Approach to Pediatric Eye Discharge and Periorbital Swelling
December 1, 2017
Reprints
AUTHORS
Mahnoosh Nik-Ahd, MD, MPH, Resident, Stanford Pediatrics Residency Program, Stanford, CA
Kim Cooper, MD, Clinical Faculty of Ophthalmology, Lucille Packard Children’s Hospital, Stanford, CA
N. Ewen Wang, MD, Professor of Emergency Medicine, Stanford School of Medicine, Stanford, CA
Andrea Fang, MD, Clinical Assistant Professor of Emergency Medicine, Stanford School of Medicine, Stanford, CA
PEER REVIEWER
Larry B. Mellick, MD, MS, FAAP, FACEP, Professor of Emergency Medicine, Professor of Pediatrics, Augusta University, Augusta, GA
EXECUTIVE SUMMARY
- The initial exam should start with visual inspection of the eye. Pupils should be checked for normal red reflexes. A swinging flashlight test can assess the presence of an afferent pupillary defect. Next, examine the ocular structures from anterior to posterior starting with the eyelids, eyelashes, conjunctiva, cornea, anterior chamber, lens, and optic nerves.
- A distinguishing characteristic of allergic conjunctivitis, compared to infectious conjunctivitis, is that the onset is bilateral and pruritic in nature and that the discharge is clear. Overall, the most effective treatment is removal or avoidance of the offending agent.
- Viral conjunctivitis discharge is more often scant, serous, or mucoid in consistency, whereas the discharge of bacterial conjunctivitis is more purulent in quality. Viral conjunctivitis also frequently starts out unilateral and becomes bilateral within 24 to 48 hours.
- Viral conjunctivitis is a clinical diagnosis. Treatment generally involves supportive care, including cold compresses and artificial tears.
- Herpes simplex virus (HSV) conjunctivitis typically is unilateral with thin, serous drainage, and periocular vesicular lesions may be present on the eyelid. Providers should conduct a slit lamp examination with fluorescein staining to evaluate for dendritic lesions, which are the pathologic hallmarks of HSV conjunctivitis or keratitis.
- There should be a low threshold to refer the patient to an ophthalmologist for further evaluation if one sees classic dendritic lesions, if one notes surrounding skin lesions or vesicles, if the patient has a history of recurrent conjunctivitis (which might in fact be suggestive of reactivation of an HSV ocular infection), or if there is a previous history of herpes infection such as blisters or periocular vesicles.
- Otitis-conjunctivitis syndrome occurs when there is concomitant acute otitis media in the setting of bacterial conjunctivitis. Haemophilus influenzae has been reported as the most common pathogen.
Eye problems, particularly conjunctivitis and periorbital swelling, are very common. The majority are managed easily, but more serious disease processes must be considered. Early recognition and prompt treatment of more serious etiologies, such as gonococcal conjunctivitis and herpes simplex virus, can prevent vision loss.
— Ann M. Dietrich, MD, FAAP, FACEP
In the United States, there were an average of 2.4 million emergency department (ED) visits per year from 2007-2010 for eye-related complaints.1 Across age groups, eye-related visits due to a medical condition (as opposed to ocular trauma) were most common among those aged 18 years or younger, with a prevalence of 63.3 eye-related cases per 10,000 persons.1 This suggests that eye-related complaints are a very common reason for ED visits for children. This article will describe the evaluation and management of two of the most common eye-related medical chief complaints in the pediatric population: eye discharge and periorbital swelling.
This article will discuss two cases — one introduces pediatric eye discharge and the other addresses pediatric periorbital swelling — followed by the clinical presentation, differential diagnosis, and management of the most common causes of pediatric eye discharge and periorbital swelling. The specific population of neonates with conjunctivitis will be addressed.
Eye Anatomy
The eye sits within seven facial bones that make up the orbit and is composed of several structures. (See Figure 1.) Highlights of the anterior portion include the lacrimal gland, tear drainage system, conjunctiva, sclera, cornea, iris, pupil, and lens. Tears are secreted from the lacrimal gland and move across the surface of the cornea to the lacrimal drainage system, at the medial portion of the eye, and drain through the lacrimal sac into the nose. (See Figure 2.) The conjunctiva is the mucosal, epithelial layer covering the anterior portion of the eye and the inner eyelids. The sclera is the white portion of the eye underneath the conjunctiva. The cornea is the clear tissue covering the iris and pupil forming the anterior chamber. At its circumferential edges, the cornea is contiguous with the conjunctiva. The colored iris controls the size of the pupil, the open space in the center of the anterior chamber. Directly behind the pupil is the lens, which can change thickness to focus on near or distant objects. Thus, the cornea, iris, and lens control the sharpness and brightness of our vision, and damage to any of these structures can affect vision.
Figure 1. Anatomy of the Eye |
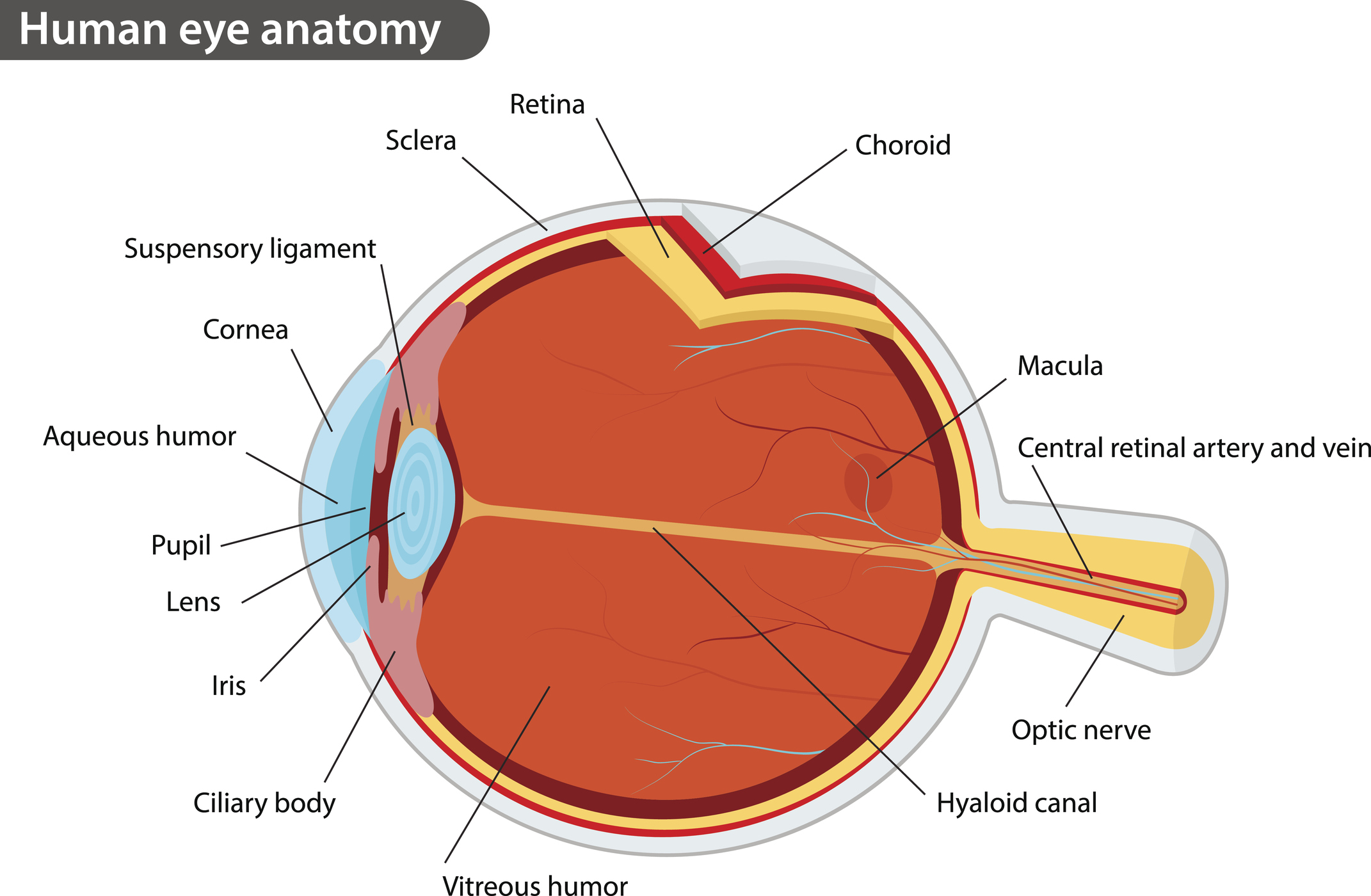 |
|
Source: Getty Images |
Figure 2. Structure of Eye Showing Lacrimal Glands and Lacrimal Drainage System |
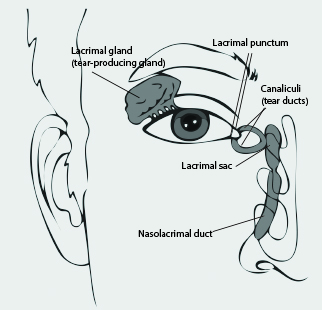 |
|
Source: Getty Images |
Pediatric Eye Exam
Just as there is a systematic approach to examination of other organ systems, such as the heart, there also is a prescribed exam for the eyes. The initial exam should start with visual inspection of the eye. Pupils should be checked for normal red reflexes. A swinging flashlight test can assess the presence of an afferent pupillary defect. Next, examine the ocular structures from anterior to posterior starting with the eyelids, eyelashes, conjunctiva, cornea, anterior chamber, lens, and optic nerves.
