Are Right-sided Leads Needed?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
The ECG in the figure below was obtained from a man in his 50s who presented with new severe chest pain. How would you interpret this tracing? What area(s) of the heart are involved? What is the likely culprit artery?
The underlying rhythm is sinus at a rate of 75-80 beats per minute. Intervals and axis are normal. There is no chamber enlargement. Regarding Q-R-S-T changes:
Narrow but fairly deep Q waves are seen in leads III and aVF. There is also a small and narrow Q wave in lead II, and a tiny Q wave in lead V6. Overall R wave progression across the chest leads is appropriate, although R wave amplitude in lead V2 is a bit taller than expected. There is dramatic ST elevation in each of the inferior leads (leads II, III, aVF) with a check-mark appearance that strongly suggests acute injury. As a subtle finding, there is ST segment coving and slight elevation in lead V1. There is marked reciprocal ST depression in leads I and aVL. Note how the shape of this ST depression in lead aVL is a precise mirror image picture of the ST elevation in lead III. There is at least 4 mm of shelf-like ST depression in lead V2, which surprisingly resolves by lead V3. There is a hint of J-point depression in leads V3-V6.
In a patient with new-onset chest pain, the ECG appearance in the figure is diagnostic of a large acute infero-posterior ST elevation myocardial infarction (STEMI). Additionally, there is almost certainly acute right ventricular involvement. This strongly suggests acute right coronary artery (RCA) occlusion. Even before looking at the ECG, there is a ~85% chance that the culprit artery with acute inferior STEMI will be the RCA, because most patients have a right-dominant circulation. ECG features that further increase the likelihood of the RCA as the culprit artery are: ST elevation in lead III that is greater than in lead II; marked reciprocal ST depression in lead aVL; relatively less (or no) lateral ST elevation, with the amount of ST elevation in lead III more than in V6; and evidence of acute RV involvement, as manifested by ST coving and slight elevation in lead V1 that is gone by lead V2. Normally, with acute posterior infarction, ST segments are depressed in leads V1 and V2, unless there is associated right ventricular infarction that attenuates or completely eliminates this by the ST elevation it produces in right-sided lead V1.
While ST elevation in right-sided leads (especially in lead V4R) clearly is the best indicator of acute right ventricular infarction, occasionally lead V1 on a standard 12-lead tracing is all that is needed to make this diagnosis.
For more information about and further discussion of this case, please visit: http://bit.ly/2zwCCR5.
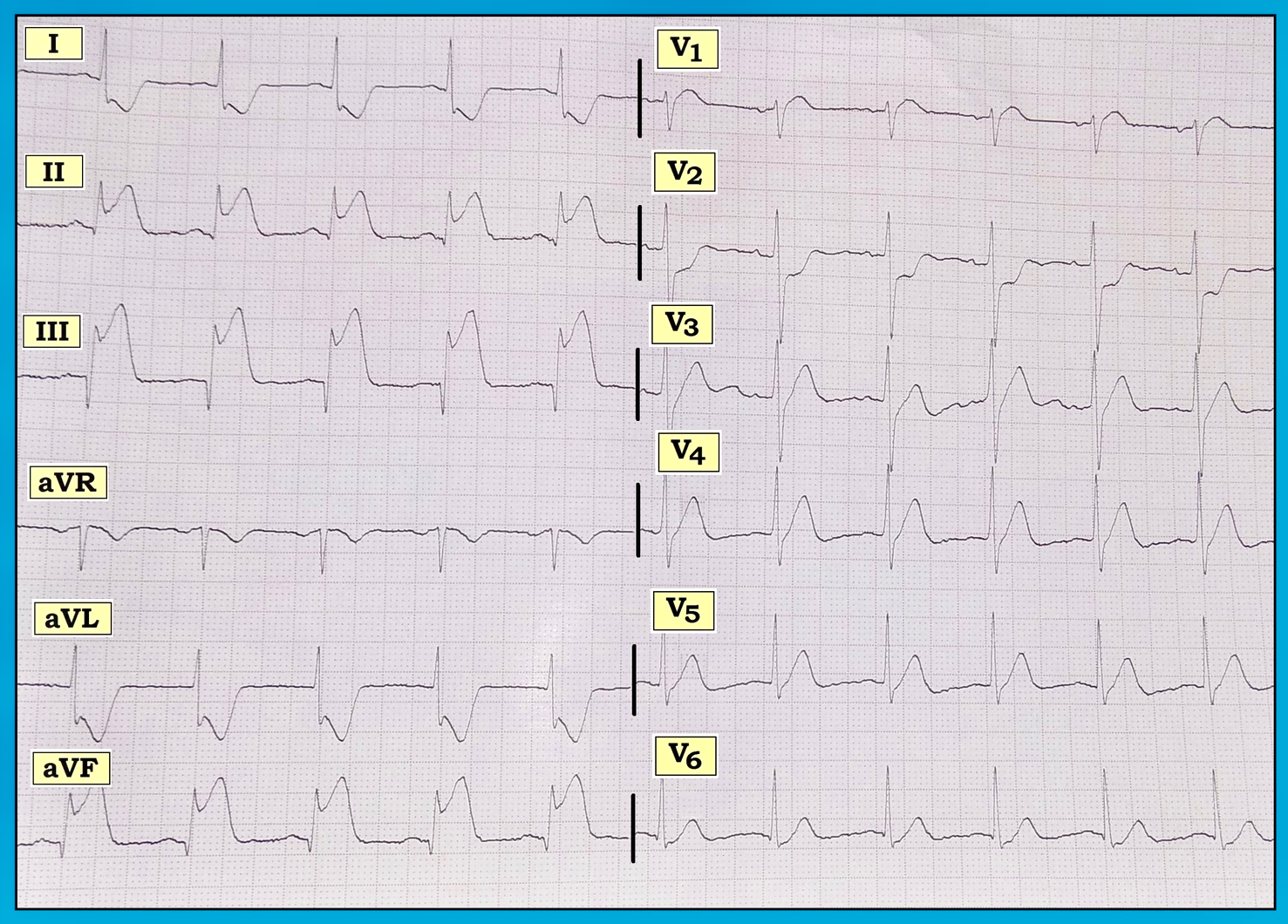
The ECG in the figure was obtained from a man in his 50s who presented with new severe chest pain. How would you interpret this tracing? What area(s) of the heart are involved? What is the likely culprit artery?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
