Pediatric Wrist and Elbow Injuries: Mechanisms of Injury, Findings, and Treatment
Pediatric Wrist and Elbow Injuries: Mechanisms of Injury, Findings, and Treatment
Authors: Carl Menckhoff, MD, Associate Professor, Department of Emergency Medicine, Medical College of Georgia, Augusta; Cherie Welter, MD, Resident, Medical College of Georgia, Augusta; and Cynthia Sessums, DO, Resident, Department of Emergency Medicine, Medical College of Georgia, Augusta.
Peer Reviewer: Moira Davenport, MD, Attending Physician, Department of Emergency Medicine, Department of Orthopaedic Surgery, Allegheny General Hospital/Drexel University School of Medicine, Pittsburgh, PA.
Injuries of the wrist and elbow in children are frequently seen in the emergency department (ED), and as children and adolescents are participating in sports in record numbers, the frequency of these injuries is continuing to rise. Sports injuries in children and adolescents are by far the most common cause of musculoskeletal injuries treated in the ED, accounting for 41% of all musculoskeletal injuries.1 This article will outline common, important wrist and elbow injuries in children and will review likely mechanisms of injury, radiographic findings, and treatment.
The Editor
Physeal Injuries
One of the major differences between the pediatric and the adult skeleton is the presence of growth plates or physes.2,3 When seeing pediatric patients with any injury to the extremity, physeal injury always must be considered. The physis is the site of ossification and longitudinal bone growth.4 It consists of four zones in order from the epiphysis to the metaphysis: the zone of resting cells, the zone of proliferating cells, the zone of hypertrophic/maturing cells, and the zone of provisional calcification. The third zone, consisting of hypertrophic maturing cells, is the weakest link in the physis.2 This area lacks mechanical strength and is more susceptible to injury than the surrounding ossified bone.2 Childrens' ligaments are stronger and more compliant when compared to bone than those of adults. This often leads to physeal or bony injury before ligamentous disruption. The main concern with these fractures is premature closure of the physis and resultant growth arrest. The risk of complications increases with the severity of the fracture. Physeal injuries account for 15-30% of all pediatric fractures and while complications are uncommon, significant growth disturbance can occur in approximately 10% of injuries.5,6 Though injury to the physis can occur at any time prior to physeal closure, it is more common during the adolescent growth spurt (between ages 10 and 16 years) and is more common in boys than in girls.2,7,8 The distal radius is the most common site of physeal injury.
Drs. Robert Salter and J. J. Harris described the Salter-Harris Classification of physeal fractures in 1963.2,9,10 This classification system describes the 5 types of fractures involving the physis and is based on the involvement of the metaphysis, physis, and epiphysis.
Type I. Salter-Harris I fractures are a disruption through the physis.2,7 Approximately 6% of physeal fractures are Type I fractures.9 These fractures do not involve any osseous fracture to the epiphysis or metaphysis. The more severe Type I injuries involve displacement of the epiphysis, usually in the dorsal direction, and require gentle reduction. The hallmark of this injury is point tenderness. These can be difficult to detect radiographically because they involve only the physis, which is radiolucent. When a child presents with point tenderness over the growth plate but has normal radiographs, clinicians should be suspicious of a Type I fracture and treat the patient accordingly with immobilization and follow-up.7,9
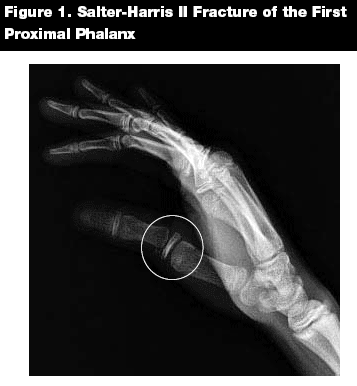
Type II. Salter-Harris II fractures (see Figure 1) are the most common type of all physeal fractures, accounting for 75%.2,11 They extend through the physis and metaphysis. The segment of metaphyseal bone is referred to as the "Thurston-Holland" fragment or sign.2 The germinal layer is not involved; therefore, growth disturbances are rare. These injuries also should be treated with gentle reduction and immobilization, along with outpatient follow-up. Excessive, closed manipulation can lead to an increase in the amount of physeal damage, increasing the risk for growth plate arrest.5 A perfect reduction is not an absolute requirement as the younger the child, the greater the capacity for bone remodeling.
 |
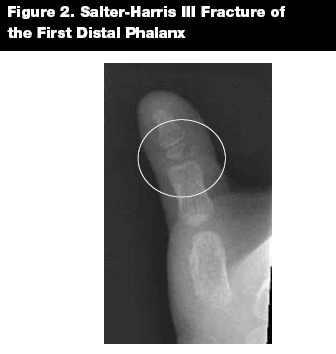
Type III. Salter-Harris III fractures (see Figure 2) are intra-articular fractures of the epiphysis that extend across the physis. They account for approximately 10% of physeal fractures.11 The prognosis is good but more guarded than with type I or II fractures and is related to the preservation of the blood supply.2 Since type III injuries occur predominantly in older adolescents, the physis has less remaining growth potential; therefore, these fractures seldom result in significant shortening. The treatment goal with these fractures is to anatomically realign the joint surface.5 Orthopedic consultation in the ED often is required.
 |
Type IV. Salter-Harris IV fractures represent approximately 10% of all physeal fractures.2,12 These are intra-articular fractures that have a high risk of growth disturbance. The fracture line originates at the articular surface, crosses the epiphysis, extends through the full thickness of the physis, and exits through a segment of the metaphysis.2 As with type III fractures, anatomic reduction is required to prevent the formation of bony bridges between the metaphysis and the epiphysis.5 Type IV fractures are more likely to require operative intervention to achieve anatomic reduction, and the risk of growth disturbance is dependent on the degree of blood supply disruption through the epiphysis.
Type V. Salter-Harris V fractures are crush injuries of the physeal plate that are usually produced by compressive forces. They account for only about 1% of all physeal fractures.2 They are by far the most likely of all of the physeal injuries to result in bone growth arrest.2,10 The compressive forces crush the physis and injure cells of the reserve and proliferative zones,2 and there is minimal or no displacement of the epiphysis. One may see narrowing of the physis radiographically, but sometimes the only radiographic evidence is a joint effusion. The injury is commonly diagnosed retrospectively once a bone growth abnormality has been identified.11
Wrist Injuries
Introduction. Fractures of the radius and/or ulna are the most common fractures in children and adolescents, accounting for 45% of pediatric fractures.12,13 Of these fractures, 78-84% occur distally13 and are usually the result of a fall on an outstretched hand (FOOSH) or blunt trauma. A common cause of distal radius fracture in children is from falling off of a skateboard, inline skates, or rollerblades.14 Falls that occur when the patient's wrist is in hyperextension can result in displaced or angulated fractures. One study found that radiographs should be obtained in children with acute wrist injuries if there is point tenderness over the distal radius and more than a 20% decrease in grip strength compared with the normal hand. The authors did not find any significant correlation between the presence of a fracture, degree of soft tissue swelling, or change in the range of motion.13 There are two types of distal radius fractures: fractures involving the distal radial metaphysis and fractures that involve the physis. While the distal radius is the most common site of physeal fractures, they are much less common than distal radius fractures involving the metaphysis.7
Traumatic injury to the immature carpal bones is infrequent in the pediatric population due to the sequence of carpal ossification, the relative strength of the surrounding ligaments, and the vulnerability of the radius to fracture. Mechanisms that would cause bony wrist injuries in the adult tend to produce fractures of the forearm in children.