If the child can verbalize a change of vision and pain, the ED physician should perform a visual acuity exam and a fluorescein test. Fluorescein is an eye stain that uses an orange dye that helps expose damage to the corneal epithelium. One useful technique to avoid placing the fluorescein dye paper directly onto the child’s eye is to take a saline bullet or syringe and apply several drops of saline to the dye paper and then withdraw the fluorescent solution back into the bullet or syringe. To ensure the solution is not too dilute, have only 1 to 2 mL of solution in the bullet or syringe. One then can apply one to two drops of this solution to each eye and use a cobalt blue light or a Wood’s lamp to visualize fluorescein-stained areas of the eye, which will appear fluorescent yellow-green. Notably, fluorescein stains contact lenses, so it is important to remove these before the fluorescein is applied.
Consider using anesthetic drops to increase patient comfort and cooperation unless there is a history of potential penetrating trauma. Since fluorescein stings, one can use a topical anesthetic prior or to wet the fluorescein strip. In a nonverbal infant, consider whether the child is able to track appropriately. If an infant has sudden-onset fussiness or tearing, a fluorescein test with topical anesthetic should be performed.
For uncooperative infants, the parents should rock or sway the infants to calm them. If they are awake, distraction techniques, such as having the infant use a pacifier or having an aide engage the infant’s tracking with a toy or penlight, may be helpful. Visual screens, such as mobile phones or tablets, also can help distract children and provide them something on which to fixate. Parents also may hold their child or the child may sit on a parent’s lap to ease the comfort level and make the child more cooperative. Some children prefer to be cuddled, so the exam also could be done with the infant looking over the parent’s shoulder.
Case 1: Pediatric Eye Discharge
A 1-year-old boy with no past medical history comes to your ED with two days of increasing discharge from the left eye. He has had a runny nose without fever for the past few days. This morning he woke up with his left eye shut from discharge. He is otherwise nontoxic, is feeding well, and has a normal exam. His vitals are a temperature of 37.6 ° C, heart rate of 106, respiratory rate of 20, and blood pressure of 98/58 mmHg. What is your course of management?
Approach to Pediatric Eye Discharge
History
When evaluating pediatric eye discharge, the history can help discern the difference between infectious and noninfectious causes of eye discharge. Classic questions include the timing of onset, unilateral vs. bilateral nature, and the quality of the discharge. Sick contacts are more suggestive of a contagious, infectious etiology. For older children, ascertain whether there is a change in vision, pain, or the sensation of a foreign body. Also ask about contact lens use, including the wearing and cleaning history. In neonates, it is important to consider sexually transmitted eye infections specifically, and, thus, it is vital to investigate the mother’s past medical history, including if the mother is having any genitourinary symptoms, whether she had prenatal care, and if the baby was born via cesarean or vaginal delivery.
Exam
Key aspects of the exam for children with eye discharge include inspecting the color and quantity of the eye discharge. Does the discharge appear to come from only the medial portion of the eye? Is there any conjunctival injection or redness? If the child is nonverbal, does the infant seem fussy or in pain? During the physical exam, the provider can look for additional signs of upper or lower respiratory infection, such as rhinorrhea, and can examine the ears for evidence of otitis media.
Differential Diagnosis. The differential diagnosis includes acryostenosis, dacryocystitis, conjunctivitis, corneal abrasion, and corneal ulcer. (See Table 1.)
Table 1. Pediatric Eye Discharge: Key Diagnostic Features |
||||
Etiology of Eye Discharge |
Discharge Quality |
Unilateral vs. Bilateral |
Distinguishing Factors |
Disposition |
|
Dacryostenosis |
|
|
|
|
|
Dacryocystitis |
|
|
|
|
|
Allergic Conjunctivitis |
|
|
|
|
|
Viral Conjunctivitis |
|
|
|
|
|
HSV (non-neonatal) Conjunctivitis |
|
|
|
|
|
Bacterial (nonspecific) Conjunctivitis |
|
|
|
|
|
Gonococcal Conjunctivitis |
|
|
|
|
|
Chlamydial Conjunctivitis |
|
|
|
|
|
Corneal Abrasion |
|
|
|
|
|
Corneal Ulcer |
|
|
|
|
Tear Duct Pathology
Dacryostenosis/Nasolacrimal Duct Obstruction
Definition/Etiology. Dacryostenosis is the most common cause of eye discharge and excessive tearing in children younger than 1 year of age and occurs in up to 20% of infants.2 It is defined by a blocked tear duct and is also known as a nasolacrimal duct obstruction. Tears are produced by the lacrimal glands, and the lacrimal drainage system consists of two small openings (i.e., puncti) on the medial surface of the upper and lower eyelid. These openings lead to two canaliculi, which then come together in the common canaliculus, which drains into the lacrimal sac through the nasolacrimal duct into the nose, exiting under the inferior turbinate. (See Figure 2.) This is the reason people get a runny nose when they cry. The pathophysiology of dacryostenosis is a blocked tear duct, generally caused by incomplete canalization of the nasolacrimal duct at the distal end under the turbinate, but it can occur anywhere in the nasolacrimal drainage system. Although this tends to be congenital and presents soon after birth, it sometimes can be associated with infection, as described in the next section on dacryocystitis.
