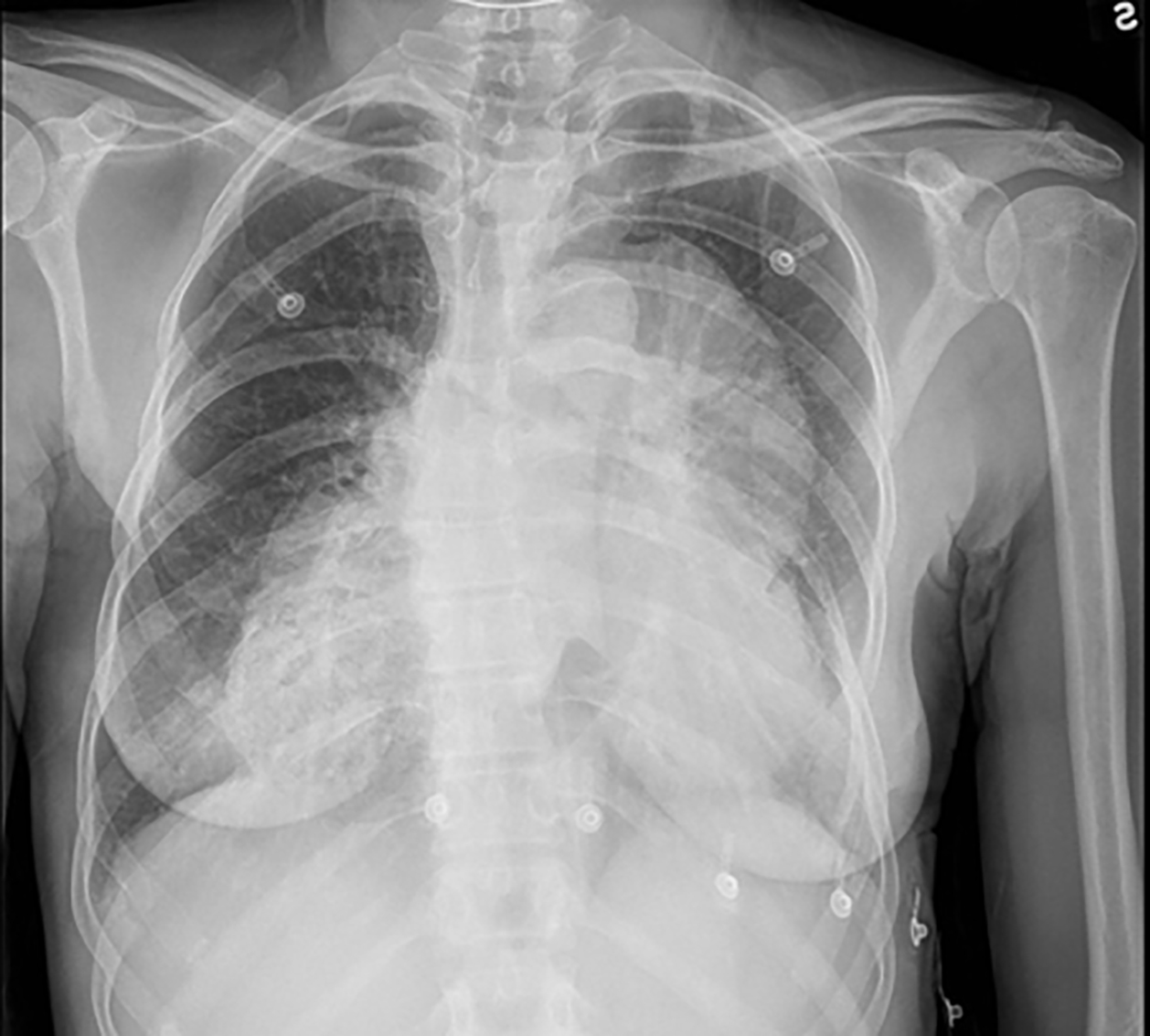
The chest radiograph demonstrates herniation of the colon within the anterior mediastinum after a previous diaphragmatic injury.