Anatomy. The wrist consists of the distal radius and ulna and their articulation with the carpal bones. The ossific nucleus of the distal radial physis appears at 10 months in girls and 12 months in boys. Cessation of growth of the distal radius occurs at age 17 years in girls and age 19 years in boys.15 The capitate is the first carpal bone to begin ossification at 2-3 months of age, with the hamate approximately one month later. Ossification then proceeds in a clockwise direction. The triquetrum begins to ossify at age 2 years, the lunate at age 3 years, the scaphoid at age 5 years, and the trapezoid and trapezium at age 6 years. The pisiform does not appear on radiographs until age 9 or 10 years of age.11
Radiographic Assessment. Anteroposterior (AP) and lateral view of the wrist are the minimum necessary to assess for fractures of the carpal bones and distal radius and ulna. An oblique view also is often helpful, and special views, such as a scaphoid view, are helpful for evaluating specific injuries. While controversial, due to the presence of the growth plate in pediatric patients, it may be helpful to get a radiograph of the uninjured side for comparison.
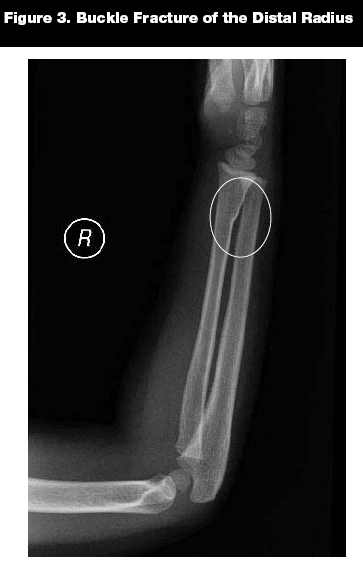
Radial Fractures. There are three types of radial metaphysis fractures: torus (buckle) fractures, greenstick fractures, and complete fractures. The most common is the torus or buckle fracture, and the distal radius is the most common site.7,13 Torus fractures (see Figure 3) are caused by compressive forces that lead to buckling of the cortex. The injury often is subtle and, therefore, commonly overlooked. The increased flexibility of children's bones allows for this phenomenon and it typically occurs in children ages 6-12 years with a FOOSH injury.16 These fractures usually do not require reduction and simple splinting/casting is sufficient.
 |
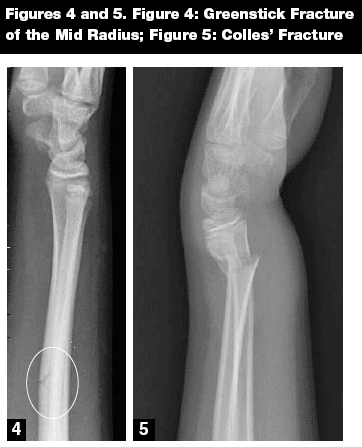
Greenstick fractures are incomplete fractures (see Figure 4), with disruption of the cortex on one side of the bone and angulation on the opposite side. The periosteum buckles on one side and breaks on the other side. These fractures are angulated but not displaced because the bone ends are not separated. Angulation of greater than 15 degrees requires closed reduction, and all fractures require immobilization in a forearm sugar tong splint and follow-up.17 These fractures have a tendency to displace if they are not properly immobilized, so radiographs should be repeated in 10 days to be certain the reduction has been maintained.
 |
Complete fractures involve the fracture line extending through the cortex at both ends. They can be displaced, nondisplaced, open, or closed. Complete fractures include transverse, spiral, and oblique fractures. Several examples are discussed below.
Colles' Fractures. Epidemiology. A Colles' fracture (see Figure 5) is a transverse fracture to the distal radial metaphysis with dorsal displacement and volar angulation16,17 (angulation direction is defined by the apex of the angle formed).
Patterns of Injury. Colles' fractures typically result from a FOOSH.
Evaluation. On exam, patients complain of pain over the dorsum of the wrist and may have a "dinner fork" deformity of the wrist secondary to the dorsal displacement and angulation of the fracture.16 A neurovascular exam should be done to exclude median nerve injury. Median nerve injury can be caused by the traction from the original fracture displacement, direct injury by fractured fragments, by traction on the nerve during closed reduction, or by position of immobilization.18 Neurologic function always should be documented before and after any fracture reduction.
Imaging. The AP and lateral views of the wrist show the fracture through the radial metaphysis. The degree of displacement and angulation usually is best seen on the lateral view.18
Management. In children, displacement of up to 40% can be tolerated because of the ability of pediatric bone to remodel, but significant rotational deformities are not acceptable and require reduction.16 Prompt reduction should be done when necessary, with an attempt to restore the distal radius toward the normal volar tilt. Closed reduction and immobilization in a forearm sugar tong splint, with slight volar angulation at the wrist, is usually successful18 and surgery is not usually necessary.
Key Points. A Colles' fracture is a transverse fracture to the distal radial metaphysis with dorsal displacement and volar angulation. These fractures usually result from a FOOSH and most often can be managed with closed reduction and splinting in the ED.
Smith's Fractures. Epidemiology. A Smith's fracture (see Figure 6) is much less common than a Colles' fracture. It is a transverse fracture of the metaphysis of the distal radius with volar displacement of the distal fragment. Because the deformity is the reverse of that seen in a Colles' fracture, it is sometimes referred to as a reverse Colles' fracture.18
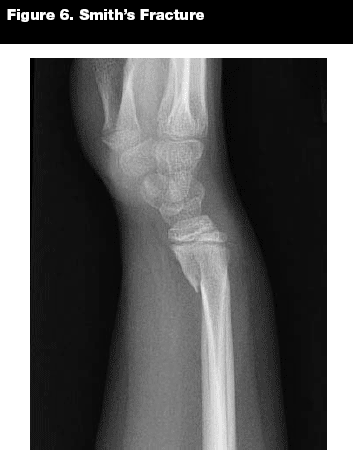 |
Pattern of Injury. There usually is a history of a direct blow to the dorsum of the wrist or a fall with the wrist in a flexed position. Smith's fractures are also sometimes seen after a fall backward on an outstretched hand with the forearm in supination.
Evaluation. The wrist is typically swollen and painful with a visible deformity on the volar aspect of the wrist. Smith's fractures are more likely to be unstable and less displacement can be tolerated (usually less than 10 degrees) before requiring closed reduction or open reduction and internal fixation (ORIF).16 There is a risk of injury to the median nerve as with Colles' fractures, and a neurologic exam should be performed and documented before and after reduction.