Clinical Features. Dacryostenosis presents as excessive tearing with an increase in discharge with digital pressure over the nasolacrimal sac. It is usually unilateral but can be bilateral. If the obstruction is at the end closer to the tip of the nose (i.e., more distal), the discharge is usually mucopurulent and there is significant matting of the eyelashes. If the obstruction is more proximal, the discharge more often is watery with scant mucopurulence. Although the history tends to be more chronic in nature and the patient is otherwise asymptomatic, tearing often is worse with a concurrent upper respiratory infection, cold air, or wind. Notably, as long as there is no concurrent infection, the conjunctiva should not be red or injected, and this will help distinguish dacryostenosis from the various types of conjunctivitis.3
Diagnosis and Management. Typically, dacryostenosis is a clinical diagnosis. First-line therapy consists of conservative management with massage from the top of the nasolacrimal sac to the bottom. This increased hydrostatic pressure may lead to rupture of the distal membrane. Most cases should resolve by 1 year of age.4 In children younger than 1 year of age, probing with topical anesthesia and papoosing may be done by an ophthalmologist in the office. After 1 year of age, probing usually is performed under general anesthesia, although the timing of probing is somewhat controversial.5 Referral to ophthalmology should be made when conservative management fails by 6 months of age.6 Urgent ophthalmology referral is warranted when a dacryocystocele is suspected. A dacryocystocele is a cyst that occurs when there is simultaneous obstruction of both the proximal and distal portions of the lacrimal drainage system. This should be suspected when there is painless, asymmetric swelling near the medial canthus, leading to upward slanting of the nasal palpebral fissure. A dacryocystocele typically involves a bluish discoloration and can present anytime during the neonatal period and beyond. Dacryocystoceles require urgent ophthalmologic referral because of the high risk of infection and because associated intranasal cysts can cause bilateral nasal obstruction and, subsequently, respiratory distress, especially during feeding, since infants are obligate nose breathers. Prophylactic antibiotic treatment is not necessary unless the eyes become infected, causing dacryocystitis (discussed below). Dacryocystoceles often are the first presentation of dacryocystitis.2 Treatment of dacryocystoceles includes digital massage or probing, either in an ophthalmologist’s office or under general anesthesia, to decompress the obstruction if conservative treatment has failed.5
Dacryocystitis
Definition. Dacryocystitis is defined as an infection of the lacrimal sac and is a clinical diagnosis. It often is caused by bacteria, similar to those that lead to cellulitis, including Staphylococcus aureus, Staphylococcus epidermidis, and alpha-hemolytic Streptococcus.7
Clinical Features. There is usually tenderness of the medial canthal area with significant erythema and edema of the overlying skin, with mucopurulent discharge from the lacrimal sac, which may be distended and palpable. Patients also may have other systemic signs, such as fever, poor feeding, and irritability. In neonates and infants, dacryocystitis may be associated with a dacryocystocele and can be rapid and progressive, evolving into a lacrimal abscess, which can form a fistula and drain externally. Left untreated, dacryocystitis can progress further and evolve to preseptal cellulitis, orbital cellulitis, orbital abscess, and, in rare cases, meningitis.7
Diagnosis and Management. Often, dacryocystitis is a clinical diagnosis. If the patient appears nontoxic and the dacryocystitis seems mild in nature, it can be treated with oral antibiotics with good staphylococcal and streptococcal coverage, such as oral amoxicillin-clavulanate or cephalexin, with urgent ophthalmology follow-up. However, neonates, toxic patients, and severe infections should receive a sepsis workup, including blood cultures and intravenous (IV) antibiotics, such as third-generation cephalosporins with clindamycin or vancomycin. Neonates also may warrant a lumbar puncture. Urgent ophthalmology consultation is recommended, as some cases will require surgical intervention. Imaging is not recommended routinely.7
Conjunctivitis
Definition. Conjunctivitis is defined as inflammation of the mucosal, epithelial membrane lining, both the surface of the globe up to the border where the sclera meets the cornea (also known as the limbus) as well as the inner surface of the eyelids. It is more common in children and comprises 30% of eye-related ED visits.8 Conjunctivitis commonly is separated into allergic, viral, and bacterial etiologies. Upon ED presentation, it is difficult to differentiate the etiologies, especially viral and bacterial conjunctivitis. All patients with conjunctivitis should be considered highly contagious before the etiology has been determined. Gloves should be worn for all examinations, and all equipment should be wiped clean with the appropriate cleaning solutions after the exam.
Clinical Features. At baseline, the conjunctiva is transparent. In conjunctivitis, the eye appears red or pink and often includes discharge. When examined closely, fine blood vessels can be seen, and this appearance is distinct from that in a subconjunctival hemorrhage, which is denoted by extravasated blood. In general, both bacterial and viral types of conjunctivitis are extremely contagious, as transmission occurs via direct patient contact or contact with the patient’s secretions or fomites.9 Day care centers, schools, and family members frequently are affected.
Allergic Conjunctivitis
Etiology. Patients with allergic conjunctivitis have an increased number of mast cells on their conjunctiva compared to the normal population and can be prone to other allergic conditions as well.10 The eye is not immune privileged, and when the eye initially is exposed to an allergen, this activates antigen-presenting cells and leads to antibody production via an immunological cascade. Once the patient has a repeat exposure to the allergen, this leads to the release of preformed inflammatory mediators, causing an inflamed conjunctiva with dilated and tortuous vessels. Various pollens, animal dander, dust mites, and other environmental antigens are said to be some of the most common allergens that cause allergic conjunctivitis.11 Among the general population, 90% of all allergic conjunctivitis in the United States is reported to be secondary to seasonal allergies.12
Clinical Features. The most common symptoms of allergic conjunctivitis are itching, tearing, burning or foreign body sensation, and occasionally mild photophobia. Signs include watery discharge, lid swelling, conjunctival erythema, and edema, which can become severe chemosis. A distinguishing characteristic of allergic conjunctivitis, compared to infectious conjunctivitis, is that the onset is bilateral and pruritic in nature and that the discharge is clear.13
Diagnosis and Management. Allergic conjunctivitis is a clinical diagnosis. Although best practice guidelines currently do not exist for allergic conjunctivitis, in pediatric patients the treatment is supportive care. (See Table 2.) Overall, the most effective treatment is removal or avoidance of the offending agent. Cool compresses and use of artificial tears or saline solution to dilute and remove the offending agent also are treatment options.13,14 A recent Cochrane review suggests that when compared with placebo, topical antihistamines and mast cell stabilizers alleviate the signs and symptoms associated with allergic conjunctivitis in the short term, but data on long-term efficacy are lacking.15 Topical nonsteroidal anti-inflammatory drugs and low-dose steroids also are treatment options,13 but we would defer using these to an ophthalmologist. Allergic conjunctivitis generally can be followed up by a primary care provider.
Table 2. Pediatric Conjunctivitis Treatment Summary |
||
Type of Conjunctivitis |
Suggested Treatment |
Suggested Duration of Treatment |
|
Allergic9,13 |
|
|
|
Viral13 |
|
|
|
HSV (non-neonatal)9,25,26,39 |
AND
|
|
|
Bacterial (nonspecific)9,13 |
|
|
|
Gonococcal |
AND
AND
|
|
|
Chlamydial (non-neonatal)9 |
AND
AND
|
|
Viral Conjunctivitis
Etiology. Viral conjunctivitis is the most common type of conjunctivitis.13 It is caused most commonly by adenovirus, and several distinct serotypes have been suggested.16,17
Clinical Features. Viral conjunctivitis can occur independently, but often it is just one component of a constellation of viral syndrome findings, which may include fever, pharyngitis, upper respiratory infection findings, and lymphadenopathy. Initially unilateral, evolving to bilateral, conjunctival injection, mild to moderate discharge, and early morning crusting all can be seen.18 Viral conjunctivitis discharge is more often scant, serous, or mucoid in consistency, whereas the discharge of bacterial conjunctivitis is more purulent in quality. Viral conjunctivitis also frequently starts out unilateral and becomes bilateral within 24 to 48 hours. Most viral conjunctivitis is contagious before the patient shows any symptoms. The contagious period may last three to five days after symptoms appear. The average duration of viral conjunctivitis symptoms caused by adenovirus is reported to be two to three weeks.19 Further distinguishing characteristics between viral vs. bacterial conjunctivitis are discussed below.