Image courtesy of A. Adewale, MD.
Diagnostic imaging of these injuries begins with a chest radiograph. Injuries that are large enough cause the bowel to herniate into the thorax, which can be seen on chest X-ray. Additionally, a coiled nasogastric tube in the thoracic cavity is diagnostic of a diaphragmatic injury. However, small injuries often are mistaken for other pathologies on chest X-ray. The sensitivity for a CT scan in diagnosing diaphragmatic injury approaches 84% with a specificity of 77%.69 MRI has a better sensitivity but has limited use in the acute trauma patient.70 Laparoscopy, a minimally invasive approach, has a sensitivity of 88% and specificity approaching 100% for diagnosing diaphragmatic injuries.71 Thoracoscopy is another modality for patients who have no other injuries requiring emergent operative management. A thorascope is inserted through a small incision, allowing the surgeon to visualize the lungs, mediastinum, and diaphragm directly.
Most diaphragmatic injuries require surgical management. The exception is small right-sided injuries that can be tamponaded by the liver. In stable patients, delayed surgical management may be preferred because it allows for more minimally invasive techniques. Although laparotomy always has been the treatment of choice for surgical repair of diaphragmatic defects, thoracolaparoscopic intervention is a newer, less invasive method of treatment.72
Conclusion
Penetrating chest trauma can be life-threatening because vital structures are housed within the thoracic cavity. Although much of the management of trauma patients has not changed over the years, better imaging modalities have allowed less invasive and more portable options for diagnosing injuries. Also, advances in resuscitation strategies with massive transfusion protocol, permissive hypotension, and availability of hemoglobin oxygen-carrying products has led to a decrease in morbidity. Regardless of the type of injury, an algorithmic approach to the trauma patient ensures a thorough evaluation and effective management strategy.
REFERENCES
- Centers for Disease Control and Prevention. National Center for Injury Prevention and Control. 2015.
- Rhee P, Joseph B, Pandit V, et al. Increasing trauma deaths in the United States. Ann Surg 2014;260:13-21.
- LoCicero J 3rd, Mattox KL. Epidemiology of chest trauma. Surg Clin North Am 1989;69:15.
- Spitzer A, Staudenmayer K, Tennakoon L, et al. Costs and financial burden of initial hospitalizations for firearm injuries in the United States, 2006–2014. Am J Public Health 2017;107:770-774.
- Boyd AD, Glassman LR. Trauma to the lung. Chest Surg Clin N Am 1997;7:263-284.
- Stefanopoulos PK, Hadjigeorgiou GF, Filippakis K, Gyftokostas D. Gunshot wounds: A review of ballistics related to penetrating trauma. Journal of Acute Disease 2014;3:178-185.
- Kirkpatrick AW, Ball CG, D’Amours SK, Zygun D. Acute resuscitation of the unstable adult trauma patient: Bedside diagnosis and therapy. Can J Surg 2008;51:57-69.
- Inaba K. Priorities in penetrating chest trauma. Lecture. UW Medicine EMS & Trauma Conference. Seattle, WA, September 28, 2015.
- Cannon CM, Braxton CC, Kling-Smith M, et al. Utility of the shock index in predicting mortality in traumatically injured patients. J Trauma 2009;67:1426-1430.
- Vandromme MJ, Griffin RL, Kerby JD, et al. Identifying risk for massive transfusion in the relatively normotensive patient: Utility of the prehospital shock index. J Trauma 2011;70:384-388.
- Sartorius D, Le Manach Y, David JS, et al. Mechanism, Glasgow coma scale, age, and arterial pressure (MGAP): A new simple prehospital triage score to predict mortality in trauma patients. Crit Care Med 2010;38:831-837.
- Rahmani F, Bakhtavar HE, Vahdati SS, et al. Evaluation of MGAP and GAP trauma scores to predict prognosis of multiple-trauma patients. Trauma Mon 2017;22:e33249.