Imaging. The fracture can be seen on AP and lateral radiographs of the wrist. The lateral view is best for showing the degree of displacement and angulation.18
Management. The management for a Smith's fracture typically involves closed reduction, immobilization in a sugar tong splint, and orthopedic follow-up or consultation.16 Keep in mind that less than 10 degrees of displacement is tolerated; if this is not maintained by immobilization, ORIF may be required.
Key Points. Smith's fractures are less stable than Colles' fractures and may need ORIF if splinting doesn't maintain adequate reduction.
Galeazzi Fractures. Epidemiology. Galeazzi fractures (see Figures 7a and 7b) are fractures of the distal radius with disruption of the radio-ulnar joint (RUJ). These fractures are rare in children, with one study finding that less than 5% of all radial shaft fractures in children were associated with obvious disruption of the RUJ.17 Children may have separation of the ulnar physis rather than true disruption of the RUJ. This injury is known as a Galeazzi-equivalent injury.18
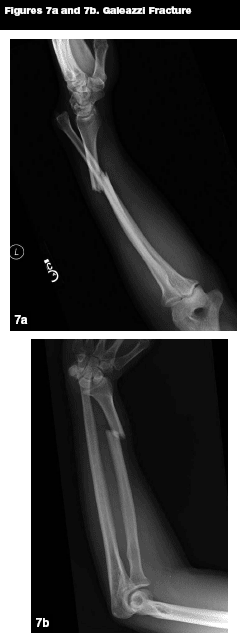 |
Patterns of Injury. The mechanism of injury is typically a fall from a height or a similar mechanism such as a fall that occurs while running, playing football, or rollerblading.17,19
Evaluation. The patient usually will complain of distal radius pain, and there may be deformity noted in the distal forearm. Neurovascular injury is uncommon. Supination and pronation of the forearm causes pain.
Imaging. An AP and a true lateral radiograph should be taken to assess the injury. Every effort should be made to obtain a true lateral radiograph so that any displacement of the distal ulna will be noted. In general, the distal ulna is seen posterior to the distal radius on the true lateral radiograph, but if this distance exceeds 4 mm, a RUJ disruption should be suspected. On the AP view, the distance between the radius and ulna at the RUJ should not exceed 2 mm.
Management. In contrast to adults, both Galeazzi and Galeazzi-equivalent injuries usually can be treated in young children with closed reduction and immobilization.18 Once the radial fracture is reduced, relocation of the RUJ should be checked. The arm should then be immobilized with a long arm splint. It is recommended that the forearm be held in supination in the splint to provide maximum stability.17
Key Points. Always assess the distal RUJ in any patient with a radius fracture. If the joint is disrupted, then a Galeazzi fracture exists. Unlike in adults, many of these can be treated with closed reduction and splinting in children.
Monteggia Fractures. Epidemiology. In 1814, Giovanni Monteggia first described a proximal ulna fracture with an associated radial head dislocation (see Figure 8).20,21 The Monteggia fracture accounts for only 2-3% of elbow injuries that occur in childhood.20,22
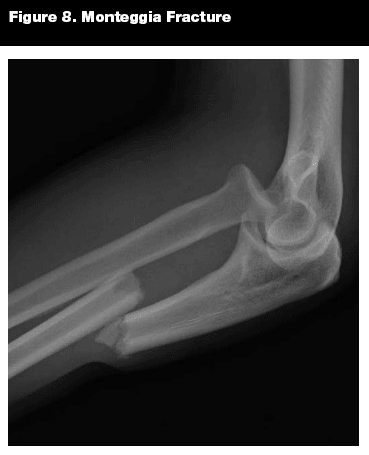 |
Patterns of Injury. The typical mechanism of injury is forced pronation of the forearm during a fall on the outstretched arm, but it also can result from a direct blow to the posterior aspect of the ulna.18,23
Evaluation. On exam, pain and tenderness are present at the fracture site and there is a decrease in the range of motion at the elbow. Elbow swelling also may be present, and forearm shortening may be appreciated when compared with the unaffected side.18 Palpation of the radial head may confirm its dislocation. Depending on the position of the dislocated radial head, it may be palpable in the antecubital fossa, laterally or posteriorly. Weakness or inability to extend the fingers or thumb is indicative of an injury to the posterior interosseous nerve.23 This is a deep branch of the radial nerve, which lies close to the neck of the radius and may be stretched when the radial head is dislocated.23
Imaging. Obtain AP, lateral, and oblique radiographs of the forearm, and AP and lateral views of the elbow. To avoid missing a subtle radial head dislocation, always confirm good radiocapitellar alignment (described below) on the AP and lateral radiographs.23 Keep in mind that even bowing fractures of the ulna can be associated with a radial head dislocation.
Management. Obtain an orthopedic consultation for these patients. The majority of Monteggia fractures in children can be treated by closed reduction and splinting, although delayed treatment in teenagers sometimes requires open reduction.24
Key Points. Carefully evaluate the radial head in all ulna fractures to avoid missing radial head dislocations. If unrecognized, these injuries can result in chronic pain and long-term limitation of function.
Carpal Injuries. Traumatic injury to the immature carpal bones (several of which are described below) is infrequent because of the sequence of carpal ossification, the resiliency of the surrounding ligaments and the vulnerability of the radius to fracture. Fractures of the proximal carpal row (scaphoid, lunate, triquetrum, and pisiform) are more frequent than fractures of the distal row (trapezium, trapezoid, capitate, and hamate). The capals are composed of cartilage at birth, which helps to dissipate energy and axial loading and minimizes fractures. Mechanisms that would cause bony wrist injuries in the adult tend to produce fractures of the forearm in children. Fractures of carpal bones comprise less than 2% of all fractures.25
Carpal fractures usually result from direct trauma or significant loading. Carpal fractures in younger children are rare and frequently associated with other fractures. Direct blows to the carpal region usually are associated with sports activities such as hockey, lacrosse, and martial arts.
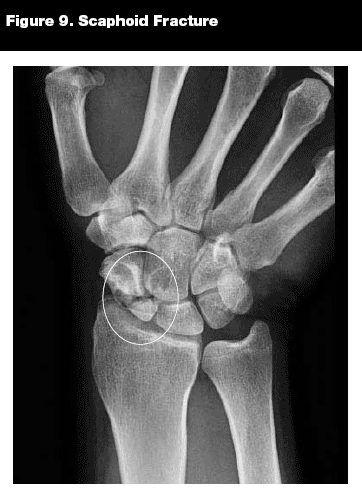 |
Scaphoid Fractures. Epidemiology. The scaphoid is the most commonly fractured carpal bone (see Figure 9).26 Most pediatric fractures to the scaphoid occur in children ages 11-15 years,7,25 and are rare in children younger than age 10 years.5 The blood supply to the scaphoid comes from the radial artery, feeding the bone in the dorsal surface near the tubercle and the scaphoid waist. The proximal portion has no direct blood supply, so nonunion and avascular necrosis can be important complications of scaphoid fractures;27 this occurs more frequently in proximal scaphoid fractures. Since 90% of scaphoid fractures that occur in children tend to be in the distal one-third of the scaphoid,25 avascular necrosis occurs less frequently.