Diagnosis and Management. Viral conjunctivitis is a clinical diagnosis. Treatment generally involves supportive care, including cold compresses and artificial tears. (See Table 2.) Most viral conjunctivitis is extremely contagious. Good eye and hand hygiene are essential to preventing disease transmission. Secondary infection leading to bacterial conjunctivitis is rare, but if suspected, due to symptoms of discharge or matting of the eyelids, topical antibiotics are a reasonable treatment plan. (See Table 2.) In addition, because it can be difficult to distinguish between viral and bacterial conjunctivitis at times, and because many day care centers will not take children with even viral conjunctivitis, treatment with a topical antibiotic is a reasonable management plan if it is required for return to day care. (See Table 2.) Uncomplicated viral conjunctivitis can be followed up by a primary care provider.
Special Consideration: Herpes Simplex Virus Conjunctivitis and Herpes Simplex Virus Keratitis
A much less common cause of viral conjunctivitis is herpes simplex virus (HSV), which constitutes 1.3-4.8% of all cases of conjunctivitis.13 HSV keratitis is an active corneal infection and is classified by the layer of the cornea involved, that is the epithelium, stroma, or endothelium. HSV keratitis can be caused by a direct viral infection or an immune response.20 HSV ocular infections are significant because if untreated they can lead to corneal blindness. Neonatal HSV conjunctivitis is discussed below.
Clinical Features. HSV conjunctivitis typically is unilateral with thin, serous drainage, and periocular vesicular lesions may be present on the eyelid.13 Vesicular or crusted lesions near the eye with even mild conjunctival injection should raise the index of suspicion for HSV conjunctivitis. Providers should conduct a slit lamp examination with fluorescein staining to evaluate for dendritic lesions, which are the pathognomonic hallmarks of HSV conjunctivitis or keratitis.
HSV keratitis can have various presentations depending on the type. Epithelial HSV keratitis more classically will have dendritic lesions or the cornea may stain more diffusely with fluorescein. In the various forms of HSV keratitis, the provider also may note keratic precipitates, infiltrates, ulcers, corneal edema, or anterior chamber inflammation.20 However, it may take the trained eye of an ophthalmologist to truly see these and differentiate between the various forms of HSV keratitis.
The decision to perform a fluorescein exam because of concern for HSV should be based on whether there are surrounding vesicular periorbital lesions suggestive of a herpes simplex infection or if the patient notes blurry vision, pain, and/or the sensation of a foreign body.9 A fluorescein exam also should be performed on all nonverbal infants or children who have increased fussiness.
Diagnosis and Management. HSV conjunctivitis and keratitis often are clinical diagnoses but can be confirmed with a viral culture, direct fluorescent antibody (DFA) test, or polymerase chain reaction (PCR) of surrounding vesicles or conjunctival discharge. Urgent consultation with ophthalmology is recommended for further evaluation, given the risk of corneal blindness. In addition, should a patient have a confirmed diagnosis of an HSV ocular infection, parents should be educated to see their ophthalmologist, not their primary care physician, with any future episodes of “pink eye” to rule out HSV keratitis.
An ocular HSV infection often is mistaken for common conjunctivitis because it is a self-limited disease, and, subsequently, few patients realize they have had a primary herpes infection. Thus, there should be a low threshold to refer the patient to an ophthalmologist for further evaluation if one sees classic dendritic lesions, if one notes surrounding skin lesions or vesicles, if the patient has a history of recurrent conjunctivitis (which in fact might be suggestive of reactivation of an HSV ocular infection), or if there is a previous history of herpes infection such as blisters or periocular vesicles.
HSV conjunctivitis or keratitis should be treated with both topical and systemic antivirals, such as acyclovir or valacyclovir, given the difficulty in dosing frequent antiviral drops in children.9 (See Table 2.) Normal renal function should be confirmed prior to dosing oral antiviral medications. Parents should be cautioned to keep patients hydrated to prevent acute kidney injury. HSV epithelial keratitis may need surgical debridement, while HSV stromal keratitis also may be managed with additional topical steroids.21 However, the decision on management should be deferred to the ophthalmologist. HSV conjunctivitis and keratitis both should have urgent follow-up with an ophthalmologist comfortable examining children.
Bacterial Conjunctivitis
Etiology. The most common causes of bacterial conjunctivitis are S. aureus, S. epidermidis, Streptococcus pneumoniae, Moraxella catarrhalis, Pseudomonas aeruginosa, and Haemophilus influenzae. As vaccination against Haemophilus has increased, incidence of conjunctivitis due to H. influenzae has decreased.18
Clinical Features. Bacterial conjunctivitis involves unilateral or bilateral conjunctival injection, mild to moderate discharge that generally is more purulent, and early morning crusting.18 A Dutch cohort study including 177 adults suggested that the most predictive factor in making a diagnosis of bacterial conjunctivitis, confirmed by positive bacterial cultures, is whether the patient wakes up with bilateral gluing of the eyes.22,23 The hyperemia of bacterial conjunctivitis is said to be more severe than that of viral conjunctivitis, such that the vessels of the inner eyelids may be obscured. Bacterial conjunctivitis also has been noted to be more common in the winter and spring months.23 Another entity associated with bacterial conjunctivitis is otitis-conjunctivitis syndrome. This occurs when there is a concomitant acute otitis media in the setting of bacterial conjunctivitis. H. influenzae has been reported as the most common pathogen.24
Diagnosis and Management. Bacterial conjunctivitis is a clinical diagnosis based on history and symptoms. Most cases are treated empirically initially. Topical antibiotics commonly used include trimethoprim-polymyxin B, erythromycin, and tobramycin. (See Table 2.) The majority of cases of bacterial conjunctivitis are self-limited and are said to last one to two weeks.13 However, antibiotics are said to shorten the course of illness.18 If there is a concomitant acute otitis media consistent with otitis-conjunctivitis syndrome, treating the acute otitis media with oral antibiotics in addition to topical antibiotics for the conjunctivitis is recommended. The provider should continue to emphasize hand hygiene to prevent disease transmission.13 Bacterial conjunctivitis follow-up can be performed by a primary care provider.
Contact lens wearers, especially those noncompliant with wearing and cleaning regimens, are at increased risk for corneal ulcers, which can threaten vision. These patients should be instructed to remove their contacts and only wear their glasses. Topical fluoroquinolones are used in contact lens wearers for Pseudomonas coverage. All contact lens patients with conjunctivitis should receive urgent ophthalmology follow-up.
Gonococcal Conjunctivitis
Clinical Features. Gonococcal conjunctivitis presents with extremely copious, purulent discharge. Although sexually active patients or their partners also may demonstrate symptoms, such as urethral or vaginal discharge, conjunctivitis may be the only presentation of a gonococcal infection. Neonatal gonococcal conjunctivitis is discussed further below.