- Soar J, Perkis GD, Abbas G, et al. European Resuscitation Council Guidelines for Resuscitation 2010 Section 8: Cardiac arrest in special circumstances: Electrolyte abnormalities, poisoning, drowning, accidental hypothermia, hyperthermia, asthma, anaphylaxis, cardiac surgery, trauma, pregnancy, electrocution. Resuscitation 2010; 81:1400-1433.
- Leis CC, Hernandez CC, Blanco MJ, et al. Traumatic cardiac arrest: Should advanced life support be initiated? J Trauma Acute Care Surg 2013;74:634-638.
- Orman R, Weingart S. No CPR in trauma arrest? ERCAST.ORG Podcast. March 10, 2015. Available at: http://blog.ercast.org/no-cpr-trauma-arrest/. Accessed June 23, 2017.
- Rhee PM, Acosta J, Bridgeman A, et al. Survival after emergency department thoracotomy: Review of published data from the past 25 years. J Am Coll Surg 2000;190:288-298.
- Beall AC Jr, Diethrich EB, Cooley DA, DeBakey ME. Surgical management of penetrating cardiovascular trauma. South Med J 1967;60:698–704.
- Seamon, MJ, Haut ER, Van Arendonk K, et al. An evidence-based approach to patient selection for emergency department thoracotomy: A practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 2015;79:159-173.
- Jones RF, Rivers EP. Resuscitative thoracotomy. In: Roberts JR, Custalow CB, Thomsen TW, et al, eds. Roberts and Hedges’ Clinical Procedures in Emergency Medicine. 6th ed. Philadelphia: Elsevier Saunders; 2014:325-340.
- American College of Surgeons Committee on Trauma. Advanced Trauma Life Support for Doctors (ATLS). 6th ed. Chicago: American College of Surgeons; 1997.
- Alrajab S, Youssef AM, Akkus NI, Caldito G. Pleural ultrasonography versus chest radiography for the diagnosis of pneumothorax: Review of the literature and meta-analysis. Crit Care 2013;17:R208.
- Patel AN, Brenning C, Cotner J, et al. Successful diagnosis of penetrating cardiac injury using surgeon-performed sonography. Ann Thorac Surg 2003;76:2043-2047.
- Salhanick M, Corneille M, Higgins R, et al. Autotransfusion of hemothorax blood in trauma patients: Is it the same as fresh whole blood? Am J Surg 2011;202:817-822.
- Rhee P, Inaba K, Pandit V, et al. Early autologous fresh whole blood transfusion leads to less allogenic transfusions and is safe. J Trauma Acute Care Surg 2015;78:729-734.
- Mapstone J, Roberts I, Evans P. Fluid resuscitation strategies: A systematic review of animal trials. J Trauma 2003;55:571-589.
- Dente CJ, Shaz BH, Nicholas JM, et al. Improvements in early mortality and coagulopathy are sustained better in patients with blunt trauma after institution of a massive transfusion protocol in a civilian level I trauma center. J Trauma 2009;66:1616-1624.
- Seamon MJ, Medina CR, Pieri PG, et al. Follow-up after asymptomatic penetrating thoracic injury: 3 hours is enough.
J Trauma 2008;65:549-553. - Ziegler DW, Agarwal NN. The morbidity and mortality of rib fractures. J Trauma 1994;37:975-979.
- Flagel BT, Luchette FA, Reed RL, et al. Half-a-dozen ribs: The breakpoint for mortality. Surgery 2005;138:717-723.
- Witt CE, Bulger EM. Comprehensive approach to the management of the patient with multiple rib fractures: A review and introduction of a bundled rib fracture management protocol. Trauma Surgery & Acute Care Open 2017;2(1). [Published online Jan. 5, 2017.]
- Sirmali M, Türüt H, Topçu S, et al. A comprehensive analysis of traumatic rib fractures: Morbidity, mortality and management. Eur J Cardiothorac Surg 2003;24:133-138.
- Pettiford BL, Luketich JD, Landreneau RJ. The management of flail chest. Thorac Surg Clin 2007;17:25-33.