Patterns of Injury. The mechanism of injury is typically hyperextension of the wrist due to a FOOSH or direct axial compression. When the wrist is hyperextended greater than 95 degrees, the indentation in the midbody of the scaphoid is forced against the dorsal lip of the distal radius and creates a fulcrum.25 When this motion is forceful, such as with a FOOSH, there can be enough stress on the scaphoid to cause a fracture.
Evaluation. The patient usually will complain of pain on the radial side of the wrist, which is worsened by gripping, flexion, or extension. There may be wrist swelling and fullness in the anatomic snuffbox (the triangular depression defined by the abductor pollicis longus and extensor pollicis brevis anteriorly and the extensor pollicis longus posteriorly),29 suggesting a wrist effusion.25
On exam there is tenderness of the anatomic snuffbox, decreased range of motion in flexion and extension, pain with radial deviation of the wrist, and a positive scaphoid compression test. The scaphoid compression test is performed by holding the thumb and pushing in toward the scaphoid along the longitudinal axis of the thumb metacarpal. Pain elicited over the palmar scaphoid tubercle constitutes a positive test.5,28 Pain on palpation of the volar prominence at the distal wrist crease is common in distal pole fractures.
Imaging. AP, true lateral, oblique, and scaphoid views should be obtained for suspected scaphoid fractures.26 A scaphoid view is taken in an AP projection with the wrist in full pronation with ulna deviation and is shot at a 20-degree angle toward the elbow. This view shows the scaphoid in its most longitudinal axis and serves to separate it on the x-ray from the shadows of the distal radius.28
Knowledge of normal carpal radiographic anatomy is essential when evaluating the x-ray, particularly on the lateral view. In this view, the distal radius, lunate, and capitate should align along a longitudinal axis. The scapholunate angle is formed by a line bisecting the scaphoid in its longitudinal axis, and a line bisecting the lunate. Any angle less that 40 degrees or more than 60 degrees indicates ligamentous instability and/or fracture.
A significant number of scaphoid fractures are occult and x-rays should be repeated in 10-14 days when fracture lines would be more apparent. Additional imaging studies may be necessary such as MRI, CT scan or a bone scan but are not usually obtained in the ED.
Management. Any scaphoid fracture diagnosed radiographically should be placed in a thumb spica splint with the wrist in slight extension (15-20 degrees). Since many of these fractures do not show up initially on radiographs, any patient with tenderness in the anatomic snuffbox or an exam suspicious for a scaphoid fracture should have a thumb spica splint applied. All children should be referred for follow-up in 10-14 days. It is recommended that the splint be extended to the tip of the thumb and that clinicians ensure the child can pinch the thumb and the index finger. This will secure good immobilization of the scaphoid while allowing function of the hand for children who are in school.
Key Points. Many scaphoid fractures are not evident on initial radiographs and patients with tenderness should be treated as a fracture and given prompt follow-up. Delayed treatment can increase the risk for complications. It also is important to do a good physical exam. Carpal bone fractures frequently are associated with other fractures. A patient may present complaining of distal radius pain from a radius fracture, and an associated scaphoid fracture could be missed if this area is not examined well.
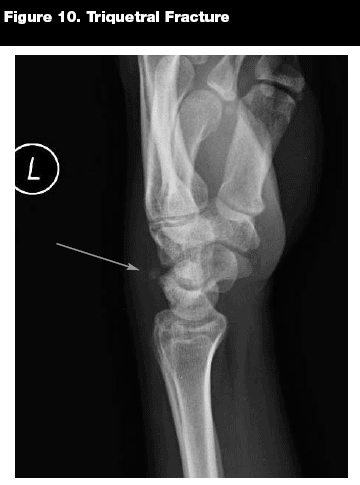
Triquetral Fractures. Epidemiology. Fracture of the triquetrum (see Figure 10) is the second most common carpal bone fracture and is associated with carpal instability.19
 |
Patterns of Injury. The mechanism of injury usually involves either a direct blow to the bone that causes a fracture of the body or a fall on an extended wrist in ulnar deviation, causing impingement of the hamate or the ulnar styloid on the dorsal edge of the triquetrum.19
Evaluation. Patients present with a history of fall or direct blow and pain over the ulnar aspect of the wrist. There usually is point tenderness just distal to the ulnar styloid (triquetral point) or dorsally directly over the triquetrum.5,19 The triquetrum is most easily palpated with the wrist in radial deviation. There may be swelling in this same area, and range of motion may be limited secondary to pain.27
Imaging. A triquetral fracture is best seen on a lateral view of the wrist as a small dorsal chip. A more oblique pronated lateral view may sometimes be required to visualize the fracture.
Management. The wrist should be immobilized with a short arm splint for 3-6 weeks. An athlete can return to play early with a playing splint. Immobilization usually leads to an uncomplicated course.5,19
Key Points. Triquetral fractures are easy to miss, as the only abnormality seen radiographically may be a small chip seen dorsally on the lateral view.
Lunate Fractures. Epidemiology. The incidence of lunate fractures is rare (0.5-6.5%), especially in comparison to the high incidence of scaphoid fractures.23 Risk factors include any repetitive pressure to the base of the hand with the wrist in extension (e.g., gymnastics).30
Pattern of Injury. Most lunate fractures occur as the result of a fall on an extended wrist or some other wrist hyperextension injury. Force applied to the heel of the hand can cause a dorsal lip avulsion fracture of the lunate. With the exception of corner fractures and dorsal or palmar horn fractures, all lunate fractures have a high probability of osteonecrosis.30
Evaluation. Patients typically present complaining of pain in the wrist area that is aggravated by movement of the wrist or by gripping. Tenderness to palpation is usually present on the dorsum of the wrist just distal to Lister's tubercle30 (a bony prominence on the dorsum of the distal radius).
Imaging. AP, lateral, and oblique views of the wrist should be obtained for a suspected lunate fracture. The fracture line is difficult to detect, but when seen will appear as a thin translucent, usually transverse line. The dorsal rim of the radius makes visualization of the fracture difficult on the AP view. Other carpal bones that are superimposed make visualization of the fracture difficult on the lateral view.30 A CT scan or MRI may be required for diagnosis.
Management. The patient should be immobilized in a long arm splint or a double sugar tong splint. All patients with lunate fractures should be referred to an orthopedic surgeon because of the significant potential for nonunion and osteonecrosis.30
Key Points. Lunate fractures, especially those that have a delayed diagnosis and treatment, may lead to osteonecrosis (also known as Kienböck disease).