Diagnosis and Management. Gonococcal conjunctivitis is an ophthalmologic emergency because of the risk of corneal involvement with possible perforation and associated vision loss.18 A Gram stain and culture of the discharge can be used to confirm the diagnosis of Neisseria gonorrhoeae. Neisseria requires systemic treatment with a single dose of ceftriaxone in conjunction with either erythromycin or azithromycin for empiric treatment of chlamydia.9 (See Table 2.) Hourly saline lavages often are necessary initially in gonococcal conjunctivitis to remove debris, and patients must be seen daily by an ophthalmologist.18 Pediatric patients should be admitted for cultures, IV antibiotics, and hourly lavage. Topical antibiotics can be considered in conjunction with consultation with the infectious disease (ID) service. The parents of infected infants also should be tested and treated. In sexually active patients, partners should be informed of their risk of infection. In non-sexually active patients who are not neonates, Child Protective Services should be consulted for concerns of sexual abuse.
Chlamydial Conjunctivitis
Clinical Features. Chlamydia has been associated with 1.8-5.6% of acute conjunctivitis.13 There is usually mild discharge and erythema of the conjunctiva. This may be difficult to distinguish from other bacterial conjunctivitis, especially since it is less prevalent. One should have a higher clinical suspicion for chlamydia conjunctivitis when there is a lack of symptom resolution for presumed and treated bacterial conjunctivitis or after inquiries of sexual activity imply genitourinary or oral symptoms suggestive of a concomitant chlamydial infection. However, patients can have isolated eye symptoms in the absence of genitourinary symptoms.
Diagnosis and Management. Chlamydia conjunctivitis requires urgent referral to ophthalmology because of risk of corneal scarring and vision impairment.18 Diagnosis can be confirmed via cultures, DFA testing, enzyme-linked immunosorbent assay (ELISA), or PCR testing of ocular and genital samples, if available. Chlamydia conjunctivitis also requires systemic treatment with erythromycin, azithromycin, or doxycycline. Topical treatment is optional and consists of erythromycin ointment, although it has not been shown to improve outcomes.9 The patient also should be treated with ceftriaxone for empiric coverage of N. gonorrhoeae. (See Table 2.) As with gonococcal conjunctivitis, sexual partners should be informed of their risk of infection, and Child Protective Services should be involved in patients who are not sexually active.
Special Considerations for Neonatal Conjunctivitis
Definition/Etiology. Neonatal conjunctivitis (also known as ophthalmia neonatorum) is defined as conjunctivitis occurring in the first month of life. Although prenatal screening of mothers and prophylactic erythromycin at birth have been implemented as standard of care to prevent ophthalmia neonatorum, it is not always successful. Cultures of disease-causing entities should be obtained in all cases of neonatal conjunctivitis, and all patients should be admitted. Neonatal conjunctivitis most commonly is caused by normal skin flora. However, gonorrhea, chlamydia, and HSV are causes that must be considered. They are acquired mostly during vaginal delivery but also can be associated with prolonged rupture of membranes. Neonatal conjunctivitis caused by gonorrhea vs. chlamydia can be distinguished by the age of onset and associated discharge, as discussed below and in Table 3. HSV usually will have the classic dendrite pattern on fluorescein exam. Neonates will not necessarily have other systemic signs, and those who require a full sepsis workup will be discussed below.9 Treatment for neonatal conjunctivitis is summarized in Table 4.
Table 3. Neonatal Conjunctivitis: Key Features |
||||
Etiology of Eye Discharge |
Discharge Quality |
Unilateral vs. Bilateral |
Distinguishing Factors |
Disposition |
|
Gonococcal Neonatal Conjunctivitis |
|
|
|
|
|
Chlamydial Neonatal Conjunctivitis |
|
|
|
|
|
HSV Neonatal Conjunctivitis |
|
|
|
|
Table 4. Neonatal Conjunctivitis Treatment Summary |
||
Type of Conjunctivitis |
Suggested Treatment |
Suggested Duration of Treatment |
|
Gonococcal Neonatal9 |
AND
|
|
|
Chlamydial Neonatal9,41 |
AND
|
|
|
HSV Neonatal9,26 |
AND
|
|
Gonococcal Neonatal Conjunctivitis
Clinical Presentation. This typically presents on day 2 to 4 of life and is characterized by severe, purulent discharge.18 Patients typically are born via vaginal delivery, but also may be at risk if there was prolonged rupture of membranes. Inquiries into the mother’s prenatal history and current genitourinary symptoms also should be made.
Diagnosis and Management. Ophthalmology should be consulted emergently, and the patient should be admitted for IV antibiotics and hourly lavage. Again, topical antibiotics can be considered in conjunction with consultation with ID. Although a full sepsis workup is not necessary in localized neonatal gonococcal conjunctivitis, any suggestions of sepsis, meningitis, or arthritis warrant further diagnostic testing, including blood and cerebral spinal fluid cultures and appropriate treatment. Neonatal gonococcal conjunctivitis is considered an ophthalmologic emergency because of the risk of corneal perforation and blindness. Primary systemic treatment with ceftriaxone or cefotaxime is recommended.9,18 We also recommend empiric treatment for chlamydial conjunctivitis.
Chlamydial Neonatal Conjunctivitis
Clinical Presentation. This usually presents on day 5 to 14 of life and is characterized by minimal mucoid discharge.18
Diagnosis and Management. These cases require admission until a diagnosis of chlamydial neonatal conjunctivitis is confirmed, and patients should be evaluated by ophthalmology during their admission. Testing can be confirmed via cultures, DFA, ELISA, or PCR testing. Neonatal chlamydia conjunctivitis is managed with erythromycin for 14 days or azithromycin for three days, although erythromycin is the first-line treatment. (See Table 4.) Data have not shown that the addition of topical therapy adds significant benefit.9 Empiric treatment for gonorrheal conjunctivitis with a single dose of ceftriaxone also is recommended.
HSV Neonatal Conjunctivitis
Clinical Presentation. Neonates also may contract HSV from their mother via vertical transmission and would present with an inflamed conjunctiva and possibly dendrites on fluorescein examination. The quantity of discharge may be less than that expected with chlamydia. The baby also should be inspected for any skin or mouth lesions, since these can be associated with HSV conjunctivitis.9
Diagnosis and Management. Neonatal HSV conjunctivitis warrants admission with urgent ophthalmologic consult and a full sepsis workup including lumbar puncture. Viral cultures and PCR studies can be obtained. DFA and enzyme immunoassays also may confirm diagnosis. Viral studies can be gathered from conjunctiva and any active or weeping lesions. Patients should be treated with intravenous acyclovir25 as well as topical antiviral ophthalmic solutions, such as trifluridine, iododeoxyuridine, or ganciclovir.26 (See Table 4.) Treatment should begin immediately before any viral culture results are confirmed.
Corneal Abrasion
Clinical Features. Corneal abrasions typically present with clear discharge or tearing of the eye. Depending on the patient’s age, there may be eye pain ranging from a mild foreign body sensation of the eye to severe eye pain and discomfort with blinking. Photophobia is very common. Contact lens wearers who present with eye discomfort and/or discharge should raise the index of suspicion for a corneal abrasion or ulcer. Prolonged use of contacts, noncompliant wearing schedules, and poor cleaning techniques can lead to corneal abrasions, ulcers, and possibly subsequent vision loss. In infants, sometimes the first indication of a corneal abrasion is inconsolable crying, and in the absence of an obvious, more serious etiology, corneal abrasion should be considered, especially if it is sudden in onset with eye tearing, redness, and/or periorbital erythema.