- Livingston DH, Shogan B, John P, Lavery RF. CT diagnosis of rib fractures and the prediction of acute respiratory failure.
J Trauma 2008;64:905. - Bayouth L, Safcsak K, Cheatham ML, et al. Early intravenous ibuprofen decreases narcotic requirements and length of stay after traumatic rib fracture. Am Surg 2013;79:1207-1212.
- Galvagno SM Jr., Smith CE, Varon AJ, et al. Pain management for blunt thoracic trauma: A joint practice management guideline from the Eastern Association for the Surgery of Trauma and Trauma Anesthesiology Society. J Trauma Acute Care Surg 2016;81:936-951.
- Slobogean GP, MacPherson CA, Sun T, et al. Surgical fixation vs nonoperative management of flail chest: A meta-analysis.
J Am Coll Surg 2013:216:302-311. - Bulge EM, Arenson MA, Mock CN, Jurkovich GJ. Rib fractures in the elderly. J Trauma 2000;48:1040-1046.
- Wilkerson RG, Stone MB. Sensitivity of bedside ultrasound and supine anteroposterior chest radiographs for the identification of pneumothorax after blunt trauma. Acad Emerg Med 2010;17:11-17.
- Lichtenstein DA, Mezière GA. Relevance of lung ultrasound in the diagnosis of acute respiratory failure: The BLUE protocol. Chest 2008;134:117-125.
- Husain LF, Hagopian L, Wayman D, et al. Sonographic diagnosis of pneumothorax. J Emerg Trauma Shock 2012;5:76-81.
- Stevens RL, Rochester AA, Busko J, et al. Needle thoracostomy for tension pneumothorax: Failure predicted by chest computed tomography. Prehosp Emerg Care 2009;13:14-17.
- Inaba K, Branco BC, Eckstein M, et al. Optimal positioning for emergent needle thoracostomy: A cadaver-based study.
J Trauma 2011;71:1099-1103; discussion 1103. - Kulvatunyou N, Erickson L, Vijayasekaran A. Randomized clinical trial of pigtail catheter versus chest tube in injured patients with uncomplicated traumatic pneumothorax. Br J Surg 2014;101:17-22.
- Broderick SR. Hemothorax: Etiology, diagnosis, and management. Thorac Surg Clin 2013;23:89-96.
- Ojaghi Haghighi SH, Adimi I, Shams Vahdati S, Sarkhoshi Khiavi R. Ultrasonographic diagnosis of suspected hemopneumothorax in trauma patients. Trauma Mon 2014;19:e17498.
- Abboud PA, Kendall J. Emergency department ultrasound for hemothorax after blunt thoracic injury. J Emerg Med 2003;25:181-184.
- Inaba K, Lustenberger T, Recinos G, et al. Does size matter? A prospective analysis of 28-32 versus 36-40 French chest tube size in trauma. J Trauma Acute Care Surg 2012;72:422-427.
- Raghavendran K, Notter RH, Davidson BA, et al. Lung contusion: Inflammatory mechanisms and interaction with other injuries. Shock 2009;32:122-130.
- Mizushima Y, Hiraide A, Shimazu T, et al. Changes in contused lung volume and oxygenation in patients with pulmonary parenchymal injury after blunt chest trauma. Am J Emerg Med 2000;18:385-389.
- Ganie FA, Lone H, Lone GN, et al. Lung contusion: A clinico-pathological entity with unpredictable clinical course. Bull Emerg Trauma 2013;1:7-16.
- National Guideline Clearinghouse (NGC). Guideline summary: Management of pulmonary contusion and flail chest: An Eastern Association for the Surgery of Trauma practice management guideline. National Guideline Clearinghouse (NGC) Rockville (MD): Agency for Healthcare Research and Quality (AHRQ); 2012 Nov 01.
- Mattox KL, Feliciano DV, Burch J, et al. Five thousand seven hundred sixty cardiovascular injuries in 4459 patients. Epidemiologic evolution 1958 to 1987. Ann Surg 1989;209:698-705.