Lunate and Perilunate Injuries. Epidemiology. Lunate and perilunate dislocations are very rare in children. Both of these injuries have significant morbidity if they are not diagnosed early and treated appropriately. The incidence of scapholunate injuries is becoming more common in children with the increased levels of athletic competition.23
Patterns of Injury. The mechanism of injury is a fall on an outstretched hand that causes hyperextension and ulnar deviation of the wrist.23 This can occur secondary to collisions and contact sports. The protection by the radial articular surfaces causes perilunate dislocations to occur more often than lunate dislocations. In lunate dislocation, the lunate dislocates volarly and the capitate appears to be aligned with the distal portion of the radius.28 In perilunate dislocations, the lunate lines up with the radius and the capitate is dorsally dislocated. Median nerve injury may occur acutely from a contusion to the nerve or may be secondary to swelling or hematoma formation.23
Evaluation. Lunate and perilunate injuries may be subtle and, therefore, are frequently missed. Patients present with a history of a fall on an outstretched hand or a collision type injury such as a motor vehicle or motorcycle collision. The injury also may have occurred while playing contact sports and colliding with another player.5
The patient may complain of pain and swelling either on the volar aspect or the dorsum of the wrist. On physical exam, there may be tenderness to palpation over the dorsum of the wrist with slight deformity and the range of motion may be somewhat limited. Sensation and function of the median nerve should be assessed as well as two-point discrimination in the median nerve territory.23
Imaging. AP and lateral views of the wrist should be obtained (see Figures 11a and 11b). On the AP view, the spaces between the carpal bones should be 1-2 mm and equal. A scapholunate space greater than or equal to 3 mm (Terry Thomas sign) indicates a scapholunate ligamentous injury. The distance in children may be difficult to interpret because of eccentric ossification of the carpal bones.5
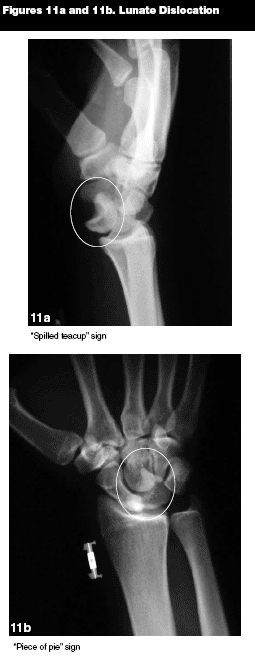 |
On the AP view, the lunate is quadrangular in shape. Dislocation of the lunate results in a triangular shaped lunate (piece of pie sign) (see Figure 11b). On the lateral view, the capitate, lunate, and radius should line up longitudinally, with the capitate resting in the cup of the moon-shaped lunate and the lunate resting in the cup of the radius. In a lunate dislocation, the lunate is rotated in a volar direction and looks like a spilled teacup (see Figure 11a). With a perilunate dislocation, the capitate lies dorsally to the lunate and the lunate lines up with the radius on the lateral view.23
Management. An orthopedic surgeon may be called to assist in closed reduction of the dislocation in the ED. If this is successful, a long arm splint should be applied. If closed reduction is not possible, open reduction with internal fixation (ORIF) is recommended.23
Key Points. Carefully assess the appearance of the lunate on the radiograph; specifically, be aware of the alignment of the radius, lunate, and capitate on the lateral view, and of the appearance of the lunate and scapho-lunate joint on the AP view. Ligamentous disruption can cause significant injury in the absence of a fracture.
Elbow Injuries
Introduction. Pediatric elbow trauma is a common condition seen in the ED. Children, like adults, use their outstretched arms to brace their falls, often resulting in fractures of the elbow.31,32 Sixty-five to 75% of all fractures in the pediatric population occur in the upper extremity.31,32 Supracondylar fractures predominate, accounting for 60% of all elbow fractures.31-33 Diagnosis of elbow fractures can be quite challenging because of several factors specific to pediatrics. Ossification centers of growth appear and fuse at various times of skeletal maturity, and some fractures are very subtle on radiographs.32 In addition, children are limited in their ability to communicate specific complaints and can be difficult to examine in a reliable fashion.32 It is important to understand the normal bony anatomy and sequence of ossification growth centers of the pediatric elbow and apply an organized approach to interpreting radiographs. Along with this, knowing the incidence of the various fractures about the elbow and common mechanisms of injury will improve the emergency physician's (EP) ability to accurately diagnose pediatric elbow fractures.32,34
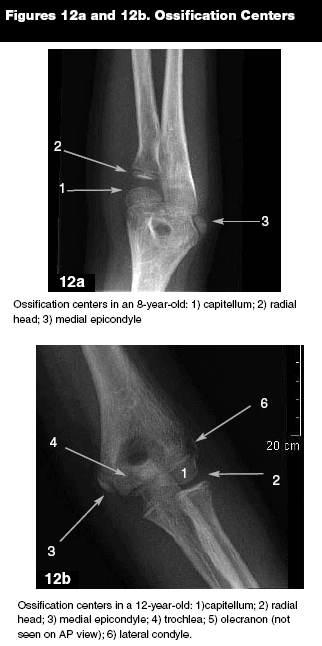
Anatomy. The secondary ossification centers of the elbow become calcified and appear in childhood and fuse to their respective long bones in adolescence.6 Elbow skeletal growth begins with the humerus as a single cartilaginous epiphysis. It differentiates into the capitellum and trochlea (2 epiphyses) and the medial and lateral epicondyles (2 apophyses).6 The 6 growth centers in the distal humerus and proximal radius and ulna appear in a predictable chronological order; however, the age is somewhat variable.31 The capitellum appears between ages 1 and 2 years, followed by the radial head between 2 and 4 years, the medial epicondyle between 4 and 6 years (range, 2-8.5 years) (see Figure 12a), the trochlea between ages 9 and 10 years (range, 5.5-14 years), the olecranon between ages 9 and 11 years, and finally the lateral epicondyle between ages 9.5 and 11.5 years (range, 7-14 years) (see Figure 12b).31 The mnemonic that refers to the 6 ossification centers is CRITOE. (See Table 1.) A way to remember the approximate ages of each center's appearance is counting by odd numbers (1, 3, 5, 7, 9, 11). Ossification centers appear 1-2 years earlier in girls than in boys.31,32
 |
 |
Radiographic Assessment. Standard radiographs of the elbow include AP and lateral views and are sufficient in most cases of elbow injury. Obtain oblique views if a fracture is not evident but suspected. The lateral and medial condyles are better visualized with oblique views.6
Comparison views of the uninjured elbow may help clarify fractures versus secondary ossification centers and normal bony anatomy.6,31,34 As mentioned before, there is some debate as to whether comparison views actually improve diagnostic accuracy. Some studies suggest they do not,34-36 so while routine comparison films on every child are not indicated,35 they remain useful in select cases.