Diagnosis and Management. Diagnosis is made via fluorescein staining, which will allow the provider to see a notable abrasion via fluorescein uptake. In addition to clear discharge, the exam also may be notable for periorbital erythema. If the patient is cooperative, a slit lamp exam may confirm the diagnosis. It is important to evert the eyelid to rule out a foreign body that may be causing the abrasion. If an epithelial defect with corneal infiltrates or a crater-like lesion is noted, this is concerning for a corneal ulcer.
Corneal abrasions require urgent follow-up with a primary care physician, ideally the next day to ensure the abrasion has healed. Treatment depends on the etiology of the abrasion. Simple abrasions can be treated with erythromycin ointment or trimethoprim-polymyxin B drops. (See Table 5.) In general, antibiotics are used to prevent infection and promote healing. The patient’s needs should be considered in choosing between drops vs. an ointment. Ointments tend to blur vision, but also provide better lubrication between the injury and the eyelid. Avoid steroids as they can delay epithelial healing and place the patient at higher risk of infection.27,28
Table 5. Pediatric Corneal Abrasion Treatment Summary |
||
Etiology of Abrasion |
Suggested Antimicrobials |
Suggested Duration of Treatment |
|
Simple Abrasion27,28 |
|
|
|
Contact Lens, Fingernails, or Vegetable Matter27,28 |
|
|
|
Corneal Ulcer |
|
|
Contact lens users are at risk for Pseudomonas infections, and abrasions associated with contact lenses, fingernails, or vegetable matter should be treated with a topical fluoroquinolone, such as ciprofloxacin or ofloxacin.27 Contact lens users with a corneal abrasion should be seen by an ophthalmologist the next day. If it is unclear whether the contact lens-using patient has an associated corneal ulcer vs. a corneal abrasion, then he or she should be seen by an ophthalmologist on the same day of presentation. In general, patients with corneal ulcers should be started on a topical fluoroquinolone and be seen urgently by an ophthalmologist.
Case 1 Conclusion
Upon examination, the patient appeared well, non-fussy, and the discharge appeared diffusely along his eyelashes. Given his concomitant upper respiratory infection symptoms and history of his eye being shut in the morning, his presentation was suggestive of bacterial conjunctivitis. He subsequently was started on topical erythromycin. His symptoms resolved over the following days and he was able to return to day care.
Case 2: Pediatric Eyelid Swelling
A 15-year-old female with no significant past medical history comes to the ED with three days of redness around the eye. She has had a mild cough and nasal congestion without fever for more than a week, and now has developed worsening pain with movement of her eye. She has no other visual symptoms and is otherwise nontoxic. Her exam is notable for subtle proptosis and decreased visual acuity. Her vitals are a temperature of 37.4 ° C, heart rate of 84, respiratory rate of 16, and blood pressure of 116/78 mmHg. What is the differential diagnosis and course of management?
History
When evaluating pediatric eyelid swelling, it is important to pay attention to the timing of symptoms and other associated signs or symptoms, including fever or other systemic signs, trauma, insect bites, discharge, pain or an irritated sensation, visual symptoms, and history of preceding facial cellulitis, sinusitis, seborrheic dermatitis, eczema, or acne. Relevant past medical history also would include inquiring about whether the patient is diabetic or immunosuppressed.
Exam
The initial exam should begin with examination of the face and eyes, paying attention particularly to the location of the swelling. Is it confined to one eyelid? Does it affect only the upper or lower lids? Is it more localized to the eyelid margins near the eyelashes? The general appearance of the eye is also important. Is a stye visible? Are there signs of trauma, an abrasion, an insect bite, or a puncture wound? An assessment of extraocular movement also is vital. Proptosis can be assessed by looking down the patient’s nose from above the patient’s head. True proptosis with forward displacement of the eye may be difficult to distinguish from severe lid swelling. Finally, consider a fluorescein stain to rule out a foreign body if symptoms are suggestive of one.
Differential Diagnosis. The differential diagnosis includes blepharitis, hordeolum, preseptal cellulitis, orbital cellulitis, corneal abrasion, allergic reaction, and insect bite reaction. (See Table 6.)
Table 6. Pediatric Periorbital Swelling Features |
|||
Etiology of Periorbital Edema |
Distinguishing Factors |
Can Be Associated With |
Disposition |
|
Blepharitis |
|
|
|
|
Hordeolum |
|
|
|
|
Preseptal Cellulitis |
|
|
|
|
Orbital Cellulitis |
|
|
|
Blepharitis/Meibomitis
Definition. Blepharitis is a chronic eye condition, and patients with seborrheic dermatitis, eczema, or dry eye are at higher riskof developing blepharitis. It is defined as inflammation or infection of the eyelids secondary to dry skin and associated bacterial overgrowth on the eyelashes. Meibomitis is an inflammation of the oil-producing meibomian glands of the eye.
Clinical Features. Patients generally present with swelling and redness of the eyelid. They also may have a red eye, crusted eyelashes upon awakening, tearing, loss of eyelashes, or a foreign body sensation. (See Table 6.) Moderate or severe pain should prompt consideration of corneal involvement, which can make blepharitis, which typically is a benign condition, a more serious one.29
Diagnosis and Management. Blepharitis is a clinical diagnosis. Eyelid hygiene with regular and consistent warm compresses is the mainstay of treatment. Patients with more severe blepharitis who do not respond to eyelid hygiene can be initiated on antibiotic therapy with topical bacitracin or erythromycin ointment for one to two weeks. (See Table 7.) If patients do not respond to topical antibiotic therapy or if corneal involvement is suspected because of significant or persistent pain, the patients should be evaluated by an ophthalmologist. Some of these patients may benefit from oral antibiotics and/or topical cyclosporine, which should be initiated and managed by an ophthalmologist.29 Chronic blepharitis can be treated with azithromycin, doxycycline, or minocycline, although these treatments have not been proven to show benefit and, as previously stated, use should be deferred to the ophthalmologist.30 In addition, tetracyclines, such as doxycycline and minocycline, should be not be used in children younger than 8 years of age, as they carry the risk of tooth discoloration.
Table 7. Pediatric Periorbital Edema Treatment Summary |
||
Etiology of Periorbital Edema |
Suggested Treatment and Antimicrobials |
Suggested Duration of Treatment |
|
Blepharitis29 |
|
|
|
Hordeolum31 |
|
|
|
Preseptal Cellulitis32,36,37 |
|
|
|
Orbital Cellulitis32 |
AND Clindamycin IV, or Vancomycin IV |
|
Hordeolum
Clinical Features. Hordeolum, or a stye, represents inflammation of the eyelid margin that presents as an acute onset furuncle that is painful, erythematous, and swollen. (See Table 6.) The most common infectious cause of a hordeolum is S. aureus, and when caused by infection, the severity of the infection is reported to be directly correlated to the size of the swelling.31
A hordeolum can be either external or internal. An external hordeolum is caused by infection or inflammation of the glands of Zeis or eyelash follicles, whereas an internal hordeolum is caused by infection or inflammation of the meibomian glands.