- Stassen NA, Lukan JK, Spain DA, et al. Reevaluation of diagnostic procedures for transmediastinal gunshot wounds.
J Trauma 2002;53:635-638. - von Oppell UO, Bautz P, De Groot M. Penetrating thoracic injuries: What we have learnt. Thorac Cardiovasc Surg 2000;48:55-61.
- Ball CG, Williams BH, Wyrzykowski AD, et al. A caveat to the performance of pericardial ultrasound in patients with penetrating cardiac wounds. J Trauma 2009;67:1123-1124.
- Gussack GS, Jurkovich GJ, Luterman A. Laryngotracheal trauma: A protocol approach to a rare injury. Laryngoscope 1986;96:660-665.
- Scope A, Farkash U, Lynn M, et al. Mortality epidemiology in low-intensity warfare: Israel Defense Forces’ experience. Injury 2001;32:1-3.
- Balci AE, Eren N, Eren S, Ulku R. Surgical treatment of post-traumatic tracheobronchial injuries: 14-year experience. Eur J Cardiothorac Surg 2002;22:984-989.
- Karmy-Jones R, Wood DE. Traumatic injury to the trachea and bronchus. Thorac Surg Clin 2007;17:35-46.
- Chen D, Han L, Hu Y, et al. Diagnosis and treatment of bronchial rupture from blunt thoracic trauma. Chin Med J (Engl) 2001;114:540-541.
- Kunisch-Hoppe M, Hoppe M, Rauber K, et al. Tracheal rupture caused by blunt chest trauma: Radiological and clinical features. Eur Radiol 2000;10:480-483.
- Cassada DC, Munyikwa MP, Moniz MP, et al. Acute injuries of the trachea and major brochi: Importance of early diagnosis. Ann Thorac Surg 2002;69:1563-1567.
- Asensio JA, Chahwan S, Forno W, et al. Penetrating esophageal injuries: Multicenter study of the American Association for the Surgery of Trauma. J Trauma 2001;50:289.
- Wu JT, Mattox KL, Wall MJ Jr. Esophageal perforations: New perspectives and treatment paradigms. J Trauma 2007;63:1173.
- Moore EE, Jurkovich GJ, Knudson M, et al. Organ injury scaling. VI: Extrahepatic biliary, esophagus, stomach, vulva, uterus (nonpregnant), uterus (pregnant), fallopian tube, and ovary. J Trauma 1995;39:1069-1070.
- Port JL, Kent MS, Korst RJ, et al. Thoracic esophageal perforation: A decade of experience. Ann Thorac Surg 200;75:1071-1074.
- Murray JA, Demetriades D, Asensio JA, et al. Occult injuries to the diaphragm: Prospective evaluation of laparoscopy in penetrating injuries to the left lower chest. J Am Coll Surg 1998;187:626-630.
- Fair KA, Gordon NT, Barbosa RR, et al. Traumatic diaphragmatic injury in the American College of Surgeons National Trauma Data Bank: A new examination of a rare diagnosis. Am J Surg 2015;209:864.
- Larici AR, Gotway MB, Litt HI, et al. Helical CT with sagittal and coronal reconstructions: Accuracy for detection of diaphragmatic injury. AJR Am J Roentgenol 2002;179:451-457.
- Barbiera F, Nicastro N, Finazzo M, et al. The role of MRI in traumatic rupture of the diaphragm. Our experience in three cases and review of literature. Radiol Med 2003;105:188-194.
- Friese RS, Coln CE, Gentilello LM. Laparoscopy is sufficient to exclude occult diaphragm injury after penetrating abdominal trauma. J Trauma 2005;58:789.
- Lomanto D, Poon PL, So JB, et al. Thoracolaparoscopic repair of traumatic diaphragmatic rupture. Surg Endosc 2001;15:323.
Penetrating trauma of the chest can have severe and devastating consequences. Advances in ultrasound and treatment therapies have improved survival. A high degree of suspicion is indicated to identify the more subtle injuries associated with penetrating trauma to the chest.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