Anterior and Posterior Fat-Pad Signs. Assessment of fat pads around the elbow is essential in interpreting radiographs and is helpful in identifying occult fractures in children. First described in 1954 by Norell, fat pads overlie the anterior and posterior aspects of the joint capsule.32,37 The anterior fat pad is a normal finding on the lateral flexed view (see Figure 13a). If there is a joint effusion and hemarthrosis, however, the fat pad becomes elevated and projects outward, assuming a triangle shape like the sail of a ship (see Figure 13b). The "sail" sign indicates an intra-articular joint effusion with probable associated fracture.6,31
The posterior fat pad is normally hidden in the olecranon fossa on the lateral flexed view (see Figure 13a), and when visualized is always pathognomonic for intra-articular disease (see Figure 13b). Joint trauma displaces the posterior fat pad as blood and marrow accumulate in and expand the joint capsule.32,38 In a skeletally immature child, assume a distal humerus fracture if you see a posterior fat pad.6,31,34 False positives occur when the elbow is in extension.38 Studies have demonstrated the positive predictive value of the posterior fat-pad sign to be greater than 76% for occult pediatric elbow fractures.37,38
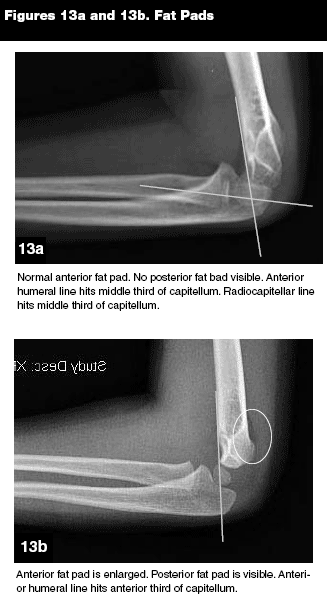 |
Anterior Humeral Line. A line drawn down the anterior humeral cortex on lateral view should intersect the middle third of the capitellum (see Figure 13a). The line may pass through the anterior third of the capitellum in children younger than age 2.5 years because of the small size of the ossification center.31,32
Radiocapitellar Line. A line drawn down the middle of the long axis of the radius should intersect the middle third of the capitellum (see Figure 13a). Unlike the other signs mentioned above, this holds true regardless of the radiographic view or the degree of elbow flexion or extension.32,38
Supracondylar Fractures. Epidemiology. Supracondylar (SC) fractures are the most common pediatric elbow injuries, accounting for 60% of all fractures surrounding the elbow. Most occur in children younger than age 8 years.32
Patterns of Injury. SC fractures usually result from a fall on an outstretched hand (FOOSH), and 95% are extension-type fractures. Anterior displacement fractures are rare and usually result from a flexed arm hitting the ground.34
Evaluation. The classic history in this instance will be a child who falls and tries to break the fall with an outstretched hand. The child will present to the ED holding the arm in pronation and will not move the arm because it hurts. Swelling, ecchymosis, and/or deformity may be present. Point tenderness over the distal humerus may be elicited. The median nerve is most commonly injured, followed by the radial nerve and then the ulnar nerve. Incidence of neurovascular injury in SC fractures is 12% overall, and increases up to 49% as the degree of displacement increases.38 To assess the anterior interosseous branch of the median nerve, have the patient make an "OK" sign and test for strength. Check vascular status by assessing color, pulses, temperature, and capillary refill.
Imaging. Obtain AP and lateral views of the elbow. Perform a systematic analysis of fat pads, anterior humeral and radiocapitellar lines, and ossification centers, and search for fractures. Extension-type fractures are classified by the Gartland system. Type 1 fractures are nondisplaced, type 2 are displaced with an intact posterior cortex, and type 3 are displaced with no cortical contact.32,34 Type 1 fractures may be difficult to visualize; however, the posterior fat pad is almost always present. Anterior humeral line deviation should alert the clinician to a possible SC fracture as well.32
Management. Gartland type 1 fractures (see Figures 14a and 14b) that are minimally displaced can be immobilized in a long-arm posterior splint with the elbow at 90 degrees of flexion for 3 weeks. These fractures are stable and have minimal complications. Outpatient orthopedic follow-up in 7 days is acceptable.33,38
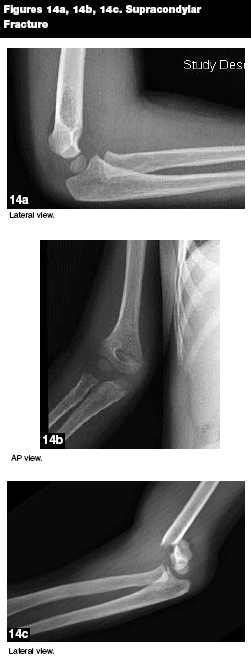 |
Gartland types 2 and 3 fractures (see Figure 14c) should have orthopedic evaluation in the ED as there is a greater risk of neurovascular compromise and they often require reduction with percutaneous pinning.38 The recent literature suggests that delayed intervention in patients without neurovascular deficit does not compromise outcome or result in increased complication rates.33,39
If there is neurovascular compromise and orthopedic consultation is not immediately available, the EP should attempt reduction using traction, counter-traction, and reapproximation techniques. Always assess neurovascular status after manipulation and splint the arm in at least 90 degrees of flexion. The distal pulse may disappear with the degree of flexion often needed to hold the reduction. In that case, gently extend the elbow until the pulse returns.38
Complications of SC fractures include compartment syndrome, which can lead to subsequent Volkmann's ischemic contracture if untreated (fixed elbow flexion, forearm pronation, wrist flexion, metacarpal-phalangeal joint extension, and interphalangeal flexion).38 Cubitus varus or "gunstock" deformity is a long-term complication and may develop despite appropriate treatment.6,38 This is more of a cosmetic issue, however, as functional problems are uncommon.
Key Points. Maintain a high index of suspicion in a child with elbow pain and suitable mechanism of injury. Systematically examine radiographs to find subtle evidence of occult fractures. Test the anterior interosseous nerve by having the child make an "OK" sign. Immediately consult orthopedics for all types 2 and 3 supracondylar fractures. Perform immediate reduction if there is neurovascular compromise.
Lateral Condyle Fractures. Epidemiology. Lateral condyle fractures (see Figure 15) are the second most common pediatric elbow injury, accounting for 10-20% of all fractures around the elbow.31,32 It should be noted that the terms "medial" and "lateral" refer to the anatomic position. The lateral condyle, therefore, is on the radial aspect of the forearm, whereas the medial condyle is on the ulnar aspect.
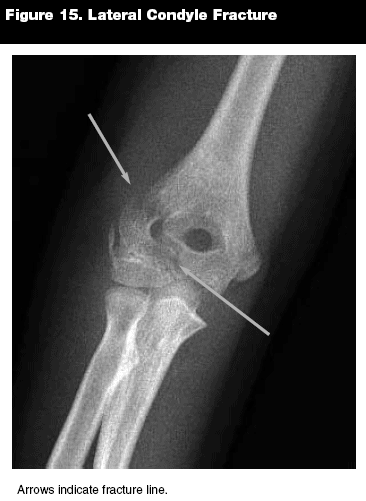 |
Patterns of Injury. Mechanism of injury is a FOOSH, causing a varus stress on an extended elbow with a supinated forearm.32,34
Evaluation. The child will present to the ED with swelling and tenderness that is usually localized to the lateral elbow. Neurovascular injury is not common and the soft tissue injury is not as severe as with SC fractures.6,34
Imaging. Obtain AP and lateral radiographs. An oblique view is beneficial if suspicion is high and the AP and lateral radiographs are normal, as a minimally displaced fracture that doesn't disrupt the joint surface is subtle and often is only demonstrated with this view.32,34
Management. Nondisplaced fractures or those with less than 2 mm displacement are treated with long-arm cast immobilization for 3-4 weeks. Even the non-displaced fractures need orthopedic follow-up and re-evaluation in 1-2 days as they can become displaced and require prompt surgery. Fractures with greater than 2 mm displacement are treated with closed reduction and percutaneous pinning with casting for 3-4 weeks. If there is malrotation, open reduction and internal fixation is required with at least 6 weeks of immobilization. Complications include nonunion, avascular necrosis, cubitus valgus deformity, ulnar nerve palsy, and physeal arrest, and can be minimized by timely diagnosis and treatment.31,34
Key Points. Clinicians should obtain oblique views if a lateral condyle fracture is suspected and a fracture on standard AP and lateral views cannot be visualized. Soft tissue injury is not as severe as that seen with supracondylar fractures, but long-term complications tend to be functional. Fractures with greater than 2 mm of displacement or malrotation will require surgery. Complications can be minimized by timely diagnosis and appropriate treatment.