Diagnosis and Management. Hordeolum is a clinical diagnosis. Treatment for both external and internal hordeola generally is conservative and consists of warm compresses several times a day. (See Table 7.) Over-the-counter lid scrubs and topical antibiotics can be considered. Oral antibiotics for coverage of S. aureus are recommended only if there is concern for simultaneous preseptal cellulitis (discussed below). Follow-up for a hordeolum can be performed by a primary care provider, but if a lesion is resistant to conservative management after one to two weeks, then nonurgent referral to an ophthalmologist is recommended, as the lesion may require incision and curettage. In pediatric patients, this procedure may require general anesthesia.31
Preseptal (Periorbital) Cellulitis
Definition/Etiology. Preseptal cellulitis is an infection usually limited to the soft tissue anterior to the orbital septum and does not involve the orbit itself. Preseptal cellulitis is three times more prevalent than orbital cellulitis and usually does not warrant aggressive treatment like orbital cellulitis.32 Preseptal cellulitis most commonly is caused by a soft tissue infection from Staphylococcus and Streptococcus pathogens, most commonly from S. aureus with methicillin-resistant S. aureus (MRSA) becoming more prevalent.32,33 Other causes of preseptal cellulitis include trauma, an insect bite, previous ocular surgery, and sinus or dental disease. In children younger than 3 years of age who present with systemic signs and rapidly progressive eyelid edema in the setting of a recent viral upper respiratory infection, consider direct spread from sinusitis or hematogenous spread with preseptal seeding and orbital cellulitis.32 It is essential to differentiate preseptal cellulitis from orbital cellulitis, an ophthalmologic emergency, which is discussed below.
Clinical Features. Signs of preseptal cellulitis include unilateral periorbital erythema, edema, warmth, and tenderness.32 (See Figure 3.) Fever may or may not be present on initial presentation. Preseptal cellulitis may be associated with an insect bite, dental infection, or sinusitis. Consider impetigo in the presence of honey crusted lesions.
Figure 3. Preseptal (Periorbital) Cellulitis |
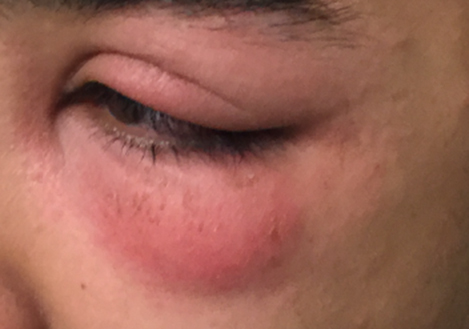 |
|
Image courtesy of Andrea Fang, MD |
Diagnosis and Management. Preseptal cellulitis typically is a clinical diagnosis. Warm compresses can be used to physically promote drainage. There is said to be no difference in efficacy of treatment with IV vs. oral antibiotics for uncomplicated preseptal cellulitis.34,35 Selection of antibiotics depends on the underlying etiology, summarized in Table 7. In uncomplicated patients with preseptal cellulitis, such as those due to a hordeolum, an insect bite, or eczema, oral dicloxacillin or a first-generation cephalosporin can be used. If there is suspicion for MRSA based on community prevalence or failed methicillin-sensitive S. aureus treatment, then oral clindamycin or trimethoprim-sulfamethoxazole is recommended.32,36 Frequent warm compresses markedly shorten the clinical course. Expect clinical improvement to occur within 24 to 48 hours.32 These patients can be discharged home with close follow-up with a primary care provider within 24 to 48 hours.
If sinusitis is a suspected underlying cause, consider high-dose amoxicillin-clavulanate or a third-generation cephalosporin for 10 to 14 days to cover for S. pneumoniae, H. influenzae, and M. catarrhalis. Also consider referring the patient to otolaryngology.32,37 If dental disease is the etiology, consider dental evaluation as well as oral clindamycin, high-dose amoxicillin-clavulanate, or ampicillin-sulbactam to cover for aerobic and anaerobic flora.32,36
Complications of preseptal cellulitis include local abscess formation, development of orbital cellulitis, and extension of infection into the intracranial space.32 If there is suspicion for complicated preseptal cellulitis, we recommend emergent ophthalmologic consult to rule out orbital cellulitis, as differentiating these two entities clinically may be difficult, as further discussed below. In severe or complicated preseptal cellulitis, providers should give IV clindamycin or vancomycin to cover MRSA and consider broader Gram-positive and Gram-negative coverage with cefotaxime or ceftriaxone.32,36 (See Table 7.)
Orbital Cellulitis
Definition/Etiology. Orbital cellulitis is defined by an invasive bacterial infection of the orbit or intraocular structures posterior to the orbital septum,32 most commonly due to sinusitis.33 In one study, 40 out of 41 patients (98%) with orbital cellulitis had sinusitis.38 S. pneumoniae, M. catarrhalis, Haemophilus species, S. aureus, group A Streptococcus, and upper respiratory anaerobes are the most common bacterial etiologies.33 Fungal etiologies also should be considered in an immunocompromised patient. Trauma also may be an inciting factor.
Clinical Features. Consider orbital cellulitis in a patient with a history of sinusitis-like symptoms, such as a prolonged upper respiratory infection, and in a patient with concerning unilateral eye symptoms. The seven most distinguishing ocular signs of orbital cellulitis are:
- Restriction of or pain with extraocular movements, especially with diplopia;
- Proptosis (see Figure 4);
- Decreased visual acuity;
- Afferent pupillary defect;
- Decreased color vision, especially red;
- Conjunctival involvement, especially with chemosis (see Figure 4);
- Papilledema of the optic nerve.
Figure 4. Orbital Cellulitis |
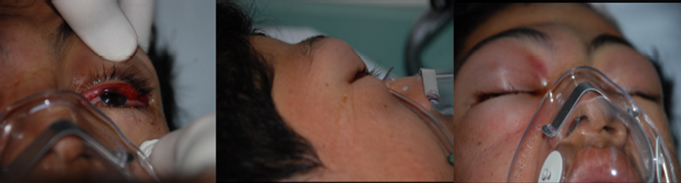 |
|
Image courtesy of Marianne Gausche-Hill, MD |
These signs and symptoms are due to infection of the ocular and orbital structures behind the septum or a posterior orbital abscess invading the orbital space. Optic nerve involvement is an ominous sign and is suggested by an afferent pupillary defect. Additional complications include subperiosteal abscess, cavernous sinus thrombosis, or extension in the intracranial space. These can cause permanent loss of vision and can be associated with notable morbidity and even mortality.33
Systemic symptoms may include fever, leukocytosis, malaise, headache, altered mental status, sinus pressure, or pain to palpation. Since the frontal sinuses do not form until 8 to 10 years of age, sinus symptoms may be absent in younger children.
Diagnosis and Management. Orbital cellulitis requires emergent consultation with ophthalmology. Providers should obtain a computed tomography (CT) scan in all patients with suspected orbital cellulitis since the results might affect medical management.
Inpatient hospitalization is recommended for patients with orbital cellulitis, both for close monitoring and for IV antibiotic therapy. Multiple services, including general pediatrics, ophthalmology, otolaryngology, and possibly plastic surgery, should be involved in the patient’s care. The antibiotic regimen can include a third-generation cephalosporin, such as ceftriaxone, to cover common sinusitis pathogens, and clindamycin or vancomycin to cover MRSA.32 The timing and need for surgical intervention is determined by the ophthalmologist and is aimed at infection control, abscess drainage, and obtaining wound cultures to guide antimicrobial treatment.
Case 2 Conclusion
Given the patient’s pain with extraocular motion and subtle proptosis, a CT scan was obtained confirming orbital cellulitis with sinus disease, and ophthalmology was consulted immediately. The patient was admitted and started on ceftriaxone and IV vancomycin, and was managed jointly by general pediatrics, ophthalmology, otolaryngology, and plastic surgery. After approximately 48 hours of IV antibiotic therapy, her symptoms improved and by day 5 of her hospitalization, she was transitioned to cefdinir and oral vancomycin. After she continued to demonstrate clinical improvement on oral therapy, she was discharged home on day 7 on these antibiotics to complete a full 14-day course of treatment.