Medial Epicondyle Fractures. Epidemiology. Medial epicondyle fractures (see Figure 16) account for up to 12% of fractures surrounding the elbow and are most commonly seen in the throwing athlete.6 They tend to occur in children between ages 10 and 14 years.32,34
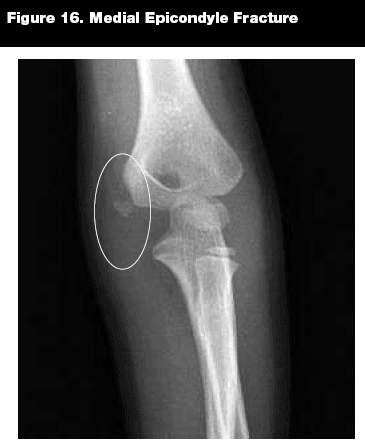 |
Patterns of Injury. This is an acute injury caused by a severe valgus stress on the elbow, such as with repetitive powerful throws by a baseball pitcher.6 The ulnar collateral ligament and the flexor muscles insert at the medial epicondyle. Valgus forces cause traction on the medial epicondyle through the flexor muscles.32
Evaluation. Physical examination may reveal swelling and tenderness over the medial epicondyle, a 10-15 degree flexion contracture, and weakness of the flexor-pronator muscles.6 There usually is limited soft tissue injury. Elbow dislocation occurs in about 50% of cases.32,34 Suspect an associated elbow dislocation if there is significant swelling, gross instability of the elbow joint, or neurovascular compromise.34
Imaging. Obtain AP and lateral radiographs of the elbow. Stress views usually are done only in consultation with orthopedics. Simple medial epicondylar fractures are extra-articular and usually do not display a posterior fat pad sign on lateral view.34 If a posterior fat pad is seen, suspect an additional fracture or concomitant elbow dislocation.
The medial epicondyle (fragment) may become entrapped in the joint after reduction of an elbow dislocation; however, this may be difficult to appreciate on radiographs, especially in children younger than age 10 years in whom it may be mistaken for the trochlea. Suspect entrapment if the medial epicondyle is not plainly seen in anatomical position on radiographs.32,34
Management. Patients with simple medial epicondyle fractures should be splinted in a long arm posterior splint with the arm in 90 degrees of flexion. They may be sent out of the ED with outpatient orthopedic follow-up in 1-2 days for further treatment and physical therapy.
There is controversy regarding the appropriate treatment of displaced medial epicondyle fractures. The literature supports either conservative treatment or surgical fixation for intra-articular loose bodies and displaced fractures.6,34 Fractures displaced greater than 3-5 mm may potentially need surgical fixation;6,31 however, is not clear that this threshold for operative treatment improves outcomes over closed reduction.34 Absolute indications for surgery include a medial epicondyle entrapped in the joint, open fractures, and the presence of ulnar nerve dysfunction.6,31,34
Complications include nonunion, delayed union, valgus instability, cubitus valgus deformity, ulnar nerve palsy, and loss of extension.6
Key Points. Medial epicondyle fractures are more common in the throwing athlete. Elbow dislocation occurs in about 50% of cases. Simple fractures usually do not display a posterior fat pad sign. Suspect epicondyle entrapment if it is not clearly seen on a radiograph. Fractures other than simple ones should prompt a call to an orthopedist.
Radial Head Subluxation (Nursemaid's Elbow). Epidemiology. Radial head subluxation (RHS) is the most common upper extremity injury in children younger than age 6 years who present to the ED.34,40 It is seen most frequently in toddlers and tends to occur more in girls than boys.34
Patterns of Injury. Typical history involves a pull mechanism causing longitudinal traction of the pronated forearm with the elbow in extension. The radial head slips out of the annular ligament, which normally holds it in place, and becomes trapped in the radio-capitellar articulation. The annular ligament is weak in infants and young children. With age, it becomes stronger and the radial head size increases, making RHS uncommon after the age of 7 years.34 The left arm is affected more often, likely due to the fact that most caregivers are right handed.34 Keep in mind that only around 50% of children will have this classic history. A fall has been described in 18-22% of cases.34,41
Evaluation. Classically, the child will present with arm pain but is not in a great deal of distress. The child will not move the arm and holds it in an adducted, semi-flexed and pronated position. Physical examination reveals no significant point tenderness, swelling, or ecchymosis; however, there may be some discomfort at the radial head. The child has pain with any pronation or supination movement.
Imaging. Routine radiographs are not indicated or recommended when there is a high suspicion of RHS. Radiographs will invariably be normal. If reduction attempts are not successful or the history and physical is not typical, radiographs may be helpful to rule out a more significant injury such as a radial head fracture or dislocation or a humerus fracture.34 In one study, the relative risk of fracture in children with an atypical history of mechanism was not high when the child had a classical presentation.41
Management. Two reduction techniques are typically described: the supination/flexion technique and the hyperpronation technique. To perform the supination/flexion technique, the elbow is held with the thumb on the radial head, while the other hand supinates the wrist followed by flexion of the elbow. An audible and palpable click with spontaneous movement of the extremity after several minutes indicates successful reduction. To perform the hyperpronation technique, the elbow is held while the other hand hyperpronates the forearm. Supination/flexion success rates are reported to be up to 92%, while hyperpronation rates are higher at 97.5%, and often successful after supination/pronation fails.6 One study suggested that forced pronation was perceived as less painful than supination/flexion by parents whose children were treated in the ED.42 RHS recurs in about 26.7% of cases.34
Key Points. RHS is commonly seen in the ED and is most often seen in the 1-4 year age group. Classic history includes a pull to the arm and a child who doesn't move the affected arm. Radiographs are not routinely performed if the history is consistent and there are no focal findings on exam. Hyperpronation technique may be more successful and less painful for reduction of RHS.
Conclusion
Pediatric wrist and elbow injuries are commonplace in the ED. While many are easily diagnosed and treated, some have subtle radiographic findings and can lead to functional impairment if not promptly recognized and appropriately treated. With a careful history and physical exam, meticulous examination of radiographs, and an awareness of potential pitfalls, all emergency medicine practitioners should be able to successfully diagnose and optimally treat children with injuries to their wrists and elbows.
References
1. Damore DT, Metzl JD, et al. Patterns in childhood sports injury. Pediatr Emerg Care 2003;19:65-67.
2. Perron AD, Miller M, et al. Orthopedic pitfalls in the emergency department: pediatric growth plate injuries. Am J Emerg Med 2002:20:50-54.
3. McQuillen K. Musculo skeletal disorders. In: Marx JA, Hockberger RS, et al, eds. Rosen's Emergency Medicine. 6th ed. Philadelphia: Mosby; 2006:2689-2692.
4. Iannotti JP. Growth plate physiology and pathology. Orthop Clin North Am 1990;21:1-17.
5. DeLee and Drez's Orthopaedic Sports Medicine. 2nd ed. Philadelphia: Saunders; 2003.
6. Benjamin HJ, Hang BT. Common acute upper extremity injuries in sports. Clin Pediatr Emerg Med 2007;8:15-30.
7. Uptod S, Chorley J. Acute wrist injuries in children and adolescents. Up to Date. 2007. Available at http://www.Uptodate.com.
8. Gill TJ 4th, Micheli LJ. The immature athlete. Common injuries and overuse syndromes of the elbow and wrist. Clin Sports Med 1996;15:401-423.
9. Novelline R. Men, women and children. In: Squire's Fundamentals of Radiology. Massachusetts: Harvard University Press; 1999:448-449.
10. Salter RB, Harris WR. Injuries involving the epiphyseal plate. J Bone Joint Surg Am 1963;45:587-622.
11. Carson S, Woolridge DP, et al. Pediatric upper extremity injuries. Pediatr Clin North Am 2006;53:41-67.
12. Jones E. Skeletal growth and development as related to trauma. In: Green NE, Swiontkowski MF, eds. Skeletal Trauma in Children. Philadelphia: Saunders; 2003.
13. Pershad J, Monroe K, et al. Can clinical parameters predict fractures in acute pediatric wrist injuries? Acad Emerg Med 2000;7:1152-1155.
14. Eilert R. Orthopedics. In: Current Pediatric Diagnosis and Treatment. Williams WH, Levin MJ, et al, eds. McGraw Hill: Philadelphia; 2004:803.
15. Lawton L .Fractures of the radius and ulna. In: Letts RM, ed. Management of Pediatric Fractures. Philadelphia: Churchill Livingstone; 1994.
16. Canale TS. Physeal injuries. In: Campbell's Operative Orthopedics. St Louis: Mosby; 1998:2364-2367.
17. Walsh HP, McLaren C, et al. Galeazzi fractures in children. J Bone Joint Surg Br 1987;69:730-733.
18. Woolfrey K, Eisenhauer MA. Wrist and forearm. In: Marx JA, Hockberger RS, et al, eds. Rosen's Emergency Medicine. 6th ed. Philadelphia: Mosby; 2006:642-643.
19. Yamamoto L, Chung S. Galeazzi's injury: radiology in pediatric emergency medicine. Vol. 1, Case 16. Kapiolani Medical Center For Women And Children, University of Hawaii John A. Burns School of Medicine.
20. McDollough MD. Pediatric radiology: What do you need to know? Emergency Medicine Spring Congress. April 24-26, 2007. San Diego, CA.
21. Monteggia's fracture. In: Wheeless CR, ed. Wheeless' Textbook of Orthopaedics. http://www.wheelessonline.com.
22. Deshpande S, O'Doherty D. Type I Monteggia fracture dislocation associated with ipsilateral distal radial epiphyseal injury. J Orthop Trauma 2001;15:373-375.
23. Menckhoff C, Welter C. Orthopedic pearls and pitfalls. Emergency Medicine Reports 2007;28(16):181-192.
24. Letts M, Locht R. Monteggia fracture-dislocations in children. J Bone Joint Surg Br 1985;67:724-727.
25. Fractures of the carpal bones. In: Letts RM, ed. Management of Pediatric Fractures. Philadelphia: Churchill Livingstone; 1994.
26. Phillips TG, Reibach AM, et al. Diagnosis and management of scaphoid fractures. Am Fam Physician 2004;70:879-884.
27. Inaba A, Boychuk R. A hand contusion: radiology cases in pediatric emergency medicine. Vol. 1, Case 14. Kapiolani Medical Center For Women And Children University of Hawaii John A. Burns School of Medicine.
28. Shearman C, EL-Khoury G. Pitfalls in the radiologic evaluation of extremity trauma: part I the upper extremity. Am Fam Physician 1998;57:995-1002.
29. Saverland E. The upper limb. In: Delly, P ed. Grant's Dissector. Philadelphia: Lippincott Williams and Wilkins; 1999.
30. Burroughs K. Lunate fractures. Up to Date. 2005. Available at http//:www.uptodate.com
31. Lins RE, Simovitch RW, et al. Pediatric elbow trauma. Orthop Clin North Am 1999;30:119-132.
32. Jacoby SM, Herman MJ, et al. Pediatric elbow trauma: an orthopaedic perspective on the importance of radiographic interpretation. Semin Musculoskelet Radiol 2007;11:48-56.
33. Carmichael KD, Joyner K. Quality of reduction versus timing of surgical intervention for pediatric supracondylar humerus fractures. Orthopedics 2006;29:628-632.
34. Skaggs D, Pershad J. Pediatric elbow trauma. Pediatr Emerg Care 1997;13:425-434.
35. Kissoon N, Galpin R, et al. Evaluation of the role of comparison radiographs in the diagnosis of traumatic elbow injuries. J Pediatr Orthop 1995;15:449-453.
36. Chacon D, Kissoon N, et al. Use of comparison radiographs in the diagnosis of traumatic injuries of the elbow. Ann Emerg Med 1992;21:895-899.
37. Skaggs DL, Mirzayan R. The posterior fat pad sign in association with occult fracture of the elbow in children. J Bone Joint Surg Am 1999;81:1429-1433.
38. Wu J, Perron AD, et al. Orthopedic pitfalls in the ED: pediatric supracondylar humerus fractures. Am J Emerg Med 2002;20:544-550.
39. Simanovsky N, Lamdan R, et al. Underreduced supracondylar fracture of the humerus in children: clinical significance at skeletal maturity. J Pediatr Orthop 2007;27:733-738.
40. Macias CG, Bothner J, et al. A comparison of supination/flexion to hyperpronation in the reduction of radial head subluxations. Pediatrics 1998;102(1):e10.
41. Macias CG, Wiebe R, et al. History and radiographic findings associated with clinically suspected radial head subluxations. Pediatr Emerg Care 2000;16:22-25.
42. Green DA, Linares MY, et al. Randomized comparison of pain perception during radial head subluxation reduction using supination-flexion or forced pronation. Pediatr Emerg Care 2006;22:235-238.
Injuries of the wrist and elbow in children are frequently seen in the emergency department (ED), and as children and adolescents are participating in sports in record numbers, the frequency of these injuries is continuing to rise. Sports injuries in children and adolescents are by far the most common cause of musculoskeletal injuries treated in the ED, accounting for 41% of all musculoskeletal injuries.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