REFERENCES
- Centers for Disease Control and Prevention. Average annual rate of eye-related emergency department visits for injuries and medical conditions, by age group—United States, 2007-2010. May 10, 2013. Available at: https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6218a9.htm. Accessed Oct. 25, 2017.
- O’Connor MM, King MA. Visual diagnosis: 2-month-old girl with left eye swelling, profuse tearing. Pediatr Rev 2013;34:e27-30.
- Olitsky SE. Update on congenital nasolacrimal duct obstruction. Int Ophthalmol Clin 2014;54:1-7.
- Takahashi Y, Kakizaki H, Chan WO, Selva D. Management of congenital nasolacrimal duct obstruction. Acta Ophthalmol 2010;88:506-513.
- Orge FH, Boente CS. The lacrimal system. Pediatr Clin North Am 2014;61:529-539.
- Pediatric Eye Disease Investigator G. Resolution of congenital nasolacrimal duct obstruction with nonsurgical management. Arch Ophthalmol 2012;130:730-734.
- Ali MJ. Pediatric acute dacryocystitis. Ophthal Plast Reconstr Surg 2015;31:341-347.
- Udeh BL, Schneider JE, Ohsfeldt RL. Cost effectiveness of a point-of-care test for adenoviral conjunctivitis. Am J Med Sci 2008;336:254-264.
- American Academy of Ophthalmology Cornea/External Disease Panel. Preferred Practice Pattern® Guidelines. Conjunctivitis. San Francisco, CA: American Academy of Ophthalmology; 2013.
- Leonardi A. The central role of conjunctival mast cells in the pathogenesis of ocular allergy. Curr Allergy Asthma Rep 2002;2:325-331.
- Bielory BP, O’Brien TP, Bielory L. Management of seasonal allergic conjunctivitis: Guide to therapy. Acta Ophthalmol 2012;90:399-407.
- Bielory L. Allergic conjunctivitis: The evolution of therapeutic options. Allergy Asthma Proc 2012;33:129-139.
- Azari AA, Barney NP. Conjunctivitis: A systematic review of diagnosis and treatment. JAMA 2013;310:1721-1729.
- Berger WE, Granet DB, Kabat AG. Diagnosis and management of allergic conjunctivitis in pediatric patients. Allergy Asthma Proc 2017;38:16-27.
- Castillo M, Scott NW, Mustafa MZ, et al. Topical antihistamines and mast cell stabilisers for treating seasonal and perennial allergic conjunctivitis. Cochrane Database Syst Rev 2015(6):CD009566.
- Sambursky RP, Fram N, Cohen EJ. The prevalence of adenoviral conjunctivitis at the Wills Eye Hospital Emergency Room. Optometry 2007;78:236-239.
- Zhang L, Zhao N, Sha J, et al. Virology and epidemiology analyses of global adenovirus-associated conjunctivitis outbreaks, 1953-2013. Epidemiol Infect 2016;144:1661-1672.
- LaMattina K, Thompson L. Pediatric conjunctivitis. Dis Mon 2014;60:231-238.
- Wilkins MR, Khan S, Bunce C, et al. A randomised placebo-controlled trial of topical steroid in presumed viral conjunctivitis. Br J Ophthalmol 2011;95:1299-1303.
- White ML, Chodosh J. Herpes Simplex Virus Keratitis: A Treatment Guideline. Hoskins Center for Quality Eye Care, American Academy of Ophthalmology in the Compendium of Evidence-Based Eye CareTM. 2014.
- Weiner G. Demystifying the ocular herpes simplex virus: Basic principles and common misconceptions. EyeNet, American Academy of Ophthalmology. January 2013:41-46.
- Rietveld RP, ter Riet G, Bindels PJ, et al. Predicting bacterial cause in infectious conjunctivitis: Cohort study on informativeness of combinations of signs and symptoms. BMJ 2004;329:206-210.
- Narayana S, McGee S. Bedside diagnosis of the ‘red eye’: A systematic review. Am J Med 2015;128:1220-1224 e1221.
- Palmu AA, Herva E, Savolainen H, et al. Association of clinical signs and symptoms with bacterial findings in acute otitis media. Clin Infect Dis 2004;38:234-242.
- Non-HIV Antiviral Drugs. In: Kimberlin DW, Brady MT, Jackson MA, Long SS, eds. Red Book® 2015: Committee on Infectious Diseases; American Academy of Pediatrics. 30th ed: American Academy of Pediatrics; 2015:919-926.
- Herpes Simplex. In: Kimberlin DW, Brady MT, Jackson MA, Long SS, eds. Red Book® 2015: Committee on Infectious Diseases; American Academy of Pediatrics. 30th ed: American Academy of Pediatrics; 2015:432-445.
- Browner EA. Corneal abrasions. Pediatr Rev 2012;33:285-286.
- Wipperman JL, Dorsch JN. Evaluation and management of corneal abrasions. Am Fam Physician 2013;87:114-120.
- American Academy of Ophthalmology Cornea/External Disease Panel. Preferred Practice Pattern® Guidelines. Blepharitis. San Francisco, CA: American Academy of Ophthalmology; 2013.
- Wladis EJ, Bradley EA, Bilyk JR, et al. Oral antibiotics for meibomian gland-related ocular surface disease: A report by the American Academy of Ophthalmology. Ophthalmology 2016;123:492-496.
- Lindsley K, Nichols JJ, Dickersin K. Non-surgical interventions for acute internal hordeolum. Cochrane Database Syst Rev 2017;1:CD007742.
- Hauser A, Fogarasi S. Periorbital and orbital cellulitis. Pediatr Rev 2010;31:242-249.
- Aguilera ZP, Chen PL. Eye pain in children. Pediatr Rev 2016;37:418-425.
- Al-Nammari S, Roberton B, Ferguson C. Towards evidence based emergency medicine: Best BETs from the Manchester Royal Infirmary. Should a child with preseptal periorbital cellulitis be treated with intravenous or oral antibiotics? Emerg Med J 2007;24:128-129.
- Cannon PS, McKeag D, Radford R, et al. Our experience using primary oral antibiotics in the management of orbital cellulitis in a tertiary referral centre. Eye (Lond) 2009;23:612-615.
- Stevens DL, Bisno AL, Chambers HF, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis 2014;59:e10-52.
- Chow AW, Benninger MS, Brook I, et al. IDSA clinical practice guideline for acute bacterial rhinosinusitis in children and adults. Clin Infect Dis 2012;54:e72-e112.
- Nageswaran S, Woods CR, Benjamin DK Jr., et al. Orbital cellulitis in children. Pediatr Infect Dis J 2006;25:695-699.
- Kimberlin DW, Jacobs RF, Weller S, et al. Pharmacokinetics and safety of extemporaneously compounded valacyclovir oral suspension in pediatric patients from 1 month through 11 years of age. Clin Infect Dis 2010;50:221-228.
- Gonococcal Infections. In: Kimberlin DW, Brady MT, Jackson MA, Long SS, eds. Red Book® 2015: Committee on Infectious Diseases; American Academy of Pediatrics. 30th ed: American Academy of Pediatrics; 2015:356-367.
- Chlamydia trachomatis. In: Kimberlin DW, Brady MT, Jackson MA, Long SS, eds. Red Book® 2015: Committee on Infectious Diseases; American Academy of Pediatrics. 30th ed: American Academy of Pediatrics; 2015:288-294.
Eye problems, particularly conjunctivitis and periorbital swelling, are very common. The majority are managed easily, but more serious disease processes must be considered. Early recognition and prompt treatment of more serious etiologies, such as gonococcal conjunctivitis and herpes simplex virus, can prevent vision loss.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
